Research Paper - (2012) Volume 20, Issue 4
Professor, Centre for Research on Ageing, Curtin University, Australia
A McManus PhD MPH (Research)
Professor, Curtin Health Innovative Research Institute (CHIRI), Curtin University, Australia
J Comfort MIH
WA Centre for Health Promotion Research, Curtin University, Australia
R Freijah
WA Centre for Health Promotion Research, Curtin University, Australia
G Lovelock
GRAI (GLBTI Retirement Association Inc), Perth, Australia
M Hunter
GRAI (GLBTI Retirement Association Inc), Perth, Australia
M Tavener PhD
Research Centre for Gender, Health and Ageing, A WHO Collaborating Centre, University of Newcastle, NSW, Australia
Received date: 28 November 2011; Accepted date:1 May 2012
ObjectiveTo explore attitudes, knowledge and current practices of retirement and residential aged care providers in Western Australia towards accommodating older gay, lesbian, bisexual, transgender and intersex (GLBTI) individuals. GLBTI is used throughout as a general term to include people who are not exclusively heterosexual in identity, attraction and/or behaviour. MethodsPostal surveys were sent to 329 providers of accommodation to ask about their attitudes, knowledge and current practices towards older GLBTI people. Two focus groups were also held with managers of accommodation facilities and GLBTI community members. ResultsFew respondents reported having experience with any older GLBTI residents in their retirement or residential aged care facility. There was poor inclusion of GLBTI issues in policy frameworks, and limited understanding regarding same-sex law reforms. ConclusionOlder non-heterosexual people are often obscured within ageing population discourses, and conceal their identity for fear of discrimination. GLBTI-sensitive practices can help to facilitate the disclosure of sexual orientation and/or gender identity that may assist in meeting the unique needs of this group.
ageing, attitudes, homosexuality, long-term care, non-heterosexual, retirement needs
How this fits in with quality in primary care
This study highlights the importance of recognising the specific needs of minority groups within aged care facilities. It is essential that measures of quality in primary care include cross discipline training for all health professionals involved in the delivery of healthcare within the aged care sector.
What do we know?
The care needs of older GLBTI people are less likely to be recognised in residential aged care. The likelihood that they will discuss their care needs with health professionals and carers is influenced by previous experience around revealing their sexuality. They are a hidden population within residential facilities.
What does this paper add?
This study reveals a lack of understanding of the unique needs of older GLBTI people due to the general assumption of residential aged care providers that all clients are heterosexual. The study demonstrates that the care needs of GLBTI older adults may be different from other populations. It also reveals that there is little staff education to assist staff to communicate appropriately or to provide relevant and sensitive care. This study provides a strategy and tools to assist organisations to improve care outcomes for GLBTI older adults.
Australia’s future population growth, distribution and age structure is predicted to have significant impli-cations for long-term policy, particularly service pro-vision for health and aged care.[1] It is estimated that by 2051 between 23 and 25% of Australians will be aged 65 years and over, compared with 13% in 2007.[2] This includes individuals who identify themselves as gay, lesbian, bisexual, transgender and intersex (GLBTI).[1]
Older GLBTI people often remain ‘invisible’ from the general population, as they conceal their identity for fear of discrimination and retribution.[3–7] In ad-dition to other risks which older adults can face, such as loneliness, isolation, loss of autonomy and increas-ing dependence, older GLBTI individuals may experi-ence further psychosocial stressors.[8,9] These are usually associated with sexual orientation, disclosure, dis-crimination, lack of legal recognition, little if any protection of lifetime partnerships and limited op-portunities to meet other older GLBTI people.[8,10]
The proportion of older Australian GLBTI people aged 65 years and over is 6–8% of the general population and is expected to rise in line with national trends.[11,12] However, it is difficult to estimate accu-rately the proportion of the population who identify as GLBTI for a number of reasons. Although limited data are available on sexual identity in Australia,[13] the Australian 2006–2007 Census identified 27 000 same-sex couple families living in Australia during that period,[14] but cautioned that this figure was not rep-resentative of the GLBTI population overall.[14] The 2003 study Sex in Australia: Australian Study of Health and Relationships approximated that 97% of Australian males identified as heterosexual, 1.6% as homosexual and 0.9% as bisexual, and 98% of females identified as heterosexual, 0.8% as lesbian and 1.4% as bisexual.[12]
In comparison, the Kinsey Institute (USA) estimate that 10% of the USA adult male population identify as gay and 5–6% of the female population identify as lesbian.[11] Based on this, between 492 300 and 1.7 million people in Australia could identify as GLBTI ( 8% of older adults).
The fluidity of sexuality further complicates data collection as identity, attraction and behaviour arecomplex and changable; and there is not always con-sistency between the three.[11,12,15] Older GLBTI Aus-tralians grew up during a time when homosexuality was illegal and societal attitudes were generally ones of persecution, condemnation, hatred and discrimi-nation.[8] Homosexuality was commonly viewed as a ‘sickness, sin and disgrace’.[6] Consequently few GLBTI people openly disclosed their sexual orientation for fear of reprisal and/or prosecution.[6] As a result, growing older for many GLBTI people has meant increased fear of being ‘outed’ (to have sexual orien-tation and/or gender disclosed without consent) after a lifetime of avoiding disclosure of their sexuality, or fear of lack of understanding and support as they seek care. Of particular social and economic interest, is the potential impact GLBTI baby boomers will have in the future on the retirement and residential aged care industry. In addition to predictions of heightened consumer expectations,[16] this demographic is the first generation to be more open about their sexuality.[17]
Chamberlain and Robinson (2002) reported that many older GLBTI people felt particular discomfort disclosing their sexual or gender identity when util-ising the services of aged care organisations.[18] In turn, concealment of identity by older GLBTI people may result in service providers failing to address or meet their emotional and physical needs. The argument that GLBTI individuals have special needs is based on shared experiences of marginalisation and invisi-bility.[3,19,20] The situation is compounded further for older age GLBTI individuals, who have been living longer with the effects of homophobia, heteronor-mativity (the presumption and preferences of hetero-sexuality) and oppression.[18] Therefore, it is expected they may have some specific needs in older age that heterosexual individuals do not.
Barrett (2008) reported that the heteronormativity of retirement and residential aged care facilities is of concern to many older GLBTI people.[3] Heterosexual assumptions coupled with the notion of older people being asexual, can make GLBTI people feel that their same-sex relationships are not understood and that partners and GLBTI friends will be devalued during care planning and decision making.[21] In addition, Addis et al[22] reported that some older GLBTI people fear a lack of recognition and support of their ‘families of choice’ (usually friends rather than biological family members) from service providers. A monoculture often exists within the aged care sector in relation to sexual diversity which perpetuates the mantra that ‘we need to treat everyone the same’.[23]
Some older GLBTI people fear that going into residential aged care will render them socially and emotionally isolated from their communities: no longer able to mix with other GBLTI people, to access GLBTI services and activities or celebrate/attend special events and festivals.[9,18,24,25] Engaging older GLBTI residents in GLBTI community activities can be challenging due to their own identity concealment;[4] however, encour-aging GLBTI elders to remain connected to their GLBTI community is important as such social support can contribute to positive health outcomes.[26]
State and federal legislation guide the practices of residential aged care service providers. As such, prac-tices across the industry work within similar govern-ance frameworks. While there are good practices in some facilities, the providers of residential aged care are not a uniform group and consequently differences in practices and attitudes will exist. Generally speak-ing, Australian gerontology and the aged care industry operate within a heteronormative framework, dis-regarding diverse sexual orientations and sexual iden-tity.[27,28] Additionally, the aged care industry generally employs the notion that older people are asexual and that matters of sexuality are private.[29,30]
Heteronormativity assumes that heterosexual orien-tation and heterosexual perspectives are the norm and therefore disregards diverse sexual orientations and gender identity.[31] Current policy governing the aged care industry is framed in a heterosexual context and can unintentionally and indirectly marginalise and discriminate against GLBTI people.[21] This results from specific needs not being consciously considered by providers, as well as a lack of awareness of relevant GLBTI issues.[31]
Older GLBTI people are not considered as a specific needs group in the Aged Care Act which reinforces their invisibility and further marginalises them.[28] Admission and intake forms into residential aged care services often use heteronormative language such as: husband, wife, married, divorced and family.[21] Rarely do they provide an opportunity for individuals to declare same-sex partners, nor do they employ a broader definition of ‘next of kin’ to encompass ‘families of choice’ rather than biological families.[21] This is significant as visiting rights, access to client information and involvement in client decision making is determined by such information.[21] Furthermore, marketing material used by the aged care industry is also based on heteronormative assumptions with opposite-sex couples depicted on brochures, to the exclusion of same-sex couples.[28,31] Tolley and Ranzijn (2006) theorise that the aged care industry is not immune from heteronormative assumptions as staff working within this industry are likely to hold hetero-normative assumptions in line with the general popu-lation.[31] Consequently, older GLBTI people are not usually perceived by staff and service providers to have specific needs.
For the purposes of this study, the GLBTI popula-tion refers to diverse sexuality groups whose sexualities and/or gender identities fall outside the traditional heterosexual norm.[32] It is recognised that the GLBTI population is not homogeneous and that subpopu-lations and diversity exist. Other terminology used includes: queer, transsexual, gender queer, gender non-conforming and minority sexuality groups.[33] For the purposes of this study, the term GLBTI will be used as a representation of all subgroups within this target group. It is difficult to accurately estimate the proportion of the population who identify as GLBTI for a number of reasons. There are very little data being collected on sexual identity within current research.[13] Additionally, many GLBTI individuals may not feel comfortable identifying in a public arena due to fears of discrimination and homophobia. Consequently, the GLBTI population as a whole remains relatively invisible and un-numerated.
A more comprehensive literature review was compiled during this study and can be sourced from https://www.grai.org.au. The literature review was conducted to identify previous research undertaken in this area, ascertain a better understanding of the general and GLBTI ageing issues and establish lessons learned from previous findings. Additionally, the literature review aimed to build on the findings of other researchers, identify any gaps in the current knowledge and highlight the significance of historical context when researching GLBTI issues.
This project evolved from formative research conduc-ted by Curtin University and GLBTI Retirement Association Inc (GRAI) in 2006/07, which confirmed that unmet needs and fears of discrimination existed among older and ageing GLBTI individuals accessing retirement and residential aged care services in West-ern Australia. Consequently, this investigative study was undertaken to explore Western Australian resi-dential aged care service providers’ practices and attitudes towards older GLBTI individuals.
The study adopted a mixed methods approach. Mixed methods research is a research design with philosophical assumptions as well as methods of inquiry. As a methodology, it involves philosophical assumptions that guide the direction of the collection and analysis of data and the mixture of qualitative and quantitative approaches in many phases in the research process. As a method, it focuses on collecting, analys-ing, and mixing both quantitative and qualitative data in a single study or series of studies. Its central premise is that the use of quantitative and qualitative ap-proaches in combination provides a better under-standing of research problems than either approach alone.[34]
This study investigated attitudes, knowledge and practices of retirement and residential aged care pro-viders in the State of Western Australia (WA) in relation to older GLBTI people. It also sought to determine if providers viewed older GLBTI people as a specific needs group.
The study addressed the following research ques-tions:
• How well do existing retirement and residential aged care providers understand and currently meet the needs of GLBTI people?
• How can retirement and residential aged care providers become informed about the needs of GLBTI people?
Ethical approval was granted by the Curtin Uni-versity’s Ethics Committee (Perth, WA). The study involved a number of steps, outlined here.
Step 1: formation of project working groups
A project control group (PCG) was formed to guide and monitor the project, and to act as an interface between Curtin University and GRAI. The group comprised academic representatives from Curtin University’s WA Centre for Health Promotion Re-search (WACHPR) and Centre for Research on Ageing (CRA), a public health practitioner from Curtin University’s Curtin Health Innovation Research In-stitute, the project manager, the research officer and representatives from the GRAI board.
In addition to the PCG, an Industry Advisory Group (IAG) was established which comprised rep-resentatives from Carers WA, Aged Care Association Australia (WA), Council on the Ageing (WA), Retire-ment Villages Association (WA) and Aged and Community Services (WA). The IAG acted as an industry feedback mechanism to the PCG, contribu-ting to the research schedules, industry surveys, best practice guidelines for residential aged care providers and dissemination of the final project report.
Step 2: identification of study population
The target group for the study was all providers of retirement and residential aged care accommodation in Western Australia. A database of such providers was constructed from the Department of Health and Ageing’s database of Western Australian aged care service providers, the Centre for Research on Ageing’s database of retirement village providers, the DPS Guide to Aged Care: Western Australia (2008), the Telstra White Pages1 and the Aged Care On-Line website www.agedcareonline.com.au. The search in-cluded both independent entities (that is, the owner-operator organisations), and corporate entities (that is, corporate companies which govern multiple facili-ties). All providers on the list were eligible to receive the study survey.
Step 3: survey development and administration
The survey design for this study was informed by an extensive literature review of issues pertaining to:
(1) ageing GLBTI individuals and (2) aged care accommodation. A number of leading themes were
identified and developed into a survey format using key examples.[35–38] Members of the PCG and IAG reviewed the draft survey for readability and content validity. Members of the research team and a rep-resentative from the Aged Care Association Australia (WA) met to discuss the cognitive and motivational qualities of the survey.[39] Steps 1 and 3 resulted in a survey ready for pilot testing with a local residential aged care organisation.
Step 4: pilot testing
The pilot survey asked about: (1) staffing capacity and services provided (eight items); (2) length of personal service within the industry and position held (two items); (3) experiences of, and attitudes towards, accommodating GLBTI residents (eight items); (4) organisational policy regarding GLBTI residents (seven items); (5) current facility practices regarding GLBTI residents (five items); and (6) issues and challenges in accommodating GLBTI residents in the future (five items). There was also space provided for respondents to record general qualitative comments.
The survey was tested with the departmental man-agement team from Swan Care Group, one of the larger residential care providers in Perth, WA. The team comprised of managers from community care, independent living and the low and high care facilities. Pilot participants completed and returned the survey according to project protocols. In addition to general terminology and question order refinement, feedback from the pilot testing indicated that two separate surveys were necessary, instead of one.
An Executive Survey – which asked about organ-isational policy in terms of GLBTI residents as well as background information about the organis-ation; to be completed by the chief executive officer (CEO) of the organisation.
A Facility Survey – which asked about experiences, attitudes and future directions in terms of accom-modating GLBTI residents, to be completed by the senior manager of the facility at the operational level.
Owing to the complexity of the aged care industry, and upon advice from the IAG it was agreed that for large corporations with multiple facilities, initial consent would be sought from the CEO via a telephone call, while also checking the number of facilities under their jurisdiction. Upon receipt of verbal consent, each CEO was sent an Executive Survey and copies of the Facility Survey to distribute to their senior managers. For single independent entities, no initial telephone contact was required, and each CEO was sent the Executive Survey and Facility Survey directly. All surveys were accompanied by an information letter, consent form and self-addressed reply paid envelope (Figure 1).
Step 5: data collection
A modified Dillman protocol was used to guide the survey administration and follow-up process.[39] Two weeks after the initial mail out of both the Executive and Facility Surveys a thank you/reminder card was sent, with a follow-up letter sent another two weeks after that to all non-respondents. One week later a follow-up phone call was made to all non-responding CEOs of corporate organisations. Individual entities did not receive this call due to the large number of organisations (Figure 1).
Two focus groups were conducted after the surveys responses were analysed, to further explore key themes from the quantitative findings: issues of ‘we treat everybody the same’ and ‘sexuality is none of our business’, as well as perceptions of what constituted ‘best practice’ in the delivery of retirement and aged care accommodation for GLBTI people. The first focus group was planned with senior management of retirement and residential aged care facilities, who had indicated on their survey that they wished to partici-pate further. Respondents were invited via email and a follow-up phone call to confirm participation and focus group details. The second focus group was planned with members of the local GLBTI com-munity. Recruitment was through established GLBTI networks in Perth, including the gay media (Out in Perth newspaper) and an invitation sent to members of ‘Prime Timers’, a WA-based community organis-ation providing kinship for mature gay and bisexual men. In order to facilitate participation for this focus group a $20 shopping voucher was offered.
Step 6: data analysis
Quantitative data analysis was conducted using SPSS v. 17. The main features of the data were summarised descriptively, because the sample was not large enough to assess statistical significance. Area classification as metropolitan, rural and remote was according to the Australian Institute of Health and Welfare guidelines (2004). The focus groups were recorded and tran-scribed verbatim, then imported into Nvivo v. 8. Content analysis was undertaken by systematically reading the transcripts and assigning codes to the data. The raw data from the transcripts were examined for elements and phrases. These elements were then examined for common meanings which were com-bined into subthemes. Subthemes were then clustered to reveal broader themes that could be supported by examples from the raw data. This analysis was reviewed by the research team to ensure appropriate represen-tation of the data. This enabled the researchers to identify six overarching categories: (1) experiences with GLBTI residents, (2) challenges of accommodating GLBTI residents, (3) benefits of knowing resident’s sexual orientation and/or gender identity, (4) differ-entiating sexual activity from sexual orientation and/ or gender identity, (5) federal and state legislation and (6) size of the GBLTI population. Support for these findings is demonstrated with quotes from focus group participants throughout the qualitative results section of this report.
Quantitative data
The sampling frame comprised 431 facilities. From this, 149 (35%) were independent organisations and the remainder (n = 282, 65%) were governed by 36 corporate entities (that is 36 corporations governing multiple facilities). One hundred and eleven (of 282) facilities governed by 19 corporate entities requested not to participate in the study, during initial telephone contact. Therefore, 149 independent organisations were posted Facility Surveys and Executive Surveys, and corporate entities were sent 171 Facility Surveys plus 17 Executive Surveys. The number of Executive Surveys returned from corporate entities was 13 (of 17, 76%). The number of Executive Surveys returned from independent entities was 23 (of 149, 15%). The number of Facility Surveys returned was 83 (of 320, 26%). Descriptive comparisons between facility size, geographic location and service type revealed little difference in terms of attitudes and practices towards older GLBTI people.
Responder characteristics
Sixty-one Facility Survey respondents (73%) were from corporate governed facilities and 22 (26%) were from independent entities. The greater proportion of Executive Survey respondents were also from corpor-ate facilities (76%). Over half of respondents in general (53%) were from the Perth metropolitan area. The type of care service reported by most respondents was ‘low care’ (50%), with ‘dementia specific’ reported as being the least provided (10%). Over half were ‘not for profit’ organisations (n = 20, 56%), 33% (n = 12) were for profit, with the remainder being state govern-ment or local authorities (n = 4, 10%). The average number of years worked in the aged care sector was 13 years for responding CEOs and 12 years for facility managers.
Non-responder characteristics
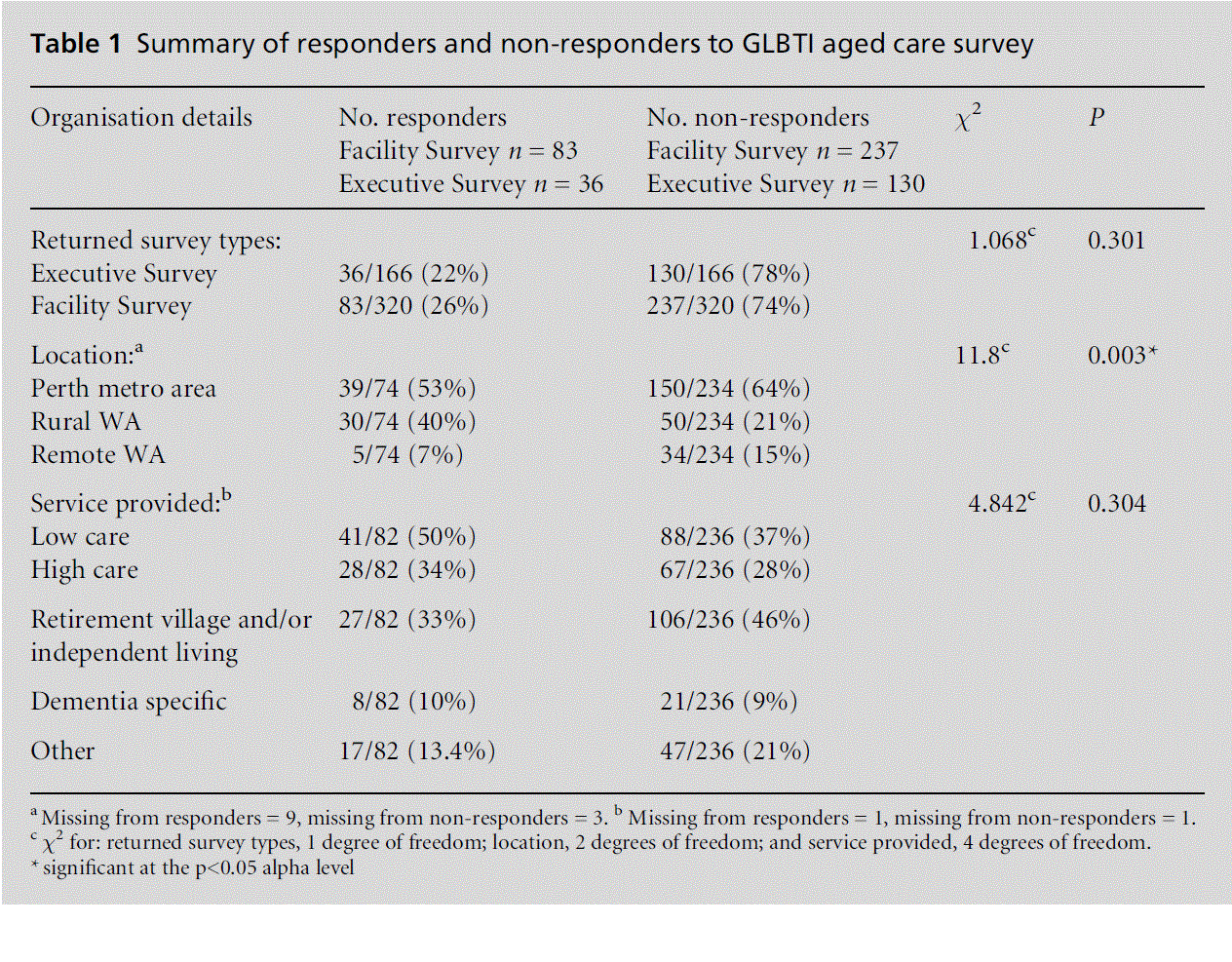
A comparison of responders and non-responders is given in Table 1. The majority of non-responders were from the Perth metropolitan area (n = 150, 64%), 50 (21%) facilities were from rural Western Australia and 34 (15%) were from remote Western Australia. Reasons for non-participation (where provided) in-cluded: not being interested, being a small facility and not accommodating GLBTI persons, not having enough time and being understaffed, and that partici-pation would go against the ‘ethos’ of organisation.
Experiences and attitudes towards GLBTI residents
The Facility Survey collected data relating to senior staff experiences and attitudes towards accommodat-ing GLBTI residents. Eighty-six percent (n = 71) of respondents were unaware of, or unsure about having, GLBTI residents within their facility. Fewer than one-third (n = 23, 30%) of respondents stated that their facility recognised GLBTI residents as having specific needs, and 79% (n = 63) agreed that a resident’s sexuality was not the concern of staff or management. Sixty-six percent of respondents (n = 55) felt that they provided a GLBTI-friendly and trusting environment in which they ‘treated everyone the same’, and 88% (n = 70) indicated that a resident’s right to beliefs and personal diversity were promoted within their facility’s policies and procedures. No facility reported provision of GLBTI-specific training for staff. Two respondents did indicate that they had provided staff training with regard to sexual needs of older people in general, but was not GLBTI-specific.
Organisational policy
The Executive Survey collected data pertaining to overarching organisational policy. Ninety-seven per-cent (n = 33) of respondents reported having an established complaints process for residents and the majority (n = 24, 77%) of respondents were aware that residents could lodge a complaint regarding discrimi-nation based on sexual orientation and/or gender identity. However, few respondents (n = 13, 37%) reported that organisational policy and procedures made specific reference to GLBTI people, and that issues of sexuality were dealt with under general equal opportunity and anti-discrimination policies. From the Facility Survey, 12% of respondents (n = 9) were aware of GLBTI State and/or Federal legislation being incorporated into their facility’s policy. When asked to specify such policies, three respondents referred to same-sex law reforms, which had received prominence nationally as they were enacted in 2009 (Department of Health and Ageing, 2009).
Current practices
The majority of respondents (n = 65, 83%) indicated that the data and information collection forms used by their facility did not allow a person to self-identify as GLBTI. Yet 28% (n = 23) of Facility Survey respon-dents indicated that they promoted a welcoming and accepting atmosphere for GLBTI people, including
treating everyone equally, employing gay and lesbian staff and ‘making everyone feel welcome’. However, few respondents (n = 4, 5%) reported that their facility had a nominated GLBTI support person (n = 5, 6%) and no facility reported having partnerships with GLBTI community organisations.
Future directions for accommodating GLBTI people
Whereas over half of the respondents (n = 48, 59%) did not perceive any challenges for staff when accom-modating GLBTI people, another 14% (n = 11) thought there would be some challenges for staff due to lack of knowledge and education of GLBTI issues, combined with their own personal attitudes and beliefs. Results were similar when asked about perceived challenges for other residents. Of the 59% who thought chal-lenges did exist, 19% (n = 15) cited personal attitudes and beliefs of other residents (not the staff) as the most likely cause.
When asked about training needs for staff, respon-dents agreed that the potential impact of staff beliefs and values in the delivery of care, and safeguarding GLBTI individuals from discrimination by other resi-dents were important topics for consideration. En-abling factors for the uptake of GLBTI sensitivity staff training included having organised sessions, qualified trainers, accessibility, funding and human resources. Barriers included limited funding, time and human resources, staff and residents’ attitudes and beliefs, accessibility and the fact that GLBTI training was considered ‘not applicable’ to their facility.
Focus group with facility managers
Of the 28 aged care organisational managers invited to take part in a focus group, three were able to attend: one CEO of a corporate entity that governed five facilities, one manager of an independent retirement village and one care manager of a corporate entity that governed 20 facilities. The focus group lasted for 90 minutes. Few interactions with known GLBTI clients were reported by group attendees, with two out of the three not having any experience with GLBTI staff and/ or residents. As one said:
In all my years of working in health I’ve never had someone ever say to me, I’m a lesbian female.
And another:
Lots of sexual issues between staff, between clients, be-tween clients and family and all sorts of things, but never non-heterosexual issues. (Respondent, independent living)
Client isolation was raised as one issue, as a result of clients feeling that they have to hide their sexual orientation and/or gender identity. Participants spoke of older GLBTI people coming into a smaller com-munity setting and no longer being able to keep their private lives totally private from other people, ultimately having to disclose more of themselves: ‘... they make a decision that they want to let people know about their sexuality or they decide not to let people know ...’ (Respondent, high/low care facility). All agreed that discrimination by other residents and members of staff was not a specific issue, as discrimi-nation for other reasons could occur ‘... you could equally have a problem with a staff member or a resident or somebody else in terms of prejudice or problems’ (Respondent, independent living).
Group knowledge of recent same-sex legislative changes was minimal. In terms of sexuality (in gen-eral), participants also spoke of sexuality not forming part of the aged care standards, nor any required assessment criteria, and therefore was not considered: ‘... it’s not captured anywhere ... so there may well be a lot of people within our facilities who have all sorts of different backgrounds that we just don’t know about’ (Respondent, low/high care facility). Focus group participants agreed that treating ‘everybody the same’ reflected a strong anti-discrimination and equal opportunity focus within the care sector. However, when a vignette about an older gay man who receives friends and GLBTI-community reading material was introduced as a strategy for inclusion, it brought about a discussion which centred around such literature being considered pornography and directed the dis-cussion away from social connectedness. This may suggest a need for a criteria of acceptable reading material for all residents plus education among staff about inclusivity.
Many competing priorities in the aged care sector meant that GLBTI individuals would need to be classified as a special needs/minority group before facilities could respond accordingly. For one person this meant seeing ‘... evidence of 5–15%’ of the population being GLBTI, so they ‘... suddenly become the biggest, the biggest minority group’ (Respondent, independent living). Participants believed that having a large older GLBTI population would justify inte-grating this issue into aged care training:
I think given the range and the level of training that currently aged care facilities have to do as a requirement I’d be honest and say I think that [GLBTI training] would be quite low down on the list of priorities. (Respondent, independent living)
Overall, there was agreement that for the aged care accommodation industry to be receptive to GLBTI-related issues, the training would have to be: well resourced, sympathetic to the limited resources avail-able to facilities, readily available and delivered exter-nally.
Focus group with GLBTI community members
There were three final participants from the GLBTI community: two lesbians and one gay male, and the session lasted for 90 minutes. Participants talked about their personal experiences with providers of residential high care accommodation only, which they perceived as institutionalised with regimented routines. Partici-pants viewed themselves as being able to self-fund their own aged care needs and unlikely to access formal aged care accommodation. There was a belief that if a person had the financial means, then they could ‘buy’ good care in later life, free from discrimination and prejudice:
We thought if we couldn’t find care we’re going to have to take care of ourselves. I mean we’ve got nurses and doctors [as friends] so we’re a group of professionals and we thought that we could build a little community ... and take care of ourselves. (Female participant)
The group acknowledged that not all GLBTI people had the same financial means to seek private care in older age, and some would have to rely on the public system. Said one:
... I have a son, all of his friends who know that we’re gay ...they’re going to be our carers and I’d like to think that they’ll take good care of us, without prejudice, without anybody actually having to tell them that they need to be nice to us.
Participants agreed strongly that the culturally diverse workforce which exists within the aged care sector could pose a challenge, should staff hold religious, political and/or cultural beliefs which sanction against individuals who identify as non-heterosexual. There was overall agreement that acceptance and integration of openly GLBTI people into retirement and residen-tial aged care accommodation was an evolving pro-cess, linked to society’s acceptance of GLBTI people in general:
How do we effect the change? And I don’t know whether we can ... but in the end I don’t know, I suppose ultimately it would lead to something but not in our lifetime, not as we know it. (Female participant)
Participants identified education, accreditation and compliance within the aged care industry as oppor-tunities for overcoming some of the issues. They believed that there had to be explicit legislation refer-ring to discriminatory practices based on sexual orientation and/or gender identity, which was linked to accreditation to ensure compliance. They agreed that specific best practice guidelines should form a necessary part of the process in educating the aged care sector of the needs of older GLBTI people, but recognised that ‘Just simple change in a hospital environment is extremely difficult, this is a huge change. It will take a long time and be extremely difficult’ (Male participant).
This research investigated the attitudes, knowledge and practices of retirement and residential aged care providers in the State of Western Australia (WA) in relation to older GLBTI people. A wide range of practices and attitudes was identified between the different accommodation providers, with only small acknowledgement given to GLBTI individuals as having specific needs with regard to older age accom-modation. The findings from this study confirm the formative work undertaken by Curtin University and GRAI[40] in addition to other national and international research findings.[4,23,30,41–43]
Older GLBTI people currently accessing retirement and residential aged care appear to be a hidden popu-lation, as demonstrated in this and other studies.[3,5–7]
Older GLBTI people may not feel comfortable or safe disclosing their gender identity and/or sexual orien-tation, potentially resulting in significant health issues that can manifest as stress, anxiety and depression. It may also have significant consequences if important health information that could affect the provision of care remains undisclosed, and thus untreated. As a consequence of non-disclosure, providers are not afforded the opportunity to encourage and support community connectedness and sexual expression, both of which can impact positively on overall well-being.[26] The majority of respondents who participated in this study did not have any organisational procedures for managing disclosure of sexual orientation and/or gender identity. Staff training should be available to provide skills to deal with such issues, ensuring that the person(s) are safe from discrimination by staff and other residents, their families and friends.
Heteronormativity and homophobia exist within the broad community and are therefore likely to exist in retirement and residential aged care facilities.[23,44] Additionally, there is a steady increase in the pro-portion of residential aged care workers born in countries other than Australia, from 25% in 2003 to 33% in 2007.[45] The aged care workforce has become very multicultural, with many personal carers from different countries being employed. Cultural diversity in the workforce presents opportunities for creativity and new ideas; however, it may also present additional challenges as a carer’s value system can help to shape their perception of residents’ language and behav-iours.[46] Additionally, perceptions, values and attitudes can impact on an individual’s level of comfort when dealing with issues of sexuality and in particular diverse sexuality groups.[44] It is likely that standards of care may be compromised should staff hold negative personal attitudes towards GLBTI people.[21]
Employing superior GLBTI-sensitive practices within aged care organisations requires a fundamental under-standing of diversity as well as knowledge of the potential impact of an individual’s past experiences of homophobia and social exclusion.[47,48] Older GBLTI people in general may not feel safe disclosing their sexual orientation and/or gender identity to aged care providers as a result of their past experiences of discrimination,[3] with some people fearful that homo-phobic attitudes within institutionalised aged care facilities will impact on the quality of care they receive.[11]
Organisational policy sets the benchmark for expected staff behaviours and practices,[47] and can work to minimise (or stop) unintentional and indirect mar-ginalisation and discrimination of GLBTI people.[21,31] Despite this, very few survey respondents’ policies and procedures made specific reference to GLBTI people in this study.
The low response rate by aged care organisations to the postal survey and focus group invitation needs to be acknowledged as a limiting factor in our ability to report fully the attitudes, knowledge and practices of WA aged care accommodation providers. Forty percent of corporate-run facilities declined to partici-pate during their initial phone call with research staff. Further, despite efforts to make the survey as brief and user-friendly as possible, and the inclusion of step-wise follow-up strategies, organisations returned only 15% of posted Executive Surveys and 25% of Facility Surveys to the project team. Those who returned their surveys were similar to non-responders in terms of their geographic location. However, a greater proportion of respondents were from corporate-governed facili-ties compared with non-responders, perhaps attribu-table to the fact that consent to participate in the study was sought at the CEO level and that one overarching consent from a corporate organisation resulted in the participation of multiple facilities.
Dillman suggested that surveying businesses and other organisations presents different challenges than individual and household surveys.[49] Additionally, the aged care industry itself is a difficult industry to access for research: reportedly under-resourced, extremely time poor, over surveyed and greatly regulated with significant reporting requirements. Consequently, re-sponding to an optional survey may have been a low priority for most facility managers. Also, the low response rate may be a direct result of the research topic itself. The aged care industry and perhaps much of the wider community generally do not perceive sexual activity and ageing as co-existing,[23] and do not perceive older GLBTI people as having specific needs. Consequently, the response rate for the current study may relate to issues of client sexuality representing a low priority for aged care providers.[23]
The current results indicated a divergence between services offered by aged care providers, and the unique needs and concerns of older GLBTI people, based on a postal survey and focus groups. In terms of providing a GLBTI-inclusive environment within retirement and residential aged care accommodation, our find-ings suggest that current practices may not be in keeping with practices and needs identified by GLBTI community members, GLBTI community groups and other research findings. Until wide recognition is paid to older GLBTI people as a minority group with specific needs, it may be that the needs of GLBTI people seeking supported accommodation as they age will remain unmet.
This study has clearly identified a need for further research. However, equally as important, it has ident-ified the need for staff education and translation of understanding that might come from such education into policy and practice. The next stage of this study will involve the implementation and evaluation of the principles and guidelines that were the outcome of this study in organisations commitment to improving practice.
Lotterywest Social Research Grant [10321/20080692]
Ethical approval was granted by the Curtin Uni-versity’s Ethics Committee (Perth, WA).
Not commissioned; externally peer reviewed.
None.
This work was supported by a Lotterywest Social Research Grant [10321/20080692] and initiated by Curtin University in collaboration with GRAI (GLBTI Retirement Association Inc.). The research team at Curtin University included investigators from WA Centre for Health Promotion Research, Centre for Research on Ageing and Curtin Health Innovation Research Institute. GRAI (GLBTI Retirement Associ-ation Inc.) membership refers to gay, lesbian, bisexual, transgender and intersex individuals and therefore, this language is used in this study.