Keywords
|
| Health inequalities, Ethnicity, England, Health Survey for England, Logistic regression |
Introduction
|
| The Marmot Review (Marmot, 2010) reported on health inequalities within the UK. Implicit in the report’s title, ‘Fair Society Healthy Lives’, is that health inequalities are the product of an unfair society. Whilst issues of social justice and social and spatial inequalities in health have long been researched (Townsend et al., 1988; Shaw et al., 1999; Bajekal et al., 2013; Barr et al., 2012), there has been a relative paucity of comparable research on ethnic inequalities in health. |
| Nazroo (2014) identified a gap in this field in both evidence and policy debates in the UK, including their absence from the Marmot Review, attributing this gap to inadequate conceptions about the drivers of ethnic inequalities in health or assumptions that existing discussions of social and spatial inequalities in health also capture ethnic disparities. Explanations for ethnic inequalities in health are often sought in cultural or genetic differences. For example, babies of Pakistani origin have some of the highest rates of infant mortality in the UK (Hollowell et al., 2011): the most common cause of death amongst these infants is due to congenital anomaly (Evans, 2010). Consanguinity is a major risk factor for congenital anomalies in infants. It accounts for nearly a third of congenital anomalies in babies of Pakistani origin (Sheridan et al., 2013: 1354). Sheridan and colleagues highlighted that consanguineous unions are a part of Pakistani heritage which arguably lends credence to assertions that some ethnic inequalities in health are in part explained by differences in culture. However, there is little evidence that cultural factors have an important explanatory role in explaining health disparities (Nazroo, 1998). It should also be noted that ethnic origin is not necessarily associated with particular cultures. For instance, it would not be appropriate to assume that all ethnic Pakistanis follow particular traditions and norms just as it would be inappropriate to assume that all White populations have the same cultural traditions and customs. |
| South Asian groups disproportionately suffer from cardiovascular disease (CVD) and type II diabetes (Gupta et al., 2006a; Hussain et al., 2013), with some explanations pointing to factors such as a heightened insulin resistance amongst South Asians compared to Whites (Gupta et al., 2006b) or changes in life-style following migration to Western states (Gujral et al., 2013). However, a recent systematic review of genomic research investigating racial disparities in CVD, decisively concluded that ‘the accumulated evidence for a genetic contribution to CVD disparities in blacks versus white has been essentially nil’ (Kaufman et al., 2015: 468). Susceptibility to specific morbidities which may be associated with differences in culturally influenced lifestyle choices or the prevalence of insulin resistant genes, for example, do not adequately explain overall ethnic differences in health. There is no inherent underlying biological risk of poor health for minority ethnic groups (Nazroo, 2001; Bhopal et al., 2002) as the results of Kaufman et al.’s (2015) study clearly showed. If differences in culture or genetics have such a limited scope to explain ethnic disparities in health, research should surely look beyond ethnicity to explain health inequalities in society. Current discussions of social and spatial inequalities would therefore be sufficient to capture all health inequalities in society, arguably without reference to ethnicity. These discussions do not, however, go far enough. |
| Health invariably follows social and spatial gradients with inequalities observed by social class, income, educational attainment and area-based deprivation (Smith et al., 1997; Graham, 2000; Mackenbach et al., 2008; Wilkinson and Pickett, 2010; Stafford and Marmot, 2003). Different ethnic groups are disproportionately distributed across the social classes or between area-types, achieve different levels of qualifications or earn different incomes (e.g. Modood, 1997). Whilst ethnicity may not be directly relevant to health, it is evidently relevant to experiences or access to social determinants of health. To exemplify, consider that more than half of Maori populations in New Zealand live in the most deprived areas and experience some of the poorest health in New Zealand; the association between deprivation and mortality is significantly stronger for Maori compared to non-Maori groups (Robson and Harris, 2007: 38). Similar patterns and associations are found globally. Thus, the indirect relevance of ethnicity to health necessitates consideration of ethnicity in discussions of social and spatial inequalities in health. |
| Single measures of socioeconomic status often inadequately describe the complexity of the social and spatial inequalities faced by ethnic minority groups (Chandola, 2001; Cooper, 2002). Previous use of such measures has included salary differences between ethnic groups assigned to the same occupational class (Nazroo, 1997) and unemployment figures which, at the time, showed that minority ethnic men were more likely to be unemployed or employed in part-time work than their White counterparts (ONS, 1996). Nearly twenty years later, little has changed with recent data from the Labour Force Survey reporting higher rates of unemployment for all minority ethnic groups compared to White people (DWP, 2014). We must, therefore, also consider whether there is an additive penalty of not only being of a certain ethnicity but also experiencing social and spatial disadvantage to ensure that ethnic health gradients are substantively addressed within the policy agenda. |
| We suggest an additional explanation for the gap in policy and research. Quantitative research into ethnic differences in health is hampered by a lack of detailed ethnic data with large enough sample sizes for meaningful investigation. However, a lack of robust data should not undermine efforts to use that which is available. Indeed this was the impetus for Ajwani et al.’s (2003) and Blakely et al.’s (2007) innovative work anonymously and probabilistically linking death registrations to census data in New Zealand to demonstrate the widening mortality gap between Maori, Pacific and non-Maori non-Pacific groups. |
| The strength of these three explanations waivers when reviewing international literature on ethnicity and health: research (Abdalla et al., 2013; Bécares et al., 2013; Mitrou et al., 2014) consistently demonstrated that ethnic inequalities in health are perpetuated within unfair societies, divided along social and economic lines, and worsened by discrimination or the marginalisation of minority ethnic groups. Although the socio-political context may vary, a common theme is that minority ethnic groups are disproportionately concentrated in more disadvantaged circumstances characterised by poorer quality housing or temporary tenancies (private and social rentals); unemployment, under-employment, or employment in low skilled occupations (Nazroo, 1997); lower levels of educational attainment or less return on their educational investment (Lynch and Kaplan, 2000; Krieger et al., 1993); and low incomes (Hills et al., 2010; Nandi and Platt, 2010). These factors are all associated with poorer health (Marmot et al., 1991; Bartley and Blane, 2008; Bambra and Eikemo, 2009; Gibson et al., 2011, van de Knesebeck et al., 2006). Thus, where minority ethnic groups concentrate in more disadvantaged circumstances, (Modood et al., 1997; Nazroo, 1998; Barnard and Turner, 2011) it is reasonable to assume that they will also experience poorer health. |
| The marginalisation of minority ethnic groups in society is a form of racial discrimination, evident across the world from the United States (Williams and Mohammed, 2009) to New Zealand (Harris et al., 2006). In England the educational attainment gap between ethnic groups is a permanent feature of the education system due to the inherent structural racism unconsciously practiced in schools and which may explain differences in earnings between ethnic groups (Gibson 2008, Nazroo, 1997) or different opportunities in the workforce and the under-employment of minority ethnic groups given their educational attainment (Heath and Cheung, 2006). Even where improvements are seen, such as in the narrowing employment gap between White and minority ethnic groups between 1993 and 2013 (down to 11.9 percentage points from 15.2), gaps persist (DWP, 2014). Racism is not only divisive, compounding experiences of disadvantage amongst minority groups, it also jeopardises health (Williams, 1999; Karlsen and Nazroo, 2002; Harris et al., 2006). Whether direct or indirect, the stressors of racial harassment or discrimination are associated with adverse mental health (Krieger et al., 2005), poor self-assessed general health (Karlsen and Nazroo, 2004) and early child health and development (Kelly et al., 2012). |
| The relationship between health and racism has been extensively explored in the literature cited here. This review has outlined evidence illustrating that ethnic inequalities in health are the product of an unfair society, deserving substantive consideration in reports such as the Marmot Review. The possibility of a multiplicative effect of being of a certain ethnicity and experiencing multiple socioeconomic disadvantages may explain a large amount of observed ethnic inequalities in health. This paper contributes to the evidence base. It aims to |
| a) quantify ethnic inequalities in health over a long-run time-series. |
| b) examine whether these inequalities remain when sociodemographic circumstances are accounted for. |
| We do this by: |
| a) accessing annual data from the Health Survey for England and harmonising variables over time. |
| b) calculating a time-series of health measures by ethnic group. |
| c) modelling health outcomes controlling for various sociodemographic attributes. |
| Although there is some overlap with previous work, it is justified given that research in this area is often challenged by sample sizes. |
Data
|
| The Health Survey for England (HSE) is an annual representative household survey of England’s population covering a range of core topics each year alongside rotating special themes. Although the HSE is used to investigate ethnic differences in health (Cooper, 2002; Sproston and Mindell, 2006; Karlsen and Nazroo, 2010), no study has created a long-run data timeseries to explore how ethnic differences in health have changed over time. The study period here was largely determined by the availability of sufficiently consistent variables but is a period which is apt for analyses of ethnic difference and changing population health. England became increasingly diverse with the UK’s White population reducing from 91.4% to 86% between 1991 and 2011 (ONS, 2012). This period was characterised by sustained economic growth from 1998 to 2007 (Barr et al., 2007) followed by recession, important factors affecting socioeconomic inequality. The time-series started with a 10 year period of targeted political action on health inequalities from the then Labour government. Tracking wider changes in population health during and after such an intervention is important when looking to contribute to evidence-based policy. |
| Annual variation in the survey content requires that consistent variables are derived before creating a 1998-2011 time-series dataset. For a detailed account of this see Darlington et al., (2014). However, for clarity the following sections will briefly outline our manipulation of the HSE data for the purposes of this analysis. The HSE sample analysed is restricted to adults aged 16 and over. Two binary health outcomes are derived from the HSE’s limiting long-term illness (LLTI) and self-assessed health variables. For the latter, ‘less than good health’ is classed as poor health. Both measures are widely used in the health inequalities literature and self-assessed health in particular has been shown to be a valid measure for investigating ethnic differences in health (Chandola and Jenkins, 2000). The independent variables included are widely acknowledged as social determinants of health. These variables characterise various social and, to a small extent given the lack of geographic detail in the HSE, spatial experiences between ethnic groups in England. |
| Age is collapsed into five categories to reflect breaks in the lifecourse. Ethnicity distinguishes between White, Black, Indian, Pakistani and Bangladeshi, and Mixed and Other. Sample sizes for Black African and Black Caribbean are too small to distinguish between, as are those for Pakistani and Bangladeshi, or for the heterogeneous Mixed and Other groups. Results for the latter group will largely be discarded, as will extensive discussion of the Black group within which socioeconomic and health experiences are particularly divergent. Although not ideal, these are the most detailed ethnic classifications achievable over time. Social class is defined by the Registrar General’s scheme (social class based on occupation), a widely used measure in health literature. To avoid small numbers, classes I and II, and IV and V are combined, and Government Office Region (GOR) is simplified to North, Yorkshire and the Humber, Midlands, London, East of England, and South. Educational attainment distinguishes between those qualified at degree level, those qualified below this threshold and those with no qualifications (including foreign and other qualifications). Tenure distinguishes between owner-occupied, privately rented and socially rented accommodation. The small proportion living in care homes are excluded. |
| All non-responses for the health outcomes are taken to indicate no LLTI or good health on the assumption that respondents to a health survey will confirm poor health, if present. This should be interpreted cautiously as questionnaires focussing on health can produce higher (although not necessarily false) estimates of poor health in a population (Taylor et al., 2014). Since similar assumptions cannot be made about the independent variables, non-responses are excluded. |
Methods
|
| Data were pooled over rolling three-year periods to smooth annual fluctuations and increase sample sizes. Changing population health by ethnic group was first assessed using indirectly standardised illness ratios (SIRs) which controlled for the group’s age structure. The standard population were all present in the dataset to allow comparisons over time. SIRs of more than 100 indicated poorer than expected health, whereas less than 100 indicated better than expected health. Rate ratios were then calculated to explore whether ethnic inequalities in health between minority and majority groups were changing. If the ratio had a value greater than 1, the minority ethnic group had poorer health than the White group and vice versa. If this value changed over time, this indicated that the gap between the White majority and a minority group was changing. Rate ratios were also calculated to explore inequalities within the South Asian groups. |
| The relationships between each health outcome and the independent variables were then modelled using binary logistic regression (using SPSS v20). These models illustrated the extent to which the independent variables explained differences in health. Results for ethnic groups were modelled in relation to the White group. Reported results included odds ratios, 95% confidence intervals (CIs) and modelled probabilities of LLTI or poor health. |
| Thus, using samples from repeated cross-sectional data of England’s population, we examined ethnic inequalities in health between 1998 and 2011 using SIRs to quantify these inequalities. Rate ratios were then used to assess whether gaps in health between ethnic groups had widened, constrained or been maintained over time. To explore the nature of these inequalities, we then modelled health to assess the contribution of ethnicity, sociodemographic and broad geographic factors to differences in health within the population. We therefore asked, how have ethnic inequalities in health in England changed over time? Further, what explains these changing health gradients? |
Results
|
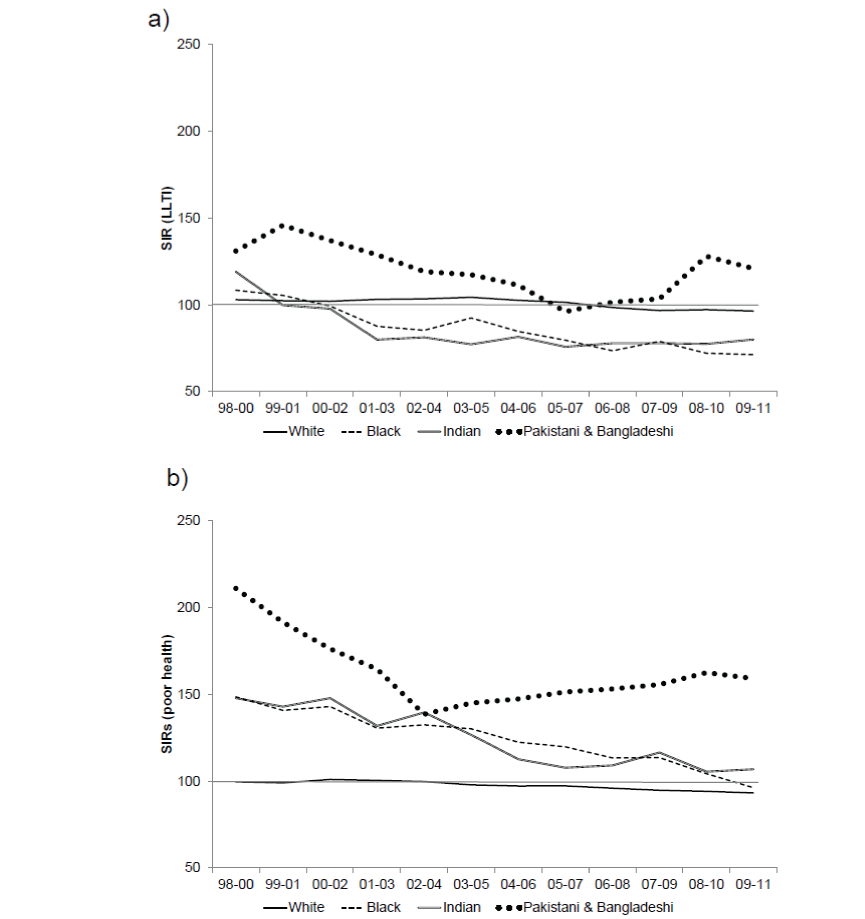
| Figure 1 illustrates changing patterns of health by ethnic group using the SIRs. For both health outcomes, the Pakistani and Bangladeshi group has relatively poor health circumstances. After an initial decline, the SIRs climb from around 2005 for LLTI, and 2002 for poor health. Further, the SIRs invariably remain above 100 indicating consistently poorer than expected health for both health outcomes. Conversely, levels of poor health for Indian and Black groups are in decline with the SIR for LLTI falling to less than 100 from 2000. However, the SIRs for these ethnic groups remain above 100 for poor health, although these are not significantly different from the White group by 2008. In both health outcomes, the White group tends to have expected levels of LLTI and poor health over the study period. However, this is largely because the Whites are the majority population. |
| The SIRs indicate that a) minority ethnic groups consistently have higher than expected levels of poor health with significantly higher levels in the Pakistani and Bangladeshi group; b) Indian and Black groups have lower than expected levels of LLTI, below those of the White majority; c) the health of Pakistani and Bangladeshi groups appears to be worsening whereas Indian and black groups experience improvements; and finally d) gaps between all ethnic groups persist for the duration of the study period. The CIs (not presented on the graphs) tend to be large for the minority groups due to sample sizes. Notwithstanding small numbers, some significant differences are found. |
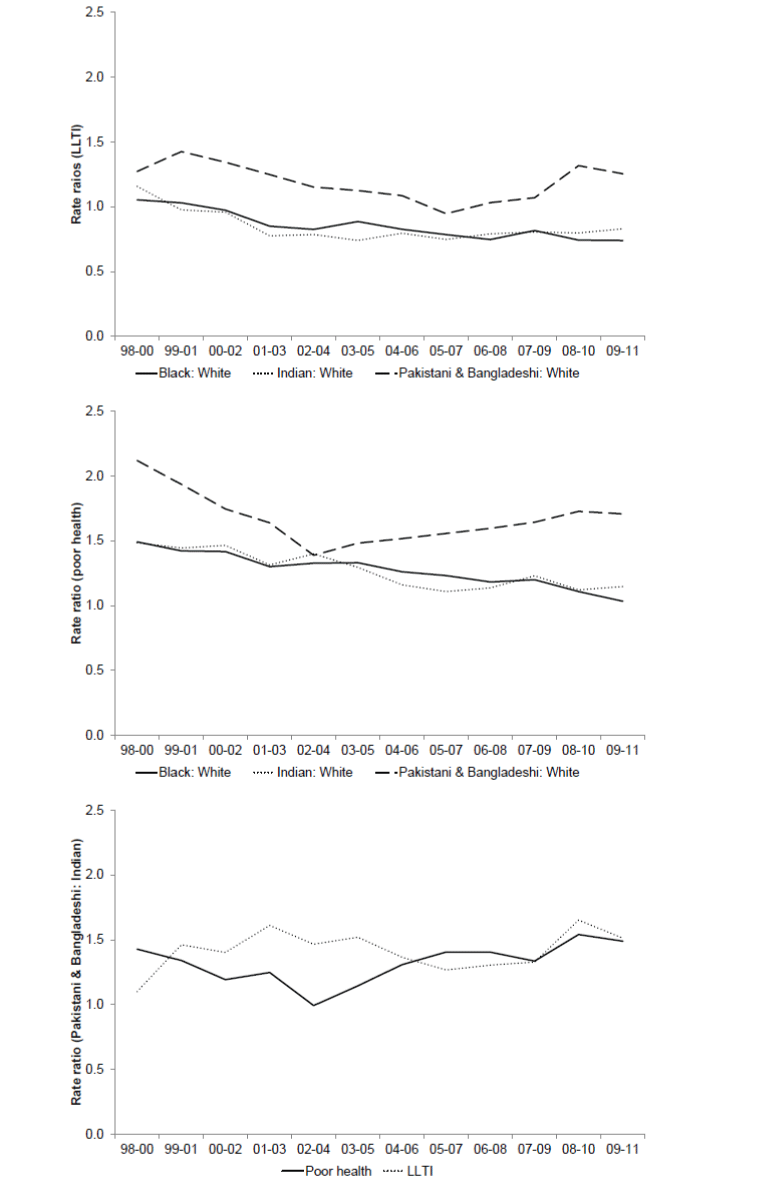
| Rate ratios relative to the White group illustrate whether these gaps are changing. In Figure 2, after an initial reduction, the gap between the White and the Pakistani and Bangladeshi groups increases over time for both health outcomes. Conversely, the gap between White and Black groups, and the White and Indian groups is narrowing over time. For LLTI, this indicates that these groups fare better than the White majority. |
| Differences in health between the Indian and the Pakistani and Bangladeshi groups are evidenced by widening gaps for both measures. For LLTI, the largest health gap is within these South Asian ethnicities. Recognising these divergent health experiences is important given a tendency to group these ethnicities together in public and academic research (e.g. Norman and Fraser, 2013). |
| Comparing the distributions of each ethnic group within the independent variables (Table 1) over time is revealing regarding persisting and changing inequalities. Indians consistently have high concentrations in more advantaged circumstances: higher social classes, in employment, educated to degree level or above, living in owner-occupation. This contrasts with the socioeconomic experiences of Black, Pakistani and Bangladeshi groups who tend to be concentrated in more disadvantaged circumstances: lower social classes, unemployed or economically inactive, lower levels of educational attainment and living in socially rented accommodation. Whilst the White group are generally, although not exclusively, in better circumstances than either the Black or Pakistani and Bangladeshi groups, they do not appear to be more likely than Indian groups to experience advantage. |
| Notwithstanding the coarse GOR geography available in the HSE, there are differences in the spatial distribution of these ethnic groups. Whilst the minority ethnic groups overwhelmingly concentrate in London, with Black groups having the largest proportion there, they are not then equally spread across England. For example, Pakistanis and Bangladeshis cluster in the North and Yorkshire, with a marked increase over time in the North. Conversely, a large proportion of Indians are resident in the Midlands. |
Modelling poor health
|
| Tables 2 and 3 present the Binary Logistic Regression results as Odds Ratios (OR) for selected years: an OR of more than one indicates a greater likelihood of the outcome relative to the reference group and vice versa. Model 1a estimates LLTI and 2a estimates poor health adjusting for each of the demographic variables. To determine the contribution of socioeconomic and spatial variables to differences in health, models 1b and 2b additionally adjust for the socioeconomic variables and Government Office Region (GOR). All differences in health are relative to the White group. |
| When adjusting only for demographic variables in models 1a and 2a, females have marginally higher odds of both outcomes than males, though differences are rarely significant. Odds of LLTI increase steeply with age relative to those aged 16-24, with a similar although shallower gradient evident for poor health. |
| Relative to the White group, from 2000-2002 onwards Black and Indian groups have lower likelihoods of LLTI whereas the Pakistanis and Bangladeshis have higher odds (mainly significant). Conversely, the odds of poor health are significantly raised for Black groups up to 2008-2010, mainly significantly raised for Indian groups, and consistently significantly raised for Pakistanis and Bangladeshis. |
| Models 1b and 2b also adjust for the socioeconomic variables and GOR. For both health outcomes, social classes IIIN to V have raised odds relative to classes I and II. However, the ORs for social classes IV and V suggest that the magnitude of health penalty is lower than one might expect. For employment, education and tenure, the patterns of differences in both LLTI and poor health are generally consistent with expectations. Spatial differences in health, particularly between the North and South, are demonstrated by the generally significantly lower odds of LLTI and/or poor health for the East of England, London and the South relative to the North. For gender, the inclusion of these additional variables largely reversed the odds such that females are now less likely than males to report LLTI or poor health (mainly significant). The gradient of ORs by age is somewhat attenuated but successive increases in likelihoods of either health outcome by age are found. |
| Model 1b in table 2, shows persons of Black ethnicity have significantly higher odds than the White group for LLTI until 2007-2009, for recent years there are no differences. For poor health in model 2b, as shown in table 3, Black groups have significantly lowered odds relative to the White group for the latter half of the period, contrasting with no difference for the earlier years. The Indian group has significantly higher odds of LLTI throughout the study period, but generally no difference for poor health. The same pattern is evident for the combined Pakistani and Bangladeshi group. |
| ORs indicate the position of groups relative to the outcome for the reference group. Insights can be gained by calculating modelled probabilities that demonstrate the different chances of LLTI or poor health for each group. These show that a White individual in classes I and II living in the North has a higher probability of LLTI than if they lived in the South (3.9% versus 2.9% in 2009-2011). An Indian living in the South in the same social classes has the health chances of the White individual living in the North (3.9% probability of LLTI). The probability of LLTI climbs to 5.2% for an Indian of classes I and II living in the North. Whilst more favourable socioeconomic (higher social classes) or spatial (living in the South) circumstances are associated with lower probabilities of LLTI, the benefits of these circumstances are not equally distributed between ethnic groups. Although probabilities of LLTI do decline for all groups over time, the highest probabilities are consistently found for ethnic minorities, controlling for social and spatial variations. |
Discussion
|
| We aimed to quantify ethnic inequalities in health over time and examine whether inequities experienced by different ethnic groups remain after accounting for sociodemographic circumstances. In quantifying ethnic inequalities in health, our results suggest that inequalities appear to be widening between the White and Pakistani and Bangladeshi groups and within South Asian ethnicities by general health and LLTI as shown in figure 2. Conversely, health inequalities between White and Black or White and Indian groups have narrowed such that these groups increasingly fare better in terms of LLTI than White groups. Whilst the gap has similarly narrowed in terms of general health, Black and Indian groups are still in poorer health than Whites by this measure. |
| The divergent health experiences of each ethnic group are echoed in their contrasting socioeconomic experiences. While the gap widened between the Pakistani and Bangladeshi group and both the White majority and the Indian group, Pakistani and Bangladeshis remained concentrated in more disadvantaged circumstances as seen in table 1. The relative disadvantage of certain groups, particularly Pakistani and Bangladeshi groups, is common in the literature as is the relative advantage of Indian groups (e.g. Bhopal et al., 2002). The rising and falling economic prosperity which characterised England’s economic climate during the period of study had no notable beneficial or detrimental effect on the socioeconomic circumstances of each ethnic group according to their socioeconomic distribution over time. All groups experienced some improvements in their socioeconomic circumstances, although this did not necessarily close the gap between ethnic groups. More may be gleaned by extending the study period to examine more closely the impact of the slowly recovering economy post 2009-2011 on different ethnic groups and their socioeconomic circumstances. |
| These contrasting experiences according to either health measure may reflect cultural interpretations in the meaning of ‘limiting long term illness’ (Mitchell, 2005). Self-assessed general health is a valid measure to investigate ethnic differences in health (Chandola and Jenkins 2001). Perhaps the actual health of ethnic groups more closely matches the picture revealed by poor health than LLTI. |
| In examining whether inequities experienced by different ethnic groups remain after accounting for sociodemographic circumstances, our results were clear. The addition of socioeconomic and spatial variables consistently modifies the ORs observed by age, ethnicity and gender as seen by comparing the ORs in models 1a with 1b and 2a with 2b. This suggests that some of the variation in health between males and females, age groups and ethnicities is explained by socioeconomic and spatial factors. However, there were notable differences between ethnic groups and by health outcome. Adjusting for socioeconomic and spatial variables reversed the odds of LLTI for Indians such that this group moved from significantly lowered to significantly raised odds of LLTI relative to the White group when accounting for social and spatial variables. Conversely, the opposite effect was found when modelling poor health. Given the more advantaged circumstances of Indians relative to not only the White group, but also Pakistanis and Bangladeshis combined, we might have anticipated lowered odds of LLTI when adjusting for the socioeconomic and spatial variables. Bhopal et al., (2002) also found unexpected associations between factors such as class or household income and health for South Asian ethnic groups. Rather than leading the authors to refute the existence of a socioeconomic patterning to ethnic health gradients, they questioned whether socioeconomic indicators are sufficient to capture these patterns for ethnic groups. They called for better data to alleviate concerns about sample sizes and allow for discrete analysis of Indians, Pakistanis and Bangladeshis. |
| Results from our analyses are consistent with the wider literature with the influence of ethnicity on health decreasing when adjusting for socioeconomic factors (e.g. Williams, 1996; Cooper, 2002; Karlsen and Nazroo, 2010; Nazroo, 2014; Mindell et al., 2014). While some may argue that the differences which remain are attributable to genetic or cultural differences, there is evidence that wider experiences of racial harassment and discrimination experienced by minority ethnic groups account for these differences (e.g. Nazroo, 1998; Harris et al., 2006; Harris et al., 2012) rather than genetics or culture. |
| The possible multiplicative or additive penalty of minority ethnic status is perhaps evident in our modelled probabilities of LLTI. Probabilities vary between ethnic groups within the same social class and area suggesting that the influence of social class or area on health is not necessarily equally beneficial or deleterious for different groups. Thus, the influence of socioeconomic position on health is in some part contingent on ethnicity. The idea of an ethnic penalty may also explain the raised odds of LLTI for Indians relative to White groups when adjusting for socioeconomic and spatial factors: are these groups penalised due to their ethnicity over and above the benefits of their more prosperous circumstances? This is consistent with differences in income between ethnic groups of the same class (Nazroo, 1997), the employment gap (DWP, 2014) and the under-return on educational investment (Heath and Cheung, 2006), as well as substantiating arguments about the suitability of single measures in capturing ethnic differences. Variations in the probabilities of LLTI between ethnic groups in comparable socioeconomic circumstances also highlights the possible inadequacies of existing measures of socioeconomic position when applied to different ethnic groups. Our results support previous work highlighting the shortcomings of these measures (e.g. Harding, 2003). These measures may not fully illustrate the interaction between ethnicity and socioeconomic position which may differently influence health between ethnic groups. We therefore recognise this as a limitation of our study but it is also highlights valuable future avenues for research. |
| Further work should investigate how ethnicity may interact differently with different socioeconomic attributes to influence health for different ethnic groups. Sample sizes in the HSE prevented this from being investigated here. However, we can assert that if the influence of socioeconomic and spatial factors on health varies between ethnic groups, whether or not this relates to issues of marginalisation or the operation of an ethnic penalty, then it cannot be assumed that existing discussions of socioeconomic difference adequately capture the diverse experiences of ethnic groups. |
Strengths and weaknesses
|
| A strength of this study is the use of long-run time-series data to analyse changing ethnic health in a period characterised by rising and falling economic prosperity, targeted intervention in health inequalities, and increasing ethnic diversity. The conclusions add to the growing evidence base needed to address ethnic disparities in health policy. |
| However, working within the constraints of predetermined (by data collectors) and contested constructs of ethnic groups is not without problems. Here we balanced the need for statistical robustness in terms of sample size whilst maintaining as much ethnic detail as possible. Although a large scale survey, the sample sizes are not large when analysing ethnic differences. However, the value of the research or the data should not be contingent on statistical significance. Any patterns revealed may be indicative of broader trends which should be considered in the absence of more robust data, particularly where results replicate findings of other studies, as ours do. Our ethnicity variable will mask health differences within groups but the categories are as detailed as possible and still valuable in investigating ethnic variations in health. |
| Finally, the measure of social position reflects availability within the HSE and allows comparability with existing research. However, it is limited with respect to analyses of ethnic differences as this measure of social status may not have the same meaning between different ethnic groups. Indeed, if a higher overall percentage of each minority ethnic group could be assigned to a social class it might be more illuminating as to the extent of ethnic gradients in health. To illustrate, 31.3% of the White group could not be assigned to a social class yet this increased to as much as 65.6% for Pakistanis and Bangladeshis. The inability to assign social class may also mask gendered differences in not only social class, but also economic activity and educational attainment between ethnic groups which may be revealing as to ethnic differences in health (see Nazroo, 1998). Despite this, it is believed that the results underestimate rather than overestimate the extent of the health gap due to data constraints and definitional limitations. |
Conclusion
|
| We found that socioeconomic disadvantage better accounts for ethnic variations in health than ethnicity, although not necessarily for both health outcomes. These patterns hold for the duration of the study period despite overall improvements in population health. We build on and confirm existing literature investigating ethnic differences in health by using the HSE in a novel way by focussing on a time period appropriate to the study of ethnic differences. The novelty of this approach rests in the creation of a long-run time series dataset specifically intended for the analysis of ethnic differences in society. While the HSE has been used elsewhere to explore ethnic differences over shorter time periods (e.g. Cooper, 2002; Mindell et al., 2014) or as a time-series to investigate obesity trends (e.g. Sperrin et al., 2014), no work to date has used the data in this way. Furthermore, our paper further demonstrates the importance of exploring the interaction between socioeconomic and spatial differences and ethnicity to explain ethnic health gradients. We demonstrate that neither ethnicity alone, nor existing discussions of socioeconomic and spatial inequalities are sufficient to account for ethnic health gradients thus necessitating a more substantive discussion of ethnic inequalities in health within the policy agenda. |
| The possible multiplicative deleterious effects of being of a certain ethnicity and experiencing disadvantage necessitates more focussed discussions on ethnic socioeconomic inequalities in health. We cannot assume either that minority ethnic groups are genetically predisposed to poorer health or that existing discussions of socioeconomic and spatial difference fully capture the contrasting experiences of different ethnic groups. |
| We account for socioeconomic inequalities between ethnic groups with available measures of class, economic status, tenure, educational attainment and area. However, these measures are unlikely to capture the full complexities of these inequalities between ethnic groups (Chandola, 2001). It is possible our results based on these uni-dimensional measures underestimate the extent to which socioeconomic difference explains ethnic inequalities in health. Whilst more research is required, our results contribute to the growing evidence base which demonstrates the role of socioeconomic and spatial difference in contributing to ethnic inequalities in health. These differences, particularly if maintained over life-spans and between generations, must therefore become a prominent feature of the policy rhetoric. |
CONFLICT OF INTEREST
|
| None |
Tables at a glance
|
|
|
Figures at a glance
|
 |
 |
| Figure 1 |
Figure 2 |
|
References
|
- Abdalla S, Kelleher C, Quirke B et al. (2013) All-Ireland Traveller Health Study T. Social inequalities in health expectancy and the contribution of mortality and morbidity: the case of Irish Travellers. Journal of Public Health 35:533-40.
- Ajwani S, Blakely T, Robson B et al. (2003) Decades of disparity: Ethnic mortality trends in New Zealand 1980-1999. Wellington: Ministry of Health and University of Otago.
- Bajekal M, Scholes S, O’Flaherty M et al. (2013) Unequal trends in coronary heart disease mortality by socioeconomic circumstances, England 1982-2006: An analytical study. PLoS ONE 8(3): e59608. Doi:10.1371/journal.pone.0059608 [accessed June 2014]
- Bambra C and Eikemo TA (2009) Welfare state regimes, unemployment and health: a comparative study of the relationship between unemployment and self-reported health in 23 European countries. Journal of Epidemiology and Community Health 63: 92-98.
- Barnard H and Turner C (2011) Poverty and Ethnicity: a review of evidence. York: Joseph Rowntree Foundation.
- Barr B, Taylor-Robinson D and Whitehead M (2012) Impact on health inequalities of rising prosperity in England 1998-2007, and implications for performance incentives: longitudinal ecological study. British Medical Journal 335: e7831. DOI:10.1136/bmj.e7831
- Bartley M and Blane D (2008) Inequality and social class, in G Scrambler (ed) Sociology as applied to medicine. London: Elsevier Limited; 115-132.
- Bécares L, Cormack D and Harris R (2013) Ethnic density and area deprivation: Neighbourhood effects on Maori health and racial discrimination in Aotearoa/New Zealand. Social Science & Medicine 88:76-82.
- Bhopal R, Hayes L, White M et al. (2002) Ethnic and socio-economic inequalities in coronary heart disease, diabetes and risk factors in Europeans and South Asians. Journal of Public Health 24:95-105.
- Blakely T, Tobias M, Atkinson J et al. (2007) Tracking Disparity: Trends in ethnic and socioeconomic inequalities in mortality, 1981-2004. Wellington: Ministry of Health.
- Chandola T (2001) Ethnic and class differences in health in relation to British South Asians: using the new National Statistics Socio-Economic Classification. Social Science& Medicine 52: 1285-1296.
- Chandola T and Jenkinson C (2000) Validating self-rated health in different ethnic groups. Ethnicity & Health 5: 151-159.
- Cooper S (2002) Investigating socio-economic explanations for gender and ethnic inequalities in health. Social Science& Medicine 54: 693 – 706.
- Department for Work and Pensions (2014) Labour market status by ethnic group https://www.gov.uk/government/uploads/ system/uploads/attachment_data/file/383677/labourmarket-
status-by-ethnic-group.pdf [last accessed March 2015].
- Evans J (2010) Gestation-specific infant mortality in England and Wales, 2010. Child Health London: Analysis Team Office for National Statistics, 2010.
- Gibson M, Petticrew M, Bambra C et al. (2011) Housing and health inequalities: A synthesis of systematic reviews of interventions aimed at different pathways linking housing and health. Health & Place 17: 175-184.
- Gillborn D (2008) Racism and Education: Coincidence of Conspiracy? London: Taylor and Francis.
- Graham H (2000) Understanding Health Inequalities. Maidenhead: OUP.
- Gujral UP, Pradeepa R, Weber MB et al. (2013) Type 2 diabetes in South Asians: similarities and differences with white Caucasian and other populations. Annals of the New York Academy of Sciences 1281: 51-63.
- Gupta M, Singh N, Verma S (2006a) South Asians and Cardiovascular Risk, What clinicians should know.
Circulation 113: 924-929.
- Gupta M, Brister S, Verma S (2006b) Is South Asian ethnicity and independent cardiovascular risk factor? The Canadian Journal of Cardiology 22 (3): 193-197.
- Harding S (2003) Social mobility and self-reported limiting long-term illness among West Indian and South Asian migrants living in England and Wales. Social Science& Medicine 56: 355-361
- Harris R, Cormack D, Tobias M et al. (2012) The pervasive effects of racism: experiences of racial discrimination in New Zealand over time and associations with multiple health domains. Social Science & Medicine 74: 408-415.
- Harris R, Tobias M, Jeffreys M et al. (2006) Effects of selfreported racial discrimination and deprivation on M?ori health and inequalities in New Zealand: cross-sectional study. The Lancet 367: 2005-2009.
- Heath A and Cheung SY (2006) Ethnic penalties in the labour market: Employers and discrimination. Research Report No 241. London: Department for Work and Pensions.
- Hills J, Brewer M, Jenkins S et al. (2010) An Anatomy of Economic Inequality in the UK: Report of the National Equality Panel. London: Government Equalities Office/ Centre of Analysis of Social Exclusion.
- Hollowell J, Kurinczuk J, Brocklehurst P et al. (2011) Social and ethnic inequalities in infant mortality: a perspective from the United Kingdom. Seminars in Perinatology 35 (4): 240-244.
- Hussain SM, Oldenburg B, Wang Y et al. (2013) Assessment of cardiovascular disease risk in South Asian populations.
- International Journal of Vascular Medicine 786801: 1-10. Karlsen S and Nazroo J (2002) Relation between racial discrimination, social class and health among ethnic minority groups. American Journal of Public Health 92: 624-631.
- Karlsen S and Nazroo J (2004) Fear of racism and health. Journal of Epidemiology and Community Health 58: 1017- 18.
- Karlsen S and Nazroo J (2010) Religious and ethnic differences in health: evidence from the Health Surveys for England 1999 and 2004. Ethnicity & Health 15: 549-68.
- Karlsen S, Nazroo J and Stephenson R (2002) Ethnicity, environment and health: putting ethnic inequalities in health in their place. Social Science & Medicine 55: 1647-1661.
- Kaufman JS, Dolman L, Rushani D et al. (2015) The contribution of genomic research to explaining racial disparities in cardiovascular disease: a systematic review. American Journal of Epidemiology 181 (7): 464-472.
- Kelly Y, Bécares L and Nazroo J (2012) Associations between maternal experiences of racism and early child health and development: findings from the UK Millennium Cohort Study. Journal of Epidemiology and Community Health. DOI:10.1136/jech-2011-200814jech-2011.
- Krieger N, Smith K, Naishadham D et al. (2005) Experiences of discrimination: validity and reliability of a self-report measure for population health research on racism and health. Social Science & Medicine 61:1576-96.
- Mackenbach JP, Stirbu I, Roskam AR et al. (2008) Socioeconomic inequalities in health in 22 European countries. The New England Journal of Medicine, 358: 2468-241.
- Marmot M (2005) Social determinants of health inequalities. The Lancet 365: 1099-1104.
- Marmot M (2010) Fair Society, Healthy Lives. The Institute of Health Equity: London. https://www.instituteofhealthequity. org/projects/fair-society-healthy-lives-the-marmot-review [last accessed January 2014]
- Marmot M, Smith GD, Stansfeld S et al. (1991) Health inequalities among British civil servants: the Whitehall II study. The Lancet 337: 1387-1393.
- Mitchell R (2005) The decline of death – how do we measure and interpret changes in self-reported health across cultures and time? International Journal of Epidemiology 34: 306-8.
- Mitrou F, Cooke M, Lawrence D et al. (2014) Gaps in Indigenous disadvantage not closing: a census cohort study of social determinants of health in Australia, Canada, and New Zealand from 1981-2006. BMC Public Health 14: 201.
- Mindell J, Knott CS, Ng Fat LS et al. (2014) Explanatory factors for health inequalities across different ethnic and gender groups: data from a national survey in England. Journal of Epidemiology and Community Health 68 (12): 1133-1144.
- Modood T, Berthoud R, Lakey J et al. (1997) Ethnic Minorities in Britain: Diversity and Disadvantage. London: Policy Studies Institute.
- Nandi A and Platt L (2010) Ethnic Minority Women’s Poverty and Economic Well-Being. London: Government Equalities Office.
- Nazroo J (1997) The Health of Britain’s Ethnic Minorities: findings from a national survey. London: Policy Studies Institute.
- Nazroo J (1998) Genetic, cultural or socio-economic vulnerability? Explaining ethnic inequalities in health. Sociology of Health and Illness 20: 710-30.
- Nazroo J (2001) South Asians and heart disease: an assessment of the importance of socioeconomic position. Ethnicity and Disease 11: 401-411.
- Nazroo J (2003) The structuring of ethnic inequalities in health: economic position, racial discrimination and racism. American Journal of Public Health 93: 277 – 84.
- Nazroo J (2014) Ethnic Inequalities in Health: Addressing a Signifi cant Gap in Current Evidence and Policy’ in L Newby and N Denison (eds) “If you could do one thing…” Nine local actions to reduce health inequalities. London: The British Academy: London; 91 – 101.
- Norman P and Fraser L (2013) Self-reported general health and Body Mass Index: a U-shaped relationship? Public Health 127: 938-945.
- Office for National Statistics (1996) Social focus on ethnic minorities. London: H.M.S.O.
- Office for National Statistics (2012) Ethnicity and national identity in England and Wales 2011. https://www.ons.gov.uk/ons/dcp171776_290558.pdf [accessed January 2013].
- Rees P, Wohland P, Norman P et al. (2011) A local analysis of ethnic group population trends and projections for the UK. Journal of Population Research 28: 129-148.
- Robson B and Harris R (eds) (2007) Haoura: Maori Standards of Health IV. A study of the years 2000-2005. Wellington: University of Otago.
- Shaw M, Dorling D, Gordon D et al. (1999) The widening gap: health inequalities and policy in Britain. Bristol: Policy Press.
- Sheridan E, Wright J, Small N et al. (2013) Risk factors for congenital anomaly in a multi-ethnic birth cohort: an analysis of the Born in Bradford study. The Lancet 382 (9901): 1350 – 1359.
- Smith GD, Hart C, Blane D et al. (1997) Lifetime socioeconomic position and mortality: prospective observational study. British Medical Journal 314: 547-552.
- Sperrin M, Marshall AD, Higgins V et al. (2014) Slowing down of adult body mass index trend increases in England: a latent class analysis of cross-sectional surveys (1992-2010). International Journal of Obesity 38: 818-824.
- Sproston K and Mindell J (2006) Health Survey for England 2004: The Health of Minority Ethnic Groups. London: The Information Centre.
- Stafford M and Marmot M (2003) Neighbourhood deprivation and health: does it affect us all equally? International Journal of Epidemiology 32: 357-366.
- Taylor J, Twigg L, Moon G (2014) The convergent validity of three surveys as alternative sources of health information to the 2011 UK census. Social Science & Medicine 116: 187-192.
- Townsend P, Phillimore P and Beattie A (1988) Health and Deprivation: Inequality in the North. London: Croom Helm.
- van de Knesebeck O, Verde PE and Dragano N (2006) Education and health in 22 European countries. Social Science & Medicine 63: 1344-51.
- Wilkinson R and Pickett K (2010) The Spirit Level, Why Equality is Better for Everyone. London: Penguin Books.
- Williams DR (1996) Race/Ethnicity and Socioeconomic Status: Measurement and Methodological Issues. International Journal of Health Services 26: 483-505.
- Williams DR (1999) Race, socioeconomic status and health The added effects of racism and discrimination. Annals of the New York Academy of Sciences 896: 173-188.
- Williams DR and Mohammed SA (2009) Discrimination and racial disparities in health: evidence and needed research. Journal of Behavioural Medicine 32: 20-47.
- Williams R, Williams W and Hunt K (1998) Social class and health: the puzzling counter-example of British South Asians. Social Science & Medicine 47: 1277-1288.
|



