- (2014) Volume 15, Issue 4
Vasilis S Ramfidis1, Amanda Psyrri1, Kostas N Syrigos2, Muhammad Wasif Saif3
1Oncology Unit, Second Department of Medicine, Attikon University Hospital. Athens, Greece
2Oncology Unit, Third Department of Medicine, University of Athens, Sotiria General Hospital. Athens, Greece
3Department of Medicine and Cancer Center, Tufts Medical Center. Boston, MA, USA
Pancreatic cancer is a lethal disease and its prognosis remains dismal. The modest results of existing available treatments in the first line setting reveal the need of new therapeutic strategies. In this year’s American Society of Clinical Oncology (ASCO) Annual Meeting four remarkable studies were presented regarding this vulnerable group of patients. The efficacy and toxicity profile of gemcitabine plus erlotinib plus capecitabine (Abstract #4122), refametinib plus gemcitabine (Abstract #4025), gemcitabine plus docetaxel plus capecitabine plus cisplatin (Abstract #4135) were examined and the predictive value of a biomarker panel testing response to gemcitabine with or without the addition of erlotinib (Abstract #4133) was also presented.
Antineoplastic Agents; Drug Therapy; Pancreatic Neoplasms
Pancreatic cancer is a lethal disease and despite the progress that has been achieved the last years, its prognosis remains poor. More than 50% of patients have locally advanced or metastatic disease at the time of initial diagnosis and the five-year relative survival rate is approximately 2% [1, 2].
The therapeutic approach of patients with pancreatic adenocarcinoma in the first line setting is based in combination chemotherapy when Eastern Cooperative Oncology group (ECOG) performance status allows it. Results from the randomized phase III PRODIGE trial evaluating FOLFIRINOX versus gemcitabine showed significant superiority of the combination, but with considerable toxicity [3]. Gemcitabine-based combinations with albumin-bound paclitaxel, 5FU, erlotinib, capecitabine or cisplatin are also acceptable treatment options but clinical benefit remains modest [4-8].
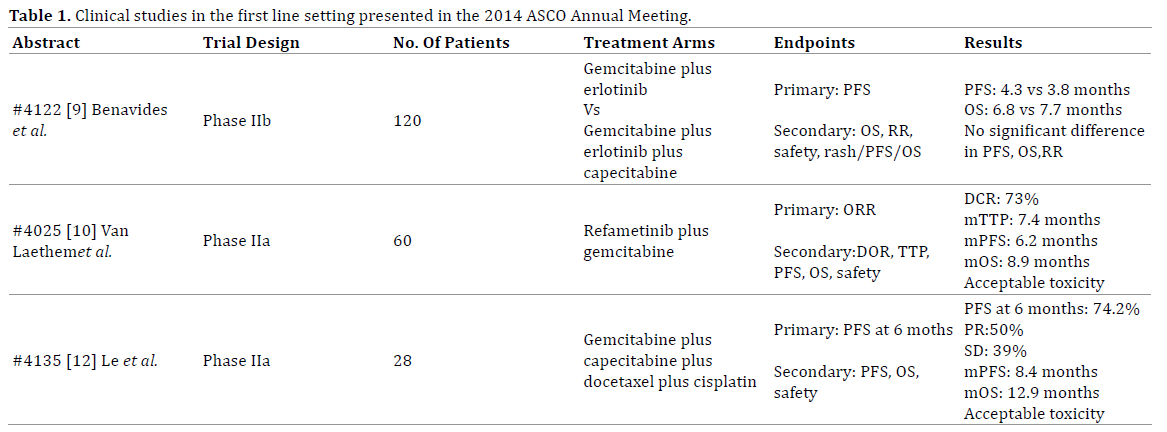
In this year’s ASCO Annual Meeting, four remarkable abstracts about advanced or metastatic pancreatic cancer were presented concerning first line treatment. The purpose of this paper is to dispose the data and the main findings of these studies as shown collectively in Table 1. The incorporation of the new data on a patient approach algorithm is illustrated in Figure 1.
Gemcitabine and Erlotinib plus Capecitabine in the First Line Setting
Benavides et al. (Abstract #4122) conducted a phase IIb randomized trial in the first line setting in chemonaïve patients with advanced or metastatic pancreatic adenocarcinoma [9]. The 120 enrolled patients were equally randomized to receive gemcitabine plus erlotinib or Gemcitabine plus Erlotinib plus Capecitabine. The primary endpoint was PFS and the study didn’t achieve to show statistically significant difference between the two arms. Concerning the secondary endpoints, overall survival (OS) and response rate (RR) also failed to show significant difference. Patients who experienced skin rash demonstrated better PFS and OS and toxicity profile was more severe in the triplet arm.
Refametinib (a MEK1/2 Inhibitor) plus Gemcitabine and Their Role in the First Line Setting
MEK has been suggested as pivotal pathway for malignant progression in pancreatic cancer [10]. Refametinib, an allosteric dual MEK1/2 inhibitor, seem to have a role in the management of pancreatic cancer according to a single-arm, open-label, phase IIa study by Van Laethem et al. A total of 60 patients were recruited and received both rafametinib and gemcitabine as first line treatment [11]. Best overall response was partial response in 35% and stable disease in 38%. Disease control rate (DCR) was 73%, time to progression (TTP) was 7.4 months, median PFS was 6.2 months and OS 8.9 months. The subgroup of KRAS wild type population has significant better ORR and longer median PFS and OS. The toxicity profile of the combination was acceptable and manageable.
Multi-Agent Chemotherapy with Four Drugs in The First Line Treatment
A single arm phase II study examined the clinical activity of four therapeutic regimens in the first line setting [12]. The 28 patients that participated in the trial received low dose of capecitabine, gemcitabine, docetaxel and cisplatin. The primary endpoint of PFS at 6 months was 74.2%. The median PFS was 8.4 months, the OS 12.9 months and the disease control rate (DCR) was 89% with manageable toxicity.
Predictive Value of a Biomarker Panel Testing Response to Gemcitabine With or Without the Addition of Erlotinib
The addition of erlotinib to gemcitabine has shown statistically significant benefit in OS. At the NCIC Clinical Trials Group PA.3 study plasma samples were examined before receiving either monotherapy with gemcitabine or gemcitabine plus erlotinib. The 483 available samples showed on one hand that lower levels of IL-8 were correlated with longer OS if treated only with gemcitabine and on the other patients with lower levels of IL-8, CEA and HIF-1 alpha seem to benefit more if receiving both gemcitabine and erlotinib [13].
Looking back few years ago, our therapeutic options in the first line setting in pancreatic cancer were limited. The recent years, clinical research revealed new treatment strategies that were added to our therapeutic quiver. Nevertheless, the prognosis of advanced or metastatic pancreatic cancer remains dismal and the need of newer more active approaches is imperative.
In this year ASCO Annual Meeting, two studies examined the efficacy of a triplet combination and a four-regimen combination. The first one of gemcitabine plus erlotinib plus capecitabine showed no significant clinical benefit compared to gemcitabine plus erlotinib alone. The second one examined the efficacy of capecitabine plus gemcitabine plus docetaxel plus cisplatin. Although it was a small trial, the results showed that this treatment strategy might be clinically active and these results remain to be examined in larger studies.
MEK pathway seems to play a role in carcinogenesis of pancreatic cancer but MEK inhibitors are still looking for their role in the therapeutic algorithm. Refametinib, a MEK 1/2 inhibitor, that was presented in this year ASCO Meeting in combination with gemcitabine showed remarkable clinical activity and especially in the subgroup with KRAS wild-type status. These results could help further the understanding of molecular biology of pancreatic cancer. Molecular alterations have not yet been elucidated in pancreatic cancer and these kinds of trials are useful research tools.
Finally, the development of drug strategies demands the presence of biomarkers with prognostic and predictive value. The last presenting abstract of this paper revealed the potential predictive value of plasma IL-8, CEA and HIF-1 alpha in patients that received gemcitabine plus erlotinib. Tailoring therapies to individual tumor and patient characteristics based on predictive biomarkers could change the therapeutic landscape of pancreatic cancer in the future.
The authors have no conflicts to disclose.