Keywords
Osteoporosis; Sarcopenia; Frailty; Old age care
Introduction
Clinical identification of frailty is a major step in taking care of elderly population. Previously, due to poor understanding and lack of definition, frailty was often mistaken for senile weakness and physical disability. However, due to increased elderly population and multiple studies, we now have a better understanding of frailty. Moreover, one of the primary definition and phenotype of frailty was described by Fried et al. [1] in 2001, and has been regarded as a standard definition and characterization of frailty in elderly population. This defined frailty with 5 criteria - exhaustion, weakness, slowness, physical inactivity and weight loss. Based on these criteria and the progression of osteoporosis, co-relation among these two should be relevant.
Understanding Frailty
Even if most of the researchers agree on the model provided by Fried et al, there have been numerous attempts at defining frailty using other methods and criteria [2,3]. Frailty is a wide concept, and no two frail individuals are similar. Many people recognize frailty but, quantification and analysis may prove difficult. With numerous descriptive terms like pre-frail, frail, etc the proper classification of frailty may be seriously hindered.
With the increase in elderly population, incidence of frailty is also increasing. UN recent data suggests projections of elderly population to 2 billion by 2050, with 426 million above 80 age group [4]. Looking at this trend, it seems a safe bet to expect the increase in frail population in the future.
With numerous health implications such as functional decline, loss of independence, deterioration in health status, increased risk of hospitalization [5] resulting in death, frailty syndrome warrants the most concern for caretakers among elderly . Since it is mainly considered an irreversible state [6], prevention or taking care of frailty once set seems more feasible than actually trying to nurse the patient from `frailty` or `pre-frail` to `fit` state.Multiple factors are responsible for development of frailty syndrome in the elderly. Malnutrition [7], osteoporosis and/or sarcopenia [8], smoking, alcohol consumption, lack of education and awareness, lack of physical activity [9], and many more. Prevention and caretaking are the only two socially and economically feasible options available at this stage.
Understanding Osteoporosis and Sarcopenia
Changes in musculoskeletal health in accordance with age are a well-established concept. Muscle mass and strength decline is commonly referred as sarcopenia [10] and bone mineral density and bone strength reduction is called osteoporosis [11]. Multiple factors such as reduced dietary protein intake, low Vitamin D levels, resistance of muscle protein synthesis to anabolic stimuli, menopause (in women) , lack of physical activity, obesity, all contribute to development of osteoporosis and sarcopenia [12,13]. Both phenomena contribute to higher risk of fall and fractures which later contribute to disability, dependence and decrease quality of life [14].
From the previous studies, sarcopenia is broadly used to describe the observed age-related decrease in muscle mass. It is associated with diminished physical ability, exhaustion, predisposition to fall injuries and proneness to incidental liability thus associating it with frailty. Sarcopenia is considered to have multifactorial etiologies. Commonly associated etiology is old age, when multiple disease burden associated pain and lack of ambulation likely contributes to sarcopenia and as a consequence, frailty [15]. Malnutrition also plays a vital role, with appetite reducing up to 25% in elderly population [16]. Along with contributing lack of Vitamin D and reduced protein intake, sarcopenia is more likely to occur [17,18]. Another theory that has wide acceptance is hormone theory. Studies have proven that testosterone level is associated with muscle mass [18] and women experience a sharp fall in muscle strength after the age of 55 often attributed to estrogen concentration decline [19,20].
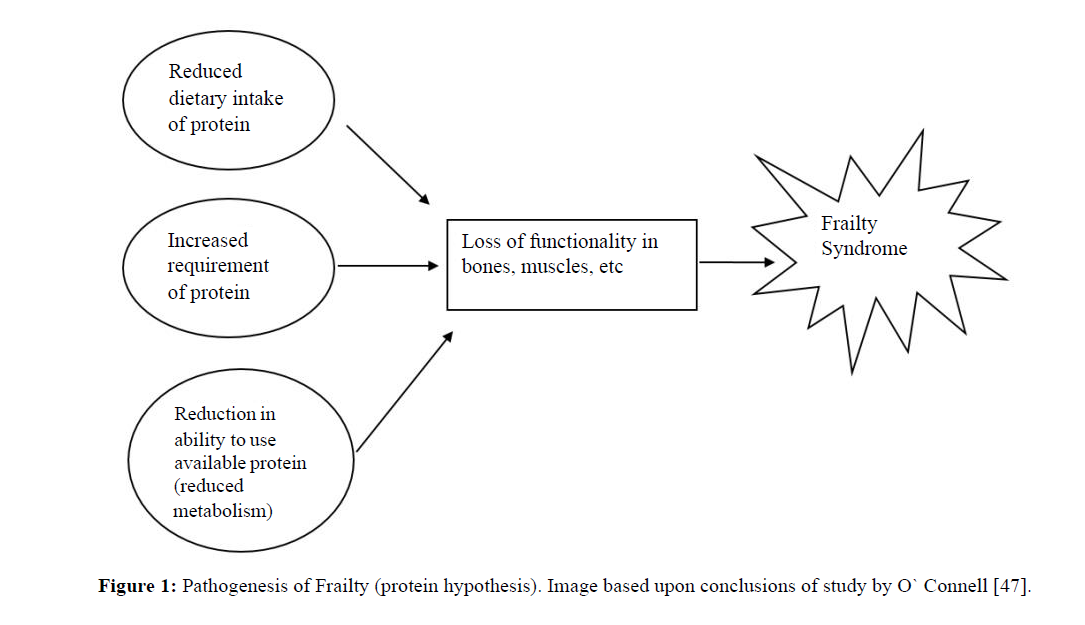
Osteoporosis, on the other hand has long been associated with old age and frailty. It is often described as micro architectural deterioration of bone tissue, low bone mass and increase in bone fragility and chances of fracture [21]. One of the indicators of osteoporosis is Bone Mineral Density or BMD. Although, by definition BMD should be bone related, it is however integrally related to decreased muscle, increased adiposity and frailty [22]. However, in multiple studies, BMD is described as the precursor to osteoporosis and prevention of osteoporosis is targeted towards improvement of BMD. Osteoporosis is not always single-handedly responsible for frailty, reduced dietary intake of protein however; osteoporosis with sarcopenia is a perfect recipe for frailty (Figure 1).
Figure 1: Pathogenesis of Frailty (protein hypothesis). Image based upon conclusions of study by O` Connell [47].
Tackling Osteoporosis and Sarcopenia
Osteoporosis once set is virtually impossible to reverse to the original condition. However, preservation of functionality along with bone composition should be the focus of health personnel in patients with osteoporosis. Multiple modalities of prevention of osteoporosis have been proposed. Most prominent among them are: Lifestyle modification, healthy lifestyle from a young age, Hormone replacement therapy (female targeted), exercise regimens, drugs and supplement therapy and prevention of falls. Each modality comes with their own pros and cons and a blanket protocol may not be sufficient for an individual or racial group. Moreover, HRT (Hormone Replacement Therapy) may come with its own set of complications including CHD and other cognitive function disorders that may complicate matters further. Other proposed management protocols are not mainstream or too experimental to be of significant clinical use. Multiple studies have been done to address the optimal type of intervention with the aim of taking care of patient with osteoporosis (Table 1).
| Study |
Year |
No. of cases |
Modalities |
Result |
Limitation |
| Bernard PL, et al. [35] |
2018 |
338 |
PBM-HE |
Improved |
Boot straping method utilized, no control population |
| Man-Ying Wang, et al. [36] |
2016 |
20 |
Hatha Yoga |
Improved |
Not RCT, small sample size, no significant variance among subjects |
| Yoo EJ, et al. [37] |
2010 |
28 |
3 month walking exercise program |
Improved |
Effects on balance not addressed, small sample size |
| Stone TM, et al. [38] |
2018 |
28 |
12 weeks yoga or cardio-kickboxing |
BMD not deteriorated |
Small sample size, no control group, limited timeframe of study |
| Gába A, et al. [39] |
2016 |
104 |
10 weeks of self-regulated brisk walking |
Modest effect on BMD |
Short study duration |
| Silverman NE, et al. [40] |
2009 |
86 |
Aerobic exercise with weight loss program |
Significant increase in BMD |
Non-RCT, DXA (Dual Energy X-ray absorptiometry) use during weight loss may incur a biased result |
| Yamazaki S, et al. [41] |
2004 |
50 |
Daily outdoor walking, minimum 1 hour with minimum 8000 steps, over 12 months |
No significant changes in BMD, however, NTX (N-terminal telopeptide) value could be used as an indicator |
Subjects not randomly divided, very modest change in BMD |
| Wu J, et al. [42] |
2006 |
136 |
Isoflavones(75mg/day) combined with walking(1 hr/3 times a week) vsisoflavonesvs walking vs placebo |
Combination of isoflavones+ walking shows significant improvement in BMD |
Japanese study population, so controlled intake of soy products could not be done, shorter duration of study |
Table 1: Some representative studies for prevention and management of osteoporosis.
Table 1 outlines some of the representative studies done for prevention of osteoporosis and increase in BMD approximately for the past 15 years. These studies mainly focus on the lifestyle modification and various exercise regimens for prevention of osteoporosis. The result gist shows that these studies may have succeeded in preventing/managing osteoporosis and increasing/ maintaining BMD.
Sarcopenia prevention, on the other hand relies exclusively on dietary supplementation and balanced nutrition. Since most components are responsible for development of sarcopenia are dietary in nature (protein, calcium, vitamin D), correction of these deficiencies may go a long way in preventing sarcopenia (Table 2).
| Study |
Year |
No. of cases |
Modalities |
Result |
Limitation |
| ShikanyJ.M, et al. [43] |
2014 |
5925 |
Diet quality index vs frailty status |
Diet quality was inversely proportionate with frailty |
Study limited to community dwelling white men. No significant racial variance |
| Roth SM, et al. [44] |
2004 |
302 |
Association with vitamin D receptor(VDR) with fat free mass in cohort study |
VDR translation site is closely associated with sarcopenia |
Older Caucasian males were the only subjects |
| Scott D, et al. [45] |
2010 |
686 |
Association between Vitamin D vs sarcopenia and low physical activity |
Baseline Vitamin D level was a positive indicator for muscle strength |
Less follow up, short period, other endocrine functions were not considered |
| RondanelliM, et al. [46] |
2016 |
130 |
Nutritional supplementation along with moderate exercise to tackle age related skeletal muscle weakness |
In comparison with placebo group, nutritional supplementation and exercise helps in generalized wellbeing and boosts strength |
Blood Vitamin D assay was not done. |
Table 2: Some representative studies for prevention and management of sarcopenia.
In addition to above studies linking different nutritional and endocrine causes to sarcopenia, exercise also plays a role in preventing sarcopenia [23]. Sedentary lifestyle is one of the main causes of sarcopenia and exercise plays a vital role in preventing sarcopenia. Some studies [24-26] have gone on to record that exercise is the most effective way of tackling sarcopenia (Table 2).
Path Forward After Onset of Osteoporosis and/or Sarcopenia
Frailty due to onset of osteoporosis and/or sarcopenia is a debilitating condition that severely reduced the quality of life of an individual. Severe limitation in skeletal muscle strength with recurrent fractures, primarily of large joints (eg. Hip joint) may impair mobility, reduce day to day activities and hamper the physical and psychological wellbeing. Once osteoporosis has onset and shown its effects(i.e.fractures), then it becomes vital for the individual to immediately undergo surgery to prevent long term complications. There are currently no consensual guidelines to improve the motility after hip joint surgery, however, all clinical protocols agree on early mobilization to prevent deep vein thrombosis.
More important than surgery, is the prevention. Since most fractures occur in frail population due to fall injuries, their prevention makes more sense. Home based exercises and other activities have shown to play a vital role in preventing fall injuries [27]. This method, however applies to people requiring very little or no care at home. In hospital or care facilities, however, it is a different matter altogether. Difference in interventions and level of dependency play a vital role [28]. Exercise, alongwith Vitamin D supplementation may be beneficial in these cases.
There are a very few specific interventions once osteoporosis and sarcopenia have set in. Most researchers agree on exercise and nutritional supplementation. High protein intake is recommended by some landmark studies [29]. On a similar note, ESCEO guideline proposes optimized recommended nutrient intakes for calcium (1000 mg/d), vitamin D (800 IU/d) andprotein (1.0–1.2 g/ kg BW/d) for the general management of patientswith osteoporosis [30]. Further, supplementation with branched-chain amino acid including but not limited to lucine has also been advocated [31]. Some home diet derived nutrients are also said to be beneficial [32-48].
Conclusion
Ageing is the inevitable part of life. By that logic, age related changes in the musculoskeletal system are also inevitable. Changes such as reduction in muscle mass, strength, power, BMD, bone strength tends to cause an increase in fracture, tendency of fall injury, and hamper the quality of life. However, the degree of changes and the quality of changes seem to be controllable. Due to multiple factors such as dietary habits, smoking, exercise, genetics, etc frailty affect some portions of populations more than the other.
Osteoporosis and/or sarcopenia are both very vital contributing factors for frailty. Even if we follow the age old doctrine of “prevention is better than cure”, osteoporosis and sarcopenia have multifactorial and multi faceted origin and effects, thus making it very difficult to prevent and manage. The only conclusion we can draw from this study alongwith conjunction with the above mentioned studies is that healthy lifestyle from mid-age combined with proper nutrition and exercise is the only reasonable way to prevent frailty. A multi-disciplinary approach including physicians, nurses, dietician, nutritionists, family members and caretakers is the only feasible way.
References
- Fried LP, Tangen CM, Walston J, Newman AB, Hirsch, C et al. (2001) Frailty in Older Adultsâ?¯: Evidence for a Phenotype. J Gerontol A Biol Sci Med Sci 56(3): 146-57.
- Clegg A, Young J, Iliff S, Rikkert MO, Rockwood K (2013) Frailty in elderly people. 381(9868):752-62.
- Morley JE, Argiles JM, Evans WJ, Bhasin S, Cella D, et al. (2008) Nutritional Recommendations for the Management of Sarcopenia. J American Med Directors Assoc 11(6): 391-96.
- ONU (2019) World Population Prospects 2019: Highlights. Futuribles141: 1-39.
- Bollwein J, Volkert D (2013) Nutritional Status According to the Mini Nutritional Assessment (MNA ®) And Frailty In Community Dwelling Older Personsâ?¯: A Close Relationship. J Nutr Health Aging 17(4):351-6.
- Cederholm T, Bosaeus I, Barazzoni R, Bauer J, Gossum A, et al. (2015) Diagnostic criteria for malnutrition - An ESPEN Consensus Statement. Clinical Nutrition 34(3): 335-40.
- Laur CV, Mcnicholl T, Valaitis R, Keller HH (2017) Malnutrition or frailtyâ?¯? Overlap and evidence gaps in the diagnosis and treatment of frailty and malnutrition. Appl Physiol Nutr Metab 42(5):449-58.
- Yoshimura N, Muraki S, Oka H, Iidaka T, Kodama R et.al (2018) Do sarcopenia and / or osteoporosis increase the risk of frailtyâ?¯? A 4-year observation of the second and third ROAD study surveys. Osteoporos Int 29(10):2181-90.
- Yu R, Wu WC, Leung J, Hu SC (2017) Frailty and Its Contributory Factors in Older Adultsâ?¯: A Comparison of Two Asian Regions ( Hong Kong and Taiwan ). Int J Environ Res Public Health 14(10):1096.
- Barry BK, Carson RG (2004) The Consequences of Resistance Training for Movement Control in Older Adults. J Gerontol A Biol Sci Med Sci 59(7): 730-54.
- Keaveny TM, Kopperdahl DL, Iii LJM, Hoffmann PF, Amin S (2010) Age-Dependence of femoral Strength in White Women and Men. J Bone Mineral Res 25(5): 994-1001.
- Maltais ML, Desroches J, Dionne IJ (2009) Changes in muscle mass and strength after menopause. J Musculoskelet Neuronal Interact 9(4): 186-97.
- Walrand S, Guillet C (2011) Physiopathological Mechanism of sarcopenia. Clin Geriatr Med 27(3): 365-85.
- Cruz-Jentoft AJ, Baeyens JM Bauer, Cederholm T, Landi F, Martin FC et.al (2010) Sarcopeniaâ?¯: European consensus on definition and diagnosis Report of the European Working Group on Sarcopenia in Older People. Age Ageing 39(4)412-423.
- Walston JD (2012) Sarcopenia in older adults. CurrOpinRheumatol24(6): 623-27.
- Nieuwenhuizen WF, Weenen H, Rigby P, Hetherington MM (2010) older adults and patients in need of nutritional support: Review of current treatment options and factors influencing nutritional intake. Clin Nutr 29(2): 160-69.
- Houston DK, Nicklas BJ, Ding J, Harris TB, Tylavsky FA, et al. (2008) Dietary protein intake is associated with lean mass change in older, community-dwelling adults: the Health, Aging, and Body Composition (Health ABC) Study. The American J Clin Nutri 87(1): 150-155.
- Morley JE, Anker SD, von Haehling S (2014) Prevalence, incidence, and clinical impact of sarcopenia: facts, numbers, and epidemiology-update 2014. J Cachexia Sarcopenia Muscle 5(4): 253-259.
- Samson M (2000) Relationships between physical performance measures, age, height and body weight in healthy adults. Age Ageing 29(3): 235-242.
- Lowe DA, Baltgalvis KA, Greising SM (2010) Mechanisms Behind Estrogen’s Beneficial Effect on Muscle Strength in Females. Exerc Sport Sci Rev 38(2): 61-67.
- Laurent M, Gielen E, Claessens F, Boonen S, Vanderschueren D (2013) Osteoporosis in older men: Recent advances in pathophysiology and treatment. Best Practice & Research Clinical Endocrinology & Metabolism 27(4): 527-539.
- Erlandson KM, Guaraldi G, Falutz J (2016) More than Osteoporosis: Age-Specific Issues in Bone Health. Curr Opin HIV AIDS 11(3): 343–350.
- Wohlgemuth SE, Lees HA, Marzetti E, Manini TM, Aranda JM (2011) An Exploratory Analysis of the Effects of a Weight Loss Plus Exercise Program on Cellular Quality Control Mechanisms in Older Overweight Women. Rejuvenation Res 14(3): 315-324.
- Landi F, Marzetti E, Martone AM, Bernabei R, Onder G (2014) Exercise as a remedy for sarcopenia. Curr Opin Clin NutrMetab Care 17(1):25-31.
- Marzetti E, Calvani R, Bernabei R, Leeuwenburgh C (2012) Apoptosis in Skeletal Myocytes: A Potential Target for Interventions against Sarcopenia and Physical Frailty – A Mini-Review. Gerontology 58(2): 99-106.
- Marques EA, Mota J, Machado L, Sousa F, Coelho M, et al. (2011) Multicomponent Training Program with Weight-Bearing Exercises Elicits Favorable Bone Density, Muscle Strength, and Balance Adaptations in Older Women. Calcified Tissue International 88(2): 117-29.
- Gillespie LD, Robertson MC, Gillespie WJ, Sherrington C, Gates S, et al. (2012) Interventions for preventing falls in older people living in the community. Cochrane Database Syst Rev.
- Cameron ID, Gillespie LD, Robertson MC, Murray GR, Hill KD, et al. (2012) Interventions for preventing falls in older people in care facilities and hospitals. Cochrane Database Syst Rev.
- Bauer J, Biolo G, Cederholm T, Cesari M, Cruz-Jentoft AJ, et al. (2013) Evidence-Based Recommendations for Optimal Dietary Protein Intake in Older People: A Position Paper From the PROT-AGE Study Group. J Am Med Dir Assoc 14(8): 542-59.
- Kanis JA, McCloskey EV, Johansson H, Cooper C, Rizzoli R, et al. (2013) European guidance for the diagnosis and management of osteoporosis in postmenopausal women. Osteoporos Int 24(1): 23-57.
- Katsanos CS, Kobayashi H, Sheffield-Moore M, Aarsland A, Wolfe RR (2006) A high proportion of leucine is required for optimal stimulation of the rate of muscle protein synthesis by essential amino acids in the elderly. Am J Physiol Endocrinol Metab 291(2): E381-7.
- Phillips SM, Tang JE, Moore DR (2009) The Role of Milk- and Soy-Based Protein in Support of Muscle Protein Synthesis and Muscle Protein Accretion in Young and Elderly Persons. J Am Coll Nutr 28(4): 343-54.
- Caroli A, Poli A, Ricotta D, Banfi G, Cocchi D (2011) Invited review: Dairy intake and bone health: A viewpoint from the state of the art. Int J Dairy Sci 94(11): 5249-62.
- Rizzoli R (2014) Dairy products, yogurts, and bone health. Am J Clin Nutr 99(5): 1256S-62.
- Bernard PL, Blain H, Gerazime A, Maurelli O, Bousquet J, et al. (2018) Relationship between a three-month physical conditioning posture-balance-motricity and health education (PBM-HE) program on postural and balance capacities of sedentary older adults: influence of initial motor profile. Eur Rev Aging Phys Act Eur Rev Aging Phys A 15(1): 14.
- Wang MY, Greendale GA, Yu SSY, Salem GJ (2016) Physical-Performance Outcomes and Biomechanical Correlates from the 32-Week Yoga Empowers Seniors Study. Evid Based Complement Alternat Med 2016:1-10.
- Yoo EJ, Jun TW, Hawkins SA (2010) The Effects of a Walking Exercise Program on Fall-Related Fitness, Bone Metabolism, and Fall-Related Psychological Factors in Elderly Women. Res Sports Med 18(4): 236-50.
- Stone TM, Wingo J E, Young JC, Navalta JW (2018) An Evaluation of Select Physical Activity Exercise Classes on Bone Metabolism. Int J Exerc Sci 11(2): 452-61.
- Gaba A, Cuberek R, Svoboda Z, Chmelík F, Pelclova J, et al. (2016) The effect of brisk walking on postural stability, bone mineral density, body weight and composition in women over 50 years with a sedentary occupation: a randomized controlled trial. BMC Women’s Health 16(1): 63.
- Silverman NE, Nicklas BJ, Ryan AS (2009) Addition of Aerobic Exercise to a Weight Loss Program Increases BMD, with an Associated Reduction in Inflammation in Overweight Postmenopausal Women. Calcif Tissue Int 84(4): 257-65.
- Yamazaki S, Ichimura S, Iwamoto J, Takeda T, Toyama Y (2004) Effect of walking exercise on bone metabolism in postmenopausal women with osteopenia/osteoporosis. J Bone Miner Metab 22(5): 500-8.
- Wu J, Oka J, Tabata I, Higuchi M, Toda T, et al. (2006) Effects of Isoflavone and Exercise on BMD and Fat Mass in Postmenopausal Japanese Women: A 1-Year Randomized Placebo-Controlled Trial. J Bone Miner Res 21(5): 780-9.
- Shikany JM, Barrett-Connor E, Ensrud KE, Cawthon PM, Lewis CE, et al. (2014) Macronutrients, Diet Quality, and Frailty in Older Men. J Gerontol 69(6): 695-701.
- Roth SM, Zmuda JM, CauleyJA, Shea PR, Ferrell RE (2004) Vitamin D Receptor Genotype Is Associated With Fat-Free Mass and Sarcopenia in Elderly Men. J Gerontol 59(1): B10-15.
- Scott D, Blizzard L, Fell J, Ding C, Winzenberg T, et al. (2010)A prospective study of the associations between 25-hydroxy-vitamin D, sarcopenia progression and physical activity in older adults. Clinical Endocrinology 73(5): 581-7.
- Rondanelli M, Klersy C, Terracol G, Talluri J, Maugeri R, et al. (2016) Whey protein, amino acids, and vitamin D supplementation with physical activity increases fat-free mass and strength, functionality, and quality of life and decreases inflammation in sarcopenic elderly. Am J Clin Nutr 103(3): 830-40.
- O’Connell ML, Coppinger T, McCarthy AL (2020) The role of nutrition and physical activity in frailty: A review. Clin Nutr ESPEN 35: 1-11.
- Marzetti E, Calvani R, Tosato M, Cesari M, Di Bari M, et al. (2017) Physical activity and exercise as countermeasures to physical frailty and sarcopenia. Aging Clin Exp Res 29(1): 35-42.