Review Article - (2017) Volume 25, Issue 5
ZHEN LING TEO
Singapore National Eye Center, Singapore Singapore Eye Research Institute, Singapore
LOUIS TONG*
Singapore National Eye Center, Singapore Singapore Eye Research Institute, Singapore Duke-NUS Medical School, Singapore Yong Loo Lin School of Medicine, National University of Singapore, Singapore
Corresponding Author:
Louis Tong
Head of Ocular Surface Research Group
Singapore Eye Research Institute, Singapore
Tel: (65) 6227 7255
E-mail: louis.tong.h.t@singhealth.com.sg
Submitted date: September 26, 2017; Accepted date: October 10, 2017; Published date: October 17, 2017
In rapidly aging populations, the increasing prevalence of chronic diseases represents the biggest challenge of modern health care. Many interventions have been performed worldwide to encourage the integration of primary care and specialised services for the treatment of chronic diseases traditionally managed by specialists. Such interventions have been recently reviewed, and are found to vary in value and cost effectiveness. An example of a 'specialised chronic disease' is dry eye, also known as Keratoconjunctivitis sicca. In this article, we will propose specific interventions in dry eye at the primary-secondary care interface, based on evidence seen in other health conditions. 'Integration' does not aim to physically relocate a specialised clinic into the community. Instead, it is characterized by the interaction between a specialist and a team of community carers who perform secondary care, or the care of post-hospital discharge patients. Community carers may include general practitioners with a special interest in dry eye, optometrists, psychologists, nurses or social workers. Professional and patient behavioural changes are also critical for healthcare integration. With the use of specific effective measures, the integration of specialist and community healthcare services can provide holistic, efficient and affordable care.
Primary care; Integrated care; Dry eye disease
Worldwide, there is heightening interest in integrated health care and the potential benefits of integration between primary care and specialised health services. Several investigators have claimed that such integration is critical for an efficient and sustainable health delivery model. However, unless the term integration is carefully defined, it is often misunderstood, leading to a lack of concrete action and ineffective measures.
The evidence in favour of health integration has been examined recently by Winpenny et al. in 2017 [1]. Specific interventions at the primary-secondary care interface were classified into 5 domains. These interventions were then summarized and evaluated. The 5 domains are: Transfer of services from hospital to primary care; relocation of hospital services to primary care; liaison between primary care practitioners and specialists; professional behaviour change to reduce rates of referral; and patient behavioural change. The review showed that different interventions have varying extents of cost-effectiveness. However, in practice, it is unclear if the evaluated interventions are effective in other diseases not previously studied [1].
Based on the collective evidence for intervention [1], we aim to identify interventional measures that are feasible and beneficial to a specific disease context. Dry eye is used in this article as a model to assess these interventions for integrative care as it has a chronic nature, significant population burden, and multiple holistic risk factors [2] (Supplementary File). Please refer to the Table 1 for the definition of terms used in this paper.
| Chronic Disease | A chronic disease is defined by the U.S. National Center for Health Statistics as a disease that last for 3 months or more. In some countries, many chronic diseases are currently managed by specialists in tertiary centres. |
| Primary Care | Primary care is the first level of health care contact for individuals, families and the community. It constitutes the first step of a continuing health care process. In Singapore, primary care is provided by general practitioners in outpatient polyclinics and private general practitioners clinics. |
| Tertiary Care | Tertiary care refers to specialised consultative care provided by hospitals. Specialised consultative care is delivered by specialists working in a center that has the personnel and facilities for special investigation and treatment. |
| Medical specialist | A doctor who has received advanced training and education in a specific and limited area of medicine. |
| Dry eye disease | A multifactorial disease of the tears and ocular surface that can result in ocular discomfort and visual impairment |
| Integrated care | In this article, we define integrated care as a coordinated care service provided by both specialists and primary care physicians. It involves the coordinated delivery of services between different health service providers to tailor to the needs and preference of the individual patient. |
Table 1: Glossary of terms used in the article.
Primary Care
The randomized trials reviewed by Winpenny et al. [1] showed that care for chronic diseases can be provided safely and effectively by primary care physicians. Primary care physicians are able to provide regular follow ups for a range of conditions including cancer, dementia and renal failure [1]. In the context of dry eye, the transfer of services can be in the form of intermediate care services provided by practitioners with a special interest in dry eye. Intermediate care services include the diagnosis and management of patients with uncomplicated dry eye. Providers of intermediate care may be general medical practitioners (GPs), optometrists or community nurses. While such intermediate care services can handle most patients with dry eye, they may require specialist help in the management of patients with severe dry eye conditions who require more medical resources for treatment. Severe dry eye conditions include patients with significant cornea epitheliopathy and non-healing epithelial defects. These patients may require bandage lenses, corticosteroids, or surgical measures provided only by specialists.
Studies have also showed that GPs who receive additional training in specific fields are able to handle post-acute follow up, including post-surgical patients [3]. Although a large majority of dry eye disease does not require surgical procedures, some patients require minor surgeries such as incision and curettage of chalazion. Chalazia are painful eyelid lumps due to obstructed meibomian glands, often found in dry eye patients [4]. It is possible for minor surgery, such as incision and curettage of chalazion and post-surgical follow up to be conducted in a community setting by a GP with a special interest in this area. However, more complex surgeries, like tarsorrhaphy to close the eyelids for cornea healing, should still be done at tertiary centres.
Evidence has also shown that the transfer of care from specialists to primary care service is beneficial for patients who have already been diagnosed by specialists and patients with previously severe disease that has since stabilized. After their visits to tertiary centres, patients can be transferred to primary care for monitoring of disease progression, instead of hospital specialist outpatient clinics for follow up. The long term monitoring of stable patients in tertiary centers is inappropriate and uneconomical if no further specialist intervention is required. By keeping stable patients in tertiary centres, there are fewer resources for other patients in need.
The transfer of the abovementioned services from hospitals to GPs may reduce hospital visits for patients and indirectly save time and effort. With this transfer, GPs may also be able to provide the coordinated and holistic care desired by patients. The medical specialist at a tertiary centre is often less familiar with the patient’s background and family resources as compared to primary care physicians. Primary care practitioners can better provide tailored advice on diet, lifestyle [5], and community comprehensive programs, which are important in the management of co-morbidities of dry eye such as depression and anxiety [6].
Studies showed that GPs were able to effectively use a wide range of diagnostic & monitoring tools [1]. GP clinics currently lack diagnostic equipment and consumables such as a slit-lamp microscope, fluorescein dye or Schirmer strip. These are required for making a definitive diagnosis of dry eye. On the contrary, such equipment are commonplace in community optometrist clinics [7]. However, few optometrist clinics are involved in the diagnosis and management of dry eye. Hence the provision of tools may empower primary care to better diagnose and manage dry eye patients. For a start, simple tools such as a hand-held camera to detect cases of significant corneal epitheliopathy and a questionnaire to monitor the severity of symptoms [8] may be provided to GPs. Further studies are required to investigate the value of such modalities as referral or diagnostic tools for dry eye.
Primary Care Settings
There is strong evidence supporting the benefits of joint clinics (specialist and primary care) in the treatment of chronic diseases [9]. However, the evidence supports only specialist attachment to primary care teams (Figure 1). The mere relocation of a hospital specialist to a community location without involvement of primary health care professionals did not provide clear benefits [10]. We do not recommend the relocation of a dry eye specialist with the entire spectrum of equipment and manpower to a clinic based in the community.
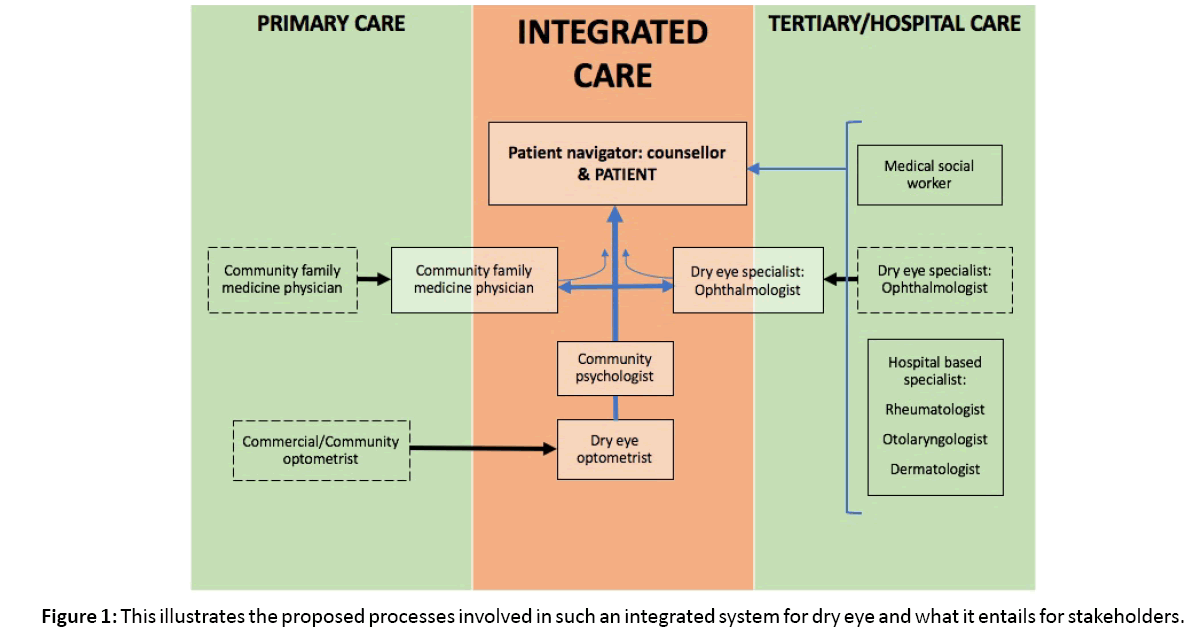
Figure 1: This illustrates the proposed processes involved in such an integrated system for dry eye and what it entails for stakeholders.
Instead, the episodic attachment of a dry eye specialist to a community clinic run by primary care professionals with an interest in dry eye may be of greater value. The specialist can provide on-site training by being physically present at periodic joint clinics held at primary care centres. Most medical practitioners have limited ophthalmic training, and 69% of medical students feel they need more training in ophthalmology [11]. Hence, providing additional ophthalmic training to GPs may address the lack of confidence in managing dry eye.
Care Physicians
Several studies have found that shared patient care between specialists and GPs can provide cost savings to patients without a loss in quality of care [1]. We suggest that shared patient care should be delivered by a multidisciplinary team, based in the community. In dry eye, the multidisciplinary team can include the primary care physician, ophthalmologist, optometrist, psychologists and medical social worker. In the presence of good communication, uniform training and shared care protocols there can be effective patient management.
The use of information technology (IT) is critical to facilitate interdisciplinary communication in a multidisciplinary team. A study showed that interventions that allowed GPs to receive email or telephone advice from specialists, reduced the number of inappropriate referrals from 25 to 10%. These interventions also resulted in an overall reduction in costs [12]. There is currently no convenient communication channel between specialists and primary care physicians for the sharing of specialist advice. This may result in unwillingness of primary care physicians to care for complex chronic diseases, resulting in increased referrals to specialists. In dry eye, communication channels such as email, telephone or web-camera can facilitate interprofessional discussions. Primary carers can send high resolution images of corneas with fluorescein staining, the patient’s symptom scores and even point-of-care test results such as tear matrix metalloproteinase-9 (an inflammatory marker found in dry eye) to specialists for advice [13]. The involvement of primary care practitioners in the use of these tests will also contribute to their training and better equip GPs to handle dry eye. However, actual e-consultations for patients have not yet been evaluated for their cost-effectiveness.
The creation of standardized coordinated care pathways improved the appropriateness of referrals to specialists. These pathways [14] should include clear criteria for the engagement of different professionals and should be part of a referral proforma. For example, the need for more sophisticated procedures such as the insertion of lacrimal punctal plugs (a procedure commonly performed for dry eye) [15] may be a criterion for referral to specialist centres.
Winpenny et al. [1] did not find evidence that financial incentives can improve referral behaviour, but we think that specific measures may still be of value in certain contexts. Some studies have put forward the concept of outcomebased payments as an alternative to traditional payments for services by individual service providers [16]. Outcome-based payments can potentially incentivize more physicians to care for chronic diseases, facilitating the transfer of patient care. It may be possible to finance patient care within a single system comprising of specialist and community carers. Unfortunately, there is limited evidence that this mode of financing is effective, except in the United Kingdom, where the budget for hospital visits is managed by a community GP [17].
The provision of subsidies for community-based services including GP clinics and community allied health services can also incentivize primary carers to acquire skills and manage more patients. Government subsidies tend to only be available for late-stage illnesses, and at public health centres. This encourages patients with chronic diseases to seek treatment from congested public polyclinics and hospitals, instead of private GP clinics. This place a strain on the manpower in public polyclinics, limiting their ability to provide the additional integrated care services suggested. Hence, the provision of GP clinic subsidies can help to shift the burden of care from public polyclinics and hospitals to GPs who form the bulk of primary care physicians. An example is the Community Health Assist Scheme (CHAS) in Singapore which allows means-tested patients to receive government subsidized care from private GP clinics. If such schemes are extended and made more ambitious, primary care services can be more easily integrated with specialised medicine.
The studies featured by Winpenny et al. [1] have showed that other tried and tested interventions focusing on professional behavior change, do not increase the appropriateness of referrals. These interventions include feedback to GPs about referrals, having an internal or external referral review or triaging center, or isolated sessions of medical education programmes [1]. We do not advocate implementing these measures to improve the quality of referrals, or to alleviate the hospital’s burden of care.
Patient trust plays a crucial role in the success of integrative medicine. Patients should cooperate when they are referred to a specific professional within the team. They should learn to trust in teams [18,19] and not only individual physicians. We suggest educating patients on the benefits of community based team care such as convenience and quality. Focus group discussions can be held with the entire healthcare team and patient to reinforce the concept of multidisciplinary team care. Consistent messages displaying interdisciplinary cooperation should also be delivered to patients during each healthcare encounter. Meanwhile, the appointment of a dedicated community-based counselor (Figure 1) or patient navigator in the team will ensure that the patient receives the appropriate healthcare services for dry eye and its associated co-morbidities, such as depression and anxiety.
We do not advocate the indiscriminate education of patients with scientific advances. In the randomised controlled trial by Leveille et al. [20], patient coaching through online resources resulted in an increase in referrals with no difference in the quality of health outcomes. The easy access to online resources can easily confuse patients, resulting in requests for unnecessary services or treatments. For example, patients with dry eye may demand specialist review and preservative-free eye drops to be supplied, even when these are not medically indicated. The risk of preservative-induced toxicity to the eye is not found to be significant if eye drops are used infrequently [21]. Unwarranted use of preservative-free eye drops may result in an overall increase in health care costs without demonstrable improvement of outcomes.
While there are benefits to an integrated healthcare system, there may be context-specific challenges that may impede these integrative efforts. In some countries, there is unequal distribution of manpower within the primary healthcare sector. In Singapore 80% of primary care practitioners are in the private sector, but the majority of chronic diseases are currently treated at public polyclinics, run by 20% of primary care practitioners [22]. A significant number of private GPs focus on acute care such as respiratory illnesses, occupational screening and aesthetic medicine. These may limit the ability of primary care centres to extend care to more chronic diseases.
In conclusion, there is a need for the seamless integration of primary and specialised healthcare services, to provide for a healthcare scene that is increasingly dominated by chronic diseases. This integration does not simply imply the relocation of a specialised clinic into the community, but rather seeks collaboration between specialists and community care professionals. Using dry eye as an example, we have proposed several specific measures to define these integrative efforts. We hold great hope that an integrated health delivery model will improve the quality, efficiency, and sustainability of our future health care system.