Keywords
|
| Cultural competence, culture, ethnic-minority, healthcare, training, critical interpretive synthesis |
INTRODUCTION
|
| Clinical practice occurs in a shared environment in which aspects of culture, diversity and equality are in constant interplay with each-other. Depending upon the clinical encounter, issues of culture, diversity and equality may have competing perspectives which act as a lens in defining an individual’s attitude, approach, expectation and standard of professional practice (Sanchez-Runde, Nardon et al. 2013). Evidence has shown the influence of culture, diversity and equality on the availability, accessibility, acceptability and quality on healthcare service provision (Napier et al. 2014; Bhui et al. 2007). |
| UK healthcare services aim to ensure that services are equitable, responsive to the diverse needs of patients and culturally inclusive. However, consistent reports of health inequalities, disparities in the quality of care, lower rates of satisfaction and a convincing perception of culturally inadequate healthcare provision for members of minority groups, demonstrate that the UK healthcare system is struggling to meet the needs of culturally diverse populations (Schouler-Ocak, 2015; Gallagher, 2015). There are continuous calls for health professionals and health services to be ?culturally competent’ so that patient needs can be met. There are several definitions of cultural competence but the commonly used is that of Cross et al. (1989): ?A set of congruent behaviours, attitudes and policies that come together in a system, agency or among professionals and enables that system, agency or those professionals to work effectively in cross-cultural situations’. In reality ‘cultural competence’ is often vaguely defined, poorly understood and used synonymously with labels such as ‘cultural sensitivity’, ‘equality and diversity’ and ‘cultural awareness’ (Papadopoulos et al. 2004). Dogra (2003) argued for a much broader definition to represent the multifacted makeup of individuals and highlighted how the field of cultural competence is subject to political rather than educational influences (Dogra and Willians, 2006). |
| Cultural competence training (CCT) has been proposed as a strategy that facilitates the provision of culturally appropriate care (Dogra et al, 2005; Dogra and Karim, 2005). CCT is specifically targeted at improving the competence of health professionals in ethnically diverse settings by either enhancing cultural knowledge, attitudinal responses or skills (Bentley et al, 2008). A major justification for CCT is the hope that it will reduce healthcare disparities and ensure accessible and effective healthcare for the whole population. |
| CCT is widely variable in UK healthcare settings (Bentley et al, 2008) in terms of their content, duration, delivery and assessment but it has not been standardized or carried out in a consistent manner although an increasing number of professional guidelines, healthcare policies and statutory requirements encourage and even mandate this training (Good Medical Practice, 2013; Workforce Race Equality Standard, 2015; Equality Delivery System II, 2015). However, evidence suggests that current CCT does not adequately prepare health professionals to meet the needs of culturally diverse communities (Bhugra, 2008; Moodley, 2002; Qureshi et al. 2008; Turner et al, 2014). The UK literature in this field has been criticised for being under-theorised, fragmented and piece meal in nature and does not appear to be consistently improving over time in the UK (George et al, 2015). In addition the trainings are often not evaluated or assessed beyond subjective measures (Bentley et al. 2008; Dogra et al. 2005). The lack of conceptual clarity has inevitably created a great deal of uncertainty as to what CCT actually is and whether or not it is beneficial. |
| To date, there has not been a systematic review of the UK literature regarding CCT in healthcare. This paper reports on a study which examined how cultural competence training is conceptualised in the context of UK healthcare settings. The two research questions were: |
| • How is cultural competence defined and articulated in the literature? |
| • What are the underlying drivers for the development of CCT, as reported in the literature? |
Methodology
|
Critical Interpretive Synthesis
|
| Critical interpretive synthesis (CIS) is a method for interpreting a comprehensive body of literature in a useful and insightful way (Dixon-Woods et al. 2006; Flemming 2010; Heaton et al. 2012). In this study CIS offered an approach to the whole process of reviewing a body of literature, rather than merely a synthesising component (i.e. meta-analysis). It advocates a preference for reflective, flexible, iterative analysis of eligible studies. The primary aim is to explore the ways in which a phenomenon and its underlying assumptions are constructed. It allows the synthesis of diverse sources of information into a format that is both empirically and theoretically grounded whilst offering a sense of critique (Dixon-Woods et al. 2006). Although relatively new, this approach counteracts the limitations of conventional systematic reviews and is justifiable in this context as diverse sources of literature were relevant to the research questions. A critical approach allowed clarification of the current conceptualisation of CCT and relevant issues surrounding the topic. CIS also allows a large body of literature to be examined, unlike other interpretive techniques. |
| Although systematic reviews are a well-established method for identifying, appraising and summarising a body of evidence, they are best used where there is a basic homogenous phenomenon and the comparability between studies is sufficient to allow the data to be aggregated for analysis (Mays et al. 2005). Cultural competence is not consistently defined nor operationalised across the field. The literature is diverse and complex. In addition, there are substantial adjunct literatures that contribute to the field and understanding of cultural competence including values, minority health issues and inter-ethnic relations. |
| CIS emphasised continual critical interpretive thought whilst ensuring transparency and explicitness regarding the method. The design incorporated methods used in conventional systematic reviews within the format of CIS. Explicit pre-tested search strategies were implemented to ensure replicability as well as specified eligibility criteria ensuring broad inclusive standards to aid in retaining diverse sources of evidence (Mays et al. 2005). Transparent data extraction procedures, a co-rated approach in determining the inclusion of studies and a quality appraisal tool were used in the analysis of studies to dissipate any personal informed judgement that might be present and to enhance comparability between studies. CIS adopts a flexible, iterative approach to formulating the research question, searching the literature, study selection, quality appraisal and extraction of data (Dixon et al. 2006). This integrated approach was seen as important in ensuring explicitness in methods and improving the accuracy of conclusions. A description of each stage of the study is described below. |
| Search strategy |
| Five electronic databases were searched: MEDLINE, EMBASE, CINAHL, PsycINFO, and Social Policy and Practice. NHS Evidence, PsycEXTRA and NICE Evidence Search were also searched but did not yield any additional items. The search strategy comprised of free-text terms and a mixture of controlled-vocabulary terms, which varied, to allow for any inadequacies in the indexing of certain databases. Acknowledgement of the multiple/related terms and meanings of the words ‘culture’, ‘competence’, ‘training’ and ‘ethnic minority groups’ was considered to maximise the retrieval of relevant studies. |
| Pilot searches were developed, tested and adapted using comparable indexing terms specific to certain databases. The search strategy was continually refined iteratively and time was taken to ensure it evolved organically. The search strategy was heavily augmented through reference chaining, consultation with experts and key-terms listed within relevant studies to increase the empirical applicability. Reference chaining of all relevant items was seen as essential, as the small body of evidence relevant to this field is generally not well-defined and is disparately spread out in different research areas. The pilot searches revealed that in the UK literature ‘cultural competence’ was synonymous with ‘racial inequalities’ in healthcare; studies which addressed issues of race could be easily captured by using the terms ‘culture’ and ‘equality’ in the search strategy. The term ‘race’ was not included in the search strategy to ensure the studies captured were focused on ‘cultural competence’ and not racial issues. The final search strategy is shown below: |
| (Process OR processes OR outcome OR outcomes OR assessment OR healthcare quality OR evaluation OR indicator* OR effective* OR impact OR curricul* development) AND (cultur* OR diversity OR equality OR cultur* awareness OR cultur* sensitivity OR cultur* literacy OR multi-cultural OR ethno-cultural care) ADJ6 (training OR assessment OR education OR teaching OR curicul* OR competency) AND (healthcare OR NHS OR National Health Service OR medic* OR nurs* OR pharm* OR health-related OR private healthcare) ADJ6 (setting* OR system* OR service* OR institution OR course* OR student*) AND (UK OR United Kingdom OR GBR OR Great Britain OR Britain OR England OR Scotland OR Wales OR Ireland) |
Eligibility criteria
|
| Inclusion criteria aimed to achieve ‘maximum explanatory value’ rather than simply an aggregation of similar concepts (Dixon-Woods et al. 2006). Consequently, preference was given to conceptual relevance rather than methodological rigour. |
| The inclusion criteria were |
| a) Studies investigating CCT in healthcare institutions/ healthcare teaching settings among healthcare professionals or prospective healthcare professionals who had or would have direct contact with patients. |
| b) All research designs and diverse sources of evidence including opinion pieces, multi-component studies and or training programmes which contained CCT. |
| c) Items/ papers published in English. |
| d) Items/ papers specific to the context of UK healthcare. |
| There was no set time period but where databases had a specific time period papers were searched from 1990 to 2013. Items/ papers that were not specific to UK healthcare or not available in English were excluded. |
Selection
|
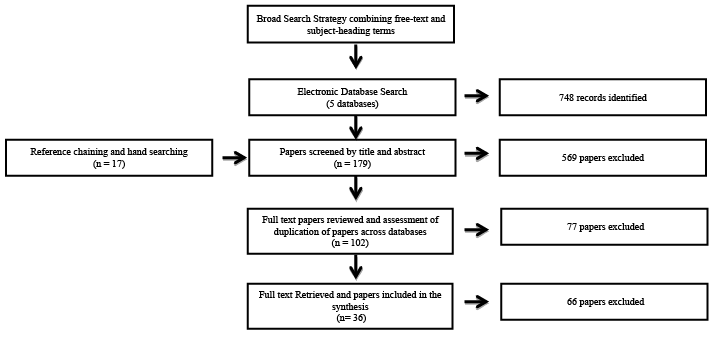
| A total of 748 unique items were found. Purposive sampling in accordance with the inclusion and exclusion criteria was then used to focus on the retrieval of items/ which explicitly described CCT in the UK context within the title and abstract. Theoretical sampling was then employed and items were selected based on their relevance to theory generation and their explanation regarding the review question to develop the emerging analysis (Figure 1). The selection of items was an iterative process which continued throughout the analytical stage. Items were co-rated by RG and SF to enhance reliability and validity of the findings. A total of 36 items, from a time span from 1996 – 2012, were chosen to be included in the synthesis. |
Quality appraisal
|
| CIS does not formally appraise the quality of literature, as a single quality appraisal tool would be insufficient to assess diverse items and heterogeneous study designs. However, in this study, a structured quality appraisal checklist constructed by Hawker et al. (2002) was used. This offers a transparent scoring system for each item, similar to the appraisal of randomised control trials and has been shown to be beneficial for CIS as it encourages reviewers to be unambiguous regarding the reasons behind their judgments (Hawker et al. 2002, Sandelowski et al. 2002). Judgements about credibility i.e. looking into the background of the authors and the contributions of items to current evidence through citation ratings were also explored to ensure that seriously flawed items were excluded but weak methodological papers which might prove theoretically insightful were included (Annandale et al. 2007). |
Data analysis
|
| The data analysis involved in CIS is similar to qualitative research and aims to produce a theoretical output in the form of a synthesising argument. This argument is a comprehensible theoretical framework which can be used to describe the findings as a whole. The standard method for data extraction analysis as outlined by Dixon Woods was adopted (Dixon-Woods et al. 2005). Key information from each item was extracted and formulated (Table 1(Included as supplementary data)). |
| Findings |
| Figure 2 shows a summary of the literature analysed. CIS was performed on 36 items and 2 synthetic constructs, also known as ‘themes’ or ‘categories’, were identified. Viewed together these generated a synthesising argument termed ‘institutional commitment’. Table 1 (Included as supplementary data) shows which items in the review contributed to the following themes and sub-themes below. |
Conflicting concepts
|
| This synthetic construct illustrates the areas of contention around defining cultural competence. It reveals significant political influence in the development of CCT and draws attention to the conflicting tensions between the uses of core terminologies relevant to the field. Finally it examines the lack of clarity in the proposed outcomes of CCT. |
i) Interchangeable terms
|
| Many of the items demonstrated that important terms were often used inter-changeably. For example, the term ‘ethnicity’ was favoured over ?race’, because of its progressive salience and acceptance among service-users as well as its compatibility with the concept of individualised care (Pfeffer, 1998; Afshari and Bhopal, 2010). However, the manner in which ?ethnicity’ was articulated appeared to be ‘colour-coded’, identifying social groups based solely on their skin colour and was often applied to those who were non-White. Issues of ?race’ were thus subsumed in the term ‘ethnicity’ and ?many features of racial thinking have permeated concepts of ethnicity and culture’ (Ahmad and Brady, 2007). ‘Ethnicity’ was rarely debated with regards to the ‘white’ race. Arguably the significance of ‘white’ ethnicity is equally applicable to that of ‘black’ ethnicity but white ethnicities were frequently overlooked (Pfeffer, 1998). The concept of the white ‘ethnicity’ was rarely addressed in relation to CCT. It seemed entirely focused on oppressed minority groups, so called ‘other’ cultures (Ahmad and Bradby, 2007). In CCT, ?minority groups appeared to be more relevant than White British…..ignoring reverse racism’ (Bennett et al. 2007; p.30). |
| The focus on ‘ethnicity’ appeared to stem from definitions of ?culture’ which was frequently defined in terms of emphasising group-based distinctions. Members of minority ethnic groups were classed as having a ?culture’ whereas the majority population was not. Definitions of ‘cultural groups’ often tended to categorise groups of individuals based on a ‘property of factors’ (Bhui and Bhugra, 1998). The analysis suggested racial inequalities were explained as a consequence of cultural differences, which in simple terms described the tension between the dominant white race and non-white races (Cully, 1996; Gurnah, 1984; Peckover and Chidlaw, 2007). |
| Definitions of cultural competence focused on catering for members of ethnically diverse populations. For example, Cross et al., (1989; p.2) described cultural competence as involving: |
| ?systems, agencies and practitioners with the capacity to respond to the unique needs of populations whose cultures are different than that which might be called the ‘dominant’ or ‘mainstream’ |
| In another example cultural competence is defined as: |
| “A continuous process in which the nurse strives to develop an ability to work effectively within the cultural contexts of an individual, family or community from a diverse cultural/ ethnic background.”(Camphina-Bacote, 2001; p.2) |
| The most common definitions were American; there was minimal questioning of the validity of importing definitions for UK settings. |
| Analysis suggested that CCT was introduced as a vehicle for tackling racism and racial inequalities. A few authors questioned the notion of CCT being a single-handed approach to resolving discriminatory practices (Bennett et al. 2007; Dogra et al, 2007; Bentley et al 2008). These papers conveyed the role of ‘culture’ in health related behaviours and appeared to suggest cultural differences as an explanation for health inequalities experienced by Black and ethnic minority groups. However authors like Gregg (2004) felt that other reasons such as racial bias were contributory factors to health inequalities. Gregg argued that ‘race is not culture and racism is not simply a lack of cultural competence’ adding that issues based on individuals’ cultural differences are questions of racial bias (Gregg, 2004). The root causes of health inequalities appeared to be assumption-based as opposed to evidence based. |
| ‘Ethnicity’ and ‘race’ were often commonly used to refer to ethnic minority groups, and ‘culture’ appeared sub-summed with these two terms. There was a lack of conceptual clarity in how these terms were defined and distinguished from each other. Many authors saw CCT as a method of increasing the capabilities of health providers in adequately meeting the health needs of member of non-white minority ethnic groups. Theoretical frameworks relating to ‘cultural competence’ were noted in a few of the items. These used broader definitions of culture and described the need for healthcare professionals to tailor care to individual needs, as opposed to only those of ethnic minority groups. The simplistic use of culture in policy documents suggested that ethnic groups were categorised by race as White, Black, Asian ?who are all the same, thereby, having a culture that is mutual and static’ (Le Var, 1998; p.3), this was apparent in both early documents and more recent policies in 2015. The manner in which the complexity of ‘culture’ was conceptualised was not reflected in policy documents. |
| Dogra et al. (2005) highlighted that the term ‘diversity’ encompasses a range of groups within society which are identified by characteristics other than culture and ethnicity (Dogra & Carter-Pokras, 2005). Diversity also acknowledges a range of ‘differences’ relating to individual characteristics, as exemplified in this example: |
| “working in partnership with service users, carers, families and colleagues to provide care and interventions that not only make a positive difference but also do so in ways that respect and value diversity including age, race, culture, disability, gender, spirituality and sexuality” (Hope, 2004: p.3). |
| Hope draws explicit attention to discrimination in healthcare systems. ‘Diversity’ became a favourable term as it broadened the concept of CCT and articulated it in a manner that did not minimise racial equality but also considered other dimensions (Bhopal, 2012; Hunt, 2007). ‘Diversity’ acknowledged ‘differences’ in systems of shared cultures and values. Although values, beliefs and practices could be shared in a ‘culture’, ‘diversity’ recognises the heterogeneity among single cultures and identifies characteristics that are autonomous and distinct (Dogra, 2005). The notion of ‘diversity’ appeared compatible with individualised care which drew attention to the unique needs of each patient. One author termed diversity as the ‘more modern term for inequalities’ (Pegg, 1997), this perception was also reflected in recent equality and diversity NHS legislaions. |
ii) Politically driven versus clinically driven
|
| CCT appeared to have developed out of efforts to bridge the cultural divide between predominantly ‘White’ biomedical cultural perspectives and those of Black and ethnic minorities. It became largely targeted towards minority populations and those whose health beliefs differed from Western ideas (Hunt, 2007; Kai et al. 2001). Theoretical models of cultural competence emphasised that clinicians and trainers needed to develop ‘cultural expertise’ in particular cultures in order to be effective providers (Curcio, Ward, and Dogra, 2014). Learners were expected to formulate levels of knowledge about specific cultures, their history, traditions and core beliefs as they affected care provision. There was also the expectation that learners would develop skills based on this knowledge including cross-cultural communication skills, and the development of culturally sensitive treatment plans. This model of ‘cultural expertise’ was reflected in definitions of ?culture’ which favoured group-based distinctions, categorising clusters of individuals based on a property of factors such as religion, race or ethnicity (Bhui, Ascoli, and Nuamh, 2012). |
| CCT appeared politically driven as a strategy to reduce health inequalities, which primarily focused on the ‘victims of inequality’ (Gould, 2009) who were non-white. Many of the items demonstrated a continuous political progression towards achieving equality in healthcare among service-users and service-providers as conceptualised in the Royal College of General Practitioners’ Curriculum statement; “equality is about creating a fairer society in which everyone has the opportunity to fulfil their potential.” (RCGP, 2007). |
| UK health services were designed to cater for more homogeneous communities, with a few authors’ labelling it as a ‘White dominated NHS’ (Sheikh et al. 2008). Reports of health inequalities, disparities in the quality of care and lower rates of satisfaction with healthcare provision among minority groups illustrated that the NHS was struggling to meet the needs of minority communities particularly where these differed from the majority and disregarding the other contributing factors which might be involved. CCT appeared to be conceptualised in a way that divided the population into two; the majority and the minority: |
| ?The training] feels like something that is done to us rather than something that we participate in. Nature of the training is ‘us’ and them [non-British]. Training is imposed, no dialogue. If you force the issue on people they will not listen? (Bennett et al. 2007) |
| CCT was proposed as a response to some high profile cases in which issues of race and racism had played a major role, for example, the Stephen Lawrence Inquiry (MacPherson, 1999) and the David Bennett Report in 2003. Critics of the definition of CCT claimed it was formatted according to ‘political correctness’ (Bennett et al. 2007), as exemplified in a participant’s statement: |
| ?What we have at the moment are largely good intentions...that's a start, I suppose...but we won't get anywhere without the curriculum board grasping the nettle and getting proactive.’(Kai et al. 2001) |
| Authors as well as study participants collectively raised concerns that political requirements rather than clinical and educational need were driving the development and delivery of CCT (Dogra et al. 2009; Dogra and Wass, 2006). The literature implied the field was more prone to being re-energised and strengthened by political motives as opposed to the changing training/ clinical needs among healthcare professionals. |
| Health policies emphasised theorising equality, at the expense of providing a sound evidence-base for specific teaching, training methods and defined measurable outcomes for these programs. The literature conveyed the tendency to focus on uniformity rather than diversity. There appeared a struggle in mediating the need for ‘equality’ and the right to acknowledge and cater for ‘diversity’. One participant’s observed that ‘you feel a sense that what is done is being `politically correct without the heart' (Kai et al. 2007). Authors argued that conceptualizing CCT within the parameters of ‘political correctness’, might inhibit change: |
| ?As awareness of racial and ethnic group oppression increases, students are less likely to voice publicly an opinion that might be construed as racist. It is difficult to determine whether racist attitudes have actually decreased, or whether ‘political correctness’ merely inhibits people from expressing them’ (Eliason and Raheim, 2000; p.4). |
iii) Equitable care versus individualised care
|
| The analysis indicated a tension between the proposed outcome of CCT in advocating either the practice of equitable and individualised care. Ensuring equality was clearly predominant in the majority of items and mirrored in authors’ opinions. For example Peckover and Chidlaw (2007, p.5) stated that healthcare providers have ?a responsibility to provide services fairly and equitably to all clients, regardless of their ethnicity or cultural backgrounds’. The language used in advocating equitable care seemed to diminish the importance of ensuring individualised, patient-centred care. Common terminology in equality and diversity health policies such as ‘regardless of their ethnicity or cultural background’ (Peckover and Chidlaw, 2007), ‘irrespective of difference’ or ‘without regard to ethnicity’ (General Medical Council, 1993) seemed to further exacerbate the perception that CCT was politically rather than clinically defined. |
| ?what does treating all patients the same, irrespective of their race or colour mean? Education and training should prepare all healthcare professionals to treat each patient and client as an individual, taking account of the specific cultural background.’ Le Var (1998; p.6) |
| ‘Diversity’, defined as recognising and valuing differences challenged the practice of ?equality’ in treating individuals the same regardless of their differences. ‘Diversity’ questioned the assumption that applying the same practice was generally valid for all persons and that equal care resulted in equal outcomes. |
| The ethos of individualised care was deeply embedded and accepted within the UK healthcare practice (Gerrish, 2000). The analysis revealed a greater awareness of the concept of equality in healthcare was needed: ?equitable care does not mean the same care. While public healthcare may be about services to groups of the population, clinical care is about service provision to individuals’ (Dogra and Carter-Pokras, 2005; p.14). Although the ‘we treat everyone the same” approach was well intended, it was often argued there should be a higher emphasis on individualised care and developing individual solutions to individual problems. For example research the care given to minority groups needs to be approached differently to the general population to ensure the health needs are met and there are comparable health outcomes (Bheenuck et al.,2007). |
Incongruence between theory and practice
|
| This construct drew attention to CCT in action and the simplicity of the content. It also examined the assumption that cultural competence could be imparted either through knowledge-based learning or practical experience and whether cultural competence was indeed a specific attainable skill set. |
i) Over-simplification in teaching
|
| There was a unanimous acknowledgment that definitions of culture are complex, nuanced and varied depending upon context and discipline. The literature conveyed the incongruence between how ‘culture’ was theorised and how it was interpreted and defined in CCT. The content of CCT was over-simplistic. There was a preference for conceptualising cultural issues as simplistic facts about specific ethnic groups’ religious and dietary needs. Healthcare settings favoured a ‘recipe’ or ‘fact file’ approach to learning (Hawthorne et al. 2009; Hutnik and Gregory, 2008). Bennett et al. 2007; Kai et al. 2000; Dogra et al. 2004, from a variety of different medical fields, advocated recognising culture as a dynamic process and warned against the presentation of cultural issues as facts, claiming that it promoted stereotypical thinking which: |
| ?Stripped minority cultures of their complexity, contingency and dynamism and presented them as static, homogenous artefacts, whereby all members of a ‘culture’ were assumed to share common features’. (Bennett et al. 2007; p.2) |
| Insensitivity towards complex cultural issues encouraged ‘unwelcome stereotyping” (Kai et al. 2001). Items showed that healthcare providers’ perceptions of learning about different cultural groups were negative, as they felt it was impossible to learn information about all cultures; ?it is acknowledged that is almost impossible to be expert in all cultures as there are more than 3000 cultures’ (Narayanasamy, 2003: p.4). |
| CCT was often provided as a separate distinct course despite its relevance in all areas of professional practice, values-based practice and patient-centred care The content of most CCT assumed that the healthcare needs of minority ethnic groups were homogeneous and that individuals of the same group were uni-dimensional, defined by their ethnicity alone. The simplistic categorisation of ethnic groups into fixed classifications was only marginally criticised; the grouping persisted as ?unquestioned constructs’ (Kai et al. 1999). The cultural practices/stereotypical knowledge learnt through training were often incongruent with the reality of issues faced by patients. Staff felt that individualised care was more appropriate but fears of asking the wrong questions often prevented them: |
| ?I don’t really think we understand other cultures…We can always very easily put our opinions (that) we think this is what’s happening…but we can’t do that, because other people’s cultures are different. We can only sort of see the outside of what’s actually happening within these cultures. I think that’s where patients lose out really’ (Kai et al. 2007). |
ii) Cultural competence achieved through learning or experience
|
| There appeared to be an assumption that cultural knowledge led to ‘cultural expertise,’ proficient knowledge of all cultural groups, among practitioners and therefore to cultural competence. There was little direct evidence of this. Research tended to focus on expert opinion and what had been done elsewhere, mostly USA (Dogra and Karnik, 2004). Whilst studies did report positive results on the improvement of cultural knowledge and attitudes, little evaluation was done to explore the how this improved services for minority populations (Bhui et al. 2007; Dogra and Wass, 2006). |
| The practical dimensions of cultural care took precedence over other aspects of cultural competence in the teaching content of CCT (Narayanasamy, 2003). A few authors’ noted that these practicalities, such as language, food and religion were the responsibility of health institutions rather than practitioners, yet it appeared cultural issues in care were addressed as if this was not the case. Teaching reflected a superficial understanding of healthcare practitioners’ role. For example, when asked to describe how they might meet a patient’s cultural needs, the response was: ?moving a bed in a side room so that the patient was facing the correct way for praying’ (Narayanasamy, 2003; p.6). Cultural care appeared synonymous with addressing practical issues; minimal attempts were made to dissect the complexity of cultural issues in the clinical context at both a patient and provider level. |
| It was often strongly argued that, in order to achieve an attitude change, CCT needed to occur outside the context of clinical practice, during study-abroad programmes and work within ethnic minority communities (Greatrex-White, 2008). Evidence for this argument is lacking. One article in particular strongly advocated the benefits of study-abroad programmes for increasing cultural awareness and helping in the development of cultural competence (Koskinen and Tossavainen, 2003, 2004). The literature reflected an ethos of ‘clinical education by default’, describing the persistent tendency to disregard situational, cultural and contextual factors essential to professional practice, due to the assumption they are ‘easily picked up’ (Edmond, 2001; p.1). Arguably the constant change in the demographics of the healthcare system demands a clear understanding of the expectations and pace of the clinical context which can only be successfully achieved through practice education. Equating academic excellence and rigour as the primary source for preparation to practice is questionable. Curriculum developers and educators appeared to overemphasise theory and devalue the importance of practical clinical experience (Edmond, 2001; Koskinen and Tossavainen, 2003, 2004) in regards to achieving cultural competence. Authors often highlighted the impact that lack of the practical experience with cultural issues can have on professional development as a whole: |
| ?If work-based philosophy is rejected…we serve only to deny practitioners the opportunity to become truly immersed in their craft…thus stunting professional and personal growth and decreasing an understanding of organisational development’ (Edmond, 2001;p.2). |
Discussion
|
Synthesising argument
|
| CCT is under-developed, under-theorised and piecemeal in nature. A large proportion of CCT in the UK has been founded on ‘shared political recognition’ and common goals towards equality of outcomes as opposed to rigorous theoretical frameworks which describe the role and influence of culture in clinical encounters. The review demonstrated how the literature is primarily framed in two broad directions; normative persuasion and implementation recommendations. ‘Normative persuasion’ describes the literature which advocates the importance of CCT, highlighting its influence in clinical settings and citing specific indicators of pervasive health inequalities and the need for ‘culturally competent care’ (Good et al. 2002; Richardson, 1999). ‘Implementation recommendations’ capture the suggested ‘best practice guidelines’ often derived from opinion based pieces around the implementation of training programmes. CCT has blossomed fruitfully on a policy level but has not been translated to actual changes in clinical practice and service provision. |
| The growth of this field has been more susceptible to political motives as opposed to clinical and educational need. This review shows how the UK literature about ‘cultural competence’ is predominantly empirically, rather than theoretically driven. As a consequence, the field lacks conceptual clarity and rigour with regard to addressing cultural issues in practice when caring for a diverse population. Culture has become a characteristic that can be theorised as a 'property of certain individuals' conforming to similar religious beliefs, norms and traditions irrespective of the heterogeneity within each group. This has resulted in the term ‘cultural competence’ emerging as an ‘umbrella conceptual framework’ (Ming-cheng et al. 2008), denoting ?an assorted array of efforts that aim to provide quality care to patients irrespective of race, ethnicity, culture and language’ (Betancourt et al. 2005; pp.1). This conceptual flexibility in the notion of cultural competence has allowed it to accommodate the importance of racial and ethnic disparities in healthcare, but also the ‘diverse needs of patients’ and even contradictory views and approaches. |
| The lack of conceptual clarity and coherence can be categorised into three categories: 1.) conceptualisation, 2.) implementation and 3.) assessment and evaluation. Definitions of ‘cultural competence are complex, nuanced and varied depending upon context and discipline (Curcio, Ward, and Dogra, 2012). Similar terms are used interchangeably with one other. The way in which CCT is delivered varies widely across the UK; it needs to be both broader and more systematic. Trainers need to establish a credible connection between CCT and improved patient outcomes. There remains a paucity of well-designed evaluation tools and research, resulting in a systematic lack of empirical evidence documenting the efficacy of CCT. |
Institutional commitment
|
| ‘Institutional commitment’, or the lack of it, represented the heart of the ambiguity around the lack of conceptual clarity and consistency in the development of CCT. Differentiating between key terminologies appeared problematic, as conceptualisations of key terms were blurred, prone to political influence and open to a number of interpretations. There was a lack of conceptual clarity and consistency in defining ‘cultural competence’, the proposed outcome of CCT and how ‘cultural competence’ can be learnt and ascertained. Over time, the patient groups expected to benefit from CCT broadened to include all those whose cultures differed from those of health professionals and ‘diversity’ became an increasingly favoured and utilised term. ‘Institutional commitment’ in particular, in terms of leadership was needed to collectively conceptualise, engage and frame CCT. There was a collective recognition that cultural issues were far more multi-faceted than indicated in statutory guidelines and policy documents. The literature demonstrates the internal tension in health organisational culture between these committed to CCT versus those who take a very tokenistic view. There was a lack of institutional-buy in to CCT. Collectively the findings indicated a predominant lack of institutional commitment to the development and delivery of CCT at multiple levels of the healthcare structure in healthcare practice, organisational, research and health policy stance. This suggests that little progress has been made from the findings of Bentley et al. (2008) study and Dogra et al.’s (2005) survey of cultural diversity teaching in UK medical schools. |
| The approach to CCT was superficial. Cultural issues were frequently presented as one-dimensional phenomena and stereotypes presented as facts. Healthcare providers appeared to be encouraged to adopt premature conclusions and favoured either a generalised, inclusive approach to teaching or a specific, exclusive approach, neither of which had any evidence-base. Aside from the desirability of making healthcare providers aware of cultural differences, more emphasis should be placed on treating each patient as an individual. CCT was primarily assumption-based and in line with prevailing professional preferences and opinions. |
Research implications
|
| The research-base in this field is severely underdeveloped. A core challenge is how to ensure that culture is appreciated and theorised in terms of cultural competence skills without stereotyping. In-order for progress to occur, there needs to be a change from an assumption-based approach to a research-oriented movement that prioritises evidence-based approaches. The majority of papers reviewed were qualitative or descriptive studies. Rigorous experimental designs were scarce, yet needed to guide CCT and management decisions regarding minority patients. The majority of suggestions regarding CCT are based on expert opinions, studies from abroad or low/ medium level evidence. Although various suggestions have been made as to how to ‘ensure engagement’ in CCT, these are yet to be fully investigated. The literature was predominantly focused on non-white minorities; literature exploring ‘white’ ethnicity in CCT might have generated different patterns in the findings and is a potential area for future research. |
| The literature contained discussions and descriptions of health inequalities without adequate analysis to explore the direction and nature of their cause and, frequently, little detail in respect to the specificity of the ethnic group ‘at risk’. Policy-making in the field of racial inequalities remains largely intuitive and would benefit from the incorporation of rigorous evidence-based research. Further research exploring what racism means at the individual, interpersonal and institutional level and how these influence healthcare delivery should be encouraged. Greater attention also needs to be placed on within-group variations and the inclusion of minority ethnic groups in mainstream research. |
| It was also noted that CCT appears restricted to high-income countries. Developed countries are known as ‘multi-cultural’ whilst developing countries are not recognised as having diversity in their populations. CCT appears relevant when there is an explicit racial difference in society. The recognition of heterogeneity among ethnic groups appears overlooked. |
Policy implications
|
| Although there are a range of health policy documents about ‘cultural competence’ which are important guidelines to achieving and setting good practice; these alone are limited in what they can achieve (George et al, 2015). Education and training are the mechanisms by which these guidelines and standards of good practice are operationalised and instilled in individuals (Schneider and Barsoux, 2003). Statutory documents need to provide a higher, explicit level of clarity in what is expected from CCT, for example Turner et al. (2014) suggest that organisations such as the GMC should take a lead in ensuring implementation. Health institutions must ensure a ‘collective authentic commitment’ towards providing training that is compatible with statutory requirements and facilitates sufficient opportunities for its implementation. The political influences and their philosophical stances on CCT need to be made transparent to avoid misinterpretations. Policy documents need to provide clear definitions and instructions to ensure services are culturally-competent. Organisational policies and plans for race equality should specify the training necessary to achieve strategic aims. Racial equalities and issues of ethnicity need to become a consistent focus in policy to ensure on-going commitment. |
Practice implications
|
| Defining the core topics to be covered in CCT and distinctions between key terminologies must be rectified in-order to effectively teach cultural competence. The emphasis on training should be on the improvement of professional practice and not simply the acquisition of knowledge of non-white groups. The guiding principle in CCT has been on equality as opposed to achieving optimal care for all patients. Instead, what is needed is a responsive programme that places individualised care at the centre of CCT and is clinically as well as politically informed. Training should be integrated into a wider framework and be embedded within clinical governance systems. It should address the needs of the organisation and its employees and form part of an overall strategy in reducing racial inequalities. An emphasis should be placed on the interpersonal interactions between service-users and service-providers and the organisational processes that lead to unequal treatments and outcomes. Current approaches to training are inadequate in addressing issues of racism. Organisations should involve their frontline staff or adopt a team-based approach in the development and implementation of training to gain a better understanding of current training needs regarding cultural care, and be adequately prepared to teach cultural competence. In addition, greater examination of the provision and application of individualised care in the context of a multicultural society is needed. Understanding the compatibility and relationship between advocating the principles of ‘equality’ and ‘diversity’ needs to be further explored. |
Limitations of the study
|
| Despite the great potential this methodology offered in exploring CCT within UK healthcare settings, methodological concerns were raised. Concerns over the reproducibility were raised regarding interpretations of the findings. Although recognition of the ‘analyst’s voice’ was a firmly rooted principle of the method, it was felt higher emphasis should be placed on the author presenting findings grounded within the data in a convincing and well-articulated manner. The literature primarily consisted of opinion pieces that were often hard to synthesise and, although interpretive synthesis offered great potential, it was felt a higher level of clarity was needed as to how opinions and expert recommendations could be constructively synthesised. Another limitation of the collection of items is the inconsistent focus on the topic throughout history and the lack of recent research around the field in the UK context, the majority of recent studies are originating from the USA. |
| Incorporating the methods of a conventional systematic review were felt beneficial and should be encouraged with the adoption of this methodology. The lack of incorporation of a quality appraisal method felt it would lead to bias estimates and incongruent findings. However, the quality appraisal method used was found to be inadequate as it could not be applied to all study designs because of methodological diversity. Finding a quality appraisal method that could be applicable to diverse sources of evidence will be advantageous in promoting CIS. |
Conclusion
|
| Concern and attempts to reduce racial inequalities are not confined to the UK; many of the issues identified in the UK settings have parallels in other countries. Although the study has an explicit focus on literature from the UK, the findings may partly have a bearing on other contexts internationally which are facing similar dilemmas with CCT. Current approaches to this type of training are fundamentally flawed. It is important to recognise CCT is not a single-handed strategy for eliminating healthcare disparities; however it is influential in ensuring high quality care to the entire population, if practiced effectively and should be available in all clinical areas. The emphasis must be on the improvement of professional practice and evaluation, be an integral part of the commissioning of training, and should aim to measure both short-term and long-term change. With the ever changing demographics, the desire for CCT will increase. Given the receptive climate towards recognising the importance of cultural issues in the clinical context, the best time to reform CCT is now. |
Figures at a glance
|
 |
 |
| Figure 1 |
Figure 2 |
|
| |
References
|
- Afshari R and Bhopal RS (2010b) Ethnicity has overtaken race in medical science: MEDLINE – based comparision of trends in the USA and the rest of the world International Journal of Epidemiology, 39, 1682-1683.
- Ahmad IUW and Bradby H (2007) Locating ethnicity and health exploring concepts and contexts. Sociology of Health and Illness, 29(6), 796-810.
- Annandale E, Harvey J, Cavers D and Dixon-Woods M (2007). Gender and access to healthcare in the UK: a critical interpretive synthesis of the literature. Evidence and Policy: A Journal of Research, Debate and Practice, 3(4), 463-486.
- Betancourt JR (2004) Cultural competence and healthcare disparities; key disparities and trends. Health Affairs. 24(2), 499-505.
- Bennett J, Kalathi J and Keating F (2007). Race Equality Training in Mental Health in the UK. Services in England: Does one size fit all? London: The Sainsbury Centre for Mental Health.
- Bentley P, Jovanovic A and Sharma P (2008) Cultural diversity training for UK healthcare professionals: a comprehensive nationwide cross-sectional survey. Clinical Medicine, 8(5), 493-497.
- Bheenuck S, Miers M, Pollard K and Young P (2007) Race equality education: Implications of an audit of student learning. Nurse Education Today, 27(5), 396-405.
- Bhopal RS (2012) The quest for culturally sensitive health-care systems in Scotland: Insights for a multi-ethnic Europe. Journal of Public Health, 34(1), 5-11.
- Bhugra D (2008) Psychiatric training in the UK: the next steps. World Psychiatry, 7(2), 117-118. doi: 10.1002/j.2051-5545.2008.tb00173.x
- Bhui K, Ascoli M and Nuamh O (2012) The place of race and racism in cultural competence: what can we learn from the English experience about the narratives of evidence and argument? Transcult Psychiatry, 49(2), 185-205. doi: 10.1177/1363461512437589
- Bhui K. and Bhugra D (1998). Training and supervision in effective cross-cultural mental health services. Hospital Medicine, 59(11), 861-865.
- Bhui K, Warfa N, Edonya P, McKenzie K and Bhugra D (2007). Cultural competence in mental health care: a review of model evaluations. BMC health services research, 7(15), 1-10.
- Camphina-Bacote J (2001) Cultural competence in psychiatric nursing: a conceptual model. Nursing Clinics of North America, 29, 1-8.
- Commander M, Cochrane R, Sashidharan SP, Akilua F and Wildsmith E (1999). Mental health care for Asian, black and white patients with non-affective psychosis: Pathways to the psychiatric hospital, in-patient and after-care. Social Psychiatry and Psychiatric Epidemiology, 34(9), 489-499.
- General Medical Council. (1993). 'Tomorrow's Doctors'., Editor. London.
- Cross T, Brazen B, Dennis K and Isaacs M (1989). Towards a culturally competent system of care. Washington D.C.
- Cully L (1996) A critique of multiculturalism in health care. The challenge for nurse education. Journal of Advanced Nursing, 23, 564-570.
- Department of Health. (1998). The Health of the Nation - a policy assessed: executive summary.
- Department of Health. (2005). Delivering Race Equality in Mental Health Care. An action plan for reform inside and outside services and the Government's response to the Independent Inquiry into the death of David Bennet. London, England.
- Dixon-Woods M, Bonas S, Booth A, Jones DR, Miller T and Sutton, A. J. (2006). How can systematic reviews incorporate qualitative research? A critical perspective. Qualitative Research, 6, 27-44.
- Dixon-Woods M, Cavers D, Agarwal S, Annandale E, Arthur A, Harvey J, and Smith L (2006) Conducting a critical interpretive synthesis of the literature on access to healthcare by vulnerable groups. BMC Medical Research Methodology, 6(1), 35.
- Dogra N and Carter-Pokras O (2005). Stakeholder views regarding cultural diversity teaching outcomes: a qualitative study. BMC Medical Education, 5 (37),1-12.
- Dogra N, Connin S, Gill P, Spencer J and Turner M (2005) Teaching of cultural diversity in medical schools in the United Kingdom and Republic of Ireland: cross sectional questionnaire survey. British Medical Journal, 330, 403-404.
- Dogra N, Conning S, Gill P, Spencer J and Turner, M. (2005). Teaching of cultural diversity in medical schools in the United Kingdom and Republic of Ireland: cross sectional questionnaire survey. BMJ, 330(7488), 403-404. doi: 10.1136/bmj.38338.661493.AE
- Dogra N and Karim K (2005). Diversity training for psychiatrists. Advances in Psychiatric Treatment, 11, 159-167.
- Dogra N and Karnik NS (2004). A comparison between UK and US medical student attitudes towards cultural diversity. Medical Teacher, 26(8), 703-708.
- Dogra N and Karnik K (2005). Diversity training for psychiatrists. Advances in Psychiatric Treatment, 11:159-67.
- Dogra N, Reitmanova S and Carter-Pokras O (2009). Twelve tips for teaching diversity and embedding it in the medical curriculum. Medical Teacher, 31(11), 990-993.
- Dogra N and Wass, V. (2006). Can we assess students' awareness of cultural diversity? A qualitative study of stakeholders' views. Medical Education, 40(7), 682-690.
- Edmond CB (2001). A new paradigm for practice education. Nurse Education Today, 21(4), 251-259.
- Eliason MJ and Raheim, S. (2000). Experiences and comfort with culturally diverse groups in undergraduate pre-nursing students. Journal of Nursing Education, 37(1), 27-29.
- Eshiett MUA and Parry EHO (2003). Migrants and health: A cultural dilemma. Clinical Medicine, 3(3), 229-231.
- Flemming K (2010). Synthesis of quantitative and qualitative research; an example using Critical Interpretive Synthesis Journal of Advanced Nursing, 66(1), 201-217.
- Gallagher RW and Joshua PR (2001). A meta analysis of educational interventions designed to enhance cultural competence in professional nurses and nursing students.
- General Medical Council. (1993). 'Tomorrow's Doctors'., Editor. London.
- George RE, Dogra N and Fulford, N. (2015). Values and ethics in mental-health education and training: a different perspective. The Journal of Mental Health Training, Education and Practice, 10(3), 189-204.
- Gerrish K (2000). Individualized care: its conceptualization and practice within a multiethnic society. Journal of Advanced Nursing, 32(1), 91-99.
- Gill PS and Green P (1996). Learning for a multicultural society. British Journal of General Practice, 704-705.
- Good MJ, DelVecchio James C, Byron J, Good BJ and Becker, A.E. (2002). The culture of medicine and racial, ethnic and class disparities in health. Russell Sage Foundation, Workshop Paper #199.
- Gould M (2009). Equality: Better outcomes in diverse groups. Health Service Journal, 119(6175), 20-21.
- Greatrex-White S (2008). Uncovering study abroad: foreignness and its relevance to nurse education and cultural competence. Nurse Education Today, 28(5), 530-538.
- Gregg J (2004). Letter to the editor. Journal of General Internal Medicine, 19 (900), 36 (paragraph 35).
- Gurnah A (1984). The politics of racism and awareness training. Critical Social Policy, 11.
- Hawker S, Payne S, Kerr C, Hardy M and Powell, J. (2002). Appraising the evidence: reviewing disparate data systematically. Qualitative Health Research, 12, 1289-1299.
- Hawthorne K, Prout H, Kinnersley P and Houston H (2009). Evaluation of different delivery modes of an interactive e-learning programme for teaching cultural diversity. Patient Education and Counseling, 74(1), 5-11.
- Heaton J, Corden A and Parker, G. (2012). 'Continunity of care'; a critical interpretive synthesis of how the concept was elaborated by a national research programme. International Journal of Intergrated Care, 12, 1-19.
- Hope R (2004). The Ten Essential Shared Capabilities: A framework for the whole of the mental health workforce. London: Department of Health.
- Home Office. (2000). Race Relations (Amendment) Act.
- Hunt B (2007) Managing equality and cultural diversity in the health workforce. Journal of Clinical Nursing, 16(12), 2252-2259.
- Hutnik N and Gregory J (2008). Cultural sensitivity training: Description and evaluation of a workshop. Nurse Education Today, 28(2), 171-178.
- Jhutti-Johal J (2013). Understanding and Coping with Diversity in Healthcare. Health Care Analysis, 21(3), 259-270.
- Kai J (2007). Safety and achieving equality amid diversity in health care. British Journal of General Practice, 774-776.
- Kai J, Beavan J, Faull L, Dodson L, Gill P and A, B. (2007). Professional Uncertainty and Disempowerment Responding to Ethnic Diversity in Health Care: A Qualitative Study. PLoS medicine, 4(11), 1766-1775.
- Kai J, Bridgewater, R., and Spencer, J. (2001). "Just think of TB and Asians", that's all I ever hear': medical learners' views about training to work in an ethnically diverse society. Medical Education, 35(3), 250-256.
- Kai J, Spencer J, Wilkes M and Gill P (1999). Learning to value ethnic diversity-what, why and how? Medical Education, 33, 616-623.
- Kai J, Spencer J and Woodward N (2001). Wrestling with ethnic diversity: toward empowering health educators. Medical Education, 35, 262-271.
- Koskinen L and Tossavainen K (2003) Intercultural nursing. Benefits/problems of enhancing students' intercultural competence. British Journal of Nursing, 12(6), 369-377.
- Koskinen L and Tossavainen K (2004). Study abroad as a process of learning intercultural competence in nursing. International Journal of Nursing Practice., 10(3), 111-120.
- Le Var RM (1998). Improving educational preparation for transcultural health care. Nurse Education Today, 18(7), 519-533.
- Mays N, Pope C and Popay J (2005). Systematically reviewing qualitative and quantitative evidence to inform management and policy-making in the health field. Journal of Health Services Research and Policy, 10(suppl 1), 6-20.
- MacPherson Sir William Report.(1999). The Stephen Lawrence Inquiry. Home Office, London.
- Ming-Cheng ML and Stacey CL (2008). Beyond cultural competency; Bourdieu patients and clinical encounters. Sociology of Health and Illness. 30(5), 741-755.
- Moodley P (2002). Building a culturally capable workforce — an educational approach to delivering equitable mental health services. Psychiatric Bulletin, 26(2), 63-65. doi: 10.1192/pb.26.2.63
- Narayanasamy A (2003a). Transcultural nursing: how do nurses respond to cultural needs? British Journal of Nursing, 12(3), 185-194.
- Narayanasamy A (2003b). Transcultural nursing: how do nurses respond to cultural needs? British Journal of Nursing, 12(3), 185-194.
- National Institute for Mental Health in England (2003) Inside Outside: Improving mental health services for Black and minority ethnic communities in England. Leeds.
- Norfolk, Suffolk and Cambridgeshire Strategic Health Authority (2003) Independent Inquiry into the death of David Bennett.
- Papadopoulos I, Tilki M, and Lees S (2004). Promoting cultural competence in healthcare through a research-based intervention in the UK. Diversity in Health and Social Care, 1, 107-115.
- Peckover S and Chidlaw RG (2007). The (un)-certainties of district nurses in the context of cultural diversity. Journal of Advanced Nursing, 58(4), 377-385.
- Pegg LC (1997) Diversity training and education in the workplace. Journal for Vocational Special Needs Education, 19(2), 62-66.
- Pfeffer N (1998a) Theories of race, ethnicity and culture. BMJ: British Medical Journal, 317, 1381-1384.
- Pfeffer N (1998b) Theories of race, ethnicity and culture. BMJ: British Medical Journal, 317, 1381-1384.
- Qureshi A, Collazos F, Ramos, M and Casas M (2008). Cultural competency training in psychiatry European Psychiatry, 3(26), S49-S58.
- Rex J (2001). The basic elements of a systematic theory of ethnic relations. Sociology Research Online, 6 (1).
- Richardson LD (1999). Patients’ rights and professional responsibilities; the moral case for cultural competence. Mt. Sinai Journal of Medicine. 66(4), 267-270.
- Roberston D, Sathyamoorthy G, and Ford R (2000). Asking the right questions. Community Care, 24-25.
- Royal College of General Practitioners (2007). Promoting Equality and Valuing Diversity Vol. 3.4. London.
- Rwegellera G (1980). Differential use of psychiatric services by West Indians, West Africans and English in London. British journal of Psychiatry, 137, 428-432.
- Sandelowski M, Docherty S, and Emden C (2002). Focus on qualitative methods. Qualitative meta-synthesis: issues and techniques Qualitative Health Research, 12, 1289-1299.
- Schouler-Ocak M, Graef-Calliess IT, Tarricone I, Qureshi A, Kastrump ME and Dinesh B (2015). EPA guidelines on cutural competence training. European Pyschiatry. 30(3), 431-440.
- Secker J, and Harding C (2002). African and African Caribbean users' perceptions of inpatient services. Journal of Psychiatric and Mental Health Nursing, 9, 161-167.
- Sheikh A, Gatrad R, and Dhami S (2008). Consultations for people from minority groups. British Medical Journal., 337, 51-54.
- Teal CR, and Street RL (2009). Critical elements of culturally competent communication in the medical encounter: A review and model. Social Science and Medicine, 68, 533-543.
- Tuner MA, Kelly MJ, Leftwick P, and Dogra N (2014). Medical Teacher. 36(9), 1-4.
- Wagner K, Jones J (2011). Different cultures, different needs. Community practitioner : the journal of the Community Practitioners' and Health Visitors' Association, 84(12), 40-41.
- Zeh P, Sandhu, HK, Cannaby AM, and Sturt JA (2012). The impact of culturally competent diabetes care interventions for improving diabetes-related outcomes in ethnic minority groups: A systematic review. Diabetic Medicine, 29(10), 1237-1252.
|



