Research Paper - (2011) Volume 19, Issue 5
1Specialist Registrar in Geriatric and General (Internal) Medicine, St James’s Hospital, Dublin, Ireland
2Consultant Physician and Geriatrician, St Vincent’s University Hospital, Dublin, Ireland
3Professor of Geriatric Medicine, Consultant Physician and Geriatrician, St James’s Hospital, Dublin, Ireland
Received date: 15 February 2015; Accepted date: 26 July 2011
Background The adoption of a frailty paradigm in primary care would be helpful to identify adults who need priority access to specialised resources. The frailty phenotype by Fried et al1 is a popular operationalisation of frailty, but it is not easily applicable in routine primary care practice. We recently created and validated a frailty instrument based on the Survey of Health, Ageing and Retirement in Europe (SHARE-FI),2 in order to provide primary care practitioners with an easy, reliable and freely accessible tool for the assessment and monitoring of frailty in community dwelling adults over the age of 50 years (www.biomedcentral.com/1471– 2318/10/57). Aim To provide further prospective validation of SHARE-FI, with a focus on disability. Methods Design: longitudinal study (wave 1: 2004– 2006; mean follow-up: 2.4 years). Setting: European population-based survey (12 countries). Subjects: 17 567 community dwelling participants (mean age 63.3 years), of whom 13 378 (76.2%) were non-frail, 3438 (19.6%) pre-frail and 751 (4.3%) frail. Main outcome measures: number of difficulties with basic (ADL) and instrumental (IADL) activities of daily living. Statistical analyses: repeated measures ANOVA with adjustment for baseline age. Results By wave 2, 3.6% of the non-frail, 12.2% of the pre-frail and 30.4% of the frail had increased their number of ADL difficulties by at least one. Likewise, 6.6% of the non-frail, 20.4% of the prefrail and 36.6% of the frail had, by wave 2, increased their number of IADL difficulties by at least one. Table 1 shows the repeated measures ANOVA suggested. Conclusion SHARE-FI may contribute to quality in primary care by offering a quick and reliable way to assess and monitor frailty in community dwelling individuals over the age of 50 and prioritise their access to resources, and it serves as a novel tool for audit and research.
diagnostic tests, frail elderly, persons with disabilities, primary health care, validation studies
Frailty in older adults is a key clinical concept characterised by dysregulation of multiple biological systems, accumulation of deficits, vulnerability to stressors and increased risk of adverse outcomes.[3,4] Even though there is still no international consensus on the definition of frailty,[5] one of the most widely accepted operationalisations is that of Fried et al, who defined it as a clinical syndrome in which three or more of the following criteria are present: self-reported exhaustion, unintentional weight loss, weakness (by grip strength), slowness (by walking speed) and low physical activity.[1]
Frailty, comorbidity (i.e. multiple chronic conditions) and disability (i.e. difficulties with activities of daily living) are commonly used interchangeably to identify vulnerable older adults, but there is a growing consensus that these are distinct clinical entities that are causally related.[6,7] Consistently in longitudinal studies, the frailty phenotype by Fried et al has been found to be a significant predictor of new-onset disability in older adults.[8–10] The frailty phenotype also predicts falls,[8,11,12] hospitalisation,1 institutionalisation [13] and death.[8,12,14,15]
Because of its predictive abilities, frailty is an emerging concept in primary care that may provide commissioners of health care with a clinical focus for targeting resources at an ageing population.[16] However, operationalising the frailty phenotype on an individual patient requires complex calculations on a reference sample, which is not practical in the context of primary care. Indeed, family physicians and community practitioners are in need of easy instruments for determining frailty.[17]
In order to provide European community practitioners with an easy frailty metric, we recently developed a frailty instrument for primary care (SHAREfi) based on the Survey of Health, Ageing and Retirement in Europe.[2] SHARE-fiis freely accessible on the website of BMC Geriatrics (www.biomedcentral.com/ 1471–2318/10/57) and its use is intended (via downloadable calculators) for community dwelling adults over the age of 50 years. We previously found that SHARE-fihas sufficient concurrent validity and is a powerful predictor of mortality.[2] In this report we further validate SHARE-fias a predictor of incident disability.
The full methodology for the development of SHAREfiis detailed in our main publication,[2] which departs from the premise that frailty is a complex, multidimensional concept that cannot be defined with a single measurement or variable. Frailty was therefore constructed as an unobserved (latent) variable that is indicated by five different (but related) observed variables; the latter were selected by Santos- Eggimann et al[18] from the SHARE questionnaire as being closest to those identified by Fried et al:[1]
flexhaustion was identified as a positive response to the question: ‘In the last month, have you had too little energy to do the things you wanted to do?’
• The weight loss criterion was fulfilled by reporting a ‘Diminution in desire for food’ in response to the question: ‘What has your appetite been like?’ or, in the case of a non-specific or uncodeable response to this question, by responding ‘Less’ to the question: ‘So, have you been eating more or less than usual?’
• Weakness was assessed by handgrip strength (Kg) using a Smedley dynamometer (S Dynamometer, TTM, Tokyo, 100 Kg), according to the following measurement protocol: participants were instructed to stand (preferably) or sit, with the elbow at 908, the wrist in neutral position, keeping the upper arm tight against the trunk, and the inner lever of the dynamometer adjusted to suit the hand; and they were then instructed to squeeze as hard as possible for a few seconds.[19] Two consecutive measurements were taken from the left and right hands. The highest of the four was selected. This variable was kept continuous.
• Slowness was defined as a positive answer to either of the following two items: ‘Because of a health problem, do you have difficulty (expected to last more than three months) walking 100 metres?’ or ‘... climbing one flight of stairs without resting?’
• The low activity criterion was assessed by the question: ‘How often do you engage in activities that require a low or moderate level of energy such as gardening, cleaning the car, or doing a walk?’ This variable was kept ordinal: 1 = ‘More than once a week’; 2 = ‘Once a week’; 3 = ‘One to three times a month’ and 4 = ‘Hardly ever or never’.
SHARE-fiwas created via estimation of a discrete factor (DFactor) model based on the above five frailty variables, using the LatentGOLD1statistical package (version 4.5.0). A single DFactor with three ordered levels or latent classes (non-frail, pre-frail and frail) was modelled for each gender.[2] Based on these analyses, two web-based calculators (one for each gender) were created for easy retrieval of a subject’s frailty class (relative to the SHARE sample) given any five indicator measurements. The SHARE-ficalculators use a linear combination of the standardised variables that have been entered, and incorporate the loadings of each of the indicator variables on the original DFactor.
The final formula for the predicted DFactor score (DFS) in females was:
DFS (females) = (2.077707 * Fatigue – 0.757295) * 0.4088 + (3.341539 * Loss of appetite – 0.332289) * 0.3325 + (0.132827 * Grip strength – 3.534515) * –0.4910 + (2.627085 * Functional difficulties – 0.461808) * 0.6012 + (0.918866 * Physical activity – 1.523633) * 0.4818
The predicted DFS formula for males was:
DFS (males) = (2.280336 * Fatigue – 0.592393) * 0.3762 + (4.058274 * Loss of appetite – 0.263501) * 0.3130 + (0.092326 * Grip strength – 3.986646) * –0.4653 + (3.098226 * Functional difficulties – 0.365971) * 0.6146 + (1.005942 * Physical activity – 1.571803) * 0.4680
The SHARE-ficalculators are freely available on www. biomedcentral.com/1471–2318/10/57/additional/ and translated versions in various European languages can be found on https://sites.google.com/a/tcd.ie/sharefrailty- instrument-calculators/home
As regards disability variables, SHARE participants were asked about the experience of difficulty in performing a series of tasks.[20,21] The number of experienced difficulties with basic activities of daily living (ADL) was self-reported by the participants from the following list (minimum: 0; maximum: 6): ‘Because of a health problem, do you have difficulty doing any of the following activities (exclude any difficulties you expect to last less than three months)?’:
• dressing, including putting on shoes and socks
• walking across a room
• bathing or showering
fleating, such as cutting up the food
• getting in and out of bed
• using the toilet, including getting up or down.
The number of difficulties with instrumental activities of daily living (IADL) was self-reported by the participants from the following list (minimum: 0; maximum: 7): ‘Because of a health problem, do you have difficulty doing any of the following activities (exclude any difficulties you expect to last less than three months)?’:
• using a map to figure out how to get around in a strange place
• preparing a hot meal
• shopping for groceries
• making telephone calls
• taking medications
• doing work around the house or garden
• managing money, such as paying bills and keeping track of expenses
The SHARE baseline sample (interviewed between 2004 and 2006) was composed of 28 361 community dwelling participants. After a mean follow-up period of 2.4 years, disability information was available for 17 567 respondents (i.e. 61.9% of the baseline sample, mean age 63.3 years), of whom 13 378 (76.2%) had been non-frail, 3438 (19.6%) pre-frail and 751 (4.3%) frail at baseline.
Statistical analyses were conducted with SPSS 16.0. Descriptives were given as means and standard deviations (SD), or percentages (%), as appropriate. The Chi-square test was used to assess how participants with follow-up disability data differed from those without follow-up disability data, in terms of the baseline frailty status. The two-tailed Spearman’s correlation coefficient (rs) was used to assess the correlation between baseline frailty status and the number of ADL and IADL difficulties, both at baseline and follow-up.
Analyses of frequencies were conducted to determine the proportions of non-frail, pre-frail and frail participants who had, by wave [2], increased at least one, two and three points in ADL and IADL disability. Separately for each frailty category, a repeated measures ANOVA was conducted to assess whether there were statistically significant differences in ADL or IADL scores between the two study waves. The analyses were repeated with the baseline age as covariate. In these analyses, ADL and IADL scores were used as continuous dependent variables
The level of significance was established at P <0.01 throughout.
Both at baseline and at follow-up, baseline SHARE-fihad significant direct cross-sectional correlations with the number of ADL and IADL difficulties (all rs >0.3, P <0.001).
The analysis of frequencies revealed that, by wave 2, 3.6% of the non-frail, 12.2% of the pre-frail and 30.4% of the frail had increased the number of ADL difficulties by at least one.
By wave 2, 1.0% of the non-frail, 5.3% of the prefrail and 18.2% of the frail had increased the number of ADL difficulties by at least two.
By wave 2, 0.5% of the non-frail, 2.5% of the prefrail and 8.8% of the frail had increased the number of ADL difficulties by at least three.
Likewise, 6.6% of the non-frail, 20.4% of the prefrail and 36.6% of the frail had, by wave 2, increased the number of IADL difficulties by at least one.
By wave 2, 1.7% of the non-frail, 9.0% of the prefrail and 18.0% of the frail had increased the number of IADL difficulties by at least two.
By wave 2, 0.8% of the non-frail, 4.1% of the prefrail and 10.5% of the frail had increased the number of IADL difficulties by at least three.
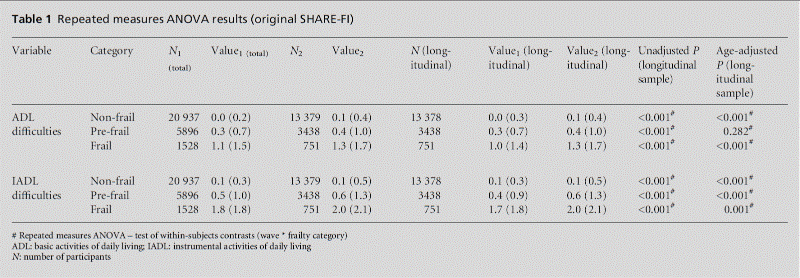
Appendix Table 1 shows the repeated measures ANOVA results, which suggest that the increment in disability at follow-up was directly correlated with the baseline frailty level. As regards ADL difficulties, the frail subgroup increased, on average, by 0.3 points, whilst the non-frail and pre-frail increased by 0.1 points. As regards IADL difficulties, the frail subgroup increased, on average, by 0.3 points, the pre-frail by 0.2 points, and the non-frail by 0.1 points. These differences were statistically significant, and most remained so after age adjustment (see Appendix Table 1).
Appendix Table 2 shows the frailty differences between participants with and without follow-up disability data. Participants with follow-up disability data were significantly less likely to have been non-frail at baseline, and more likely to have been pre-frail and frail (P <0.001).

The aim of this study was to provide further longitudinal validation (with a focus on disability) of a newly created Frailty Instrument intended for use in primary care, where reliable and easy-to-access frailty metrics are needed in order to enhance the process of identification of vulnerable adults who need priority access to resources.
Even after a relatively short follow-up (a mean of 2.4 years), the SHARE-ficlassification was a significant predictor of incident disability, even after adjusting for age. This is consistent with the properties of the original Fried et al’s frailty phenotype[8–10] and fulfils the validation aim of the present study.
From the point of view of primary care practice, SHARE-fihas the advantage of being a valid and simple tool for measuring the level of frailty in individuals aged 50 years given five simple measurements, which leads to the identification of a high frailty group relative to a large population-based sample. The main potential use of SHARE-fiis the screening and monitoring of frailty in community dwelling adults to help prioritise secondary care referrals and/or early multidisciplinary case management. Other advantages ofSHARE-fiare that it can be easily administered in the community by non-physicians (e.g. nurses, health visitors or other allied health professionals) and that it is a relatively brief instrument.
A limitation of our study is that follow-up disability was available for only 61.9% of the baseline sample. In our previous study we demonstrated that missing wave [2] participants were more frail at baseline than non-missing participants[2] and this was also demonstrated here (Appendix Table 2). This is consistent with a known pattern in longitudinal studies by which frail people have higher dropout rates and are less likely to be recontactable.[22] Therefore, and as we previously argued based on a sensitivity analysis,[2] results from this longitudinal sample are likely to represent an underestimation of the ability of SHARE-fito predict incident disability in real life.
In terms of the clinical applicability of SHARE-fi, a potential limitation is that grip strength is not typically assessed in primary care, it can take some minutes to perform and how the test is administered (e.g. sitting versus standing, forearm position) may influence patient performance.[23] Because of this, and for purposes of consistency, we recommend that practitioners follow the grip strength measurement protocol adopted by SHARE.19
In order to assess the extent to which a reduced four-item version of SHARE-fi(i.e. without the inclusion of grip strength) would perform as a predictor of increased difficulties in ADL and IADL, we reclassified the longitudinal sample according to a new DFactor based on the four subjective frailty items only (i.e. exhaustion,weight loss, slowness and low physical activity). Appendix Table 3 shows these additional results, which suggest a significant loss of predictive validity of the instrument as compared to the results shown in Appendix Table 1. This is consistent with previous research highlighting grip strength as an important objective marker of frailty[24] and a determinant of disability in the older general population.[25] SHARE-ficalculators offer a meaningful framework where grip strength results can be integrated with other frailty markers without the need for additional norms or arbitrary cut-offs, which could otherwise limit its applicability in the primary care setting.

The development of SHARE-fidid not include any cognitive exclusion criteria, so in principle SHARE-fican be applied to persons with cognitive impairment. However, because four out of the five SHARE-fivariables are based on self-report, in patients with severe dementia answers should be contrasted with those of a carer or informant.[26]
In conclusion, SHARE-fiwas found to be a significant predictor of incident disability in a European population-based sample. SHARE-fimay contribute toquality inprimary care byoffering a simple andreliable way to assess and monitor frailty in community dwelling adults over the age of 50 years, to prioritise their access to resources and serve as a tool for audit and research.
This paper uses data from SHARE release 2.3.0, as of 13 November 2009.
SHARE data collection between 2004 and 2007 was primarily funded by the European Commission through its fifth and sixth framework programmes (project numbers QLK6-CT-2001–00360; RII-CT- 2006–062193; CIT5-CT-2005–028857). Additional funding by the US National Institute on Aging (grant numbers U01 AG09740–13S2; P01 AG005842; P01 AG08291; P30 AG12815; Y1-AG-4553–01; OGHA 04–064; R21 AG025169) as well as by various national sources is gratefully acknowledged (see www.shareproject.org for a full list of funding institutions).
Not required.
Not commissioned; externally Peer Reviewed.
None.