Research Paper - (2010) Volume 18, Issue 1
Researcher, School of Occupational Therapy and Social Work, Faculty of Health Sciences, Curtin University of Technology, Perth, WA, Australia
Angela Fielding BA BSocWk PhD*
Senior Lecturer, Head of Social Work, School of Occupational Therapy and Social Work, Faculty of Health Sciences, Curtin University of Technology, Perth, WA, Australia
Received date: 31 August 2009; Accepted date: 25 November 2009
Background Effective delivery of health care is dependent on health manpower. In Thailand, an insufficiency of human resources relates to an inequitable distribution of healthcare professionals rather than to insufficiencies overall. Both internal and external factors influence healthcare professionals’ choice of where to work, although perceptions rather than actual circumstances are more influential in their decision-making process. This inequitable distribution of healthcare professionals in Thailand affects rural areas and the provision of primary health care.Objectives To understand the subjective perceptions, attitudes and dynamics among healthcare professionals regarding where they seek employment and the impact on the provision of primary care. DesignQuestionnaire survey among Thai healthcare students and professionals and semi-structured interviews with healthcare professionals investigating attitudes and perceptions. Setting Thai rural, urban and metropolitan areas. ResultsAn interesting mix of factors influences healthcare professionals with regard to where they seek employment, or continue their employment. Family and community commitments, social status and a sense of belonging were associated with healthcare professionals seeking employment in their province of origin. Tensions are also emerging between preventative and curative health. These tensions, together with financial remuneration and professional development opportunities and promotions, as perceived by healthcare professionals themselves, have implications for current and future healthcare policy.Conclusion The scaling up of human resources for health in Thailand will not, based on past experiencesand attitudes outlined in this research, ensure an equitable distribution of healthcare professionals. Further consideration of these professionals’ expectations of being able to work in areas close to their families and of sufficient financial remuneration is required. It is likely that rural regions and the delivery of primary care will be negatively affected by continued inequities. It was also found that current healthcare policies are creating new tensions.
attitude of health personnel, health manpower, health policy, Thailand
Thailand has a good fundamental healthcare infra-structure with hospitals in all of the country’s 76 prov-inces[1] (between 1200 and 1300 hospitals in total)[2,3] and 70 institutions training and educating healthcare professionals, including 17 medical schools.[3] While there have been historical internal inequities in the distribution of healthcare professionals[4–6] and signifi-cant emigration of physicians during the 1960s and 1970s,[5–9] measures including the introduction of com-pulsory public service for physicians ensured a more equitable distribution of physicians, particularly dur-ing the following decades.[5–7] This enabled the devel-opment of the rural healthcare sector and a focus on primary care. Primary care refers to the point of entry into the healthcare system and will ideally combine ‘the preventative and curative’.[10] In many healthcare systems this takes place outside the hospital system. In Thailand, primary care is often administered by the local hospital although outreach services by healthcare teams are common, particularly in rural areas. There were only 300 physicians in the rural sector in 1976. This number increased fourfold by 1985 when 1162 physicians were working in rural hospitals.[5] However, Thailand’s economic development, which by 1995 had doubled in a decade,[11] saw the growth of the private healthcare sector, leading to the re-emergence of in-equities in human resources for health.[5,6,9,12,13] Prior to the Asian financial crisis in 1997, 21 rural district hospitals did not have a single full-time physician among their staff[9] and it was estimated that only 1874 physicians were working at rural district hospitals in May 1998, in contrast to the 3161 required phys-icians.[7]
The concern about the stock and distribution of human resources for health is worldwide.[7,14] This is not limited to physicians – concern about nurses has also been noted. It has been noted that around the peak of the exodus of Thai physicians during the 1960s and 1970s Thai nurses also emigrated, although in contrast to the physicians these nurses tended to return to Thailand after working overseas.[8] The turn of the century saw a renewed increase in the emigration of nurses from Thailand.[15] Projections of the future stock of various healthcare professionals in Thailand has taken place during previous decades[16,17] and the latest estimates indicate that the healthcare system will have sufficient numbers of healthcare professionals with regard to physicians,[18] nurses,[19] dental personnel,[20] dentists,[21] pharmacists and pharmaceutical techni-cians[22] and mobile emergency technicians[23] as a result of increases in the education and training of health per-sonnel. However, these estimates cannot ensure an equitable distribution of these professionals. Increases introduced in 2004 in the numbers of Thai medical doctors being trained are expected to decrease the population–physician rate from 15 to 30% to 3% by 2020, according to Sirikanokwilai et al.[18] Although they have recognised that the improved population–phys-ician rate will not necessarily rectify the inequitable distribution of physicians, this projection has not incorporated the increased strains on the public health-care sector as a result of the newly introduced universal healthcare system and the subsequent increased de-mand for healthcare services.[4] These internal inequities are of concern, where rural district hospitals have historically suffered from a lack of physicians. Fur-thermore, as appears to be the case for professional nurses in Thailand, many qualified healthcare profes-sionals do not continue to work in their field; figures for 2002 suggest that only between two-thirds and four-fifths of qualified nurses are actually working within their profession.[4]
This paper draws on one aspect of a larger research project[4] which used a mixed methods approach to highlight attitudes and perceptions among healthcare professionals. It is proposed that attitudes are more influential than actual circumstances when individ-uals contemplate migration, and the decision to mi-grate may not be completely rational.[24] Working with key informants and snowball sampling, 93 healthcare students and professionals working or studying in the Bangkok metropolitan area or in the Northern prov-inces completed a questionnaire for the first phase of the research project in late 2005. Participants were asked to rank 39 statements on a five-point Likert scale. The questionnaire also included one open ques-tion and sought demographic data.
The second phase of the research project, from late 2005 to early 2007, consisted of semi-structured in-terviews with 33 healthcare professionals with ques-tions covering attitudes towards working in rural and urban areas and in the public and private sectors, as well as attitudes towards international migration. The interviewees were approached through key informants and through snowball sampling. The quantitative re-sponses from the questionnaires were analysed utilising SPSS and the interviews were analysed thematically. Participants for the semi-structured interviews, in particular, were sought as key informants to represent backgrounds as diverse as possible, including their professional background and geographical location. Demographic and professional characteristics of the research participants are outlined in Tables 1 and 2. This paper presents the attitudes of these participants with regard to the interrelated variables influencing their decisions to work in rural or urban areas. These attitudes should be taken into consideration when evaluating the effects of recent healthcare reform.
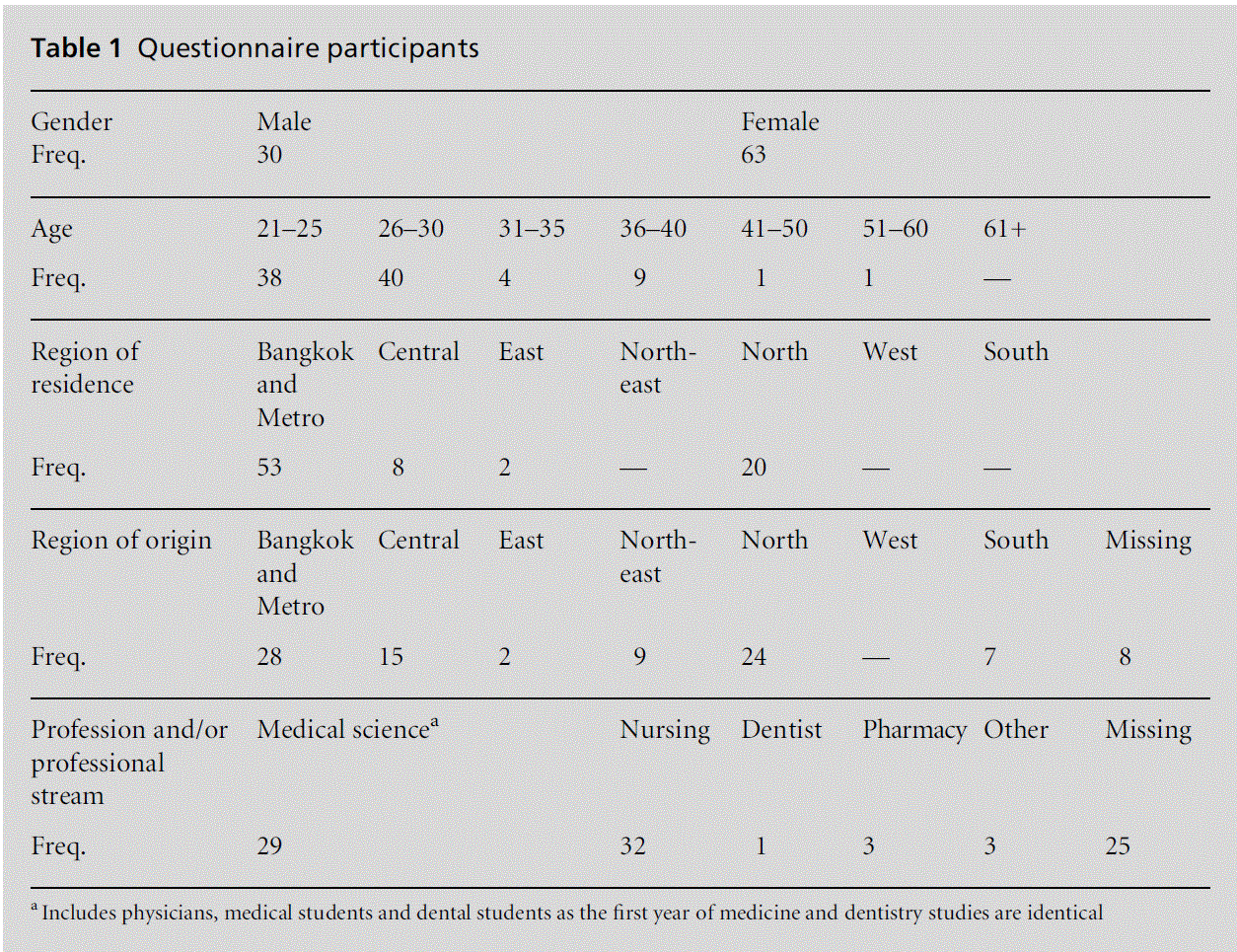
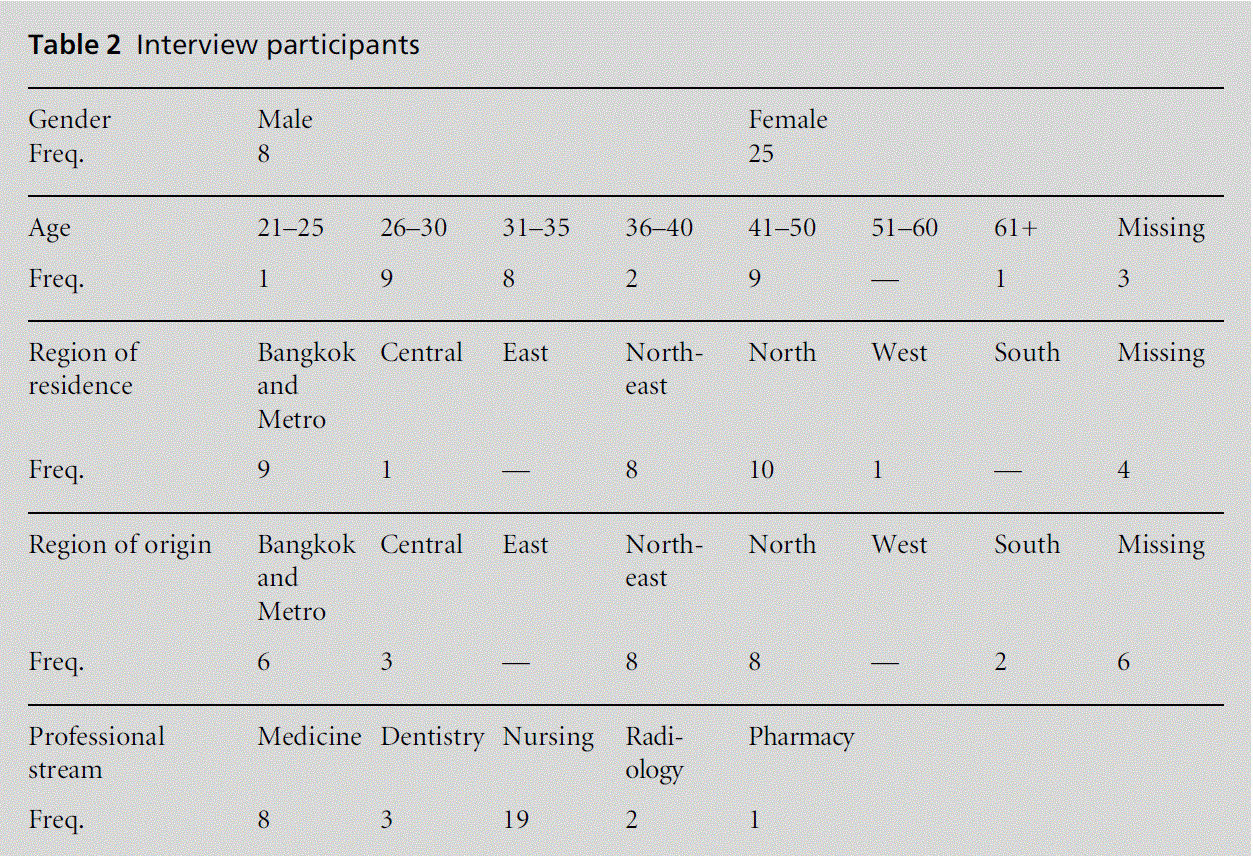
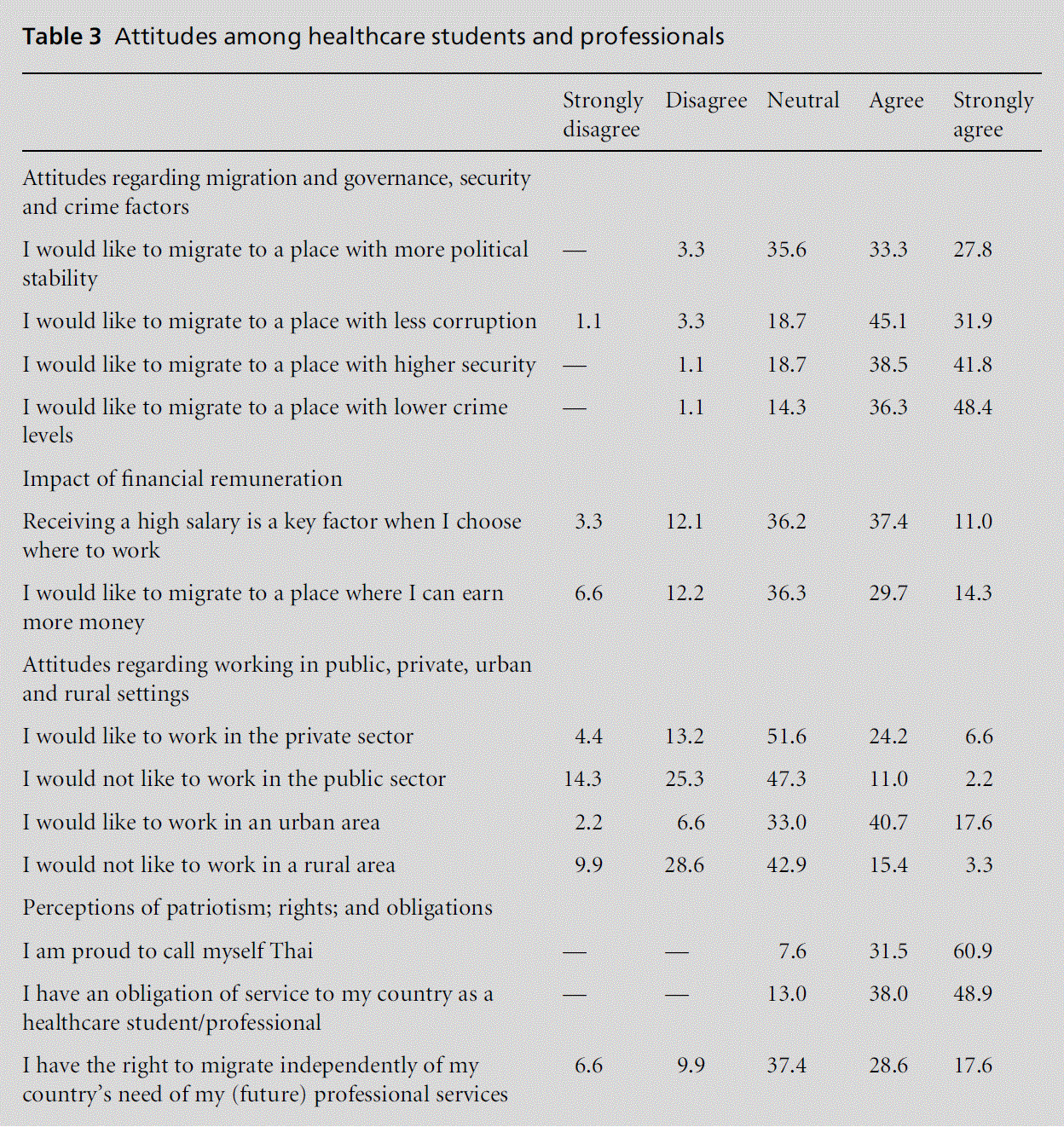
The questionnaire survey indicated an overall desire among these healthcare students and professionals to migrate because of social, political, security and governance factors. Financial remuneration and work-ing in the private sector were of lower significance, as outlined in Table 3. There appeared to be a pull towards urban areas but no significant push from rural areas in this sample. The dichotomies related to working in rural and urban areas are interrelated with other factors. The level of patriotism reflected among the question-naire participants should be noted, and their strong sense of civic obligation to serve the healthcare needs of the general population, which could be interpreted in their perception as triumphing over their individual right to emigrate. This attitude can be linked to an underlying social contract between healthcare pro-fessionals and the general population in Thailand, where these professionals, through their professional contributions and personal sacrifices, obtain high social status, independent of professional status, within their communities, which mitigates sentiments of dissatis-faction over their working conditions, workloads and financial remuneration.[4]
Attitudes towards healthcare consumption
The semi-structured interviews revealed that a propor-tion of the participants working in the public sector felt resentment towards the government and the general population regarding inappropriate healthcare con-sumption. Healthcare professionals in the public sector, independent of working in rural, urban, or metro-politan areas, indicated significant increases in patients and workloads. A common characteristic described by the interviewees was a 50–100% increase in outpatients following the introduction of a universal healthcare scheme in 2001. This policy was introduced to redress the increased lack of affordability and deficiencies, and was referred to as the 30-baht health cover, as it initially required a flat co-payment of 30 baht (equivalent to US$0.70–0.80), which was later abolished.[17,25–28] This Universal healthcare cover was introduced on a popu-list platform, but also based on a real need for new health policies. Prior to this policy, 30% of the population did not have any health cover while the remaining 70% did not necessarily have full cover.[17,26] While interviewees from the rural district hospitals to the central urban, metropolitan and university hospitals alike reported increases in workloads and number of patients, it is unclear whether the impact on the public hospitals is uniform. The interviewees indicated that the rural district hospitals experienced up to a doubling of out-patients, while other reports suggest that university hospitals providing tertiary health care, or ‘highly specialised services’,[10] exceeded their budgets due to the disproportionate increases in patients requiring complex treatments and costly procedures.[29]
Workloads
Staff at a rural district hospital in Northern Thailand disclosed that they currently had two physicians. There had been a third physician employed previously, but he resigned and opened a private clinic as a result of the increased workload following the introduction of the universal healthcare scheme. They indicated that this policy had led to an increase in the daily number of outpatients from between 150 and 200 to between 250 and 300. These increases place incredible strains on healthcare professionals and inhibit the develop-ment of the preventative aspect of primary health care. Pongsupap and Van Lerberghe[30] found that doctors’ consultation times with patients in Thailand averaged 3.8 minutes at public hospitals, 5.7 minutes at private hospitals, 5.9 minutes at private clinics and 6.2 min-utes at family practices. The increases in outpatients at this particular hospital would increase workloads based on the average consultation time of 3.8 minutes from between 4.75 and 6.33 hours to between 8 and 9.5 hours. These workloads exclude both the additional administration tasks and looking after patients in the hospital’s wards and divert attention and resources from the preventative aspects of primary health care.
The physician who recently resigned from this hospi-tal was disillusioned with the new healthcare policy, exclaiming that ‘it sucks’. While the other interviewees were more restrained, most healthcare professionals working in the public sector, particularly in rural areas, were concerned, and were experiencing increased work-loads. Prior to the universal healthcare scheme, full-time staff would work 20 days a month and could expect an additional four to five shifts. The increased workloads required staff to work ten or even 15 add-itional shifts a month; requiring them to do double shifts and leaving them very few, if any, days off.
Strengthening primary health care
It was reported that patients were seeking medical treatment with the onset of any symptoms: a slight cough; the common cold; and even what the nursing staff believed to be fatigue and tired muscles from manual labour, requiring rest and not medical treat-ment. It was also noted by a nurse working at a rural district hospital that patients requested medications prior to the doctors’ consultations, or even asked for additional medical tests, like X-rays, ultrasounds or
computerised tomography scans (CT or CAT scans). While such requests may be reasonable and reflect diligence, several of the interviewed healthcare pro-fessionals believed that patients were capitalising on the free healthcare policy rather than seeking medical advice and tests when appropriate. It was suggested that these additional services were in some cases demanded as a result of watching popular television shows, without any understanding of what the tests were.
The interviewed healthcare professionals indicated that there appeared to be a shift away from primary and preventive healthcare, both with regard to health policy and among the general population. When asked what healthcare challenges she believed Thailand was facing, a nurse working at an urban public hospital replied that the general public did not have a good general understanding or education regarding their health: What needs to be done is to make everyone understand primary health care and avoid things that will harm their health.
Impact of health policies
Numerous policies are in place to encourage health-care professionals to work in the rural areas of Thailand and ensure a minimum number of healthcare pro-fessionals in the rural district hospitals. These include the three-year mandatory public service for newly graduated physicians,[5–7] and mandatory public sector employment of two to four years for nurses and midwives.[7] However, increasing numbers of newly graduated medical doctors have been exiting the public service and have paid an exit fee. There also appear to be increased opportunities for nurses to migrate overseas.[4] Furthermore, the expanding private health-care sector has created opportunities for healthcare professionals which in turn has created fears of a new internal brain drain, particularly of physicians.[5,6,9] In response to this, new and more generous allowances have been introduced for healthcare professionals work-ing in rural areas, improving the attractiveness of employment in these regions.
Challenges regarding delivering primary health care in rural areas
Acknowledging that many healthcare professionals, particularly nurses, prefer to work in the province in which their family resides, rural recruitment has been attempted, with good results, for nurses, midwives and paramedics, but with mixed results for physicians.[5,7] The entry examinations, particularly for medical doctors, favoured those applying from rural areas. This led to an influx of aspiring physicians to rural areas prior to the entry examinations, although these entrants still considered themselves urban dwellers and would prob-ably return to work in the cities. This attitude, particu-larlyregarding being a ‘Bangkokian’, was reflectedamong the interviewees. Several healthcare professionals, even if working in other regions, still viewed themselves as metropolitans, and would move back when given the opportunity.
While the extra allowances for healthcare profes-sionals working in rural areas have had some effect, they have also created further imbalances in the distrib-ution of healthcare professionals. These extra allow-ances are based on the classification of the respective hospitals, which has created a five- to ten-fold differ-ence in allowances between hospitals which may only be separated by ten or 20 kilometres.[5] It has even been argued that these allowances are creating further tensions, as they differ for different healthcare pro-fessions, and as new graduates are earning more this may enable them to exit the public service sooner.[4] While these extra allowances can be attractive for new graduates, it was indicated by one interviewee that the opportunity for professional development and pro-motion are limited at the most rural hospitals. As such, these measures can temporarily alleviate shortages in health manpower at rural institutions, but may have a limited long-term effect in facilitating the retention of these professionals in rural areas.
Despite the mixed results and inadequacies of these policies, measures can be introduced to maximise the desired effects, for example, by only accepting students into the rural recruitment pools who can document a minimum number of years’ attachment to a local rural area with a shortage of healthcare professionals. It is also necessary to ensure that these healthcare students will be employed within their local communities upon graduation. Adjustment to the allowances at rural hospitals may also be warranted, as may a further increase in the exit fees for those opting out of the compulsory public service.
Tensions between rights and responsibilities
Table 3 indicates that there is a strong sense of obli-gation among these participants to serve the health needs of their fellow citizens. This attitude can be characterised as a social contract, placing high levels of obligation on healthcare professionals who, in return, obtain high social status. This is independent of where the healthcare professional is employed or even of his or her professional status. Low level community health workers and nurses working directly with the general public in rural areas often obtain high social status, despite their relatively low professional status, by working actively for the public good. Some of the interviews, however, indicated that this dynamic may be fading due to the increased emphasis on healthcare consumers’ rights and the introduction of universal health care.
While the interviewees recognised the general public’s right to health care, and did not object to the principle of the universal healthcare policy, many were disillu-sioned with the implementation and ripple effects of the policy. This relates to the attitude towards health-care consumption and the general public seeking medical treatments indiscriminately, as perceived by the interviewees, in an apparent breach of the social contract. This may create resentment among some healthcare professionals, such as the physician cited above who left the rural district hospital, and may push professionals away from the public sector. The policy’s emphasis on treatment and consumers’ rights can also undermine efforts in preventive and primary health care. As a nurse working at a rural district hospital narrated, she would regularly visit small rural com-munities as part of a primary healthcare team, talk with the villagers and promote primary health care, exercise and good diet. Although the team sometimes distributed vitamin supplements, she noted that the villagers would now come and request medications while the team was promoting healthy lifestyles.
Consequences of under-resourcing primary health care
As behaviour and attitude changes in the general population, combined with limited resources, appears to undermine primary healthcare efforts and creates a shift to healthcare consumption, this also has a nega-tive impact on tertiary and more comprehensive care. To be eligible for the universal healthcare scheme patients have to register at a public hospital. While those living in rural areas often only have one hospital at which they can register, there is potential for a dis-proportionate distribution of patients requiring ex-tensive tertiary care at the urban and metropolitan hospitals. The tertiary university hospitals, in particu-lar, have registered increased numbers of patients requiring extensive care, as they register with hospitals that they know provide these services; this has led to some of these hospitals becoming significantly in-debted.[29] Hence, the universal healthcare policy ap-pears to have created a significant surge in healthcare consumption, often inappropriate according to some interviewees, at the expense of both primary and tertiary health care.
The Thai health infrastructure has a sound founda-tion, but internal inequities are of concern. According to the participants in this research project, rural areas do not have sufficient human resources for health, and recent healthcare reform is creating significant add-itional pressure on the healthcare professionals working in these areas. While the initial attitudes and percep-tions outlined by the research participants did not indicate a significant pull towards the private sector or a push from rural areas, the new universal healthcare scheme has created marked changes in the consump-tion of healthcare services. This shift could have a negative impact on the particular traits among Thai healthcare professionals, including attitudes of self-sacrifice and servitude to the general population’s healthcare needs.
The increase in healthcare consumption also ap-pears to deplete the healthcare resources available for the preventative aspect of primary health care. While it is important to address the universal right to health care, these efforts can have adverse ripple effects if efforts are one-sided, do not take into account the needs of all stakeholders, and are based on political populism rather than sound health policy.
This research project was approved by Curtin Univer-sity of Technology’s Human Research Ethics Com-mittee.
Not commissioned; externally peer reviewed.
Conflicts of Interest
None.
The authors would like to thank and acknowledge all the research participants and everyone else who as-sisted with this research project including the referee, whose insightful comments added to the strength of this article.