Key words
Breast cancer, South Asian, Psychosocial,
Indian, Gujarati, Non-English speaking
What is known about this subject?
• Breast cancer is one of the most common forms of cancer in all ethnic groups.
• Black and Minority Ethnic groups are under-represented in the psychosocial breast cancer literature.
• Potential participants who are not fluent in the English language are often excluded from research studies because of language barriers.
What this paper adds
• An in-depth understanding of the experience of breast cancer diagnosis and treatment amongst Gujarati-speaking Indian women with Limited English Proficiency (LEP).
• Qualitative evidence that highlights the importance of providing information in patients’ preferred language in order to
provide the best possible care and support for those with LEP.
• Support for previous research and policy calling for healthcare professionals to be aware of patients’ cultural and
language needs in order to provide them with culturally competent care and support.
Introduction
Breast cancer is the most common form of cancer in women
of all ethnic groups (Breast Cancer Care, 2005). In 2011, 49,936
women in the United Kingdom (UK) were diagnosed with the
disease (Cancer Research UK, 2014). UK data, albeit limited,
suggest that South Asian women have a lower incidence of breast
cancer than non-South Asian women (Farooq and Coleman,
2005; Zaman and Mangtani, 2007, Box 1). However, incidence
rates are higher amongst South Asian women living in the UK than those living in the Indian sub-continent (Jain, Mills and
Parikh-Patel, 2005). The incidence is expected to rise further
as Black and Minority Ethnic (BME) groups become more
acculturated and adopt Western lifestyles (Velikova et al, 2004).
Furthermore, data within the UK suggests that South Asian
women tend to be diagnosed at a younger age, at an advanced
stage of disease and with larger tumours than White women
(Farooq and Coleman, 2005; Velikova et al, 2004), and rates of
mastectomy are higher amongst South Asian women (Velikova
et al, 2004). These differences suggest that South Asian and White women’s breast cancer experiences may differ. However, research into the psychosocial impact of breast cancer has predominantly been conducted on White women and very little attention has been paid to those from BME groups, particularly South Asian women (Knobf, 2007; Thompson et al, 2008).
The existing, but limited, research conducted with South Asian breast cancer survivors has found that their experiences are influenced by socio-cultural norms, behaviours and beliefs (Balneaves et al, 2007; Banning et al, 2009; Bottorff et al, 2007; Howard, Bottorff, Balneaves and Grewal, 2007; Gurm et al, 2008). For example, Howard et al (2007) explored the experiences of 12 Canadian Punjabi women and highlighted their emotional reactions to their diagnosis, the impact the diagnosis had on their families, the importance of family support, the challenges associated with the stigma of the disease and the importance of religion in terms of beliefs and as a support mechanism. Another qualitative study with 20 Canadian Punjabi breast cancer survivors also found that participants’ experiences were shaped by their cultural background (Gurm et al, 2008). Many women wanted support from other breast cancer survivors but felt isolated because of cultural pressures to keep personal issues, such as ill-health, private. Their distress was further exacerbated by the judgemental and insensitive comments they often received from other community members, particularly those described as uneducated and older. Receiving information and talking to others in their own language was important to these women, as was spirituality and religion in helping them to manage their feelings about the situation.
Whilst these two studies contribute to the limited literature about BME women with breast cancer, both were conducted in Canada. It would be inappropriate to assume that the findings can be generalised to the UK, particularly as the healthcare systems in the two countries are not directly comparable; there may also be differences in culture and lifestyle (Farooq and Coleman, 2005). In addition, although Howard et al (2007) and Gurm et al (2008) provide valuable insight into the experiences of one specific BME sub-group their findings are not necessarily representative of other South Asian groups. There is considerable diversity between South Asian groups, for example, in terms of religion, language, cultural beliefs and traditions, even though they share similar ancestry (Ahmed and Lemkau, 2000).
Breast cancer research amongst the BME population in the UK is scarce (Banning, 2011). To date, only two UK-based studies have explored this phenomenon (Blows et al, 2009; Patel et al, 2014). Patel et al (2014) interviewed 22 Black and South Asian breast cancer survivors and highlighted the importance of social support, spirituality and body image concerns resulting from treatment. Women’s experiences were also influenced by socio-cultural norms and beliefs. Similarly, Blows et al (2009) conducted focus group interviews with 20 Black and South Asian women, and also described how social support, body image, and cultural influences, such as taboos about cancer, affected the women’s experiences. Furthermore, women expressed a preference for wanting to communicate with healthcare professionals and other breast cancer survivors in their mother-tongue. However a limitation of both these studies, and of most other research with BME groups, is that they excluded potential participants who were not proficient in the English language. These people are often excluded from research due to language barriers and practical reasons, such as the cost of and difficulty in using interpreters or validating questionnaires in other languages (Blows et al, 2009; Stirland et al, 2011). This is unfortunate as women with Limited English Proficiency (LEP) may encounter barriers to accessing healthcare services which can hinder their ability to communicate their concerns and health problems clearly, or lead them to avoid seeking medical advice entirely (Deepak, 2004).
Some American and Canadian studies have recognised this limitation and included women with LEP (Ashing et al, 2003; Bottorff et al, 2007; Howard et al, 2007; Gurm et al, 2008) but, to date, no UK based research has explored the experiences of breast cancer in women with LEP. It is important that groups with LEP are included in research so that their experiences are understood in order to guide healthcare professionals in providing culturally competent care and to help reduce inequalities in healthcare. The present study builds from the limitations of our previous study (Patel et al, 2014), and therefore aims to explore the experiences of one specific group of women with LEP, namely Gujarati-speaking Indian women, who had previously been diagnosed and treated for breast cancer (Box 2).
Method
Design
A qualitative approach based on phenomenological epistemology was used as this allows researchers to explore participants’ lived experiences in detail. Individual interviews were conducted, using a semi-structured interview schedule which was developed based on the existing breast cancer literature. Broad topics were used to encourage women to share
their experiences (table 1).
Table 1: Extract of Interview guide.
The study focused on Gujarati speaking Indian women with
LEP as this language is the lead researcher’s (GP-K) mothertongue.
However, her understanding of Gujarati is better than her
verbal skills and so she was assisted by a professional interpreter
who asked some of the questions during the interviews.
Interpreter
A professional female interpreter, with over 22 years’
experience, who was fluent in Gujarati and its various
dialects was employed to assist in this study. She also had an
understanding of health terminology and experience in dealing
with sensitive health issues. Before the interviews began, the
lead researcher (GP-K) met with the interpreter to discuss the
aims of the study and their respective roles during the interview
process. The interpreter’s role was to translate the researcher’s
questions to the participants, if necessary, since the researcher’s
understanding of Gujarati meant she was able to ask most
questions and understand participants’ replies. The interpreter
was also required to sign a confidentiality agreement form,
which stated she would not divulge any information to third
parties and would respect the confidentiality of the study at all
times.
Recruitment
All the women were recruited from the London region. Two
were recruited via the Asian Women’s Breast Cancer Group
(AWBCG). Support group facilitators announced recruitment
of participants for this study in their monthly meetings. Two
women expressed an interest and gave permission to the group
facilitators to forward their contact details to the researcher.
Another 3 participants were recruited via snowball sampling
(introduced to the researcher through Indian community events,
such as annual social gatherings). The researcher telephoned
each potential participant to explain the study in detail and to
arrange a suitable time and place to meet. These conversations
took place in Gujarati.
Sample
Five women agreed to take part. They were all first generation
immigrants and had been living in the UK for an average of
36 years. Three were from India and two from Kenya. Their
ages at the time of interview ranged from 55 to 76 years (mean
66 years). Age at initial diagnosis ranged from 29 to 69 years
(mean 51 years) and time since initial diagnosis ranged from
4 to 32 years (mean 15 years). All the women had a diagnosis
of primary breast cancer. Three had undergone a mastectomy and 2 had had a lumpectomy. Four had also undergone one or
more adjuvant therapies (chemotherapy (n = 1), radiotherapy
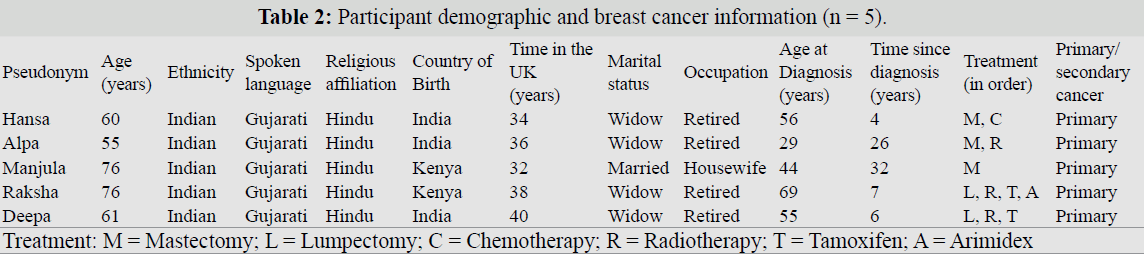
(n = 3), Tamoxifen (n = 2) and Arimidex (n = 1). See table 2 for a summary of the participants’ demographic and disease/
treatment-related information.
Procedure
Ethical approval was obtained from the School of Life
Sciences Research Ethics Committee at the University of the
West of England, Bristol.
At the beginning of each interview, participants were given
an information sheet to read and the consent form to complete.
The information sheet outlined the purpose of the research and
nature of participation in detail. Both the information sheet and
consent form were prepared in English. As many of the women
were unable to read in English or Gujarati, the interpreter verbally
went through the information sheet with them. It was for this
reason, that the information sheet was not translated into Gujarati
(and also due to the variation in dialects). On understanding
the information sheet, participants were given the opportunity
to ask any questions. They were reminded of the rationale of
the study and their right to withdraw. The confidentiality of
their responses was also emphasised. Once satisfied with the
information provided, participants were required to sign the
consent form before the interview commenced.
All the interviews were conducted in Gujarati, predominately
by the researcher, with assistance from the interpreter to relay
the interview questions, if necessary. Four interviews took place
in participants’ homes in London. The final interview took
place at the participant’s local library, in a private room. All the
interviews were audio-recorded and lasted between 55 and 74
minutes (mean = 67 minutes). On completion of the interview,
participants received a £20 gift card to thank them for sharing
their experiences.
Data Analysis
The interviews were translated and transcribed into English
by the researcher (GP-K) and checked for accuracy by the
interpreter. Any discrepancies in the translations were discussed
and amended accordingly.
Interpretative Phenomenological Analysis (IPA) was used to
analyse the data, using Smith and Osborn’s (2003) step-by-step
approach. IPA is ῾concerned with the detailed examination of
individual lived experience and how individuals make sense of
that experience’ (Eatough and Smith (2008) p179). This method
of analysis has become an established analytic method within
the realms of health psychology; particularly when exploring illness experiences such as cancer, chronic pain and heart disease (Smith, 2011) and is appropriate for use with a small sample size, ranging between 3 and 6 participants (Smith and Osborn, 2003).
Table 2: Participant demographic and breast cancer information (n = 5).
A qualitative software programme, QSR NVivo (version 9), was used to analyse and manage the data. Each transcript was read several times, noting interesting points in the left-hand margin. The right hand margin was then used to document emergent theme titles. This was then studied in detail, modified and further developed until a master list of themes was created. A final table consisting of themes and sub-themes was constructed. The interpretations were verified by an independent researcher (PV), who is familiar with researching populations drawn from BME groups and experienced in conducting IPA, to ensure the validity of the data (Reid et al, 2005). At this stage, the independent researcher was presented with three of the five transcripts (chosen at random) to study and check that the themes provided a clear and accurate account of the participants’ experiences. Any concerns were discussed but on the whole, the independent researcher was in full agreement of the initial interpretations.
Findings
IPA of the dataset captured the women’s experiences of breast cancer diagnosis and treatment through three main themes (with sub-themes emerging within each theme): 1) ‘Making sense of the cancer’, 2) ‘Importance of support’ and 3) ‘Body image concerns’. Each theme is described in detail below with extracts from the data and using pseudonyms throughout.
Making sense of the cancer
All the women described their experiences of breast cancer as being very difficult and distressing. For some, this was the first time they had heard the word ‘cancer’, which prompted feelings of shock and confusion. It was important for them to be able to understand the concept of cancer and make sense of it in order to accept and manage their experiences.
• Limited understanding
At the time of diagnosis, the women’s understanding and awareness of breast cancer was very limited. They were unaware that a lump can be serious and potentially related to cancer or that cancer symptoms can be asymptomatic. Ignoring symptoms resulted in a delayed diagnosis for Deepa and Raksha:
῾I found a lump. I just ignored it thinking it happens, you know.’(Deepa)
῾This [points below her armpit] became very hard and would hurt but I just thought it’s nothing so I didn’t do anything about it.’ (Raksha)
Some also stated that they were unaware of an illness such as cancer which can vary in type and affect different parts of the body. Throughout the diagnosis and treatment period, the women’s knowledge and understanding of breast cancer, and cancer in general, was increasing.
῾When I went for my treatment, that’s when I saw that SO MANY people get cancer. You see that some don’t have a right [breast], some don’t have a left [breast] and then you can get cancer anywhere can’t you? And there was purple marks on a man there. So I asked someone. I said “why does he have purple marks there”, and she said “because he has cancer there”. I was shocked seeing that, that day. Before that I thought I was the only one.’ (Alpa)
While Alpa’s understanding of her illness was increasing, she also felt that her limited ability to communicate in English hindered her ability to find out more or ask questions. This was a commonly held view amongst all the women.
῾At times you do want to know more but because you don’t know how to and can’t speak [in English], you just sit there quietly.’ (Alpa)
However, many of the women acknowledged that over time, this has become less of a problem as information in their mother-tongue is now readily available, prompting them to understand their illness more.
• Searching for answers
The unexpected diagnosis led the women to want to understand why and how they had developed cancer. For example, Deepa believed that breastfeeding reduces one’s risk of developing breast cancer and therefore was confused as to why she had developed the disease.
῾I felt like why has it happened? I don’t know. I have breastfed all my children and I still got it so I don’t know.’ (Deepa)
However, Manjula did not want to understand the cause and believed her diagnosis was out of her control. She accepted her diagnosis as part of her fate and attributed it to being God’s will. Some women also discussed their diagnosis in relation to karma, fate, and believed they had to endure the illness to make amends for bad deeds from their past lives. However, there were times when the treatments would get too much to bear, leaving some women temporarily feeling like the cancer was an act of punishment from God.
῾I just thought it was written for me, it was my fate.’ (Manjula)
῾What we have done in our past life will happen to us. It’s not God’s fault, it’s our doing.’ (Deepa)
῾At the beginning when I found out, I thought why me? Why did God choose me?’ (Alpa)
Importance of support
As the women told their stories, it became evident that support, particularly from their family members, was very important in helping them get through their experiences of diagnosis and treatment.
• Sources of support
Family members, particularly immediate family, were described as providing practical support such as taking participants to hospital appointments, helping with household chores, assisting with tasks such as bathing or brushing their hair, which the women found difficult after surgery, and caring for other family members.
῾He [husband] would do all the house work. And when I had
my operation, my son had an operation on the tonsils. So he
was in hospital, I was in hospital and my eldest son would go
to school. And my husband would go work, drop him to school,
then come to see me and then go see the other son. So my
husband was very supportive. He would cook for me too’ (Alpa)
Hansa had very little family around to support her, yet
still felt well supported as she reached out to her friends and
community members.
῾I didn’t feel alone. [Friend] was always with me. She used
to visit me every day.’ (Hansa)
Participants described how faith in God was an important
source of support and engaging in religious activities, such as
praying, helped them. While some women accepted their illness
as being God’s will, they also believed that God would give
them strength and help them to overcome it.
῾Even though God gave me this cancer but along with that he
sent me very good treatment and support and gave me strength
that I needed to get over it.’ (Manjula)
Healthcare professionals were also described as supportive,
with nurses providing women with emotional support,
reassurance and encouragement throughout the cancer journey.
῾I was shattered and the nurse came and gave me
encouragement and consoled me.’ (Manjula)
• Being dependent on others
All of the women who took part in this study were very
limited in their ability to understand and communicate in English.
For this reason, they relied heavily on others (typically family
members) to accompany them to hospital appointments and act
as interpreters. This often meant that healthcare professionals
would communicate with the family members instead of talking
directly to the patient, expecting the family member to pass the
information on.
῾They would explain everything to [niece], not me. But they
did explain things to her.’ (Hansa)
To some extent this enabled some women to feel involved
in consultations and informed at each stage but others
acknowledged that relying on family members to translate
information meant they might not always get a detailed
understanding and that information could be lost in translation
if, for example, family members or children were unable to
fully understand all the information themselves. Nonetheless,
women preferred to rely on family members or close friends
who they knew and felt comfortable with, rather than relying on
professional interpreters.
῾I can’t understand English well or read it and when you ask
them [children], they read it once and tell you the main things
but kids don’t explain everything in detail do they?’ (Deepa)
While Raksha, Deepa and Manjula relied on fluent Englishspeaking
family members to interpret information, Alpa and
Hansa depended on people who did not speak the language very
well. This did not concern Alpa or Hansa because, even though
their interpreters spoke only basic English, they still felt that
they still understood the main information.
῾I wouldn’t understand much but my husband would. His
English wasn’t good but it was better than mine.’ (Alpa)
Although the women in this study had had to rely on others
to help them overcome language barriers, some voiced their
concerns about burdening others with their problems as it often
meant family members would need to take time off from work
in order to be present.
῾Someone would always be with me but I did think that it
would be nice if I knew it [English] then it’s better, then you
wouldn’t have to waste her [daughter-in-law] time but I can’t
communicate everything’ (Raksha)
While some women felt they had no choice but to rely on their
family members, others tried to avoid inconveniencing them
by attending hospital appointments alone and ‘getting by’ with
their limited grasp of English. This limited their understanding
of the information they received and also prohibited them from
asking for further advice and information. For example, when
asking Deepa if the hospital staff had given her information
about financial support that she might be eligible to receive, she
replied by saying:
῾They may have but I don’t understand English too well.’
῾I would just guess what they are saying. Even now I go to
the hospital on my own and some things I don’t understand but
I guess as to what they may be saying.’ (Deepa)
Relying on family members and other people to act as
interpreters also meant that treatment decisions were often
made as a family. In these circumstances the family helped the
women to make decisions about the best treatment for them.
In many cases, the women were satisfied with this format as
they felt they had been informed and involved in the decision
making process and ultimately placed greater trust in literate
and educated family members.
῾They [daughter] would still understand that little bit more
than me as they have grown up here [UK]. So she said to me
“Mummy what’s the point in taking it all out”. They [consultant]
did say that it will take a couple of years for it to fill but after that
it will be normal whereas if you do the other [mastectomy], then
you could get an artificial one [reconstruction]. So my daughter
said rather than do the artificial thing, it’s better to have some of
your breast. So I said okay we’ll do it that way.’ (Deepa)
Body image concerns
• Effects of treatment
The extent and nature of appearance-related concerns were
dependent on the type of treatments that women underwent and
the side effects they had experienced. Three had undergone a
mastectomy and these women spoke of the impact this had on
their body image. For example, Manjula felt that she had lost
an important part of her body, and no longer felt balanced or
‘whole’, which resulted in not feeling feminine enough. Some
women also expressed feeling body conscious, especially when
going out in public and, as a result, limited their social activities.
Women felt that wearing a breast prosthesis helped them to
overcome their body image concerns and helped them to regain
their body shape. Such feelings were more prominent during
the time the women underwent their treatments. However, over time and as the women accepted their altered appearance, these feelings became less of an issue.
῾Initially I did feel like less of a woman but now it’s all forgotten, it’s in the past.’ (Manjula)
῾At the beginning it was all new but now I go swimming, sauna, everywhere. I don’t even put a pad [prosthesis] in either. I don’t feel like I will be embarrassed or anything like that.’ (Alpa)
Hansa was the only participant who received chemotherapy treatment and concerns about losing her hair were evident as she took measures to avoid hair loss by wearing a cold cap to cool the scalp in order to prevent or minimise hair loss. She also dealt with this issue positively by reassuring herself that the hair loss would be temporary.
῾There’s no use in worrying. If they [hair] go they go, if they stay they stay [laughs].’ (Hansa)
• Importance on being alive
All the women underwent changes to their appearance of some kind or another as a result of treatment, but Deepa and Raksha were not particularly concerned by the changes they experienced. Instead, they placed greater emphasis on their health and being alive. They also felt that due to their age, appearance issues were not so important. They believed they were less bothered by the changes than younger women would be, as these women likely to be more invested in their appearance.
῾I'm not …into my body…yeah I am into my body as in it should work properly, or walk or get you to places.’ (Deepa)
῾I’m not too bothered. Younger people would feel it more.’ (Raksha)
Discussion
This study has offered an insight into the experiences of Gujarati-speaking Indian breast cancer survivors living in the UK. The findings of the study show the importance of social support, body image concerns, cultural beliefs and the need for an awareness and understanding of breast cancer. These findings support previous studies that have explored the experiences of South Asian women (both English speaking and those with LEP) who have been diagnosed and treated for the disease (Bottorff et al, 2007; Howard et al, 2007; Gurm et al, 2008; Blows et al, 2009; Patel et al, 2014). The findings also concur with the results of research involving breast cancer survivors from other BME groups (Ashing-giwa et al, 2004; Blows et al, 2009; Patel et al, 2014). Furthermore, the present study particularly captures women’s experiences from a cultural perspective, specifically in relation to language.
The women in this study had very little knowledge of cancer before receiving their own diagnosis. There is evidence of a lack of knowledge and awareness about breast cancer amongst White and other BME populations (Dein, 2004) but women with LEP are even less likely to know about this disease (Bottorff et al, 2007; Howard et al, 2007). An additional factor is that, despite living in the UK for most of their lives, first generation immigrants maintain strong cultural beliefs and practices from their country of origin, and do not socialise with members outside of their community (Meneses and Yarbro, 2007). This can be especially true for those with LEP and can result in people associating with other people whose knowledge about cancer is inaccurate or limited. This can possibly explain why the women in the present study had very little knowledge of breast cancer. Lack of knowledge about cancer may also be linked to cultural taboos and stigma which result in an avoidance of open discussion about the disease (Scanlon and Wood, 2005). It is also possible that the limited availability of information and educational materials about breast health and cancer in languages other than English contributed to the women’s limited knowledge and understanding of breast cancer, particularly at the time when the women in this study were diagnosed.
Our study also emphasises the impact that language barriers can have on women’s experiences of breast cancer. Their inability or lack of confidence in communicating in English appears to have contributed to a limited understanding of their condition and resulted in them being unable to gain the full extent of information and emotional support potentially available from healthcare professionals. Language barriers appear to have resulted in many women adopting a passive role in consultations. Other studies have reported that patients with LEP value the importance of shared language in communicating with health professionals. They also benefit from receiving printed information in their own language to aid their understanding of their condition (Kumar et al, 2004; Gurm et al, 2008; Blows et al, 2009).
The present study highlights the importance of family, both as a source of support and to help overcome language barriers, with family members acting as interpreters during health consultations. It is interesting to note that only one woman in our study was aware that professional interpreters could be requested, and she discovered this after she had been diagnosed and treated. It could be that professional interpreter services were less readily available at the time the women in our study were treated. Alternatively, health professionals may not have been aware of the need for interpreters or how to access such services. The provision of interpreter services has improved in recent times; guidelines and policy documents now explicitly recommend the use of interpreters in addressing the healthcare needs of patients with LEP, and also provide information on how to access interpreters (Department of Health, 2004; NICE, 2004; NHS Health Scotland, 2008; Pankhania, 2011). While patients often prefer to use family members as interpreters (Grewal et al, 2005) and healthcare professionals also rely on family members to take on this role (Gerrish, Chau, Sobowale and Birks, 2004), there is a danger that family members may not always relay information accurately between patients and health professionals. This is especially true for family members who themselves are not entirely fluent in English but who may be the only ones available to translate the information.
The breast cancer literature has consistently reported the negative impact of treatment on women’s body image, regardless of ethnicity (Ashing-Giwa et al, 2004; Helms et al, 2008; Russell et al, 2008; Patel et al, 2014). Whilst the women in the current study expressed appearance-related concerns, an emphasis on being alive and regaining health was also embedded in their stories. Factors such as age may help to explain this finding as
some women expressed the view that younger women may be
affected more than they had been themselves. Previous research
has reported that while breast cancer is distressing for women
at any age, it tends to have a greater adverse impact on younger
women (Avis, Crawford and Manuel, 2004; Baucom et al, 2006;
Bloom et al, 2012).
Methodological considerations
All the participants in this study were Gujarati-speaking
Indian women, which allowed the researcher to personally
conduct the interviews with support from an interpreter; this
facilitated a detailed and natural conversation. Previous research
has highlighted the potential complications of a heavy reliance
on an interpreter, including the level of accuracy in relaying
questions and responses (Farooq and Fear, 2003; Flores et al,
2003; Pitchforth and van Teijlingen, 2005; Flores, 2005). This
issue of accuracy was also evident in the current study but was
detected due to the researcher’s understanding of Gujarati.
For example, in the first interview, one of the questions to be
translated to the participant was “How were you told about
the cancer”. The interpreter reworded the question and added
a question of her own, saying “How did they [healthcare
professionals] tell you? Did they tell you straightaway?” This
resulted in the participant responding to the latter question and
replied by saying “Yes they told me straightaway”. It was due
to the researcher’s (GP-K) understanding of the language that
allowed her to detect such inaccuracies. This happened on a few
occasions during the first interview. These errors were discussed
with the interpreter after the first interview and it was stressed
that the researcher’s questions be translated as accurately as
possible for subsequent interviews.
Members of South Asian and other BME communities
are often excluded in research, especially if they have LEP
(Stirland et al, 2011). The researcher’s South Asian background
and ability to speak in Gujarati may have helped recruit
participants for this study. Other non-Gujarati speaking South
Asian communities were excluded from the sampling process
and their experiences require investigation. The women were all
recruited from the London area and therefore the findings may
not be representative of South Asian breast cancer survivors
with LEP across the UK.
Implications
These findings have implications for healthcare professionals
wishing to provide culturally appropriate care and support to
South Asian women with breast cancer. It is important that
patients with LEP are provided with detailed information in their
own language, together with an opportunity to ask questions,
in order to facilitate an understanding of their diagnosis and
treatment. It is also possible that women whose first language
is not English yet have a fluent understanding of the English
language may also find this useful and prefer to receive
information in their mother-tongue. Healthcare professionals
should also be aware that not everyone, particularly first
generation immigrants, can read or write in their own language
(as was the case in the present study). Ideally, information
should also be available using other media such as audiotapes,
CDs, DVDs or videos. These have been reported to be beneficial in overcoming literacy barriers and deemed an effective mode
of delivering information to patients with LEP (Husson et al,
2010).
It is important to acknowledge that the women in this study
were diagnosed and treated for cancer some time ago. Information
about breast cancer is now readily available in many South Asian
languages (Macmillan Cancer Support, 2014). Furthermore,
Macmillan have set up the first national interpreting telephone
cancer helpline service, which is available in over 200 languages.
The provision of interpreters during consultations can encourage
effective communication between the patient and healthcare
professionals, and enhance the patient’s understanding and
knowledge of health related issues (Szczepura, 2005). It is
important to note that the onus for effective communication
need not be entirely on health professionals; they may not
know that patients lack fluency in English until they arrive at
the consultation. Interpreters need to be booked in advance and
patients should inform healthcare professionals that they need an
interpreter. However, in our study, several women were unaware
of the potential for such services to be provided. Barron et al,
(2010) noted in their study that participants from BME groups
were also unaware that healthcare professionals could access
interpreting services during medical appointments if requested.
This problem could be overcome if the patient’s language ability
and need for an interpreter were to be assessed at the point of
referral. It would also be useful for GPs to inform patients of
the availability of interpreter services in secondary care settings
should the patient need them.
Conclusion
This is, to the best of our knowledge, the first UK-based
study to explore breast cancer diagnosis and treatment amongst
Gujarati-speaking Indian women who have limited proficiency
in English. The results offer insights into the psychosocial
impact of breast cancer in Indian women with LEP, specifically
from a cultural perspective. The study adds to the existing
BME and breast cancer literature and offers valuable pointers
to improve effective communication between patients and
healthcare professionals. Future studies should continue to
explore the psychosocial impact of breast cancer amongst
BME women, paying particular attention to other non-English
speaking groups.
ACKNOWLEDGEMENTS
This research was funded by a Breast Cancer Campaign
PhD studentship; grant reference 2007NovPhD12. We also
wish to thank Asian Women’s Breast Cancer Group for their
help with recruitment and, most importantly, the women who
shared their experiences with us. A final thank you to Preeya
Vara (PV), independent researcher, for her assistance in the
analysis process.
CONFLICT OF INTERESTS
None
References
- Ahmed SM and Lemkau JP (2000) Cultural issues in the primary care of South Asians. Journal of Immigrant Health 2 (2):89-96.
- Ashing KT, Padilla G, Tejero J et al, (2003) Understanding the breast cancer experience of Asian American women. Psycho-Oncology 12(1):38-58.
- Ashing-Giwa KT, Padilla GV, Tejero JS et al, (2004) Understanding the breast cancer experience of women: A qualitative study of African American, Asian American, Latina and Caucasian cancer survivors. Psycho-Oncology 13:408-428.
- Avis NE, Crawford S and Manuel J (2004) Psychosocial problems among younger women with breast cancer. Psycho-oncology 13:295-308.
- Balneaves LG, Bottorff JL, Grewal SK et al, (2007) Family support of immigrant Punjabi women with breast cancer. Family and Community Health 30(1):16-28.
- Banning M (2011) Black women and breast health: A review of the literature. European Journal of Oncology Nursing 15:16-22.
- Banning M, Hafeez H, Faisal S et al, (2009) The impact of culture and sociological and psychological issues on Muslim patients with breast cancer in Pakistan. Cancer Nursing 32(4):317-324.
- Barron DS, Holterman C, Shipster P et al, (2010) Seen but not heard ÃÆÃâÃââÃÆââ¬Å¡Ã¢ââ¬Å¡Ã¬ÃÆââ¬Å¡Ã¢ââ¬Ã
â ethnic minoritiesÃÆÃâÃââÃÆââ¬Å¡Ã¢ââ¬Å¡Ã¬ÃÆââ¬Å¡Ã¢ââ¬Å¾Ã¢ views of primary health care interpreting provision: A focus group study. Primary Health Care Research and Development 11:132-141.
- Baucom DH, Porter LS, Kirby JS et al, (2006) Psychosocial issues confronting young women with breast cancer. Breast Disease 23:103-113.
- Bhopal R (2007) Ethnicity, Race, and health in multicultural societies. New York: Oxford University Press.
- Bloom JR, Stewart SL, Oakley-Girvan I et al, (2012) Quality of life of younger breast cancer survivors: persistence of problems and sense of well-being. Psycho-Oncology 21:655-665.
- Blows E, Scanlon K, Hatfield J et al, (2009) The Better Access Better Services (BABS) Project. Accessing information and support from the NHS and voluntary sector: Experiences of Asian and African Caribbean women with breast cancer.
- Bottorff JL, Grewal S, Balneaves LG et al, (2007) Punjabi womenÃÆÃâÃââÃÆââ¬Å¡Ã¢ââ¬Å¡Ã¬ÃÆââ¬Å¡Ã¢ââ¬Å¾Ã¢s stories of breast cancer symptoms: Gulti (lumps), bumps and darad (pain). Cancer Nursing 30(4):36-45.
- Breast Cancer Care (2005) Same difference: Breast awareness is for everyone.
- Cancer Research UK (2014) Breast cancer statistics.
- Deepak N (2004) Beyond the barriers providing cancer information and support for Black and Minority Ethnic communities. London: Cancer BACUP.
- Dein S (2004) Explanatory models of and attitudes towards cancer in different cultures. The Lancet Oncology 5:119- 124.
- Department of Health (2004) Guidance on Developing Local Communication Support Services and Strategies. The Department of Health Equality and Human Rights Group. London: Department of Health.
- Eatough V and Smith JA (2008) Interpretative Phenomenological Analysis. In: C Willig and W Stainton- Rogers (Eds.) The Sage Handbook of Qualitative Research in Psychology (pp. 179-194). London: Sage.
- Farooq S and Coleman MP (2005) Breast cancer survival in South Asian women in England and Wales. Journal of Epidemiology and Community Health 59:402-406.
- Farooq S and Fear C (2003) Working through interpreters. Advances in Psychiatric Treatment 9:104-109.
- Flores G (2005) The impact of medical interpreter services on the quality of care: A systematic review. Medical Care Research and Review 63 (3):255-299.
- Flores G, Laws MB, Mayo SJ et al, (2003) Errors in medical interpretation and their potential clinical consequences in pediatric encounters. Pediatrics 111:6-14.
- Gerrish K, Chau R, Sobowale A et al, (2004) Bridging the language barrier: the use of interpreters in primary care nursing. Health and Social Care in the Community 12 (5):407-13.
- Grewal S, Bottorff JL and Hilton BA (2005) The influence of family on immigrant South Asian womenÃÆÃâÃââÃÆââ¬Å¡Ã¢ââ¬Å¡Ã¬ÃÆââ¬Å¡Ã¢ââ¬Å¾Ã¢s health. Journal of Family Nursing 11(3):242-263.
- Gurm KB, Stephen J, MacKenzie G et al, (2008) Understanding Canadian Punjabi-speaking South Asian womenÃÆÃâÃââÃÆââ¬Å¡Ã¢ââ¬Å¡Ã¬ÃÆââ¬Å¡Ã¢ââ¬Å¾Ã¢s experience of breast cancer: A qualitative study. International Journal of Nursing Studies 45:266-276.
- Helms RL, O'Hea EL and Corso M (2008) Body image issues in women with breast cancer. Psychology, Health and Medicine 13 (3): 313-325.
- Howard AF, Bottorff JL, Balneaves LG et al, (2007) Punjabi immigrant women's breast cancer stories. Journal of Immigrant and Minority Health 9(4):269-279.
- Husson D, Mols F and van de Poll-Franse LV (2010) The relation between information provision and health-related quality of life, anxiety and depression among Cancer survivors: A systematic review. Annals of Oncology [online] doi: 10.1093/annonc/mdq413.
- Jain RV, Mills PK and Parikh-Patel A (2005) Cancer incidence in the South Asian population of California, 1988 - 2000. Journal of Carcinogensis 4:21.
- Knobf MT (2007) Psychosocial responses in breast cancer survivors. Seminars in Oncology Nursing 23 (1):71-83.
- Kumar DM, Symonds RP, Sundar S et al, (2004) Information needs of Asian and White British cancer patients and their families in Leicestershire: A cross-sectional survey. British Journal of Cancer 90:1474-1478.
- MacMillan Cancer Support. (2014). Cancer information in other languages [online].
- Meneses KD and Yarbro CH (2007) Cultural perspectives of international breast health and breast cancer education. Journal of Nursing Scholarship 39 (2):105-112.
- NICE. (2004). Guidance on Cancer Services: Improving Supportive and Palliative Care for Adults with Cancer: The Manual. London: NICE.
- NHS Health Scotland (2008) Now weÃÆÃâÃââÃÆââ¬Å¡Ã¢ââ¬Å¡Ã¬ÃÆââ¬Å¡Ã¢ââ¬Å¾Ã¢re talking: Interpreting guidelines for staff of NHS Scotland. Health Scotland. Edinburgh: NHS Health Scotland.
- Pankhania G (2009) Interpretation and translation policy and procedure. Peterborough: NHS Peterborough.
- Patel G, Harcourt D, Naqvi H et al, (2014) Black and South Asian womenÃÆÃâÃââÃÆââ¬Å¡Ã¢ââ¬Å¡Ã¬ÃÆââ¬Å¡Ã¢ââ¬Å¾Ã¢s experiences of breast cancer: A qualitative study. Diversity and Equality in Health and Care 11:135-149.
- Pitchforth E and van Teijlingen E (2005) International public health research involving interpreters: A case study from Bangladesh. BMC Public Health, [online] doi:10.1186/1471-2458-5-71.
- Reid K, Flowers P and Larkin M (2005) Exploring lived experience. The Psychologists 18(1):20-23.
- Russell KM, Von DM, Giesler RB et al, (2008) Quality of life of African American breast cancer survivors: How much do we know? Cancer Nursing 31(6):36-45.
- Scanlon K and Wood A (2005) Breast cancer awareness in Britain: Are there differences based on ethnicity? Diversity in Health and Social Care 2:211-221.
- Smith JA (2011) Evaluating the contribution of interpretative phenomenological analysis. Health Psychology Review 5(1):9-27.
- Smith JA and Osborn M (2003) Interpretative Phenomenological Analysis. In: JA Smith (Eds.) Qualitative Psychology. London: Sage.
- Stirland L, Halani L, Bhopal R et al, (2011) Recruitment of South Asians into asthma research: Qualitative study of UK and US researchers. Primary Care Respiratory Journal 20 (3):282-290.
- Szczepura A (2005) Access to health care for ethnic minority populations. Postgraduate Medical Journal 81:141-147.
- Thompson A, Brennan K, Cox A et al, (2008) Evaluation of the current knowledge imitations in breast cancer research: A gap analysis. Breast Cancer Research 10:R26.
- Velikova G, Booth L, Johnston C et al, (2004) Breast cancer outcomes in South Asian population of West Yorkshire. British Journal of Cancer 90:1926-1932.
- Zaman MJS and Mangtani P (2007) Changing disease patterns in South Asians in the UK. Journal of the Royal Society of Medicine 100(6):254-255.