What is known on this subject
• Overseas-qualified doctors have always made up at least a third of the NHS medical workforce.
• Geriatric (or old age) medicine has been one of the least popular clinical specialties.
• Occupational clustering tends to be seen as a feature associated with less skilled migrants.
What this paper adds
• The combined effects of fluctuating labour scarcity in sectors of the medical labour market, discrimination
against outsiders and level of skill led to a clustering of skilled migrants in geriatrics.
• Clustering in the geriatric specialty followed advice from more senior doctors who acted as patrons.
• Ethnic clustering was compounded by geography and type of hospital, as opportunities for employment
and progression tended to occur mainly outside London and the south east of England, and away from
teaching hospitals.
Introduction
Since the inception of the National Health Service,
overseas-qualified doctors have been an integral part
of the health service, with 37% of the doctors on the
General Medical Council register in 2008 having qualified
outside the UK (Catto, 2008), particularly in
South Asia. Yet despite some recognition of the significance
of South Asian doctors in the provision of
healthcare in the UK, there has been little research
on their clustering within specific parts of the health
service (see, however, Esmail, 2007). This echoes the
wider literature on ethnic clusters, which has tended to
focus on clustering as a function of lower-level skills,
and ignored the nature and extent of ethnic clustering
that operates within skilled sectors of the labour market.
In this article we show how ethnicity and skill work
together, under certain conditions, resulting in clustering
in areas of employment traditionally associated
with high status. With regard to the health services,
concern has tended to highlight the importance of a
diverse workforce with appropriate representation of
ethnic minority groups (Notter, 2006). However, ethnic
clustering can also be a marker of discriminatory
practices and lack of access to equal opportunities.
Under-representation in some areas can be accompanied
by over-representation in others, a pattern that
is also prevalent in skilled sectors of the labour market.
In this paper we analyse participants’ narratives and
policy documents on the process of ethnic clustering
in the geriatric specialty within the NHS, and the
factors that led to it from the late 1960s. Using evidence
from oral history interviews, we explore some of the
ways in which this clustering was experienced as
discrimination based on nationality, race and country
of qualification. We also highlight some of the intersecting
forms of ethnic clustering based on professional
hierarchy (specialty), geography, type of hospital and
client group that influenced geriatricians between the
1960s and the 1980s. We show how some of these
issues seem to have continued into the 1990s and
beyond, and we raise some questions about what this
means for the future.
The paper draws on two data sets. The first is a set of
oral history interviews conducted by Professor Margot
Jefferys with pioneers who established geriatrics as
a medical specialty in the UK during the post-war
period (the Jefferys interviews are catalogued in the
British Library Sound Archive with the collection title,
‘Oral History of Geriatrics as a Medical Specialty’ at www.bl.uk/catalogues/sound.html (accessed 26 November
2008). They are open access and hence details of
the interviewees have been presented in this paper. However, interviews with the South Asian geriatricians
have not yet been archived and have stipulations for
access. For this reason they have been anonymised).
These pioneers were identified by their peers in the
British Geriatrics Society (BGS). Jefferys’ sample largely
consists of those selected for the BGS ‘Hall of Fame’ of
members who played a significant role in developing
the care of older people in the second half of the 20th
century. This Hall of Fame was established by the then
president Bobby Irving around 1989. Although several
interviewees mention the significance of overseastrained
South Asian doctors in building the specialty,
the Jefferys data set includes only one interview with a
South Asian doctor.
In this paper we use the term ‘overseas-trained
doctor’ for most of the paper, in line with the early
use of this term to cover medical migrants. More
recently they have come to be called international
medical graduates (IMGs). In this research project
they were all ethnically Asian. It is worth noting that
for most of the period about which our interviewees
were speaking, data on ethnicity and on country of
qualification were not routinely collected. Moreover,
even now the types of data collected vary across the
nations, so it is impossible to make UK-wide comparisons.
For most of the period that we discuss,
country of initial qualification was the major marker
of distinction, although this distinction was then racialised,
as for example through the use of the term
‘brown-skinned specialty.’ More recently, the number
of doctors born and educated in the UK but of South
Asian ethnicity has been increasing, so the match
between race and ‘overseas qualified’ has become diluted.
The second data set of interviews, conducted with
doctors trained in South Asia who joined geriatrics in
the last 40 years, complements the Jefferys data set.
The interviews were conducted in 2008–2009 as part
of an ongoing ESRC-funded project (overseas-trained
South Asian doctors and the development of geriatric
medicine’, ESRC grant reference number RES-062–
23–0514) exploring the contribution of South Asian
geriatricians to the National Health Service. The two
sets of interviews together cover a time period of
medical practice from before World War Two up to
the first decade of the 21st century. Geriatrics (now
known as old age medicine) offers us an interesting
site for exploring the processes and experiences of
ethnic clustering in a highly skilled sector of the labour
market. It also raises an interesting paradox because,
although geriatricians are highly skilled and relatively
well paid, geriatrics is viewed as a marginalised area of
medicine within the spectrum of medical specialties.
Similar patterns can be observed in other specialisms,
such as psychiatry and general practice.
Ethnic clustering
In the context of the wider literature on labour market
integration, labour market clustering into niche occupations
has gained considerable attention. Clustering
is seen as the effect of social networks that channel
migrants into specific parts of the labour market, and
is observed to have mixed effects onmigrants (Bonacich,
1973;Waldinger, 1994). Economists, in particular, have
conducted large multivariate studies on occupational
clustering.
For some, clustering can be seen as a manifestation
of labour market discrimination, whereby migrants
find jobs in the few sectors of the labour market that
are open to them. This form of clustering was explained
in the 1970s through a Marxist analysis of labour
market segmentation into a primary market with better
wages and a secondary market with temporary labour
on lower-paid wages, which was largely populated by
migrants (for a more detailed discussion, see Colic-
Peisker, 2006). Subsequently, racewas seen as working
alongside class to segment labour (Reid and Rubin,
2003), so that it is the fertile intersection of race and
class that keeps migrants within limited sectors of the
secondary labour market. This structural analysis has
been added to and refined in subsequent years.
For others, clustering is about people’s agency
within the context of labour market discrimination.
Clustering may be seen as an effect of the way in which
people negotiate networks (Elliott and Lindley, 2006),
or of the social capital that migrants possess, whereby
some migrants are able to network in order to gain
access to particular types of jobs (Schrover et al, 2007).
These studies increasingly differentiate between immigrant
clustering, where all immigrants cluster, and
ethnic clustering, where people fromone ethnic group
employ others from the same ethnic group.
Despite these variations, certain common features
of existing research on clustering can be identified. For
instance, because of the interest in clustering as a
marker of disadvantage, most of the literature on
labour market clustering focuses on entrepreneurship
or on employment in less skilled sectors of the labour
market, such as domestic work (Kloosterman and Rath,
2001). It also tends to look at ethnicisation as a process
‘whereby an association develops between a certain
economic sector and an ethnic group’ (Schrover et al,
2007, p. 535). There is little in the literature on ethnic
clustering as a process that marks migrants in skilled
sectors of employment. Yet as we shall show below,
ethnic clustering may also operate among highly skilled
migrants.
Clustering may also be analysed as a mark of relative
failure within the labour market. As a result, social
networks that lead to clustering are usually seen as
disadvantageous both to labour market integration and to social mobility (Smith et al, 2006). However,
the terms and basis of social mobility and labour
market integration are often not interrogated. As a
result, the nature of networks, the form of clustering
and the shifting status of a labour market niche within
narratives of success may be ignored. For example, is
ethnic clustering among highly skilled migrants still a
form of relative disadvantage, or can it allow some
forms of career progression? Moreover, how is the
labour market experienced and narrated by those who
work in these niches? These are some of the questions
that remain unanswered in the large literature on
ethnic clustering.
In this paper we explore the processes that led
to ethnic clustering among a group of highly skilled
migrant workers. We explore how an ethnic niche was
constructed within geriatric medicine over a particular
time period, fromthe late 1960s to the 1980s, which
was a period of growth both in geriatrics and in
recruitment of overseas-qualified doctors in the NHS.
We also explore the complex multi-dimensionality of
ethnic clustering and suggest the need to undertake
further research into the implications of such clustering
for understanding the diversity of healthcare in
the UK.
Our research
Migrant doctors were an essential but devalued part
of the health workforce. They were necessary for its
operation, providing a mobile army of labour on the
lower rungs of the medical hierarchy, but they were
systematically disadvantaged in terms of access to jobs,
career mobility, the places where they found employment
and the specialties that they could occupy
(Kyriakides and Virdee, 2003). These doctors were
ethnically marked both through their race and through
their countries of qualification (Anwar and Ali, 1987;
Coker, 2001; Robinson and Carey, 2000). The fact that
in 2003 only 17% of South Asian doctors were consultants,
compared with 42% of white doctors (Decker,
2001, p. 34; Goldacre et al, 2004), provides some
evidence that migrant doctors from South Asia found
their careers limited by the institutionally racist and
hierarchical nature of the NHS (Esmail and Carnall,
1997; Hutton, 2001).
Since its inception, geriatric medicine has been a
‘Cinderella specialty’ (Smith, 1980; Jefferys, 2000; Thane,
2000), treating one of the least regarded groups of
patients, namely frail older people (Evans, 1997). As
such, geriatrics became a field in which South Asian
doctors could find jobs, and consequently 23% of
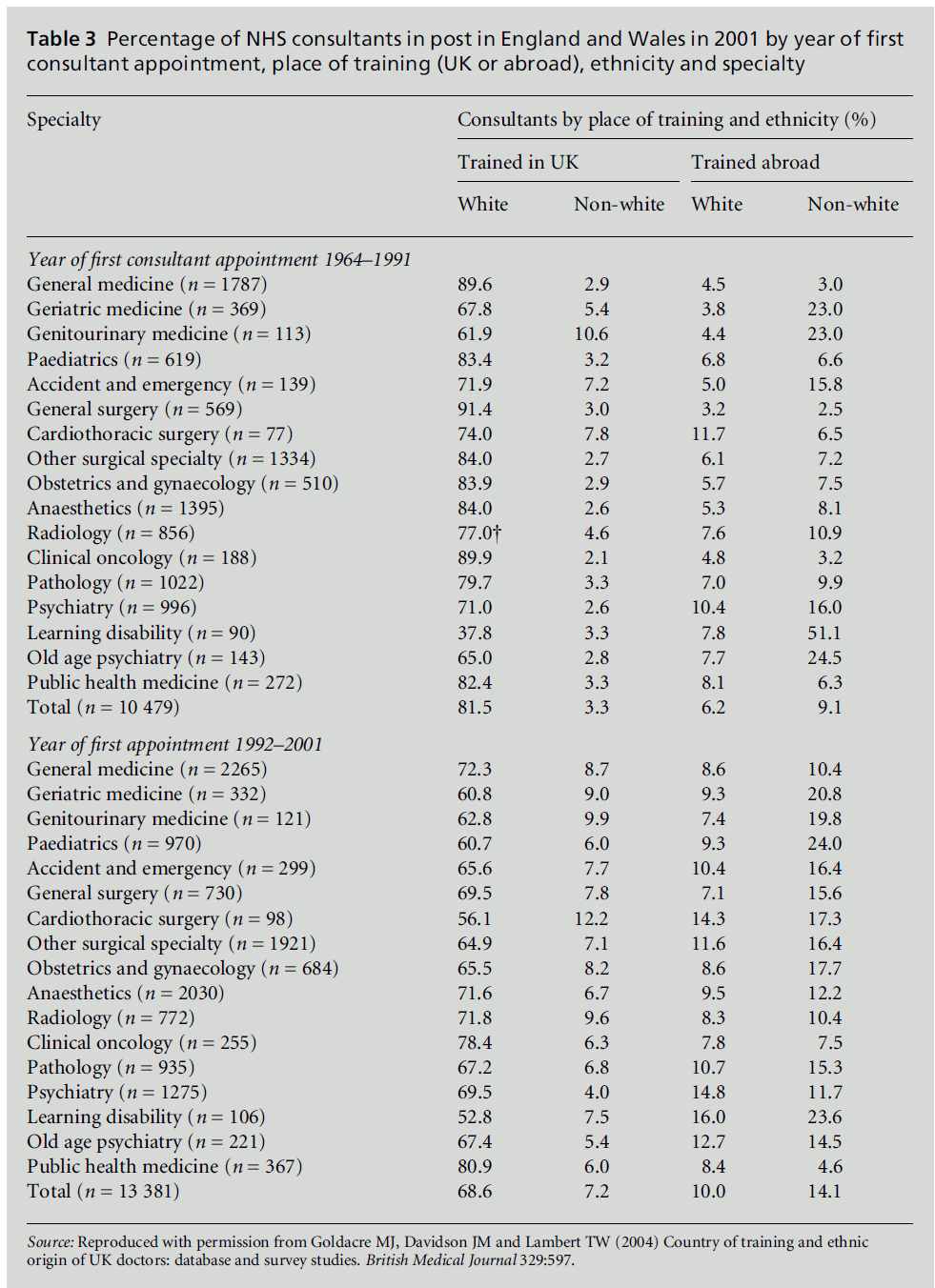
consultant geriatricians appointed between 1964 and
1991 were non-white and had trained outside the UK,
compared with only3%in general medicine and9%of
all consultants in the NHS. Between 1992 and 2001, 21% of all geriatric consultants appointed were nonwhite
and had trained outside the UK, compared with
14% of all consultants in the NHS and 10% in general
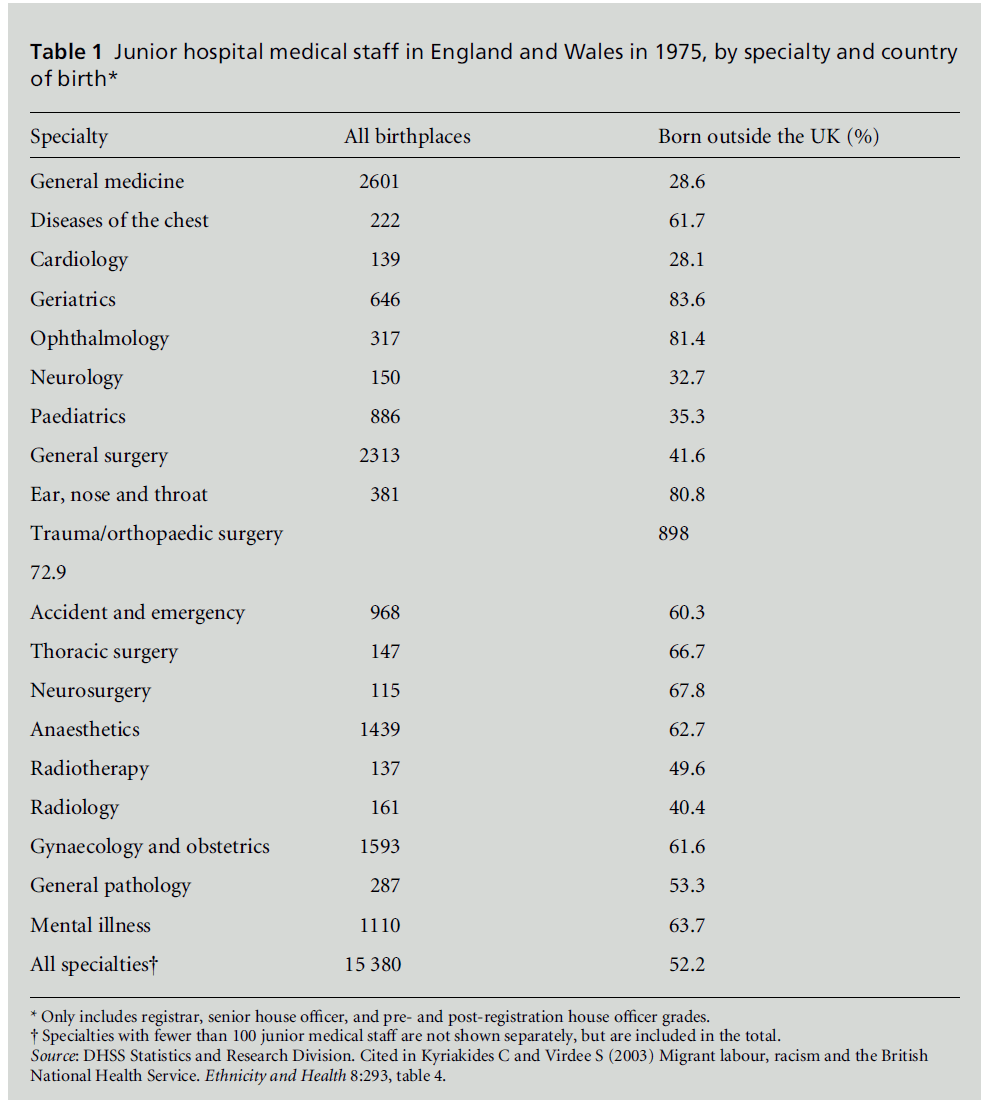
medicine (Goldacre et al, 2004; Table 1).
Migrant doctors working in the geriatric specialty
are an example of a group that operates within a
secondary medical labour market, despite their skills.
By looking at the complexities of the formation of
skilled labour markets, we can also see that narrations
of career success and of career mobility cannot be
treated as given for skilled migrants. Geriatrics thus
offers us an ideal point from which to explore ethnic
clustering among skilled migrants. The period that we are discussing is also interesting because the concerns
that were predominant then resonate with many today,
namely anxieties about an ageing population (Royal
College of Physicians 1968), a highly politicised environment
with regard to issues of migration and race,
as evidenced by the Commonwealth Immigrants Act
(1968) and the Immigration Act (1972), and concerns
about the management and future of the NHS
(Merrison, 1979). However, this was also a period
during which there was a rapid increase in the number
of geriatricians, especially those who qualified overseas
(see Table 2).
Table 1 :Junior hospital medical staff in England and Wales in 1975, by specialty and country
of birth
Table 2 :Populating geriatrics.
It is worth noting that the early 1970s were a period
of greater acceptance of geriatrics and a relative
improvement in its status. The role of geriatrics as a
discipline had already been lauded by the Ministry in
its publication Care of the Elderly (Ministry of Health,
1965). During 1972–1973, a standing committee on
geriatric medicine was set up by the Royal College of
Physicians, and in 1973 for the first time a geriatrician,
Dr John Wedgwood, was appointed as an examiner
for MRCP exams. In 1984, 40% of all patients in
hospital were over 65 years of age, so the centrality
of care for older people within the NHS became
cemented (Denham, 2004). Moreover, it was recognised
that one-third of all doctors had to look after
older patients. As a result, although geriatrics had low
status, it also came to be increasingly recognised as
playing a crucial role in theNHS, just as the immigrant
status of many people who populated it became
marked and problematic in the early 1970s.
Methods
The paper draws on a secondary analysis of interviews
conducted by Professor Margot Jefferys with the
pioneers of geriatrics in the UK, and a new data set
of interviews with South Asian geriatricians, who also
entered this profession and played a central role in its
development (Bornat, 2003). The first data set consists
of the 72 interviews that Jefferys and colleagues conducted
in 1990–1991 with the founders of the specialty
of geriatric medicine. Between them they cover the
history of developments in the healthcare of older
people from the late 1930s to the end of the 1970s. This
was a period of profound change in health policy in
the UK. The interviews open up a fascinating picture
of class and privilege in the medical profession while at
the same time revealing attitudes and practice in
relation to the care of the most marginal of all patient
groups, frail older people. The second data set generated
in this project consists of oral history interviews
with 60 South Asian overseas-trained doctors.
The decision to use the oral history method was felt
to be appropriate for several reasons. In both cases,
our own and that of Jefferys, the aim was to retrieve
eye-witness testimony to changes in an area of medical
practice which had consistently been marginalised
within the medical hierarchy and which had, in consequence,
enjoyed little attention from researchers. In
recording the experiences of those older doctors who
are ethnically marked we also aimed to capture accounts
of professional lives and working conditions which
might otherwise be lost to public record, given their
marginal and uncelebrated status within histories of
theNHS(for exception to this, see Smith, 1980; Rivett,
1998). We were also conscious of the tendency of oral
history, given its origins, to focus on those lower in the
social and professional hierarchies. In seeking accounts
from those who might be described as elite,
we were taking oral history as a method into relatively
uncharted territory (Bornat et al, 2009).
The project was submitted for ethical review and
approved by the Human Participants and Materials
Ethics Committee of the Open University, and by a
committee of the NHSNational Research Ethics Service.
The research was conducted in line with the ethical
recommendations of the UK Data Archive. Ethical and
copyright issues relating to the rights and perspectives
of the interviewees were taken into account during the
training of the research team members. Members of
the research team attended an oral history training
day, run by the Oral History Society, at which issues of
confidentiality, disclosure, copyright and consent were
addressed. Before each interview the interviewee’s rights
under copyright law and the aims and objectives of the
project were explained to them. Following the interview,
participants were invited to sign a consent form
which enabled them to stipulate the conditions under
which their words could be quoted in publications and
their interview would be archived.
Our target of 60 interviews was designed to represent
40 retired, semi-employed doctors who had
arrived in the UK in 1976 or earlier. We expected many
of them to have worked with the Jefferys pioneers. As a
control, we also aimed to interview 20 serving doctors, younger in age and with more recent experience of
geriatric medicine. The size of the sample was designed
to match Jefferys’ data set and to enable a broad
enough reach with which to capture the diversity of
the South Asian experience. The initial pool of potential
informants consisted of 28 South Asian geriatricians
who responded to a letter of invitation sent by
the British Geriatrics Society (BGS) in 2003. Of this
group, 12 geriatricians responded positively and a
total of ten were interviewed. This was followed up
by an advertisement in the BGS newsletter to which
one person responded, and this individual was interviewed.
A follow-up mailshot to retired BGS members
yielded a further six interviewees. One informant was
recruited after seeing correspondence relating to him
in the National Archives; another was the only South
Asian Jefferys informant. An additional 33 informants
were identified from contacts generated in previous
interviews, of whomten individuals were interviewed.
The majority of the potential informants (n = 110)
were identified by snowballing fromthe above sources
and, of these, 25 individuals were interviewed. This
was supplemented by purposive searches of Internet
sources such as hospital websites and doctors’ directories
for particular categories of geriatricians (women,
staff, and associate specialists), which yielded 18 potential
informants, of whom six individuals were interviewed.
Our interviewees included doctors who had trained in
India, Bangladesh, Sri Lanka, Pakistan and Burma,
ranging in age from 40 to 91 years, and having arrived
in the UK from the late 1940s onwards. All except two
of our interviewees serve or served as consultants, and
some also held senior academic posts.
As shown above, most of the informants (41%) and
over half of the retired informants were recruited
through snowball sampling. We are aware that this
approach is likely to have replicated a bias in our
sample towards relatively successful geriatricians. Of
course such a bias is an inherent aspect of not being
able to access a doubly invisible group (retired and
unsuccessful), and it also illustrates the contradiction
between making a public record of achievement of
South Asian geriatricians and recruiting a representative
sample of geriatricians. However, diversity of experience
was revealed in the interviews, in the geriatricians’
early lives, migration decisions, experiences of networking
and progression within the medical hierarchy, as
well as in the geography of employment opportunities.
At the same time, patterns and regularities in the
accounts were clearly evident both within our data set
and between our data set and the Jefferys recordings.
The interview schedule used a life history approach
(Thompson, 2000), asking participants to talk about
their childhood, upbringing, education at school and
college, and subsequent training and careers in their
home countries and after arrival in the UK. The
doctors were asked about their reasons for migrating to the UK, and their arrival and subsequent career
progression in the UK, with a focus on opportunities,
barriers and sources of support. All of the interviews
have been transcribed and will be deposited in the
British Library, where they will be archived alongside
the Jefferys collection.
The choice of oral history as a method in migration
studies is well attested. Both as an approach and as a
source of evidence, interviewing leads to rich and
more greatly nuanced theorising, as well as adding
directly to knowledge of particular migrant experiences
(Thomson, 1999). In this paper it provides
personal accounts of the experience of clustering in a
skilled sector of the labour market.
The oral history interviews are supplemented by
archival research. The archives of the Department of
Health, the British Geriatric Society, the British Medical
Association, the Wellcome Institute, the Royal
College of Physicians, the Royal Society of Medicine
and the papers of organisations such as the Overseas
Doctors’ Association have all been consulted to provide
an understanding of official narratives and policy
discourses related to the issues facing doctors working
in the specialty in the second half of the 20th century.
Clustering: geriatrics as a
discipline
For almost all of the informants, geriatrics was not
their first choice of specialty, but rather their entry to
the specialty was the result of an interplay between the
failure of their UK-based networks to facilitate entry
into the specialty they hoped to enter during their time
in the NHS, and the support given by their network in
finding alternative channels of career advancement.
Many of those who were interviewed reported that
their networks were not able to overcome barriers to
entry into high-status specialties even in times of relative
labour shortage. After repeated failure to secure a post
as a consultant or specialist registrar in their chosen
specialty, the informants who subsequently became
consultants (46 out of 48) were advised by their patrons
that as overseas-trained doctors the most direct route
to becoming a consultant was to become a geriatrician:
‘So I actually, I applied for the job for cardiology ... the
reference came to Dr Mitra you see – and he said to me
‘‘Oh, you applied for this job?’’ I said ‘‘Yeah’’. ‘‘So you’re
going for a job to Leeds for cardiology?’’ I said ‘‘Yes, I am
thinking about it’’. ... And he said ‘‘I’ll show you something
then’’. So there was a job in Newcastle coming up
applying for cardiology consultant job, you see. And he
showed me the applicants you see, because he was on the
interview panel for that consultancy. So a guy from
Edinburgh, a guy from Cambridge, a guy from Oxford,
one guy coming from Canada, one coming from New Zealand, one coming from London from Brompton. And
he said ‘‘Have a look at their names as well. They are all
local graduates’’. So he said ‘‘Where do you fit in there?Do
you think you have any chance there?’’ (laughs). So I said
‘‘Probably not’’, so he said ‘‘Well, my advice to you [is to]
forget about it because you could be wasting your time by
doing cardiology’’.’
(L040 male consultant, born in 1947,
arrived in the UK in 1973)
This repeated pattern of pressure on overseas doctors
to enter geriatrics rather than their chosen specialty
can be seen as reinforcing their marginalisation from
themainstreamlabourmarket, as although their patrons
highlighted the realities of discrimination against
foreigners in the networks in which they, of course,
played a critical part, they apparently did little to
challenge the discriminatory practices within their
networks.
Interestingly, however, they were also remarked upon
in the interviews that Jefferys conducted:
‘One of the problems has been that staffing of geriatric
departments hasn’t always been easy, we have had to
appoint quite a lot of doctors from the Indian subcontinent
to be registrars and even senior registrars, so
for quite a period the only applicants for consultant jobs
were in fact not British citizens trained by British methods.
They had been to respectable geriatric departments and
learnt the trade but when they got appointed to x, y, z, they
had Indian or Pakistani names or whatever else. And it
tended to get known as the sort of, you know, darkskinned
specialty.’
(John Agate, male consultant, born in 1919,
Jefferys interview conducted in 1991)
Those who were interviewed were of course aware that
geriatrics had a low status:
‘In medicine, geriatric medicine was the most unglamorous.
People who can’t get in[to] any other specialty will
try geriatric medicine. This will come every time you talk
to one of us. And that becomes a subject of pain for rest of
the life for these people, do you see what I mean. ... If your
colleague has gone into say rheumatology or cardiology,
somehow they squeezed in, and they say ‘‘What do you
do?’’ [When you say] ‘‘Geriatric medicine’’, the conversation
stops almost because you have [gone into] the lower
unglamorous [specialty], you are a failed physician.’
(L034, male professor, born in 1940,
arrived in the UK in 1969)
However, patrons could also offer advice on the basis
of their analysis of gaps in the labour market and
future developments within medicine. Sometimes this
might be more than simply verbal assistance:
‘Now that was a time I started seriously thinking about my
future. Especially in 1971, after 1971 events in Bangladesh.
And I wanted to do general medicine. My mentor, Dr
Kenneth Chalmers, he was a Scottish chest physician. He was a very kind-hearted man. He gave me a lot of advices
and encouragements and discouragements about everything,
and one thing he said [was] ‘‘our best bet would be
not to compete for general medicine because you will find
it very difficult. (a) You are slightly older than [the] other
competitors, and (b) there is still a lot of discrimination
against Asian doctors in such posts. So you either consider
to be a general practitioner or a dermatologist or a geriatrician
to remain in the general medical field you see, and
take your pick of these three’’. And he even arranged for
the local general practice to take me as their partner, you
understand.’
(L037, male consultant, born in 1935,
arrived in the UK in 1967)
Furthermore, our interviewees suggest that clustering
was multi-dimensional. For instance, South Asian
geriatricians appeared to cluster in hospitals with
fewer facilities and in areas that UK-qualified graduates
avoided:
‘First of all in the initial days they filled the jobs when
nobody else would take it. And they tried to copy the best
leaders. And implement changes in their own patch like
the best leaders had done. So there were geriatricians in
hospitals where facilities were so poor I probably wouldn’t
work in those even today. And so that’s one of the things
that they went to the areas where local doctors didn’t go.
And they filled those jobs where local doctors weren’t
interested. It wasn’t that the local doctors didn’t get those
jobs. They weren’t interested in those jobs.’
(L022, male consultant, born in 1945,
arrived in the UK in 1973)
Overseas-qualified doctors found it easier to get posts
in provincial district general hospitals, rather than in
major metropolises or teaching hospitals.
LH:
‘And why do you think there’s so many South Asian
doctors went into geriatrics?’
L039:
‘I think, yes, it should be, it should be, one should
recognise it actually, that that was a specialty where the
local graduates were not attracted to at that time because it
was not very attractive to go to. So it was easier to get
probably to become a consultant actually, yes. But then
places like King’s College or Greenwich, not easy, it was
not easy there, OK. So in provincial hospitals it was
probably easier.’
(L039, male consultant, born in 1939,
arrived in the UK in 1965)
The doctors were advised not to apply for jobs in the
southern parts of the UK where competition fromUK
graduates was high:
L044:
‘And by chance there were a lot of jobs in the
Southampton and Bath and, you know, Portsmouth
area and I would go there and there would literally be one that is hell of a good candidate. So, you know, be
careful. They didn’t want me really. So ultimately one
consultant told me ‘‘You will not get on in the South.
Don’t even think about it. I feel sorry for you’’.’
LH:
‘Right, so what was it about the south that ...?’
L044:
‘They wanted people from, you know, indigenous population
here. They didn’t want people like me. Sad but
true.’
(L044, male consultant, born in 1952,
arrived in the UK in 1978)
Instead they found opportunities in the more remote
parts of the country, a pattern that continued into the
1990s, as we shall see below:
‘After I passedmy PLAB in July I came to Wrexham to stay
with my friend, and then I started to apply and there was
no job and then one of my friends who used to work in
Oswestry ... cosWrexham had a rotation which was shared
through Oswestry and he knew one of the persons whose
duty start on the 3 August has stroked out. So the post was
vacant and it was so small a place, there wasn’t any ... they
are used to employing overseas graduates. All the three
SHO posts is always employed by overseas graduates
because none of the British graduates would want to
come and work there because it was so remote. Unless
they are in a rotation and compelled to come. So they
knew that there was no place they were going to get a
British graduate.’
(L026, male consultant, born in 1966,
arrived in the UK in 1995)
Ethnic clustering was thus layered with geographical
clustering, with South Asian geriatricians being pushed
into the more remote areas and into areas with a
poorer client base. They were largely excluded from
the metropolises and the big teaching hospitals.
However, there is more than one way of viewing this
particular aspect of clustering which occurred in geriatrics,
as the clustering was not only a result of discrimination,
but was also a result of recognition of
opportunity. A shortage in a particular area of medicine
or in a particular locality was also a gap that could
be filled, and for many informants this provided
opportunities for career progression. Talking about
the late 1970s, one of our interviewees said:
‘I knew that I will never get a job in general medicine, it is
highly competitive and the preference is given to the local
population. I didn’t feel bitter about it because I’ve
experienced that before in another country (laughs). So
I didn’t feel bitter about it. I said ‘‘Whatever the job I get,
I’ll take geriatric medicine and then see how it is’’. Within
six months I cleared the membership, part of it at least.’
(L025, male consultant, born in 1946,
arrived in the UK in 1976)
This ability to recognise and make space for personal
career development also continued into the late 1990s,
the period to which the interviewee below refers:
‘Because my consultant, who was exactly like me, I know
him now, he was a trained cardiologist and then there
were openings in geriatrics so he quickly moved into that
area and he said ‘‘Look, if you want to go through the fast
track up, then this is a less crowded road. You could do
geriatrics and you could do cardiology and you could, it
would be a good way up rather than waiting in the
queue’’.’
(L023, male professor, born in 1958,
arrived in the UK in 1996)
Most of those who were interviewed came to the UK
with a particular specialty in mind, such as cardiology,
gastroenterology, neurology or general medicine.
They were quickly disabused of their ambitions and
found a new chosen career in geriatrics. This movement
across disciplines brought benefits in terms of
training and progression.However, the changing nature
of geriatrics in the 1970s and 1980s, and particularly
the emergence of sub-specialties, meant that many
were able to maintain a specialist interest, while some
went on to specialise within geriatrics. Although the
broad scope of geriatrics marked it as a non-specialty
in the eyes of some doctors, for others it offers an
opportunity to gain experience of a wide range of acute
and longer-term conditions and to work with other
professionals, social workers, occupational therapists
and nurses in a less hierarchically organised arrangement.
In addition, for those interested in developing a
research base, there was some possibility of developing
a specialism, such as treatment of stroke, parkinsonism
and other conditions more typical of late life. Once
within the specialty, these more successful geriatricians
describe careers which have brought research-based as
well as material rewards, although these opportunities
were sometimes limited by their location outside the
teaching hospitals where funding and time for such
work was concentrated.
However, this clustering also caused concern. For
instance, the minutes of a ’special meeting’ of senior
officers of the Department of Health and Social
Security and Responsible Medical Officers (RMOs)
at the Nuffield Provincial Hospitals Trust on 5 June
1975 recorded the following statement:
‘At the present time, 30% of consultant posts in the
specialty were occupied byUKgraduates, and the position
was likely to deteriorate further during the next few years
when a large number of UK-born consultants would be
retiring ... it was apparent that geriatrics was in imminent
danger of becoming an ‘‘overseas’’ specialty. Such a state
was in his opinion unfair and unacceptable to the senior
citizens of our society. There was an urgent need to decide
what should be the fate of the specialty of geriatrics.’
Table 3 :Percentage of NHS consultants in post in England and Wales in 2001 by year of first consultant appointment, place of training (UK or abroad), ethnicity and specialty.
(Department of Health and Social Security, 1975a)
Clustering was seen to have a negative effect not only
on the patients but also on the future of the specialty.
The uncertainty over staffing that dependence on
medical migrants created was noted by the following Professor of Geriatric Medicine in a letter to the Royal
Commission on the NHS:
‘This concentration of overseas graduates in what remains
a low status specialty is undesirable on many grounds, and for the future it is not clear that plans for future expansion
cannot be based on the assumption that the supply of such
graduates will continue.’
(letter dated 13 December 1976 from Professor Ferguson
Anderson, the first British Professor of
Geriatric Medicine, BGS archives)
They sought diversity in the labour force, but interestingly,
their notion of diversity was a shift away from
the ethnic clustering which they noted. Moreover, the
ethnicity of the doctors was seen as an indicator of
the discrimination that older people faced, and it was
precisely by removing that dependence on South
Asians that equality with regard to older people was
sought.
Conclusion
Today, the issue of care of older people has resurfaced
as a major item on the political agenda (Caldwell et al,
2008; Department of Health, 2009). However, these
concerns are not new. They echo, for instance, those
raised in the Royal Commission’s report on the NHS
in 1979:
‘The demographic change which will be the greatest single
influence on the shape of the NHS for the rest of this
century is the growing number of old people and particularly
those over 75. This will increase the need for
long-term care.
(Royal Commission, 1979)’
Comparing the two data sets, our own and that of
Jefferys, highlights much that is similar in terms of
career progression and the development of the specialty.
For both groups of doctors, non-standard career
histories led to the opportunity for progression within
a marginalised specialty. However, as we have shown
here, the formal and informal mechanics of progression,
as described by the South Asian doctors, expose
the linkages between skill, ethnicity and marginalisation,
and present a perspective on clustering which,
we argue, has not so far been given sufficient attention
within the literature. Although the profession was aware
of the extent to which the development of geriatric
medicine occurred largely as a result of the marginalisation
of the specialty, rather than active choice on
the part of those employed as geriatricians, there have
so far been few attempts to explore the experiences of
geriatricians or to trace the complexities of opportunity
and constraint that this placed on individual
doctors, resulting in clustering. However, the academic
literature has explored the experiences of clustering,
although these accounts have been limited to the less
skilled and the entrepreneurial sectors of the labour
market. The focus of this article on the experiences of this group of marginalised elites in the medical labour
market in the UK thus contributes to both literatures,
providing a personal account of the process and experience
of clustering in a skilled specialty.
The status of geriatrics as a discipline that is involved
in the cure of those who face health problems in later
life has much to tell us about care provision. The care
and cure of older people share a status based on the
marginalisation of older people and dependence on
migrant labour. Issues of racism and ageism come
together to present challenges but also opportunities
for migrant workers (Raghuram et al, forthcoming).
We would argue that despite the extant critique of
clustering and its causes, there are also some positive
side-effects for both geriatricians and older people.
There is a perversity in the situation with regard to the
relationship between older people and South Asians
because, as one informant remarked, ‘Without racism
there would be no discipline of geriatrics’ (personal
communication, L035, male consultant in geriatric
medicine, arrived in the UK in 1975).
So what lessons can be learned from the historical
experience of clustering in geriatrics?
The existence and nature of clustering in the medical
labour market have not received the attention they
deserve. The medical profession, Department of Health
administrators and policy makers need to be aware of
the issues that clustering raises, and the impact that
these may have both on the medical specialists and on
patients. Both the Department of Health and the British
Medical Association Central Consultants and Specialists
Committee (2005) increasingly recognise the need
to provide appropriate environments in which doctors
can practise their skills, not only in order for doctors to
fulfil their potential, but also to ensure that patients
receive the best possible treatment. This paper has
provided some empirical evidence which suggests the
complexity of the discriminatory processes that are
limiting such efforts, some of which are, perhaps, still
occurring in the NHS.
CONFLICTS OF INTEREST
None.
References
- Anwar M and Ali A (1987) Overseas Doctors: experience and expectations – a research study. London: Commission for Racial Equality.
- Bonacich E (1973) A theory of middleman minorities. American Sociological Review 38:583–94.
- Bornat J (2003) A second take: revisiting interviews with a different purpose. Oral History 31:47–53.
- Bornat J, Henry L and Raghuram P (2009) ‘Don’t mix race with the specialty’: interviewing South Asian overseastrained geriatricians. Oral History 38:74–84.
- British Medical Association Central Consultants and Specialists Committee (2005) Tackling Racism in Medical Careers: the role of consultants; www.bma.org.uk/ap.nsf/ AttachmentsByTitle/PDFTacklingRacisminMedicalCareers/ $FILE/Racism.pdf (accessed 19 November 2008). Ethnic clustering among South Asian geriatricians 11
- Caldwell K, Saib M and Coleman K (2008) The ageing population: challenges for policy and practice. Diversity in Health and Social Care 5:11–18.
- Catto G (2008) A profession of equals. Diversity in Health and Social Care 5:235–6.
- Coker N (ed.) (2001) Racism in Medicine: an agenda for change. London: King’s Fund.
- Colic-Peisker V (2006) Employment niches for recent refugees: segmented labour market in twenty-first century Australia. Journal of Refugee Studies 19:203–29.
- Decker K (2001) Overseas doctors: past and present. In: Coker N (ed.) Racism in Medicine: an agenda for change. London: King’s Fund. pp. 25–47.
- Denham MJ (2004) The history of geriatric medicine and hospital care of the elderly in England between 1929 and the 1970s. Unpublished PhD thesis, University College, London.
- Department of Health (2009) Shaping the Future of Care Together. London: The Stationery Office.
- Department of Health and Social Security (1975a) Notes of a special meeting of senior officers of the DHSS and RMOs at the Nuffield Provincial Hospitals Trust, 3 Prince Albert Road, London, on Thursday 5 June 1975. Archives of the British Geriatrics Society, 1/12/224.
- Department of Health and Social Security (1975b) Medical manpower policy in relation to the NationalHealth Service. Notes of a meeting, Archives of the British Geriatrics Society, 1/12/224.
- Elliott R and Lindley J (2006) Skill specificity and labour mobility: occupation and sectoral dimensions. Manchester School 74:389–413.
- Esmail A (2007) Asian doctors in the NHS: service and betrayal. British Journal of General Practice 57:827–34.
- Esmail A and Carnall D (1997) Tackling racism in the NHS. British Medical Journal 214:618.
- Evans J (1997) Geriatric medicine: a brief history. British Medical Journal 315:1075–7.
- Goldacre MJ, Davidson JM and Lambert TW (2004) Country of training and ethnic origin of UK doctors: database and survey studies. British Medical Journal 329: 597.
- Jefferys M (2000) Recollections of the pioneers of the geriatric medicine specialty. In: Bornat J, Perks R, Walmsley J and Thompson P (eds) Oral History, Health and Welfare. London: Routledge. pp. 75–97.
- KloostermanR and Rath J (2001) Immigrant entrepreneurship in advanced economies: mixed embeddedness further explored. Journal of Ethnic and Migration Studies 27: 189–202.
- Kyriakides C and Virdee S (2003) Migrant labour, racism and the British National Health Service. Ethnicity and Health 8:283–305.
- Merrison A (1979) Royal Commission on the National Health Service: report. London: HMSO. Ministry of Health (1965) The Care of the Elderly in Hospitals and Residential Homes. London:
- Ministry of Health. Notter J (2006) Practising what we preach: working towards a diverse workforce in the UK. Diversity in Health and Social Care 3:231–2.
- Reid W and Rubin R (2003) Integrating economic dualism and labour market segmentation: the effects of race, gender and structural location on earnings, 1974–2000. Sociological Quarterly 44:405–32.
- Rivett G (1998) From Cradle to Grave: 50 years of the NHS. London: King’s Fund.
- Robinson V and Carey M (2000) Peopling skilled international migration: Indian doctors in the UK. International Migration 38:89–108.
- Schrover M, van der Leun J and Quispel C (2007) Niches, labour market segregation, ethnicity and gender. Journal of Ethnic and Migration Studies 33:529–40.
- Smith DJ (1980) Overseas Doctors in the National Health Service. London: Policy Studies Institute.
- Smith G and Nicolson M (2007) Re-expressing the division of British medicine under the NHS: the importance of locality in general practitioners’ oral histories. Social Science and Medicine 64:938–48.
- Smith P, Allan H, Henry L et al (2006) Valuing and Recognising the Talents of a Diverse Healthcare Workforce. Guildford: University of Surrey. https://portal.surrey.ac. uk/reoh
- Thane P (2000) Old Age in English History: past experiences, present issues. Oxford: Oxford University Press.
- Thompson P (2000) The Voice of the Past. 3rd edn. Oxford: Oxford University Press.
- Thomson A (1999) Moving stories: oral history and migration studies. Oral History 27:24–37.
- Waldinger R (1994) The making of an immigration niche. International Migration Review 28:3–30.