Case Report - (2023) Volume 20, Issue 5
Mishaps during Composite Restoration: Acute Allergic Angioedema and Contact Dermatitis
Sameer Makkar,
Shabnam Negi,
Vanshish Sankhyan* and
Ajitesh Kaplish
Department of Conservative Dentistry and Endodontics, Bhojia Dental College and Hospital, Himachal Pradesh, India
*Correspondence:
Vanshish Sankhyan, Department of Conservative Dentistry and Endodontics, Bhojia Dental College and Hospital, Himachal Pradesh,
India,
Email:
Received: 05-May-2023, Manuscript No. IPDEHC-23-16379;
Editor assigned: 08-May-2023, Pre QC No. IPDEHC-23-16379 (PQ);
Reviewed: 22-May-2023, QC No. IPDEHC-23-16379;
Revised: 05-Jul-2023, Manuscript No. IPDEHC-23-16379 (R);
Published:
12-Jul-2023, DOI: 10.36648/2049-5471.20.5.37
Abstract
Unexpected results and negligence can lead to mishaps in the dental operatory. With the trend of
using tooth colored restorations mishaps have also increased which are sometimes ignored due to
lack of knowledge. Although, resin based restorative materials are considered safe, their constituents
can leach out and cause allergies in patients as well as dental professionals. Safe handling of these
resin based materials is critical due to increased risk of occupational health hazards. Most of the
allergies caused by resins are related to monomers based on methacrylic acid which is found in almost
all types of dentin bonding agents. Also, it is estimated that 5% to 10% of all allergic contact
dermatitis reports in dental professionals are due to contact with methacrylate. On the contrary, 37%
phosphoric acid in etchant results in necrosis and ulcerative lesions due to vascular nature of the oral
cavity. The purpose of this article is to help dentists to become aware of allergies/mishaps that can
occur due to bonding agents and phosphoric acid, thereby leading to prevention and their early
management.
Keywords
Allergic contact dermatitis; Bonding agents; Allergic reaction; Anaphylaxis; Angioedema;
Dental allergens; Mucosal burn; Acid etching; Adverse reaction; Hypersensitivity reaction
Introduction
Wretched and unforeseen occurrences can occur during
dental treatment. Most common being anaphylactic reactions
to local anesthetics, allergic reactions to dental materials,
antibiotics, nonsteroidal anti-inflammatory drugs, etc. A
patient with orofacial edema arouses several possibilities in
the dental practitioner’s mind [1]. However, rare diseases may
mimic or present similarly to common diseases, resulting in a
“medical mystery.” Such diagnostic quandary can be
disturbing for both the patient and the dentist.
The resin based restorations as well as their constituents
must satisfy the biocompatibility testing as they are indicated for a long time period in the mouth and can cause allergic
reactions in the form of urticaria, swelling, rash, contact
allergy and rhinorrhea. The clinical features include burning,
pain and dryness of mucosa, nonspecific stomatitis and
cheilitis. Composites, latex gloves, local anesthetic agents,
endodontic materials, impression materials, and metals are
some of dental materials suspected with biocompatibility
issues.
The demand for esthetics has increased the application of the
acid-etch technique thus increasing the use of phosphoric
acid as an etchant. 30% to 40% phosphoric acid is the most
used concentration however the chemical is potentially
caustic in higher concentrations. In a review of local and systemic responses related to the effects of dental restorative
materials, Stanley found that inappropriate acid etching
procedures with 50% phosphoric acid could lead to ulceration
and sloughing of oral tissues [2]. To date, adverse reactions
caused by its contact with the oral mucosa are rare except for
the references to such occurrences only in oral pathology
texts [3-5].
Allergic Contact Dermatitis (ACD) is a non-infectious
inflammatory disease of the skin characterized by a delayed
hypersensitivity reaction (type IV T-cell-mediated) due to
contact with methacrylate present in bonding agents [6,7].
The first case report that follows showed an adverse reaction
to etchant thus indicating the need of taking precautions to
prevent its spillage in undesired areas while the purpose of
second case report was to promote the awareness regarding
the allergies due to methacrylate in bonding agents when
placed on gloved hands during composite restorations.
Case Presentation
Case 1
A 32 years old male patient working in a local pharma
company attended for dental treatment at Bhojia dental
college and hospital. He was treated by an intern, and as a
treatment plan composite restoration was to be carried out in
37. Rubber dam isolation could not be accomplished due to
the recalcitrance of the patient.
The ivoclar Te-Econom plus composite material was used.
While etching the surfaces with 37% phosphoric acid of a
lower left second permanent molar, the applicator tip of the
etchant contacted the upper lip leading to accidental spillage
of the acid (Figure 1a). In the process of cleaning the etchant
with the gloved hands, phosphoric acid also encountered the
cheek on the right side and area below the supraorbital ridge
of the eye on left side (Figure 1b). Meanwhile, the
patient started complaining of itching and swelling over the
affected area. The clinical examination revealed a diffuse,
painless, pale, soft, non-tender, non-pitting erythematous
swelling without the evidence of erosion and ulceration. The
patient gave no history of allergy. The vital parameters
measured were normal. On further examinations, no other
signs and symptoms were diagnosed. As the patient seemed
stable, he was discharged with the prescription of
prednisolone 10 mg and cetirizine 10 mg orally, once daily for
3 days. Follow-up examination after 24 hr showed a
resolution of swelling drastically (Figure 2a). The patient
reported that he didn’t take the medications due to some
emergency work and instead applied glycerine and coconut
oil which was readily available with the patient and there
was an improvement in symptoms (Figure 2b). A followup
examination after 2 months revealed no sign of
previously reported lesions (Figure 2c). The diagnosis of
acute allergic angioedema of upper lip was made based
on the following criteria, the swelling was sudden in onset,
limited to oral mucosal regions, absence of pain, pruritus,
pitting, and erythema and the symptoms subsided in 24 hr.
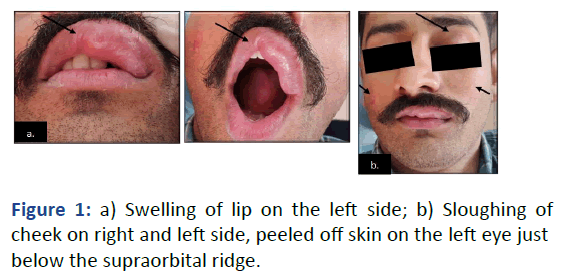
Figure 1: a) Swelling of lip on the left side; b) Sloughing of
cheek on right and left side, peeled off skin on the left eye just
below the supraorbital ridge.

Figure 2: a) Follow-up after one day; b) One month; c) Two
months follow-up.
Case 2
A post-graduate resident was performing esthetic restorations
on anterior teeth with composite resin. Despite of practicing
all standard measures of infection control including gloves
and maintaining the cleanliness of the working area, the
bonding agent came in contact with the gloved hand for
around 34-40 minutes (Figure 3a and 3b). As soon as the
resident noticed the contamination and mild itching, he
immediately replaced his gloves. The dorsum of the left hand
was affected the most which was thereafter recalled by the
resident as his habit of placing the bonding agent over the
gloved area for ease and convenience (Figure 3c). The
application of topical corticosteroid cream for a few days
relieved his signs and symptoms (Figure 3d).
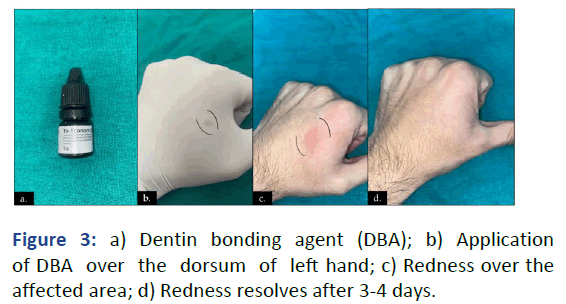
Figure 3: a) Dentin bonding agent (DBA); b) Application
of DBA over the dorsum of left hand; c) Redness over the
affected area; d) Redness resolves after 3-4 days.
Results and Discussion
The introduction of resin composites in 1950’s has
revolutionized the current dental practice. A saying describing
the resin composites aptly “Nothing is free everything in life
comes with the price so is the resin-based composites with their allergies. As these are tooth colored restorations, there
demand is booming at a much faster rate and so are the
mishaps associated with them. A matter of utmost
importance is the accidents associated with the use of
etchant and bonding agent. The first case was diagnosed with
acute allergic angioedema of upper lip due to the mishandling
of 37% phosphoric acid by the intern. In such cases, the first
line of treatment is oral antihistamines if it does not help
corticosteroids/antihistamines intravenously should be
administrated.
Frequent monitoring of the patient should be done till the
symptoms subside. Careful attention when using etchant
along with the proper use of rubber dam is a must to avoid
such mishaps. Precautions include the proper identification as
well as the exclusion of the causative agent. Educating the
patient regarding the symptoms and management strategies
are essential in these cases. The diagnosis of cheilitis
granulomatosa and cheilitis glandularis as the cause was ruled
out as there were no signs of ulceration in the case.
In the second case, the post-graduate resident was diagnosed
with Allergic Contact Dermatitis (ACD) as he applied bonding
agent on his left hand during the restorative procedure.
Incidence of 5% to 10% of all ACD in dental health care team
members are due to methacrylate [8,9]. The primary
manifestation of methacrylate present in bonding agent is
eczematous rash [10,11]. Also, repeated exposure to
unpolymerized methacrylate may cause finger or hand
neuropathies, with burning or prickling sensations. A detailed
history from affected colleagues and interns on placement on
bonding agent was also taken in which each student
described applying uncured dentin bonding adhesive material
on the gloved area. The reason given for bonding agent
application on hand was to lubricate the composite
placement instrument while placing and packing uncured
paste into the cavity and to prevent instrument/composite
sticking. However, it is possible that other constituents in the
bonding agent led to the development of redness and itching.
Prevention is always better than cure. These two case reports
highlighted that dental health professionals must be aware of
all the possible allergic manifestations due to inattention to
detail and negligence.
Conclusion
Having encountered the hazardous complications, we as
dentists should be prepared to expect the unexpected
situations when confronted and to render the most decisive
treatment possible. Regular use of rubber dam should be
encouraged to prevent perilous effects of etchant containing
37% phosphoric acid and bonding agent used in the esthetic
procedures, which is ultimately the main bread earner for the
clinician in present esthetic world.
Acknowledgments
The authors would like to thank Dr. Anurag, Dr. Sandeep, Dr.
Jyotsana and Dr. Rishika for their collaboration during this
project.
Conflict of Interest
The authors do not have any financial interest in the
companies whose materials are included in this article.
Consent Statement
Written informed consent was obtained from the patient to
publish this report in accordance with the journal's patient
consent policy. Informed consent was also obtained from the
patient informing the clinical procedure to be carried out and
its related complications which are attached below.
References
- Kulthanan K, Jiamton S, Boochangkool K, Jongjarearnprasert K (2007) Angioedema: Clinical and etiological aspects. Clin Dev Immunol. 2007:26438
[Crossref] [Google Scholar] [PubMed]
- Stanley HR (1993) Effects of dental restorative materials: Local and systemic responses reviewed. J Am Dent Assoc. 124(10):76-80.
[Crossref] [Google Scholar] [PubMed]
- Regezi JA, Sciubba J, Jordan RC (2016) Oral pathology: Clinical pathologic correlations. Elsevier Health Sciences.
[Google Scholar]
- VJ B (1994) Red and white lesions of the oral mucosa. In: Lynch MA. Brightman VJ, Greenberg MS, editior. Burketts oral medicine: Diagnosis and treatment. Rashid Latif Medical College, Pensyvania. 58-59.
[Google Scholar]
- LR E (1992) White Lesions. Clinical outline of oral pathology: Diagnosis and treatment. 3rd edition. Pennsylvania, Lea and Febiger. 9-29.
[Google Scholar]
- Milia E, Cumbo E, Cardoso RJ, Gallina G (2012) Current dental adhesives systems. A narrative review. Curr Pharm Des. 18(34):5542-5552.
[Crossref] [Google Scholar] [PubMed]
- Martin SF (2015) Immunological mechanisms in allergic contact dermatitis. Curr Opin Allergy Clin Immunol. 15(2):124-130.
[Crossref] [Google Scholar] [PubMed]
- Sanchez-Perez J, Gonzalez-Arriba A, Goiriz R, Garcia-Diez A (2008) Occupational allergic contact dermatitis to acrylates and methacrylates. Contact Dermatitis. 58(4):252-254.
[Crossref] [Google Scholar] [PubMed]
- Hunasehally RY, Hughes TM, Stone NM (2012) Atypical pattern of (meth) acrylate allergic contact dermatitis in dental professionals. Br Dent J. 213(5):223-224.
[Crossref] [Google Scholar] [PubMed]
- Wrangsjo K, Swartling C, Meding B (2001) Occupational dermatitis in dental personnel: Contact dermatitis with special reference to (meth) acrylates in 174 patients. Contact Dermatitis. 45(3):158-163.
[Crossref] [Google Scholar] [PubMed]
- Hamann CP, Rodgers PA, Sullivan K (2003) Allergic contact dermatitis in dental professionals: Effective diagnosis and treatment. J Am Dent Assoc. 134(2):185-194.
[Crossref] [Google Scholar] [PubMed]
Citation: Makkar S, Negi S, Sankhyan V, Kaplish A (2023) Mishaps during Composite Restoration: Acute Allergic Angioedema and
Contact Dermatitis. Divers Equal Health Care. 20:37.
Copyright: © 2023 Makkar S, et al. This is an open-access article distributed under the terms of the Creative Commons
Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author
and source are credited.




