- (2012) Volume 13, Issue 4
Puja Srivastava1, Nusrat Shafiq2, Deepak Kumar Bhasin3*, Surinder Singh Rana3, Promila Pandhi2, Arunanshu Behera4, Rakesh Kapoor5, Samir Malhotra2 and Rajesh Gupta4
Departments of 1Internal Medicine, 2Clinical Pharmacology, 3Gastroenterology, 4Surgery, and 5Radiotherapy, Post Graduate Institute of Medical Education and Research (PGIMER), Chandigarh, India
Received March 31st, 2011 - Accepted April 23rd, 2012
Context The role of heat shock protein (HSP) 70-2 gene polymorphism (at position 1267, A to G transition) in patients withpancreatic disorders is not clear. Objective To evaluate HSP 70-2 gene polymorphism (at position 1267, A to G transition) inpatients with acute and chronic pancreatitis as well as pancreatic carcinoma, and to find any association of this polymorphism with disease complications and severity. Methods One-hundred and fifty patients (50 each of acute, chronic pancreatitis, and pancreatic carcinoma) and 50 healthy blood donors as controls were prospectively studied. Three alleles (AA, AG and GG) of HSP 70-2 gene determined by PstI restriction fragment length polymorphism. Results There was a statistically significant difference in the distribution pattern of HSP 70-2 gene polymorphism in patients with acute pancreatitis (P=0.001) and pancreatic carcinoma (P0.001) as compared to controls. The frequency of mutant allele (G allele) was significantly higher in diseased group as compared to control group (19% in control group, 40% in acute pancreatitis, 33% in chronic pancreatitis and 45% in pancreatic carcinoma). No association of this polymorphism was found with disease severity in patients with acute and chronic pancreatitis or pancreatic carcinoma. Conclusions In our patient sample the frequency of mutant allele (G allele) of HSP 70-2 gene is significantly higher in patients with acute pancreatitis and pancreatic carcinoma compared to controls (50 healthy blood donors). However, this polymorphism was not associated with disease severity and complications.
Genetics; Pancreas; Pancreatic Neoplasms; Pancreatitis, Acute Necrotizing; Pancreatitis, Chronic
HSP: heat shock protein
A genetic predisposition to pancreatic diseases was recognized by Comfort et al. [1] as early as 1952. Subsequently in 1996, it was shown that mutations in cationic trypsinogen gene (PRSS1) lead to hereditary pancreatitis [2]. Later other gene mutations such as mutations in serine protease inhibitor Kajal type 1 (SPINK1), cystic fibrosis trans-membrane receptor (CFTR), and alpha 1 antitrypsin have been shown to be associated with recurrent acute and chronic pancreatitis. However, these mutations have not shown a definite cause effect relationship with pancreatitis, though they definitely increase susceptibility of an individual to chronic pancreatitis. According to the Verona Classification for Pancreatitis [3] many as yet unknown mutations/polymorphisms may have a role in pancreatic diseases, which are currently classified as idiopathic. After decoding of human genome, it is becoming clear that many pancreatic diseases have a genetic basis.
Heat shock proteins (HSPs) are proteins synthesized by eukaryotic cells and bacteria upon exposure to sublethal stress such as hyperthermia, hypoxia, ischemia/reperfusion, and other environmental stresses [4]. In humans, three members of the HSP 70 gene family have been mapped and described. They include HSP 70-1, HSP 70-2, and HSP 70-HOM, of which HSP 70-2 encodes the major heat inducible HSP 70. This gene has been shown to be polymorphic by Milner and Campbell [5] who identified the polymorphic A to G transition PstI site at position 1267 in the coding region of HSP 70-2. This polymorphism has been studied in various other diseases besides pancreatitis, like myocardial infarction [6], Crohn’s disease [7], renal failure in preterm neonates [8], rheumatoid arthritis [9], systemic lupus erythematosus [10], congestive heart failure [11], stroke [12], and diabetes mellitus [13]. Few recent studies [14] have shown that HSP 70 has dual role in pancreatic diseases. It has a protective role in pancreatitis but its exact role in pancreatic cancer is still not clear. HSP 70 protects against cellular injury and acinar necrosis in pancreatitis, leading to reduced severity of acute pancreatitis [14]. HSP 70 was over expressed in pancreatic cancer and this over expression is probably responsible for the resistance to cell death. Inhibition of HSP 70 expression lead to apoptotic cell death in pancreatic cancer cells and is a promising therapeutic strategy for the treatment of pancreatic cancer [14]. No clear information is available about the role of HSP 70 in patients in chronic pancreatitis. This study was conducted to evaluate HSP 70-2 gene polymorphism (at position 1267, A to G transition) in patients with acute and chronic pancreatitis of various etiologies as well as with pancreatic carcinoma, and to find any association of this polymorphism with disease complications and severity.
Study Population
Patients with acute pancreatitis, chronic pancreatitis and pancreatic cancer, who visited our out-patients clinic and/or were admitted as inpatients from January 2008 to May 2009 in our hospital, were screened for the eligibility criteria.
The eligibility criteria were
1) acute or chronic pancreatitis: the diagnosis made on the basis of clinical, biochemical and radiological investigations [15, 16];
2) pancreatic carcinoma: tissue diagnosis obtained by fine needle aspiration cytology/biopsy or widespread disease on radiological investigations.
Exclusion criteria included conditions, which are known to be associated with increased levels of HSPs, such as recent stroke (less than 3 months), recent acute coronary syndrome (less than 1 month), any other malignancy except pancreatic malignancy, rheumatoid arthritis and inflammatory bowel disease.
A total of 180 patients were screened for potential eligibility and 150 (83.3%) were included in the study, while others (n=30) were excluded on account of the following reasons: not willing to give consent (n=12) or not satisfying the inclusion criteria as well as those having one of the exclusion criteria (n=18). Among the 150 patients included, there were 50 cases each of acute and chronic pancreatitis and 50 cases of pancreatic cancer.
The various etiologies and varying disease severity were evaluated in the 50 patients with acute pancreatitis. The etiology of acute pancreatitis was alcohol in 25 (50%) patients, gallstones in 15 (30%) patients, both alcohol and gallstones in 2 (4%) patients, hypertriglyceridemia in 2 (4%) patients, hyperparathyroidism in 1 (2%) patient and pancreas divisum in 1 (2%) patient. No definite cause of acute pancreatitis could be found in 4 (8%) patients and these were labeled as acute idiopathic pancreatitis. Among the 50 patients of chronic pancreatitis, 26 (52%) were alcohol related, 20 (40%) were idiopathic, 2 (4%) were related to primary hyperparathyroidism and 2 (4%) had pancreatic divisum. Of the 50 patients with pancreatic cancer, the tumor was located in the head region in 33 (66%) patients whereas in 17 (34%) patients it was located in the body or tail region. Tissue diagnosis was available for 46 (92%) patients, which included 41 (82%) adenocarcinoma, 3 (6%) pancreatic neuroendocrine tumor (out of which two were insulinoma) and 2 (4%) papillary mucinous cystadenocarcinoma of the pancreas. In 4 (8%) patients, biopsy or fine needle aspiration cytology could not be performed as family decided against any further treatment or investigation as patients had widespread metastatic disease. All the patients were clinically evaluated and various hematological, biochemical and radiological investigations necessary for the clinical management of patient were performed and findings recorded.
Fifty healthy blood donors were included as control subjects. These controls did not have any history of pancreatitis in them or in their family.
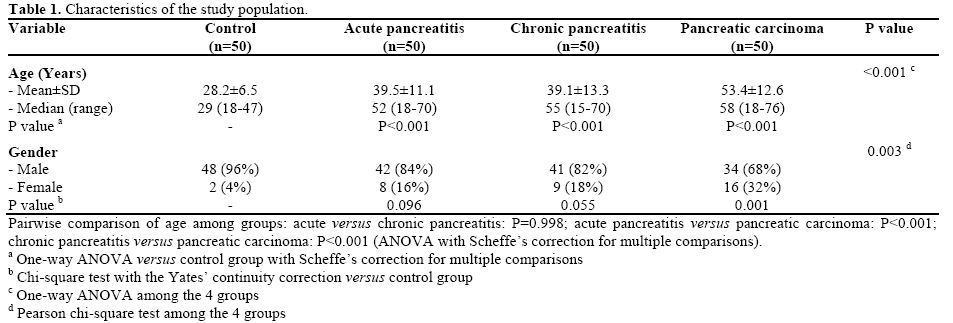
Ten mL of serum samples of patients and controls were stored in deep freezer and thawed later for HSP 70-2 gene polymorphism analysis. The demographic profile of study population is given in Table 1.

Determination of HSP 70-2 Gene Polymorphism by PCR-RFLP Technique
Genomic DNA was extracted from peripheral blood leucocytes by phenol-chloroform extraction method. The gene in concern was amplified by means of polymerase chain reaction (PCR) technique. Following primers spanning the polymorphic PstI site (nucleotide 1267) were used: sense (nucleotides 1083-1102 within the coding region) 5’-CAT CGA CTT CTA CAC GTC CA-3’ and antisense (nucleotides 2180-2199 within the 3’untranslated end) 5’-CAA AG T CCT TGA GTC CCA AC-3’. The PCR reaction mixture (30 μL) contained approximately 150 ng genomic DNA, 1 mmol of primers, 2.5 U Taq polymerase, 1.5 mmol/L MgCl2, and 10 mmol/L of each deoxyribonucleoside- 5’triphosphates (dNTPs). The PCR procedure was started at 95°C for 5 minutes, then 35 cycles of denaturing at 94°C for 1 minute, annealing at 56.2°C for 1 minute, extension at 72°C for 1.5 minute, and finally 10 minutes at 72°C. For RFLP analysis, the PCR products were digested by PstI restriction enzyme (3 U) at 37°C for 3.5 h. The digestion products were electrophorezed on a 1.5% agarose gel, and visualized under UV illumination after staining with 0.4 mg/L ethidium bromide. Following digestion with RFLP, homozygous wild types (A allele) showed single band of 1117 base pair, while homozygous mutants (G allele) had two bands each of 936 and 181 base pairs and heterozygous variants (AG allele) were found to have three bands of 1117, 936 and 181 base pairs.
Informed consent was obtained and study protocol conforms to the ethical guidelines. The project was approved by the institute ethics committee.
Continuous data were expressed as mean and SD values. Dichotomous data were expressed as absolute and relative frequencies. Comparisons for continuous data were done by ANOVA followed by post hoc Scheffe’s test. The genotypes and allelic frequencies were studied and compared by using the Pearson chi square test, the liner-by-linear association; the Yates’ correction was applied to the 2x2 tables. Odds ratio with 95% confidence interval was calculated for G allele by means of the logistic regression model. A two-tailed P value less than 0.05 was considered to be statistically significant. A commercially available statistical program (SPSS version 10.1; SPSS Inc., Chicago, IL, USA) was used.
Distribution of HSP 70-2 Gene Polymorphism in the Study Population
There was a statistically significant difference in the distribution pattern of HSP 70-2 gene polymorphism in patients with acute pancreatitis (P=0.001) and pancreatic carcinoma (P<0.001) as compared to the control population (Figure 1). Similar difference in genotype distribution pattern was not noticed in patients with chronic pancreatitis as compared to control (P=0.075) (Figure 1). No significant difference was noticed in polymorphism distribution pattern among the different diseased groups; i.e., patients with acute pancreatitis, chronic pancreatitis and pancreatic carcinoma (P=0.198).
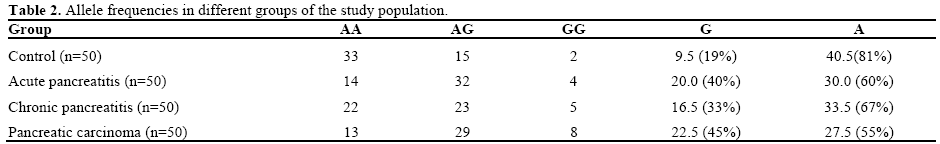
Percentage of specific allele was calculated to find out the impact of various alleles, on the disease parameters. Assigning one full point to AA and GG allele and half point each for A and G did this to AG allele. The G allele was 19% in control as compared to 40%, 33% and 45% in acute pancreatitis, chronic pancreatitis and pancreatic carcinoma, respectively (Table 2).

The odds ratio of G allele versus the control group for acute pancreatitis was 2.84 (95% CI=1.15-7.03), for chronic pancreatitis was 2.10 (95% CI=0.84-5.27), and for pancreatic carcinoma was 3.49 (95% CI=1.42-8.58) (Table 3).
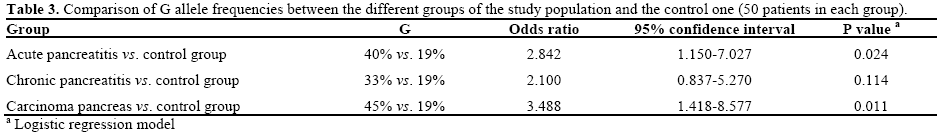
Association of HSP 70-2 Gene Polymorphism with Disease Severity and Complications
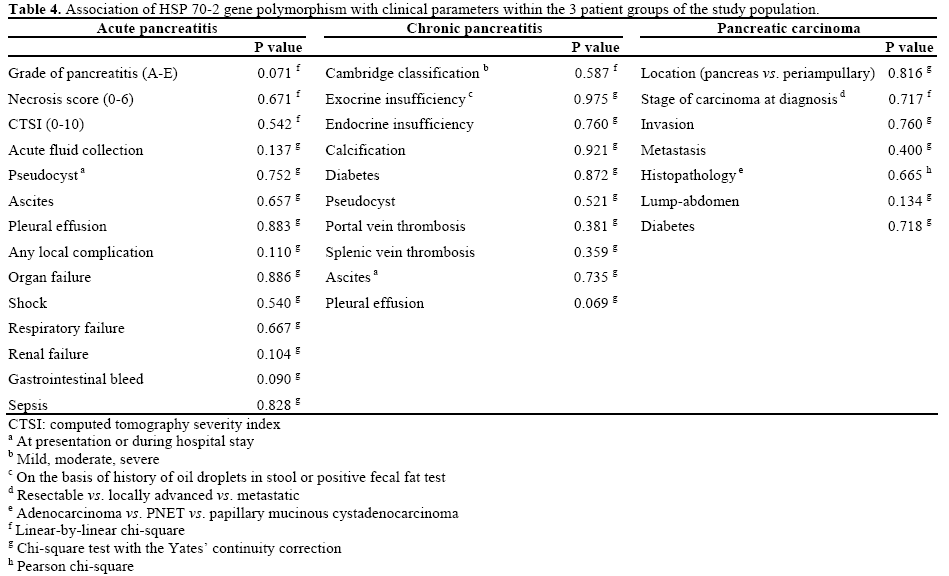
In the present study we did not find any association of this polymorphism with disease severity in patients with acute or chronic pancreatitis or pancreatic carcinoma. Similarly, there was no significant difference in polymorphism distribution pattern and disease presentation or presence of disease related complications (Table 4).
It is becoming clear that some combination of genetic mutation polymorphisms provide predisposition for pancreatitis; and if a risk factor is introduced (e.g., alcohol, metabolic derangement, physiologic stress to acinar cells), this polygenic predisposition sets the stage for pancreatitis. Recently HSP 70-2 gene has also been associated with pancreatic diseases, and various studies have given conflicting results, and a definite role of this polymorphism has not yet been confirmed in these diseases [14]. In the present study, mutant allele of HSP 70-2 gene (G allele) was significantly higher as compared to control population in patients with acute pancreatitis and pancreatic carcinoma. However, in the chronic pancreatitis patients though AG and GG alleles were more common, the difference did not reach a statistical significance. Fifty healthy blood donors were included as control subjects. To avoid bias a detailed history was taken from them and their family members about pancreatitis or any serious illness in them or in their family.
Three studies in which this specific polymorphism was evaluated in patients with pancreatic diseases were identified. Two of these were carried out in acute pancreatitis patients [17, 18] and one in chronic pancreatitis patients [19]. While one study evaluated the role of three specific polymorphisms (TNF-alpha, HSP 70-2, and CD14 genes) in determining susceptibility to severe acute pancreatitis of various etiologies, the second study evaluated the role of TNF, CD14, and HSPA1B gene polymorphisms in susceptibility to acute alcohol induced pancreatitis. The third study evaluated the role of MCP 1 and HSP 70-2 genes in susceptibility to alcoholic chronic pancreatitis. To the best of our literature search, no study has analyzed the association of this polymorphism with pancreatic carcinoma. However, few studies have evaluated HSP in pancreatic carcinoma at proteomic level, and have given conflicting results. One study [20] reported that higher levels of HSPs are associated with more advanced disease in German population whereas another study [21] reported that higher levels of HSP expression in cancer tissues was associated with less advanced and more resectable disease in Turkish population.
Interestingly, the percentage of G allele was increased in all the three diseased conditions as compared to the control group (40%, 33% and 46% in acute pancreatitis, chronic pancreatitis and pancreatic cancer, respectively vs. 19% in the control group). Similar results were noted in a study [18] in patients with acute pancreatitis in Hungarian population where G allele frequency was higher (40.2% vs. 35.9%) in acute pancreatitis patients as compared to control group. However, in another study [17] conducted in patients with acute pancreatitis in Finish population, G allele frequency was found to be no significantly different between patients with acute pancreatitis as compared to controls (52% in acute pancreatitis vs. 49% in control group). This is not surprising as controversy between the sequential studies is a common phenomenon in case-control studies [22]. A similar study [19] in patients of alcoholic chronic pancreatitis in Korean population, found no statistically significant difference in G allele frequency between patient and control group (52% in chronic pancreatitis vs. 49% in control group) as compared to significant difference in the present study (33% in chronic pancreatitis vs. 19% in control group). No studies are available which compared the G allele frequency in carcinoma and control population although we found a higher mutant allele frequency in carcinoma as compared to control population (45% vs. 19%).
The polymorphism distribution pattern of HSP 70-2 gene polymorphism in normal population of our country is not available at present. However data about the polymorphism distribution from other populations are available. A study conducted by Xie [23] in 88 chronic obstructive pulmonary disease patients and 87 healthy smokers as control in Chinese population reported G allele to be 23% among control population and 19.3% among chronic obstructive pulmonary disease patients. The prevalence of G allele frequency of this control population was comparable to ours (23% in Chinese vs. 19% in Indian population). If we consider this to be representative genotype distribution pattern in our population, results of our study suggest a role of mutant G allele in susceptibility to acute pancreatitis and pancreatic carcinoma, and a similar trend in chronic pancreatitis. However, distribution of polymorphism under evaluation was markedly different from control groups of other ethnic populations (35.9% in Hungarian, 49% in Finish and 49% in Korean population). This difference in genotype distribution pattern in different population can also be attributed to differences in inherent genetic composition of these population as well as other environmental effects.
Previously, Balog et al. [18], Saluja and Dudeja [14], and Aghdassi et al. [20] have evaluated the association of HSP 70 polymorphism with development of complications in pancreatic diseases and have shown that higher G allele frequency is associated with more severe disease. In our study, in patients with acute pancreatitis complications like acute fluid collection, pseudocyst, ascites, pleural effusion, any local complication, organ failure which included gastrointestinal bleed, renal failure, respiratory failure, shock and sepsis were evaluated for their association with the HSP 70 polymorphism. However, no significant association was noted in the distribution of genotype and development of any of the above complications. Similarly no such association could be found in patients with disease severity and complications in patients with chronic pancreatitis (Cambridge score, exocrine insufficiency, endocrine insufficiency, diabetes, calcification, steatorrhea, pseudocyst, splenic vein thrombosis, portal vein thrombosis, ascites) or advanced, metastatic disease in pancreatic adenocarcinoma (Table 4). The possible reasons for lack of such association can be: 1) larger sample size is required for genetic association studies; 2) different ethnic composition of our population as compared to other studies, in which polymorphism distribution was not comparable even among control population; 3) different haplotypes in chromosome 6 (e.g., TNF alpha and beta, complement components C2, C4 and Bf, enzyme 21 hydroxylase, etc.) which are in close proximity of HSP 70-2 genes may have an impact on disease severity and predisposition for development of complications via the effect of linkage disequilibrium, via promoter, modifier or suppressor effect.
In conclusion, our study showed significantly higher frequency of HSP 70-2 gene mutant allele (G allele) in patients with acute pancreatitis and pancreatic carcinoma as compared to control population. Frequency of mutant allele was higher in all three diseased groups as compared to control group. No association was seen between this polymorphism and disease severity as well as complications. However, further studies with large sample size are needed in order to confirm our results and to study the association of this polymorphism with disease severity and complications. Further studies are also warranted to look at the modifier role of other genes located on chromosome 6 in close proximity with HSP 70-2 gene that may have an impact on disease severity.
We thank and acknowledge Professor Ashok Saluja, Professor and Vice Chair of Surgery, University of Minnesota, Minneapolis, MN, USA for his help and guidance. This work had been presented at DDW 2010, New Orleans, LA, USA
No financial support and no financial disclosures to be made