Review Article - (2024) Volume 21, Issue 2
The Law and Patient Beneficence: Provider Competency on Involuntary Hospitalization, a Systematic Review
Jennifer L. Robertson* and
Candice C. Beasley
School of Social Work, Tulane University, New Orleans, LA, United States
*Correspondence:
Jennifer L. Robertson, School of Social Work, Tulane University, New Orleans, LA,
United States,
Email:
Received: 29-Jun-2023, Manuscript No. IPDEHC-23-16771;
Editor assigned: 03-Jul-2023, Pre QC No. IPDEHC-23-16771 (PQ);
Reviewed: 17-Jul-2023, QC No. IPDEHC-23-16771;
Revised: 28-Feb-2024, Manuscript No. IPDEHC-23-16771 (R);
Published:
04-Mar-2024, DOI: 10.36648/2049-5471.21.2.12
Abstract
The aim of this systematic review is to evaluate competencies of healthcare providers in addressing psychiatric emergencies that may result in involuntary hospitalization. Specifically, this review explores if healthcare providers are competently prepared for involuntary hospitalization. Federal and state laws must be followed if a provider is to be competent in addressing a psychiatric emergency. According to federal law HR 4302, District of Columbia Mental Health Civil Commitment Modernization Act of 2004, the involuntary care of a person is defined as one “who is an imminent risk to themselves or others or is gravely disabled due to mental illness.” In accordance with federal law, all states have the ability to write and maintain their own statutes specific to involuntary hospitalization. It is notably difficult to address and evaluate competency across the nation with 50 different sets of statutes. However, if competency is not achieved by providers related to involuntary hospitalization, vulnerable people are at risk for harm and the loss of civil liberties. A systematic review of literature, since the October 2004 enactment of HR 4302, across the disciplines of social work, psychology, psychiatry, medicine, and law has yielded 461 articles. Using the Preferred Reporting Items for Systematic Reviews and Meta- Analyses (PRISMA), 12 articles meet the requirements for inclusion for competency in knowledge on involuntary hospitalization by health care providers. People with mental health diagnoses have been marginalized and stigmatized throughout history due to antiquated education and the misuse of policy. Through innovative education, continued research, introspective growth, and systematic change, healthcare providers in the United States can be the competent practitioners that communities depended upon.
Keywords
Law; Patient; Hospitalization; Psychiatry; Diagnoses
Introduction
The Mental Health Civil Commitment Act of 2002, revised to
the District of Columbia Mental Health Civil Commitment
Modernization Act of 2004 (HR 4302), has outlined an
updated national policy on involuntary hospitalization.
The act set forth the Commission on Mental Health, laws for
emergency observation detention, and providing counsel for
patients. In addition, this law provided checks and balances
for involuntary hospitalization, protections for professionals
acting in good faith, and protections for vulnerable patients
[1].
The Civil Rights of Institutionalized Persons Act of 1980 and
the Americans with Disabilities Act (ADA) were instrumental in
developing and implementing HR 4302. These two Acts
required agencies to utilize the ‘least restrictive’ care to meet
the needs of patients, like outpatient, community-based
services as feasibility permits [2]. ‘Least restrictive’ is a
common clinical term referring to using treatment and care to
maximum autonomy while meeting the behavioral and
healthcare treatment needs recommended by the attending
providers [3]. Along with utilization of least restrictive care,
HR 4302, the Civil Rights Act, and ADA, emphasizes the
protection of individual rights and protects against
discrimination. However, the lack of understanding by
healthcare providers on national and state statute related to
involuntary hospitalization continues to put patients at risk of
improper and illegal care, increasing the likelihood of
iatrogenic illness [4,5,3].
Literature Review
The policies and statutes on involuntary hospitalization stem
from the social construct of ‘parens patriae’ or a society's
governmental responsibility to protect the people within the
society [6-8]. During involuntary hospitalization, a person is
linked to crisis and emergency mental health services that are
inaccessible to many people [9]. However, the limitation on a
person’s liberties often mirrors the limitation in the criminal
justice system, (i.e. unable to leave at will, clothing and skin
checking, limited access to friends/family, etc.). A major
difference is involuntary hospitalization is often initiated by
medical and mental health professionals that have little to no
training in state statue [10,11] and frequently without a court
hearing [9,2]. Additionally, unlike the medical health system,
patients can be mandated to access mental health treatment
[12].
Accessing mental health care through outpatient treatment
continues to be challenging, often increasing the perceived
need for inpatient treatment. Even with the Affordable Care
Act implementation, the increasing insurance coverage for
patients hoped to rectify the lack of accessibility to services,
but the number of providers has not risen to meet the service
demand [13]. In rural areas, there are few, if any, specialized
mental health practitioners (psychiatrists, psychologists, social
workers, counselors, etc.) [14]. Olfson, found that rural states,
like Idaho, have only 5.2 psychiatrists per 100,000 people, and
urban states, like Massachusetts, have 24.7 psychiatrists per
100,000. These numbers would equate to caseloads ranging
from 4,000 to 20,000 people if every resident needed services.
Lueck and Poe found college campuses, on average, only had
one counselor per 1,737 students [15]. The shortage of access
to mental health professionals affects over 100 million
Americans [16]. Due to the shortage of providers and the
increase in the use of the emergency room, healthcare
professionals face mental health emergencies at a significantly
higher rate. Changes to healthcare usage are forcing
healthcare professionals to respond to the community's needs
with limited access to specialized care.
The most recent report to Congress, from the U.S.
Department of Health and Human Services, found that from
2004-2016 there was a 44% increase in emergency room
usage with a primary need for mental health or substance use
disorder [17].
The Federal Emergency Medical Treatment And Active Labor
Act, commonly known as EMTALA, requires hospitals to
triage all patients, providing evaluation and stabilization,
before transferring for specialized care where possible
[18]. Systemic constraints of the United States
healthcare system means the only place a person can be
guaranteed an acute mental health evaluation is the
emergency room. Unfortunately, emergency rooms are
counterproductive to mental health healing as they are
notoriously loud, busy, lack privacy, and are over stimulating
[19]. Brennanman also explains that due to a lack of
specialized care, patients with mental health diagnoses are in
the emergency room longer than patients with medical
diagnoses, exacerbating the crowding. Dolan, also reports the
overcrowding in emergency rooms makes it challenging for
those who need emergent care to get that care quickly, and
provides additional complication to serving families of a
patient in a mental health crisis. The lack of appropriate beds
in appropriate places is a nationwide crisis yet to be solved by
policymakers; therefore, continuously leaving healthcare
professionals without resource allocations so that they may
best meet their professional abilities and ethical requirements
mandated by their profession.
The ethics of involuntary hospitalization has been an ongoing
conversation as the mental health field has progressed [10].
In both mental health and medical treatment, there is a
constant cost-benefit analysis of autonomy versus
beneficence [10,20]. Arena Ventura et al. found mental health
professionals, in the admissions department of a mental
health hospital, lack knowledge about involuntary
hospitalization laws and regulations [21]. Kaufman and Way,
found resident psychiatrists identified knowledge of
involuntary hospitalization criteria is important, however in
the study scenario, 74% of the residents improperly
involuntarily hospitalized a patient with mental health
concerns. Hotzy et al., found non-psychiatric residents
showed low levels of confidence in their ability to decide if
involuntary hospitalization was needed, suggesting the need
for specialized teams to support decision making. When
providers are unable to appropriately assess risk and
inappropriately assign an involuntary status, patients and
their civil liberties reap the consequences.
A significant amount of stigma comes with a mental health
diagnosis in the United States. For example, Yanos et al.,
found those people diagnosed with mental illness are
perceived as more dangerous than people who do not have a
mental health diagnosis. This perception of “dangerousness”
increases the likelihood that a healthcare provider will
involuntarily hospitalize the patient [10]. Involuntary
hospitalization increases stress-related stigma, suicidality [22],
and increases distrust of the healthcare system [23]. The
stigma and distrust of the system decreases the likelihood of
ongoing care while, increasing the need for emergency care.
Discrimination is common among people who have been
diagnosed with a mental health illness. A person's ability to
make decisions for themselves is overridden by the simple
diagnosis of a mental illness; as a result, people with
mental illness are seen as incompetent in making “sound”
decisions [24].
There is also the potential for involuntary commitments to
be seen as a “transfer of responsibility.” For example, a
hospital or provider can be viewed as needing to rescue or
save a person from themselves; therefore, this person may
not have to take (or may take less) responsibility for their care
[25].
Research has shown people are more likely to respond to
treatment when they take responsibility for their care, make
decisions about care, and are offered hope [2]; in contrast to
those who are negatively impacted due to the involuntary
hospitalization process. Zervakis et al., report patients who
have been involuntarily hospitalized felt discouraged from
seeking future treatment, had a decrease in rapport with
healthcare providers, and had an overall increase in feelings
of coercion, even during voluntary hospitalizations.
Understanding and utilizing positive pressure in statements
such as: “This must be scary for you,” “the doctor is
recommending this medication to help you feel more calm
and less scared so we can figure this out together;” or, “can I
tell you more about this medication?” versus lack of
transparency in the negative pressure process “if you do not
calm down and take your pill I will just give you a shot.”
creates a feeling of coercion [26,27]. Nurses, like other
medical and mental health professionals, have a code of
ethics that does not condone the use of coercion and
encourages professionals to obtain consent to the extent
possible [20]. Nurses have found themselves justifying
coercion, despite not wanting to participate in forced care,
and would benefit from training in decision-making during
potentially coercive situations.
Healthcare professionals and legal professionals see
involuntary hospitalization from different perspectives. While
both seek the best interest and care for the patient,
healthcare professionals will look at symptomatology, and
legal professionals will look for proof of predicted
dangerousness [28]. The balance between what is legal,
ethical and in the best care for the patients is delicate. While
an involuntary hospitalization’s intended purpose is the safety
and well-being of people, the iatrogenic harm may be greater
than the benefit sought [29]. Kaufman and Way and Hotzy et
al., both explain the amount of knowledge on involuntary
hospitalization among psychiatric and non-psychiatric
residents is lacking. The knowledge, education, and
competency of providers charged with the welfare of patients
can be one of the most important protections patients have.
If the information is not received in school or residency,
where is it acquired?
Under HR 4302, individual states can develop and implement
statutes related to involuntary hospitalization for mental
health. Over the 50 United States, there are eight different
possible reasons for involuntary hospitalization and 22
different types of professionals/citizens who can initiate
involuntary hospitalization [9]. Additionally, the length of the
hospitalization and rights available to patients vary greatly,
state to state; therefore, it is difficult to summarize. Law
ambiguity serves a purpose for broad application to various
people in different situations.
However, it often creates difficulties for providers and
patients to understand their rights and responsibilities [30].
When healthcare providers are not knowledgeable about legal
rights and responsibilities, there is a greater risk of iatrogenic
harm to patients [4]. Risks include but are not limited to
stigma-related stress, post-traumatic stress, an increase in
suicidal thoughts, the feeling of coercion, distrust of the
healthcare system, delirium, and loss of family, jobs, money,
and housing [4,25,31-33,20,22,23,27]. Further, providers risk
being viewed as "fraudulent" if they do not accurately
represent important information about hospitalization [8].
Methods
A preliminary literature search shows a theme of healthcare
providers lacking education and knowledge on involuntary
hospitalization. The authors seek to understand if healthcare
providers have the competency, through education and
knowledge, to address the increasing need for mental health
emergencies through the application of involuntary
hospitalization in the United States. Through a systematic
review of the literature published since the enactment of HR
4302 in 2004, the authors attempt to understand the scope of
competency of healthcare professionals related to involuntary
hospitalization.
The PRISMA flow diagram was used to perform a systematic
review [34]. The purpose of this comprehensive assessment
of the literature, which spanned seventeen years, was to
determine if the body of literature supporting healthcare
professionals' competency adequately equipped them to
handle involuntary hospitalization. Seventeen years began in
October of 2004, the first month after the enactment of HR
4302 to the beginning of systematic review in October 2021.
Gray literature was excluded from this systematic search since
only peer-reviewed, published literature was sought. There is
not yet a mandate that researchers use gray material while
conducting systematic reviews. According to Paez [35], while
gray literature is referred to as an “important resource”, it is
not required for a reliable systematic review and is viewed as
one tool to address publication bias. Due to the sensitive
nature of involuntary hospitalization, the authors decided the
use of peer-reviewed literature was best suited for this
endeavor. A two-reviewer process was used to critically
appraise articles, with each author appraising independently
for inclusionary and exclusionary criteria. All reasonable
attempts were made to retrieve articles, however due to
copyright laws; three articles were unable to be obtained by
either author, therefore excluding them from this study. Each
author read all retrieved articles, rating each as included or
excluded with reason. Any discrepancies were discussed, and
a consensus was achieved.
PRISMA Flow Diagram
The authors completed the following steps to gather
generalized, operational, and current literature regarding
guidance in critically identifying ways by which health
professionals gain competency regarding involuntary
hospitalization.
To locate this body of literature, a systematic search was
performed utilizing the following EBSCO Research databases:
SocINDEX with Full Text, Academic Search Complete,
Alt HealthWatch, APA PsycArticles, APA PsycInfo, Criminal
Justice Abstracts With Full Text, ERIC, Family Studies
Abstracts, Health Source: Nursing/Academic Edition, Legal
Source, LGBTQ+ Source, MEDLINE, Military And Government
Collection, Professional Development Collection, Psychology
and Behavioral Sciences Collection, Race Relations Abstracts,
Social Work Abstracts, Urban Studies Abstracts, Violence and
Abuse Abstracts, Women's Studies International, and CINAHL
Complete. Through a seventeen-year review, these databases
were searched from October 2004 through October 2021
screening for peer-reviewed publications. The keywords
utilized were: health professional, nurses, physicians,
counselor, psychologist, social work, mental health law,
mental health professional, education, knowledge, practice,
competency, involuntary hospitalization, and emergency
mental health, (Appendix 1). Inclusionary criteria entailed that
articles were to be published within the last seventeen years;
the articles must be peer-reviewed, in the English language
with full text available. The articles also were to be specific to
involuntary hospitalization conducted within the United
States of America and identify involuntary hospitalization
efforts that reflect healthcare professional competence.
Exclusionary criteria included: Articles and journals that were
not peer-reviewed, articles published prior to October 1,
2004, articles where research was not conducted within the
United States of America, were not peer-reviewed, were not
in the English language, and articles that did not include
mention of healthcare professional, involuntary
hospitalization, competency, and knowledge.
Results
Through the use of the 2020 PRISMA flow diagram [34],
records identified, through the keyword search, yielded 461
possible articles; 136 duplicate articles were removed.
Therefore, 325 full-text articles were assessed for eligibility.
Authors were unable to retrieve three articles through
university libraries and digital resources. Out of the 322
articles, 310 articles failed to meet the inclusionary standards;
201 articles possessed research that was conducted or
published outside of the USA; 40 articles were not peer
reviewed research (i.e. first person narratives, instructional
guides, and book reviews), and 69 articles did not meet the
Boolean search terms for the aforementioned inclusionary
criteria. Therefore, twelve articles (n=12), met all aspects
of the inclusionary criteria (Figure 1 and Table 1).
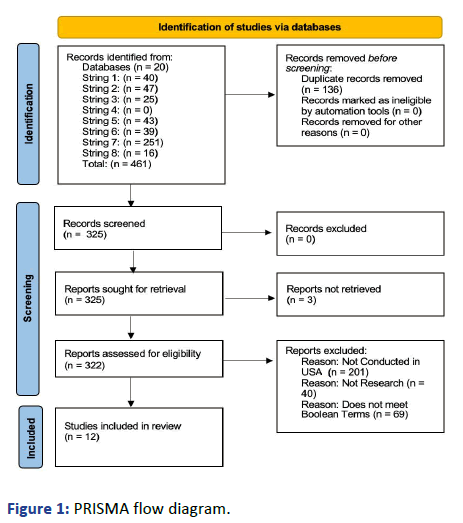
Figure : PRISMA flow diagram.
| Inclusionary articles |
Peer Reviewed |
Published 10/2004-10/2021 |
Conducted in USA |
Healthcare professional knowledge/education |
Involuntary hospitalization |
| Allen |
X |
X |
X |
X |
X |
| Brodwin |
X |
X |
X |
X |
X |
| Brooks |
X |
X |
X |
X |
X |
| Hashmi, et al. |
X |
X |
X |
X |
X |
| Holder, et al. |
X |
X |
X |
X |
X |
| Hom, et al. |
X |
X |
X |
X |
X |
| Jain, et al. |
X |
X |
X |
X |
X |
| Lincoln |
X |
X |
X |
X |
X |
| Reder and Quan |
X |
X |
X |
X |
X |
| Sattar, et al. |
X |
X |
X |
X |
X |
| Shdaimah and O'Reilly |
X |
X |
X |
X |
X |
| Westmoreland |
X |
X |
X |
X |
X |
Table 1: Systematic review results.
Discussion
This systematic review focuses on the importance of
competence regarding involuntary hospitalization among
healthcare professionals as there must be a collective
understanding regarding the importance and shared
responsibility of balancing the safety of the community with
protecting the civil liberties of those with psychiatric
emergencies. Although such a responsibility is seemingly
apparent; the policies, procedures, and legal mandates in
actualizing this responsibility may be quite difficult as laws
governing involuntary hospitalization, from its definition and
verbiage to its procedures, are governed by the states;
therefore, there are no federal standards allowing for
cohesive application and practice on a national level [36].
The literature regarding the connection between involuntary
hospitalization laws and professional healthcare practice
reveals a myriad of reasons why authentic, meaningful, and
non-performative training and application of involuntary
hospitalization laws are imperative for mental healthcare
professionals. Differing themes may emerge when both
novice and veteran professionals are either partially or not
well versed on the involuntary hospitalization laws and
policies that govern their state as well as the ethical tenets
assumed within this decision-making process.
Brodwin, offers the theme of ambivalence; defined as the
“The spontaneous expressions about right and wrong, the
obligatory and the forbidden and the legitimacy of medical
power made by clinicians immersed in ordinary work
routines” (p. 528). [37]. In short, when themes of
ambivalence enter into the practice of involuntary
hospitalization, it allows mental health care professionals to
authentically presume their clinical actions support patient/client beneficence while consciously disregarding state
involuntary hospitalization laws.
In a study by Jain et al., which surveyed one hundred sixty-five
physicians that specializes in substance use disorder, the
theme of ambivalence is expressed through the mental health
provider’s personal values and beliefs [38]. The findings of the
study showed that approximately twenty-one percent of the
physicians were not in favor of involuntary hospitalization
laws in their state and approximately eighteen percent were
uncertain of their thoughts regarding this issue. Further,
thirty-nine percent of participants reported that they were
“somewhat familiar” with involuntary committal laws within
their state and thirty-eight percent of participants reported
being “not familiar” with involuntary hospitalization laws.
Lincoln, infers agreement with the theme of ambivalence by
finding how social factors, such as: the positive correlation
between the professional’s personal risk taking behaviors and
being agreeable to engaging in the involuntary hospitalization
process [39], direct decision making in who will be
involuntarily hospitalized; thus, allowing for the perception
that it is the mental health professionals explicit intent to
place their own values and beliefs regarding involuntary
hosptialization-even above that of state law.
Westmoreland et al., reveals the theme of bias within the
involuntary hospitalization process [36]. In this analysis of the
application of involuntary hospitalization with those
diagnosed with anorexia nervosa, the study found that
although this diagnosis is amongst the more lethal of the
psychiatric diagnoses, there is often reluctance to subject
patients with anorexia nervosa to involuntary hospitalization
due to the patients with this diagnosis being viewed as
"intelligent" and "self-disciplined" in comparison to patients
with subsequent mental health diagnoses.
In contrast, Hom et al., describes bias through the removal of
client/patient autonomy. This study identified bias, among
mental health care professionals, by analyzing the
perspectives of service received by ninety-six suicide attempt
survivors. Of these survivors, eighty-two percent reported at
least one negative experience while in contact with a mental
health care professional with common experiences being:
“stigma from the provider, involving being belittled for having
attempted suicide; poor therapeutic alliance; and inadequate
training to work with individuals at elevated suicide risk, often
evidenced by discomfort with participant disclosure" [29].
This study also found that participants who ascribed to be
female were more likely to have reported negative
experiences than participants that ascribed to be male,
inferring bias in the mental healthcare experience based upon
sex/gender. The Jain et al., study also shares the sentiment in
that there is a concept of privilege within the involuntary
hospitalization process. As it relates to substance use
disorders, this study reports that physicians were more likely
to support involuntary hospitalization for opioid and alcohol
addiction but not for subsequent substances such as over-thecounter
medications and inhalants.
Themes of professional competency must also be explored as
there is a lack of uniformity in the understanding and
application of involuntary hospitalization policy, procedures,
and laws [40].
Hom et al., further found that study participants that reported
negative mental health care experiences associated these
experiences with involuntary hospitalization, including “being
confined to the same space with individuals with more severe
psychopathology and being physically restrained” [29]. In a
study of approximately seven hundred mental health care
professionals across the United States, Brooks, found that
respondents exemplified competency in conceptualizing the
legal components of involuntary hospitalization which focuses
upon danger to self-and/or others. However, when examined
on subsequent legal grounds of this concept, such as: grave
disability, substance addiction, and in some states “sexual
predator status,” competency seemingly declined. Further,
this study identified that mental health care professionals,
within the study, were not well versed on legal grounds of
involuntary hospitalization, beyond those that were commonly
experienced within their practice setting as well as having
limited knowledge of outpatient involuntary hospitalization
procedures within their state [7]. Even more concerning, a study
by Hashmi et al., found that out of 81 patients within their study
that were involuntarily hospitalized, “more than one third of the
patients lacked sufficient clinical justification for involuntary
hospitalization” (p. 621) [41].
Holder et al., study within an emergency department, found
that procedural competency, regarding involuntary
hospitalization, lacks consistency across health care
disciplines with social workers performing better than medical
doctors and nurse practitioners [36]; results that are
concerning as it is not uncommon for social workers to take
orders and directives from these professionals within the
emergency department. A study by Reder and Quan, found
that mental health professionals and administrators within
their study, believed that it was not the emergency
department’s responsibility to “pry” into the lives of their
clients; hence, the emergency department is to only concern
itself with acute life-threatening mental health behaviors and
not “unclear” mental health issues [42].
Continuing the theme of competency, Allen, discusses an
intersectional theme of violence, finding that when compared
to licensed nurses, unlicensed mental health care workers
were three times more likely to be assaulted within in-patient
setting causing difficulty in sustaining safe environments for
all involved within the in-patient setting [43].
Finally, Westmoreland et al., discusses physician
countertransference and how the physician “bears the brunt”
of anger from clients’ families when the idea of involuntary
hospitalization stems from the mental healthcare team and is
not a request from the family [44]. When this occurs, especially
for a mental health diagnosis that may also be viewed as a
physical medical diagnosis, the physician may concede and
allow the patient more autonomy regarding their mental health
care plan. This type of countertransference is yet another
barrier in adhering to state involuntary hospitalization laws by
unintentionally disregarding professional competency.
Future Implication
Consistently throughout the literature, researchers call for
training and education to support providers in making ethical,
statute driven, and safe decisions related to involuntary
hospitalization [43,19,41,36,29,10,11,45,39,40].
Offering acontinuing education course is a cost-effective way
to engage healthcare and mental health professionals.
Allen, notes education does not create ‘one and
done’ change, continuous conversation about ethics and
decision making provide for a culture of commitment to
meaningful patient care. Whether implemented by state
regulatory boards, the Centers for Medicare and
Medicaid Services, universities or individual agencies, the
benefit of continued education and training on involuntary
hospitalization will resonate within the communities
served.
Additionally, these authors seek more structural changes
along with education. Several mental illnesses fall under the
protection of disability rights, however, the accommodations
made for people with mental illnesses are not comparable to
those made for people with mobility disabilities [24]. For
example, ramps and elevators are commonplace in western
society; however, Szmukler, brings up the concept of
supportive decision making for people with severe mental
illness as an accommodation in a society with few
accommodations for people with mental illness. An invisible
disability deserves equal accommodation to ‘visible’
disabilities. As part of their Mental Health Act (MHA), Alberta,
Canada has implemented the use of mental health patient
advocates. Under the MHA, which has similar wording to
American state statutes, access to mental health patient
advocates is a right of any person involuntarily hospitalized
that is deemed unsafe to self or other due to mental health
reasons [46]. The primary purpose of advocates is to provide
information, help patients advocate for themselves, and
investigate concerns or questions of patients. Advocates can
assist patients in obtaining legal counsel, apply for an appeal
of treatment decisions, review patient records, and ask
reasonable questions of providers involved in care [47].
Additionally, advocates and the advocacy office provide
presentations and training, free of charge, to professionals,
community organizations, people who use mental health
services, family and caregivers of those with mental illness,
students, and any interested community members [48]. The
transparency and support given to patients can increase use
of services, positively impact people and communities, and
increase ethical care of all patients.
Hom et al., study participants provided recommendations of
different support systems being offered during hospitalization
to improve outcomes. An option for hospitals is to have a
specialty team for supportive decision making and patient
advocacy. Potentially housed within the emergency
department, this team would be able to help patients who are
at risk for involuntary hospitalization or have medical and/or
mental health struggles that may require additional
explanation to ensure informed consent is achieved. This team
would also be able to support hospital staff in
understanding involuntary hospitalization statutes and patient
rights. Led by a mental health nurse practitioner (or the
state’s equivalent) and made up of different levels of medical
and mental health staff, including licensed practical nurses,
registered nurses, and bachelor’s and master’s level social
workers.
Bachelor’s level social workers and LPNs are able to serve on
this team as they are not performing assessments of the
patient but supporting the patient’s ability to make
informed decisions. Like a mental health patient advocates,
their primary job would be the rights of patients with a
secondary job of providing knowledge and training to the
hospital staff. With a patient’s right specialty team, patients
will have additional protections on their autonomy, and
providers will have additional resources to support their
ability to provide high quality care to more patients.
Decreasing unnecessary involuntary hospitalization can
decrease the crowding in the emergency room allowing for a
more efficient flow of services [49,50].
Conclusion
Without increasing advocacy for patients and education for
providers, our society both decreases the positive impact of
treatment and places vulnerable people at risk. An article
written for the New York Times in November of 2022
reports on the mayor of a major city announcing concerns
over the ‘crisis’ of homelessness in the city, insinuating it is a
mental health crisis. The article reports the mayor pushing for
law enforcement to force people struggling with housing
instability to be evaluated for mental health, equating housing
instability with grave disability due to mental health.
Currently, New York state statute Chapter 27, Title B, Article 9
does not allow for involuntary hospitalization due to
‘grave disability’, only for suicidality and homicidality.
In cases like the aforementioned, whose responsibility is it to
know the state statutes and ethics of caring for the
community? If local authorities and providers are not
knowledgeable on the state statutes and advocacy groups are
unable to keep up with the high demand for services, what is
the risk to the vulnerable populations? Involuntary
hospitalization is not just an emergency room or psychiatric
hospital issue. The effects of involuntary hospitalization are
pervasive and worth the time of all providers to attain the
knowledge to provide the best quality services to their
communities.
Limitations
The most notable limitation of this systematic review is the
small sample size. The size is limited due the absence of peer-reviewed
studies on health provider competency conducted in
the United States. This limitation highlights a significant gap in
the literature and research on health care provider
competency, indicating that in the United States, perhaps a
greater focus should be placed on the evaluation of our
practices and processes related to involuntary hospitalization.
Other countries have shown, through the literature, an
importance placed on the evaluation and competency of
providers. Additional systematic reviews would be indicated
once the United States have bridged the current gaps by
researching and evaluating the process by which they allow
providers to remove civil liberties of vulnerable people.
References
- District of Columbia Mental Health Civil Commitment Modernization Act (2004) HR 4302, 108th Cong., U.S. Government information, GPO.
- Substance Abuse and Mental Health Services Administration (2021) Civil commitment and the mental healthcare continuum: Historical trends and principles for law and practice.
- Tebaldi C (2012) Understanding involuntary hospitalization and use of seclusion and restraint. Nurse Pract. 37(6):13-16.
[Crossref] [Google Scholar] [PubMed]
- Becker MA, Boaz TL, DeMuth A (2012) Predictors of emergency commitment for nursing home residents: The role of resident and facility characteristics. Int J Geriatr Psychiatry. 27(10):1028-1035.
[Crossref] [Google Scholar] [PubMed]
- Henwood B (2008) Involuntary inpatient commitment in the context of mental health recovery. Am J Psychiatr. 11(3):253-266.
[Crossref] [Google Scholar]
- Appelbaum PS (1996) Civil mental health law: Its history and its future. Mental Physical Disability L Rep. 20:599.
[Google Scholar]
- Brooks RA (2007) Psychiatrists' opinions about involuntary civil commitment: Results of a national survey. J Am Acad Psychiatry Law. 35(2):219-228.
[Google Scholar] [PubMed]
- Garakani A, Shalenberg E, Burstin SC (2014) Voluntary psychiatric hospitalization and patient-driven requests for discharge: A statutory review and analysis of implications for the capacity to consent to voluntary hospitalization. Harv Rev Psychiatry. 22(4):241-249.
[Crossref] [Google Scholar] [PubMed]
- Hedman LC, Petrila J, Fisher WH (2016) State laws on emergency holds for mental health stabilization. Psychiatr Serv. 67(5):529-535.
[Crossref] [Google Scholar] [PubMed]
- Hotzy F, Marty S, Moetteli S, Theodoridou A, Hoff P, et al. (2019) Involuntary admission of psychiatric patients: Referring physicians’ perceptions of competence. Int J Soc Psychiatry. 65(7-8):580-588.
[Crossref] [Google Scholar] [PubMed]
- Kaufman AR, Way B (2010) North Carolina resident psychiatrists knowledge of the commitment statutes: Do they stray from the legal standard in the hypothetical application of involuntary commitment criteria?. Psychiatr Q. 81:363-367.
[Crossref] [Google Scholar] [PubMed]
- Clark C, Becker M, Giard J, Mazelis R, Savage A, et al. (2005) The role of coercion in the treatment of women with co-occurring disorders and histories of abuse. J Behav Health Serv Res. 32:167-181.
[Crossref] [Google Scholar] [PubMed
- Olfson M (2016) Building the mental health workforce capacity needed to treat adults with serious mental illnesses. Health Aff (Millwood). 35(6):983-990.
[Crossref] [Google Scholar] [PubMed]
- Arbore P (2019) Suicide prevention among rural older adults. Generations. 43(2):62-65.
[Google Scholar]
- Lueck JA, Poe M (2021) Bypassing the waitlist: Examining barriers and facilitators of help-line utilization among college students with depression symptoms. J Ment Health. 30(3):308-314.
[Crossref] [Google Scholar] [PubMed]
- Sisler SM, Schapiro NA, Nakaishi M, Steinbuchel P (2020) Suicide assessment and treatment in pediatric primary care settings. J Child Adolesc Psychiatr Nurs. 33(4):187-200.
[Crossref] [Google Scholar] [PubMed]
- U.S. Department of Health and Human Services (2021) Trends in the utilization of emergency department services, 2009-2018.
- Brennaman L (2015) Exceeding the legal time limits for involuntary mental health examinations: A study of emergency department delays. Policy, Politics, and Nursing Practice. 16(3-4):67-78.
[Crossref] [Google Scholar] [PubMed]
- Dolan MA, Fein JA (2011) Committee on pediatric emergency medicine. Pediatric and adolescent mental health emergencies in the emergency medical services system. Pediatrics. 127(5):e1356-e1366.
[Crossref] [Google Scholar] [PubMed]
- Vuckovich PK, Artinian BM (2005) Justifying coercion. Nurs Ethics. 12(4):370-380.
[Crossref] [Google Scholar] [PubMed]
- Ventura CA, Moll MF, Junior RC, de Moraes VC, Silva LD, et al. (2016) Involuntary hospitalization of patients with mental disorders: knowledge of health professionals. Arch Psychiatr Nurs. 30(6):700-703.
[Crossref] [Google Scholar] [PubMed]
- Xu Z, Muller M, Lay B, Oexle N, Drack T, et al. (2018) Involuntary hospitalization, stigma stress and suicidality: A longitudinal study. Soc Psychiatry Psychiatr Epidemiol. 53:309-312.
[Crossref] [Google Scholar] [PubMed]
- Yanos PT, DeLuca JS, Gonzales L (2020). The United States has a national prostigma campaign: It needs a national, evidence-based anti-stigma campaign to counter it. Stigma and Health 5(4):497-498.
[Crossref] [Google Scholar]
- Szmukler G (2020) Involuntary detention and treatment: Are we edging toward a “paradigm shift”?. Schizophr Bull. 46(2):231-235.
[Crossref] [Google Scholar] [PubMed]
- Borecky A, Thomsen C, Dubov A (2019) Reweighing the ethical tradeoffs in the involuntary hospitalization of suicidal patients. Am J Bioeth. 19(10):71-83.
[Crossref] [Google Scholar] [PubMed]
- Shields MC, Ne'eman A (2018) Expanding civil commitment laws is bad mental health policy. Health Affairs Forefront.
- Zervakis J, Stechuchak KM, Olsen MK, Swanson JW, Oddone EZ, et al. (2007) Previous involuntary commitment is associated with current perceptions of coercion in voluntarily hospitalized patients. Int J Forensic Ment Health 6(2):105-112.
- Abramowitz MZ, Bentov-Gofrit D, Khawaled R, Bauer A, Cohen T (2011) Attitudes among medical and law students toward decision-making in regard to involuntary psychiatric hospitalization. Int J Law Psychiatry. 34(5):368-373.
[Crossref] [Google Scholar] [PubMed]
- Hom MA, Albury EA, Gomez MM (2020) Suicide attempt survivors’ experiences with mental health care services: A mixed methods study. Prof Psychol: Res Pract. 51(2):172.
[Crossref] [Google Scholar]
- Gregoire CL, Joshi KG, Gehle ME (2021) Legal Standard for Emergency Mental Health Seizure by Law Enforcement. J Am Academy Psychiatr Law. 49(2):260–262.
- Cohen E, Wusinich C, Friesen P (2019) Considering the social variable in psychiatric hospitalization: A case for structural competency. Ethical Hum Psychol Psychiatry. 20(3):127-132.
[Crossref] [Google Scholar]
- Guzman-Parra J, Aguilera-Serrano C, Garcia-Sanchez JA (2019) Experience coercion, post-traumatic stress, and satisfaction with treatment associated with different coercive measures during psychiatric hospitalization. Int J Ment Health Nurs. 28(2):448-456.
[Crossref] [Google Scholar] [PubMed]
- Jones N, Gius BK, Shields M, Collings S, Rosen C, et al. (2021) Investigating the impact of involuntary psychiatric hospitalization on youth and young adult trust and help-seeking in pathways to care. Soc Psychiatry Psychiatr Epidemiol. 1:1-11.
[Crossref] [Google Scholar] [PubMed]
- Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, et al. (2021) The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. Rev Esp Cardiol. 372.
[Crossref] [Google Scholar] [PubMed]
- Paez A (2017) Gray literature: An important resource in systematic reviews. J Evid Based Med. 10(3):233-240.
[Crossref] [Google Scholar] [PubMed]
- Holder SM, Warren C, Rogers K (2018) Involuntary processes: Knowledge base of health care professionals in a tertiary medical center in upstate South Carolina. Community Ment Health J. 54:149-157.
[Crossref] [Google Scholar] [PubMed]
- Brodwin P (2014) The ethics of ambivalence and the practice of constraint in US psychiatry. Cult Med Psychiatry. 38:527-549.
[Crossref] [Google Scholar] [PubMed]
- Jain A, Christopher PP, Fisher CE, Choi CJ, Appelbaum PS (2021) Civil commitment for substance use disorders: A national survey of addiction medicine physicians. J Addict Med. 15(4):285-291.
[Crossref] [Google Scholar] [PubMed]
- Sattar SP, Pinals DA, Din AU, Appelbaum PS (2006) To commit or not to commit: The psychiatry resident as a variable in involuntary commitment decisions. Acad Psychiatry. 30:191-195.
[Crossref] [Google Scholar] [PubMed]
- Shdaimah C, O’Reilly N (2016) Understanding US debates surrounding standards in involuntary inpatient psychiatric commitment through the Maryland experience. Social Work in Mental Health. 14(6):733-751.
[Crossref] [Google Scholar]
- Hashmi A, Shad M, Rhoades H (2014) Involuntary detention: Comparison of clinical practices of psychiatry residents and faculty. Acad Psychiatry. 38:619-622.
[Crossref] [Google Scholar] [PubMed]
- Reder S, Quan L (2004) Emergency mental health care for youth in Washington State: Qualitative research addressing hospital emergency departments' identification and referral of youth facing mental health issues. Pediatr Emerg Care. 20(11):742-748.
[Crossref] [Google Scholar] [PubMed]
- Allen DE (2013) Staying safe: Re-examining workplace violence in acute psychiatric settings. J Psychosoc Nurs Ment Health Serv. 51(9):37-41.
[Crossref] [Google Scholar] [PubMed]
- Westmoreland P, Johnson C, Stafford M, Martinez R, Mehler PS (2017) Involuntary treatment of patients with life-threatening anorexia nervosa. J Am Acad Psychiatry Law. 45(4):419-425.
[Google Scholar] [PubMed]
- Lincoln A (2006) Psychiatric emergency room decision-making, social control and the ‘undeserving sick’. Sociol Health Illn. 28(1):54-75.
[Crossref] [Google Scholar] [PubMed]
- Province of Alberta Mental Health Act, (2022). Revised Statutes of Alberta 2000, Chapter M-13.
- Canadian Mental Health Association, Calgary Region (2010) The Alberta mental health act-A guide for mental health service users and caregivers. The Alberta Mental Health Act.
- Government of Alberta (2023) Alberta mental health advocate. Alberta.ca.
- Fitzsimmons EG, Newman A (2022) New York's plan to address crisis of mentally ill faces high hurdles. The New York Times.
- New York State Statute (2021) Hospitalization of persons with a mental illness. Mental Hygiene (MHY) Chapter 27, Title B.
Citation: Robertson JL, Beasley CC (2024) The Law and Patient Beneficence: Provider Competency on Involuntary Hospitalization, a Systematic Review. Divers Equal Health Care. 21:12.
Copyright: © 2024 Robertson JL, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.


