Research Paper - (2004) Volume 12, Issue 1
Director of Service Improvement, Salisbury NHS Foundation Trust and Visiting Professor in Healthcare Improvement, Bournemouth and Derby Universities, UK
Received date: 3 August 2010; Accepted date: 22 August 2010
Background Procedures for reporting ‘near misses’ are well established in many large organisations such as, Shell Petroleumand British Airways, which take a less punitive approach to management error than the British NHS. Recent British government documents along with guidance from the National Patient Safety Agency provide the opportunity forthe reporting and learning from experience of adverse events and near misses within a culture of self-re? ection and appraisal.Objective To report the processes and outcomes of an investigation of an incident involving medical equipment and the recommendations that should improve safety and learning.Methods Structured interviews were conducted with ten health personnel in one primary care trust. Interviews were analysed using the protocol developed by the Clinical Risk Unit and the Association of Litigation and Risk Management, which is basedon Reason’s framework.Results The investigation revealed a number of organisational factors which went unnoticed until the incident occurred. Work environment factors were identiŽ ed both at the speciŽ c and general level. The lack of suitable sta¡, or insu¤cient sta¡ wereidentiŽfied as major concerns. The absence of agreed referral criteria and lack of clarity about responsibilities were identiŽfied as contributory factors to the incident. The transitional and transactional arrangements for moving from a primary caregroup to a primary care trust were also highlighted as contributing to the incident.Conclusions The investigation shows that an adapted human factors methodology can be usefully applied to the health sector to enable managers to understand why events occur and, therefore, removes the emphasis from individual errors. A recommendation from the study is that contractor services and independent practitioners would benefit from the use of the primary care trust’s incident reporting framework.
care management problems, factors influencing clinical practice, risk management
Recent British government documents acknowledge the lack of a systematic approach to the reporting of serious failures in healthcare.[1,2] Viewed within the government’s drive to modernise health services and healthcare, these documents, along with guidance from the National Patient Safety Agency set the stage for the reporting and learning from experience of adverse events and near misses within a culture of self-reflection and appraisal.[3] Research on learning from experience in healthcare is relatively sparse, but within the past ten years a critical mass of evidence has been emerging. Included are studies in intensive care, cardiac surgery and medical devices.[4–6] This paper reports the processes and outcomes of investigating an incident involving medical equipment, and details recommendations that should improve safety and learning.
Procedures for reporting ‘near misses’ are well established in many large organisations such as, Shell Petroleum, British Rail and British Airways, which take a less punitive approach to error management than the British NHS.[7] Each year about 400 people die or are seriously injured in adverse events involving medical devices, the causes of which are due to a multiplicity of factors.[1] Reason’s model, developed for use in complex industrial systems, has proved useful in analysing medical accidents and incidents, since the results of these accidents show that medical errors share commonalities with the breakdown of other complex socio-technical systems.[8,9] The Clinical Risk Unit (CRU) and the Association of Litigation and Risk Management (ALARM) have produced a protocol, based on Reason’s framework, for use in the healthcare context.[8,10] The following brief overview is based on Reason’s model which is pro-vided to introduce the basis of the ALARM protocol. (A full discussion of Reason’s thesis is explained elsewhere.)[8,11]
Human errors
Two types of human error contribute to accidents: active failures and latent failures. Active failures refer to unsafe acts committed by people at the ‘sharp-end’ of the system (pilots, air traffic controllers, main-tenance workers, doctors, nurses) whose actions can result in immediate adverse consequences. Latent failures are fallible decisions usually taken at senior management level of the organisation or within soci-ety. Their detrimental e¡ects may go unnoticed for some time, becoming clear only when they combine with other factors such as active failures and mechan-ical faults to bypass or break through the system’s established defence mechanisms. It is suggested that the people most often responsible for the commission of latent failures are removed in time and distance from the frontline personnel.[8] Error-producing con-ditions can therefore occur at any stage along the continuum. Thus, the model comprises four essential components; reading from top to bottom these are: organisational processes, task and environmental con-ditions, individual unsafe acts and failed defences (see Figure 1).
Reason’s error producing conditions and organ-isational factors have been grouped together to pro-duce ALARM’s framework of factors influencing clinical practice, outlined in Box 1.[8,12]

Factors influencing clinical practice
Reading from the bottom upwards of Box 1, ‘patient factors’ refers to the contributory factors which may have influence upon their relationship with the health personnel involved in their care, for example barriers to e¡ective communication, hence increasing the probability of an accident. Individual factors are crucial to good health service delivery since they involve the caregiver’s knowledge, skills and com-petencies to undertake the task. The practices of the individual and their relationship with the patients are constrained by the behaviour of other members of the team. They, in turn, are influenced by decisions, actions and policies of management at the organ-isational level. The organisation, on the other hand, operates within a broader context of regulatory bodies, financial, economic and political influences. Reason’s active failures, that is, unsafe acts or omis-sions committed by those at the ‘sharp end’ of the
system, are replaced by care management problems (CMPs).[8] CMPs have two critical components, both of which are necessary for a CMP to be listed. These are:
1 care deviated beyond safe limits of practice
2 the deviation had a direct or indirect e¡ect on the eventual adverse outcome for the patient.[10]
The framework therefore encompasses the range of possible circumstances to be considered and can be used as a guide for the investigation and analysis of an incident. With the use of CRU and ALARM’s proto-col, the following section provides an outline of the incident before addressing the method and analysis of the case.[10]
Outline of incident
An ultrasound investigation of an elderly female patient was undertaken in the community and was reported to be normal. The investigation was repeated ten days later in a hospital setting and liver metastases were clearly visible. Liver metastases do not normally materialise so suddenly. The primary care trust (PCT) was unsure about the measurement of the quality of the scans and the frequency of the measurements. Given this position, there was a concern that other scans in the community had been similarly mis-reported. The implications of this warranted the instigation of a serious incident investigation.
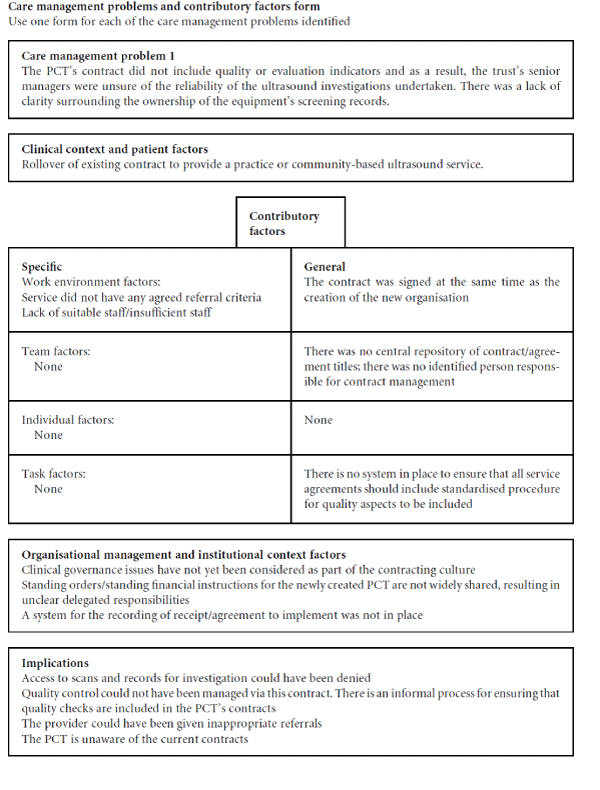
The incident occurred mid-week on a day when scans were not normally undertaken and this was reported formally, triggering the investigation process. Initially, two people were involved in the clinical element of the case: the general practitioner (GP) and the radi-ographer. A wider strategic perspective led to contact with an additional eight people. These were two GPs, one radiologist, one radiographer, one senior com-munity manager, the director of clinical governance and nursing, the director of primary care and the risk manager, giving a total of ten individuals. The facts surrounding the case with these key personnel were established, and details of the service contract were also reviewed. These were undertaken within two working days of the incident being reported. An initial summary was recorded on Appendix 1 as suggested by the protocol.[10] Four CMPs were identified at this stage. Appendix 3 gives an example of one of the four CMPs. The personnel were interviewed indi-vidually, having been assured about confidentiality and that participation was voluntary.
Interview structure
Structured note-taking interviews were recorded by an independent note-taker and conducted by RM with the key personnel identified above, using Appendix 2, which seeks to identify key care management prob-lems involved in the incident. A care management problem is an action or omission by sta¡ in the process of care. This could be due to failure to observe a situation, incorrect decision or action, wrong treat-ment given or non-application of protocol. Although the interviews were structured, the approach was informal and participants were reminded of the purpose of the investigation, namely to:
• begin to establish a ‘no-blame’ culture within the organisation
• encourage the reporting of incidents, accidents and near misses
•seek clarification of the sequence of events and about each of the CMPs identified at the outset of the investigation
•ask supplementary questions about the reasons for each CMP.
The interview lasted between 30 and 45 minutes depending on the extent of the interviewee’s involve-ment in the case. All members were willing to discuss the case and some expressed concerns about similar issues.
Analysis of the case
The interviews were analysed manually by JS and RM using the format identified on Appendix 3 and which is based on the contents of Box 1. It shows some of the organisational factors (latent failures) which went unnoticed until the incident occurred. Work environ-ment factors were identified both at the specific and general level. The lack of suitable sta¡ or insufficient sta¡ were identified as major concerns, and in this case ‘short-cuts’ were made in order to complete tasks. For this CMP there were more general factors than specific ones. These suggest there were outstanding problems within the organisation that had not been addressed. The absence of agreed referral criteria and lack of clarity about responsibilities were identified as con-tributing to the incident. A major aspect of this was the transitional and transactional arrangements for moving from a primary care group (PCG) to a PCT. Previously, the contract process of the PCG was ‘rolled over’ to the next financial/commissioning cycle with-out wider discussions between the contract manager and the director of finance regarding the cost of the service level agreements and clinical need. Thus poor communication is of critical importance, largely due to lack of procedures in a new organisation.
A full report, including the causes of each CMP and recommendations to prevent further occurrence was compiled (see Box 2) and submitted to the board, the professional executive committee of the PCT and the strategic health authority in which the PCT was located. A meeting was held with the interviewees to discuss the outcome and recommendations and how these should be implemented and monitored.

Positive features of the case
The investigation revealed that the contractor for the ultrasound equipment had appropriate systems in place to audit the quality of the screening undertaken. These included:
• twice yearly clinical audit of the screenings under-taken
• database of screenings undertaken
• professional support and continuing professional development both on an individual basis and as part of a network supported by the Society of Radiographers
• a full service profile which included the quality measures in place.
The investigators were commended by the strategic health authority for identifying the issue and the manner of investigation. This was communicated to those involved in the case.
The utility of an organisational analysis framework is that it provides a sound methodology on which to improve safety and simultaneously a¡ords the organ-isation a robust risk management strategy. Addressing only the active failures, that is, those at the ‘sharp end’ of the system, and not the organisational or latent failures, is akin to papering over the cracks: another fault will appear. The deep-seated organisational fail-ures must be addressed since they provide the condi-tions that allow frontline workers to commit errors of judgement. Frequent changes are occurring in the health service and these place added pressures on health personnel to maintain their skills and know-ledge base as well as keeping abreast of organisational procedures.
Although staffing difficulties were identified as a specific issue, they are of major concern in the NHS generally and the drive to recruit, train and retain sta¡ is a national prerogative. This incident analysis has raised issues about change management, the need to keep ‘business’ running smoothly whilst simultan-eously maintaining an uncompromised safe environ-ment for clients and sta¡.
The use of the framework highlighted the need for establishing service agreement guidelines, which should be undertaken with the director of finance and those with responsibility for commissioning services. Thus root causes for unsafe practices can be addressed before serious incidents occur. The framework also acted as a prompt for the interviewees, as they volunteered information about past issues with which they were concerned. The framework and the volun-teering of information provide a rationale to establish ‘learning fora’ between the PCT and the hospital trust under the auspices of the clinical governance frame-work.[13] The essence of this would be to share news and provide support for debate about issues of concern, within a safe environment. This approach and the methodology of the investigation concur with guid-ance from the National Patient Safety Agency whose intention is to promote an open and fair culture in the NHS by encouraging health personnel to report incidents without fear of personal reprimand.[2] The agency intends to collate published reports from throughout the country and initiate preventative measures so that the NHS can learn from each case and improve patient safety.
The study has shown that adapted human factors methodology can be usefully applied to the health sector and enable managers to understand why events occur and, therefore, removes the emphasis from individual errors. Care problems that result in adverse outcomes provide opportunities for quality improve-ment. This incident has given rise to consideration of whether or not to continue with scans in the com-munity. To date this has continued without detri-ment. By highlighting this incident, the PCT intends to continue open learning, the sharing of good practice to improve patient care.
A recommendation from this study is that contrac-tor services and independent practitioners would benefit from the use of the PCT’s incident reporting framework.
None.
Appendix 1

Appendix 2

Appendix 3