Clinical Governance in Action - (2004) Volume 12, Issue 1
Audit Co-ordinator
John Gillies MBChB FRCP FRCGP DCH DTm&H MA
General Practitioner
Department of Public Health, Borders NHS Board, Newstead, Melrose, Roxburghshire, UK
Erkki Vartiainen MD PhD
Professor of Public Health, Director, Department of Epidemiology and Health Promotion, National Public Health Institute, Helsinki, Finland
James Dunbar MD MBChB FRCGP FRCP FFPHM
Professor of Rural Health, Director, Greater Green Triangle University, Department of Rural Health, Warrnabool, Victoria, Australia
Barbara Nettleton BSc MSc
Senior Health Promotion O¤cer, Health Promotion Department, Borders NHS Primary Care, Tweed Horizons, Newtown St Boswells, Roxburghshire, UK
Accepted date: 8 October 2003
Scotland has one of the highest rates of coronary heart disease (CHD) in the world. The Hearts in the Borders project was set up in the Scottish Borders with the aim of providing the highest possible standards of care and improving the health of patients with CHD. The project is multidisciplinary and multi-organisational with an innovative implementation strategy involving guideline development and implementation, audit, sta¡ training, and the development and use of a resource pack. The project started in 1998 and three audit cycles (in late 1999, 2000 and 2002) have been conducted to date. All practices in the Borders now have a CHD register. The project targeted patients under the age of 75 years with a history of myocardial infarction, coronary artery bypass grafting and/or angioplasty. Major improvements occurred in cholesterol control with the number of patients with cholesterol below 5 mmol/l improving from 29% to 62%. Aspirin prescribing is high with trends towards better control of blood pressure. Improvements in lifestyle advice given were also found. A positive outcome of the project was a reduction in hospitaladmissions from 32% in the 1999 audit to 20% in 2002. The project has beneŽ ted the Borders by introducing new ways of working across professional and organisational divides, and provided a foundation for the development of a management clinical network for CHD. The model developed has also allowed more rapid planning of a local project to implement the hypertension guidelines. The project has been awarded three national awards for its innovative approach to CHD.
There is good evidence that reduction in cardio-vascular events and mortality can be achieved in coronary heart disease (CHD) patients by lowering serum cholesterol, controlling blood pressure, and taking aspirin and making lifestyle changes such as stopping smoking.[1–5] Therefore a good scientific con-sensus exists on e¡ective measures in secondary pre-vention of CHD.[6,7] The potential for preventive action is great in CHD patients but research indicates that considerable improvement is needed in practice.[8] In Scotland it is not known how these recommendations are followed and to what extent health board level programmes can improve the situation.
Based on the European recommendations all cor-onary patients should have their blood pressure con-sistently below 140/90 mmHg.[6] If the goal is not achieved with lifestyle changes, drug therapy should be used. In blood total cholesterol the goal is below 5 mmol/l and in low-density lipids (LDLs) 3 mmol/l. Statins should be used if the goal is not achieved by dietary changes. Aspirin should be given to virtually all patients, beta-blockers after myocardial infarction (MI), and angiotensin converting enzyme (ACE) inhibitor to patients with heart failure.
Scotland has one of the highest rates of CHD in the world and CHD is therefore a major national and local priority.[9,10] The decision to target secondary preven-tion was made after a local review of CHD services. A practice nurse survey was also performed which high-lighted the need for training and better patient information materials. These led to the formation of the Hearts in the Borders project, which is a multi-disciplinary multi-organisational initiative with the aim of providing the highest possible standards of care, and improving the health of patients with CHD in the Scottish Borders. This paper describes the successful implementation initiative.
The Scottish Borders is a large (4700 km2) rural area with a population of 106 000, of which 19% are over 65 years. Healthcare is provided by a single health board and by one acute hospital trust, one primary care trust (PCT), and two local health care co-operatives, which include 87 general practitioners (GPs) and 22 practices.
The project’s multidisciplinary steering group con-sisted of a cardiologist/physician, guidelines advisor, audit co-ordinator, health promotion specialist, sup-port pharmacist, GPs, practice and hospital nurses,
dietician, and public health consultant. The project’s implementation plan was divided into three sections with smaller multidisciplinary subgroups set up to manage each stage (see Figure 1).
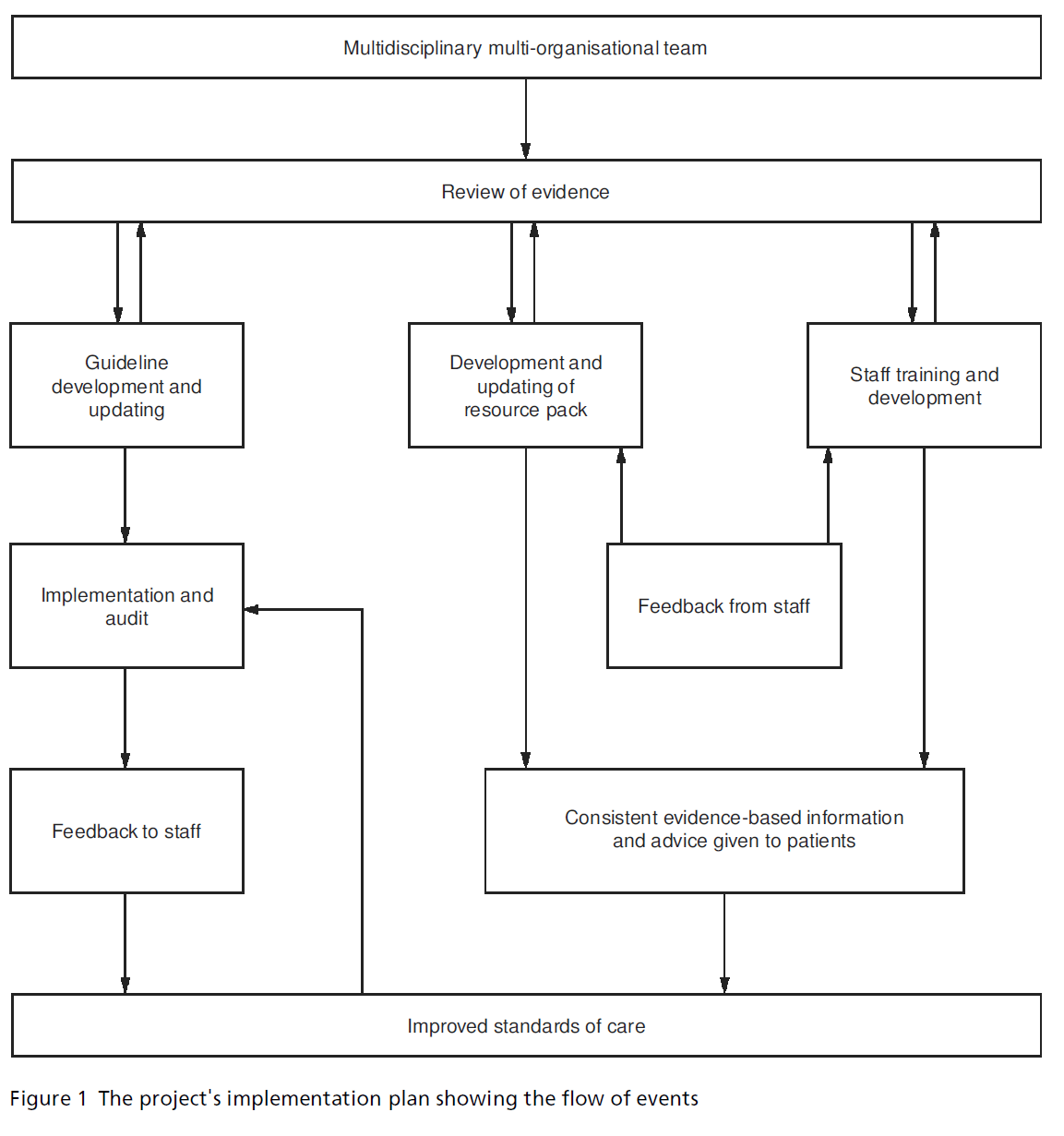
Figure 1: The project's implementation plan showing the flow of events
Stage 1
A local guideline for the management of secondary prevention of CHD was developed and a draft presented at a consensus meeting to improve the acceptance and implementation (see Figure 2). The guideline was modified in the light of the comments made and a system was set up to review the evidence. The guideline was updated after two years.
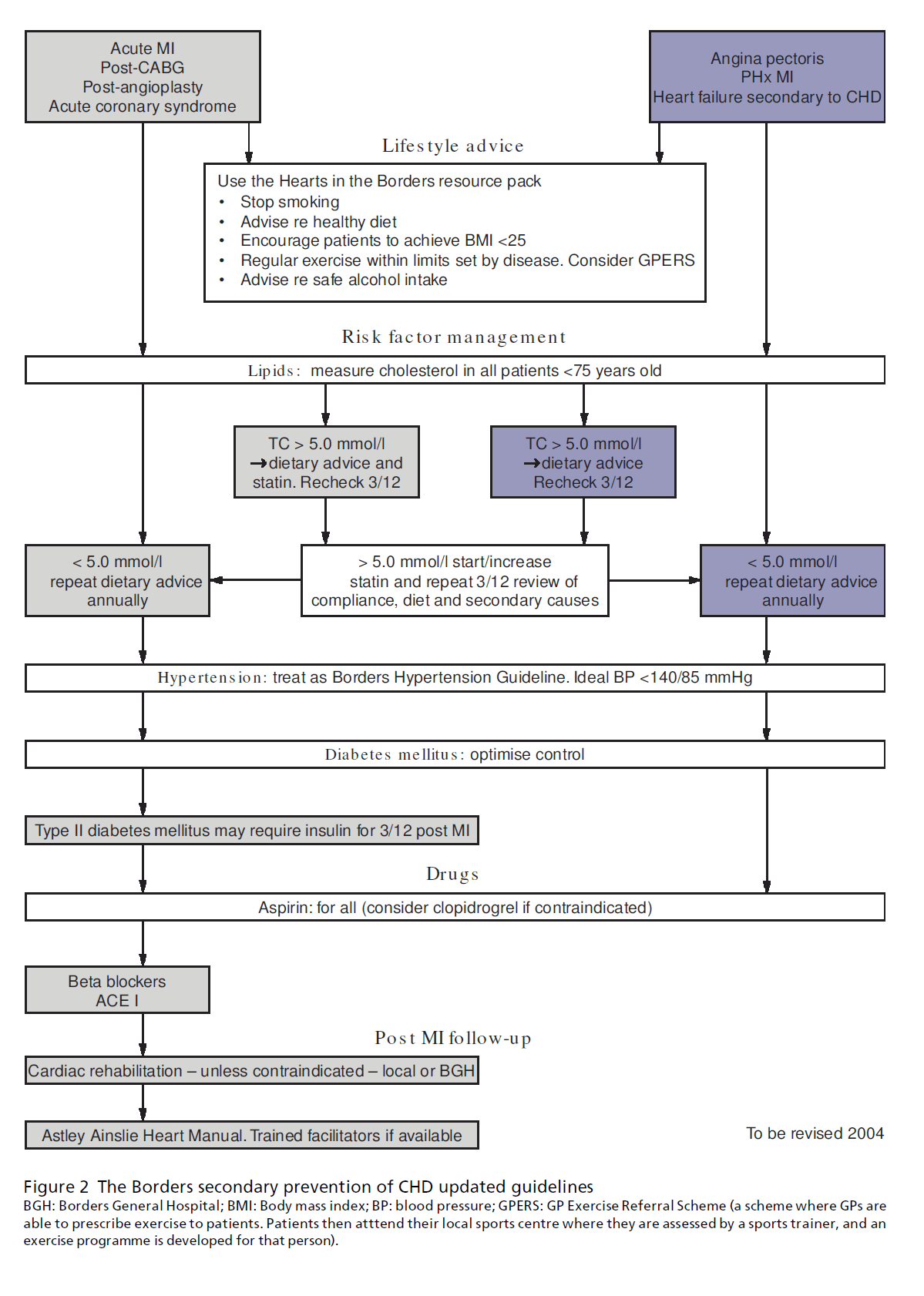
Figure 2: The Borders secondary prevention of CHD updated guidelines.
BGH: Borders General Hospital; BMI: Body mass index; BP: blood pressure;GPERS: GP Exercise Referral Scheme (a scheme where GPs are
able to prescribe exercise to patients. Patients then atttend their local sports centre where they are assessed by a sports trainer, and an
exercise programme is developed for that person).
To measure the impact of implementing the devel-oped guideline, a baseline audit was conducted prior to their publication and a disease management system for secondary prevention of CHD introduced. An audit database was set up of patients under 75 years with a recent event or past medical history of MI, angioplasty and/or coronary artery bypass grafting (CABG) based on review of medical records in health centres and hospitals.
Following the baseline audit the guideline was released and an audit report provided sta¡ with feed-back regarding their practice and comparisons between practices of targeted standards for improve-ments. The targeted standards were blood cholesterol levels, blood pressure, lifestyle measures (that is, smoking, dietary and exercise advice) and prescribing of aspirin, statins, ACE inhibitors and beta-blockers. Data on hospital admissions were also collected. The audit cycle was repeated at a 12- and 24-month interval after the baseline audit.
Stage 2
Following the baseline audit, practices set up disease registers to facilitate the management (for example, recall of these targeted patients). The audit allowed us to identify areas where change was necessary (for example, smoking cessation counselling). Auditing was both labour intensive and expensive under the current auditing system which involved manual data collection at each practice and inputting the informa-tion into a central CHD database for analysis and reporting. In order to improve e¤ciency and e¡ect-iveness and enhance the project’s achievements, a subgroup was set up to introduce a system that will facilitate paperless data collection and automatic analysis and reporting, allowing easy identification of this high-risk group of patients and their modifiable risk factors.
We are currently piloting a system that involves electronic data collection using the Clinical Disease Support System (CDSS) for the General Practice Support System for Scotland (GPASS) at practice level. From GPASS the anonymised information can flow into a central SQL database for automatic Borders-wide analysis and reporting. At practice level electronic auditing functions will also be provided through CDSS and GPASS.
Stage 3
Following the outcome of the practice nurse survey a subgroup was set up to address patients’ lifestyles. A training programme was introduced and a resource pack was developed to support it, containing informa-tion sheets, lea• ets, patient diaries, etc, covering generic motivational interviewing and the major lifestyle risk factors. The information contained in the pack is consistent with current knowledge, on CHD risk factors and relevant to the area (for example, walking groups in the Borders).
The lifestyle counselling training programme was developed locally and attendance is multidisciplinary. A two-day course on motivating change is followed by topic-based courses on stress management, smoking cessation, healthy eating, safer drinking and working with people with learning disabilities. Uptake of this rolling programme is high with 225 participants in the first two years. Feedback from the courses ensures quality.
The resource pack is used in all training and sent to every practice, hospital and pharmacy. Combining the use of the resource pack with all the training ensures that all health professionals in the Borders provide consistent and up to date information regardless of professional background or location. A questionnaire survey of users of the pack found it to be useful.
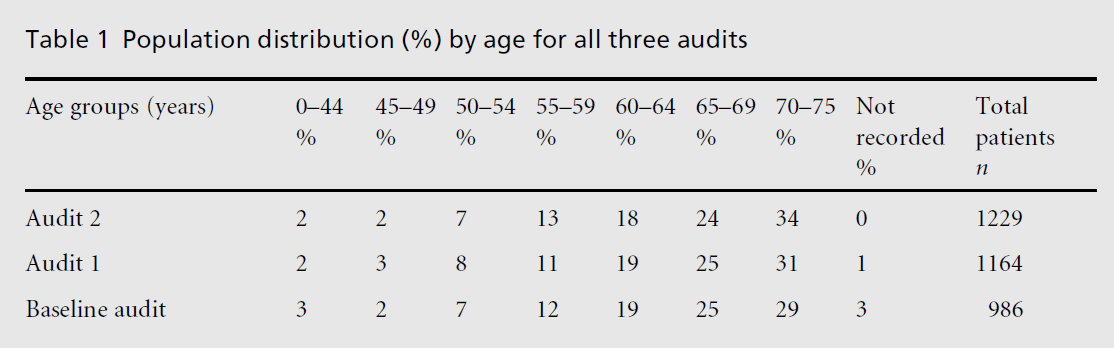
For all three audits the sex distribution was approxi-mately three-quarters male to one-quarter female. The percentage prevalence was calculated by dividing the CHD population by all patients registered with a GP and multiplying by 100. The overall prevalence of CHD increased with age, peaking in the 70–75 years age group (see Table 1) with an overall prevalence of 0.93% (n = 986) at baseline, which stabilised at around 1.1% for the other two audits (that is, 1.10% (n = 1164) for audit 1 and 1.14% (n = 1229) for audit 2), re• ecting improved case finding.

Cigarette smoking habits remained at 19% (see Figure 3) despite targeted resources to reduce this. However, the number of ex-smokers increased from 48% (n = 476) at baseline to 51% (n = 594) and 53% (n = 651) for audits 1 and 2 respectively, suggesting better recording. Over the three audits carried out, dietary advice was given to patients more often than exercise advice (see Figure 4). Dietary advice given increased from 66% (n = 702) at baseline to 90% (n = 995) in the last audit. Similarly, exercise advice given improved from 52% (n = 516) to 72% (n = 883) in the final audit. This shows the huge focus on lifestyle issues re• ected by the guidelines, training and the resources pack.
In the baseline audit, the number of patients with target total blood cholesterol below 5 mmol/l was 29% (n = 283) (see Figure 5). This increased to 45% (n = 528) 12 months later (that is, audit 1) and 62% (n = 763) by audit 2. This improvement was mainly achieved through targeted statin prescribing which rose from 51% (n = 507) at baseline to 63% (n = 739) at audit 1 and 75% (n = 917) at audit 2 (see Figure 6). The evidence-based benefits of lowering total choles-terol are reduced morbidity and mortality, and the results show improving standards of care for this high-risk group of patients.
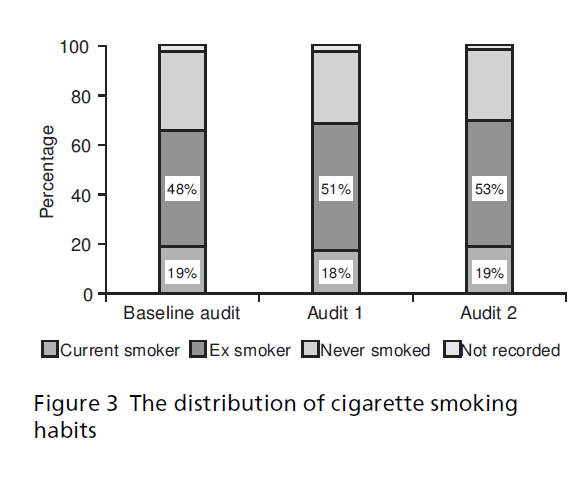
Figure 3: The distribution of cigarette smoking habits.
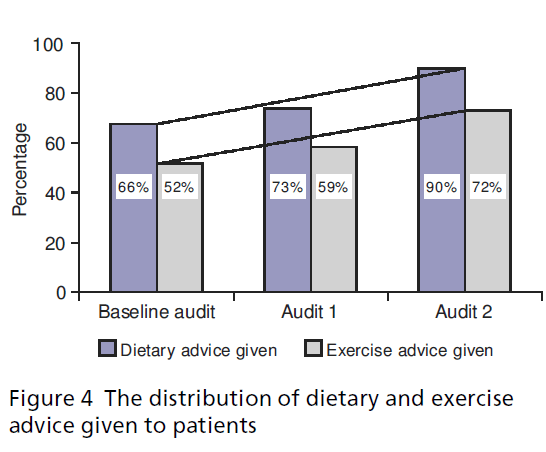
Figure 4: The distribution of dietary and exercise advice given to patients.
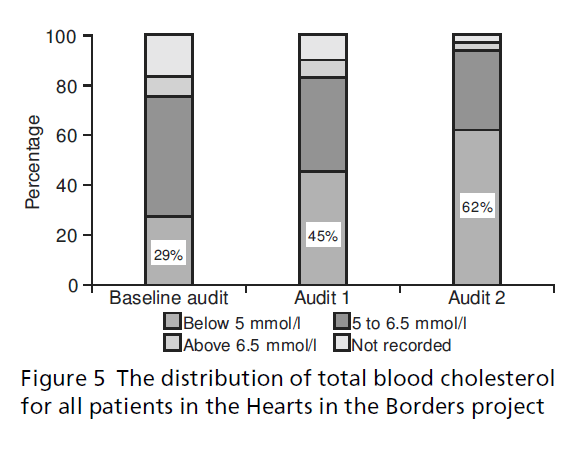
Figure 5:The distribution of total blood cholesterol for all patients in the Hearts in the Borders project.
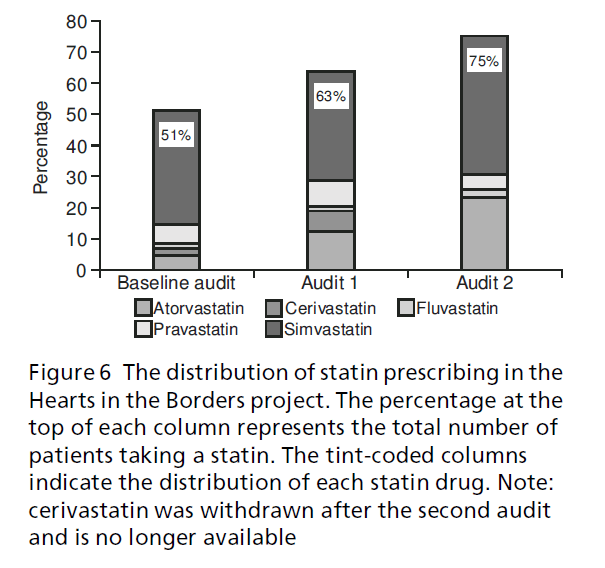
Figure 6:The distribution of statin prescribing in the Hearts in the Borders project. The percentage at the top of each column represents the total number of patients taking a statin. The tint-coded columns indicate the distribution of each statin drug. Note: cerivastatin was withdrawn after the second audit and is no longer available.
The number of patients within the target systolic blood pressure of below 140 mmHg increased from 43% (n = 428) at baseline to 49% (n = 565) by audit 1 and 55% (n = 679) by audit 2, showing an improving trend in patients within the target systolic blood pressure (see Figure 7). Target diastolic blood pressure showed a similar improving trend with 61% (n = 601) of patients with a diastolic blood pressure below the target of 85 mmHg at baseline increasing to 66% (n = 766) by audit 1 and 74% (n = 905) by audit 2 (see Figure 8).
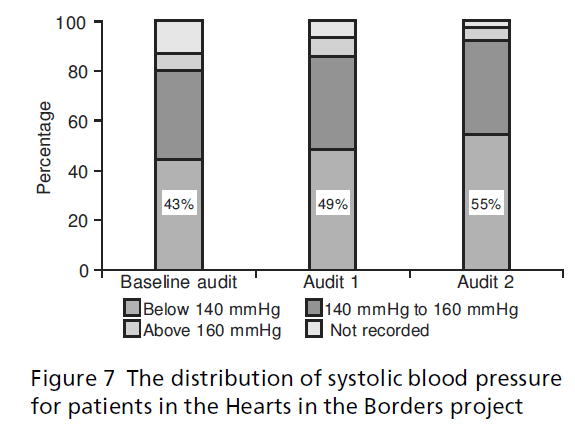
Figure 7:The distribution of systolic blood pressure for patients in the Hearts in the Borders project.
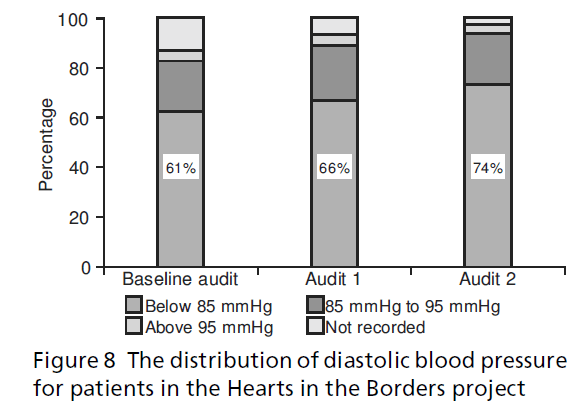
Figure 8:The distribution of diastolic blood pressure for patients in the Hearts in the Borders project.
In the baseline audit, aspirin prescription level was 87% (n = 862), increasing to 88% foraudit 1 (n = 1025) and remaining at 88% for audit 2 (n = 1085) (see Figure 9). In all the audits 5% of patients had a contraindication to aspirin use.
In the baseline audit 15% (n = 149) of patients had been admitted with a cardiac episode (see Figure 10). By audit 1, 12 months later, cardiac admissions had reduced to 11% (n = 132) and a further reduction to 10% (n = 124) was achieved by audit 2. The percentage of patients admitted to hospital for other reasons was reduced from 17% (n = 164) at baseline to 10% (n = 122) by audit 2. Overall, total admissions were reduced from 32% (n = 313) at baseline to 20% (n = 246) by audit 2.
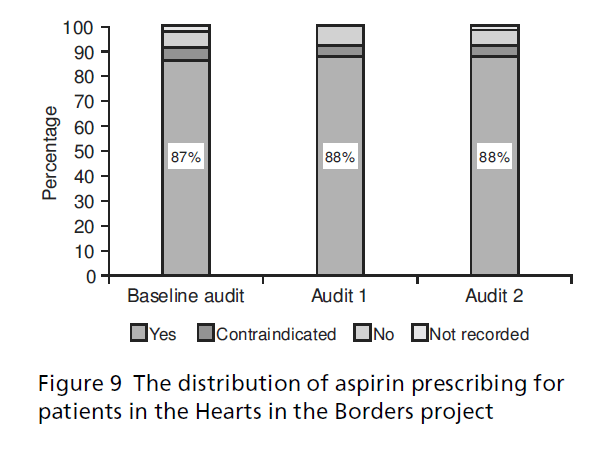
Figure 9:The distribution of aspirin prescribing for patients in the Hearts in the Borders project.
Major improvement occurred in cholesterol control: the proportion of patients with their cholesterol below 5 mmol/l, which was the target in the programme, increased from 29% to 62%. The main reason for this was the increase in statin treatment. Reducing choles-terol to this extent, by extrapolation from the 4S-study, suggests that over a five-year period in this population, 31–65 coronary events will be avoided, and 11–27 coronary deaths avoided or delayed.[1] Hospital admissions decreased from 15% to 10% for cardiac events while non-cardiac admissions for this group decreased from 17% to 10%. A reduction in acute admissions was also found in Campbell’s study and requires more investigation.[11,12] It suggests that disease management programmes in primary care can keep CHD patients out of hospital. This is a major benefit for patients and can generate considerable hospital savings. The local health board has recognised this success by allocating additional funds to the primary care prescribing budget for statins. The additional funding was important not only for bud-geting reasons, but as recognition for GPs that the local decision-making process re• ected the increasing costs of improving quality in primary care.
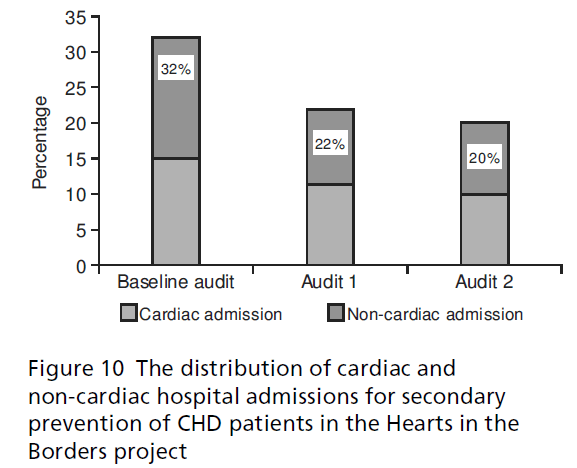
Figure 10:The distribution of cardiac and non-cardiac hospital admissions for secondary prevention of CHD patients in the Hearts in the Borders project.
However, the percentage of patients who had received dietary advice was relatively low at baseline. There can be two main reasons for this: dietary advice is not regarded as treatment and it is not recorded in the medical files, or it is not given to patients for the same reason. The e¡ect of dietary changes depends on the baseline diet and individual sensitivity to dietary changes. In spite of the huge number of studies done on blood cholesterol and diet, the original Key’s equation is still valid. Cholesterol decline depends mainly on the decline in saturated and increase in polyunsaturated fats following the formula: decline in cholesterol (mmol/l) = 0.0397 £ (2 £ decline in saturated fats as energy percent + increase in poly-unsaturated fats as energy percent). If we take a typical traditional western diet with 20% of energy intake in saturated fats and 5% of polyunsaturated fats, and change it to 8% of saturated and 8% of polyunsatu-rated, the serum cholesterol will decline by about 1 mmol/l.[13] However, there is a large variation in how individual people react to dietary changes. By the last audit with the large focus on lifestyle changes through training and the resource pack, ‘dietary advice given’ had risen to 90% and ‘exercise advice’ to 72%. This demonstrates the e¡ectiveness of a centrally driven approach. With the targeted training and resource pack, not only has the lifestyle advice given to patients improved but also the quality of the advice given (that is, it is up to date and evidenced based).
Aspirin is an evidence-based cost-e¡ective drug and prescribing was high in all three audits. Trends towards better control of blood pressure, both for systolic and diastolic pressure, were evident. The evidence suggests that lowering blood pressure and prescribing aspirin has a beneficial e¡ect in reducing cardiovascular events.[14]
There was no change with regard to smoking cessation despite the focus and resources allocated to this. This suggests that for patients who have not given up smoking following a myocardial episode, giving up smoking may prove more di¤cult. Introduction of practice-based smoking cessation support, with nico-tine replacement therapy or bupropion, could be the most important health intervention for these cardio-vascular patients. If CHD patients continue smoking, the risk of new infarction or graft occlusion is much higher compared with patients who quit smoking.[4] Following the last audit, new methods of helping this high-risk group of patients are being investigated.
One major positive e¡ect of the audits was that all practices now have a CHD register. Also new ways of working across professional and organisational divides, re• ected in the guideline, training pro-gramme and resource pack, were developed. Evidence alone seldom changes practice but recently we have understood better how to lead improvements.[15,16] The successful implementation of this project is due to the use of multiple approaches including system redesign, clinical leadership, evidence-based guidelines, audit and feedback, training, peer group e¡ects and prac-tical support for the participating practices including IT-based solutions. Lessons learnt have allowed more rapid planning of a project to implement hypertension guidelines throughout the region.
We are grateful to all 22 primary healthcare teams in the Scottish Borders, who participated in this project. The project was funded by grants from the Primary Care Development Fund of the Scottish Executive, Borders NHS Board and an educational grant from Bayer PLC.
None.