Key words
client–providercommunication, clinical
encounters, ethnic minorities, hospital setting, intercultural
mediation, interpreting services, language
barriers, migrants
Introduction
The provision of culturally and linguistically appropriate
communication in healthcare poses considerable
challenges to health policy and frontline service
provision alike. Hospitals in particular are consulted
by an increasingly diverse clientele (Hampers and
McNulty, 2002; Yeo, 2004). As a consequence, there
are language barriers between specific patients and
providers: patients coming to the hospital may not be
able to speak and/or understand the local language,
and staff may not be able to communicate in the
patients’ mother tongue or a common language. This
frequently leads to communication problems and
misunderstandings that may negatively affect clinical
encounters and treatment outcomes.
Clinical encounters are defined as client–provider
communications occurring as part of diagnosis and
treatment and which involve the negotiation of explanatory
models between physician and patient
(Pirbhai, 2003). In clinical encounters it is important
that relevant clinical information is elicited from and
conveyed to the patient in a correct and appropriate
manner as a prerequisite for both clinical decision
making and the establishment of trust between the
two parties concerned. Effective communication is an
essential part of successful treatment and in securing
patients’ co-operation. Furthermore, it plays an important
role in assessing pain and prescribing adequate
medication (Cleeland et al, 1997; Brown et al,
1999).
Language barriers are a major obstacle in providing
effective health services; they have adverse effects on
accessibility, quality of care, patient satisfaction and
patient health outcomes (Bischoff, 2003; Murphy, 2004).
For example, language-related communication difficulties
are associated with a higher rate of resource
utilisation for diagnostic testing (Waxman and Levitt,
2000; Hampers and McNulty, 2002) and an increase
in the likelihood of unnecessary invasive procedures
(Bard et al, 2004); they negatively affect the continuity
of care (Sarver and Baker, 2000; Yeo, 2004; Brotanek
et al, 2005), and they create a barrier to the use of
preventive services (Woloshin et al, 1997). Miscommunication
can also lead to substantial extra costs
in the provision of services: more time resources are
required for routine encounters in the treatment process,
leading to longer periods of stay (John-Baptiste et al,
2004) or additional organisational burden for the staff
(Drennan, 1996). Moreover, delays in the treatment
process or clinical decisions based on inaccurate information
can result in poor treatment outcomes. In
addition to threats to patients’ health and quality of
life, these delays also bear the risk of actual liability
costs for the healthcare institution (Bischoff, 2003).
Addressing the language gap
Healthcare institutions have devised responses to
these communication barriers in order to provide
effective services to their linguistically diverse clientele.
In the past, however, these responses have relied
heavily on the ad hoc use of bilingual staff or patients’
family and friends to bridge language gaps. Such
reliance carries several risks, including the likelihood
of poorer healthcare due to inadequate communication
and undesired health outcomes.
In recent years, however, many hospitals have seen
the need to go further to ensure that quality care is
provided to all patients. Professional strategies to facilitate
communication between patients and providers
have proven effective in improving service quality and
outcomes for migrant and ethnic minority patients
who face language barriers in utilising health services
(Tocher and Larson, 1998; Jacobs et al, 2004), the most
effective approach being the introduction of professional
medical interpreters (Jacobs et al, 2004). In
addition to their language competence, professional
interpreters have a strong medical vocabulary and
specific communication skills, as well as an understanding
of the ethical issues involved in their role
(Bischoff et al, 2003). While the cost of hiring interpreters
or contracting their services from outside
agencies may present barriers to their employment,
a study in the US showed that the annual cost of
interpreters per patient was compensated by significant
improvements in patients’ service use, compliance
and health outcomes (Jacobs et al, 2004).
The type of interpreting support provided differs
significantly in terms of the healthcare systems concerned,
the demographic make-up of communities,
and the type of services provided (Schulze et al, 2003).
For example, a hospital serving a clientele that has a
high proportion of people who speak a specific language
may benefit from hiring full-time interpreters. Another
hospital with the same number of non-native speakers
of many different languages will not be able to provide
on-site service for everyone. In this case, making arrangements
with freelance interpreters would seem
to be the more feasible option. Hospitals that have to
provide emergency services may benefit most from
telephone interpreting services or may need translated
material to support clinical communication.
A European perspective
With increases in global migration flows, the challenges
posed to healthcare by cultural and linguistic
diversity are likely to intensify. This calls for a concerted
response and an expansion of the evidence base for effective strategies to address language barriers across
a range of services and specific local circumstances.
TheMigrant-friendlyHospitals Project (Box 1) represented
a wide spectrum of hospital services, ranging
from large metropolitan university teaching hospitals
to small-town community hospitals, with diverse
migration situations in their catchment areas and
different levels of experience in serving populations
with limited proficiency in the local languages.
The project provided a range of solutions that were
developed and implemented based on a combination
of local needs assessments at the different sites, and a
systematic review of effective interventions (Bischoff,
2003).
In the needs assessment, communication was identified
as the most prominent area of concern in dealing
with migrant and ethnic minority populations in
clinical routines. The development of effective services
to bridge the language gap between providers and
diverse patient groups was therefore a central focus in
the project. The emphasis in the project work under
discussion here was on interpreting in clinical communication;
that is to say, on conveying medical information
across language barriers in spoken conversation,
with the presence of an interpreter either in person or
in a remote setting connected via telephone, video or
other media.
Aims
Nine hospitals in Denmark, Finland, Greece, Spain,
Ireland, Italy, The Netherlands, Sweden and the UK
co-operated to improve clinical communication with migrant and ethnic minority patients (see Box 2).
Altogether, 37.9% of the clinical staff in these hospitals,
including doctors, nurses, therapists, social workers
and clerical workers, reported daily contact with this
patient group; another 28.5% reported contact two or
three times per week. The aims of this part of the
Migrant-friendly Hospitals Project were to ensure:
• the provision of professional interpreter services
whenever necessary to ensure good communication
between non-local language speakers and clinical
staff
• that patients were informed about the language
services available and how to access them
• that clinical staff were empowered to work competently
with interpreters to overcome language
barriers and obtain better outcomes
• the provision of education materials for patients in
non-local languages.
Interventions
In order to enhance clinical communication between
staff and migrants, the participating hospitals implemented
different measures to develop new and/or
improve existing interpreting services.
Measures were planned according to the individual
needs of each hospital. In some cases, no interpreting
services existed, so those hospitals developed an entire
plan for service development and implementation.
More commonly, though, measures focused on improving
existing services to increase their efficiency
and effectiveness. Taking into account specific hospital structures and processes, different types of interpreting
services were implemented: telephone interpreting,
face-to-face interpreting, intercultural mediation,
and/or written material as communication aid.
Box 1: The European project ‘Migrant-friendly Hospitals’ (MFH)
Box 2: The composition of the subproject group.
Two models of good practice that were developed
and implemented in the project framework are described
below to illustrate the type of specific solutions
applied (see Boxes 3 and 4).
Evaluation design
A pre- and a post-intervention staff survey and a postintervention
patient survey were conducted using a
benchmarking learning and evaluation design.
Hospital staff were questioned twice, once in a baseline
survey in February 2004 (n = 479 in seven hospitals),
and a second time in a further survey in June
2004 (n = 282 in six hospitals) after implementation
of the measures. One hospital did not conduct the
second staff survey because the intervention employed
extended until after completion of the project.
Medical and nursing staff were asked, in a standardised
written questionnaire, about their experiences
of encounters with patients who had a limited command
of the local language, and about how they (the
staff) rated the quality of the available interpreting
services. They were also asked to provide information
on how they thought interpreting support should be
improved. In the second survey, there was an extra
question about the extent to which the individual
work situation had improved as a result of project
measures.
Three hospitals conducted a post-intervention patient
survey (n = 42) parallel to the second staff survey in
June 2004. Following a clinical encounter involving
an interpreter, patients were interviewed about the attendance of the interpreter, their ratings of the
interpreter’s work, the encounter with the doctor
and their views as to how interpreting support should
be improved.
In a third evaluation step, project managers at the
hospitals answered a short questionnaire which asked
them to assess the extent to which the measure could
be implemented, to list both enabling factors and
obstacles in the implementation process, and to provide
information on the sustainability of the measures.
Findings
Staff survey
Analysis of the pre- and post-intervention staff surveys
showed that the interventions, such as the soundstation,
were effective. Comparison of the baseline and
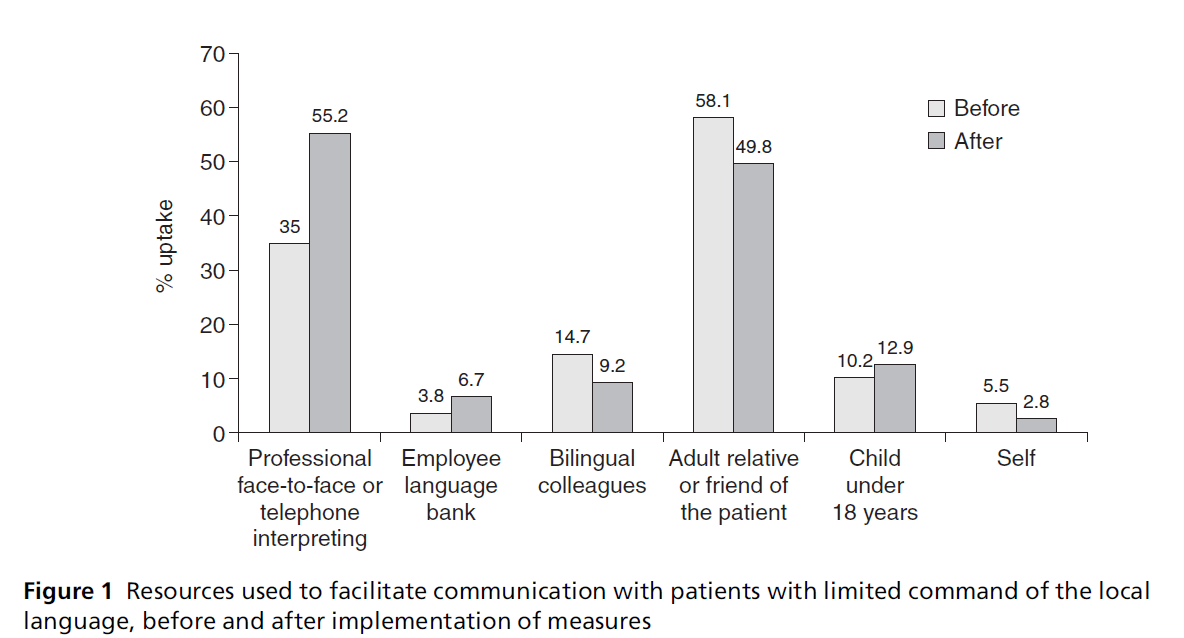
second staff surveys showed that the uptake of professional
interpreting increased by 20.2%, with a
concurrent decrease of nearly 10% in interpreting provided
by adult relatives and friends (see Figure 1).
However, a 2% increase was observed in the use of
children, under the age of 18, as interpreters.
In addition, the quality of interpreting services was
evaluated more positively after the interventions were
introduced. Interpreters were said to be available in a
timely manner and more frequently than they had
been in the baseline survey (+17.5%). Furthermore, an
improvementwas noted for all defined quality indicators
for interpreting services, such as introduction and role
explanation by interpreters (+10.8%), accurate transmission
of information (+6.8%), clarification by interpreters
(+7.7%), clarification of cultural beliefs (+10.5%) and
the identification of patients’ further needs by interpreters
(+7.3%). There was an improvement in the overall rating of interpreting services; the proportion
of those judging the service to be excellent or very
good increased by 21.3% and 54.9% of the staff
members stated that the work situation had improved
because of the interventions employed.
Box 3:Good practice experience 1: telephone interpreting in Denmark.
Figure 1: Resources used to facilitate communication with patients with limited command of the local
language, before and after implementation of measures
Box 4: Good practice experience 2: mediation services in Italy.
Patient survey
Analysis showed high levels of patient satisfaction with
the performance of hospital interpreters: 78% of patients
strongly agreed that, with the interpreter’s help, they
understood all the medical information (the other
22% agreed); 83% strongly agreed that the interpreter
assisted them in relaying important (lifestyle) information
to the doctor (17.1% agreed). In general, ratings
concerning the doctor’s performance were also very
high: patients felt that doctors took time to talk with
them (70.7% strongly agreed/29.3% agreed), showed
sensitivity to their cultural beliefs and needs (68.3%/
29.3%), encouraged them to ask questions (68.3%/
29.3%) and worked together with the interpreter to
make sure they understood everything (67.5%/30.0%).On the other hand, patients were less satisfied with
direct doctor–patient communication: only 31.7%
strongly agreed (14.6%agreed) that the doctor talked
directly to them rather than to the interpreter when
giving or asking for information, but 48.8% disagreed
and 4.9% even strongly disagreed.
Evaluation of implementation
The interventions can be categorised in four groups:
• development/improvement of face-to-face interpreting
• development/improvement of telephone interpreting
• development/translation of written material as
supporting communication
• implementation of intercultural mediation.
It was not possible to identify one specific measure as
a model of best practice. In fact, the combination of
the local situation, involved partners and the concrete
measures seemed to be the determining factor for the acceptance, feasibility and the effectiveness of interventions.
Implementing the interventions turned out to be a
difficult task. Local project managers had to adjust
their strategies, make compromises and demonstrate
considerable flexibility. Four interventions were implemented
completely, eight to some extent, and two
not at all. Two-thirds of the interventions were difficult
to implement because of factors such as lack of
acceptance and utilisation of the service, lack of
sufficient time, and logistics. Only four could be easily
implemented and these are described in Box 5.
From the project managers’ point of view, the aims
of the project were very worthwhile. All of the interventions
that were implemented will be continued.
Three have become an established part of the hospitals’
service, four will be adapted and then included in
service routines, and five will even be extended.
Discussion
The evaluation confirmed existing international
knowledge and experience about improving the quality
of interpreting services in hospitals (Jacobs et al,
2004; Bischoff et al, 2003). Hospital co-operation
within a scientifically supported benchmarking approach
proved to be feasible and effective. Despite the
huge diversity of healthcare systems, hospital and
departmental structures, and migrant population characteristics,
all partner hospitals had to handle very
similar problems.
Comparability of data and experiences was, on the
one hand, assured by a central benchmarking evaluation
of procedures with questionnaires, guidelines
and documentation sheets as standardised tools, and
there was a central analysis of survey data on the basis
of detailed documentation of the diverse evaluation procedures. On the other hand, a high degree of
flexibility was allowed concerning the individual design
of procedures for conducting the surveys, for
selecting target groups and for planning and implementing
the measures.
Box 5: Measures that could be implemented easily, from the project manager’s point of view.
In order to ensure the viability of the benchmarking
group and to support the hospitals’ processes of
learning from one other, a co-ordinated schedule for
central project steps was necessary, and there was a
clear need for information about the context of each
partner’s work in order to allow for a determination of
where each partner ranged in the group of hospitals.
The design, the services of the project’s expert consultant
as a practical advisor, and scientific support
and co-ordination all proved to be essential for the success of the benchmarking. Box 6 presents an
account of some of the concrete difficulties faced,
taking as an example the pilot hospital in Spain.
Conclusion and
recommendations
The experiences of nine pilot hospitals across Europe
show that the central steps in setting up interpreting
services in a hospital setting are:
1 obtaining both symbolic and practical support
from management
Box 6:The Spanish partner hospital’s experiences.
2 establishing central co-ordination of interpreting
services, and hiring an interpreting co-ordinator or
appointing staff from within the hospital to control
the budget, track volume increase and assure quality
of service
3 choosing appropriate interpreting resources, for
example, employee language bank, telephone interpreters
or face-to-face interpreters, either from
external interpreting agencies or from in-house
professional clinical interpreters
4 training for interpreters and clinical staff
5 marketing of the service to increase awareness and
visibility
6 asystematic approach to the production of policies
and guidelines and to the translation of written
materials.
Further, the outcomes of the project reveal the central
prerequisites for the successful and sustainable implementation
of measures to improve the quality of
clinical communication with migrant or ethnic minority
patients. There are several preconditions that
have to be met in order to improve clinical communication
for migrants consistently:
• linguistically adequate clinical communication has
to be integrated into a hospital’s general policy on
diversity. As an important step, the needs and assets
of all stakeholders – including both users (patients,
relatives, community) and providers (staff) – should
be monitored. The outcomes of implemented
interpreting services, as well as the structures and
processes that influence access to interpreting services
and their quality, must be monitored
• services and processes have to be sustained by
becoming mainstream and not relying on local
champions alone. In other words, an organisational
development process should be initiated,
supported and monitored by those responsible
for hospital leadership, overall management and
quality management. It is necessary to invest in
both the medical interpreters’ and clinical staff ’s
developing skills and competences regarding the
effective performance and use of interpreting services
• adequate political and managerial will and funding
have to be assured. Adequate resources – working
time, financial resources, and qualification – must
be provided if changes are to be realised. By providing
legal and financial support and by formulating
organisational aims, health policy must
provide a framework in order to make the development
of interpreting services on the hospital
level relevant and feasible.
ACKNOWLEDGEMENTS
Special thanks to the many partners in the pilot
hospitals of the Migrant-Friendly Hospitals project
that implemented the interventions and were most
helpful in evaluation. Representing their teams, the
authorswould like to thank the subproject co-ordinators
Antonio Chiarenza, Ulises Penayo, Fiona McDaid,
Adrian Manning, Jette Ammentorp, Anne-Mette
Rasmussen, Minna Pohjola, Marja-Leena Pilkkinen,
Ines Garcia-Sanchez, Carmen Fernandez Guerra and
Georgia Vasilopolous. Special thanks is also expressed
to Lourdes Sanchez, our expert consultant from
Boston, USA.
\
References
- Bard MR, Goettler CE, Schenarts PJ et al (2004) Languagebarrier leads to the unnecessary intubation of traumapatients. The American Surgeon 70:783–6.
- Bischoff A (2003) Caring for Migrant and Minority Patientsin European Hospitals. A review of effective interventions.Study commissioned by the Ludwig Boltzmann Institute forthe Sociology of Health and Medicine, Vienna, ‘MFH –migrant-friendly hospitals, a European initiative to promotehealth and health literacy for migrants and ethnic minorities’.
- Neuchatel, Basel: Swiss Forum for Migration andPopulation Studies.
- Bischoff A, Perneger TV, Bovier PA, Loutan L and Stalder H(2003) Improving communication between physiciansand patients who speak a foreign language. British Journalof General Practice 53:541–6.
- Brotanek JM, Halterman J, Auinger P and Weitzman M(2005) Inadequate access to care among children withasthma from Spanish-speaking families. Journal of HealthCare for the Poor and Underserved 16:63–73.
- Brown AF, Perez-Stable EJ, Whitaker EE et al (1999) Ethnicdifferences in hormone replacement prescribing patterns.Journal of General Internal Medicine 14:663–9.
- Cleeland CS, Gonin R, Baez L, Loehrer P and Pandya KJ(1997) Pain and treatment of pain in minority patientswith cancer: The Eastern Cooperative Oncology GroupMinority Outpatient Pain Study. Annals of Internal Medicine127:813–16.
- Drennan G (1996) Counting the cost of language services inpsychiatry. South African Medical Journal 86:343–5.
- Hampers LC and McNulty JE (2002) Professional interpretersand bilingual physicians in a pediatric emergencydepartment: effect on resource utilization. Archivesof Pediatrics and Adolescent Medicine 156:1108–13.
- Jacobs EA, Shepard DS, Suaya JA and Stone EL (2004)Overcoming language barriers in healthcare: costs andbenefits of interpreter services. American Journal of PublicHealth 94:866–9.
- John-Baptiste A, Naglie G, Tomlinson G et al (2004) Theeffect of English language proficiency on length of stayand in-hospital mortality. Journal of General InternalMedicine 19:221–8.
- Krajic K, Karl-Trummer U, Novak-Zezula S, WirtenbergerMandPelikanJM (2005) Migrant-Friendly Hospitals in anEthno-culturallyDiverse Europe. Experiences froma EuropeanPilot Hospital Project. Final Report, Booklet and CDROM. Vienna: Ludwig Boltzmann Institute for the Sociologyof Health and Medicine.
- Murphy S (2004) Communicating with limited Englishproficiency (LEP) patients: question of health-care access.Journal of Medical Practice Management 20:23–7.
- Pirbhai A (2003) Communicating in the clinical encounter:dealing with the disparities. The Einstein Journal of Biologyand Medicine 20:19–22.
- Sarver J and BakerDW(2000) Effect of language barriers onfollow-up appointments after an emergency departmentvisit. Journal of General Internal Medicine 15:256–64.
- Schulze B, Nowak P, Krajic K, Trummer U and Pelikan JM(2003) Improving Interpreting in Clinical Communication.Pathway for implementation and evaluation. Vienna:Ludwig Boltzmann Institute for the Sociology of Healthand Medicine.
- Tocher TM and Larson E (1998) Quality of diabetes carefor non-English-speaking patients. A comparative study.Western Journal of Medicine 168:504–11.
- Waxman MA and Levitt AM (2000) Are diagnostic testingand admission rates higher in non-English-speakingversus English-speaking patients in the emergency department?Annals of Emergency Medicine 36:456–61.
- Woloshin S, Schwartz LM, Katz SJ and Welch HG (1997) Islanguage a barrier to the use of preventive services?Journal of General Internal Medicine 12:472–7.
- Yeo S (2004) Language barriers and access to care. Annual Review of Nursing Research 22:59–73.