Editorial - (2018) Volume 19, Issue 3
Tufts University School of Medicine, Boston, MA, USA
Received March 16th, 2018 - Accepted May 07th, 2018
Carcinoma; Carcinoma, Pancreatic Ductal; Early Detection of Cancer; Endosonography; Neoplasms; Neoplasm Metastasis; Pancreas; Pancreatic Neoplasms; Therapeutics
EUS endoscopic ultrasound; MDCT multidetector computed tomography; MRCP magnetic resonance cholangiopancreatography; MRI magnetic resonance imaging; ERCP endoscopic retrograde cholangiopancreatography
Pancreatic cancer is the fourth leading cause of mortality related to cancer among both genders in the United States [1]. Unfortunately, the majority of the patients are diagnosed at an advanced stage. Moreover, poor prognosis even after complete surgical resection further justifies the urgency and need to detect pancreatic cancer earlier, especially in those individuals with identified high-risk factors [2]. Though, pancreatic cancer is a rare disease before the age of 45, however, the incidence rises sharply in the younger patients over the last decade.
Risk factors to develop pancreatic cancer include hereditary diseases, environmental and social conditions (Table 1 and 2). Familial aggregation and genetic susceptibility account for approximately 10% of all pancreatic cancer cases [3]. Nonhereditary/environmental risk factors for pancreatic cancer include chronic pancreatitis, diabetes mellitus, cigarette smoking, obesity and Helicobacter pylori infection [4, 5] (Table 1).
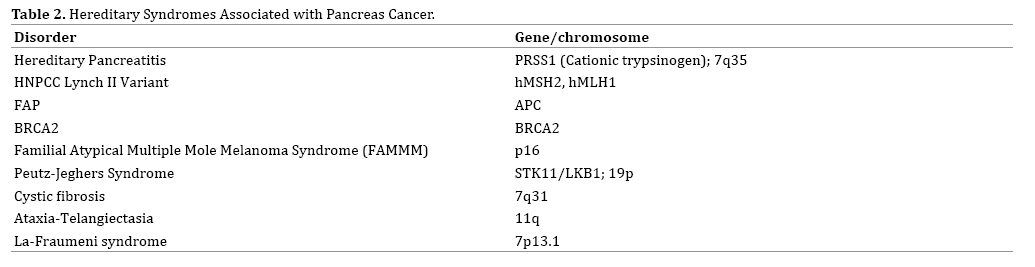


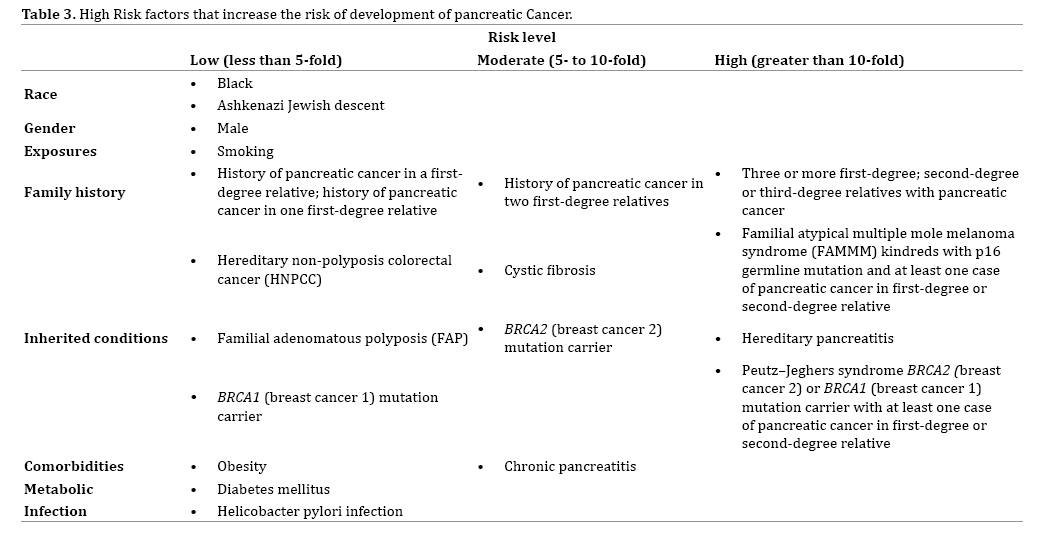
However, with better understanding of human genetics we can now identify those at high risk for developing pancreatic cancer [3, 4, 5, 6, 7, 8, 9] (Table 3).
Despite we have established many risk factors that predispose pancreatic cancer in large studies; data pertaining to its early detection remains undetermined and inadequate. Carbohydrate Antigen 19-9 (CA 19-9) is usually elevated in patients with pancreatic cancer; however, its role in early detection marker in pancreatic cancer has been discouraging in many studies [10]. One meta-analysis, that included 2, 316 individuals, showed that the pooled sensitivity of CA 19-9 was 0.80 (95% CI 0.77-0.82) and specificity of 0.80 (95% CI 0.77-0.82), in detection of pancreatic cancer [11]. On the other hand, imaging techniques might be helpful in early detection of pancreatic cancer, but of limited utility for mass screening purposes, primarily due to cost.
In high risk asymptomatic individuals or those with family history of pancreatic cancer, investigators evaluated the utility of one time screening with MRI, CT scan and EUS, or EUS and/or MRI with CA19-9 and genetic testing respectively [5, 6, 7, 8, 9]. The yield of these screening modalities was not being uniformly high and did not show a cost effective benefit in detection of pancreatic cancer. The U.S. Preventive Services Task Force (USPSTF) found no evidence that screening for pancreatic cancer is effective in reducing mortality; however, there is a potential for significant harm due to the very low prevalence of pancreatic cancer, limited accuracy of available screening tests, the invasive nature of diagnostic tests, and the poor outcomes of treatment [12]. At present, the USPSTF has not addressed the effectiveness of screening in individuals with hereditary pancreatitis or other hereditary conditions that predispose to develop pancreatic cancer [13]. Similarly, no society or national practice guidelines recommend screening for pancreatic cancer in the general population.
One could argue that diet prevention and life style modification should at least be adopted. Currently, there were no clear guidelines regarding diet-based prevention, however, a balanced diet with good fruit and vegetable intake, abstaining from tobacco products along with lifestyle modifications that can help in to reduce the risk of pancreatic cancer [6, 7, 14].
With the identification of the above factors and development of new diagnostic tools, the experts have suggested screening for individuals with high risk for pancreatic cancer. One such guidelines were devised by the participants of the Fourth International Symposium of Inherited Diseases of the Pancreas, held in Chicago, IL, USA on November 7-9, 2009 [15], who recommend screening only for those at high risk (more than 10-fold relative risk (Figure 1) for pancreatic cancer.
Diagnostic imaging tools used in high-risk individuals may include endoscopic ultrasound (EUS), multidetector computed tomography (MDCT), magnetic resonance cholangiopancreatography (MRCP), magnetic resonance imaging (MRI), and endoscopic retrograde cholangiopancreatography (ERCP). It is important to borne in mind that the application of these diagnostic tests for pancreatic cancer detection screening is very limited for the general adult population.
Medical literature suggests that micoRNAs (miRNA) are related to many different cancers including pancreatic cancers [16, 17] Ding et al. conducted a meta-analysis including 2, 036 patients and 1, 444 controls to assess the use of miRNAs as possible biomarkers to be used a s as a screening tool for pancreatic cancer [18]. This meta-analysis showed that the use of multiple miRNA for discriminating pancreatic cancer patients from healthy individuals had a pooled sensitivity of 82% (95% CI, 78– 86%) and specificity of 77% (95% CI, 73–81%), suggesting a potential diagnostic value of miRNAs for pancreatic cancer.
Other biological markers, such as PAM4-enzyme Macrophage inhibitory cytokine, carcinoembryonic antigen cell adhesion molecule, DNA methylase transferase, osteopontin, mucin, S100A6 and others are undergoing testing but none of them have been validated up to date [19, 20, 21].
In summary, many efforts have been undertaken to find effective ways to detect pancreatic cancer earlier as the majority of the patients are diagnosed at an advanced stage and bears grave prognosis. Despite all previous attempts at finding a reliable screening modality for pancreatic cancer, no study to date has shown improved survival. CA19-9 is not a screening test. However, a multidisciplinary group of experts should be involved in detecting noninvasive precursor lesions to pancreatic cancers at a curative stage in high risk patients, such as those with inherited cancer susceptibility syndromes and patients with hereditary pancreatitis.
The project described was supported by the National Institutes of Health through grant numbers UL1 TR001064.
The author has no potential conflicts of interest.