Clinical Governance in Action - (2003) Volume 11, Issue 1
General Practitioner and RCGP Project Director for Drugs Training Programme, Royal College of General Practitioners, London, UK
Carol Limber MA RGN
Director, Practitioners with Special Interests, NatPaCT, NHS Modernisation Agency, London, UK
Accepted date: January 2003
The appointment of general practitioners with special interests (GPwSIs) is an important element of health service policy in the UK. Primary care organisations (PCOs) need a framework for addressing the quality and standards issues raisedby the design of new services delivered by GPwSIs. Important issues such as patient safety, accreditation, quality assurance, and maintaining competence are raised. This article suggests a framework that PCOs can use for addressing these concerns and ensuring that the clinical governance obligations of GPwSIs are discharged.
clinical governance, general practitioners with special clinical interest
The NHS Plan for modernising the health service in the United Kingdom first announced the creation of general practitioners with special interests (GPwSIs).[1] It was envisaged that up to 1000 GPs would be appointed with special interest in fields such as ear, nose and throat (ENT), and dermatology with a view to taking referrals from other GPs.[2,3] Subsequently the idea of nurses delivering specialist services has also been suggested. The generic title of practitioners with special clinical interest is increasingly used. While some primary care organisations (PCOs) have already established schemes, for example Bradford Primary Care Trust, many are still at a planning stage. Uncertainty about the process for appointment and approving GPwSIs is commonplace. As many PCOs in the UK are currently involved in designing services delivered by GPwSIs, in this article we consider the implications for clinical governance leads and directors of quality. The article suggests a quality framework for dealing with GPwSI issues.
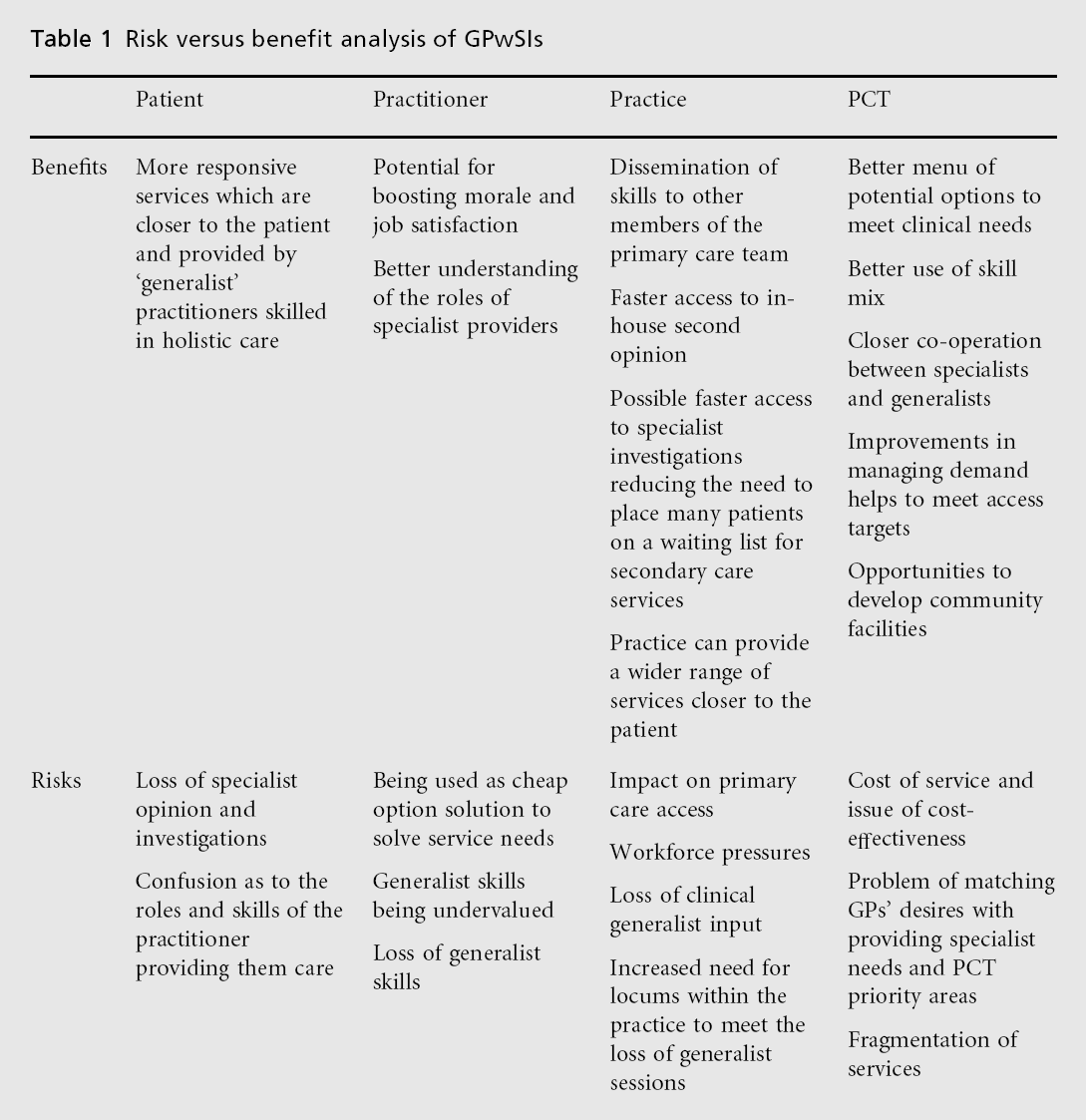
Box 1 shows the definition of a GPwSI, while Table 1 details a risk–benefit analysis.

General practitioners (GPs) with special clinical interest should be seen as one of a number of options available to a primary care trust (PCT) in designing services for their population.[4] A GPwSI is a doctor who, through undertaking specific training, is qualified and competent to provide not only the full range of generalist services but also those defined by the special interest service. In most circumstances a GPwSI will work in a community setting, though circumstances will exist where a GPwSI works entirely in an acute setting, for example a GPwSI in a hospital emergency care department or in a nonclinical setting such as a prison. Different service models will be developed according to local need though in all circumstances clinical accountability rests with the GPwSI who is responsible for his or her actions, including referral to specialist care and the need to work with other professional groups where appropriate. Overall accountability rests with the employing or contracting authority. Quintessential to being a GP is that doctors will work independently of direct supervision. This may include accepting referrals, making diagnosis, supervising or administering treatment and discharging from care or running a care programme for specific conditions. A GPwSI could be said to extend this means of working beyond the confines of their practice.
There are a number of aspects of the GPwSI quality framework. These are:
• establishing evidence of need
• obtaining stakeholder involvement
• developing the infrastructure for the service
• establishing the competencies for the service
• identifying a suitably qualified person.
Establishing evidence of need
The service needs to based on objective assessment of need taking into account national and local priorities, national service frameworks, waiting and access targets, value for money, assessment of clinical risk, regulatory requirements, staff capabilities, and met and unmet patient needs.
Obtaining stakeholder involvement
Ownership of the service needs to be not just at PCT board level but right down through the organisation to individual service providers. It is important that local specialist and secondary care providers are involved at the service planning stage; not only will this ensure that services are coordinated across the PCO but it will also serve to inform the specialists as to the overall aims and objectives of a GPwSI service (see Figure 1).
Developing the infrastructure for the service
This should involve defining the aims and objectives of the service, the core activities expected of the clinician – including the type of patients seen by the service, the interventions offered, conditions to be managed, severity, and case load as well as practical issues such as ensuring access to office space, secretarial and administrative staff, and arrangements for reviewing and maintaining equipment, etc.
It is important that there is local agreement as to the inclusion and exclusion criteria, type of patients seen, time to first appointment, and communication and follow-up arrangements.
Experience suggests that where co-operation has been achieved between primary and secondary care in these areas the GPwSI is able to offer a much enhanced service to patients by enabling faster access to investigations and waiting lists and to specialist opinion where this is required.
Establishing the competencies for the service
Establishing that the GP has the necessary skills, competencies and experience is most important in the genesis of a GPwSI service. The core competencies or skills and knowledge required must be based on the core activities needed, with the additional requirement that the clinician is first and foremost a competent generalist. On this latter point, the Royal College of General Practitioners (RCGP) recommends that a GPwSI has at least two years’ experience in general practice post Joint Certificate or Professional Training (General Practice) and ideally has MRCGP status or equivalent. In defining the competencies required for the special interest area the PCO (or employing authority) should take into account existing professional guidance, for example those that have been developed by primary care special interest groups, universities and Royal colleges and hence wherever possible these should be consulted and taken as a benchmark for local variation. In all cases local postgraduate primary care organisations together with specialist providers should be instrumental in determining these competencies and the evidence required to meet them.
Whatever the core competencies for the GPwSI these can be broadly be considered to fit into the areas shown in Box 2.

Identifying a suitably qualified practitioner
After defining the core skills, experience and knowledge necessary for the GPwSI, the next stage will involve identifying acceptable standards of accreditation for each special interest area. End-point exams, diplomas and certificates are not the only means of providing evidence of training and their use should only be justified where there is strong evidence that this is the only means of a GPwSI being able to demonstrate acquisition of the necessary skills for the service area. Presenting evidence of competencies is best done through a personal learning portfolio, which can form part of the practitioner’s future personal development plan. This portfolio can contain examples of experience (for example clinical attachments), skills (for example through direct observation, video) and knowledge (for example attendance at a bench marked course, certificate, completion of a logbook).
Figure 2 summarises the stages of the accreditation process.
Continuing professional development
Each GPwSI is expected to maintain their competency level and to keep a portfolio with evidence of this. The type and level of evidence will vary with each GPwSI area with options similar to those submitted as initial evidence for acquisition of core competencies. The RCGP recommends that a GPwSI undertakes a minimum of 15 hours per year of continuing professional development (CPD) in their special interest area.
Appraisal and revalidation
CPD should meet the requirements for revalidation and the appraisal mechanism needs to meet the approval of the PCO and needs to include appraisal of the GP’s generalist and special interest work, ideally as part of a single process using lay, peer and specialist appraisers.
Quality and monitoring framework
All clinical practice should be audited and evaluated to identify errors, ensure safety and raise standards. The methods used to assess the GPwSI care must be appropriate to the service defined and be resourced as part of the work specification. This should be a joint process carried out across the entire service to include secondary care practitioners, nurses and other professionals as appropriate.
The following clinical governance arrangements should be in place:
• quality framework (clinical audit standards, communication standards)
• risk management systems (signification event monitoring, complaint handling)
• quality assurance mechanism for the service
• accreditation framework
• accountability arrangements.
The RCGP together with the NHS Modernisation Agency is currently developing frameworks in a number of clinical areas together with guidance for PCOs in developing this service further.[3]
The development of GPs with special clinical interest is an exciting opportunity for GPs to develop their interests and widen their clinical horizons. However, it is important that PCOs and clinicians understand that if patient safety is not to be jeopardised, these services should be underpinned by robust clinical governance frameworks.