Quality Improvement Report - (2009) Volume 17, Issue 2
1Family Doctor, Chief Executive Officer
3Family Doctor, Head of the Quality Improvement Team
4Family Doctor, Quality Improvement Team
5Family Doctor, Quality Improvement Team
6Family Doctor, Public Health Officer Consorci d’Atencio´ Prima` ria de Salut de l’Eixample, Barcelona, Spain
Received date: 8 September 2008; Accepted date: 29 December 2008
IntroductionThe article describes evaluation of the first year of implementation of a process-management project and a quality-improvement programme linked to economic incentives carried out at CAPSE (Consortium of Primary Healthcare of Eixample, Barcelona City, Catalonia, Spain). ObjectiveTo evaluate the changes and to describe the experience of a variable payment scheme linked to quality objectives in two primary healthcare centres in Spain. MethodData from a variable payment scheme for professionals, where the variable payment consisted of three parts, were analysed. The three areas included in the variable payment were the results of management by objectives, performance evaluation, and participation in a quality-improvement programme. Parallel to this the actions of continuous quality improvement that had been proposed during 2006 were described and evaluated. ResultsParticipation among personnel in the quality- improvement programme was high, including 96% of doctors and 100% of nurses. Seventy-two improvement actions were proposed and accepted; 56% of the improvement actions took place within the established period of time, 18% did not finish within the deadline and 26% could not be accomplished for various reasons. DiscussionThe following areas needing improving were detected: process-management training for healthcare professionals, process orientation to the patients, the need to develop a communication plan, the selection of process and outcomes indicators, appropriate use of information systems and the time spent in implementation of the qualityimprovement programme. ConclusionOur preliminary results are encouraging. More studies and comparison of similar experiences are required before widespread use of this system can be recommended.
improvement groups, incentive systems, pay for performance, process management, quality management, variable payment
It is currently widely accepted that there is a need to develop new methods for evaluating and improving the quality of health care, and there is growing interest among professionals, health managers and politicians in the impact that these methods could have on health systems.[1]
In the area of primary health care in Spain, one of the first examples here, called the Proyecto Ibe´rico (Iberian Project), was carried out in 1989 between Spain and Portugal. More than 200 primary health centres started cycles of evaluation and quality-improvement strategies over the two years that the project took place.
The 1985 reform in primary health generated the creation of some highly motivated multidisciplinary teams which, with the support of quality groups within family and community medicine, incorporated quality methodology in the detection of problems.[2] However, these initiatives were altruistic, unsystematic and not rolled out.
Since 2000,when the total decentralisation of health services in Spain was achieved, Catalonia has had its own independent budgetary and planning system. The separation between finance (managed by the Servei Catala` de la Salut, referred to as CatSalut) and the provision of services allows private and not-for-profit public providers to offer publicly funded services. Historically, the ratio of public/private and not-forprofit providers is 70/30.
The Catalan administration finances and regulates primary healthcare providers through a contract that has given rise to the development of systems for monitoring indicators. The use of these indicators helps with the management of companies contracted by the government through CatSalut. The latter regularly evaluates the quality of care services supplied using these indicators. The largest public primary healthcare provider, the Catalan Health Institute (ICS), is evaluated using this model as well.
These indicators refer to the following key care attributes in primary care: quality of care/high level of performance, co-ordination with other healthcare levels, efficiency, accessibility and patient satisfaction. If these standards are not achieved by the health provider, their value, set out in the contract, is deducted from the annual Funding.
Some primary healthcare providers have introduced a model of incentives among their own professionals, incorporating variable payments related to the achievement of the standards imposed by the administration.[3] Nevertheless, none of them are linked to quality programmes. Our experience of linking quality improvement to economic incentives is the first initiative among Catalan primary healthcare providers.
The Consortium of Primary Health Care of the Eixample (Consorci d’Atencio´ Prima`ria de Salut de l’Eixample, CAPSE) is a public organisation, created in 2001 by the ICS and the Hospital Clinic of Barcelona (Hospital Clı´nic i Provincial de Barcelona, HCPB).
Since then, CAPSE has been managing two primary health teams, providing health care to almost 70 000 inhabitants in a specific area in the centre of Barcelona city.
CAPSE’s catchment area population is upper-middle class, and about 40% have double insurance cover – both public and private insurance schemes. Thirty per cent are elderly and the proportion of immigrants from non-EU countries is around 15%.
For historical reasons related to the creation of CAPSE, there is a variety of contracts among the personnel in CAPSE. There are eight civil servants from ICS, with a 35 hour per week contract; 19 civil servants from ICS, with a contract which is no longer issued, consisting of 15 hours per week, and 55 professionals with an outside contract. Human resources management is determined by two different collective agreements.
All the civil servants from ICS were working in public facilities in the Eixample quartier long before the foundation of CAPSE. In 2001 they were moved to the newly built CAPSE facilities in order to work together with the recently contracted CAPSE professionals. However, the formermaintained their contracts with ICS. The current project of quality improvement and incentives was designed only for the external professionals, who are directly contracted by CAPSE. The other professionals, contracted by ICS, were not allowed by law to receive any economic incentives from CAPIt must be mentioned that since 2001 CAPSE’s externally contracted professionals had a payment scheme which included a variable percentage in addition to the base salary, which was calculated on professional outcomes. These objectives were agreed by management and evaluated annually by the heads of each professional sector. This additional payment, which applied to all sectors and was a percentage of the total salary, ranged from 13% for medical doctors to 7% for administrative staff. This voluntary improvement in salary was not written in the collective agreement: it was a new initiative in the public health sector in Catalonia, because at that time variable payment was emerging slowly in health professionals’ salaries.SE.
In human resources terms, 82% of the professionals are of the same sex (women). There is a big generational difference: the average age of ICS professionals is 58 years, whereas the average age of external professionals is 32 years.
During the first years of CAPSE’s existence a series of problems arose related to the following issues: variability of clinical practice, low orientation to the health needs and demands of patients, financial compensation not in line with performance, and gaps in the organisation.
Thus, in 2004, management decided to take up the challenge involved in the implementation of a quality system that included a variable payment scheme. They developed tools that allowed them to improve the management of human resources and create a quality culture within the organisation, with the final objective of improving outcomes.
The objective of this project was to evaluate the changes and describe the experience of applying a variable payment system related to quality objectives in two primary healthcare centres in Spain.
Specific objectives were to:
• describe the implementation of ‘process management’
flexplain the relationship between economic incentives and the programme of quality improvement
• list and briefly describe the quality-improvement actions that developed during 2006
• debate the improvements that were brought about related to work methods and clinical outcomes
• detect the barriers in implementation of the project and detect opportunities for improvement.
In 2004 CAPSE started the implementation of process management, and due to the complexity of the project, a consultancy group was contracted to supervise the process.
During the implementation period the following stages were observed:
1 definition of mission, vision and values of CAPSE
2 management training in the methodology of process management
3 definition of the algorithm of the processes of CAPSE
4 pilot test of four managerial processes carried out by the team’s heads
5 in-house training of a first group of professionals by the team heads and delegation of ownership of the pilot processes to the professionals
6 ongoing management development of all the processes
7 creation of multidisciplinary quality-improvement groups
8 creation of the role of quality co-ordinator
9 setting up the balanced scorecard.
In 2005, participation in the quality system was evaluated and incentivised for the first time. This incentive system was incorporated into the variable payment scheme for all the professionals involved. The variable payment scheme was structured in three sections, on a percentage basis, as follows:
1 set of clinical indicators referred to as management by objectives: 50%
2 performance evaluation: 25%
3 involvement in the quality system: 25%.
Therefore, the weight of the variable payment linked to quality incentives was up to a maximum of 25% of the theoretical total bonus.
The following subheadings describe the three sections in detail.
CAPSE management, in line with the general objectives in the annual contract of the public health insurance (CatSalut), set objectives for each professional group. The results were evaluated in a system referred to as management by objectives. Each objective was measured individually, and the sum of all the indicators constituted a percentage of the achievement, which at most counted for a maximum of 50% of the total variable payment, i.e. the sum of the percentages obtained for each of the standards represented at most 50% of the variable payment.
The system of indicators was evaluated annually by an automatic auditing processing of computerised clinical records, which allowed professionals to receive continuous information regarding the evolution of their goals for the development of corrective measures, if these were considered necessary.
The number of indicators included annually in the variable payment was between 10 and 15. A number of these were indicators that the administration included in its contract with the company. Management decided which other indicators were included, depending on both projects being carried out and the objectives proposed in the process management plan.
The indicators were set according to professional status and, hence, to the activities performed: doctors (general practitioners (GPs) and paediatricians) were measured through indicators related to drug prescriptions, vaccinations and quality of care provided; nurses (community nurses, homecare nurses)were measured through indicators related to vaccinations and quality of care provided; and social workers were measured through indicators related to the quality of care provided.
For example, in the case of GPs/family medicine doctors, one indicator for drug prescriptions was the percentage of generic drugs prescribed over that year (cut-off 25%); one indicator for immunisations was the percentage of attending population over 24 years of age correctly vaccinated against tetanus over that year (cut-off 50%); and one indicator related to quality of care provided was the percentage of attending population over 14 years old having diabetes mellitus with acceptable control over that year (cut-off: mean of data values of glycosylated haemoglobin A1c under 8.0%).
The weight of the mentioned indicators within the global total varied according to its importance (decided by the executive board). The computerised datacollection process helped make the results of indicator measurement more objective.
Performance evaluation was carried out by means of a standardised questionnaire and an interview between the professional and the team leader. Between them they discussed and agreed the final score. There were no cases of absolute disagreement. The sum of the percentages obtained in each of the items in the questionnaire represented at most 25% of the total of the variable payment.
The indicator usedwas ‘to take active part (or not) in a working group’. This involvement was evaluated through the minutes issued after every meeting by the quality-improvement groups. Individuals who had participated in the quality system achieved the indicator. There was no discrimination in the level of involvement or in the level of work carried out. This indicator represented at most 25% of the total of the variable payment.
The evaluation methodology raised some issues that were broadly debated among professionals and managers. The main issues were:
• management by objectives: although the indicators were well defined and objectively analysed, the computerised register could have been inaccurate, for example, activities not carried out that were registered as actually performed, non-existent measurements that had been recorded, actual measurements that may have been decreased or increased, and so on
• performance evaluation: although this was based on a semi-structured questionnaire, it was criticised as a subjective measurement. It is well known that there is no gold standard for performance evaluation. For these reasons, the result of the evaluation carried out by the team leader had to be agreed by the evaluated person
• involvement in the quality system: as mentioned above, a professional with a low level of involvement received the same bonus as a professional with a high level of involvement.
However, the use of this payment scheme allowed the executive board to distinguish between different levels of performance among professionals and these were considered reasonably appropriate. For this reason, at the beginning of 2006 all professionals were informed of the indicators and evaluation methods that would be used at the end of the year.
During 2006 the following groups of professionals within CAPSE were involved: management, external health professionals and external non-health professional staff. In total 72 professionals, representing 88% of the people employed, were involved. Civil servants contracted by ICS were not included. In terms of professional groups, the participation of external personnel was 96% among doctors and 100% among nurses. Social workers and auxiliary nurses were included in the latter group. Participation was 57% among administrative staff. Some civil servants from ICS participated voluntarily in the project without receiving any additional payment from CAPSE: this indicated that the quality programme, traditionally not linked to economic incentives, was sufficiently attractive by itself to gain altruistic commitment of professionals without their being incentivised.
A total of 1484 hours were invested in implementing the process-evaluation cycle, developing SWOT (strengths, weaknesses, opportunities, threats) analysis, defining improvement actions and defining and managing steps that were progressively implemented, described in the process algorithm.
Furthermore, 352 hours were invested in the supervision and methodological support of the qualityimprovement groups.
The time invested can be translated into monetary equivalents based on the salary of the professionals involved in each process. Thus, by adding the quality training awards, it was possible to calculate exactly the costs of the quality-improvement cycle.
There were 12 management processes running at the beginning of 2006. Seventy-two actions of improvement were proposed and accepted. Of these, 12 were related to internal administrative processes, 16 to customer service processes, eight to research and continuous training and 36 to healthcare processes (see Table 1).
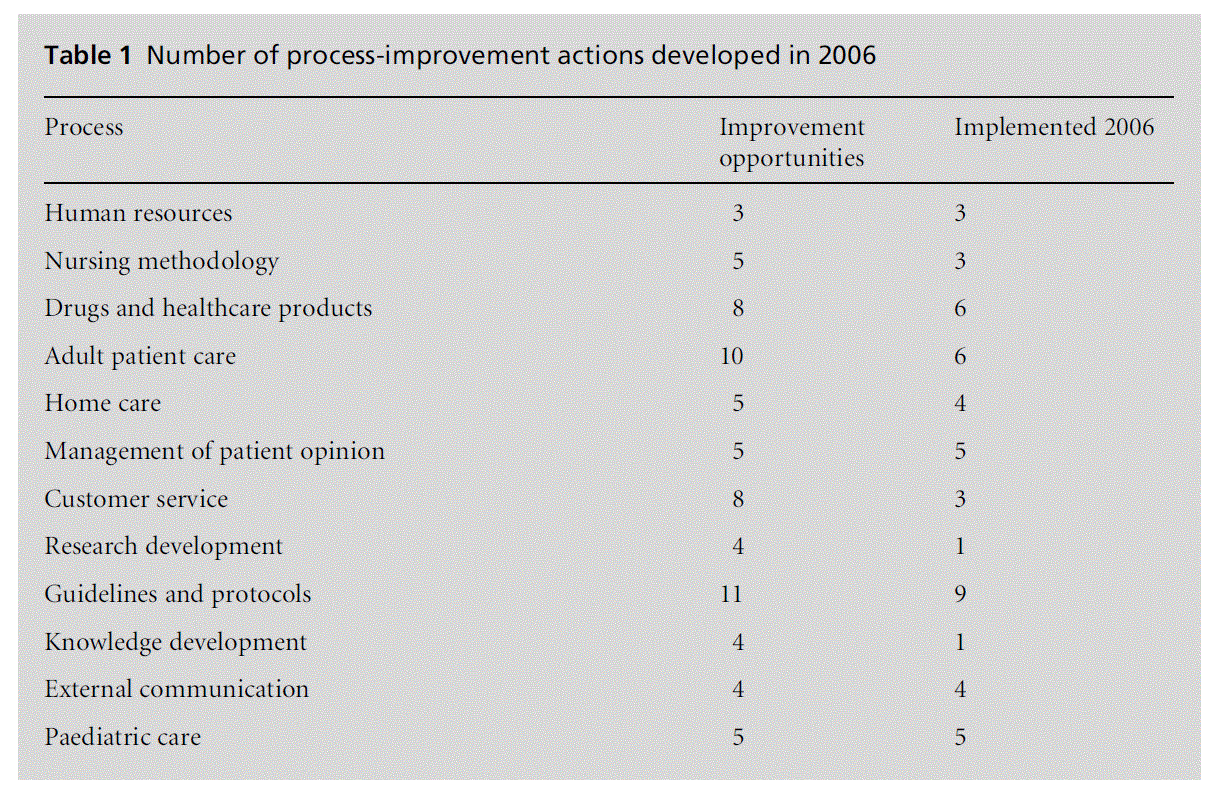
Fifty-six per cent of the quality-improvement actions were carried out within the time established, 18% did not finish within the deadline and 26% could not be successfully accomplished for varying reasons.
The quality-improvement actions were approved by management and were carried out by 24 multidisciplinary improvement groups. For example, the process ‘home care’ carried out the following improvement actions: improvement of the criteria for inclusion in the homecare programme, improvement in access for appointments with doctors and nurses, updating of intranet data, performing clinical sessions with homecare cases, and, as an ongoing improvement action, improvement in the care given by the multidisciplinary team.
By the end of the 2006 cycle there were 15 management processes taking place and two more processes had been established that were to be put into practice in the 2007 cycle. Since the beginning of the project, ten multidisciplinary protocols have been put into action.
In line with the strategy to improve knowledge in quality and process management, each year more resources were dedicated to training professionals in the areas of evaluation methodology and healthcare quality improvement.
Between 2004 and 2006, two CAPSE professionals were awarded a masters degree in methodology and evaluation of quality healthcare, and ten professionals were at different stages in their training. Furthermore, three professionals in the customer service unit had completed a 20-hour course in quality healthcare methodology.
Most professional groups achieved above 80% of the variable payment in all the three sections (see Figure 1). In the section related to management by objectives (MBO) (see Figure 2), and in the section related to performance evaluation (see Figure 3), paediatricians had the highest achievement.
In the section related to involvement in the quality system, 96% of the professionals achieved the maximum score (see Figure 4). Note that the involvement of professionals in the quality programme linked to economic incentives was nearly 100%.
The main difficulties that arose over implementation were as follows:
• quality language: this is very different from the medical language that health professionals are used to. The technical jargon of quality improvement was sometimes misunderstood by the professionals. This was revealed through qualitative analysis of the meeting minutes and in-depth interviews of the quality teams
• leadership: the commitment and involvement of the executive board in the quality system sparked the teams to go a step further when they felt they had reached a dead end. Where leadership was lacking in process management, improvement actions were less successful. For instance, in the process referred to as ‘drugs and healthcare products’, the improvement action ‘reduce the variation in the treatment of acute and chronic diseases with high prevalence in primary care’ failed by the end of the year 2006. Furthermore, the shift from a vertical to a matrix organisation chart required time and clear leadership to avoid hierarchical confusion
• information management: this includes using information technology, setting indicators and designing the balanced scorecard. The availability of information led to an excess of information which was then not used.
Existing models of payment for quality in our review of the literature differed slightly from our experience in this project. Various approaches involving different types of incentives to stimulate quality improvement,[4] or co-payments are currently impossible to implement in Spain.[5] Furthermore, pay-for-performance experiences applied to hospitals were not applicable in our case.[6,7] The recent introduction of pay-for-performance in primary care in the UK has some similarities to our model.[8] However, it would be useful to have more data available before establishing the costeffectiveness of pay-for-performance.
Emerging models of pay-for-performance in primary care are being tested in the US.[9] The trends show that quality-improvement initiatives can improve efficiency and reduce costs. However, when making comparisons between pay-for-performance schemes, the payment structure of the public health system should be taken into account. In Catalonia, where primary care professionals are usually salaried and not paid for performing quality activities, CAPSE was the first public company to create a quality-improvement model linked to economic incentives.
Below is the analysis of the key elements of the implementation of the quality programme. Our results show that the pay-for-performance system met its main objectives. Involvement of professionals in the management of the two centres was made possible throughmultidisciplinary quality-improvement groups, through leadership from the owners of each process and with the support of a quality co-ordinator. In our opinion, there was a major commitment in the decision- making process and in the culture of teamwork, even though the final results on achievement of the objectives are not yet available.
A systematic process of developing healthcare protocols and guidelines was initiated in order to provide support to professionals for decision making in the clinical setting. While the project results show that overall it has been useful, its strengths and limitations are discussed below.
The first difficulty encountered was the language of process-management methodology, which healthcare professionalswere not familiar with.Doctors and nurses, who were focused on their own clinical disciplines and not trained in quality management, showed initial opposition to a project that they thought was an improvement tool for managers rather than a tool for improving their own clinical activity. At this stage of the project, clear leadership was a facilitating element, and played a key role in reducing the resistance to change expressed by other managers, who did not always give support to the project as a whole.[10]
Training of the managers and all the professionals involved in process management was considered essential, in order to facilitate their work and gain acceptance for the culture of change. We strongly recommend a continuous education programme in quality improvement to support such initiatives.
Orientation of the patient processes was also critical. Very often patient priorities did not coincide with those of the professionals.[11] Orientation to health users can be easily understood when talking about health outcomes, but less so when talking about accessibility or time management by the professional. The expectations of patients, assessed through annual satisfaction surveys, have to be taken into account.
Other problems faced were the dissemination and progress of the project. A well-designed communication plan was fundamental when implementing such an organisational change,[12] but normally there is insufficient knowledge regarding communication strategies and, furthermore, there is insufficient administrative support because this is mainly orientated to customer services. In addition, there is often a scarcity of economic resources for such projects. Bearing the above in mind, it is important not to improvise the planning of strategies, in order to avoid future problems. When resources are scarce the best communication plan is one that managers can carry out with a positive attitude towards change, with commitment to the new methodology, and where they inform and involve their teams through team meetings and other strategies of direct communication. Indirect or ‘grapevine’ communication should be avoided.
Professional acceptance of the project was mainly positive; however, in our experience, the simultaneous introduction of a variable payment scheme, in which quality payments were included, influenced the acceptance of the project in a positive way. We may recommend the use of economic incentives in order to achieve major involvement of staff in the qualityimprovement project.
There were various elements that influenced the motivation of many personnel, such as the opportunity to improve daily activities and the recognition of professionals as experts in specific processes. It was easy for professionals to use process methods as a rigorous way of solving evident and serious problems that managers had not foreseen. In our opinion it was most important to develop the following: an organisational culture of quality; evaluation methods; improvement quality cycles; and, at the same time, flexibility with the methodology, which could be improved later once commitment to the project was established.
A further difficulty was the quantity of indicators generated at the start of the project. The professionals, with the opportunity to define the processes for the first time, had a tendency to maximise the information needed to manage them. It is recommended that those who design indicators should emphasise that they should be practically useful in the decision-making process and take into account which indicators are actually needed.[13,14]
Management of processes requires feedback and monitoring. Consequently, information analysis becomes of vital importance for systems management, as does investment in information technology. The design of the strategic map of the organisation and the definition of the balanced scorecard should facilitate the task of rationalising the numerous indicators.
Another aspect to highlight was the new information generated when the owners of processes started managing information and when they played their new role. In a typical vertical hierarchical structure, horizontal influences also occur, creating uncertainty, which can generate insecurity. Correctly defining the roles of the team head and that of the owner of the process into a matrix organisation chart, and reviewing them with those involved, facilitated good development of the project,[15] and clarified new hierarchical roles.
Finally, it was impossible for reflection to have taken place, and for improvement of group dynamics, without enough shared time of its members to do so.[16] Consequently, the cost of the project in terms of time and organisation was high, and had to be taken into consideration from the start.
We are currently working on consolidation of the project and clarification of certain questions that have arisen, such as: the role of financial incentives in the acceptance of the change process, how to identify the extent of participation of professionals in the process, new formulas to relate payment to quality performance, and to what degree the quality-improvement programme and process management improve the needs of patients. We hope future research will shed more light on these issues.
Not commissioned, externally Peer Reviewed.
None.