- (2016) Volume 17, Issue 2
Savio George Barreto*
Department of Gastrointestinal Surgery, Gastrointestinal Oncology, and Bariatric Surgery, Medanta Institute of Digestive and Hepatobiliary Sciences, Medanta, the Medicity, Gurgaon, India
*Corresponding Author:
Savio George Barreto
GI Surgery, GI Oncology and Bariatric Surgery
Medanta Institute of Digestive and Hepatobiliary Sciences
Medanta, The Medicity
Sector 38, Gurgaon
Haryana - India
Phone: 91-9971900644
E-mail : georgebarreto@yahoo.com
Received September 20th, 2015 - Accepted October 30th, 2015
Background With the looming fear of costs for cancer care escalating over the next decade, the general aim of policy makers the world over is directing efforts towards “bending the cost curve”. Pancreatic cancer is on the rise and pancreatoduodenectomy is the only curative option available. The aim of the current report is to analyze the published literature on data addressing the issue of costs in pancreatic cancer surgery (with a focus on pancreatoduodenectomy) in an effort to determine how disparate are the lines of investigation of health economics and quality indicators of surgery. Methods A systematic and comprehensive search of major reference databases (MEDLINE, EMBASE, PubMed, and the Cochrane Library) was undertaken using a combination of text words “cost”, “pancreatoduodenectomy”, “pancreaticoduodenectomy”, “health care”, “surgery”. The search was restricted to human studies published in literature but was not language restricted. Results The initial search yielded 116 studies of which 25 manuscripts were retrieved for further evaluation. Of the 25 studies retrieved, 7 manuscripts were excluded from the final analysis as the variables analyzed did not significantly influence the costs of pancreatoduodenectomy. The factors most frequently noted (≥2 studies) to influence costs of pancreatoduodenectomy were hospital and surgeon volume the occurrence of complications and the implementation of clinical pathways. Conclusions Using pancreatoduodenectomy, as an example, it is evident that the key to ‘bending the cancer cost curve’ is designing strategies to improve quality of the not only the procedure, but the process. Costs and quality cannot be separated. Reduction in costs can, and must only, be achieved by targeting excellence.
Keywords
Outcome Assessment; Pancreas; Pancreatoduodenectomy
INTRODUCTION
Pancreatoduodenectomy (PD), the only curative surgery for cancer of the periampullary and pancreatic head region, is a technically challenging procedure with the risk of morbidity and mortality. The incidence of pancreatic cancer is rising [1] and it is projected to be the second most-common cause of cancer-related deaths by 2030 [2]. Thus, treatment of this cancer needs attention from global perspective. PD has evolved tremendously over the last few decades [3] initially from a life threatening, two-stage surgery to a singlestage procedure with steadily reducing operating times, the requirement for perioperative blood transfusion [4] as well as post-operative morbidity and mortality [5]. Encouraged by these improvements, there is a drive towards making PD not only more ‘patient-friendly’, but also cost effective [6, 7].
With the looming fear of costs for cancer care escalating over the next decade [8], the general aim of policy makers the world over is directing efforts towards “bending the cost curve” [9-11]. Unfortunately, in this endeavor, instead of focusing on the costs of treating individual patients with specific medical conditions over their full cycle of care, providers aggregate and analyze costs at the specialty or service department level [12]. In this case, efforts aimed at cost containment must ensure that in an attempt at reducing costs, the quality of care and the surgery are, in themselves, not compromised. The situation is compounded in solid organ cancers such as pancreatic cancer, where surgery is the mainstay for cure [13]. On this background, pancreatic surgeons have begun to assess the health economics of PD [6, 14].
Thus, the aim of the current report is to analyze the published literature on data addressing the issue of costs in pancreatic cancer surgery (with a focus on PD) in an effort to determine how disparate are the lines of investigation of health economics and quality indicators of surgery.
Literature Search
A systematic and comprehensive search of major reference databases (MEDLINE, EMBASE, PubMed, and the Cochrane Library) was undertaken using a combination of text words “cost”, “pancreatoduodenectomy”, “pancreaticoduodenectomy”, “health care”, “surgery”. The search was restricted to human studies published in literature but was not language restricted. Articles were compiled into a database and duplicates were removed. The abstracts were then screened for relevance. Subsequently, the reference lists of relevant trials, reviews, and international guidelines were hand-searched. Reference lists of the retrieved literature were cross-searched manually for additional publications. The inclusion criteria were all types of study (randomized, prospective observational, and retrospective observational) describing the analysis of factors influencing costs in PD. The articles that did not report on the factors influencing costs were excluded. Review articles, letters to the editor, comments and editorials were also excluded.
Results
The search yielded 116 studies of which 25 manuscripts [6, 14-37] were retrieved for further evaluation. Of the 25 studies retrieved, 7 manuscripts [31-37] were excluded from the final analysis as the variables analyzed did not significantly influence the costs of PD (Figure 1).
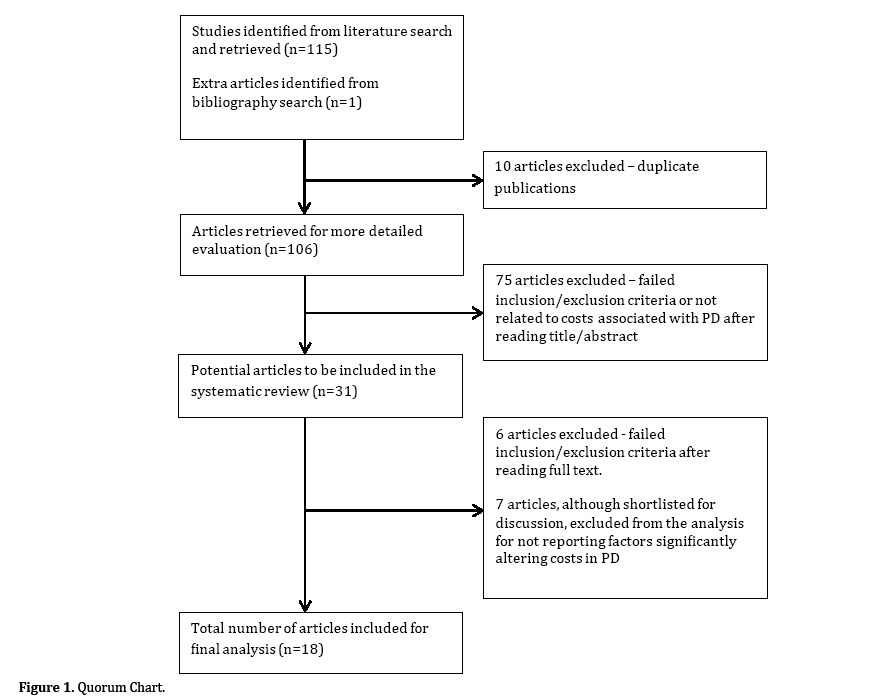
Figure 1. Quorum Chart.
Table 1 summarizes the 18 studies that includes 35,322 patients (patients from multiple publications by the same authors [6, 25] included in the current analysis were excluded if they could be clearly accounted for). The majority of the studies were based on multicentre data analyses from the United States (7 studies) with an additional 5 single centre studies from the same country. Two studies reported data from a single centre in Italy while the only study from Japan was a multicentre analysis. There are also single studies from Belgium, The Netherlands and China.

The factors most frequently noted (≥2 studies) to influence costs of PD were hospital [18, 19, 25, 27, 30] and surgeon volume [18, 20, 24], the occurrence of complications [17, 21, 26] and the implementation of clinical pathways [6, 23]. Low surgeon and hospital volumes were associated with significantly increased hospital costs as was the occurrence of post-operative complications. Costs escalated with the rising severity of the complication [17, 26], the development of post-operative infections [17, 26] or post operative pancreatic fistula (POPF) [14, 16, 17]. The implementation of perioperative clinical pathways was associated with reduced hospital costs.
Other factors noted to significantly increase PDassociated hospital costs included a higher American Society of Anesthesiologists (ASA) grade [22], complications such as medical complications [17], delayed gastric emptying (DGE) [17], post-pancreatectomy hemorrhage (PPH) [26], bile leak [17], and the need for resurgery for the complications [17], length of post-operative hospital stay [14], surgery for malignancies other than pancreatic ductal adenocarcinoma [26], the performance of laparoscopic PD [28] and the delayed removal of peroperatively placed intra-abdominal drains [15].
On the other hand, regionalization of the performance of PD [19] and selective use of the somatostatin analogue, octreotide, in high risk patients [29] significantly reduced total costs o fPD.
The studies not included in the review that addressed factors suspected to alter costs but, on analysis, failed to do so are mentioned below. Elderly patients with their higher propensity for co-morbidities as well as post-operative complications [38] have been thought to incur higher costs should they need PD. However, all 3 studies addressing the aspect of PD in elderly [35-37], found no significant differences in terms of the cost. Studies investigating the use of energy devices for dissection in PD (suggested to reduce operative times and consequently surgical costs) failed to reduce total costs [32, 33]. Similarly, laparoscopic PD costs were not found to be significantly different from open surgery in an analysis of 123 patients (75 of whom underwent laparoscopic PD) [31] which the authors attributed to the shortened hospital stay using the minimally invasive approach. Selective use of diagnostic laparoscopy in pancreatic cancer, too, failed to show a significant impact on total costs [34]. No difference in the impact of the pathology for which PD was performed (neoplasm versus chronic pancreatitis) was noted in the analysis by Holbrook et al. [21].
Reducing Costs and PD – The Way Forward
The manner in which Healthcare costs are borne vary in different parts of the world. The three most common stake holders in bearing cancer-therapy related costs are the patients themselves [39] (self funded - who pay ‘out of pocket’), the Health Insurance companies, and the National health care systems such as the National Institute of Health (NIH) in the United States, the Medicare in Australia and the National Health Service (NHS) in the United Kingdom. The financial burden to the patient even in the case of existing comprehensive health insurance policies [40] or state plans [41], is immense. Reduction in costs would as a rule benefit all the above stake holders and most certainly the patient. However, we must not lose focus of the fact that cost is not the most important aspect of patient care.
In order to understand the factors influencing costs following surgery performed with a curative intent, we reviewed the published data on costs associated with PD – the surgical treatment for periampullary and pancreatic head cancer. This review, the first of its kind, highlights various factors that influence costs following PD, the most prominent being hospital and surgeon volume, the occurrence of complications, and the implementation of clinical pathways.
Interestingly, pancreatic surgeons have long-been challenging themselves in attempting to continuously improve procedural outcomes. From acknowledging the impact of surgeon [42] and hospital volume [43] on perioperative outcomes leading to the drive towards centralization / regionalization of pancreatic surgery [44] to developing quality indicators for not only overall post-operative morbidity (<55%) and mortality (<5%) but even specific complications such as POPF (<16%) [45] there has been a constant thrust towards achieving better results overall. The initial belief that higher hospital or surgeon volumes correlate with better outcomes was critically analyzed [46]. This analysis by Ghaferi et al. [46] determined that that the difference in mortality between high- and low-volume centers was not so much a result of reduced morbidity as it was the ability of these high-volume centers to effectively manage the complications or what was described as low ‘failure to rescue rates’.
Further taking cues from the successful implementation of enhanced recovery protocols following surgery in other subspecialties [47, 48], pancreatic surgeons have attempted to develop and implement clinical pathways following PD [49-51]. This, too, has shown not only to reduce hospital stay, but also costs [6, 23].
Morbidity following PD has remained one of the most stubborn statistics that has dogged pancreatic surgeons. The most common complications following PD include POPF, PPH and DGE. In this regard, surgeons have tried to systematically address these complications. The International Study Group for Pancreatic surgery (ISGPS) has provided evidence-based definitions for each of these entities [52-54] to ensure uniformity of their expression and comparability of data between centers and studies. The underlying risk factors for the development of POPF are the texture of the pancreatic gland and the diameter of the pancreatic duct. A soft, fat infiltrated gland with a small duct diameter (≤3 mm) is associated with a high risk of POPF [55, 56]. Thus, over the last few decades pancreatic surgeons have tried various techniques to tailor the strategy of the pancreaticoenteric anastomosis to the risk factors. Certain factors have been identified to help in reducing the risk such as the use of stents [57] and the use of octreotide. Octreotide has been used by some surgeons in the perioperative period with some evidence to suggest a reduction in the incidence of POPF [58]. This may be the reason for the reduced costs noted in patients who were selectively treated with octreotide [29]. As for the type of anastomosis, despite a fair amount of clinical research into this aspect [59] there remains work to be done to identify the best anastomosis for a particular gland texture. However, standardization of the technique employed by surgeons has been shown to reduce the risk of POPF [60]. The incidence of DGE has been suggested to be influenced by the location of the gastro-/duodenojejunostomy (antecolic versus retrocolic). However, the appropriate technique remains to be determined [61]. The placement of intra-abdominal drains during PD has been the focus of various studies. The rationale [62] behind abdominal drainage has been the value afforded by drains in forewarning the surgeon of potential intraabdominal complications [63] without putting the patient at risk of complications of the drain such as local pain, ascending infection via the drain [64, 65], and interference with patient ambulation. The issue of routine peritoneal drainage following PD suggests reduced risk of morbidity with routine drainage [66]. However, these drains must be removed as soon as possible [67] once sinister complications can be safely ruled out.
Minimally invasive PD was introduced with an aim to reduce the morbidity associated with the large incision utilized in open PD as well owing to its ability to improve vision during dissection. However, an analysis of a large cohort of patients has indicated that minimally invasive PD for cancer has been found to be associated with an increased 30-day mortality [68] and thus comprehensive protocols outlining criteria for implementation are warranted to optimize patient safety.

Thus, from the above analysis two things emerge, viz. factors influencing total hospital costs for PD are in essence markers of surgical quality and secondly, these factors can only be addressed by a true scientific approach and appraisal of the literature. Thus, rather than implementing cost-cutting measures such as across-the-board cuts in expensive services, staff compensation, and head count [12], focusing on improving the quality of surgery and care, itself, are potentially the best strategies to guarantee reduced costs. There are numerous methodologies to critically analyze processes and implement changes for improving outcomes. The author has previously suggested ways in which clinicians can utilize process excellence tools such as the Six Sigma methodology [69] with an aim to improving outcomes of hepatopancreatobiliary surgery and more specifically pancreaticoenteric anastomosis in PD [57]. This is just one of the many tools available. Either way, the bottom line is to reduce costs, we must improve quality!
Conclusion
Using PD, as an example, it is evident that the key to ‘bending the cancer cost curve’ is designing strategies to improve quality of the not only the procedure, but the process. Costs and quality cannot be separated. Reduction in costs can, and must only, be achieved by targeting excellence.
Conflict of Interests
Authors declare no conflict of interests for this article.