Research Paper - (2014) Volume 22, Issue 2
Senior Lecturer in HRM & Leadership
Steve Willcocks BA MA (Econ) PhD*
Principal Lecturer in Management Lancashire Business School, University of Central Lancashire, Preston, UK
Received date: 20 November 2013; Accepted date: 28 January 2014
Background Clinical commissioning is the centrepiece of government health reforms. Engagement with the reforms is important if they are to bring about improvements in the quality of healthcare. This is important in any healthcare system, not just the UK National Health Service (NHS). This study draws on data from a specially commissioned survey, exploring the extent to which general practitioners (GPs) in East Lancashire are engaged with clinical commissioning. Aim The aim of this study was to assess levels of engagement with clinical commissioning using a Clinical Commissioning Engagement Scale (CCES). Methods A six-point Likert scale CCES was distributed to all GPs within the boundary of East Lancashire Clinical Commissioning Group (CCG). The GPs are distributed across five localities that vary in terms of geography, demography and previous commissioning experience. The CCES aimed to capture comparative levels of engagement across twelve items, three for each of four dimensions of engagement: (1) personal attitude, (2) perceived capacity, (3) perceived capability and (4) opportunity. Eighty-five returns were received, representing a response rate of 35.3%. A full analysis of the data was conducted using SPSS v. 19. Results The results demonstrate concern for capacity and capability across the localities, where mean scores are universally well below the midpoint of the scale. However, attitude and opportunity were relatively positive indicators with mean scores above midpoint for all localities. Conclusion The findings highlight the potential challenges for CCGs in engaging GPs and in particular responding to perceived problems of capability and capacity. Further research is required to shed light on whether East Lancashire is typical of other CCGs.
clinical engagement, commissioning, general practice, GPs
How this fits in with quality in primary care
What do we know?
Engagement is a crucial aspect of improving quality and performance in any healthcare system. It is important to ascertain the reasons for a lack of engagement.
What does the paper add?
This paper explores these reasons from the perspective of clinicians involved in the context of one clinical commissioning group. This study confirms the findings of other studies suggesting that there is a problem with the capacity of general practitioners to take on the commissioning role.
Clinical commissioning is regarded as the centrepiece of recent UK health service reforms and a way of improving quality and performance in the National Health Service (NHS). This paper examines the extent to which general practitioners (GPs) in East Lancashire are engaged with the principles and practice of clinical commissioning. It draws on data from a commis-sioned survey of GPs in East Lancashire and concludes that, whilst degrees of engagement across the entire region are relatively uniform, the average level may be lower than what is considered necessary with particu-lar concern surrounding the capacity and capability of GPs to get involved with commissioning.
Clinical commissioning and GP engagement
The rationale behind the emphasis on clinical engage-ment in UK NHS reforms is that it will improve the ability of organisations to facilitate change and trans-formation, and thus result in improvements to organ-isational performance and, ultimately, quality of care. Desired improvement in the way in which healthcare is delivered is likely to be dependent on doctors’ active engagement[1] and research does suggest that change in clinical domains can be better realised with the coop-eration and support of clinicians.[2] It follows that engaging clinicians means involving them in all as-pects of healthcare provision including the planning, delivery and transformation of services.[3]
Nevertheless, it seems that ‘clinical engagement’ is an elusive concept, with limited agreement as to what precisely it entails or delivers. But it has been argued that engagement might constitute a continuum, ranging from passive support through active participation to e?ective leadership.[4] Ideally, engagement will be em-bedded completely such that doctors are fully involved with the design and delivery of service innovations, and commissioning particularly.[1]
Clinical engagement is part of a wider initiative that is changing the culture of healthcare towards one in which GPs are more involved in leadership, quality, service improvement and working in partnership with other clinical and non-clinical sta?.[1] However, there has been, and to a large extent still is, a problem with engendering clinical engagement. For example, it is argued that ‘many doctors are not positively engaged with the system in which they work, and their per-formance in the clinical management and leadership localities falls short of what it could be’.[5] Despite incentives such as financial payments, there remain barriers to clinical engagement that include lack of time and resources, alongside the existence of poor rela-tionships between clinicians and primary care trusts.[6]
Barriers to engagement include the pressure of competing occupational demands, lack of adequate information systems, limited training, insu?cient skills, inadequate rewards, sta? turnover, lack of interest and resistance.[4] Alternatively, there are some factors that can encourage engagement with an emphasis on avoiding abstract issues that are not relevant to day-to-day healthcare and concentrating on aspects that are beneficial directly to patients and colleagues.[4]
The notion of clinical engagement incorporates attitudinal attachment to a variety of interrelated principles and practices. The research focus here, how-ever, is on engagement with one particularly import-ant aspect of current health service reforms – clinical commissioning. Commissioning is defined as ‘prior-itising, securing, funding and monitoring all of the health improvement and healthcare services provided in a defined geographical locality, or for a specific group of individuals’.[7] It is seen as ‘a complex process with responsibilities ranging from assessing popu-lation needs, prioritising health outcomes, procuring products and services to managing service providers’.[8]
The King’s Fund argues that the success of com-missioning (and ultimately improving quality) will depend on ‘engaging a critical mass of enthusiastic and competent GPs’. Their survey of 500 GPs indicates that the majority (62%) are confident of there being GPs in their locality with the capacity to lead GP commissioning consortia.[9] However, a problem in the NHS has been resistance within the GP community to the idea of involvement with commissioning. It has been pointed out that GP commissioning has a 20-year history and ‘evidence suggests it has the potential to strengthen primary care services and to engage GPs in decisions about local service planning ... however, the same evidence base highlights significant chal-lenges in trying to engage more than an enthusiastic minority of GPs’.[10] The Health and Social Care Act 2012 requires every GP to be signed up to their local clinical commissioning group (CCG). Consequently, avoiding clinical commissioning is no longer an op-tion for GPs, although varying depths of individual engagement may be acceptable. The challenge for the NHS is how to create the right systems and culture to encourage doctors to engage adequately as stake-holders in commissioning and improving the delivery of healthcare for their local population.[1]
The question regarding clinical commissioning engagement (CCE), therefore, remains of interest in the context of implementing health service reforms and improving quality. Evidence indicates that the capacity of GPs to be involved in commissioning, given finite resources, and how capable they feel personally about conducting commissioning are key factors in understanding engagement. Research into previous incarnations of clinical commissioning found that a significant barrier to progress was limited GP capacity and capability.[11] Another factor that can impact upon engagement is GP perceptions of the value of clinical commissioning activity. Their attitude, in this regard, may be influenced by personal ideology and whether they feel there are conflicts of interest that could impact adversely upon their own practice.[12]
In addition to capacity, capability and attitude, it might be anticipated that the past and current avail-ability of opportunities for GPs to be involved in clinical commissioning activity will have a direct im-pact on their levels of engagement. It remains an open question as to whether it is feasible or necessary for all GPs to have first-hand experience, but the principle enshrined in the Health and Social Care Act 2012 indicates a wider distribution of participation and responsibility for commissioning that will require opportunities for participation to be provided and taken.
For the purposes of this research, a survey of GPs in East Lancashire was conducted with the aim of assessing levels of engagement with clinical commis-sioning. A Clinical Commissioning Engagement Scale (CCES; Appendix A) was designed and distributed to all GPs in East Lancashire in July 2012. A detailed review of the relevant literature was undertaken and discussions held with interested and knowledgeable parties (GPs from outside East Lancashire and rep-resentatives of the Trust) in order to facilitate design of the CCES. It was trialled with colleagues in order to ensure the accuracy and clarity of items, but has not yet been subject to rigorous validation. The CCES was interpreted as comprising four dimensions – specifi-cally:
• personal attitude towards clinical commissioning;
• perceived capacity to engage with clinical com-missioning;
• perceived capability to engage with clinical com-missioning; and
• opportunity to engage with clinical commissioning.
The CCES utilises a single six-point Likert scale to capture comparative levels of engagement across 12 items (three for each dimension). Every CCES return can be ‘scored’ to indicate a level of engagement between 1 and 6. Scores can be calculated at the individual level as well as aggregated and averaged across the regional and locality echelons. The GPs in East Lancashire are distributed across five localities (Burnley, Hyndburn, Pendle, Ribble Valley and Rossendale) that vary in terms of their geography, demography and previous commissioning experience, so it was considered important to collect information on location in case such factors had an impact on levels of CCE. The survey was an anonymised census of all GPs in the five localities, but it was not designed to obtain specific information on individual GPs or GP practices.
Eighty-four returns were received, representing a response rate of 35.3% which although not as high as might be considered ideal, is normal for this type of survey, gives statistically significant results and an important aspect of the response is that the five geographical localities are equally represented. A full analysis of the data was conducted using SPSS v. 19, however, for purposes of clarity, only significant results are presented.
Involvement in clinical commissioning activity ap-pears to be somewhat restricted across the sample with nearly two-thirds of GPs having never or only rarely been involved with clinical commissioning and the majority of those GPs indicating that they fall into the rarely involved category (Table 1) – a finding that will be discussed shortly.
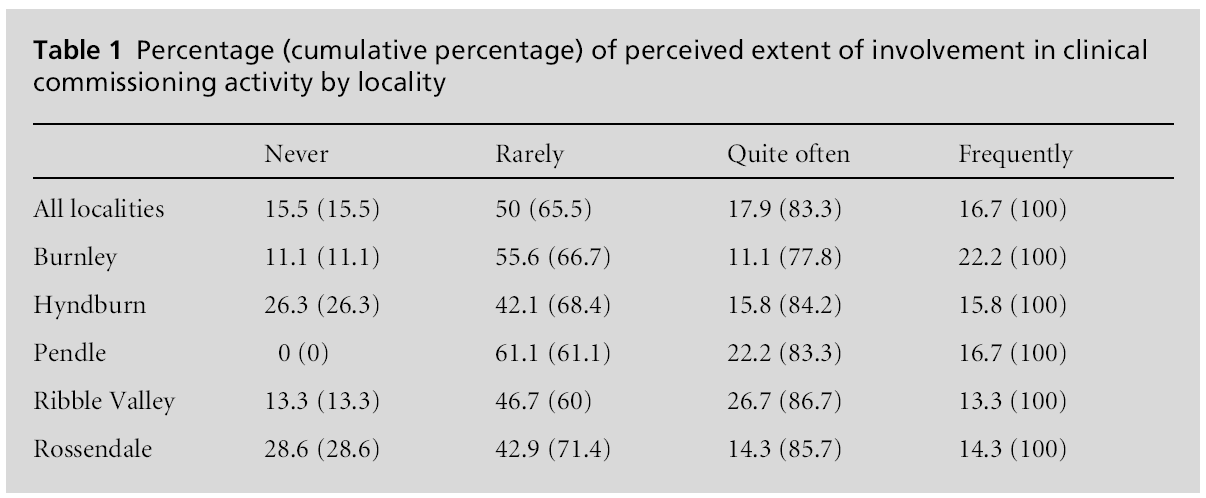
Variation in the extent of involvement between the five localities is relatively slight and the only excep-tional result of note is that every respondent in the Pendle locality had at least some experience of clinical commissioning activity, although the majority still claimed to be only rarely involved.
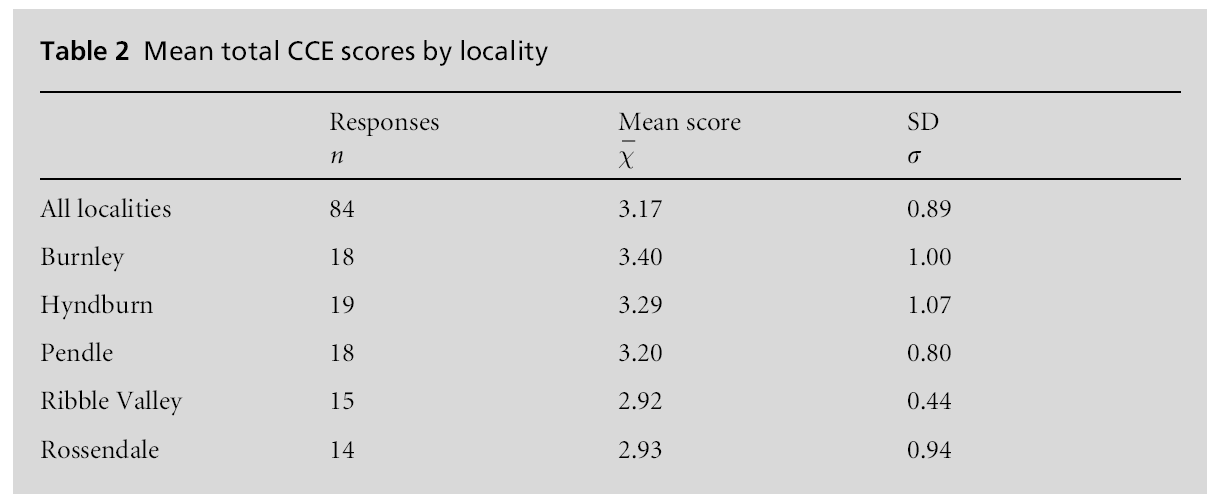
Table 2 shows that the mean total score for this CCE survey across the localities is 3.17 (s = 0.89), some-what below the midpoint of the scale that runs from 1 to 6, and there is only limited variation in CCE across localities with a di?erence of just a half point between the highest locality CCE score (Burnley) and the lowest (Ribble Valley). This seems to suggest that the variables mentioned earlier, such as demography and previous commissioning experience, had no signifi-cant e?ect.
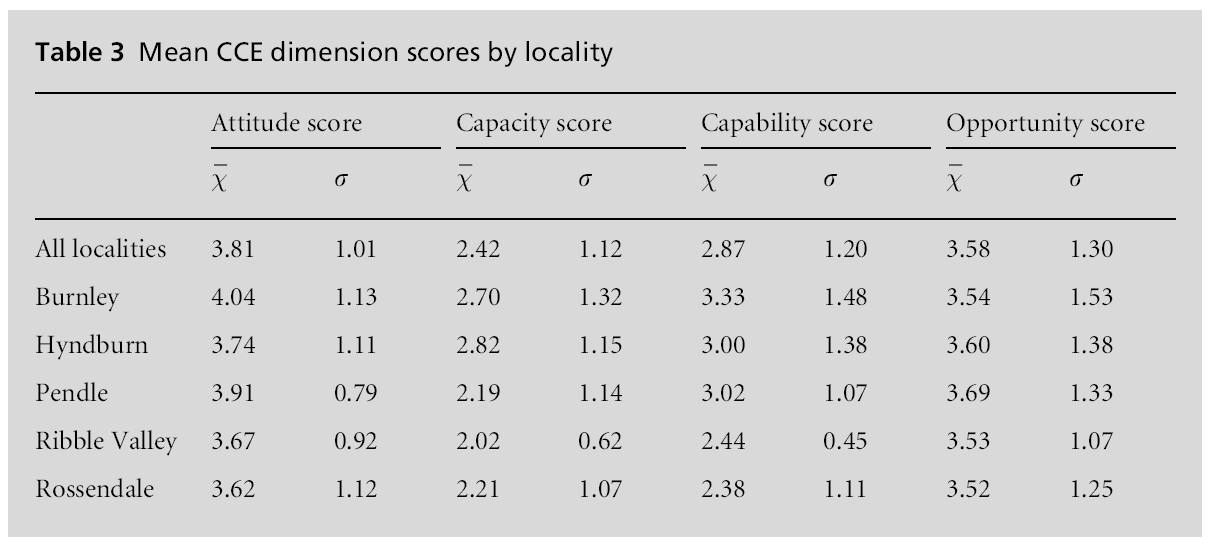
A review of engagement scores across each of the four CCE dimensions, presented in Table 3, indicates that the mean scores for capacity (across all localities = 2.42) and capability (2.87) are significantly lower than the mean scores for attitude (3.81) and opportunity (3.58). Furthermore, capability, and especially ca-pacity, appears to account for the greater part of the variance in CCE levels across the five geographical localities.
Relationships between variables
Given that the CCES is designed to assess a single construct through four dimensions it is to be expected, as shown in Table 4, that all of the variables are correlated significantly with one another. The results confirm the coherence of the CCE construct and indicate that no single dimension can be treated as being independent of the others. Nevertheless, there are di?erences in the strengths of the various corre-lations.
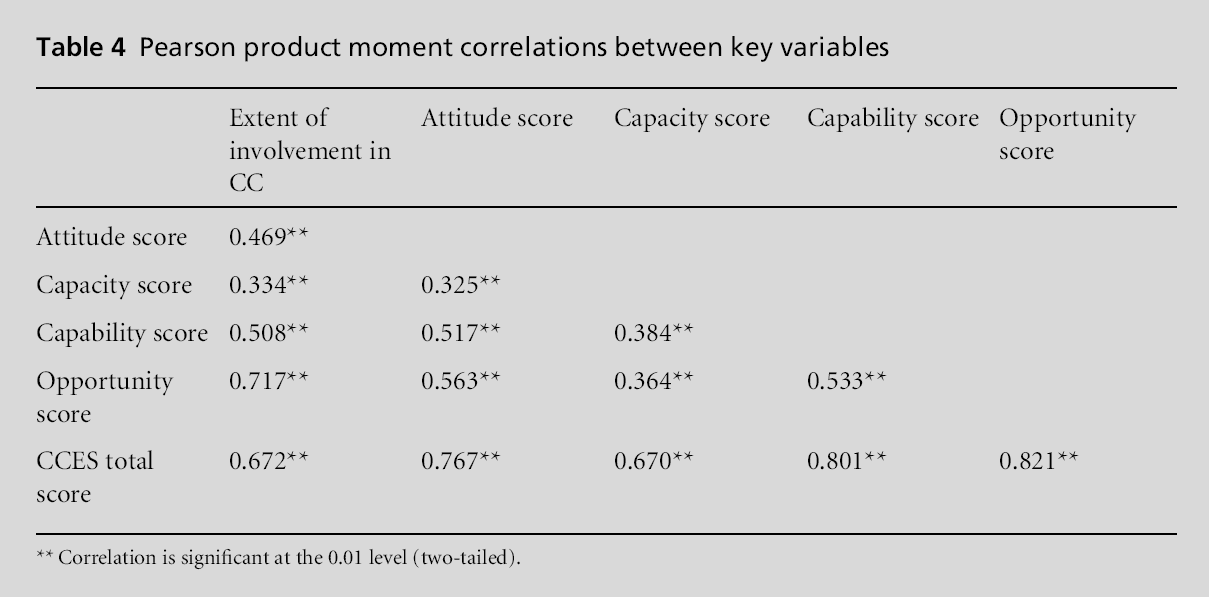
Whereas the capacity score is correlated quite strongly with the CCES total score, its correlation with the other three dimensions is comparatively modest. This may indicate that, whereas lack of capacity acts as a barrier to an overall sense of engagement, creating capacity will not, on its own, necessarily influence the other dimensions. The relatively higher correlations between the attitude, capability and opportunity di-mensions suggest that they are more likely to have a significant influence on one another.
The perceived extent of involvement in clinical commissioning is strongly correlated with the CCES total score, which indicates that the greater GP in-volvement with clinical commissioning was in the past, the more positive their level of engagement is likely to be now. In other words, past involvement in commissioning may have been a key factor.
It was noted earlier that that the majority of GPs had little or no involvement with clinical commissioning and it is evident from Table 5 that GPs who have never undertaken clinical commissioning garner the lowest engagement scores across the board, however, the direction of causality cannot be established from this data alone. Thus, we do not know for certain if they have never been involved because they are disengaged or if they are disengaged because of no involvement, although the fact that the mean capacity and capability scores are somewhat lower than the mean scores for attitude and opportunity may be indicative of a lack of confidence to participate.
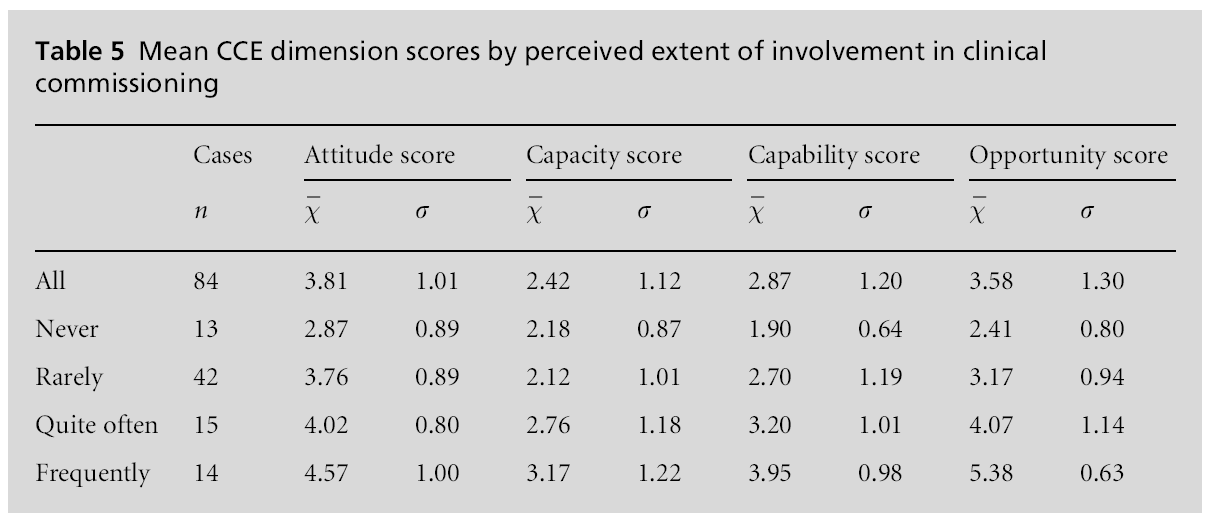
Indeed, at the extremes of the extent scale (never and frequently) there is evidence that perception of capability may have an impact on involvement. The very low mean capability score (1.90) and the modest spread (s = 0.64) under the ‘never’ category are striking and may indicate that some GPs avoid in-volvement in clinical commissioning because of un-certainty about their ability. The incidence of GPs who feel that they lack the necessary ability when compared with those who feel confident in their ability is skewed towards the former with only six GPs scoring at 5 or higher on the capability dimension, whereas 27 GPs scored at 2 or lower.
An analysis of GPs declaring that they are ‘rarely’ involved in clinical commissioning, which is by far the largest category consisting of half of all respondents, does not present such a clear contrast. An assessment of capability scores among the ‘rarely’ group shows a very wide distribution of responses. A similar pattern is found for the other three dimensions. Given the number of GPs in that category, they may represent the greatest challenge for spreading engagement.
The survey shows that participation in clinical commissioning in this context has a significant re-lationship with levels of engagement among GPs. Those who have had little involvement with commis-sioning show lower levels of engagement than those who feel that they have often been involved, although the direction of cause and e?ect is not known. Do GPs become engaged because they are involved in com-missioning activity or do they get involved because they are already engaged? The former would suggest that the obvious course of action is to get GPs ‘doing’ clinical commissioning and their engagement to some extent should follow. The alternative situation, how-ever, presents a more complex issue of creating en-gagement in the first instance.
This study confirms previous findings,[6,11] suggesting that there is a problem with the capacity of GPs to take on the commissioning role. Indeed, lack of capacity was an area of concern in earlier experiments in clinical commissioning.[11] This paper adds a more sophisticated understanding of the di?erent dimen-sions of engagement, utilising a specially developed engagement tool, the CCES. Policy makers in any healthcare system need to understand the extent of engagement with government health reforms and the implications for improving quality and performance.
The maximum possible score for the CCES was 6. It is reasonable to suggest that a mean score of 3.17 is lower than policy makers would like – given the high priority of clinical commissioning as a transformative strategy. The fact that a below midpoint score applies to all localities may be a cause for concern, although the relatively consistent levels across localities can be viewed as a positive sign. However, it might have been interesting to have found one locality where involve-ment was higher, to enable further exploration of this situation. No single locality is adrift from the others and so engagement activities and initiatives can be applied across East Lancashire without fear of them being redundant in some areas.
With the political controversy surrounding UK health reforms it is perhaps surprising that attitude and opportunity are relatively positive indicators with mean scores above the scale midpoint for all localities. The greater concern lies with capability and capacity where mean scores are universally well below the midpoint.
Strengths and limitations
The study utilised a specifically designed scale, derived from the literature and discussions with experts, although it was not formally validated. The survey was a census of GPs in the East Lancashire region and so, whilst the response rate allows generalisation of the findings at the locality level, it does not permit gen-eralisation beyond the borders of the East Lancashire CCG. More research is needed to validate the CCES and to enable generalisations in other areas or con-texts. There is the likelihood that variables such as list size, GP seniority and case mix may have an important influence on the extent to which GPs engage with commissioning. Such variables were excluded from the CCES in order to ensure coherence and manage-ability, but they certainly represent important con-siderations for further enquiry.
Implications for practice
The distribution of results concerning the perceived extent of involvement in clinical commissioning, particularly the positive relationship with overall level of engagement, has parallels with Rogers’[13] well-known model of innovation di?usion (Figure 1).
The implication is that those GPs who have frequent involvement in clinical commissioning also have the highest engagement scores (across all dimensions) and so can be likened to the ‘early adopters’ of an inno-vation and be encouraged to act as change agents or champions of change and development. Of course, the issue for clinical commissioning is less to do with temporality (early or late) and more to do with the extent of GP involvement (more or less). The GPs who fall into the ‘rarely involved’ category may be likened to Roger’s ‘late majority’ although the size of the group is much larger at 50% of the sample rather than Roger’s expected 34%.
In general, the findings from this survey highlight the potential challenges for the new CCGs and, in particular, raise the importance of training, skills development and job design for GPs. For example, it is possible that a lack of involvement means that GPs simply lack knowledge and understanding of what is required, and that more training is required. The findings certainly beg questions regarding the extent to which GP specialty training and development is ‘fit for purpose’ in preparing primary care providers for the challenges of the future. Further research is required to shed light on the drivers for the creation of positive engagement with clinical commissioning, the possible reasons for resistance and any limitations in terms of GP development.
Engagement is a crucial aspect of improving quality and performance in any healthcare system. As noted by the King’s Fund, ‘there is strong evidence that organisations in which doctors are both valued and engaged perform better than those in which this is not the case’.[14] It has been argued that doctors should be engaged, alongside managers, with the drive for qual-ity improvement.[15] However, lack of clinical engage-ment is well known, and it is important to ascertain the reasons for a lack of engagement. This paper attempts to reveal the reasons from the perspective of those involved – clinicians – and in the context of one CCG. It reveals that it is not necessarily ideological but a concern for capacity and capability of GPs with regard to clinical commissioning, and that they may need more support in this role.
This study did not require NHS ethical approval, although it was cleared by the university. The authors acknowledge the East Lancashire PCT who funded this project.
Not commissioned; externally peer reviewed.
None.