Research Paper - (2012) Volume 20, Issue 5
Professor, Faculty of Nursing, University of Calgary, Canada, formerly School of Health & Social Care, Bournemouth University, UK
Louise Worswick MSc HDCR DMU
Researcher
Peter M Wilcock BSc Dip Psych MSc PGCert (THE) C Psychol FBPsS FHEA
Visiting Professor, School of Health & Social Care, Bournemouth University, UK
Charles Campion-Smith MBChB (Edin) DCH FRCGP
General Practitioner, Dorchester, UK and Visiting Fellow, School of Health & Social Care, Bournemouth University, UK
Dries Hettinga PhD MSc BSc
Diabetes Fonds, Netherlands, formerly BackCare, UK
Received date: 1 March 2012; Accepted date: 15 July 2012
Introduction Studies exploring the role of patients in interprofessional education (IPE) are found primarily in undergraduate programmes with few reporting on the postgraduate (continuing professional development) setting. This paper describes an interprofessional quality improvement project around the management of back pain in a primary care setting where patients were part of the practice team. Methods Patients participated in eight half-day IPE workshops delivered to nine general practice teams in the UK. Educational content included knowledge about quality improvement and evidencebased back pain knowledge, with teamwork, experiential and didactic learning approaches. On-site practice support from a quality improvement facilitator occurred between the workshops to strengthen practice-based learning. Forty-four practice staff and 11 patients attended the workshops and the facilitated project meetings. Evaluation occurred through focus groups with practice teams (including patients) both before and after the workshops. These were recorded, transcribed and analysed by coding and the inductive development of themes. Results The context of managing back pain was particularly challenging. Focus group participants indicated that patient involvement was highly valued as it gave practitioners a greater understanding of the effects of back pain on their lives whilst permitting patients to hear the experiences of others and to understand their own world better. Listening was important to patients’ experiences of healthcare and practitioners’ experiences of the workshops. Learning together emerged as particularly important and finally the challenge of finding time to learn together infiltrated the entire endeavour and was a prominent concern. Discussion Patients sharing their experience of back pain appeared to be a particularly pivotal point in the learning for practice teams. Meaningful engagement with users in IPE was highly valued and provided a catalyst for behavioural change, where professionals relinquished an unhelpful medicalmodel in favour of an integrative biopsychosocial one.
focus groups, interprofessional edu-cation, patient involvement, practice-based learning, primary care, quality improvement, service-user
How does this fit with quality in primary care
What do we know?
The management of back pain in primary care is generally suboptimal. Quality improvement offers the opportunity for healthcare professionals to learn and work together to redesign care to meet patients’ needs better. Where patients are involved in interprofessional education (IPE), it is generally at the undergraduate level rather than with continuing professional development initiatives.
What does this paper add?
A detailed understanding of the processes used to meaningfully engage patients in a quality improvement project on the management of back pain in primary care. An insight into how patients can make an important contribution to interprofessional learning. By sharing their experiences of back pain, they can shift the perspectives of health professionals towards a biopsychosocial model of care.
In the United Kingdom (UK), the drivers for increased interprofessional working have largely occurred through policy documents[1,2] and the importance of delivering high-quality care with patients at the centre of service design and delivery is consistently highlighted.
Various models have been utilised to facilitate quality improvement in service delivery. The knowl-edge that underpins the ‘Discipline of Improvement’ in health services has four inter-related and equally important domains: systems thinking; initiating and sustaining improvement in daily work; personal and organisational development; and involving patients, carers, staff and the public.[3]
Involvement of patients as members of practice teams designing improvements to care is key to effective service improvement[4,5] and is congruent with the notion of interprofessional learning as part of the improvement process[5] with a key potential benefit of improved communication.[6]
This paper describes the experience of involving patients (who endured chronic back pain) in an interprofessional education (IPE) project. This was part of a larger project in which evidence about back pain management and quality improvement was offered to nine primary care practices through workshops and accompanied by practice support between workshops to undertake improvement projects. An evaluation of patient, professional and practice outcomes was also undertaken.[7]
IPE has been defined by the Centre for the Ad-vancement of Interprofessional Education (CAIPE) as ‘when two or more professions learn with, from and about each other to improve collaboration and the quality of care’.[8] IPE aims to improve care by pro-moting teamwork and strengthening a shared under-standing of roles between professional groups.[9] Involving patients in health professional education has primarily occurred in undergraduate programmes[10–12] with few studies considering their role in continuing pro-fessional development.[13]
Two reviews evaluate the level of involvement of patients and healthcare staff,[11,14] but do not specifi-cally focus on IPE. Although there has been a call for studies articulating the processes of patient involve-ment,[14] none could be identified that considered the role of a patient within the interprofessional team. The aim of this part of the project was to explore and capture the processes and experiences of the practice teams and patients in the interprofessional learning within a quality improvement project.
In our study, patients were people who are currently in receipt of healthcare or not currently receiving healthcare but who may have done in the past and may do in the future.
Design
The project described in this paper is a discrete part of a larger mixed methods study ‘Learning to Improve the Management of Back Pain in the Community’ (LIMBIC, www.limbic.org.uk). The quantitative com-ponent was a matched case-controlled cohort using a ‘before and after’ design and the main outcomes for this study are described elsewhere.[7] This paper focuses on describing the processes of patient engagement and the qualitative component (focus groups) which re-ports the experiences of nine participating practices in two south of England primary care trusts (PCTs) in the UK. Patients joined practice teams at eight work-shops, which ran over nine months, and assisted in practices’ improvement projects with dedicated sup-port from a quality improvement facilitator between workshops.
Evaluation occurred through focus groups with each practice team, including their patient representative;
one before the workshops commenced (late 2007) and one after completion of the workshops (early 2009) following a favourable ethical opinion through the National Health Service Research Ethics Service.
Sample
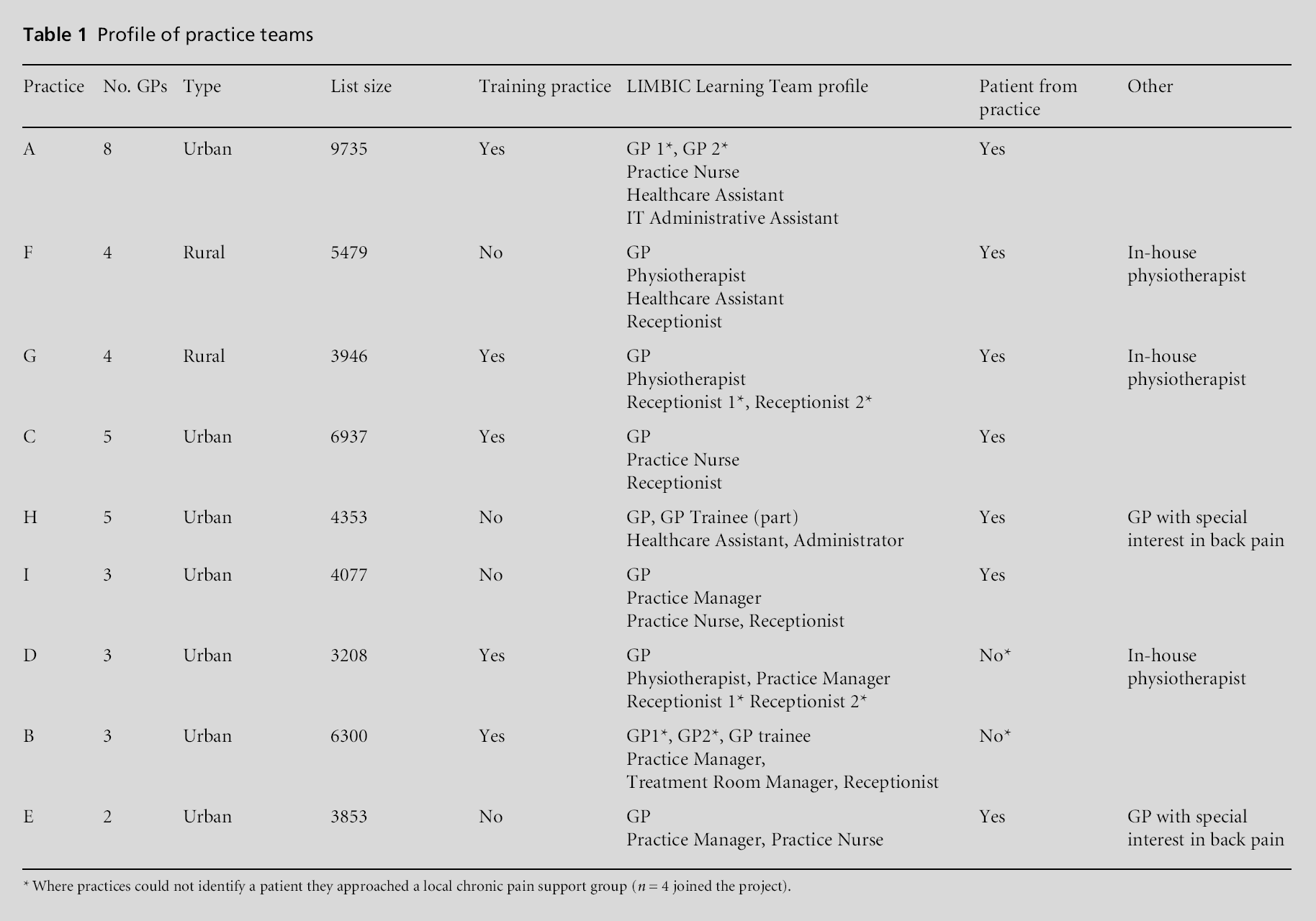
The sample included 44 practice staff and 11 patients who attended the workshops and the facilitated project meetings. Practice team profiles are shown in Table 1.
Format of support for patient involvement in educational workshops
Before the workshops, practices and patients were provided with written guidance and verbal support on patient involvement.[15] Patients attended a pre-workshop briefing meeting at the start of the work-shop programme to follow-up on written materials, share experiences and concerns, prepare ground rules (such as no jargon, being respectful and being willing to ask and respond to questions) and generally offered support. Following the first preparatory meeting, patients requested that each workshop should be preceded by a similar meeting. These were facilitated by a member of the research team and a representative from a national patient organisation; both members of the project steering group.
Throughout the project, support for patients in-cluded newsletters, telephone and email, access to the project wiki and payment for their work (honorarium and travel expenses). A delegate information pack and refreshments were provided at the workshops. Recog-nising that some people may find it distressing talking about their own or others’ experiences of back pain, support was made available to participants. Partici-pants signed a confidentiality agreement regarding the discussions within the workshops.
The patients participated as equal members of the practice team on their improvement projects, both at the workshops and in the practice between the work-shops. Practice teams sought the advice of their patient in developing their high-level aims and process maps, identifying topics for improvement, designing their service improvement, and working together on plan–do–study–act (PDSA) cycles.[16] In the work-shops, patients worked with their own team, with other teams and occasionally as a group with the other patients. Patients presented their own stories of their experience with back pain which became a pivotal point in the progression of the project impacting on the attitudes of the healthcare professionals in relation to the purpose and value of user involvement.
Data collection
Focus group
Each team participated in recorded focus groups held in their practice, one before and one after the completion of the workshops. Focus groups allow an exploration of expectations and experiences17 and permit a space where discussion can occur and their interactions with others are visible.18 Focus groups were facilitated by the project manager and, with the preworkshop group, the quality improvement facilitator. Key areas for discussion are highlighted in Box 1. Focus group interviews lasted between 20 and 50 minutes.

Data analysis
Focus groups were transcribed within two days fol-lowing the focus group interview. Prior to analysis, the transcripts were shared with the practice teams in order for them to clarify their accuracy and agree the content for use in the research. The transcripts were initially coded and themes, patterns and relationships which emerged across the data were identified. From this analysis, emergent themes for the pre-workshop focus groups and the post-workshop focus groups were compared using a matrix analysis.[19]
Findings
Attendance at focus groups ranged from two to six participants. Box 2 outlines the key themes that emerged. Quotes are presented by individuals with the anonymised practice in brackets.

The context of managing back pain
This theme provides the context for the management of back pain in the community. These include lengthy waits for referrals, reduction in service provision due to a lack of funds and concerns about employment.
‘A lot of patients do get referred to physio with back problems but because it’s taking so long to see a physio they don’t turn up to that appointment.’ Physiotherapist [I]
‘We’ve found this before, we have tried to introduce innovative clinics and you don’t get the support or the resources from the Primary Care Trust [PCT]. It’s not that we’re not willing, we are, we just don’t get the support.’ Healthcare Assistant [H]
‘[The consultant] said to me ‘‘sorry you’re not in enough pain, we’re not going to do anything’’. So then I decided I was going to appeal and then I’m getting better treatment now I’ve appealed. I find it annoying that I had to appeal because they presumably think I’m a pain in the backside, which I’m not.’ Patient [E]
‘They’ve taken away the acupuncture, they’ve restricted the chiropractor, we used to have better access to physio.’ GP [C]
‘[Our physiotherapist was taken out of the practice] because of the financial pressure and they’re changing things to try and save money.’ Practice Manager [E]
There was concern from both GPs and patients in terms of the impact back pain had on their employ-ment and especially those who were self-employed:
‘Don’t forget the patients who are working, if they don’t go to work they don’t get paid.’ GP [H]
‘I’m self-employed, I couldn’t work.’ Patient [E]
‘They’re off work and you [the GP] can’t do anything.’ GP [F]
The opportunity for practices to use their improve-ment knowledge from the project was reported posi-tively after their engagement in the project that accessing services became better due to their improve-ment project work.
‘So that [our first PDSA] was very satisfactory and even more so that routines continued and access times aren’t too bad.’ Physiotherapist [D]
Value of involving patients
Patient involvement with the practices was seen as extremely valuable to the teams. The two sub-themes of ‘influential stories’ and ‘different perspectives’ illuminate how their participation contributed to the theme. The stories told by patients were powerful in different ways. The practitioner valued them for giving greater understanding of the effect of back pain on their lives:
‘All [of the] patients were very good indeed, fantastic. I learned a lot from what they said. More so than what the doctors were talking about.’ GP [I]
‘... you know, we probably wouldn’t have made any changes if the patient’s voice hadn’t been there.’ Physio-therapist [F]
‘Actually listening to patients’ experiences made us look at things very differently as well and perhaps understand more about what the patient has to deal with after they leave the surgery. It was quite enlightening.’ Practice Manager [I]
For patients, their stories helped to shape and under-stand their own world better:
‘I found that very helpful, just being able to talk to others and find out what their experiences are.’ Patient [F]
The patients’ stories gave a different perspective which might not normally have been considered.
Listening
The importance of listening was an important theme which crossed both patients’ experiences of healthcare and the practitioners’ experiences of the workshops:
‘A lot of people when they have been to secondary care come back and talk to their GP about how it went and how the person didn’t listen to them.’ Patient [F]
‘I think one of the most important things was listening to what some of the patients said. It was really informative to me.’ GP [I]
‘I thought that I picked up [at the workshops] that they [patients] wanted to be listened to and that is very fair.’ GP [A]
Two further themes emerged following a matrix evaluation of the analysis which were ‘time’ and ‘learning together’.
Time
Time was seen as a finite resource which was highly valued and not to be spent unwisely as well as being particularly challenging:
‘I don’t actually have time [to do home visits].’ Physio-therapist [G]
‘So it’s not that people want to not do things, or aren’t interested, but it’s just the sheer pressure of time and keeping things afloat.’ GP [A]
Practices found it difficult to find the time to attend workshops and do their improvement projects. Indi-vidual clinicians found it difficult to manage their clinical caseloads, and patients noticed this and com-mented upon it.
Learning together
The value of learning together and sharing learning across the different practices stood out as really important. Prior to the workshops, practice teams and patients expressed positive anticipation about learning together as a team despite none of them having done so before. After the workshops, this was borne out by their enthusiasm for engaging with patients and having ‘good fun’ as well as learning.
‘I also enjoyed working with other people, well both within the practice and with other groups, other teams. I think I learnt a lot from listening to them and hearing the things that they tried.’ GP [E]
The discussion draws on the findings to explore three key aspects that were illustrated by the focus group discussions and subsequent thematic analysis. These relate to the context in which back pain is managed, the power of patient stories as part of the learning and the extent to which this educational initiative develops our understanding of ways of meaningfully including patients within IPE.
Central to our study was the inclusion of patients as part of the interprofessional learning teams. Our quality improvement approach started from a deep
understanding of patients’ needs and allowed services to be redesigned to meet these needs.[4,20] It has been
important to make transparent the patient involve-ment in our description of methods and processes.[21] Patients’ experiences of back pain, and sharing these stories, appeared to be particularly pivotal in the learning for practice teams.
The context of managing back pain in the community
It was evident that practitioners and patients faced multiple challenges relating to the management of back pain. A reduction in services, lengthy waiting times for referrals and investigations appear to be an inevitable part of the experience of back pain.[22] Managing patients with enduring chronic pain, who perhaps fail to respond to interventions, can challenge the professional’s self-image of adequacy, competence and authority.[23,24] The overarching educational in-itiative aimed to combine improvement knowledge with evidence-based back pain knowledge so that practices could undertake small ‘improvement projects’ to alter the trajectory of back pain for their patient
population. It was evident that these permitted them to address some of the challenges they faced.
The power of patient stories to influence communication and collaboration
A consistent argument for IPE is that sharing an understanding of each other’s role provides an oppor-tunity to improve communication and collaboration in clinical practice, with an expected improvement in patient care.[25] The use of narrative (sharing experi-ences) has been identified as influential in shaping professional behaviour and potentially influencing patient outcomes.[26] Proposals for core capabilities and competencies in IPE have identified that com-munication skills are a common area germane to all professional groups.[1] The value of involving patients and listening to them were key themes in our study and are integral to good communication. Guidelines for the management of low back pain[27] state that good communication between healthcare professionals and patients is essential in the delivery of best practice for the care of people with non-specific low back pain.
A Canadian study, which tested a communication protocol, aimed to improve communication between health professionals but found little change despite placing the patient as the central focus.[28] It is possible that such approaches do not always permit the patient to have a legitimate ‘voice’. In our study, we explicitly gave the patients the opportunity to both share their back pain stories and participate in the learning with their practice team. Considerable preparation took place prior to each workshop to support patients and they were actively part of the practice teams. The model of patients telling their story has been identified as an effective educational tool for healthcare pro-fessionals.[22] The importance of listening is central to good communication skills and emerged as another important theme in our study.
Each improvement project involved the patient and the choice of project was strongly guided by the patient perspective. In the focus groups conducted prior to the workshops, many practitioners initially aspired to achieve direct access to MRI scans and one practice aiming for a ‘pain-free patient’. Both practices adjusted their aspirations following input from their patients and managed to achieve their goals because they were more realistic and relevant and therefore achievable. Some of the patient stories, shared during workshops, appeared to provide powerful learning insights that created a shift in practitioners’ thinking about the management of back pain.
Studies with patients and education
Patient involvement in health and social care edu-cation has been growing steadily, but tends to focus on patients telling their stories and primarily occurs in undergraduate programmes. The postgraduate or continuing professional development arena of user involvement has predominantly been focused on the areas of mental health, cancer care and social care[29] and usually driven by policy.[30,31] At an organisational level, successful patient, carer and community in-volvement in health and social care education has been implemented across an academic institution using a systematic whole-faculty approach to im-plementation.[32] This is a compelling initiative which places patients at the centre of education.
Collaborative practice has been advocated as essen-tial for the delivery of care and is well reported in IPE, but there appears to be a lack of clarity around the concept of ‘collaboration’. In our study, the role of patients in the interprofessional teams was one of learner, which perhaps served to change the nature of the conversations. Their participation provided an integrator for the learning, with the patient at the centre and also a driver for the improvement – giving both a clear purpose and value. This is very different to professionals gaining feedback from patients and then making their own decisions in isolation. Understand-ing and appreciating professional roles and responsi-bilities and communicating effectively emerged as the two perceived core competencies for patient-centred collaborative practice.[33] The conversations between practitioners and patients also provided an oppor-tunity to construct new meaning around previous experiences and reinterpret events which could be seen to inspire them to manage back pain differently.
We suggest that IPE, which includes the partici-pation of patients as equal team members, working and learning together on service redesign in the practice setting, provided a different way of doing things. The quality improvement approach, used for service redesign, also depends on an in-depth under-standing of the system of care and the processes involved. This can only be achieved by working as an interprofessional team. It was important to estab-lish ground rules and strategies to ensure that all team members could contribute. The focus was to change practice to better reflect clinical evidence. Evidence suggests that simply giving professionals information is largely unsuccessful in modifying practice.[34] We offer this interprofessional approach, which dynamically involves patients, as an alternative.
At the start of the project, many practitioners voiced their frustration at the lack of referral services and the lengthy waiting times. It became evident, following the workshops, that the meaningful in-clusion of patients and their stories appeared to
transform their perspective on the management of back pain. The medical model, acknowledged by pro-fessionals and users to rarely be helpful, was replaced by a biopsychosocial model of care; the emphasis shifting from a fruitless search for cure to one that empowered patients to reclaim their lives. Patients were ahead of the professionals in realising that a total cure was an unrealistic goal and helped the pro-fessionals relinquish this unhelpful pursuit. Patients not only had a voice in the redesign of services related to the management of back pain but they were part of the interprofessional team learning about improve-ment methodology and back pain; they became co-learners.[35] They were given a voice both individually and collectively. The ability to articulate their stories appeared powerful in influencing attitudes and sub-sequent beliefs and behaviours of healthcare teams and individuals. The parity of the relationship between patient and healthcare professional in the learning environment may provide the catalyst to change the learning outcome. Whilst we cannot say that we changed their beliefs, the themes from the focus groups indi-cated that listening and valuing patients seemed piv-otal in changing how they viewed people with back pain and their role in managing back pain.
Strengths and weaknesses
The strengths of the study relate to the detailed processes which illuminated the processes of mean-ingful engagement with patients. The involvement of patients was at the centre of this project and much effort was put into enabling patients and professionals to cooperate on a level playing field. The focus groups provided in-depth insights generated from conver-sations between and across professions and patients. There was a rich diversity of practice profiles which added to the different experiences and perspectives.
The weaknesses of the study relate to practice demands which meant that one team only had two of the team participate in one of the focus groups and the maximum attending was just six. This possibly limited the range and depth of discussions. A further limitation was the absence of behavioural measures to capture changes in clinician behaviour which might have provided additional data to support the con-clusions. The practice teams were self-selected and probably more motivated to effectively manage back pain and therefore probably not representative of practice teams in primary care.
This paper provides an account of the role and experience of involving patients in an IPE project. We conclude that true engagement with patients and their inclusion in IPE, in ways that reinforced practice-based learning, was a catalyst for hallenged the unhelpful medical model in favour of a more integrative biopsychosocial one. We propose that this model has made a contribution to the understanding and impact of patient participation in postgraduate IPE and its influence on professional behaviour. Further research, which engages patients in IPE, should test out this model.the sort of behav-ioural change which leads to improved patient out-comes.[35] Opportunities for patients to share their personal stories of back pain appeared to improve communication and in particular listening. Their presence challenged the unhelpful medical model in favour of a more integrative biopsychosocial one. We propose that this model has made a contribution to the understanding and impact of patient participation in postgraduate IPE and its influence on professional behaviour. Further research, which engages patients in IPE, should test out this model.
The LIMBIC project (Learning to Improve the Man-agement of Back Pain in the Community) was funded by an award from the Health Foundation, UK.
The study received a favourable ethical review in June 2007 (UK NHS Research Ethics Service reference 07/ H0205/36).
Not commissioned; externally peer reviewed.
None.
We would like to thank the practice teams who participated in the LIMBIC project for their time and effort in engaging in the project. Patients, integral to the practice teams, made a unique and pivotal contribution to the project and our learning, thank you. We would also like to acknowledge support given to the research team from the members of the LIMBIC project steering group (see www.limbic.org.uk/steer.html) who offered their collective expertise through-out the course of the project. We were honoured to have some excellent contributors to the workshops who generously shared their experience and expertise with the project participants. These respected individ-uals included Dr Alf Collins, Meherzin Das, Dr Peter Tate, Dr Peter Thorne and Antony Chuter. We would also like to thank Professor Judith Lathlean for her incisive and very helpful comments on an earlier draft of this paper. Finally we thank the Health Foundation whose funding award made the project possible.