Original Article - (2018) Volume 19, Issue 4
Oguzhan Karatepe1,2, Pinar Yazici3, Muharrem Battal3
1Department of General Surgery, Medical Faculty, Yeni Yuzyil University, Istanbul, Turkey
2Department of General Surgery, Memorial Sisli Hospital, Istanbul, Turkey
3Sisli Hamidiye Etfal Training and Research Center, General Surgery Clinic, Istanbul, Turkey
Received April 09th, 2018 - Accepted June 28th, 2018
Background Pancreatic fistula rate remains a matter of debate as the most important morbidity after pancreaticoduodenectomy. The aim of the present study was to investigate the utility of V-Loc suture in laparoscopic pancreaticojejunostomy. Methods Between January 2012 and March 2017, 42 consecutive patients who underwent a totally laparoscopic pancreaticoduodenectomy were prospectively included into the study. Postoperative pancreas fistula, anastomosis duration, hospital stay, postoperative morbidity, and mortality were recorded. International study group of pancreatic fistula definition system was used to classify postoperative pancreas fistula. Results There were 25 male and 17 female patients with a mean age of 56±7 years, ranging from 38 to 75 years. The mean operation time for the surgical procedure and Pancreaticojejunostomy was 339±43 min (range: 250-415 min) and 36±4.8 min (range: 30-46 min), respectively. Ten patients (23%) had 15 complications including postoperative pancreas fistula, postoperative hemorrhage, hepaticojejunostomy stricture, and wound infection. Nine patients with postoperative pancreas fistula (21%) were as follows; Grade A: 6, Grade B: 2, Grade C: 1. There was no 30-d postoperative mortality. Conclusion This report suggests a potential utility of V-Loc suture device during laparoscopic pancreaticojejunostmy that has showed promising outcome regarding operation time and fistula rate.
Pancreaticoduodenectomy; Pancreaticojejunostomy; Pancreatic Fistula
PD pancreaticoduodenectomy; POPF postoperative pancreas fistula; TPLD totally laparoscopic pancreaticoduodenectomy
Total laparoscopic pancreaticoduodenectomy (TLPD) was first reported in 1994 by Gagner et al. [1]. During the past two decades, there has been a growing interest in minimally invasive pancreatic surgery that requires surgeons with highly experienced laparoscopic skills. Although minimally invasive approaches have several advantages including short hospital stay, less scar, decreased postoperative morbidity, there are only limited series showing their feasibility and adequacy [2, 3, 4, 5, 6, 7]. Several advantages, including faster recovery period, short hospital stay and advantageous for adjuvant therapy, have been showed in comparative series and meta-analysis [5, 8].
Despite technical advancements, postoperative complication rate continues to be high. Postoperative pancreatic fistula/anastomotic leakage (POPF) remains the single most important morbidity after pancreaticoduodenectomy (PD) with a rate reaching up to 40% [9, 10] and results in prolonged hospitalization and mortality [11]. Although the type of pancreaticoenteric anastomosis, external pancreatic duct stenting, use of perioperative somatostatin were investigated, none has been found to be effective in decreasing the POPF [11, 12, 13].
There is an adaptation period for TLPD procedure for the surgeons who perform conventional PD before. The steep learning curve is of particular concern, because pancreaticojejunostomy (PJ) anastomosis, which is the key point of PD, is the most in-demand skill and requires a sophisticated level of practice. There has been a growing interest for the use of barbed sutures, predominantly in urologic procedures within robotic approach depending on its feasible and practical application compared to other suture materials [14]. We published our recent experience in using V-loc suture device during our modified PJ technique with the promising outcome considering the fistula rate [9]. In another report pointing out the difficulties encountered in the conversion from conventional PD to the TLPD, the feasibility of our modified PJ anastomosis technique using V-Loc suture was also mentioned in detail [15]. The aim of the present study was to evaluate the utility of V-Loc suture device for PJ anastomosis during totally laparoscopic pancreaticoduodenectomy.
Patient Selection
From January 2012 to March 2017, 42 consecutive cases (25 male and 17 female) underwent TLPD procedure by the same surgical team including two experienced hepato-pacreato-biliary surgeons. Informed consent form was obtained before surgery. The local ethical committee approved this study with an IRB number of 1249 and the research was conducted in accordance with the Helsinki Declaration. Exclusion criteria for TLPD procedure included vascular involvement, previous history of pancreatic trauma or injury, history of major abdominal surgery and severe cardiopulmonary morbidity. For initial case series, small tumor size was preferred. Data collection was prospectively performed and entered in SPSS by an assistant secretary.
The outcome measures included operation time, duration of laparoscopic PJ anastomosis, postoperative morbidity and mortality rates. The clinical course was documented for each patient, and the complications were classified according to the criteria of Clavien and Dindo [16].
POPF rate was also evaluated according to the international study group on pancreatic fistula (ISGPF) definition [17]. Pancreatic fistula was diagnosed when there was measurable drain output on or after postoperative three days, with amylase content three-fold greater than the synchronous serum amylase level. Three different grades of POPF (grade A, B, C) were defined by ISGPF according to the clinical impact on the patient’s hospital course. Grade A, also called “transient fistula,” has no clinical impact. A CT scan typically shows no peripancreatic collections and the use of total parenteral nutrition, antibiotics, or somatostatin analogs are not needed. Grade B is mostly associated with abdominal pain, fever, and/ or leukocytosis, and antibiotics are usually required; somatostatin analogs may also be used. A CT scan may show peripancreatic collections. Grade C is severe, and always shows a significant change in clinical management or a deviation from the usual clinical pathway. A CT scan usually shows worrisome peripancreatic collections that require percutaneous drainage or re-exploration. Mostly, there are associated complications such as sepsis and organ dysfunction, and the possibility of postoperative mortality rises. And another common postoperative morbidity, delayed gastric emptying, according to international study group of pancreatic surgery (Grade A-B-C: nasogastric requirement in the postoperative period, unable to tolerate solid orally, vomiting, need for prokinetics).
Suture Material
Following completion of resection procedure (PD), previously transected jejunum was removed up through mesentery of transverse colon to the anastomosis field. Following seromucosal approximation with 6-0 polydioxanone (PDS), three sutures with 5-0 PDS were located into the Wirsung duct to ensure better exposure. After then, 6-inch length, green 4-0 V-Loc™ 180 barbed suture material with V20 needle was introduced for laparoscopic reconstruction. The V-Loc™ absorbable wound closure device (Covidien Healthcare, Mansfield, MA) was produced from a copolymer of glycolic acid and trimethylene carbonate, and consisted of a barbed absorbable thread armed with a surgical needle at one end and a loop end effector at the other. The barbed structure and loop end design allowed for tissue approximation without the need to tie surgical knots and squeeze the pancreatic tissue. It was fully absorbed by 180 days.
Surgical Technique
This technique was a laparoscopic modification of our previously described open PJ procedure [9]. The patient was placed on a split-leg table and positioned in reverse Trendelenburg position. The monitor was put on the patient’s left side toward the head, and the operating surgeon located between the legs of the patient or on the right side considering the stages of the procedure. Five trocars (two 5mm, two 10 mm and one 12 mm) (Figure 1) were used. After pneumoperitoneum, the operation began with staging laparoscopy. In our previous paper, the procedure until pancreatic transection was described in detail [9]. After mobilization of the head of the pancreas, a tunnel was formed between the posterior aspect of the neck of the pancreas and the anterior to the superior mesenteric and portal veins. And pancreatic parenchymal transection was performed using an endostapler. The inferior part of remnant pancreas was mobilized 2-3 cm towards the superior and laterally in preparation for easy PJ. The dissected segment of the jejunum was brought up through the dorsal plane of mesentery for reconstruction.
Firstly, the dorsal part of the jejunal seromuscular layer and the dorsal part of the capsular parenchyma of the pancreatic stump were sutured with 4-0 V-Loc suture in a continuous manner (Figures 2a, b). Following dorsal external suturing layer, at the second step, a stent was inserted into the main pancreatic duct and reconstruction process began with 2-layers end-to-side dunking technique of PJ. At an approximate length of 2 cm from the closed stump of the jejunum, a small hole about 5 mm in diameter, -considering the pancreatic duct diameter- in the jejunum on the antimesenteric side was created. Then, the dorsal inner layer was performed with interrupted stitches, 0.5-1 cm apart, using 5-0 polydioxanone (PDS) sutures. Thirdly, the ventral inner layer was created between the ventral cut edge of the pancreatic stump, and the ventral jejunal seromuscular part using 5-0 PDS interrupted sutures (Figures 3a, b). Lastly, the ventral external layer of PJ was also performed using another 4-0 V-Loc suture device (Figures 4a, b). We placed the sutures 5 -7 mm apart.
Internal pancreatic ductal stenting using 6 or 8 Fr PVC stent was routinely used without securing. The reconstruction was continued with end-to-side hepaticojejunostomy (HJ), and completed with an end-toside gastrojejunostomy. The specimen was extracted into an endobag through the extended infraumbilical trocar site. Two Jackson-Pratt drains were placed near the PJ and HJ anastomosis.
Drains remained in place for at least 5 days after surgery, and the volumes and the amylase concentration of the drainage were recorded. Drains were removed regarding the volume and structure of the drainage fluid, and also amylase concentration. After discharge, patients were recommended to visit surgical outpatient department on the postoperative day 7, then every 3–6 months for surveillance of tumor recurrence distinct from the course of adjuvant management.
Statistical Analysis
IBM SPSS version 20 (IBM, Chicago) was utilized for analysis. There were only descriptive measures. Continuous variables were represented as mean±standard deviation or median and range. Categorical variables were expressed as percentages.
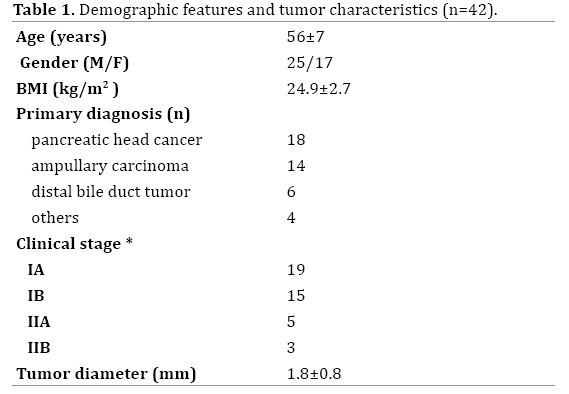
Demographic features and the underlying diseases are shown in Table 1. The mean operating time was 339±43 min (range: 280-415 min), and the mean time of PJ anastomosis was 36±4.8 (range: 30-46 min). Mean diameter of pancreatic duct was 3.5±1.2 mm (range: 3-6 mm). Mean length of hospital stay was 8.1±4 day (range: 6-34 days). Detailed surgical and postoperative data are shown in Table 2.
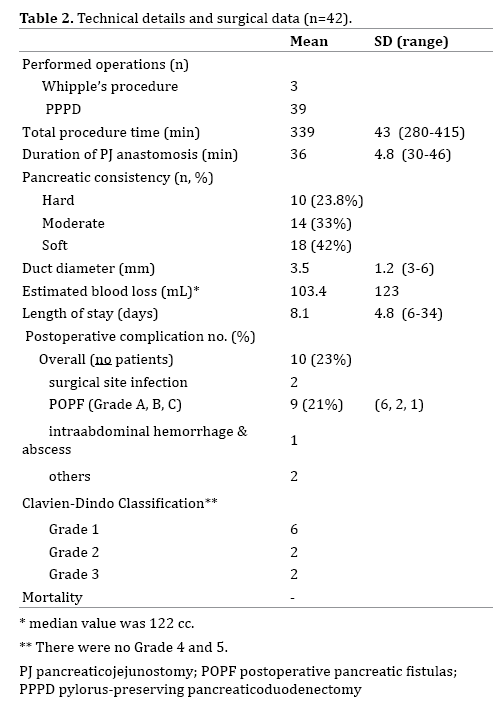
Ten (23%) patients had 15 complications and POPF was observed in nine patients (21%): Grade A in 6, Grade B in 2 and Grade C in 1 (Table 2). One patient with Grade C fistula underwent emergent reoperation due to intraabdominal abscess and subsequent hemorrhage. The recovery period was uneventful after then. One patient with HJ stricture underwent revision surgery, and reanastomosis was laparoscopically performed. One patient required percutaneous drainage catheter placement due to intraabdominal collection secondary to the POPF. The remaining complications including delayed gastric emptying (n=8, 19%) were managed conservatively. Most of them (n=5) were Grade A and no patients with Grade C were observed. There was no postoperative mortality.
Technological advances and rising availability of featured materials provide better intraoperative scores and postoperative recovery period. However, details of surgical technique remain a debate resulting in roughly similar POPF rate. In the light of this study of prospectively collected data, we suggest that the use of V-Loc suture during TLPD might be reasonable concerning with comparable results with previous series, Additionally, the V-Loc suture device can be beneficial for tissue protection avoiding tightening the pancreas after every suture bite and time-saving without need for a knot-tying.
Although minimally invasive techniques have often replaced open surgery in many abdominal surgical procedures, regarding hepato-pancreato-biliary surgery, few centers have adopted minimally invasive PD due to the complexity of the procedure and technical difficulties. PJ anastomosis is the key point in pancreatic cancer surgery. The probability of POPF after open surgery is between 5% and 40% [9, 10]. Several studies noted enhanced recovery period and significantly lower complication rates in minimally invasive PD [4, 5, 18, 19], whereas some authors reported higher or similar rate of POPF in minimally invasive approach compared to open [11, 20]. Likewise to latter group, a very recent meta-analysis of nonrandomized comparative studies demonstrated some worrisome results for the laparoscopic approach in terms of morbidity, especially when considering TLPD [21]. This could be attributed to the fact that most of the studies included are based on their initial experience. Thus, later reports probably reveal better outcomes as the surgeons overcome the learning curve.
The two-layer, end-to-side, duct-to-mucosa PJ was the most commonly used pancreatic anastomosis approach, as we also perform in our center, however, there is still no clear consensus defining 100% safe technique of pancreaticenteric anastomosis. At least ten various methods are available to prevent POPF [19]. In a very recent report by ISGPS, the risks for anastomotic complications have been mostly based on gland factors, such as texture and disease pathology. No technical variations have been found superior to another [22]. In our previous study, V-Loc knotless wound closure device used in external anastomoses of open pancreaticoduodenectomy was found advantageous and secure especially concerning soft pancreatic texture [9]. Apart from the short-term outcomes such as POPF, considering stenosis of the main pancreatic duct at the PJ anastomosis, that is one of the postoperative complications after such dunking technique, our results (2.3%) were also satisfying.
The barbed type suture was initially described for tendon repair to decrease the need for the knot and increase gripping strength between tissues. The barbed polyglyconate suture was first used for the UVA during robot-assisted radical prostatectomy beginning in 2010 [23]; safety and feasibility were previously demonstrated in several studies [24]. Application of the V-LocTM suture (Covidien, Mansfield, MA) in pancreaticojejunostomy formation may offer some advantages over conventional suture types. The V-Loc suture maintains excellent hemostasis and minimal tissue damage which is a major issue especially in patients with soft pancreas quality, provides by no need for repeated suture tightening and tissue traction after each needle passage. Moreover, barbs prevent suture slippage and distribute forces; therefore, tearing and plausible ischemic changes in the suture line are avoided.
The barbed suture technique is easy to perform which is of benefit to the surgeon during the transition period from conventional to laparoscopic or robotic PD and results in less operative time [25, 27, 28]. Most of the series using barbed sutures reported significantly shorter reconstruction time regarding V-loc suture usage for anastomosis. Tewari and colleagues recently published a retrospective comparative series -V-Loc vs. conventional suture- and noted significantly shorter total reconstruction times in V-Loc group (8 vs. 13.5 min; p<0.001) [25]. In a systematic review and meta-analysis investigating the efficacy and safety of knotless barbed sutures, both suture and operative time were found significantly reduced, and no increase was recorded with regard to the postoperative complication related to the suture material [27]. In this study, there was no comparison group laparoscopically. Comparative analysis of V-loc and conventional techniques for laparoscopic PD, Edil et al. reported less operative time with similar postoperative morbidity [28]. Our results were remarkable when compared other laparoscopic PD series. Because duration of PJ has not been routinely evaluated, it is not possible to note that PJ time is comparable.
The pancreatic texture is defined using surgeon-based experience and known to be one of the most important factors predicting the safety of anastomosis. Soft pancreas has been the most challenging type to create secure PJ avoiding POPF [29, 30, 31]. In the present study, during laparoscopic surgery, in which tactile function is absent or limited, we identify pancreatic texture during needle passing and observing elasticity gripping the pancreatic tissue delicately with a laparoscopic hand instrument. Considering quite high frequency of soft pancreas in our series that was around 40%, the frequency of POPF was 21%. This might be related to the aforementioned features of barbed suture. Edil et al. reported similar POPF rate in their comparative studies (V-loc vs. conventional suture technique), however, pancreatic texture was not mentioned in [28].
There has been a steep learning curve for laparoscopic PD, regarding especially PJ reconstruction. Difficulties during learning period were also reported in our previous paper [15]. However, we have observed easier adaptation to laparoscopic PD using V-loc suture for PJ. The shorter time for anastomosis and comparable costs were among other advantages. In the present study, we incorporated V-Loc suture into the PJ technique during TLPD. Interpreting our experience in open and laparoscopic approach, we assume that, V-Loc barbed suture allows the surgeon to focus particularly on subsequent stitch placement without any effort to prevent slippage of the suture ensuring more efficient workflow.
Laparoscopic PD remains limited to small series of patients due to technically challenging. Suturing is one of the key points of PJ anastomosis during TLPD, as also mentioned by Kendrick et al. presenting the tips of the TLPD underlining the “suturing skill is a must” [7, 32]. Given the autonomous locking mechanism of the V-Loc through a non-traumatic way, no tension or squeeze of the pancreas or knotting is required. In our study, the rate of POPF and overall morbidity were 20% and 23%, respectively. These remarkable results were attributed to a long-standing experience in conventional PD. Given the growing experience in laparoscopic procedures; complication rate is decreasing whereas popularity of this approach is rising.
Despite its merit, limitations of our study included small size, nonrandomized, single surgical team cohort, the lack of a control group and short-term follow-up.
In the last decade, rising trend in minimally invasive approach in hepato-pancreato-biliary surgery has provided promising outcome, especially in pancreaticoduodenectomy that result in enhanced recovery. The primary challenge is the pancreaticojeunostomy, the most technically demanding part that directly affects the outcome. Application of the V-Loc suture in pancreaticojejunostomy is technically easier which is of advantage to the surgeon learning laparoscopic PD and provides promising outcome.
Karatepe O and Battal M contributed to the conception and design, acquisition of data, or analysis and interpretation of data; Karatepe O and Yazici P drafted the article or revising it critically for important intellectual content; Karatepe O and Battal M made the final approval of the version to be published.
Authors declared no conflict of interest and financial disclosure.