Research Paper - (2011) Volume 19, Issue 1
Specialist Registrar, Radiology, Derriford Hospital, Plymouth, UK
Lesley Ward MBChB MRCP MRCGP
General Practitioner, GPSU lead, William Budd Health Centre, UK
Chris Salisbury MBChB MSc MD FRCGP
Professor of Primary Health Care
Sarah Purdy MBBS MPH MD FRCGP
Consultant Senior Lecturer
Academic Unit of Primary Health Care, University of Bristol, UK
Received date: 2 June 2010; Accepted date: 19 December 2010
BackgroundEmergency medical admissions to UK hospitals have been increasing steadily over the past few decades and there are likely to be a proportion of these admissions that are avoidable. This evaluation aims to demonstrate whether a general practitioner support unit (GPSU) reduces general practitioner (GP) referred emergency medical admissions to an acute hospital. MethodsThe GPSU comprises a team of GPs based in the hospital with the purpose of providing alternatives to admission for medical referrals from community GPs. This is an observational study of patients referred and admitted to the Medical Admissions Unit (MAU) of an acute hospital over two six-month periods, in 2007 prior to and in 2008 after the introduction of the GPSU. ResultsThe number of GP referrals to the MAU per day decreased by 1.55 (confidence interval –2.45 to –0.51) patients with the GPSU in place. The number admitted to the hospital per day from MAU decreased by a mean of 0.48 patients but with confidence intervals that included the null hypothesis (–1.39 to 0.44). In comparison, non-GP admissions that were not targeted by the GPSU increased by 3.99 per day (2.64 to 5.33). ConclusionAnacute GP led service run from within the hospital to provide support to community GPs led to a modest reduction in the number of GP admissions to the MAU, but did not reduce the number of GP admissions to the hospital wards.
acute medicine, clinical assessment, emergency care systems, pre-hospital care
Emergency medical admissions to UK hospitals have been increasing steadily over the past few decades despite attempts to address this issue.[1] There have been many attempts to describe the reasons behind this pattern. The most extensive recent attempt was made by the Nuffeld Trust in 2010,[2] who described the following statistics:
• The number of emergency admissions in England rose by 11.8% over the five-year period 2004/2005 to 2008/2009 – a total of approximately 1.35 mil-lion extra admissions.
• Older people are more likely to have an emergency admission. However, 40% at most of the increased number of emergency admissions over the period under study can be explained by the effects of population ageing.
• The rise in emergency admissions is not associated with any one particular type of illness or age group and levels of self-reported ill health do not appear to be rising.
• The increases have been associated with a large rise in short-stay admissions.
It follows that there are likely to be a proportion of admissions that are considered avoidable (the estim-ated proportion varies greatly from 3.4% to 41%).[3] Eradicating these unnecessary admissions would alle-viate the growing economic burdens on medical admission departments. Increasingly UK hospitals are looking towards specialist teams to reduce the number of inappropriate admissions from primary care. These teams are designed to bridge the gap between primary and secondary care, and are often comprised of general practitioners (GPs) based within the hos-pital in order to combine the generalist skills of the GP with the diagnostic technology that a hospital pro-vides. This combination is thought to prevent un-necessary admissions, which are a burden to the patient and costly to health services.
Evidence supporting acute GP admission avoidance schemes
Evidence in this area of research is generally weak because the reasons for this rising pattern of ad-missions are multifactorial and complicated[4] and are rarely amenable to randomisation. However, studies have tried looking at interventions that attempt to reduce admissions. First, primary care trusts and GPs are likely to be well positioned to implement changes in acute care services to good effect.[5] More specifically, in some studies GPs have been shown to be better than A&E doctors (particularly at junior grade level) at preventing unnecessary general emergency admis-sions when working in an emergency.[6,7] This is per-haps because they have greater awareness of holistic care, which has shown to be effective in reducing admis-sions,[8] and greater experience of alternatives within the community. Although, evidence for the effectiveness of GPs working in or alongside A&E is equivocal and the evidence for the cost effectiveness of such inter-ventions is weak, comparisons with other healthcare systems suggest that the NHS may have higher admis-sion rates for longer hospital stays.[9] However, increases in emergency admissions are probably greater for short stay rather than long stay cases,[10] which means that short stay cases could be targeted. Some research has shown that telephone interventions can be useful in reducing hospital admissions; however telephone triage which is not led by a physician may be harmful.[11]
However, senior opinion early on appears to have significant benefits.[12,13] There is some evidence that a two-tier approach to admissions may be of benefit, with targeting of low priority cases improving the effciency of admission departments.[14] There is evidence that collaborative approaches can be used to reduce admissions,[15] especially when GPs are involved.[16]
This study will interest health service policy makers and GPs, as well as clinicians who work within the admission departments of hospitals, such as A&E and medical consultants. It will also interest those who are likely to be affected by the changes described in the recent White Paper, as this was a locally commissioned project.
Overview of the admissions process in the UK
A basic knowledge of the UK healthcare system is required to understand this paper, as there are many different routes of patient admission to hospital (with the added complexity of regional variability). Firstly it is important to note the predominance of a free primary care service in the UK, which for the most part treats chronic disease but can also facilitate emergency admis-sions for patients if required. This is normally as a result of either a patient consultation, an unplanned home visit, or a telephone consultation with the patient by the GP. As well as this, acutely unwell patients can also self-present to the ‘secondary’ care hospitals via the A&E department when they seek care. In recent years other services have been set up, such as the ‘NHS Direct’ helpline and walk-in centres which offer health advice, often out of normal hours, via telephone and face-to-face consultation respectively. These may also result in unplanned admissions.
The pathway at the secondary care hospital largely depends on how the patient presents to the hospital. They may have self-referred, or have been brought in as an emergency to the A&E unit. From there patients are assessed or treated, then either discharged if no further care is necessary or referred onto a different department – for instance either the surgical or medi-cal admission units (SAU or MAU) if appropriate. These specialist admission wards can have a variety of names – Emergency Medical Unit (EMU) is another term commonly used for medical wards.
For those patients who are referred by a medical professional (primarily, but not exclusively GPs) they may bypass the A&E department and be referred straight to SAU or MAU if clinically indicated. How-ever, some GPs refer to the A&E department, espe-cially if there is doubt about the aetiology of the patient’s illness. Figure 1 figuratively demonstrates the local admission process.
Implementation of the GP support unit
This study examines the impact of a GP support unit (GPSU), a small team of GPs working from within an emergency MAU with the aim of preventing un-necessary admissions referred by GPs in the com-munity. The aim of the GPSU is to filter referrals and prevent admission for patients who can have alternative forms of disease management without detriment to their quality of care. Other studies have shown that schemes which target patients whose admissions might be avoided or curtailed can be asso-ciated with good results.[17] The GPSU team have more time, greater knowledge and experience of primary and secondary referral systems, and further access to investigations and specialist advice than community GPs – all resources that may help them to offer alternatives to admission that are beyond the means of a community GP.
The GPSU is staffed by a group of GPs who are based in the hospital near the MAU. There is a maximum of two GPs working per day. They are trained GPs with an interest in emergency medical care, some holding Membership of the Royal College of Physicians certification (MRCP). They have con-tinued working as GPs, either as locums or with regular sessions, whilst participating in the GPSU.
Initially it was decided that only GP medical referrals would be targeted by the scheme. This was because anecdotally medical referrals were believed most likely to be inappropriate admissions, and also because it was thought that this group of patients would be of significant enough size to occupy only a relatively small group of GPSU staff (often only one GP a day). It was also felt that, being staffed by GPs, the GPSU would be most capable of determining the appropri-ateness of referrals from fellow GPs, because this is their specialist medical area. Therefore, for the reasons outlined above, the GPSU did not manage patients referred by clinicians in the A&E department, GP referrals via A&E or any other referrals, e.g. from out-patients. The opening hours of the GPSU were there-fore designed to mirror the referral patterns of GPs. By starting at 10.00 hours and finishing at 19.00 hours the majority of GP referrals were fielded by the GPSU. The earliest GP referrals would tend to arrive mid-morn-ing, as the earliest community consultations were at from 08.00 hours and patients would inevitably take time to arrive, and GP practices would usually close at approximately 18.00 hours. Extension of these service hours was not therefore considered to be effcient use of time or money, neither were they extended to weekends, because they only dealt with GP referrals, which were very uncommon on Saturdays and Sundays.
There are several factors that are crucial to under-standing the economic impetus for the GPSU. As with most hospitals in the NHS, the commissioning pri-mary care trust (PCT) pays one of two tariffs per admission – one short-stay tariff, for patients staying anything up to three days in hospital (depending on the specialty), and a long-stay tariff, for patients staying longer than this, which is approximately three times the cost of the short-stay tariff. The short-stay tariff is payable as soon as a patient enters MAU, regardless of how long they stay, as shown in Figure 2. However, crucially, this tariff is not payable if the patient is managed by the GPSU, without admission to the MAU. The GPSU costs were paid directly by the PCT. The scheme was locally commissioned and the organisation and operational requirements were de-cided prior to the decision to evaluate the outcomes of the unit.
It is also important to bear in mind that this eval-uation was undertaken during the first few months of the GPSU’s operation, during which time the service was establishing new ways of working with the MAU and overcoming early operational diffculties. For example, it was not always possible to run the GPSU service as planned due to a shortage of rooms or staff.
Aims and objectives
This evaluation aimed to demonstrate whether the GPSU reduced overall emergency medical admissions to an acute hospital setting. We hypothesised that following the introduction of the GPSU there would be a reduction in the number of patients admitted to the MAU following GP referral, or at least a reduction in the increasing rate of year-on-year admissions. The study also aimed to describe any unintended consequences of the scheme. For instance, GPs might have wanted to avoid using the GPSU (by sending referrals to A&E) or become more attracted to using it as a convenience (and thus more patients might have been referred). The objectives were to analyse six months of MAU ward admission data prior to intro-duction of the GPSU, and six months following the introduction of the GPSU, to observe any changing trends in admission statistics.
This paper evaluates a local innovation that has been duplicated in other centres nationwide in order to prevent the expensive rise in emergency admissions. It used the STROBE (STrengthening the Reporting of OBservational studies in Epidemiology) criteria wher-ever applicable.[18]
Study design
The main purpose of this developmental study was to determine whether the GPSU reduced medical ad-mission rates. This was an observational analysis of the number of patients referred and admitted to an MAU period covering the same six months in 2007, prior to the setting up of the GPSU.
Participants
We included adult (patients aged 18 years and over) medical referrals made to the MAU during the period from 1 June to 30 November 2007 and 1 June to 30 November 2008. The following results describe only the number of patients seen on weekdays (when the GPSU is running) in both the pre-GPSU and post-GPSU periods. All patients were included regardless of age, sex or ethnicity.
Intervention – the GP Support Unit
All GP emergency medical referrals made between 10.00 and 19.00 hours on a weekday were put through by telephone to the GPSU, rather than to the MAU, so all referring GPs had to at least discuss the patient with the GPSU (Figure 2).
At this stage the GPSU would either: i) direct the patient to an alternative care pathway; ii) refer them directly on to the MAU; or iii) admit them to the GPSU to consider more closely whether they needed admission to the MAU.
Patients seen by the GPSU are:
• patients for whom the GP is unsure whether they need admission, further assessment, diagnosis or ruling out of a problem
• patients who prefer not to be admitted to hospital but want a safe alternative
• patients for whom it is diffcult to organise com-munity care
• patients for whom there is diffculty organising outpatient blood transfusions, urgent outpatient slots, investigations or direct access to radiology.[19]
Setting
The MAU data were collected for the following periods, 1 June to 30 November 2007 and 1 June to 30 November 2008. The GPSU was set up on 26 May 2008.
Data collection
The information on referrals and admissions was retrospectively abstracted from handwritten medical admission charts used daily in the MAU. Each new day started with a new admission chart and all patient referrals and admissions were entered onto the chart as the day progressed. The chart was regularly updated and consulted frequently by senior nurses and doctors throughout the day as it was considered the most accurate guide to the number of patients referred or admitted, the time they were referred, from where they had been referred, their presenting complaint and whether they were subsequently discharged or admit-ted. These charts were collected retrospectively and data used for this study were taken from these charts for every day during the six-month period. We felt that this was the most reliable way of assessing the numbers of admissions as well as the method of admission. Hospital admission statistics have in the past been noted as being unreliable, especially in attributing the wrong mode of admission to a patient. By going through admission sheets for each day we were able to trace each patient’s journey through the MAU, which we felt was a more accurate way of collecting data.
As well as this, information was collected on patients assessed in the GPSU. Data were collected on the patient’s name, age, presenting complaint and whether they were discharged or admitted. For hos-pitals that do not have these methods of recording patient admissions similar processes could easily be set up for the purposes of analysing admissions data.
Variables
The main explanatory variable was whether or not the GPSU was in operation. The hours of operation were weekdays between 10.00 and 19.00 hours in the 2008 study period. The main outcome variables were the number of patients referred and admitted on week-days by the different modes (A&E, GP, GP via A&E, other) and the total number of referrals and admis-sions. Other secondary outcome measures were the number of patients seen and admitted in the GPSU. All patients referred by GPs with a view to emergency medical admission were included, whether they were seen in the MAU and/or by the GPSU. The presenting complaints for the GPSU patients assessed were also recorded and are presented in the results section.
Study size
Over the study periods 12 762 patients were referred to the MAU or GPSU: 6050 patients in the period prior to the GPSU (June to November 2007) and 6712 patients in the corresponding months after the GPSU was started (June to November 2008). These figures included patients admitted at any time, including weekends, to give a full appreciation of the impact that the GPSU had on the volume of admissions over those periods, even though it was only active on weekdays for the reasons described above. The num-ber of patients involved exceeded, or was similar to, many other studies of this type.[17,20–22]
Statistical methods
We used STATA to compare data from the two six-month periods prior to and following the setting up of the GPSU. Univariable analysis was used to see if there was any significant change in the number of GP referrals and total admissions after the GPSU began operation. Means, confidence intervals, and standard deviations are given for the daily number of weekday admissions, by all modes of entry, for the two different study periods.
Assessment of GP referrals on the telephone found that the majority (66.9%) of these admissions were considered to be unavoidable, and so the patient was admitted directly to the MAU. Of the 6712 patients admitted in the 2008 period on any day, by any mode of admission, 581 (8.66%) were assessed by the GPSU (which worked only weekdays). Of those patients assessed at the GPSU, 473 (81% GPSU patients and 7.05% of MAU referrals) were discharged or put on an alternative pathway, and therefore were ultimately not admitted to the MAU.
The results comparing the two time periods are shown in Table 1.
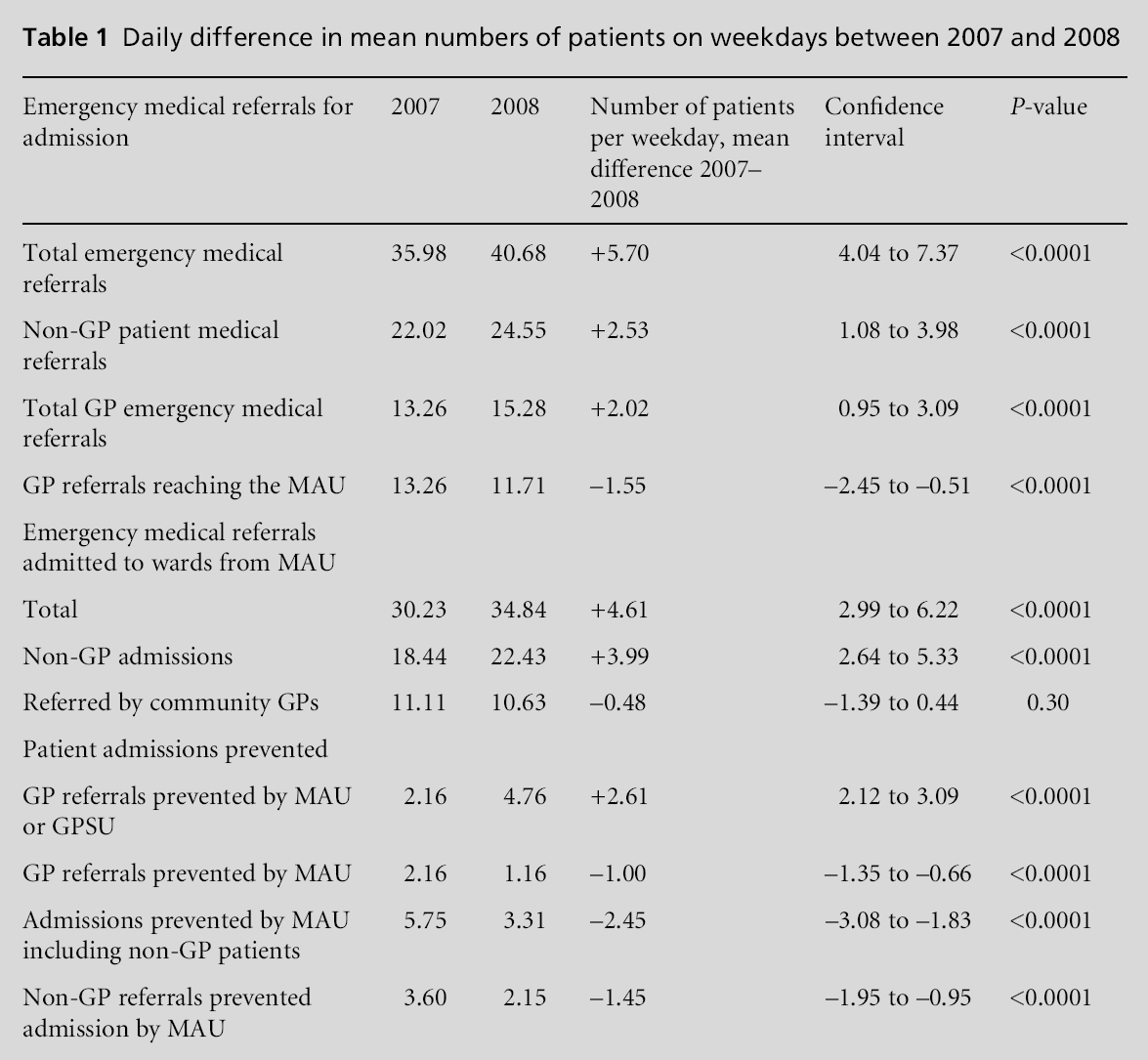
These data are presented diagrammatically in Figures 3 and 4.
Approximately 1.1 patients per day in 2007 and 1.8 in 2008 did not have a clear mode of admission stated on the MAU admissions chart and are labelled ‘un-known’.
Of all the GP emergency referrals made for MAU admission the GPSU intervened in 33.1%, either by offering an alternative care plan to the community GP over the phone or after further assessment in the GPSU based at the hospital. They found alternatives to admission for 81% of patients seen. The number of GP referrals to MAU decreased by 1.55 patients per day after GPSU filtering (confidence interval –2.45 to –0.51). However, the number admitted from MAU to the hospital only decreased by a mean of 0.48 patients per day, with confidence intervals that included the null hypothesis (–1.39 to 0.44). Overall the total number of all medical referrals admitted to the wards per weekday increased by a mean of 4.61 (P 0.001) patients/day during the study period. This rise in overall admissions was largely attributable to non-GP admissions, whilst the number of GP referrals to MAU decreased slightly or at least remained static compared with 2007.
Limitations and bias
The main limitation is that this was a before-and-after study rather than a randomised trial. There may have been other changes occurring between 2007 and 2008 unrelated to the GPSU, affecting either the organis-ation of the hospital or the characteristics of patients referred. Such changes might have included alter- ations to specific disease treatment pathways, admis-sion policies, MAU staff and GP referral behaviour although no major systematic changes were offcially introduced. It was also not possible to blind the participants, clinicians or assessors to the study’s intervention or results.
In addition, a long-term expected year-on-year increase in emergency medical admissions may have masked any effect of the GPSU. The local rates of admission did not reflect the national pattern of a consistent annual rise. Unfortunately the variable nature of the local statistics meant that it was not possible to adjust for the year-on-year increases in a time series analysis.
There is also some potential for measurement bias. Some entries for patients on the MAU’s admission sheets did not specify where they had come from, although this was far less than 5% of the overall patient sample. Also errors in recording or data synthesis may have occurred in the admission sheets. However, by using data that were taken from admission sheets that were intrinsic to the organisation of the department (senior nurses and doctors refer to these sheets regu-larly throughout the day to keep track of patients and take stock of the daily intake of patients) we felt that the source of information was the best available.
Services are understandably often evaluated when they are first established, but the findings may be misleading since new services often experience ‘teeth-ing troubles’ which reduce effciency and which do not reflect performance when the service is fully func-tioning. This bias may have affected this study. The GPSU was studied during its first six months in operation, when new skills and treatment pathways were being developed to improve its effciency. Equally, however, the service may have been vulnerable to greater ‘supply induced demand’ once it became more established. Also in the future the service may become more effective by targeting non-GP patients from the A&E department.
In conclusion, there are likely to be some limi-tations to the generalisability of this study to other NHS trusts. Nevertheless, it offers a reasonable insight into a scheme that is different from many of the other attempts to reduce hospital admissions, and one that is currently being implemented in other hospitals.
Comparison with other studies
Previous studies have shown the greater effciency of GPs when compared to A&E department doctors in preventing admissions.[4,5] Research has also shown that targeting patients who are most likely to have their admission prevented or curtailed means a greater likelihood of making admission prevention schemes effcient.[7] This study examined a scheme that com-bines these two approaches and shows that the GPSU may have a role in reducing emergency medical admissions. It also looked at the specific presenting complaints of those admissions thought to be pre-ventable, so that future studies may be able to focus on certain patient conditions.
Implications for future practice and research
The GPSU appeared to be effcient at offering alterna-tives to admission for the patients that it saw, with 81% of patients (of the 33.1% of medical GP referrals that they considered) offered alternative care. How-ever, this translated into a relatively small reduction in GP referrals to the MAU and a non-significant reduc-tion in overall admissions from the MAU to the hospital. Although the GPSU was not designed specifically as a pilot to inform future service development, its design incorporated many ways of improving the admissions services.[22] The impact of the GPSU was possibly limited by the fact that it was only targeting patients that GPs had already seen (inappropriate admissions should already have been filtered out) and perhaps not targeting certain patients (many studies focus, with good results, on certain diagnoses or social groups). The following are possible explanations why this unit failed to make a large impact on hospital admissions:
1 Rising year-on-year admissions may have masked its effect. There is no clear evidence of a year-on-year increase in GP medical admissions locally; however, PCT data from 2008 showed that GP admissions from the hospital catchment area where the GPSU operated decreased by as much as 7% in 2008, whereas other in local areas this increased by up to 6%. Also, a large rise in non-GP admissions in 2008 – a trend that GP admissions ordinarily mirror
– would suggest that there had been masking of its effect.
2 The GPSU may have attracted more GP referrals, some of which may not necessarily have needed admission. This theory is supported by an increase of 2.02 GPs referrals a day in 2008 – an increase of 15% which exceeds any expected year-on-year increase. Therefore the 2.61 extra GP patients that were not referred on by the GPSU for admission may not have actually been ‘avoided admissions’ as, prior to the GPSU, they might not have been referred to hospital at all. Community GPs in 2007 may have been advised by MAU staff over the telephone to follow an alternative care plan and no offcial recording of the ‘referral’ was made.
3 The GPSU may have prevented admissions of patients who would have been sent home by MAU staff that day in any case (probably for a similar cost) therefore not affecting the number of patients that went from MAU to the hospital wards. Approximately one less GP referral was discharged each day by the MAU staff while the GPSU was in operation. It is inter-esting therefore to note that although referrals to MAU were reduced by 1.55 patients per weekday, the number being admitted from MAU into the main hospital only shows a reduction of 0.48 patients per day.
4 Fewer non-GP referrals were discharged from MAU (1.6 less patients per weekday). This might imply that the GPSU’s involvement with GP referrals reduces MAU’s surveillance for discharging inap-propriate non-GP referrals, having the effect of increasing admissions overall.
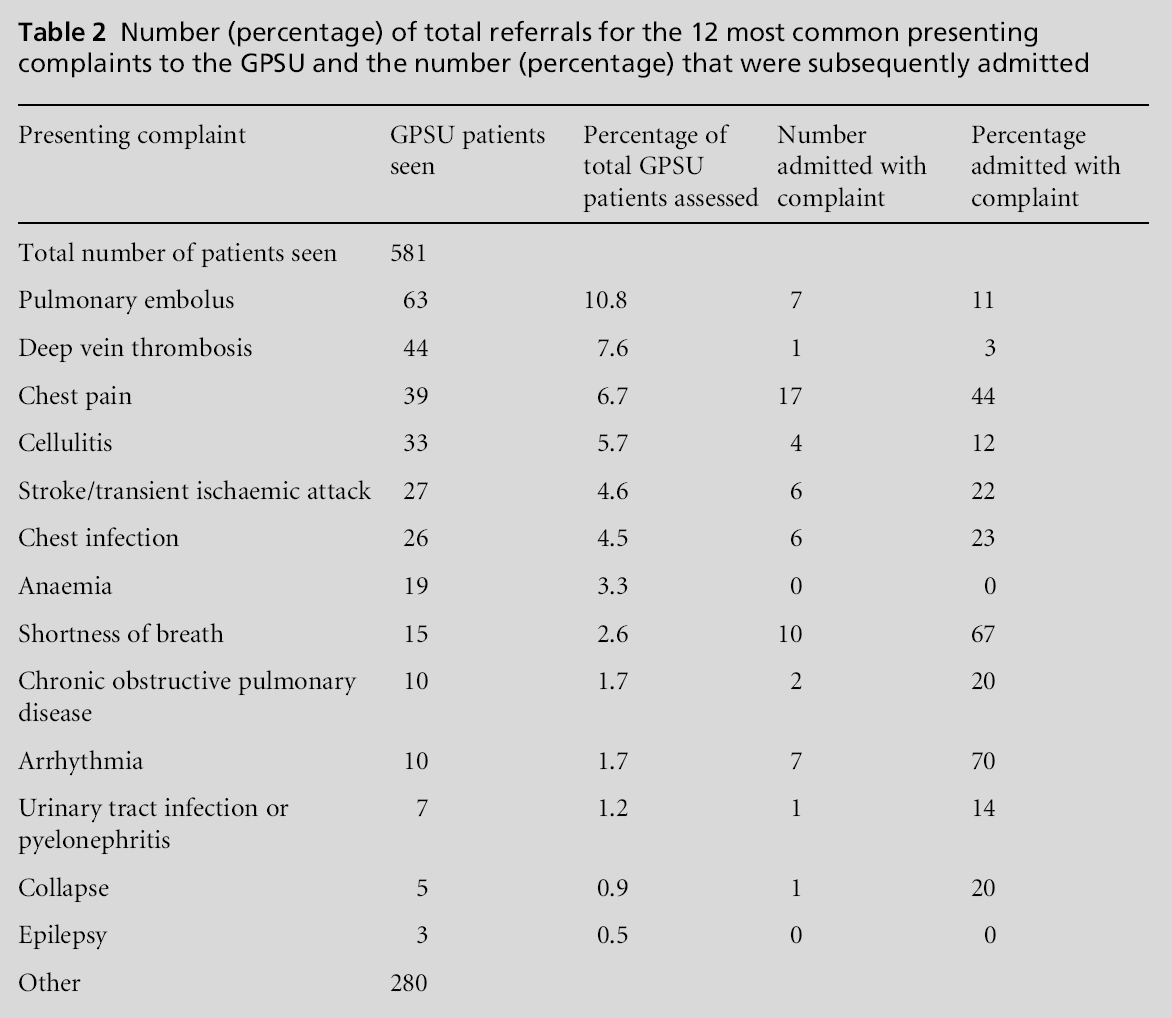
The presenting complaints recorded showed that pulmonary embolus and deep vein thrombosis were the two most common presenting complaints for which the GPSU felt they provided alternative care (Table 2). It is no coincidence that the diagnosis for these conditions involves two relatively straightfor-ward tests that are not available in primary care (computerised tomography pulmonary angiogram and venous Doppler of the lower limbs respectively). Further focus on and development of the care pathways for these conditions may improve admission rates in the future. Primary care may require easier access to diagnostic technology that can prevent unnecessary admissions.
There is a predicament here that is likely to be more and more familiar to policy makers as we enter the new era of local GP commissioning. Policy decisions affecting local care will often require complex and relatively expensive assessment to determine whether the imple-mented policies have been useful. Nationally introduced initiatives have often been evaluated at a national level by major NHS research funding bodies, who usually favour large multicentre studies over small local ones on the grounds of generalisability. However, in the future GP commissioning is likely to mean the intro-duction of many interesting locally designed initiatives with limited national generalisability, which therefore will probably not attract substantial national research funding. Are we entering a fragmented world of local policy with a lack of evidence about effectiveness? This paper highlights the importance of careful and critical assessment of the benefits of initiatives at a local level, as initiatives may not always have as great an impact as anticipated.
It is important to note that approximately two-thirds of emergency admissions were not referred by GPs. Although the intervention was targeted at GPs, and many policies are implemented to reduce hospital admissions by GPs, it may be that interventions to reduce emergency admissions may be more effectively targeted at patients who reach hospital without being referred by GPs. This might be achieved by involving the GPSU in assessing patients not referred by GPs or by increasing awareness amongst A&E and MAU staff about community alternatives to admission.
The GPSU provides only a limited reduction in the number of GP admissions to MAU and does not significantly reduce GP referred medical admissions to hospital wards, albeit against a background of increasing non-GP admissions.
Out thanks to the GPSU for providing data on their patients.
Funding for Patrick Rogers for this project came from the Severn Deanery Academic Foundation Programme.
Ethical approval was not required as this was an evaluation of a service at the request of the local commissioners.
Not commissioned; externally peer reviewed.
Lesley Ward is a general practitioner, and at the time this study was conducted was employed as the clinical lead for the GPSU.