Research Paper - (2014) Volume 22, Issue 1
Research Fellow
Jan Radford MBBS FRACGP MPsych MEd*
Associate Professor of General Practice
Anne Todd BPharm AACPA
Primary Care Clinical Audit Coordinator
Launceston Clinical School, University of Tasmania, Australia
Received date: 21 October 2013; Accepted date: 15 November 2013
Background Expanding clinical teaching opportunities is essential for securing a sustainable health workforce. Although Tasmanian general practitioners (GPs) are keen to provide learning opportunities for medical students, they have identifed time pressures due to a need to meet patient service demand and a need for more guidance on effective clinical teaching, as factors impacting their ability to increase clinical supervision. By developing a clinical audit activity, we delivered an educational resource that did not require direct GP supervision yet provided meaningful learning outcomes for students. Through systematically reviewing patient records it was hoped that students would strengthen practicebased quality improvement activities, thus ‘giving back’ to their placement practice. Methods A clinical audit curriculum was developed for fourth-year medical students at the Launceston Clinical School (n = 46) and implemented during their general practice rotation. This included a lecture and tutorial, and structured activities based on an audit of diabetes care. Preparation and support was provided to GP supervisors and practice staff through ongoing practice visits conducted by school academics. Implementation of the curriculum within general practice was evaluated through focus groups conducted with staff from five training practices (n = 29). Evaluation of student experiences is ongoing. Results This paper reports on the experiences of general practice supervisors and other practice staff. GPs and practice staff responded positively, indicating that the syllabus provided novel teaching opportunities and a modest contribution to improving patient records and patient care. Major learning opportunities identified included the development of skills working with patient records and practice software, and understanding the importance of accurate and reliable medical records for the optimal delivery of patient care. Conclusions Conducting clinical audit provides students with novel learning opportunities while also strengthening the capacity of teaching general practices to provide clinical placements. Students learnt about the importance of monitoring professional practice using systematic clinical audit, and the complexities of managing patients within primary care. In so doing, they enhanced the robustness and rigor of patient records within their placement practice.
clinical audit, general practice, precep-torship, professional education, quality improve-ment
In response to health workforce shortages, Australia has seen a rapid increase in student enrolments across a range of health disciplines. This increase has required an expansion of clinical training opportunities. This, in turn, has placed a burden on health service pro-viders and individual clinicians to increase their teaching and supervision, in an environment of lim-ited funding and considerable time constraints.[1–4] Within this climate, it is important to support existing clinical supervisors, bring new supervisors on board and develop novel clinical training opportunities wherever possible. Our project directly contributes to this effort through the development of a semi-structured teaching resource that draws on an aspect of clinical care, clinical audit, for use by Tasmanian general prac-titioners (GPs) supervising undergraduate medical students. By creating a clinical audit curriculum, we sought to provide a package that delivered peda-gogically sound learning outcomes for students while broadening their experience of the complexities of primary health and the challenges of providing effec-tive ongoing care for patients with chronic, complex conditions. An equally important issue was whether we could develop a resource that was of benefit to GP supervisors and teaching practices. Specifically, our aim was to test the hypothesis that the audit activity could trigger new teaching opportunities for GP supervisors without necessarily increasing the amount of time spent with students providing direct oversight.
Setting and study cohorts
This project involved two cohorts; GPs and practice staff in northern Tasmania, and fourth-year medical students. This paper reports on the experiences of GPs and practice staff.
In 2012, fourth-year medical students in northern Tasmania undertook a six-week placement in general practice (n = 46). Ten teaching practices were involved with teaching medical students during the calendar year, eight of which participated in the project. The remaining two teaching practices cited a lack of physical space and secure computer terminals for student use as the reasons for not participating. The eight partici-pating practices ranged from large multi-practitioner and multidisciplinary group practices, through to a solo practice.
Students received practical instruction on how to conduct an audit of electronic patient records using the Pen Systems Clinical Audit Tool (PenCAT).[5] A series of workbooks, based on a Diabetes Australia audit,[6] were developed for students to complete while on theirGP placement. The frequency of routine practice site visits by Launceston Clinical School academics was increased to inform staff about the audit curriculum and give instructions on specific student activities.
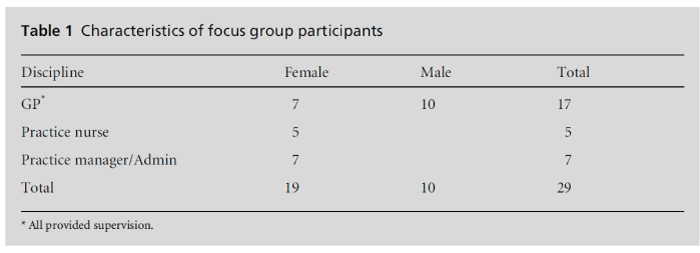
Focus groups were conducted between July and September 2012, at five training practices. Discussion group ranged between three and ten participants and included supervising and non-supervising GPs, practice nurses, practice managers and sometimes other administrative staff who assisted the students (Table 1). Thematic questions were asked, addressing perceived educational outcomes for students; the amount of work incurred for practice staff; the extent to which practice staff (especially supervising GPs) engaged with students about the audit; and whether the project increased their capacity to have students in their practice (Box 1). Feedback fromstudents was analysed separately, and will form the basis of another paper.

Focus group data were analysed using open-coding and thematic analysis.7 NVivo qualitative data analysis software was used to assist with data coding and analysis.8
Major themes that emerged during the practice focus groups are listed in Table 2.

Challenges for the practice
During the early phase of the project there was a lack of clarity around the anticipated level of involvement of the practice team. GPs and practice staff reported difficulties in knowing what was occurring with the audit activities the students were undertaking, with keeping track of their findings or with knowing what feedback they should be providing:
... with the last student I was left his auditing notes [to provide feedback] but I wasn’t told what to do with them so then he came in and said, ‘oh you know I need my auditing notes for me to finish my study’ ... that didn’t happen because I hadn’t caught up with everything ... (Female GP)
While this underscored the need to provide training to practice staff about the audit modules, it also highlighted problems with how the student activity was occurring. First, students did not undertake the audit reviews in the presence of any GPs, so it was possible that their supervisors were unaware of when the activity occurred, or how it was organised:
•.. as I said, sometimes though they would be here and I didn’t know they were until they were about to leave ...(Male GP)
I found it was a little bit messy for the students more than their placements, because their placements were a bit more structured than the auditing days ... (Male GP)
Second, although GPs were interested in discussing the work students were doing for the audit it was not something that happened during ‘corridor conver-sations’. Instead, a structure and a process needed to be put in place to ensure time was set aside to discuss audit findings. When left unscheduled, other pri-orities could arise meaning no such discussion oc-curred:
•.. and then I think [Dr Y] got held up with patients and couldn’t get into the student and then the student had to go because they planned on meeting with [Dr Y] and showing him their results. (Female Practice Manager)
•.. it would make more sense to actually have an appoint-ment time set aside to do that rather than just ‘Oh – we will just see if we can catch her’. (Female GP)
You know what we have to do for that to work nicely for the students, we will have to formalise it ... make a formal time .... (Male GP)
We wanted to know whether the practice team thought learning opportunities were being prompted by the audit. The main opportunity identified related the use of medical records, with clarification of clinical questions arising from audit results also being men-tioned. There was a clear acknowledgement that the audit activity required students to become familiar with managing medical records and systems software within general practice, to a greater degree than had previously occurred, including reflection on the rela-tionship between accurate records, data quality, quality care and patient outcomes:
[teaching the] concept of how their data entry and how GP’s data entry can affect systems in the practice and patient outcomes and practice development was very valuable because they see a patient in front of them and think ‘this is it’ but they don’t realise that there is a bigger picture there, I think it really helped. (Male GP)
There was an acknowledgement that the findings of the audit provided opportunities for discussion about clinical management of particular patients. For example, when considering why patients might fall outside recommended guidelines, one GP noted:
•.. (the student) had two or three questions and we just went over it and sorted them out. (Male GP)
We wanted to know whether clinical audit could offer a mechanism for increasing the capacity of teaching practices to provide clinical placements, and it was generally acknowledged that ‘audit’ provided an op-portunity to increase the amount of time students spent at the practice:
Yeah, things like this audit that they can do without involving us directly all the time, now that we’re set up they’re welcome any time. (Female Practice Manager)
But equal with the activity itself, was the perception that it could not take place unless there was a dedicated space for students to work. The issue of space marks a key difference between training in a larger hospital where students can access a greater range training infrastructure, compared with smaller community settings and private practice.[9] A number of practices were in the process of extending their practice space using funding distributed through the Primary Care Infrastructure Grants programme.[10] They stated that the extra and protected physical space was crucial for supporting student placements and for enabling the audit activity to take place:
The big problem now is that [the students] are not getting a good run at the moment because they rarely get a room to themselves. (Female GP)
Now that we have a dedicated space for them it should be easier ... Mechanically difficult to start off with, but once they moved into that other room it was fine. (Male GP)
Quality improvement
A core objective of quality improvement activities is their ability to prompt critical-reflection on ones’ own practice. This was acknowledged as a benefit of the programme:
I think it’s really good for a practice knowing that people are coming in who don’t actually owe you much and are going to look at your notes ... I know you can be a brilliant doctor with appalling notes and vice versa but there is a bit of a correlation I reckon, and I think it just keeps you on your toes. (Male GP)
Key to the success of the project was the question of whether the practices felt the audit resulted in an improvement to their own records or to the care of particular patients. When asked whether participants felt the activity had added anything of value to their practice it was commonly reported that students helped ‘tidy up’ medical records, and in one instance this directly related to identifying and following up ‘non-compliant patients’ in an attempt to improve their level of care:
•.. most of the things that they found that weren’t right, to be frank, were things like we hadn’t inactivated people [closed files where needed]. But at least it tidied up our records ... it meant we could delete people from the data base who might get called about unnecessary things. (Female Practice Manager)
•.. they tidied up some of the patient files when they picked up that some of the diagnoses in the drop down boxes hadn’t been checked [standardised coding had been incorrectly used]. (Female Practice Manager)
•.. I fed back the information to the nurse who does our diabetes cycle of care co-ordination and so the infor-mation that the students have come back with on the audit I fed back to her and she found that really worthwhile because ... there were some patients who were not com-pliant who had come up, and we were able to contact those patients. ... we did have one who hadn’t, when the nurse contacted them, they hadn’t actually taken the medication so we had one that was very non-compliant. (Female Practice Manager)
Clinical audit has, for a number of years, been a core-competency requirement identified in the Australian Curriculum Framework for Junior Doctors,[11] within the UK Foundation programme for prevocational training,[12] and for fellowship of a number of pro-fessional medical colleges.[13,14] There is considerable evidence for the use of clinical audit as an educational platform, with studies reporting both the positive impact of audit-related projects on quality indicators and patient care,[15,16] and an improved understanding of both the theory and practice of quality improve-ment amongst participating health professionals.[17,18 ]As much of this literature is pitched at postgraduate level and within a hospital setting,[19–21] few publi-cations canvas the experience of clinical supervisors involved with the process.[22–24] In addition, much of the published literature on educational audit inter-ventions predates the widespread use of electronic medical records[22,25,26] and lacks sufficient detail aboutthe specific activities to allow them to be replicated.[27] The development of clinical software that enable large-scale review of electronic records has greatly increased the ease with which clinical audit can be conducted.
Our findings suggest that teaching and conducting clinical audit offers an opportunity for increasing the duration of clinical placements for medical students. It does so while providing meaningful learning out-comes for students, and requiring only a minimal increase in the amount of time GPs spend providing one-on-one supervision. While completing the prac-tice-based audit activities students developed a sound knowledge of the importance of clinical audit and quality improvement for ongoing professional prac-tice. In so doing, they gained practical experience with the management and systematic analysis of electronic patient records. The practice-based components of the audit curriculum were well received, with GPs and practice staff reporting that the clinical audit provided previously unexplored teaching opportunities and a modest upgrading of patient records, thereby facilitating improved patient care (including anecdotal accounts of patients who benefited from a recall to review care). This finding is consistent with other audit-based edu-cational interventions in general practice.[22,24,28]
A number of factors contributed to the success of the student audits. Over the course of the academic year (2012) the process became more streamlined, with training practice staff better able to structure the activity into the overall rotation (e.g. scheduling meet-ings to discuss students findings). With the assistance of the project funding, most practices were also able to establish designated student computer facilities, allowing more convenient (though still controlled) access to patient records. The project continues to evolve. In 2013, audit activities were generated by the needs and interest of teaching practices and students were given formal opportunities to present their findings. In addition a number of teaching practices (though not all) now have clear processes in place to ensure im-plementation of quality initiatives resulting from the student audits.
Financial and human resources have an impact on thesuccess of curricula development and maintenance.[27] Developing our audit syllabus was a resource-intensive process and would have been difficult without grant funding that enabled both the development and eval-uation of teaching materials and substantial support for and engagement with GPs and practice staff. Developing and delivering this teaching resource shifted much of the responsibility of facilitating students learning away from the clinical supervisors and onto practice managers and practice nurses, who largely coordinated the activity in the practice, and academic staff who were responsible for designing and assessing audit modules. It is yet to be determined whether this provides a rational approach to clinical education or will be financially sustainable for our medical school.
Limitations of the study
As relatively small number of GP practice staff con-tributed to the evaluation of the curriculum extending the scope of the evaluation would be beneficial. The themes that emerged were indicative of the different discussions that took place. Ideally, a sufficient num-ber of focus groups should occur so that no new issues are emerging and ‘data saturation’ has been achieved.[29] This was not the case with our research, with the number of focus groups being limited by the avail-ability of participating practitioners. The information obtained during focus groups was, therefore, variable. Our research is ongoing, with the expectation that we will explore how this audit curriculum could be implemented in other contexts.
Teaching and conducting student-facilitated audit provided us with a mechanism for structuring activi-ties within a practice setting; activities that supported supervisors and created opportunities for teaching moments[30] which had not previously existed. In so doing, it increased opportunities for student immer-sion within a clinical setting, though not necessarily for increasing the provision of direct medical super-vision. The clinical audit curriculum provided GP supervisors with teaching resources that enabled them to engage students in quality improvement initiatives targeting the needs of the placement practice. As this occurred, students received a grounding in relevant theoretical concepts and practical experience conducting audit. Through the audit, students learnt about the challenges of the longitudinal management of com-plex and often multi-morbid patients within primary care, while reviewing and improving patient records and patient management within their placement prac-tice.
This project received grant funding from Health Workforce Australia.
The project was approved by the Tasmanian Health and Medical Human Research Ethics Committee (ref no H12445).
Not commissioned; externally peer reviewed.
None declared.