Research Paper - (2010) Volume 18, Issue 6
Formerly Advanced Medical Science Student, Emergency Practice Innovation Centre, St Vincent’s Hospital and Faculty of Medicine, Dentistry and Health Sciences, University of Melbourne, Australia
George A Jelinek MD DipDHM FACEM*
Medical Director, Emergency Practice Innovation Centre, St Vincent’s Hospital, Faculty of Medicine, Dentistry and Health Sciences, University of Melbourne, and the Gawler Foundation, Victoria, Australia
Tracey J Weiland BBSc(Hons) PhD MAPS
Senior Research Fellow, Emergency Practice Innovation Centre, St Vincent’s Hospital and Faculty of Medicine, Dentistry and Health Sciences, University of Melbourne, Australia
Claire A Mackinlay BHSc/Comm MHA
Research Offcer, Emergency Practice Innovation Centre, St Vincent’s Hospital and Faculty of Medicine, Dentistry and Health Sciences, University of Melbourne, Australia
Sherelle Dye BMus(Hons) BLitt(Hons) MPsych(Clinical) PhD
Formerly Research Offcer, The Gawler Foundation, Victoria, Australia
Ian Gawler BVSc MCounsHS
Formerly Therapeutic Director, The Gawler Foundation, Victoria, Australia
Received date: 8 June 2010; Accepted date: 26 September 2010
Aim To evaluate the effect of a residential retreat on promoting lifestyle modification for the health related quality of life (HRQOL) of people with multiple sclerosis (MS). MethodsA longitudinal cohort study of adults with self-reported MS who voluntarily attended a five-day residential retreat in rural Victoria, Australia. Participants were asked to complete the MSQOL-54 questionnaire just prior to the retreat, and at one year and 2.5 years post-retreat. Results Of 188 participants 109 (58%) completed the questionnaire. The cohort showed a significant improvement in HRQOL at one year and 2.5 year follow-up. After one year, overall quality of life (QOL) domain had increased from 73.4 to 81.7 (P0.001), physical health composite from 66.2 to 76.4 (P=0.001) and mental health composite from 73.7 to 83.6 (P0.001) in the subset of 76 with data at both time points. After 2.5 years, overall QOL had increased from 68.4 to 71.7 (P=0.03), physical health 59.7 to 70.0 (P=0.01), and mental health 66.9 to 76.6 (P0.01) in the subset of 44 with data at both time points. ConclusionsHRQOL usually deteriorates over time in people with MS. Attendance at a residential retreat promoting lifestyle modification appears to have a significant short–medium term positive effect on QOL for people with MS. General practitioners caring for people with MS should consider the potential benefits of this approach in overall management.
health-related quality of life, lifestyle modification, multiple sclerosis, MSQOL
Multiple sclerosis (MS) is a chronic inflammatory disorder of the central nervous system that is thought to be autoimmune and degenerative in nature. It is the most common cause of neurological disability among young adults,[1] affecting approximately 18 000 Austra-lians and 2.5 million people worldwide. Inflammatory lesions in the brain and spinal cord cause a range of symptoms such as visual impairment, muscle weak-ness and spasticity and bladder dysfunction.[2] This incurable disabling disease affects the psychological and social wellbeing of people with MS. Among other effects, these people experience higher rates of de-pression and suicide.[3]
MS has an unpredictable clinical course that usually evolves over several decades. The frequency and severity of new lesions appears random, and they occur more often than they are detected clinically.[4] Usually all types of MS lead to deterioration of health and per-manent disability, and sometimes death.[5] The median survival time from disease onset is around 28 years,[6] with at least a five to ten year reduction in life expectancy.[7]
Most people with MS are treated with long-term immunomodulatory therapy including the interferons, glatiramer and more recently natalizumab. However, the effectiveness of these drugs in slowing disease progression is questionable,[8] as is their cost-effective-ness.[9] A systematic review of the effcacy and cost-effectiveness found some clinical benefit of these drugs, which may be counterbalanced by side effects and cost.[9] Hence many people with MS seek non-drug therapies to manage their condition.[10] Currently there is a growing need to compare pharmacological treat-ments to other therapies that may improve QOL.[11]
Patients with chronic diseases often feel the need to actively gain control over their health and explore options beyond standard treatments.[12] For this reason, many people with MS have tried at least one alternative therapy to manage the condition.[13] Studies on ther-apies such as a low saturated fat diet,[14–16] vitamin supplementation,[17] exercise[18,19] and stress manage-ment[20–22] have suggested a benefit. There has been a call for these modalities to be considered in the primary care management of people with MS.[23]
Previous studies have explored the outcome of combined intervention programmes for people with MS, delivered through weekly sessions.[24,25] A review of the literature found no studies on residential edu-cational and experiential programmes encouraging lifestyle modifications for people with MS.
Since April 2002, we have conducted five-day resi-dential retreats for people with MS in conjunction with the Gawler Foundation, Victoria. This private organisation is a registered charity funded by do-nations and course fees. It is situated in the Yarra Valley, Victoria, and has accommodation for 36 par-ticipants, on-site catering facilities and large meeting and meditation areas. It offers programmes for people with cancer and multiple sclerosis, as well as wellness programmes. The MS programme is based on detailed literature reviews of the potential benefit of lifestyle and medication interventions in MS.[26–28] The rec-ommendations are summarised in Box 1.

This longitudinal cohort study aimed to monitor the ongoing health-related quality of life of a cohort of people with MS after attending these retreats.
Methods
Design and procedure
Participants of the MS retreats held between April 2002 and March 2008 at the Gawler Foundation were approached with regard to participating in the study. These MS retreats were advertised through some MS societies in Australia, local newspapers, a book[27] and an associated website (www.takingcontrolofmultiplesclerosis.org). People attending the retreats self-reported having MS diagnosed by a neurologist, although a small number of people with other neurological con-ditions were Accepted date: onto the courses.
Programme registrants were requested to complete the MSQOL-54 questionnaire[29] just prior to attending a retreat. Completed questionnaires were collected when the participant attended. Participants were ad-vised that they would be contacted and asked to complete follow-up questionnaires by post at intervals of one and 2.5 years after attending the retreat. Pre-paid addressed envelopes were provided for the return of consent forms and completed questionnaires.
The five-day programme consisted of educational sessions about the evidence and practical issues sur-rounding changes in diet, essential fatty acid sup-plementation, sun exposure, stress management and exercise. These sessions were presented by two of the authors (GAJ and IG). There were daily meditation sessions, group counselling and sessions of Qigong or gentle Hatha yoga exercises, with a focus on promot-ing healthy emotions and meditation to balance the effects of stress. These sessions were presented by counsellors from the Gawler Foundation. Patients were introduced to techniques such as progressive muscle relaxation meditation,[22] guided imagery and dyadic focus groups. Massage and one-to-one coun-selling sessions were also offered to participants.
Intervention
The five-day residential programme was educational and experiential, based on incorporating the best available evidence about lifestyle factors such as diet, sun exposure and vitamin D supplementation, medi-tation, exercise and stress reduction. These modalities were able to be undertaken by participants on an ongoing basis without the need for medical prescrip-tion. Some participants were also taking standard disease-modifying therapies for MS. Between 13 and 34 people with MS attended each of these retreats, which are held two or three times a year.
Patients were provided a plant-based wholefood diet consistent with Swank’s dietary recommen-dations.[30] Flaxseed oil was also incorporated into meals to ensure participants had adequate intake of essential fatty acids.
Assessment
The programmes were evaluated by administering the MSQOL-54 questionnaire. Since the instrument first appeared in 1995,[29] it has been extensively validated in people with MS worldwide,[31,32] and used in assessing the impact of fatigue,[33,34] depression[35] and exercise,[36] as well as a number of medical therapies.[37]
The MSQOL-54 uses the well-validated RAND 36-item Health Survey (SF-36) as a generic core measure.[29] To make it more MS specific, the SF-36 is supplemented with 18 additional items comprising of health distress, sexual function, satisfaction with sexual function, overall QOL, cognitive function, energy, pain and social function. Scores of individ-ual items are recorded on a Likert scale. Physical health and mental health composite scores for the MSQOL-54 are determined from the weighted sum of selected scale scores. Both scale and composite scores range from 0 (poor health) to 100 (optimal health) (Table 1).

Statistical analysis
Descriptive statistics (mean, 95% confidence interval for the mean, median, interquartile ranges, numbers and percentages) were used to describe sample charac-teristics. The results for participants who completed baseline questionnaires and one other time point were assessed separately, as most people did not complete questionnaires at all three time-points.
Comparisons between the baseline and follow-up time-point scale item and composite scores were made by using the Wilcoxon Signed Ranks test. Correlations between baseline items, domain scores and health composites were assessed using the Spearman corre-lation coeffcient.
All analyses were conducted with SPSS version 15.0 for Windows.
Results
A total of 257 people attended the MS retreats held between March 2002 and March 2008. Of these, 210 completed a baseline questionnaire, and we had con-tact details for 195 of them. Three had died and four had attended the retreats with neurological conditions different from MS. All people in the sample attended the full five days of the retreat.
Of 188 eligible subjects, 109 (58%) consented to participate in this ongoing study. Many had missing data at time points other than baseline (Table 2). Complete data across all time-points were obtained from 11 participants, all women; 65 participants only completed baseline and one-year follow-up question-naires, and 33 participants only completed baseline and 2.5 years follow-up questionnaires.
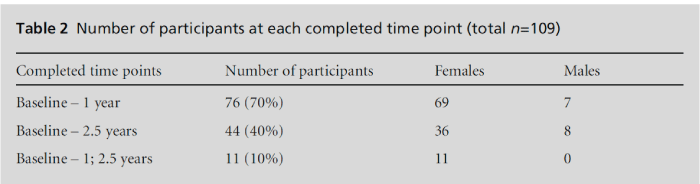
There were 94 females out of the 109 participants (86.2%). As there were so few male participants, gender differences were not assessed.
Ten out of the 14 QOL domains improved over one year. Table 3 shows the baseline and one year MSQOL-54 scale and composite scores. The role limitations due to physical problems domain had the greatest improvement (41.7 points), whereas the cognitive function domain improved the least (5.0 points). The median for role limitations due to emotional prob-lems after one year remained unchanged, but a sig-nificant increase (Z = –2.639, P=0.008) was still detected by the Wilcoxon Signed Ranks test. The changes across one year among the scores for physical health, pain, sexual and social function were statisti-cally insignificant.

Figure 1 illustrates the significant improvement found at one year follow-up in overall QOL (10.2 points), mental health composite score (9.9 points) and physical health composite score (8.3 points).
Similar improvements were seen between the base-line and 2.5 years follow-up group (Figure 2). Overall QOL increased by 3.3 points. Six of the QOL domains and the two composite scores significantly improved after 2.5 years (Table 4). The health distress domain improved by 20 points, double the improvement found at the one year follow-up.

Compared to the results at one year follow-up, at 2.5 years there were no significant changes in role limitations due to physical problems, role limitations due to emotional problems, cognitive function, change in health and satisfaction with sexual function domains. However, at the 2.5 year follow-up there was an improvement in sexual function.
Using the baseline questionnaire raw scores, many of the questions strongly correlated with each other according to criteria found in Cohen.[38] Table 5 sum-marises the baseline QOL domains and composite scores that strongly correlated with overall QOL, physical health composite score and mental health composite. Overall QOL strongly and positively corre-lated with a number of health domains, including emotional wellbeing and energy, and also the mental and physical health composite score of the MSQOL-54.

Among the baseline questionnaires, 22 questions had a missing response. Five questions had greater than 2% of responses missing.
Discussion
Our study provides evidence of a continuing improve-ment in HRQOL in people with MS after attendance at a five-day residential retreat. Almost all the QOL domains assessed by the MSQOL-54 significantly improved or remained the same at one year and 2.5 years after subjects had attended the retreat. After 2.5 years, participants who attended the retreat made significant improvements in the overall QOL domain, physical health composite and mental health com-posite scores. None of the domains revealed any deterioration at either time point. This is quite unusual for a group of people with this chronic progressively disabling condition.
Our strong impression was that participants were greatly empowered by the programme; many arrived feeling hopeless and disempowered, with no sense of being able to help themselves in managing the illness. Many participants, in written feedback for course evaluation, commented that they felt inspired to take control of the illness, and that the course was life changing. The intervention was devised to be essen-tially self-administered with periodic input from the participant’s general practitioner to provide ongoing support and to monitor, for instance, vitamin D and B12 levels, medications and quality of life; participants felt this to be a more holistic approach to their health compared with periodic specialist appointments fo-cused largely on medications.
The presenters did not find the programme diffcult to implement, although it is not really suitable for larger groups as there are often many questions from participants to be answered during the sessions, and this would be unwieldy with groups greater than about 35. The programme appears to be relatively transport-able; a similar programme has been offered (by GAJ) annually since 2007 in the Coromandel in New Zealand, in conjunction with the MS Society of Auckland and the North Shore Inc.
The MSQOL-54
Measures of treatment effectiveness in MS have tra-ditionally been based on an evaluation of a patient’s level of impairment or disability using measures such as the Expanded Disability Status Scale. Clearly meas-uring quality of life is also critically important, and some would suggest a more important outcome than clinical outcome.[39] HRQOL is a broader measure of disease impact that conceptualises aspects of life quality or function influenced by health status.[40] A recent study has shown that the MSQOL-54 is better than generic measures in detecting treatment effects.[41] Measures of HRQOL can be used with a wide variety of populations and interventions, allowing compari-son between them. MS-specific HRQOL instruments are used to evaluate the clinical effectiveness of inter-ventions because they acknowledge that health status in MS is influenced by factors other than relapse rate and level of impairment.[42] Currently the MSQOL-54 questionnaire is the most commonly used evaluation tool for patients with MS.[42]
The reasonably high survey response rate of 58% was consistent with those found in other studies sur-veying MS populations.[43–45] It suggests that people with MS have a favourable attitude towards mailed surveys, and may in this study also reflect their positivity following the retreat, and an eagerness to contribute towards MS research.
Studies assessing QOL of people with MS over more than two years are scarce. However, in general they suggest a natural decline in most HRQOL domains over time in keeping with the known physical deterio-ration. The improvements found in our study differ for example from the findings of an Italian prospective study of 251 people with MS which showed that five years after the initial MSQOL-54 was completed, MS patients significantly worsened in the domains of change in health (P<0.0001), physical function (P<0.002) and health perceptions (P=0.01).
Surprisingly, despite MS being a chronic disease that gradually causes neurological impairment over time, there was a marginal but significant improve-ment in the MSQOL-54 cognitive function domain fter one year. This is similar to the physical health domain, which was also expected to gradually worsen over time, but instead improved at 2.5 years follow up.
Our findings are consistent with the results of the UK ‘OPTIMISE’ programme, where the health pro-motion programme had significant positive effects on physical function, mental (emotional well-being) health and general health (health perceptions) domains. How-ever, unlike our study, the OPTIMISE programme found no significant improvement in the pain, physical, emotional, social function and fatigue domains of QOL.[25] Similarly, in a wellness intervention for women with MS, only pain and mental health (emotional well-being) QOL domains improved significantly.[24]
Overall QOL positively correlated with emotional wellbeing, energy, health perceptions and health dis-tress QOL domains, and physical health and mental health composites. Interestingly, three out of the four mental health composite subscales correlated with overall QOL, and six of eight physical health com-posite subscales were associated with overall QOL. It appears that the perceived QOL of our MS participants was influenced by both mental health and physical health. These results contrast with those reported in another longitudinal study which evaluated the deter-minants of QOL among people with secondary pro-gressive MS.[46] It was proposed that interventions which improve the mental health of people with MS consequently improve perceived QOL. Our results suggest that both mental and physical health were equally important in contributing to perceived QOL.
Our study participants showed less optimistic self-reported QOL at baseline than was reported in a previous cross-sectional study.[47] In contrast to our study, where 65.7% of participants reported a favour-able QOL, the Canadian study reported 77% of their participants being mostly satisfied or delighted with QOL. It could be argued that due to the self-selected nature of our study, the retreat appeals to people who are dissatisfied with their QOL, as it is less likely that someone who is satisfied would actively seek to im-prove QOL further.
Although missing data suggest that the sexual func-tion scales may not be representative of sexual prob-lems in our sample, it is crucial to investigate the impact of sexual dysfunction among the MS popu-lation. A high proportion of people with MS experi-ence at least one symptom of sexual dysfunction[48] which influences all aspects of QOL. Consequently, future studies on HRQOL of the MS population should consider modifying the sexual function and sexual satisfaction scales of the MSQOL-54 or use an additional instrument to measure sexual dysfunction.
There are a limited number of longitudinal cohort studies monitoring the HRQOL of people with MS for more than two years. MS is so variable in clinical course and effect that it is important to assess the HRQOL of participants over a long period of time. More research needs to be done in this area so that the natural course and effect of interventions on HRQOL of people with MS can be assessed. Our study is continuing to enrol patients and we aim to report our findings at the five-year time point when we have enough participants.
Ideally studies evaluating the effect of interventions in MS should include a control group. The documented improvement from baseline to subsequent years of the survey may have been an artefact of maturation, that is, people with MS learned to cope over time and their changes in attitudes and adjusting to life with MS had nothing to do with the intervention. However, this is very unlikely as previous studies of people with MS over time have shown steady deterioration in quality of life.
Longitudinal cohort studies are particularly valu-able in monitoring populations with chronic diseases that are variable in their progression, particularly those evaluating non-drug therapies as ours has. How-ever, sample size can be a problem in such long-term studies due to the waning enthusiasm of participants to be involved; this was a limitation of the current study, in particular the small number of participants completing all three (baseline, one year, and 2.5 years) time points.
A measure of adherence would have been useful in this study to allow an assessment of the relative con-tributions made by the different parts of the inter-vention. Although the response rate in our study was quite high, the validation and use of an online version of the MSQOL-54 may increase the participation rate further, and this will be trialled in ongoing studies.
Our study relied on self-report for the diagnosis of MS and we did not require proof of diagnosis from participants. Hence it is possible that some of our participants may not have had MS but a similar neurological condition, although we did exclude all participants (four) who declared an alternative neuro-logical diagnosis. The type of MS among the study population was also unknown, and we can draw no conclusions about this.
Our results may not be representative of the MS population. A high proportion of our study participants were female, which is not reflective of the estimated female–male ratio of MS incidence of 3:1.[49] The female preponderance in our study might be explained by women’s greater willingness to talk about their diff-culties and to attend self-help programmes.
Longitudinal cohort studies can be useful in monitor-ing the progress of people with MS. This study showed ongoing improvements in HRQOL after an intensive lifestyle modification course. This could potentially make a significant difference to the lives of many people with this condition. Further controlled studies are warranted to examine the long-term effects of such interventions on QOL.
Our findings contribute to the growing body of evidence that health promotion programmes and non-drug therapies for MS patients have a beneficial effect. General practitioners may find this holistic approach useful in managing people with MS.
We are immensely grateful to Annie and Jim Simpson for their kind donation that enabled this research to proceed. The findings of this study were presented at the 15th International Holistic Health Conference of the Australasian Integrative Medicine Association, 9–11 October 2009.
Funded by a donation from Annie and Jim Simpson.
Ethics approval for this study (Ethics ID: 0723028) was granted by the Human Research Ethics Com-mittee of the University of Melbourne.
Not commissioned; externally peer reviewed.
Professor Jelinek was diagnosed with MS in 1999; he has been remunerated by the Gawler Foundation since 2007 for leading the residential retreats; he has pub-lished a book about the management of MS entitled
Overcoming Multiple Sclerosis: An Evidence-Based Guide to Recovery released by Allen and Unwin in 2010. Drs Gawler and Dye were remunerated by the Gawler Foundation.