- (2013) Volume 14, Issue 4
Nilanjana Tewari1, Abed M Zaitoun2, Daniel Lindsay2, Areeg Abbas2, Mohammad Ilyas2,3, Dileep N Lobo1
1Division of Gastrointestinal Surgery, Nottingham Digestive Diseases Centre National Institute for Health Research Biomedical Research Unit, 2Department of Cellular Pathology, and 3Division of Academic Pathology; University of Nottingham, Queen’s Medical Centre. Nottingham, United Kingdom
Received February 19th, 2013 – Accepted May 17th, 2013
Context Intraductal papillary mucinous neoplasms (IPMNs) are uncommon tumours which can be associated withpancreatic and extrapancreatic malignancies. The association of IPMN and neuroendocrine tumours of the pancreas has been reported previously but is exceedingly rare. Case report We report three cases of IPMN treated with totalpancreatectomy/extended distal pancreatectomy. Histopathological analysis of the resected specimens revealedconcomitant IPMN and neuroendocrine tumour. Two patients had adenocarcinoma as well. Conclusions The presence of anIPMN may place the entire pancreas at risk of developing other tumour types and vigilance during all stages of managementis necessary to ensure optimal treatment.
Adenocarcinoma; Carcinoma, Neuroendocrine; Neoplasms, Cystic, Mucinous, and Serous; Neoplasms, Multiple Primary; Pancreas
PDAC: pancreatic ductal adenocarcinoma
Intraductal papillary mucinous neoplasms (IPMNs) are mucin-producing tumours that comprise 0.5-9.8% of pancreatic exocrine tumours [1]. IPMNs are associated with other pancreatic and extrapancreatic malignancies (colorectal, gastric, lung, breast and cholangiocarcinoma) in 25-32% of cases [2]. We report three cases of concomitant IPMN and neuroendocrine tumour, a very rare association. Two of the three patients had adenocarcinoma as well.
Abdominal CT in a 65-year-old man with malabsorption, obstructive jaundice and recent onset insulin dependent diabetes mellitus revealed a cystic mass in the head of the pancreas which was thought to be malignant, without evidence of metastatic disease.
At operation he had a large cystic lesion in the head of pancreas with mucin in the pancreatic duct which was dilated to 1.9 cm (Figure 1). As frozen section showed a solid cystic lesion with invasive cancer at the tumour margin and IPMN, a total pancreatectomy was performed. The international consensus guidelines for the management of IPMNs suggest that when adenoma or low-grade pancreatic intraepithelial neoplasia (PanIN) lesions are found intra-operatively in a resection margin, no further resection is needed, but that the presence of borderline neoplasm, high-grade dysplasia or invasive carcinoma requires an extension of the surgical resection to a negative margin, up to a total pancreatectomy [3].
Figure 1. Total pancreatectomy and cholecystectomy showing solid cystic mass in the head of pancreas with cystic changes involving the body and tail of the pancreas (top). Total pancreatectomy showing solid cystic mass in the head of pancreas with cystic changes involving the body and tail of the pancreas. The image is formed by four mega blocks stained with haematoxylin and eosin x1 (bottom).
Histopathology demonstrated IPMN, positive for CDX-2 with oncocytic metaplasia, indicating mixed intestinal and oncocytic subtypes. There was invasive carcinoma arising from the IPMN with two distinct phenotypes (Figure 2). The first had atypical cells with a glandular architecture and mucin production with prominent invasive signet ring cell areas and foci of necrosis. This was positive for MUC1, CDX2 and CK20, consistent with an invasive signet ring cell and mucinous adenocarcinoma.
Figure 2. a. Part of the lining of the cyst showing neoplastic glands with oncocytic changes (haematoxylin and eosin stain x5). b. Part of the lining of the cyst showing low branching epithelium with high grade dysplasia (haematoxylin and eosin stain x10). c. Solid component of invasive carcinoma showing typical invasive ductal carcinoma (top right and carcinoma with neuroendocrine differentiation left) (haematoxylin and eosin stain x5). d. Solid cystic component of invasive carcinoma and IPMN showing focal positivity with chromogranin A in nests of neuroendocrine carcinoma (immunohistochemistry: chromogranin A stain x5).
The second component had cells arranged in a trabecular architecture with eosinophilic cytoplasm and nuclei demonstrating prominent moulding with speckled chromatin. There was positive staining for synaptophysin and focal staining for chromagranin A (Table 1), diagnostic of a neuroendocrine carcinoma. The neuroendocrine carcinoma appeared to be arising from the IPMN. The background pancreatic parenchyma was highly atrophic and fibrotic with cystically dilated ducts. Molecular testing for K-ras showed that both tumours were wild type for K-ras.

A 79-year-old man presented with obstructive jaundice and new onset diabetes mellitus. Transabdominal ultrasound and CT demonstrated a 1.5 cm diameter common bile duct with no pancreatic or liver lesions. ERCP revealed a distal biliary stricture and biliary brushings showed adenocarcinoma cells. A biliary stent was placed at the time of ERCP.
At operation, there was a mass in the head of the pancreas infiltrating through the transverse mesocolon without vascular involvement. As there were features suggestive of IPMN in the rest of the pancreas, a total pancreaticosplenectomy with excision of the involved transverse mesocolon in continuity was performed.
Histology showed cholangiocarcinoma, IPMN of gastric subtype with low and high-grade dysplasia and low grade and in situ invasive neuroendocrine tumour of the tail of the pancreas (Figure 3). The IPMN showed focal positivity with Muc5AC, positivity with CK7 and stained negatively with CDX2, Muc2, CK20 and CEA (Table 2). The invasive carcinoma stained positively with CK7 and CEA. The neuroendocrine tumour stained positively with synaptophysin and chromogranin A. The Ki67 index of this tumour was less than 2% and testing for Kras showed wild type.
Figure 3. a. Mega block showing cystic lesions of IPMN (haematoxylin and eosin stain x1). b. IPMN showing neoplastic epithelium with micropapillary formation and overlapping nuclei indicating high-grade dysplasia (haematoxylin and eosin stain x10). c. Early invasive neuroendocrine carcinoma and neuroendocrine carcinoma in situ with cystic change in the tail of the pancreas (haematoxylin and eosin stain x1.25). d) IPMN (pancreatic subtype) showing strong positive staining (immunohistochemistry: Muc5AC stain x10).

A 67-year-old woman presented with epigastric pain and vomiting. Initial investigations including upper gastrointestinal endoscopy and flexible sigmoidoscopy were normal. CT was suggestive of a pancreatic lesion, so EUS and FNA were performed. This revealed a lesion in the body and neck of the pancreas measuring 1 cm in diameter and FNA was suggestive of neuroendocrine tumour. There was no obvious disease elsewhere and she underwent surgical resection.
At operation, the tumour was not visible or palpable. A frozen section specimen from the body of the pancreas revealed neuroendocrine hyperplasia and atypia in one section block. Therefore, extended distal pancreatectomy was performed.
Histopathology demonstrated a well differentiated pancreatic endocrine neoplasm in the body and tail of pancreas with no evidence of nuclear pleomorphism or mitoses (Figure 4). There was also focal IPMN at the margin of excision of the pancreas. On immunohistochemical analysis, the tumour stained positively with CD56, chromogranin A (Table 3) and glucagon. Ki67 index was less than 1%. Therefore, this was a well differentiated glucagonoma with an associated incidental IPMN.
Figure 4. a. Well-circumscribed tumour mass surrounded by pancreatic tissue (haematoxylin and eosin stain x1.25). b. Diffuse staining of tumour and positive staining of islets of Langerhans in surrounding tissue (immunohistochemistry: chromogranin A stain x1.25). c. Higher power image showing positive staining of tumour and islets of Langerhans in surrounding tissue (immunohistochemistry: chromogranin A stain x10). d. IPMN showing papillary formation (haematoxylin and eosin stain x20).
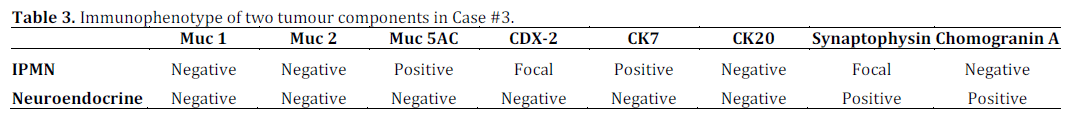
IPMNs usually occur in individuals aged 60-70 years and arise from pancreatic ductal epithelium, with the production of atypical mucin and dilatation of the main pancreatic duct or its branches. They are classified as main duct, branch-duct or combined types [4]. Clinical presentation varies from non-specific symptoms like back pain, nausea, vomiting and weight loss to recurrent pancreatitis, malabsorption and diabetes mellitus. IPMNs progress to carcinoma slowly and generally have a good prognosis.
Features suggesting malignant transformation are main duct type disease with main pancreatic duct dilatation of greater than 10-15 mm, branch duct type with tumour size greater than 3 cm and mural nodules [4]. Jaundice is more common in patients with an IPMN associated with pancreatic ductal adenocarcinoma (PDAC) than in non-invasive IPMN [5]. Concomitant PDACs occur more frequently in branch duct IPMNs, in males more than females and distal more than proximal tumours. Recent deterioration of diabetes and increase in CA 19-9 can also be predictors of the presence of PDAC in IPMNs. [6] Patients with PDAC arising in IPMN may present at an earlier stage and have a more favourable prognosis than classic PDAC. A recent study in 28 resected IPMNs showed a 78% 5-year disease-free survival [1]. In a review of existing literature, Heidt et al. suggested that IPMN should be treated with planned local resection for localised lesions with frozen section to ensure negative margins. If there is evidence of invasive disease or severe dysplasia at the resection margin, the resection should be extended up to and including total pancreatectomy. In diffuse, noninvasive disease, total pancreatectomy should also be considered to reduce the risk of recurrent, invasive disease [7].
IPMNs are divided into intestinal, pancreatobiliary, oncocytic and gastric types. In pancreatobiliary type, cells are positive for MUC1 but negative for MUC2. MUC1 immunostaining is a sensitive and specific indicator of invasiveness in IPMN [8]. K-ras mutation is seen in IPMN and mucinous neoplasms and can differentiate neoplastic pancreatic cystic lesions (IPMN) from non neoplastic cysts [9]. PDAC is generally both CK7 and CK20 positive and can also be faintly CDX-2 positive [8]. There may be a component of neuroendocrine cells which will react with somatostatin, synaptophysin, chromogranin, or other neuroendocrine markers. Mucin evaluation may be useful in evaluating prognosis. Pancreatic neuroendocrine tumours (pNETs) can be grouped by the predominant secreted hormone (e.g. somatostatin, gastrin, glucagon). pNETs show intense staining for synaptophysin and chromogranin positivity correlates with the extent of granularity on electron microscopy [10]. PNETs also stain with various keratins, including CK8, CK18, and CAM 5.2. CK7 and CK20 are usually negative [8].
Two of the three cases reported describe a typical presentation of concomitant IPMN and invasive PDAC (jaundice and new onset diabetesmellitus). The finding of neuroendocrine tumour in association with IPMN is much less common. Previous reported cases of concomitant IPMN and neuroendocrine tumour presented with abdominal and back pain, as in the third case reported in this series, or non-specific symptoms such as weight loss [11].
Two series of IPMNs found associated neuroendocrine tumours in 2.8% [12] and 4.6% [13] of cases analysed. As both tumours are rare, there has been suggestion that the frequency of association is too large to be fortuitous [13, 14]. The mechanism by which these tumour types evolve concomitantly is not yet understood. Marrache et al. [13] hypothesised that they may have a common neoplastic progenitor or there may be transdifferentiation of one cell type into another. In our study, all three tumour types found in Case #2 had weak, focal or positive staining for synaptophysin and chromogranin A suggesting that there may be neuroendocrine cells among the pancreatic ductal cells. Several molecular studies of IPMNs support the concept of a field defect. The presence of IPMN may place the entire pancreas at risk of developing other types of tumour.
The three cases reported may represent a new subtype of IPMN which is associated with neuroendocrine carcinoma. Although a few cases of this association have previously been reported, it remains rare and conclusions about the associated prognosis and optimal management cannot yet be drawn. Vigilance during surgical resection, pathological and immunohistochemical examination is required to identify these unusual tumours for further study.
None to declare
N.T. is funded by a fellowship from the CORE Foundation (London, United Kingdom)