Research Paper - (2014) Volume 22, Issue 2
Margaret Fox MA BA (Hons)*
Sociologist, Research Fellow in Dementia Care, School of Rehabilitation Sciences, Faculty of Medicine and Health Sciences, University of East Anglia, Norwich, UK
Chris Fox MBBS BSc MMedsci MD MRCPsych
Consultant Psychiatrist and Clinical Senior Lecturer in Old Age Psychiatry, Norwich Medical School, Faculty of Medicine and Health Sciences, University of East Anglia, Norwich, UK Willie Cruickshank Director, Norfolk and Suffolk Dementia Alliance, Norwich, UK
Bridget Penhale BA MSc CQSW
Social Worker, Reader in Mental Health of Older People, School of Nursing Sciences, Faculty of Medicine and Health Sciences, University of East Anglia, Norwich, UK
Fiona Poland PhD
Sociologist, Professor of Social Research Methodology, School of Rehabilitation Sciences, Faculty of Medicine and Health Sciences, University of East Anglia, Norwich, UK
Nicholas Steel MB ChB MSc PhD FFPH
Clinical Senior Lecturer, Health Services Research, Norwich Medical School, Faculty of Medicine and Health Sciences, University of East Anglia, Norwich, UK
Corresponding Author:
Margaret Fox
School of Rehabilitation Sciences
The Queen’s Building, University of East Anglia
Norwich Research Park, Norwich, NR4 7TJ, UK
Tel: +44 (0)1603 591070
Email:m.fox@uea.ac.uk
Received date: 20 December 2013; Accepted date: 17 February 2014
Background The National Health Service (NHS) has announced its new target to increase the ‘shockingly low dementia diagnosis rate’ in England from the current level of 45% to 66% by end of March 2015. Clinical commissioning groups (CCGs) in England have committed to meeting this target. The Norfolk and Suffolk dementia diagnosis rate (DDR) is below the rate for England in some areas; across the CCGs included in this study, the average DDR was 39.9% with a standard deviation of 5.3. Aims This study aimed to explore and understand the low DDR in Norfolk and Suffolk and to learn what might be needed to support general practitioners (GPs) to meet the targets set by the UK Department of Health. Methods An online survey was developed including questions from the NationalGP Audit 2009. The link to the online survey was sent via email to all GPs in four participating CCGs in Norfolk and Suffolk. SPSS was used for descriptive analysis. Chi-square tests were conducted to identify significant differences in response rates between groups of GPs. Results The survey was completed by 28% (N = 113) of 400 GPs in 108 practices across three CCGs receiving the survey link. There was a significant difference in response rates from GPs in each CCG, but there were no significant differences in terms of their answers to the questions in the survey. GP respondents expressed confidence in their ability to identify cases of dementia for onward referral to memory services. Participating GPs also acknowledged the benefits to patients and their carers of a timely dementia diagnosis at an early stage of the disease. However, they reported concerns about the quality and availability of post-diagnostic support services for people with dementia and their carers. In this survey, GPs’ attitudesweremore positive about diagnosing dementia than those responding to the National Audit 2009. Conclusions Despite GPs’ attitudes being more positive than in 2009 about diagnosing dementia, the Norfolk and Suffolk DDR remains low. This may reflect lack of GP confidence in the quality and availability of post-diagnostic support services. This study has identified a need to map the existing postdiagnostic support services for people with dementia and to identify gaps in services. This could lead to the development of a resource which might enable GPs to provide relevant advice to newly diagnosed patients and their carers, facilitate signposting to support services, and give GPs confidence to increase the DDR in their area.
Keywords
dementia, diagnosis, general practitioners, primary care
Introduction
The National Health Service (NHS) has announced its ambition to tackle the ‘shockingly low dementia diagnosis rate’ in England with the aim of increasing the rate from 45% to 66% by the end of March 2015,[1] a target set by the UK Prime Minister. The dementia diagnosis rate (DDR) is calculated nationally and locally using the NHS Dementia Prevalence Calculator Tool. It contains algorithms for each area based on local factors, such as population size, gender and age profile, to give an estimate of the expected prevalence of dementia. The actual number of dementia diagnoses recorded on each general practitioner (GP) list is then used to calculate the dementia diagnosis rate for each area.[2] Clinical commissioning groups (CCGs) in England have committed to increasing the dementia diagnosis rate.
The DDR in Norfolk and Suffolk is consistently below the rate for England (see Table 1);[2] across the CCGs participating in this study, the averageDDRwas 39.9% with a standard deviation of 5.32. CCGs in Norfolk and Suffolk aim to increase the dementia diagnosis rates to meet the UK target. However, there is no clear understanding of reasons for the DDR in areas that are below theUK average. This is potentially problematic because it might have a negative impact on efforts to achieve this target.
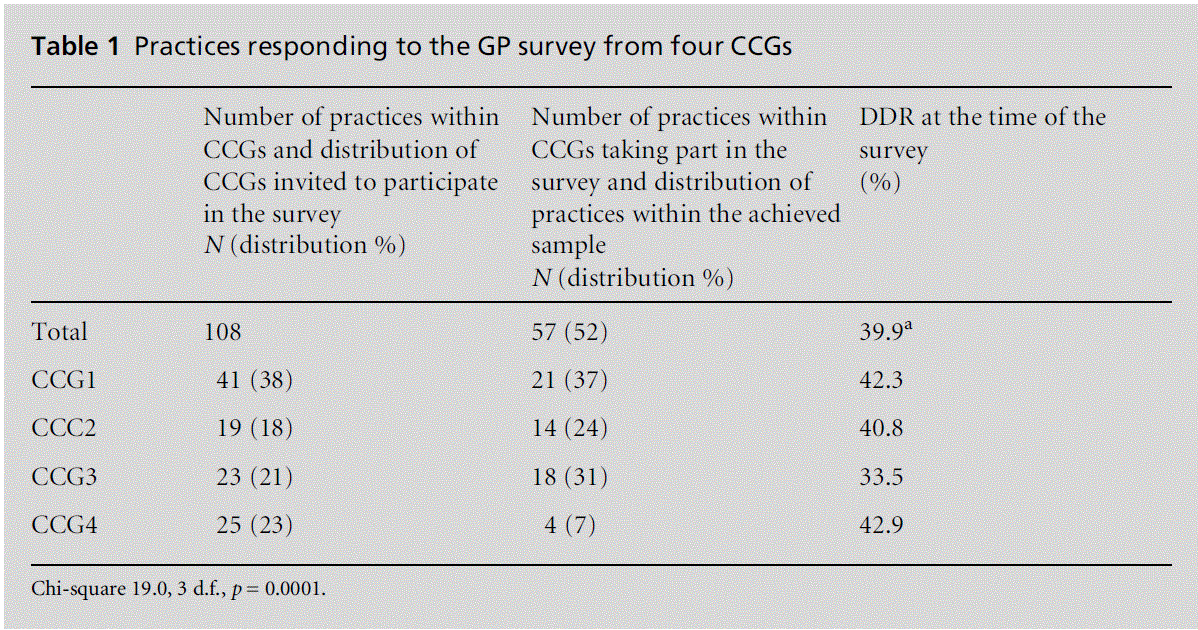
Table 1: Practices responding to the GP survey from four CCGs
This research aimed to carry out a survey of GPs in Norfolk and Suffolk to: (1) explore why the DDR in Norfolk and Suffolk is lower than the UK average DDR, and (2) to gather data to inform a strategy for increasing local DDRs.
Methods
A questionnaire was developed in consultation with Norfolk and Suffolk Dementia Alliance and the UEA Dementia Skills Staff Audit for Training Needs (DEMSTART) Advisory Group, to collect data on key indicators of GPs’ attitudes towards diagnosing dementia. The survey contained some of the key questions from the National Audit of GPs 2009 in order to assess any changes in GPs’ attitudes towards diagnosing and managing dementia since the launch of the National Dementia Strategy in 2009.[3]
A web-based survey design was used as this provided a low-cost survey, which would reach more respondents more quickly. Using web-based surveys also reduces the amount of missing data often found in postal self-completion surveys as this method can include filter questions to ensure that respondents are only asked questions relevant to them and can automatically guide them through the survey, so reducing completion time; an important factor for improving responses rates, particularly in GP surveys.[4] However, using online surveys can lead to a lower response rate.[5]
The GP survey questionnaire was uploaded onto Survey Monkey (see Appendix 1 for the paper version of the GP Survey Questionnaire). A communication strategy was developed which aimed to ensure that the survey was available to all GPs in each of the four participating CCGs within Norfolk and Suffolk. A lead person in each CCG was identified to take responsibility for implementing the survey in their area. The survey began in late July 2013, with a planned close date at the end of August 2013.However, as this period coincided with the local school vacation period, it was decided to extend the deadline to the second week of September 2013. Each lead person within the participating CCGs ensured that the link to the survey was emailed to all GPs in their area and sent out two reminders to encourage GPs to participate in the survey.
The questionnairewas sent as a link embedded in an email to all GPs practicing within three CCGs in Norfolk and Suffolk (which will be referred to as CCG1, CCG2 and CCG3 in the remainder of this paper). In the fourth participating CCG (CCG4), the survey link was embedded in a newsletter attached to an email that was sent to all GPs in this area.
Results
Responses to the survey
The questionnaire link was sent to a total of 567 GPs across Norfolk and Suffolk in 108 practices. Table 1 shows the number of general practices within each CCG invited to take part in the survey and the distribution of practices across the invited sample of CCGs. It also shows the number of practices responding to the survey and the distribution of practices in the achieved sample. The final column of Table 1 shows the DDR in each CCG at the time of the survey.
Table 1 shows that GP responses came from just over half of the practices invited to take part in the survey. It also shows that there was a significant difference in the proportion of practices within CCGs with GPs responding to the survey. There were a significantly higher proportion of practices responding in CCG2 and CCG3 than might be expected and a significantly lower proportion of practices with GPs responding in CCG4 than might be expected. The third column shows a variation in the level of diagnosis rates between the CCGs, but interestingly there is no significant difference in DDRs between the highest responding CCG (1) and the lowest responding CCG (4). It is possible that GPs in CCG4 did not see the invitation to the survey because the link (as mentioned above) was embedded in a newsletter attached to an email, rather than within an email message specifically inviting GPs to participate in the survey. Therefore, the calculation of theGP response rate excludes theGP responses from CCG4.
Four hundred GPs were invited to take part in the survey (excluding 157 in CCG4). Overall, 113 (28%) GPs completed the online survey. Table 2 shows: (1) the number of GPs in each CCG and the proportion of GPs across the CCGs invited to the take part in the survey; and (2) the number of GPs within CCGs and the proportion of GPs across CCGs invited to take part in the survey responding to the survey. A chi-square test was carried out to assess whether any of the observed proportions of GPs responding to the survey were significantly different from the expected proportions across the distribution of GPs in CCGs invited to take part in the survey.
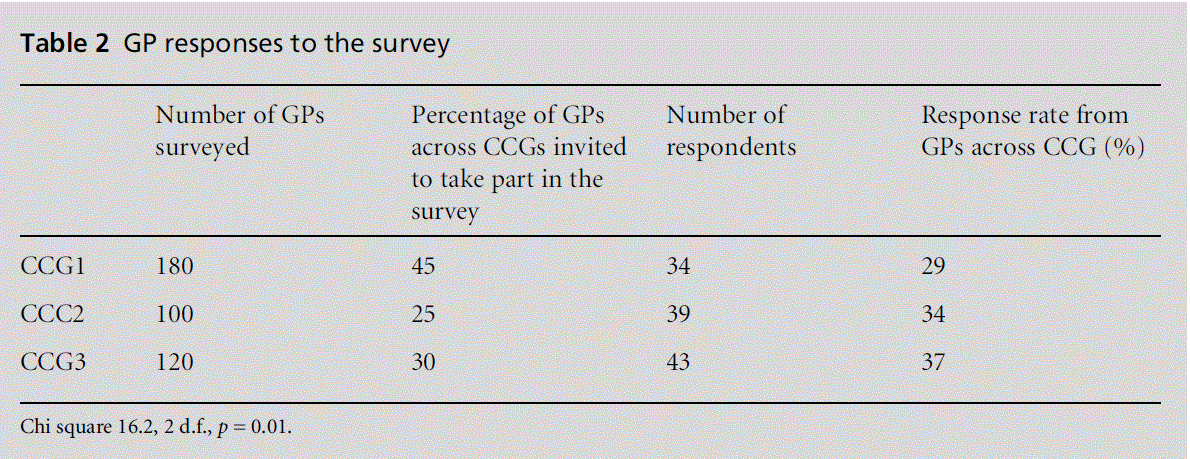
Table 2: GP responses to the survey
If GPs within each CCGs had all responded in the same proportions as the distribution of GPs across the CCGs, we would have expected the sample return to show 45% of GPs from CCG1, 25% from CCG2 and 30% from CCG3. However, only 29% of responding GPs came from CCG1, 34% from CCG2 and 37% from CCG3. The observed differenceswere statistically significant with CCG1 having a statistically significant lower proportion of responses than might be expected and CCG2 and CCG3 having a significantly higher proportion of responses than might be expected.
GPs’ attitudes to diagnosing dementia
GPs were asked to what extent they agreed or disagreed with seven statements about diagnosing dementia. They were also asked questions to assess their confidence in each of the following: (1) identifying cases of dementia for forward referral to a localmemory service, (2) advising on the management of symptoms of dementia and (3) advising carers and people with dementia about the availability of local support services. Chi-square tests were carried out to assess differences in responses to questions by GPs in each CCG. No statistically significant differences were found. Therefore, the findings are based on a descriptive analysis of the aggregated data using SPSS
Figure 1 sets out the responses from all GPs to the first seven attitudinal questions and Figure 2 sets out the answers to the three questions designed to assess levels of confidence in diagnosing and managing dementia. These are presented in descending order of agreement, as measured by percentages of the total sample. Figure 1 shows that the large majority of GPs agreed that it is beneficial to patients and their families to have a timely diagnosis of dementia (85%, N = 96). A large majority (81%, N = 92) also agreed that they had sufficient basic and post-qualifying training to identify possible cases of dementia for onward referral to a local memory service. A majority also agreed that families prefer to be told about their relative’s dementia as early as possible (72%, N = 81) and that providing a patient with a diagnosis of dementia is usually more helpful than harmful (70%, N = 79). A small minority of GPs disagreed (3%, N = 3 and 6%, N= 7, respectively) with both of these statements, with the remaining GPs neither agreeing nor disagreeing (26%, N = 29 and 24%, N = 27, respectively).
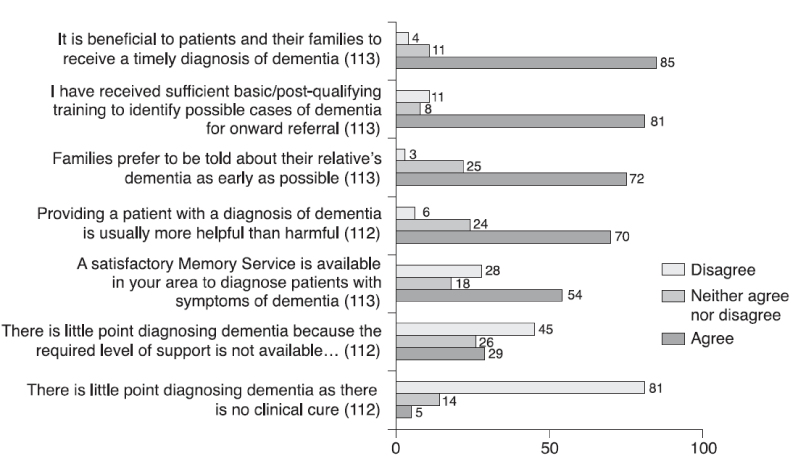
Figure 1: The extent to which GPs agreed or disagreed with each statement (%)
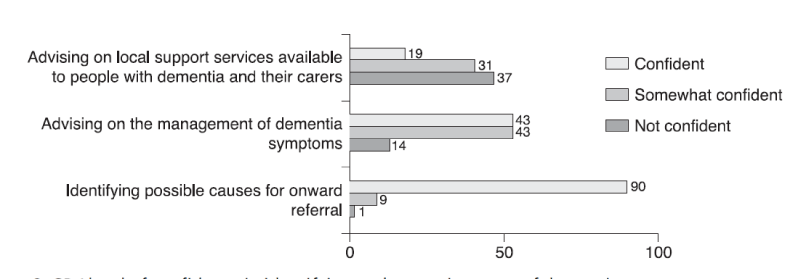
Figure 2: GPs’ level of confidence in identifying and managing cases of dementia
Just over half of all participating GPs (N = 61) agreed that there was a satisfactory memory service in their area to which they could refer people with possible or potential dementia, with 28% (N = 32) disagreeing and the remainder (18%, N = 20) stating they neither agreed nor disagreed, probably reflecting a mixed level of satisfaction with local memory services.
A large minority of participating GPs agreed that there was little point in diagnosing dementia because the required level of support for people with dementia and their carers was not available in their area following diagnosis. A small minority of participating GPs (5%, N = 6) agreed that there was little point in diagnosing dementia because there was no clinical cure.
Figure 2 shows that while 90% (N = 101) of the participating GPs were confident in their ability to identify cases of possible dementia for onward referral to a local memory service for a formal diagnosis, only 19% (N = 21) were confident of their ability to advise carers and people with dementia about other services available to them in their area and in managing the symptoms of dementia (43%, N = 49).
Discussion
This survey aimed to gather data from GPs to understand reasons for the low dementia diagnosis rate in Norfolk and Suffolk and to inform a strategy for increasing the rate to meet UK government targets. It must be mentioned, however, that the DDR is based on QualityOutcomes Framework (QOF) registers and so will be low if GPs do not record dementia diagnosis on this register; this is unlikely to be a localised challenge to increasing the DDR in Norfolk and Suffolk as the QOF is a national framework, and GPs across the UK have been incentivised to record dementia diagnoses within the QOF.
Twenty-eight per cent of the GPs invited to take part in the survey completed a questionnaire. As mentioned above, online surveys tend to achieve a lower response rate than postal self-completion surveys or telephone surveys, with responses being as low as 13% for primary care doctors participating in online surveys[4,5]. However, a benefit of web-based surveys is that data quality tends to be better than with postal self-completion questionnaires because the questions are answered more fully, reducing the level of missing data [6].
In this GP survey, each question was answered by at least 111 respondents, leading to an item response rate of 99%. Taking these issues into account, the 28% response rate is satisfactory for an online survey of GPs in primary care. Overall the survey provided a useful indication of GPs’ attitudes towards dementia diagnosis and post-diagnostic support.
It is possible that there might be some bias in the results with GPs in practices with lower DDRs being more or less likely to respond to the survey. However, on average, only one or two GPs from each practice responded to the survey. Therefore, samples of GPs within practices were too small to assess whether there was a statistical difference in response rates between practices with different in DDRs. However, the analysis indicated that this association was unlikely at the level of the CCG and therefore unlikely to have biased the results of this survey.
The NHS Dementia Prevalence Calculator was developed using robust epidemiological methods and is the most accurate tool available to estimate the prevalence of dementia presently. Therefore, the analysis of the data collected in this survey was carried out within the context of the best data available.
Taking these caveats into account, the results of this survey indicate that there have been some improvements in GPs’ attitudes towards diagnosing and managing dementia since the 2009 National Audit of GPs in the UK.[3] For example, in 2009 only 37% of GPs (based on a random sample of 1001) agreed that families would prefer to be told about their relative’s dementia as early as possible, whereas 72% of GPs in the Norfolk and Suffolk survey agreed with this statement. Additionally, in 2009 only 58% of GPs reported that they were either somewhat or very confident in advising about the management of dementia. In the Norfolk and Suffolk survey, 86% of GPs stated they were somewhat confident or confident about giving advice about the management of dementia symptoms. This gain in confidence might be expected in light of the implementation of theNational Dementia Strategy,[7]QOF’sGuidance forGMS Contract 2013/148 and the increased political debate around dementia following the UK Prime Minister’s Challenge on Dementia introduced in 2012.[9]
GPs in Norfolk and Suffolk seem to have more positive attitudes towards diagnosing dementia than those reported in earlier audits. Nonetheless, on some issues, GPs were found to be less positive and less confident, such as in their knowledge about the availability of post diagnostic support services and the satisfaction with memory services for people with dementia and their carers. In 2009, only 44% of GPs agreed that there were satisfactory specialised services for older people, and their families, in their area to meet the needs of those with dementia. In addition, over half (52%) of the GPs in the 2009 audit stated that the community mental health teams had not been in contact with them to provide support and guidance in diagnosing and managing patients with dementia. A majority (58%) of GPs stated that they were not aware of a local care pathway to guide them in the diagnosis and management of patients with dementia. Although we did not collect a full set of comparable data in this survey, the lack of reported confidence in post-diagnostic support services for people with dementia and their carers, and low levels of satisfaction with memory services expressed by GPs in this survey might indicate that little or no progress has been made since 2009 in supporting GPs to increase their dementia diagnosis rate.
Therefore, efforts to increase the dementia diagnosis rate nationally might be more effectively achieved by developing resources to support GPs in signposting patients with dementia and their families to postdiagnostic services and in providing training for them to use these resources. For example, a mapping exercise could be carried out to:
• populate a comprehensive and readily accessible regional database of current local memory and post-diagnostic support services;
• identify best practice in memory and post-diagnostic support across regions;
• inform the development of a minimumstandard of post-diagnostic support for all patients with dementia and their carers;
• identify localities deficient in the minimum standard of post-diagnostic support; and
• inform the commissioning and development of dementia post-diagnostic support options for patients with dementia and their carers.
This survey has identified some of the challenges associated with attempts by CCGs to increase diagnosis rates and suggested several steps that could be taken as part of a strategy to increase the rates achieved in future.
Acknowledgements
This survey was funded by the Norfolk and Suffolk Dementia Alliance,which identified the study requirements and developed the initial concept. This survey has benefited from the valuable support and input provided by an expert UEA Advisory Group: Professor AmandaHowe (UEA), Dr Anne Killett (UEA), and Dr Julia Baptie as GP representative. Our thanks to representatives of the Norfolk and Suffolk Clinical Commissioning Groups for collaborating with the implementations of the survey, and to all the GPs who completed the online questionnaire and gave their time freely.
Funding
This project was funded by the Norfolk and Suffolk Dementia Alliance.
Ethical Approval
This study was approved by the Ethics Committee of the Faculty of Medicine and Health Sciences, University of East Anglia, Norwich.
Peer Review
Not commissioned; externally Peer Reviewed.
Conflicts of Interest
None.