Research Paper - (2010) Volume 18, Issue 6
Professor, Institute for Health and Aging, University of California, San Francisco, CA, USA and Independent Evaluator, St Luke’s Health Care Center, California Pacific Medical Center, San Francisco, CA, USA
Desiree Arretz MD
Medical Director, HealthFirst and Director of Primary Care, St Luke’s Health Care Center, California Pacific Medical Center, San Francisco, CA, USA
Sarah Siebold RN MS CNS
Clinical Program Manager, HealthFirst and St Luke’s Health Care Center, California Pacific Medical Center, San Francisco, CA, USA
Elissa Hallen RN CDE
Certified Diabetes Educator, HealthFirst and St Luke’s Health Care Center, California Pacific Medical Center, San Francisco, CA, USA
Russell Lee PhD
Director, Health System Innovation, California Pacific Medical Center, San Francisco, CA, USA
Alana Ketchel MPP MPH
Consultant, Sutter Health Institute for Research and Education, San Francisco, CA, USA
Judy Li DrPH MBA
Vice President, Health System Innovation and Community Benefit, California Pacific Medical Care, San Francisco, CA, USA
Jeffrey Newman MD MPH
Director, Sutter Health Institute for Research and Education, San Francisco, CA, USA and the Institute for Health and Aging, University of California, San Francisco, CA, USA
Received date: 1 June 2010; Accepted date: 16 October 2010
Background The role of community health workers (CHWs) has expanded from outreach and education to working within a clinical team in a primary care setting. Aim To improve self-management among patients with type 2 diabetes incorporating CHWs as members of a clinical team. Methods A cohort of 114 patients with type 2 diabetes enrolled in 2007 participated in a teambased self-management intervention with followup in 2008. The study assessed whether significant changes occurred in clinical, patient satisfaction and activation measures after the intervention compared with baseline. The programme was located at St Luke’s Health Care Center in San Francisco, California, in an ethnically diverse neighbourhood serving predominantly low-income Latino patients. Clinical outcomes measured included glycosylated haemoglobin (HbA1c), low-density lipoprotein (LDL), blood pressure and total cholesterol. A Patient Activation Measure (PAM) assessed selfmanagement. Both provider and patient experiences with the programme were also assessed using a patient telephone satisfaction survey and provider focus group. ResultsThe majority of patients were Latino Spanish speaking women on public insurance.Thirty-one patients participated in a telephone satisfaction survey. Six providers participated in a focus group to assess satisfaction with care. HealthFirst had a positive impact, improving HbA1c among high-risk patients with type 2 diabetes (HbA1c_9.0) and maintaining glycaemic control among patients with controlled glycaemic level at baseline (HbA1c7.0). In addition, LDL, total cholesterol and self-management outcomes significantly improved. Ninety-sven percent of patients were satisfied with the CHWs’ support. Overall, providers’ comfort level in referring patients to CHWs was very high. ConclusionsPhysician–CHW partnership had a positive impact on patients’ self-management skills and clinical outcomes. Patients and physicians also had higher satisfaction with overall care. With appropriate training, CHWs can collaborate as team members with primary care providers and with non-medical providers to improve the quality of care.
community health community health worker, diabetes self-management, primary care, quality improvement, satisfaction with care
This pilot study assessed the extended role of the community health worker (CHW) in a multidisciplinary clinical team working alongside primary care phys-icians and licensed practitioners in a pilot programme, HealthFirst, a Center for Education and Prevention, at St Luke’s Health Care Center in San Francisco, California. This primary care pilot programme aimed to use the HealthFirst model to transform the primary care practice into a patient-centered ‘medical home’. The programme objectives were to recruit and train CHWs, define their extended roles and responsibilities, improve patients’ and primary care physicians’ satis-faction and track and measure clinical outcomes.
The new CHW role as a member of a clinical team
As pressures in the healthcare system, including escalating costs of care, have grown, with profound health disparities and a shortage of primary care clinicians, primary care services have often turned to community-based strategies to fill in the healthcare gaps, and these could provide an important re-source.[1–3]
The role of CHWs has expanded from mainly performing patient outreach and education to work-ing within a team in a primary care setting. In their new role as members of the clinical team, CHWs are the bridge between the primary care physician (PCP) and the patient, ensuring that patients understand, remember and are motivated to follow a care plan developed by all parties following the 15-minute visit.[4] This role is critical when working with immigrants, as well as patients who have limited English proficiency and low literacy levels.[5]
Diabetes burden among ethnically diverse communities
Type 2 diabetes is a growing worldwide health prob-lem, with broad disparities in healthcare-related out-comes between ethnic groups.[6] Diabetes is the sixth leading cause of death in the USA, affecting 10.7% of the adult population aged 20 years and older. Minority populations experience the burden of diabetes at a much greater rate than the Caucasian population.[7,8] US national data from 2007 showed that the preva-lence of diabetes was highest in the African American population (11.8%) while Latino Americans had the second highest prevalence (10.4%) compared with 7% of non-Hispanic whites.[9] The incidence of type 2 diabetes has reached epidemic proportions in the Latino American community, affecting approximately 2.5 million Latino Americans.[9] In addition, Latinos are less likely than non-Latino whites to receive appro-priate diabetes care and to self-monitor their disease.[10]
Similarly to the US, in the UK minorities continue to bear a disproportionate burden of diabetes. Patients of Pakistani and Bangladeshi origin were up to five times as likely, while the Indian population was three times as likely as white people to report diabetes.[11] Improving the quality of diabetes management is a priority worldwide for primary care practices. Therefore, it is critical to evaluate new models of chronic care.
CHWs can effectively improve patients’ manage-ment of their chronic condition by delivering health-care education and promoting healthy behaviours. Studies have found that when CHWs provide patient self-management education, HbA1c levels decrease and awareness about diabetes increases compared to baseline.[12–14] A randomised control trial with the African American population found that combining a CHW and a nurse case manager produced significant falls in diastolic blood pressure and triglycerides.[14] A study on the effectiveness of primary care interven-tions on glycaemic control and cardiovascular risk factors in minority ethnic groups with diabetes in the UK showed that case management with specialist diabetes nurses and CHWs improved glycaemic con-trol and links CHWs to the improvement of disease management. However, the relative effectiveness of these programmes, cost and sustainability of changes over time warrant further evaluation.[15]
In general, reliable data regarding CHWs working in a clinical setting remains limited. There has been a shortage of studies that show the potential role that CHWs can play in improving patients’ knowledge about their disease and satisfaction with their care.[13] More published studies in primary care settings, like HealthFirst, would help to confirm the promise of the CHW role in diabetes care management.
Pilot study design
The pilot study assessed whether significant changes occurred in clinical and Patient Activation Measures (PAMs) by comparing patients’ outcomes before (baseline) and after (follow-up) the HealthFirst inter-vention in a cohort of patients with type 2 diabetes who were enrolled in 2007 and followed up in 2008. In addition, we reviewed results of a patient satisfaction survey and the findings of a focus group assessing
providers’ satisfaction with the role of CHWs in the primary care setting.
Setting
The programme was begun in 2006 at the St Luke’s Health Care Center (HCC) in San Francisco, CA, a ‘safety-net’ group of clinics serving the underinsured and underserved Spanish-speaking population. St Luke’s Health Care Center serves approximately 10 000 low-income patients through adult and pediatric primary care clinics. As of December 2009, HealthFirst had enrolled 166 patients with type 2 diabetes.
St Luke’s HCC patients represent a wide racial and ethnic and linguistically diverse population. Accord-ing to Census 2005 data,[16] 46% of the residents within the communities served by HealthFirst have limited English proficiency and speak languages other than English at home; 42% are Hispanics, 16% are Asians, 16% are blacks and 23% whites. About 11% are below the federal poverty level.
Sample
For the purpose of this study, 114 patients were eligible to participate in the study and 23 patients (20%) were excluded because they only had one out-come measure. Only patients who had both an initial and a second measure from enrolment in January 2007 to December 2008 were included in the sample. As shown in Table 1, the majority of patients were Latino, Spanish speaking women on public insurance.

Patient satisfaction with quality of care results was based on a ten-minute telephone satisfaction survey conducted with 31 patients with type 2 diabetes randomly selected from 65 patients who were eligible to participate in the survey. Reasons for not partici-pating in the survey were: disconnected telephone, moved out of the area, answering machine or on vacation.
HealthFirst programme description
In the HealthFirst model, patients with diabetes are triaged to the programme by two primary care phys-icians. Three CHWs work closely with primary care physicians, a certified diabetes educator and a social worker to develop an action plan to improve the patient’s management of her or his chronic condition. In this model, the HealthFirst programme is com-pletely integrated with the rest of the clinic. The programme emphasises the concept of a medical home in that HealthFirst serves as the place patients come for preventive care that meets their linguistic, cultural and social needs.[17–20]
The HealthFirst intervention: CHWs as key members of the clinical team
CHWs provide a number of interventions to comp-lement the primary care provider’s role in assisting patients to manage their chronic conditions. These interventions can include: medication adherence, diabetes education, self-management support, group sessions and assistance with overcoming barriers, navigation and follow-up telephone support.
CHWs aim to gain patients’ trust and use a self-management approach to empower patients’ control of symptoms. During the HealthFirst visits, CHWs work collaboratively with the certified diabetes edu-cators who follow up on clinical issues for the PCP, such as ordering and reviewing laboratory tests, recom-mending medications and ensuring diabetes stan-dards of care are met. Types of patient contacts with CHWs include individual face-to-face visits and group sessions, as well as telephone follow-ups and reminders. This important role requires CHWs to go through intensive training to develop new competencies, in-cluding knowledge of the diabetes clinical protocols, medication reconciliation, new devices and patient self-management techniques.
Data sources
The pilot study had five data sources: a registry with clinical indicators, hospital aggregate records, a PAM, a patient telephone satisfaction survey and transcripts from a focus group to assess provider satisfaction with CHWs.
Clinical outcomes
Clinical data were gathered during routine clinical examinations at each visit, then entered into a com-puterised database by CHWs. Clinical indicators to measure improvement included HbA1c, LDL, body-mass index, systolic and diastolic blood pressure and total cholesterol.
Self-management outcomes
A PAM was administered by the CHW to each par-ticipant at baseline and one year after participating in the intervention. The PAM[21] assesses a patient’s knowledge, confidence and skills for self-management. The measure has 13 items pertaining to four domains: believing the patient role is important, having the confidence to take action, taking action to maintain healthy changes and maintaining healthy changes.
The PAM has been extensively tested in English and shown to be a valid, highly reliable instrument with good psychometric properties. The questionnaire was translated into Spanish, pretested with 15 hospital patients and translated back to English.
Patient satisfaction survey
The 11-question structured telephone patient satisfac-tion survey assessed overall approval of the HealthFirst programme and satisfaction with providers, CHWs and staff, as well as patients’ perception of the factor most helpful in improving their health. Survey ques-tions were developed by the research team including a psychologist, a primary care physician, a healthcare researcher and a nurse programme manager. The questions were adapted from the California Health Interview Survey[22] and the Consumer Assessment of Healthcare Providers and Systems survey (CAHPS),[23] a standardised survey instrument and data collection methodology for measuring patients’ perspectives of hospital care. The structured questions included: How often did the HealthFirst staff:
• explain things in a way that was easy to understand?
• listen carefully to you?
• spend enough time with you?
• treat you with courtesy and respect?
• help you make changes in your life like eating healthier, exercising more or taking care of your medications?
An open-ended question asked ‘In your opinion, what has helped you the most at HealthFirst?’ Given the low literacy level of the patients and their unfamiliarity with answering surveys, a three-point answer scale was used: agree; do not agree or disagree; disagree. A Spanish–English bilingual–bicultural co-investigator and research assistant translated and pilot tested the survey recruitment and consent materials to ensure that language was understandable, relevant and eth-nically/culturally sensitive. The survey was conducted in either English or Spanish. The questionnaire was developed in Spanish, then translated to English and pre-tested with ten patients in both languages. It was then translated back to Spanish.[24] The original and re-translated surveys were compared and points of diver-gence were noted. The translation was then corrected in order to more accurately reflect the intent of the wording in the original language.
Provider satisfaction with CHWs
To assess HealthFirst’s impact on providers’ primary care practice and relationship with CHWs, a focus group was conducted in 2009 with six HealthFirst providers: two pediatricians; two internal medicine physicians; one physician assistant; and one family nurse practitioner. The focus group guide was devel-oped by an interdisciplinary team of investigators. It was based on a review of existing literature, gaps in prior research and team input. The focus group guide included two open-ended questions and probes:
1 how has Healthfirst impacted your practice? and
2 how comfortable do you feel referring your patients to CHWs?
The facilitator followed guidelines for conducting focus groups.[25] All questions were designed to be neutral in content and tone to minimise the extent to which the session facilitator might influence partici-pants’ responses. The session facilitator also presented the questions in ways congruent with the flow of the conversation. The session lasted approximately 60 minutes.
Patient clinical outcomes
Statistical analyses include frequencies, cross-tabu-lations and t-test comparisons of clinical measures and PAMs over time from enrolment in January 2007 to December 2008. These analyses were based on data collected on a rolling basis from two measurement periods: baseline period – January to March 2007 and follow-up period – April 2007 to December 2008. Separate statistical analyses were performed using the SPSS statistical programme.[26]
Patient satisfaction survey
Patient responses to the 11 three-point Likert-type structured questions were analysed using SPSS. Pro-portions were obtained for each of the questions. Responses to the open-ended question asking for patient opinions about HealthFirst were transcribed verbatim. The first author then looked for main themes within the questions, each of which is illustrated with quotes.
Provider satisfaction focus group
Providers’ answers to the two questions designed to assess HealthFirst’s impact on provider practice and provider relationship with CHWs were transcribed verbatim. The first author read the focus group transcript and prepared a list of common themes that emerged from the group discussion. Both con-vergence and divergence of themes were explored with the research team. The team then discussed the sum-mary of emerging focus group themes. Once the coding scheme was developed after the first pro-visional definition of a category was made, excerpts were sought to help refine the category and outline the various themes within it. Emphasis was placed on a comprehensive coding scheme (i.e. topics discussed less often were included along with topics discussed more often).
A number of themes emerged from our grounded analysis of each of the two primary areas of focus. The categories described in Box 1 comprise the main themes, each of which is illustrated with quotes drawn from the excerpted sections of the transcripts.

Clinical outcomes
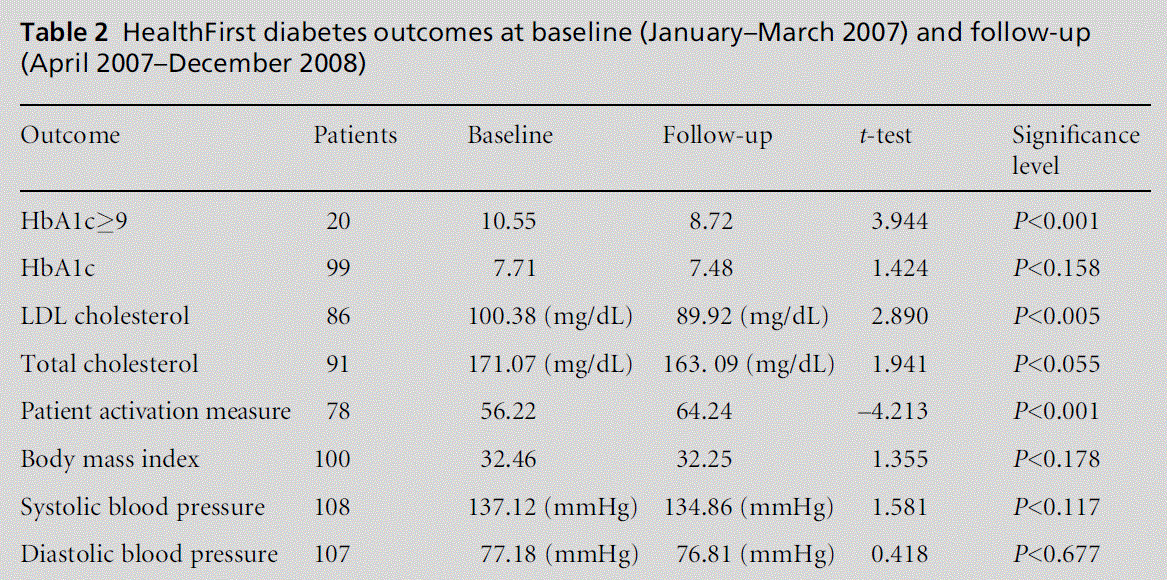
Overall, as Table 2 shows, HealthFirst had a positive impact on improving HbA1c among high-risk patients with type 2 diabetes (HbA1c 9.0) and on maintaining glycaemic control among patients with controlled glycaemic level at baseline (HbA1c<7.0). In addition, LDL, total cholesterol and self-management outcomes significantly improved among all participating patients.
Statistically significant improvements
• HbA1c significantly improved from baseline to follow-up among 20 high-risk diabetic patients whose HbA1c 9.0 at baseline. In those patients, the average HbA1c mean glucose level decreased from 10.55 at baseline to 8.72 at follow-up (t=3.944, P<0.001).
• Low density cholesterol (LDL) significantly decreased from baseline to follow-up among 88 diabetic patients (LDL mean values=100.38mg/dl and 89.92mg/dl, respectively; t=2.890, P<0.005).
• Total cholesterol average values significantly decreased from baseline to follow-up among 91 diabetic patients (total cholesterol mean values= 171.07mg/dl and 163.09mg/dl, respectively; t=1.941, P<0.055).
• Patient activation scores significantly improved from baseline to follow-up among 78 patients. PAM improved from an average score of 56.22, which means having moderate control of the dia-betes condition, to an improved control (PAM score=64.24) of the disease at follow-up (t=–4.213, P<0.001).
Patient satisfaction survey findings
Patient response rate was 47%. The majority of the survey participants (90%) were foreign born, 73% had lived in the USA for more than 21 years and were monolingual Spanish speakers (84%). About 50% had between seven and 12 years of education and the other half of the sample had one to seven years of education. About 10% reported excellent health status, 55% reported good health status, 27% perceived their health condition as fair and 13% perceived it as poor. Table 3 shows results on patient overall satis-faction with the programme and their perceptions of what was most helpful to them when participating in HealthFirst. The majority of patients (97%) were satisfied with HealthFirst services, particularly with the CHWs’ support. Most patients perceived that they were treated with courtesy and respect (97%), and reported that HealthFirst CHWs gave information in a way that was easy to understand (97%).

Patients’ satisfaction with HealthFirst and with CHWs
Patients addressed the open-ended question: ‘what do you like the most about HealthFirst?’. The most fre-quent theme mentioned was the importance of the provider–CHW–patient interpersonal relationship.
Patients most often emphasised the quality of the relationship as the main factor in trusting the HealthFirst programme. The main themes associated with trusting the provider and CHWs were: having rapport and a good relationship with the provider and the CHW; provider and CHW communication style and caring attitude; and communication in the patient’s language. All these themes fall under a main trust dimension – the importance that patients, particularly Latinos, give to their relationship with the provider and CHWs.
The following is a patient’s response regarding trusting CHWs:
‘Trust, (confianza)! I’m very happy with this excellent programme. I’m up to date with information about my health. Thanks to all the CHWs that take the time to explain and to answer questions, I don’t feel they do things in a hurry like other programmes. I like the way they treat me.’
Another dimension mentioned in the survey was patients’ perception of their improvement in self-managing their chronic condition:
‘I have learned to feel more confident. I have learned a lot, before the programme I felt insecure. This is an excellent programme. I like the care I have received from everyone, particularly the CHW.’
Provider and CHW interpersonal communication style is an important factor for patients. Patients most often favoured providers and CHWs who estab-lished rapport with good eye contact, a nice greeting, shaking patients’ hands and listening to and asking questions of patients. Patients emphasised trusting providers and staff who pay attention to them. A typical comment was:
‘This is the best programme I have joined. What I like the most is the caring attitude, the personal attention I get from the staff.’ Patients liked learning in groups coordinated by the CHWs:
‘I have lots of worries about my health. In the groups, it is good to hear other people and to know that others have problems too. The CHW always explains what to do and what not to do; the group has helped me to get support from other people.’
Provider satisfaction with HealthFirst focus group findings
A number of themes emerged from our grounded analysis of each of our primary areas of focus. The categories described below comprise the main themes:
HealthFirst positive impact on providers’ practice
Providers gave a very positive evaluation of the HealthFirst programme and were highly satisfied with CHWs helping patients to improve self-manage-ment of their chronic conditions. Providers reported that patients are better educated on how to manage their disease, medications and devices compared with other clinic patients who did not participate in HealthFirst. As a consequence of the CHW educa-tional intervention, physicians are able to see more patients. Healthcare providers also perceive that patients’ self-management skills of their chronic conditions, knowledge of their disease and improved medication adherence reduce unnecessary visits to the provider’s office, hospitalisations and visits to the emergency department.
Providers partnering with CHWs
Overall, providers’ comfort level in referring patients to CHWs is very high. They have experienced at first
hand their patients’ improvement in managing their chronic condition. Providers trust and feel comfort-able working with CHWs as partners in the education of patients to manage their chronic conditions.
Principal findings
Our findings indicate that the CHWs’ expanded role in a clinical setting had a positive impact on diabetic patients’ self-management. Results also demonstrated that with appropriate training CHWs were able to collaborate as team members with PCPs and with non-medical providers to improve patients’ out-comes. Providers and patients were highly satisfied with CHWs’ performance. The impact of CHWs seems to be higher among the group of high-risk patients with uncontrolled glycaemic levels, given that their HbA1c showed significant improvement from base-line to follow-up. As expected, those patients at higher risk met with CHWs more frequently than other patients. Our findings underscore the need to develop CHW–physician team programmes and to train prac-titioners on their implementation.
The positive effect of the CHWs and the clinical team at the individual level was evident given that the HealthFirst intervention maintained 87.2% of the patients in the well-controlled glycaemic group and moved 55% of the patients in the uncontrolled glycaemic group to a better control of their glucose level. In addition, LDL and total cholesterol improved significantly from baseline to follow-up among HealthFirst patients with diabetes.
Patients’ high level of satisfaction with HealthFirst was based on the quality of the relationship they established with the CHWs, which facilitated patients’ communication with the physician[27] and their under-standing of their condition and treatment. As expected, the majority of patients expressed the view that CHWs genuinely cared for them and this trust improved their confidence in managing their chronic condition.
As reported by previous studies, the main impact of CHWs on providers’ practices was through having motivated patients with improved knowledge of their chronic condition and better skills to prevent and manage their symptoms and adhere to medications[12–15] as compared with other healthcare centre patients.
Preventing the complications of diabetes requires a very close partnership between the patient and his or her healthcare providers. To achieve this objective, HealthFirst CHWs were essential in providing culturally competent care and supporting patients in taking control of their disease.
HealthFirst results point in the same direction as systematic reviews in the USA and the UK showing that primary practice interventions that focused on patients’ knowledge and problem-solving skills[5,15,28]
provided a higher level of interpersonal care[26] and collaboration with a multidisciplinary team improved the clinical outcomes of chronic conditions. Practices with higher scores for team climate also had higher scores for continuity of care and satisfaction.[26]
Strengths and weaknesses of the study
Our preliminary results have limitations. The absence of a control group does not allow for separating out of the outcomes of the intervention from those of other possible factors. Changes in the outcomes could well have occurred even in the absence of the intervention, due to a patient’s individual, social and contextual factors. Our findings are based on a small cohort of patients. Continuous monitoring of diabetes indicators with a larger sample of diabetic patients is critical to establish the long-term effect of the HealthFirst inter-vention. There is also insufficient evidence to assess which CHW intervention strategies are likely to be most effective. However, CHWs are most likely to be useful when delivering multilevel, culturally appro-priate strategies as suggested by the literature.[15,29,30]
Implications for practice
Our findings suggest that CHWs play an important role as members of a clinical team. Expanding the CHWs’ role liberates physician time to provide quality care and empowers patients to play a central role in managing their disease by setting obtainable goals and action plans to live a healthier life. CHWs, who are typically bilingual and bicultural individuals, have an understanding of the communities and serve as a bridge between PCPs and patients to implement lifestyle modification programmes by tailoring chronic care management plans to patients’ culture and psycho-social characteristics.[15]
Overall, the pilot study findings show promising benefits in incorporating CHWs in a clinical team working along with primary care physicians and licensed practitioners. CHWs also appear promising for improving diabetes patients’ control of their glu-cose levels and satisfaction with the quality of care received. CHWs could also potentially reduce the costs of health care by not only delivering education to patients, but by following up on treatments and providing care at a level closer to patients.[31] Further research with larger samples and a randomised control trial would be the next step to confirming our findings.
The Skirball Foundation, the Atlantic Philanthropies and the California Pacific Medical Center provided support for this pilot programme. The authors wish to acknowledge HealthFirst community health workers and staff for their dedicated service to patients.
The study was approved by the Institutional Review Boards of the Office of Human Research at the California Pacific Medical Center.
Not commissioned; externally Peer Reviewed.
None.