Key words
gay men, general practice, heterosexual
assumptions, lesbians, primary care, protocols
Introduction
This study was part of a wider initiative to explore
marginalised communities’ access to primary care
services in one London borough, conducted in the
context of researchwhich reveals considerable levels of
mistrust among lesbians and gay men about their
relations with healthcare practitioners. This particular
study aimed to draw on the experiences of lesbian and
gay informants to identify both barriers and examples
of good practice, and to engage with the growing body
of literature in this field (Silvestre, 2001; Heaphy et al,
2003; Hinchliff et al, 2005; Fish, 2006; Shankle, 2006) as a basis for formulating a body of recommendations
about how general practice might be reorganised to
benefit the health and wellbeing of lesbians and gay
men in its area of responsibility
Background
This North London borough has, according to the
2001 Census (Office of National Statistics, 2003), a
population of 218 341. It is a diverse, multiracial, multicultural population – factors that present challenges
to the primary care services offered in general
practice. The study reported here was one of several
studies commissioned by a community organisation,
with funding from the Neighbourhood Renewal Fund
(www.neighbourhood.gov.uk), into the experiences
of minority groups in accessing primary care services.
Given that there is no monitoring of lesbian and gay
people, it is difficult to estimate the size of the lesbian
and gay populations. The Department of Trade and
Industry (DTI) places the figures between 5% and 7%
of the total adult population (DTI, 2003). Given the
traditional patterns of movement to large cities by
lesbian, gay and bisexual (LGB) populations, it can be
argued that the LGB population of the borough in
which this study took place is likely to be at least 7%.
We thus deduced that the LGB population was likely
to be in the region of 15 000 people.
The approach of general practitioners (GPs) towards
the social and familial context of people who access
their services has been widely debated. The Royal
College of General Practitioners (RCGP, 2002) has
endorsed a definition of general practice/familymedicine
which is respectful of diversity, and person centred
in its focus. General practice, according to this definition,
is ‘normally the point of first medical contact
within the healthcare system, providing open and
unlimited access to its users, dealing with all health
problems regardless of the age, sex, or any other
characteristic of the person concerned’ (European
Academy of Teachers in General Practice, 2002, p. 3).
The specialty of general practice includes ‘care for
individuals in the context of their family, their community,
and their culture, always respecting the autonomy
of patients’ (European Academy of Teachers
in General Practice, 2002, p. 3). Schilder et al (2001,
p. 1646) have argued that ‘family’ can best be identified
as ‘those persons closest in knowledge and
affection, which should be the criteria in interpreting
any individual’s social support’. This definition of
‘family’ is broader than that of more traditional
models which tend, in the UK, to be based around
heterosexual couples.
Heterosexual assumptions can prevent or inhibit
practitioners from identifying particular patterns of
non-heterosexual living; this, in turn, can result in
non-communication and misdiagnosis. Heaphy et al
(2003), in a study of lesbian, gay and bisexual people
over 50years, revealed these heterosexual assumptions
on the part of health service providers as creating
barriers to care. Phillips and Marks (2006) showed
that the silencing of non-heterosexual identities in the
field of residential aged care facilities hindered the
provision of services that are culturally sensitive, safe
and inclusive. Westersta˚hl and Bjo¨rkelund (2003), in a
study of GPs, identified GPs’ traditional concepts of family and sexuality as a barrier to making lesbian
patients visible. The lack of dialogue encourages some
practitioners in the assumption that the lifestyles of
those from non-heterosexual minorities are dysfunctional
(Hinchliff et al, 2005).
The emergence of social movements since the 1960s
and the subsequent increase in the number of meeting
places openly catering for LGB people have helped
people to come out as lesbian or gay. There is huge
diversity within the LGB population. While many will
be sexually active with people of the same sex, some
will be aspiring to be so, and others will be occasionally
sexually active with people of either sex. Additionally,
there will be people living with the memory of having
been sexually active with people of the same sex.
Coming out as lesbian or gay is, however, more
than an acknowledgement of particular sexual activity.
Plummer (1995, p. 82) has argued that it can be ‘the
most momentous act in the life of any lesbian or gay
person’, not so much an exchange of information as a
redefinition of the relationship between the lesbian or
gay person and the person listening to their coming
out story (Plummer, 1995; Saddul, 1996; Taylor,
1999). Saddul (1996, p. 4) makes the point that ‘repeated
negative experiences with providers ... may cause a
person to delay or avoid seeking care’. Fish (2006) has
developed a theory of heterosexism to conceptualise
practices experienced in healthcare settings. Bakker
et al (2006) show that use of health services is higher
among lesbian, gay and bisexual people than heterosexual
people. Schilder et al (2001, p. 1656) indicate
the difficulty for health providers ‘when a minority
group itself often has discomfort self-identifying ...
when their social identity is also associated with
stigma’. The problems of living with stigma result in
manylesbian and gay people experiencingmental health,
rather than sexual health, as their primary area of
health concern (McFarlane, 1998; King and McKeown,
2003). In a study of gay men and primary care, Cant
(2002) identified a reluctance on the part of GPs to
make referrals to gay community organisations with
the potential to prevent the onset or the accumulation
of mental health problems.
Conduct of the study
London South Bank University (LSBU) was commissioned
by a lesbian and gay-led community organisation
to conduct research to explore access to
general practice services by lesbians and gay men in
one London borough. This study was one part of a
wider initiative to explore marginalised communities’
access to GP services in primary care. Ethical approval
for the study was obtained from the appropriate local
research ethics committee. The research team comprised the two authors of this paper, and two other researchers
(see acknowledgements) who facilitated
two of the focus groups and contributed to parts of
the analysis of focus group data, as described below.
Steering group meetings of staff and volunteer
managers from the community organisation and staff
from LSBU agreed that the research process would
include a variety of methods with a strong emphasis
on qualitative approaches (Cresswell, 2003; Britten
and Fisher, 1993). An overall theoretical framework
for the research was provided by intersectionality
(Sloop, 2005). Intersectionality theory originated in the
writings of African-American and Third World feminists,
concerned to counter Western feminist theory’s
insufficient attention to women of colour by providing
a more appropriately complex and nuanced analysis
that incorporated attention to other social-demographic
characteristics and the relations of inequality associated
with them alongside gender relations (Collins,
1991; Mohanty, 1991). The main premise that is pertinent
here is that any particular form of inequality or
oppression is modified by its interactions with other
forms of inequality or oppression, so that an exploration
of lesbian and gay experiences of primary care
requires a consideration of the intersections of sex,
race, class and occupation, together with sexuality.
Intersectionality provided the basis for a multimethod
approach based on a literature review; interviews with
stakeholders; focus group discussions; distribution
of a survey in the wider LGBT population in the
borough; analysis and writing up of the findings.
The literature review
The review of appropriate literature at local, national
and international level focused particularly on themes such as coming out, definitions of family and access to
primary care.
Interviews with stakeholders
Semi-structured interviews with six key stakeholders
helped set the agenda and assisted in the formulation
of the topic guide for the focus groups and the items
included in the questionnaire used with the wider
population group. These interviews were undertaken
with two service users, two stakeholders in the local
lesbian, gay, bisexual and transgender (LGBT) community
and voluntary sector in the borough and two
stakeholders in the statutory sector. One direct outcome
of these interviews was the agreement that,
because of the mobility of this population group and
the impact that stigma can have on individuals’
willingness to access local services, the opportunity
to participate in the research would be open to people who lived, worked, studied or socialised in the
borough.
Focus group discussions
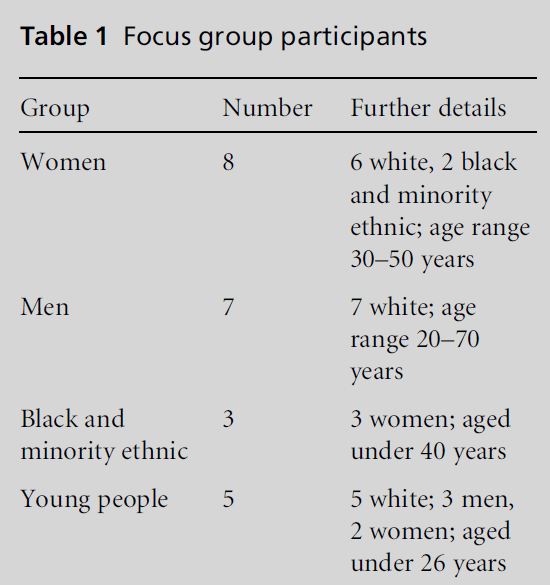
Focus group discussions were held with four subgroups
from within the larger LGBT population. The
target groups were lesbian and bisexual women; gay
and bisexual men; lesbians, gay men and bisexual
people from black and minority ethnic communities;
and young lesbian, gay and bisexual people (see Table
1). While it was agreed that the prime focus of the
research was lesbians and gay men, it was acknowledged
that some people who attended the focus
groups might also identify themselves as bisexual or
in other diverse ways. There was debate about the
organisation of sessions for groups such as people with
disabilities or asylum seekers and refugees, but questions
of resources and the perceived strength of
particular social networks resulted in a decision to
limit the groups to the above four. The topics covered
were: sources of general advice and support that might
impact upon health; finding a GP; relations with
primary healthcare team in relation to coming out;
mental health; sexual health.
Participants for the focus groups were recruited
through lesbian and gay community channels, particularly
the networks linked to thecommunity organisation
that commissioned the research. An information
sheet was made available to all potential participants,
emphasising issues of anonymity and confidentiality.
Participants were advised at the beginning of each
focus group that they could withdraw at any point
without giving any reason. The focus groupswere held
in the premises of the commissioning organisation. The facilitators shared an attachment to the population
group of each focus group insofar as the women’s
group was facilitated by a woman, the men’s group by
a man, the black and minority ethnic group by a
member of a minority ethnic group and the young
people’s group by a young person.
Table 1: Focus group participants
The survey
A questionnaire asking respondents about their views
of general practice was distributed in hard copy format
through lesbian and gay community channels such as
community mailing lists and commercial venues. It
covered topics such as preferred sources of advice in
relation to general health problems, mental health,
sexual health, gay-friendliness of current general
practice, identification of types of people to whom
respondents had come out about their sexuality. An
information sheet was made available with each questionnaire
distributed. While the forms were completed
anonymously, respondents provided information on
sexuality, gender, ethnicity, disability, age, refugee/
asylum-seeker status, postcode and relationship with
the borough in the study. Approximately 250questionnaires
were distributed and 42 were returned by
post. The informants reflected the diversity of the
borough inasmuch as, for example, they identified
themselves as coming from eight ethnic backgrounds,
23.3% (n = 42) considered themselves to have a
disability, and their ages ranged from 16 to 65 years
and over. Fuller demographic details are available in
Cant and Taket (2004). There were no incentives for
completion of the questionnaires. The response rate
achieved is reasonable considering the mode of distribution
of the questionnaire and the limited time
frame of six weeks available for response.
Data analysis
Staff from the research team at LSBU were responsible
for the analytical process. The tapes of the focus group
interviews were listened to repeatedly, and partially
transcribed with a view to identifying further emergent
themes towards the development of a grounded
theory (Strauss and Corbin, 1990); likewise themes
were identified from reading the data gathered from
the questionnaires. This particular research study was
influenced by the work of Charmaz (1990), who
argued that grounded research is threefold insofar as
it requires researchers to ‘attend closely to the data
(which amounts to ‘‘discoveries’’ for them) ... [to build]
their theoretical analyses directly on their interpretations
of processes within those data ... [and to]
compare their analyses with the extant literature and
theory’ (Charmaz, 1990, p. 1165). This grounded theory
approach enables the researchers to draw upon ‘general perspectives of their disciplines, their own philosophical,
theoretical, substantive, and methodological proclivities,
their particular research interests’ (Charmaz,
1990, p. 1170). In this particular study, the researchers
drew upon the theory of intersectionality as well as
writings on primary care and on coming out. The data
from each tape were analysed by the facilitator of that
particular group and one other member of the team.
The themes that structured the topic guide, produced
as a result of the stakeholder interviews, also informed
the analysis. This iterative process facilitated the
development of a grounded theory insofar as scrutiny
of and engagement with the data informed the formulation
of the theory, through identification and use
of emergent themes. The themes identified by these
processes shaped the overall analysis and the writing
up of the research.
Key themes arising fromanalysis of the focus group
discussions and questionnaires were finding a GP and
coming out, sexual health issues, mental health issues
and communication with the GP and other members
of the primary healthcare team. These are discussed in
turn below.
Findings
Finding a GP and coming out in the
general practice setting
All the focus group participants were registered with a
GP. Some had been registered with the same practice
all their lives and some had registered with the one
geographically nearest to them. Those who had sought
to find a practice that was LGBT friendly and thus
sensitive to their personal and social circumstances had
found that personal recommendations were particularly
helpful.One woman informant had asked an official
NHS body about gay-friendly practices in the area:
‘to be told that ‘‘all GP practices are gay friendly’’ – I was
then told by law they had to be. Then they said: ‘‘I suppose
it’s an HIV issue’’. I then went: ‘‘No, this is actually for me
and I’m a lesbian’’ and they said: ‘‘Whoops, I shouldn’t
have said that’’.’
There was nothing to suggest that this staff member,
whose responsibility was information provision, had
ever received training to assist her to be culturally
sensitive to the needs and expectations of lesbian and
gay patients.
Twenty of the 42 questionnaire informants had
come out as lesbian, gay or bisexual to their GPs; a
further four had come out to other members of staff at
the practice where they were registered; in total, 24 had
come out to members of their primary healthcare team.
This can be contrasted with the fact that 29 informants had come out to their employers, even though they had
powers of hiring and firing; these data were gathered
before the introduction of legislation outlawing discrimination
on grounds of sexual orientation in
December 2003. Thirty informants had come out to their
parents. It can be seen that this group of informants was
predisposed to be honest about their sexuality in circumstances
where there might be untoward consequences.
Despite this, a lower number had come out to
members of their primary healthcare team than had
come out to their employers or their parents. Females
were faced with a situation where many felt forced to
come out as a result of the way initial registration with
practices was structured in relation to sexual health.
This issue is also relevant in the discussion of communication
further below.
Sexual health
There was a strong, marked contrast between the
experiences of men and women focus group informants
in relation to sexual health issues in general practice.
None of the men reported ever having discussed sexual
health with their GPs.Most of them were aware of the
benefits of taking preventative measures to secure
good sexual health and attended genito-urinarymedical
(GUM) clinics of their choice. One reported his experience
of continuity of care at one such clinic.
‘I’ve actually had the same nurse at the GUM clinic for
probably five years – I feel completely free to talk to him
about anything – he’s a straight bloke and I have a better
relationship with him than with any GP.’ (Male informant)
Women’s experiences were very different. Sexual health
came onto the agenda as soon as they tried to register
with a practice. Some practices required women to
have a cervical smear test or proof of a test before they
could register with the practice. Not only was an
invasive procedure to be carried out on their initial
contact with the practice, but they also found that the
questions they were asked were insensitive to their
experiences. For example:
‘During a smear, they were asking just really inappropriate
questions – ‘‘are you having sex?’’ – yes – ‘‘are you
worried about getting pregnant?’’ – no – ‘‘why not?’’ –my
partner’s a woman – ‘‘oh’’ [with reported shock].’ (Female
informant)
The apparent lack of any protocols to engage with
lesbian and gay lifestyles suggests that, far from being a
specific problem with the knowledge base of individual
nurses, this was an institutional problem. General
practice procedures made lesbians invisible in terms of
sexual health, and required the patient not only to
come out at a time not of her choosing, but also
to assume an educational role about her healthcare needs. Gay lifestyles were made invisible differently
insofar as there was no structured opportunity for gay
men to come out if they wished. The design of the
information systems and the categories offered for
recording information were not inclusive of nonheterosexual
identities; this posed difficulties at the
time of first registering with a new practice, as well as
in later consultations.
Mental health
Mental health issues were raised as a matter of concern
by several focus group informants, many ofwhomalso
expressed concern about the reaction they would have
received if they had raised them in the general practice
setting. Both women and men had referred themselves
to lesbian, gay and bisexual counselling projects, but
there was no evidence to suggest that any GP had
referred them to such projects. Nor was there any
evidence that any referrals had been made to services
that deal with the psychological consequences of being
a victim of hate crime, although there was a wellestablished
local agency that was particularly sensitive
to lesbian and gay hate crime victims.
A participant in the black and minority ethnic focus
group highlighted her view that lesbian and gay
patients do not only present mental health issues
relating to their experiences of sexuality:
‘I would discuss mental health withmy doctor but I would
be very careful because, as a black person, I think they’re
just too quick to box you.’ (Female informant)
She was aware of the debate about the relatively high
level of African-Caribbean people being diagnosed
with illnesses such as schizophrenia (Mackenzie and
Murray, 1999); she was concerned that inappropriate
referrals to psychiatrists would not only fail to address
her emotional problems but could also result in her
being pathologised.
Communication with the GP and
other members of the primary
healthcare team
Communication between GPs and patients was
understood as being very significant, and while good
communication was welcomed and appreciated, poor
communication and the expectation of poor communications
were identified as major barriers. For
focus group informants. effective communication was
particularly appreciated in relation to the process of
coming out as lesbian or gay. For instance:
‘I was very depressed – and my GP raised the issue of my
sexuality – I was married at the time and in a complete
state of denial – and then the penny dropped and I could
talk to him – not very comfortably at first – but he supported me through the separation and divorce as well.’
(Male informant)
‘My GP gave me help without me even asking for it – she
was helpful – said I was her first gay patient.’ (Female
informant)
Both of these patients had already been with their
practice for some time when the issue of sexuality was
raised, and the fact that there was already a therapeutic
relationship may have assisted the doctors to treat the
problems connected with sexuality as part of the
patient’s personal identity rather than its single defining
feature. Several informants referred to the value of
GPs asking questions of patients rather than making
assumptions about them in the course of a hurried
appointment. For instance:
The behaviour of the individual GP was not regarded
as being the central barrier here, but the unequal
power balance between doctor and patient was seen
as problematic. If the doctor took the initiative and
asked the first question, this was perceived by several
informants as being encouraging and empowering.
Such initiatives assisted lesbian and gay patients to
articulate the whole of the narrative surrounding their
health problem and assisted the GPs to make appropriate
diagnoses and referrals.
Concerns were expressed about the difficulties of
lesbians and gay men, who had migrated to London,
talking about the health implications of their new
lifestyle with GPs and other members of the primary
healthcare team. The majority of the meeting places
for young lesbians and gay men are commercially run
venues where smoking and the consumption of alcohol
and other drugs are pervasive. This poses problems
for these new migrants. They are unsure about how to
negotiate a personal solution for themselves between
the extremes of social isolation or socialising in relatively
unhealthy environments. One young man explained
his thoughts on his experiences:
‘When you do move to London, if you haven’t got a
support network already – you have to find some support
and if you find that in a certain group that quite routinely
drinks a lot and smokes a lot, then you do it. You go on the
scene because, perhaps, you don’t talk to your family and
your confidence is at an all-time low. I was really skinny – I
was just like not eating – and they would say ‘‘Oh, you
need to put on some weight’’ and I would say that I just
wasn’t hungry – it was a whole mental health issue to do
with coming out – but I wouldn’t tell the GP – they might
not realise the pressure you’re under – it’s a physical thing
linked to mental health.’ (Male informant)
There was no continuity of care context to this
particular doctor–patient relationship and the doctor
had not developed any way of interacting with this
patient so as to enable him to tell the narrative of his
current life in London. The patient’s fear of being
stigmatised or rejected meant that he lacked the confidence
to come out and share the narrative around the
development of his sexuality; he found the advice from
this particular GP less than useful.
Other informants told narratives of their experiences
with GPs which illustrated the difficulties of
establishing a trusting relationship with a new GP.
One woman reported how ‘lesbian mother’ had been
written across her child’s health records in relation to
consultation on an unconnected issue. Several men
were unsure about the impact that information about
their sexuality would have on applications for mortgages
and insurance. One informant reported that in
a group practice, a doctor whom he had never met
provided details about his sexuality to an insurance
company, which made a false assumption about his
HIV status and increased his premium. The differing
interpretations of confidentiality and the value systems
of some health practitioners had contributed to
patients being fearful about trusting their GPs with
information about their sexuality.
The findings from the focus group informants were
reinforced by the questionnaire informants. They
were asked to identify examples of their own negative
experiences with the practice where they were registered.
Eight informants (19%) specifically said that
they were able to identify no examples of negative
experiences. From the remaining informants, issues
relating to communication were the most common
among the negative experiences cited. Several GPs and
other practice staff were criticised for making assumptions
about heterosexuality and being insensitive to
those informants who came out about their sexuality.
Staff behaviour was described as having been ‘defensive’,
‘judgemental’, ‘patronising’, ‘rude’ or ‘uncomfortable’.
Lack of respect had been shown to informants
who came out, and this had manifested itself in
inappropriate remarks about a male informant’s ‘effeminate’
behaviour, intrusive and irrelevant questions
about sexual activity, regular usage of the prefix ‘Mrs’
to an openly declared lesbian and the lack of inclusion
of an informant’s partner. Judgemental and physically
rough treatment was mentioned by one informant in
relation to her treatment by GPs whose religious
beliefs were used to justify disapproval of her lesbian
lifestyle. Health promotion advice was provided without
any acknowledgement of the social context in
which informants were living their lives. Four informants
reported that diagnoses and treatment decisions
were made without any explanations; one man had
been sent to a hospital for an HIV testwithout discussion or explanation. The repeated offers of contraception
were resented by a number of women whose coming
out seemed not to have been acknowledged by practice
staff.
Discussion
Many of the key themes presented here related to the
mode of organisation of the practice. Of particular
significance was the perceived lack of protocols to
respond to the diversity of the local population, heterosexual
assumptions, communication and accessing other
sources of healthcare. The issue of protocols is not a
request for special treatment for a minority, but reflects
the need for innovative approaches to the recording
and sharing of personal histories in practices where
there are diverse patient backgrounds. Continuity of
care is a pressing issue for such a highly mobile population
(Kelley et al, 1997; Valentine, 1999). Lesbians and
gay men are particularly likely to move accommodation
frequently and so there is less opportunity for
them to develop ongoing relationships with their
healthcare practitioners and for the practitioners to
build an in-depth knowledge of their patients’ personal
health histories. This highlights the role that
protocols could have in facilitating the sharing of
knowledge between patients and practitioners.
The approach of practices towards sexual health
was identified by many informants as both problematic
and reflective of heterosexual assumptions. There
was a clear gender differentiation in that women were
subjected to insensitive procedures before registration,
whereas men were unlikely to encounter issues of
sexual health at all. Neither with women nor with
men could the behaviour of general practice be said to
be patient centred or inclusive of diversity of need.
Communication was a key factor in determining
individuals’ level of satisfaction with service providers
and this was seen as being more problematic with the
GP services than with alternative healthcare providers.
There was concern that sexuality was likely to be
pathologised by GPs, and this frequently inhibited
people from being as open with them as they were, for
example, with their families. The process of pathologising
sexuality can prevent practitioners from understanding
the significance of particular attachments and
affiliations within lesbian and gay population groups.
Many GPs were perceived as relying on heterosexual
assumptions. While it was acknowledged that some
individual practitioners had been friendly and supportive
to individual patients, there was no evidence
to suggest that any of them had developed systems
such as protocols for recording information about
sexuality and lifestyles in ways which their patients might deem to be appropriate and respectful (Miller
and Weingarten, 2005).
The fact that many informants acknowledged that
they accessed alternative sources of healthcare such as
aromatherapy, counselling and internet support chatrooms
as well as lesbian-/gay-friendly sexual health
clinics indicates that the informants were concerned
to promote and maintain their health and wellbeing.
None was, however, totally reliant on these other
sources and it was our perception that they expected
their primary care services to be as holistic in their
approach as their other providers.
Conclusions and recommendations
The widespread perception that lesbian and gay
healthcare needs were invisible within the context of
general practice indicates the need for action on
several different levels. To clarify the extent of the
problem it would be useful, initially, for practices to
audit the frequency with which lesbian- and gayrelated
concerns are raised with practitioners; it would
also be appropriate for primary care trusts to establish
small grants schemes that could support both individual
and collective attempts at advocacy. These steps
could begin to generate debate and give pointers
towards the prioritisation of particular research-related
tasks and projects. As this process develops, opportunities
should be taken to develop partnerships
between the PCT and other community bodies, including
lesbian and gay organisations, to monitor
progress and identify future steps in the development
of healthcare practice which is more inclusive of the
needs and aspirations of the lesbian and gay populations.
These steps will also provide a framework within
which it will be possible to conduct research on the
healthcare implications of a number of dimensions of
lesbian and gay experiences such as hate crime, sexual
health and social isolation. By making the social experiences
the starting point of this process, there will be
opportunities to review and question the medical
assumptions about lesbian and gay healthcare needs
and to promote the development of more inclusive
models of practice.
One specific healthcare issue which can be addressed
within this context is the policy, or rather the lack of
policy, of general practice towards the sexual health
concerns of lesbians and gay men. This plays out
differently for lesbians and gay men. Gender distinction
within current practice leaves gay men to their
own devices and forces women to engage in procedures
at times and in ways that are not of their
own choosing. Both approaches imply an attitude of
neglect towards this significant area of health and
neither of them encourages patients to integrate their sexual health concerns into their overall healthcare
agenda. That an intersectional framework was of value
can be seen most clearly in two particular areas: how
the heterosexist assumptions and systems in relation
to sexual health operated with quite different effects
for lesbians and gay men, and how concerns around
mental health resulted in rather different presentations
of self for black lesbians and gay men in comparison to
those who were white.
This study engaged with the experiences of a diverse
sample of lesbians and gay men and, in so doing,
revealed the complexity of needs that this population
group brings to general practice. As general practice
seeks to engage and communicate more effectively
with its service users/patients, this study urges disavowal
of assumptions of heterosexuality and calls for
further research into the links between the diversity of
lesbian and gay population groups and their healthcare
needs.
ACKNOWLEDGEMENTS
The authors would like to thank Troy Fairclough and
Lisa Danquah for jointly facilitating the focus groups
for young people and people fromblack and minority
ethnic backgrounds; Troy Fairclough also took part in
the analysis of the findings of these group discussions.
The advice of the anonymous reviewers is much
appreciated. We would also like to thank the informants
for sharing their experiences with us.
CONFLICTS OF INTEREST
None.
References
- Bains A and Cross E (1997) Primary Health Care and Gay and Bisexual Men. Sheffield: Sheffield Centre for HIV and Sexual Health.
- Bakker FC, Sandfort TGM, Vanwesenbeeck I, van Lindert H and Westert GP (2006) Do homosexual persons use health services more frequently than heterosexual persons: findings from a Dutch population survey. Social Science and Medicine 63:2022–30
- Britten N and Fisher B (1993) Qualitative research and general practice. British Journal of General Practice 43: 270–71.
- Cant B (2002) An exploration of the views of gay and bisexual men in one London borough of both their primary care needs and the development of primary care practitioners. Primary Health Care Research and Development 3:124–30.
- Cant B and Taket A (2004) Exploring Marginalised Communities’ Access to General Practice Services in Primary Care in Waltham Forest – Lesbians and Gay Men. London: London South Bank University and East London Out Project. (Available from the authors at cantr@lsbu.ac.uk)
- Charmaz K (1990) Discovering’ chronic illness: using grounded theory. Social Science and Medicine 30:1161–72.
- Collins PH (1991) Black Feminist Thought: knowledge, consciousness and the politics of empowerment. New York: Routledge.
- Cresswell JW (2003) Research Design: qualitative, quantitative and mixed method. London: Sage.
- Department of Trade and Industry (DTI) Women and Equality Unit (2003) Civil Partnership: a framework for the legal recognition of same sex couples. London: Department of Trade and Industry.
- European Academy of Teachers in General Practice (2002) https://euract.org.html/
- Fish J (2006) Heterosexism in Health and Social Care. Basingstoke: Palgrave Macmillan.
- Heaphy B, Yip A and Thompson D (2003) Lesbian, Gay and Bisexual Lives Over 50. Nottingham: York House.
- Hinchliff S, Gott M and Galena E (2005) ‘I daresay I might find it embarrassing’: general practitioners’ perspectives on discussing sexual health issues with lesbian and gay patients. Health and Social Care in the Community 13:345–53.
- Kelley P, Pebody R and Scott P (1997) How Far Will You Go?: A survey of London gay men’s migration and mobility. London: GMFA.
- King M and McKeown E (2003) Mental Health and Social Wellbeing of Gay Men, Lesbians and Bisexuals in England and Wales. London: MIND.
- McFarlane L (1998) Diagnosis Homophobic: the experiences of lesbians, gay men and bisexuals in mental health services. London: PACE.
- McKenzie K and Murray RM (1999) Risk factors for psychosis in the UK African-Caribbean population. In: BhugraDandBahl V (eds) Ethnicity: an agenda for mental health. London: Department of Health, pp. 48–59.
- Miller N and Weingarten L (2005) Creating GLBTQIAInclusive Forms: suggestions for policy and implementation. https://sugroups.wustl.edu/~safezones/GLBTQIA.forms. pdf (accessed 9 December 2006).
- Mohanty CT (1991) Under Western eyes: feminist scholarship and colonial discourses. In: Mohanty CT, Russo A and Torres L (eds) Third World Women and the Politics of Feminism. Birmingham: Indiana University Press, pp. 61– 88.
- Office of National Statistics (ONS) (2003) UK 2001 Census Data. London: ONS, www.statistics.gov.uk/census (accessed 9 December 2006).
- Phillips J and Marks G (2006) Coming out, coming in: how do dominant discourses around aged care facilities take into account the identities and need of ageing lesbians? Gay and Lesbian Issues and Psychology Review 2(2):67–77.
- Plummer K (1995) Telling Sexual Stories: power, change and social worlds. London: Routledge. Royal College of General Practitioners (RCGP) (2002) The RCGP – UK Council, The European Definition of General Practice/Family Medicine. www.rcgp.org.uk/corporate/ council/european_Definition_GP.asp (accessed 9 December 2006).
- Saddul RB (1996) Coming out: an overlooked concept. Clinical Nurse Specialist 10:2–5, 56.
- Schilder AJ, Kennedy C, Goldstone IL et al (2001) ‘Being dealt with as a whole person’. Care seeking and adherence: the benefits of culturally competent care. Social Science and Medicine 52:1643–59.
- ShankleMD(ed) (2006) Handbook of Lesbian, Gay, Bisexual and Transgender Public Health: a practitioners’ guide to services. Washington DC: APHA.
- Silvestre AJ (ed) (2006) Lesbian, Gay, Bisexual and Transgender Health Issues. Washington DC: APHA.
- Sloop JM (2005) In a queer time and place and race: instersectionality comes of age. Quarterly Journal of Speech 91:312–26.
- Strauss A and Corbin J (1990) Basics of Qualitative Research: grounded theory procedures and techniques. London: Sage.
- Taylor B (1999) ‘Coming out’ as a life transition: homosexual identity formation and its implications for health care practice. Journal of Advanced Nursing 20:560–6.
- Valentine G (1999) From Nowhere to Everywhere: lesbian geographies. Binghamtown: Harrington Park Press.
- Westersta°hl AU and Bjo¨rkelund A (2003) Challenging heteronormativity in the consultation: a focus group study among general practitioners. Scandinavian Journal of Primary Health Care 21:205–8.