Quality Improvement Report - (2003) Volume 11, Issue 2
1Consultant Community Paediatrician, Medway Maritime Hospital, Gillingham, Kent, UK
2General Practitioner Registrar, Darent Valley Hospital, Dartford, Kent, UK
3Clinical Audit Co-ordinator, West Kent NHS and Social Care Trust, Maidstone, Kent, UK
Received date: 23 September 2014; Accepted date: 11 February 2015; Published date: 21 March 2015
Community paediatricians have developed a specialised role in areas of child development, disability, social and behavioural paediatrics.1 Non-attendance in community paediatric clinics has Ž nancial implications for the NHS, because the average appointment for developmental and behavioural assessments lasts one hour. Clinical governance has identiŽfied non-attendance as a signiŽ cant area for improvement. The aim of this study was to ascertain the clinical and demographic proŽ les of patients nonattending these clinics
Community paediatricians have developed a specialised role in areas of child development, disability, social and behavioural paediatrics.[1] Non-attendance in community paediatric clinics has financial implications for the NHS, because the average appointment for developmental and behavioural assessments lasts one hour. Clinical governance has identified non-attendance as a significant area for improvement. The aim of this study was to ascertain the clinical and demographic profiles of patients nonattending these clinics.
All appointments booked from 28 September 2001 to 28 December 2001 for middle-grade community paediatricians were analysed retrospectively. The community paediatric notes were handsearched and data were collected via a data sheet of age, sex and diagnosis of the patient, referrer, child protection issues, carers with learning di¤culties and/or mental health problem and single parent family. A questionnaire was sent to carers of non-attending patients enquiring about specific reasons for non-attendance, such as ill health, transport problems, non-receipt of appointment letters and forgetfulness.
For the purpose of this study, appointments cancelled by carers on the day of the appointment were regarded as non-attendance. Appointments cancelled either due to doctors not being available because of sickness, or patients cancelling their appointment early, enabling us to find another patient to fill the slot, were excluded from the analysis. Multidisciplinary, urgent and consultant appointments were excluded to avoid bias, as di¡erent booking systems were in place.
Eighty-three appointments were booked in the three-month period. Eleven fell within the exclusion criteria, 27 patients (32.5%) did not attend. Of 72 appointments that could have been analysed, five sets of notes were not available at the time of the study, therefore 67 appointments were analysed (41 attendees and 26 non-attending). The age ranged between 12 months and 13 years 9 months (mean seven years). Table 1 shows that most of under five year olds and most on the child protection register did not attend, and Table 2 shows that children with behavioural problems and learning di¤culties were most likely to attend, both initial and follow-up appointments. In addition, we found that, if the waiting time for the first appointment was less than four weeks, three out of four children attended, while 14 of 23 attended, if they had to wait over four weeks. All three referrals from general practitioners were attended. Of ten nonattending their first appointment, three were referred by health visitors, three by education professionals and one each by a hospital doctor, head teacher, child and adolescent mental health services and in-care medical sta¡.
Patients non-attending a follow-up appointment failed to attend 40% of all their previous appointments and cancelled another 14% of them on the day of the appointment. Social deprivation, described by Jarman score, influenced attendance, as 18 of 33 children failed to attend the clinic if the Jarman score in the electoral ward of their home address was higher than ten, meaning a deprivation score ten times the national average for England and Wales. Only four of 22 children did not attend from areas with Jarman score less than ten.
Not surprisingly, only four of 26 carers of the nonattending group returned the postal questionnaires (response rate of 15%), stating the following reasons for non-attendance at their appointments: one was not satisfied with the level of service given on a previous appointment and three stated that they did not receive their appointment letters.
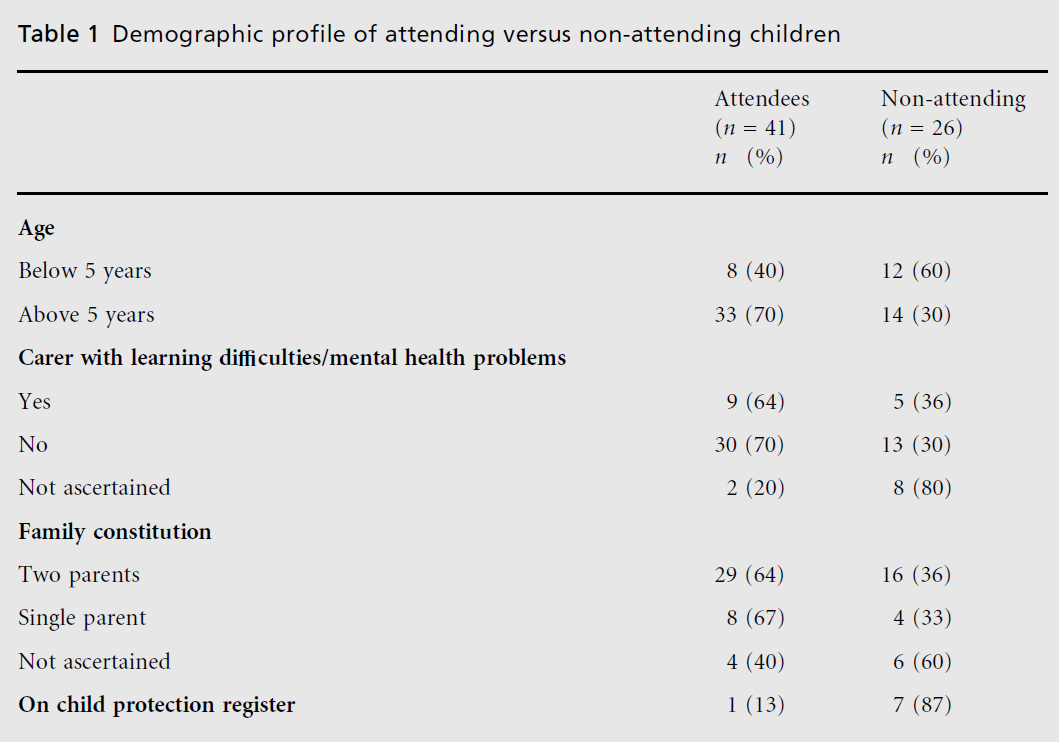

Table 1: Demographic pro® le of attending versus non-attending children
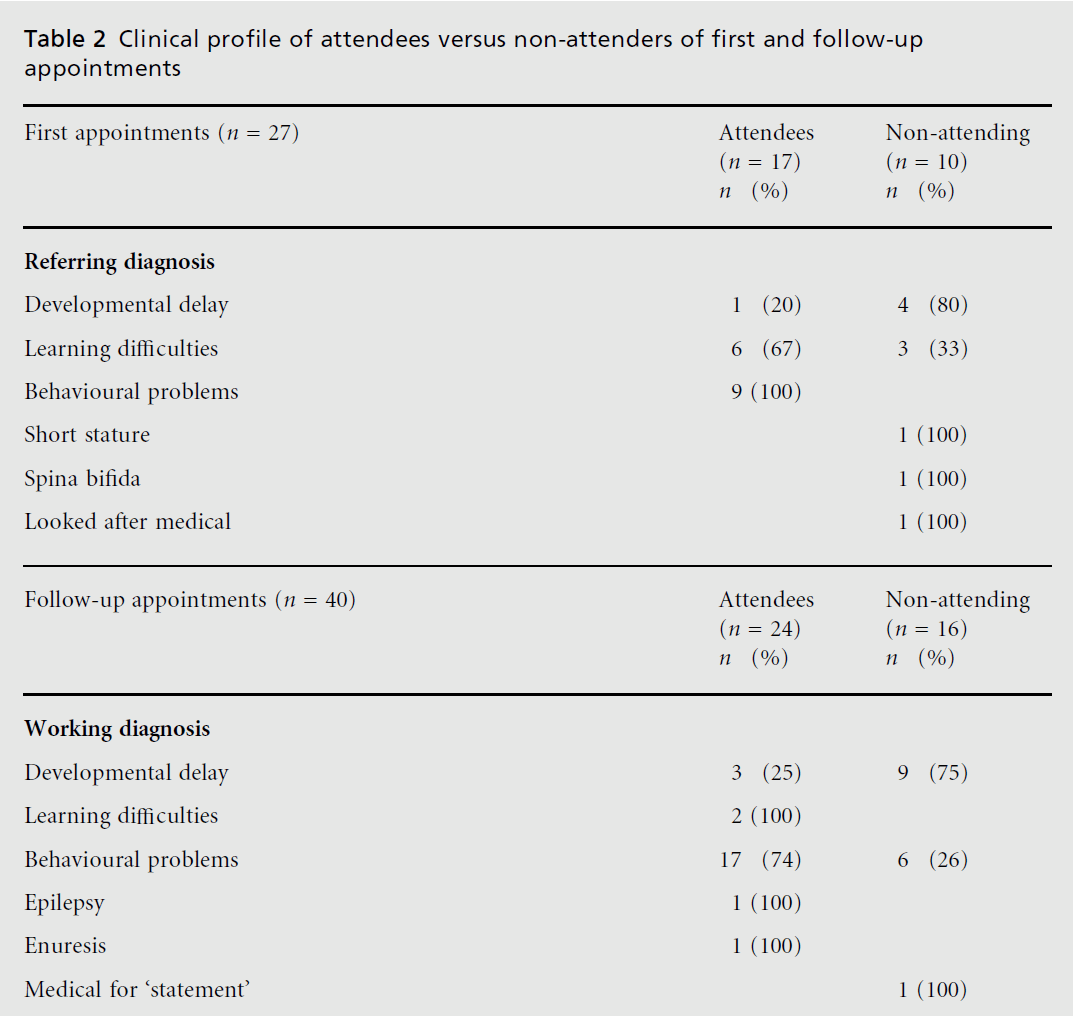
Table 2: Clinical pro® le of attendees versus non-attenders of ® rst and follow-up appointments.
The national figure for non-attendance at outpatient clinics in the UK is 12%; it ranges from 5% to 34% between specialities and regions.2 Our study found a high non-attendance rate of 32.5%. It is known that paediatric patients tend to have higher outpatient non-attendance rates, especially those from ethnic minorities.[3–7] Although targeted telephone reminders reduced non-attendance in a paediatric hospital clinic from 34% to 12.3%, extension of outpatient practice into communitybased outreach clinics has not improved attendance. [3,8] Clarifying the purpose of individual visits was identified as the most important area of improvement in paediatric and adult outpatient services.[4,5] Paediatric patients are often reviewed inappropriately and parents would be happy to be discharged or o¡ered an ‘open’ appointment to be seen when they are concerned.6 One retrospective audit of all paediatric outpatients showed that one-third of the non-attenders were known to social services.[9]
Our study is the first to investigate non-attendance in community paediatric clinics. Although the numbers in our study were relatively small, there were strong characteristics in the non-attending group. Failing to attend was most likely, if the child was under five years old, had developmental delay, waited more than four weeks, was on the child protection register and lived in a deprived area with a Jarman score more than ten times the national average for England and Wales. Children who did not attend one appointment missed 40% of further appointments. Therefore, reduction of the nonattendance in community paediatric clinics should be a priority for the children’s services.