Research Article - (2017) Volume 4, Issue 1
Baljit Singh1, Ashima Sharma2, Arunima Sharma3 and Abhishek Dhiman1
1Department of Chemistry, Himachal Pradesh University, Shimla, HP, India
2Department of Physiology, Indira Gandhi Medical College Shimla, HP, India
3Sikkim Manipal Institute of Medical Sciences, Gangtok, Sikkim, India
*Corresponding Author:
Baljit Singh
Department of Chemistry, Himachal Pradesh University
Shimla, HP - 171005, India.
Tel: 1772830944
Fax:1772830775
E-mail: baljitsinghhpu@yahoo.com
Received date: March 20, 2017 Accepted date: April 25, 2017 Published date: May 02, 2017
Citation: Singh B, Sharma A, Sharma A, et al. Design of Antibiotic Drug Loaded Carbopol-Crosslinked-Poly (2-Hydroxyethylmethacrylate) Hydrogel for Wound Dressing Applications. Am J Drug delv therap. 2017, 4:1.
Present article describes the synthesis, characterization, swelling and drug release behaviour of carbopol-cl-poly (2-hydroxyethylmethacrylate) hydrogel wound dressings. These polymers were characterized by, scanning electron microscopy, atomic force microscopy, Fourier transform infrared spectroscopy, 13C nuclear magnetic resonance spectroscopy, X-ray diffraction study, thermal degradation studies, and differential scanning calorimetry. The hydrogel film possessed smooth, homogenous surface with average surface roughness 0.570 nm. Swelling of the hydrogels increased with increase in pH of swelling medium. The hydrogel film showed 429.23 ± 33.23 % swelling in simulated wound fluid. The drug release studies showed slow drug release upto 24 h. Drug release occurred through nonFickian release mechanism and release profile of antibiotic drug moxifloxacin best followed Hixson-Crowell’s model.
Keywords
Carbopol; Drug delivery; 2-hydroxyethylmethacrylate; Hydrogel; Wound dressing
Introduction
Human skin wounds are the major threat to public health. Billions are being spent for wound management annually, due to increasing health care costs, aging population and a sharp rise in the incidence of diabetes and obesity worldwide [1]. Research in the field of wound management has led to a significant improvement in wound care technologies. The conventional wound dressing materials are not suitable for acute and chronic wounds as far as rapid healing of a wound is concerned. For this purpose functionalized wound dressings are developed. Recently, modern wound dressings containing active ingredients, such as antimicrobials and antibiotics, were used in wound dressing materials against contaminations and infections [2-4]. Out of a wide range of modern dressings, hydrogels have gained special attention because of their ability to maintain moist healing environment, soft nature and controlled drug delivery properties. Hydrogels, due to their unique biocompatibility, flexible methods of synthesis, range of constituents, and desirable physical characteristics, have been the material of choice for many biomedical applications [5]. In recent years, hydrogels have been used in various biomedical products [6]. Stimuli responsive [7] and pH responsive [8] hydrogels have been used in controlled drug delivery systems [9]. Keeping in view the suitability of hydrogels for wound dressings and drug delivery, in the present work an attempt has been made to synthesize carbopol and poly(2-hydroxyethylmethacrylate) [poly(HEMA] based hydrogel films for wound dressing applications. These hydrogel films have been loaded with an antibiotic drug moxifloxacin to study its drug delivery properties.
Carbopol is a highly hydrophilic crosslinked polyacrylic acid polymer. Carbopol hydrogels have been used as drug delivery systems due to high water affinity, environmental sensitivity, high permeability, fast swelling, high swelling ratio, enhanced absorption, low toxicity and good biocompatibility. As a vehicle for topical administration it maintains a moist environment within the wound site. Carbopol hydrogels loaded with bioactive agent have been reported to accelerate the healing process and improve the tissue quality of burn wounds [10]. Poly (HEMA) is a highly biocompatible polymer widely used for the production of materials for biomedical application [11]. Poly(HEMA) hydrogel possesses a high mechanical strength, relatively high water content in swollen state, resistance to significant chemical and microbial degradation [12] and good tolerance for entrapped cells [13,14]. Poly(HEMA) hydrogels can be designed to have optimal water or biological fluid content in an aqueous medium without dissolution, good mechanical properties, permeability to oxygen, biocompatibility, shape stability and softness similar to that of the soft surrounding tissue [13]. Because of its biocompatibility, poly(HEMA) can act as an ideal component for various biomedical and pharmaceutical applications [15] including wound dressings [16-18]. Moxifloxacin is a synthetic fluoroquinolone, with broad-spectrum antibiotic activity. It is a recent addition to the fluoroquinolone class, differing from ciprofloxacin and other older agents in having much better in vitro activity against Gram positive aerobes while retaining potent activity against Gramnegative aerobes [19]. Moxifloxacin has significant activity against Gram-positive aerobes, including potential dermatologic pathogens such as S. aureus [20].
Keeping in view the above facts of hydrogel wound dressings in consideration, in the present work an attempt has been made to prepare carbopol and poly(2-hydroxyethylmethacrylate) based hydrogel films. The polymers characterization was carried out by Scanning Electron Micrography (SEMs), Atomic Force Microscopy (AFM), Fourier Transform Infrared (FTIR) spectroscopy, 13C Nuclear Magnetic Resonance (NMR) spectroscopy, X-Ray Diffraction Study (XRD), thermal degradation studies [i.e., Thermo Gravimetric Analysis (TGA)/Differential Thermal Analysis (DTA)/ Differential Thermogravimetry (DTG)] and Differential Scanning Calorimetry (DSC) techniques. Besides, the effect of nature and temperature of swelling medium on swelling behaviour of hydrogel films was also studied. Drug release study was done in simulated wound fluid and drug release mechanism has been evaluated.
Experimental
Materials used
Carbopol 940 (Loba Chemie Pvt. Ltd., Mumbai-India), N,Nmethylenebisacrylamide (NN-MBA) (Acros organics, New Jersey- USA), ammonium persulphate (APS) (Qualigens Fine Chemicals, Mumbai-India), 2-hydroxyethylmethacrylate (HEMA), glycerol, (S.D. Fine Chemical Ltd., Mumbai, India) and moxifloxacin hydrochloride (Lifestar Pharma Pvt. Ltd., New Delhi, India) were used as received.
Synthesis of carbopol-cl-poly(HEMA) polymers
Synthesis of the polymers was carried out by chemically induced free radical polymerization method using APS as initiator and NN-MBA as cross-linker. Reaction was carried out with solution of carbopol [1.5% (w/v)], taken in beaker. After 12 h hydration, the reaction mixture was stirred at 100 rpm for definite time to get a homogenous mixture and, solutions of a definite concentration of [HEMA]=4.11 × 10−2 mol/L, [NN-MBA]=8.10 × 10−3 mol/L, glycerol=0.27 mol/L and [APS]=5.48 × 10−3 mol/L were added and the reaction mixture was again stirred, total stirring time being 12 h. The reaction mixture was then transferred to the petri dish which was placed in hot air oven maintained at 55°C to get the cross-linked polymer by solution casting method. The cross-linked polymer formed was washed with distilled water and ethanol to remove the soluble fractions left in the polymer. Then it was dried in an oven maintained at 40°C till constant weight was obtained. This cross-linked polymer was named as carbopol-cl-poly(HEMA) polymer.
Characterization
The polymers were characterized by Scanning Electron Micrography (SEMs), Atomic Force Microscopy (AFM), Fourier Transform Infrared (FTIR) spectroscopy, 13C Nuclear Magnetic Resonance (NMR) spectroscopy, X-Ray Diffraction Study (XRD), thermal degradation studies [i.e., Thermo Gravimetric Analysis (TGA)/ Differential Thermal Analysis (DTA)/Differential Thermogravimetry (DTG)] and Differential Scanning Calorimetry (DSC).
SEMs were taken on FEI Quanta 200F (The Netherlands). Scanning electron micrographs were obtained by scanning the surface of samples with a high energy beam of electrons (2−12 kV). A focused beam of high energy electrons was used to generate a variety of signals at the surface of solid specimens. These electrons interacted with atoms of the sample and produced the signal, which revealed the information about surface morphology of the sample. The SEM images of carbopol-cl-poly(HEMA) hydrogels were taken at high vacuum pressure. All SEM images were taken on carbon tape without using any staining or coating at different magnifications.
Surface morphology and roughness was studied by AFM (NTEGRA, NT-MDT, Russia) in semi-contact mode, using antimony doped, N-type, single crystal silicon probe, with resistivity (0.01-0.025 Ω.cm) at a scan frequency of 1 Hz. Imaging was done in 5 μm2 areas, with set point current 5.0 nA. The AFM images provided qualitative data (topographic images) as well as quantitative data (roughness). Images obtained were processed with using NOVA Px software to calculate roughness of sample surface.
FTIR of dried powdered polymer samples was recorded on Perkin Elmer-Spectrum RX-I (USA) FTIR spectrometer with the potassium bromide disks being prepared by compressing the polymeric powder.
The 13C NMR of polymer was carried out in solid state using JEOL RESONANCE ECX 400 solid state NMR spectrometer operating at a magnetic field of 9.3 T and at a frequency of 100 MHz for carbons.
Powder X-ray diffraction patterns were obtained using a Bruker D8 Advance diffractometer (USA), operating at 40 kV and 30 mA with Cu−Kα radiation (1.54 Å). The diffraction pattern was recorded by scanning 2 θ from 10° to 80° with a step size of 0.02°.
Thermal degradation (TGA/DTA/DTG) data of polymer was recorded using EXSTAR TG/DTA 6300 thermal analyzer (Japan), at a scan rate of 10°C/min under air atmosphere. Dried hydrogel samples were heated in an alumina crucible and the degradation profiles were recorded from 30 to 800°C.
DSC thermogram of polymer was recorded with NETZSCH DSC 204 (USA) in temperature range 25 to 500°C at a scan rate of 10°C/min.
Swelling studies
Swelling studies of the polymers were carried out in different mediums by gravimetric method [21]. Known weight of polymers were taken and immersed in excess of solvent for different time intervals. The polymers were removed, wiped with tissue paper to get rid of excess of solvent and weighed immediately. The swelling (gram per gram of gel) of the polymer was calculated by the formula given in equation 1:

where Ws is weights of swollen polymers and Wd is the weight of dried polymers. Swelling studies of hydrogels were carried out in triplicate.
Drug release studies
In vitro release profile of model drug (moxifloxacin) from drug loaded polymers was determined in simulated wound fluid to determine the drug release mechanism and kinetic models for the release of drug from drug loaded polymer matrix. All the drug release studies were carried out in triplicate. The loading of drug into the hydrogels was carried out by the swelling equilibrium method [21]. The hydrogels were allowed to swell in drug solution of known concentration for 24 h at 37°C and then were dried to obtain the drug loaded polymers. In vitro drug release studies were carried out by placing dried drug loaded polymer samples in definite volume (20 mL) of releasing medium for definite time at 37°C and then sample was transferred to the fresh releasing medium. The process was repeated up to 6 h and finally the polymers were removed after 24 h. The absorbance of the solution of drug was measured on the UV visible spectrophotometer (Cary 100 Bio, Varian) at 288 nm and concentrations were read from calibration curves. The Swelling and drug release mechanism of polymers were determined by the power law expression reported by Stenekes et al. and Mair et al. [22,23]:

Where Mt/M∞ is the fractional swelling or release of drug in time t, ‘k’ is the constant characteristic of the drug-polymer system, and ‘n’ is the diffusion exponent characteristic of the release mechanism. To find out the best fit model for drug release from hydrogels, the data were treated in different in vitro release kinetics models, i.e., zero order, first order, Higuchi square root law, Korsmeyer-Peppas and Hixson-Crowell cube root model [24,25].
Results and Discussion
Scanning electron microscopy
SEM images of carbopol-cl-poly(HEMA) polymer film at different magnifications (x100, x1000, x5000 and x10000) have been presented in Figure 1. It was observed form the images that the polymer film has homogenous and smooth surface, indicating that the components of the crosslinked polymer films were miscible. Hu et al. [26] have also observed similar results for poly(N,N-dimethylacrylamide-co-2-hydroxyethylmethacrylate) hydrogels.

Figure 1: SEM images of carbopol-cl-poly(HEMA) polymer film at different magnifications.
Atomic force microscopy
AFM image of carbopol-cl-poly(HEMA) polymer film has been presented in Figure 2. Results showed that the average surface roughness was 0.570 nm and root mean square roughness was 0.949 nm. The three dimensional image shows the presence of very few valleys on the scanned area, indicating homogeneity in the polymeric sample. AFM has been implemented as a surface characterization technique in biomaterial research. It has been proved to be very helpful for the determination and verification of morphological features. AFM particularly permits non-destructive imaging of surfaces on a molecular scale [27]. Kim et al. [28] studied surface topography of the polyHEMA and polyHEMA-methacrylic acid based contact lenses by using AFM technique. The root mean square roughness over an area of 10 × 10 mm2 was 19.73 nm for the polyHEMA lens and 23.75 nm for the polyHEMA-methacrylic acid lens. Extremely low surface roughness in present case can be attributed to high hydrophilicity of carbopol and formation of more homogenous surface, which has also been observed during SEM study. A more hydrophilic surface and high water content in the hydrogel leads to less surface roughness [29,30].
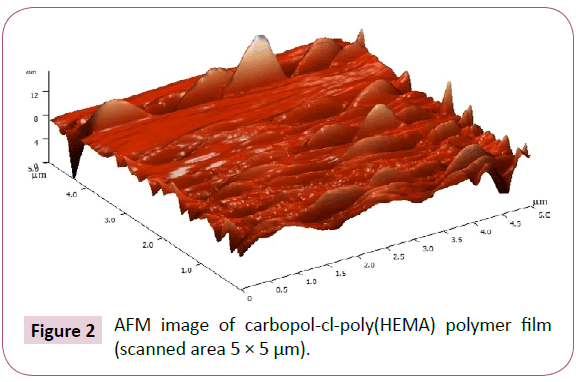
Figure 2: AFM image of carbopol-cl-poly(HEMA) polymer film (scanned area 5× 5 µm).
Fourier transform infrared spectroscopy
FTIR spectrum of carbopol-cl-poly(HEMA) polymer is presented in Figure 3. A broad band at 3422.2 cm-1 (due to -O-H stretching), a band at 2932.8 cm-1 (due to –C-H stretching), a sharp intense band at 1724.2 cm-1 (due to asymmetric –COO? stretching of carbopol and C=O stretching of polyHEMA), at 1544.0 cm-1 (due to symmetric –COO? stretching of carbopol), at 1454.8 cm-1 (due to –C-H bending), at 1399.0 cm-1 (due to O-H in plane bending of polyHEMA). Beside, absorption band at 1164.3 cm-1 (due to C-O-C stretching in carbopol), and at 1069.9 cm-1 (due to C-O-C stretching in polyHEMA), at 907.9 cm-1 (due to –O-H out of plane deformation of carbopol –COOH), at 798.7 cm-1[due to –C-H out of plane deformation of carbopol –CH(COOH)-]. It may be noted that carbonyl group stretching band (1724.2 cm-1) was broad and intense. It extended from ~1750 to ~1600 cm-1 because carbonyl group in carbopol and polyHEMA are present as acid (non-ionised and ionised) and ester, which result in shifting of vibrational frequency [31-33]. The FTIR spectrum indicates that modification in carbopol with poly(HEMA) has occurred.
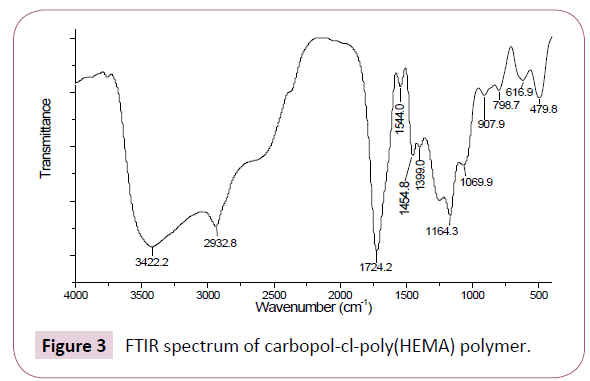
Figure 3: FTIR spectrum of carbopol-cl-poly(HEMA) polymer.
13C nuclear magnetic resonance spectroscopy
13C NMR spectrum of carbopol-cl-poly(HEMA) polymer is presented in Figure 4. In this case a peak at 178.8 ppm [due to carbonyl carbons of poly(HEMA) and, carbopol], at 67.7 and 64.0 ppm [due to -O-CH2-CH2-OH of poly(HEMA)], at 60.8 ppm [due to -CH2-OH of poly(HEMA)], at 45.5, 41.8 ppm [due to methylene and methine groups of acrylic chains of carbopol and polyHEMA], and at 17.1 ppm [due to -C-CH3 of polyHEMA] has been observed [31,34,35]. Besides a peak at 73.4 ppm has also been observed which can be attributed to formation of some new linkage during the crosslinking process. It may be noted that generally 13C NMR spectrum of carbopol shows only three peaks (i.e., due to carbonyl, methylene and methine groups) [31], but the presence of addition peaks in this case indicated that poly(HEMA) has been successfully grafted onto the backbone of carbopol.
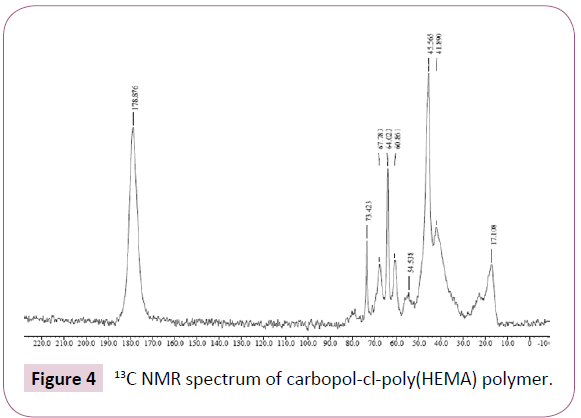
Figure 4: 13C NMR spectrum of carbopol-cl-poly(HEMA) polymer.
X-ray diffraction study
X-ray diffractogram of carbopol-cl-poly(HEMA) polymer is presented in Figure 5. It showed that there was no crystalline region in crosslinked polymer sample. The appearance of broad peaks and small edges are due to the lack of long-range crystallographic order of finite size. Process of cross-linking and grafting may have hindered formation of any regular pattern in polymeric samples. The amorphous character of the crosslinked polymer may be due to the occurrence of the grafting process in a haphazard manner along the carbopol backbone. It has been reported that pure carbopol itself does not possess any crystalline region and is completely amorphous in nature [36].
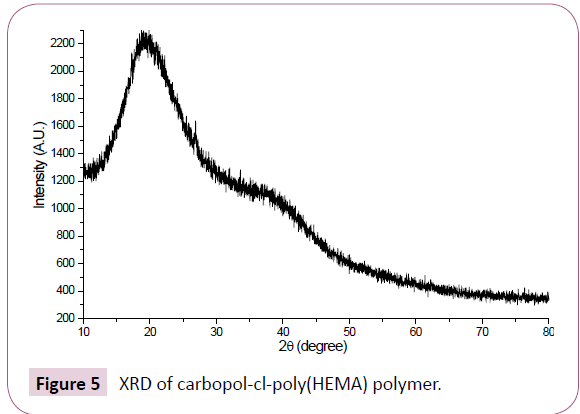
Figure 5:XRD of carbopol-cl-poly(HEMA) polymer.
Thermal degradation studies
TGA, DTA and DTG curves of carbopol-cl-poly(HEMA) polymer are presented in Figure 6. Ignoring the initial weight loss due to entrapped moisture, initial decomposition temperature (IDT) has been taken as the temperature where actual degradation of material started. Initial 3.5% weight loss occurred upto 100°C, which indicates that crosslinked polymer has 3.5% bounded water. Ignoring the initial weight loss due to free and bounded water, three stage decomposition has been observed. The first degradation stage started at 182.87°C (residue left=92.5%), second stage started at 315.46°C (residue left=81.3%) and third stage started at 450.09°C (residue left=8.9%). IDT and FDT have been observed 182.87°C and 505.76°C (residue left=0.06%) respectively. First minor degradation stage after 182.87°C can be attributed to the formation of formation of cyclic structures (anhydrides) associated with loss of water loss of water. Second major degradation stage after 315.46°C onwards occurred at a very high rate, due to decarboxylation, formation of unsaturated structures, and depolymerisation of the residual polymer. Third degradation stage can be attributed to complete degradation of polymer forming gaseous products. Maximum degradation rate 1530 μg/min (416°C) in second stage was observed. DTA curve showed an endothermic peak around 100°C due to the vaporization heat of free water present in the polymer. 3.5% weight loss due to adsorbed water has been observed in TGA curve. Further major exothermic peak at 370°C can be due to decarboxylation of acidic groups and dehydration of hydroxylate in the aliphatic structures. Another exothermic peak at 429°C can be attributed to formation of unsaturated structures, and depolymerisation of the residual polymer. Exothermic peak at 494°C in this case can be attributed to complete degradation of polymer accompanied by combustion of the degraded material. In the presence of oxygen, the oxidation of volatile products and combustion of degraded material take place in the range between 350 and 500°C, depending on the nature of the material. DTG analysis was studied as a function of rate of weight loss (μg/min) with increase in temperature. In this case three stage degradation has been observed, where first stage is associated with very slow degradation rate with a peak at 212°C (120 μg/min), second stage degradation showed two DTG peak at 362°C (660 μg/min) and at 416°C (1530 μg/min), and third stage degradation showed DTG peak at 493°C (242 μg/min) [37,38].
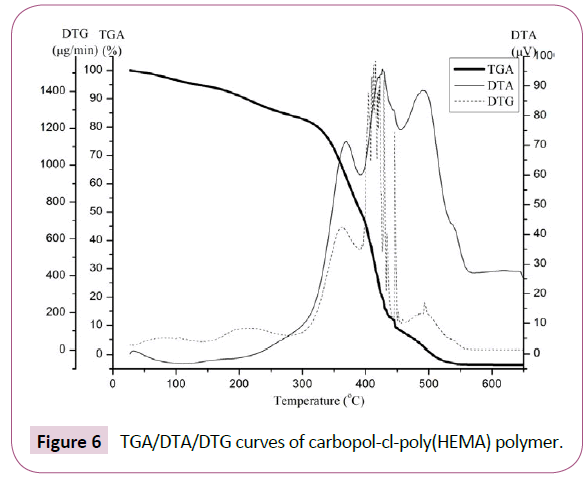
Figure 6:TGA/DTA/DTG curves of carbopol-cl-poly(HEMA) polymer.
Differential scanning calorimetry
DSC curve of carbopol-cl-poly(HEMA) polymer is presented in Figure 7. In this case two endothermic peaks, at 67.8 and 206.5°C, were observed, with a heat of fusion 111.7 and 77.66 J/g, respectively. The initial endotherm can be due to the evaporation of unbound water in the polymer and the latter can be attributed to the loss of water due to formation of anhydrides in carbopol [39]. No glass transition temperature (Tg) for crosslinked polymer has been observed. Gómez-Carracedo et al. have reported that various grades of carbopols show Tg in the range 130-140°C [40]. Loss of Tg in DSC thermogram of crosslinked polymer indicate the modification of carbopol with poly (HEMA). Contribution of different pendant short chains in polymeric network and the interactions between different side chains influences the flexibility of polymer network and consequently the thermal behaviour of the crosslinked polymer. These evidences suggest that grafting of poly(HEMA) onto carbopol led to formation of a crosslinked polymer with homogenous surface.
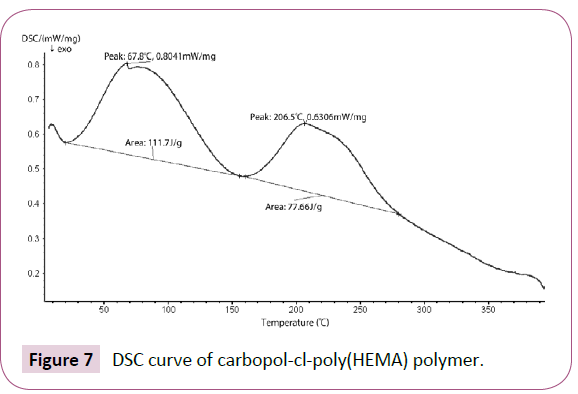
Figure 7: DSC curve of carbopol-cl-poly(HEMA) polymer.
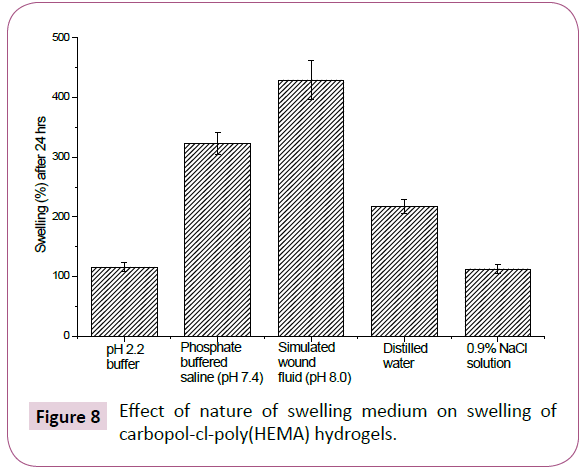
Figure 8: Effect of nature of swelling medium on swelling of carbopol-cl-poly(HEMA) hydrogels.
Swelling studies
Swelling studies of the polymers were carried out in different mediums by gravimetric method. Swelling of hydrogels was studies as a function of nature of swelling medium and temperature of swelling medium. The results are presented in Figures 8 and 9. The swelling of carbopol-cl-poly(HEMA) hydrogels was carried out in pH 2.2 buffer, phosphate buffered saline (pH=7.4) and simulated wound fluid (pH=8). It was found that swelling of hydrogels increased with increase in pH of swelling medium. Maximum swelling was observed in simulated wound fluid (429.23 ± 33.23%) followed by PBS and minimum swelling in pH 2.2 buffer was observed. Since polyHEMA is a non-ionic polymer [11], pH sensitivity of the hydrogel can be attributed to the presence of carbopol. Carboxylic groups present in the hydrogel matrix (due to carbopol) remain unionized in acidic pH (2.2), so the main anion-anion repulsive forces are eliminated. A functional moiety is ionised when pH is more than pKa. The pKa value of carbopol has been reported to be in the range of 4.9-6.7 [41]. For this reason, at pH 2.2 there are almost no negatively charged groups present. The low swelling at this pH may also be attributed to the hydrogen bonding interaction among the -COOH groups in the gel forming additional physical network. At low pH the swelling is caused by the electrostatic interaction of water with -OH and -COOH groups of the hydrogel.
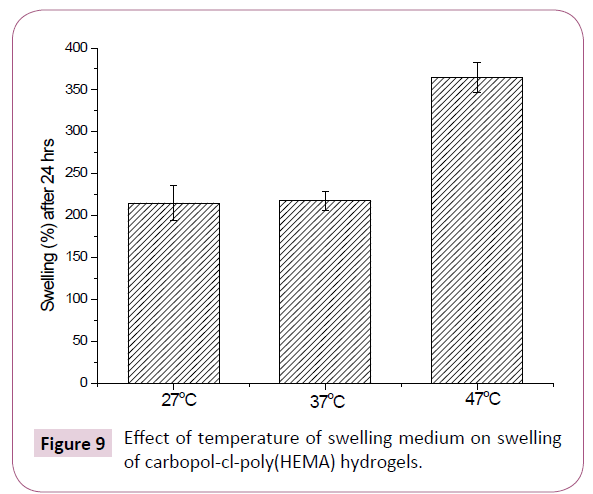
Figure 9:Effect of temperature of swelling medium on swelling of carbopol-cl-poly(HEMA) hydrogels.
At high pH (7.4 and 8.0) the carboxylic groups are converted to carboxylate anions with an expansion of the gel network due to electrostatic repulsion resulting in increased swelling. The ionization of carboxylic groups under basic conditions increases the hydrophilicity of the molecular chains also leads to the generation of negative charge repulsion among them, and hence, hydrogels show more swelling. Similar results have been reported in literature [42]. It is pertinent to mention here that many wound dressings have the disadvantage of poor absorbency and im-permeability for wound exudates which accumulates under the dressing and causes skin maceration, bacterial proliferation and the risk of infection The hydrogel synthesized in current study showed (429.23 ± 33.23%) swelling in simulated wound fluid, which indicates that these dressing could absorb and retain a high volume of fluid.
The swelling of carbopol-cl-poly(HEMA) hydrogels was carried out in 0.9% NaCl and compared with swelling in distilled water to evaluate the effect of salt concentration on swelling of hydrogels. The results of swelling are presented in Figure 8. It is observed form the results that swelling of hydrogels decreased with increase in salt concentration of swelling medium, signifying the sensitivity of the hydrogels towards ionic strength of swelling medium. Since polyHEMA is a non-ionic polymer, this sensitivity of the hydrogel can be attributed to the presence of carbopol which contain ionisable moieties. In fact, swelling of the hydrogels is caused by the repulsion of the like charges of the hydrogels (i.e., COO−) which expands the gel network with an easy penetration of the water molecules. In the presence of the salt solution the metal ions of the salts shield the ionic charges of the gels which reduce the repulsive forces among the like charges of the hydrogels. Hence, the expansion of the gels also decreases. Thus, swelling decreases in the presence of a salt [42]. Another reason for less swelling in 0.9% NaCl is that, the increasing salt concentration decreased the osmotic pressure difference between gel network and external solution, which prevented water molecules to penetrate into the hydrogels. Osmotic pressure is a result of the difference in the mobile ion concentration between gel and the aqueous phase. This difference is decreased in salt solution and consequently the absorbency is also diminished. The swelling ability of anionic hydrogels in salt solutions decreases appreciably compared to the swelling values in distilled water [26,43].
The swelling of carbopol-cl-poly(HEMA) hydrogels was also carried out in distilled water at three different temperatures (27°C, 37°C and 47°C) to evaluate the effect of temperature of swelling medium on swelling of hydrogels. The results of are presented in Figure 9. It is observed from the results that swelling of hydrogels increased with increase in temperature of swelling medium. Increase in swelling can be attributed to increase in kinetic energy of solvent molecules which caused faster diffusion of water in the polymeric network. In addition, with increase in temperature entanglement and intermolecular forces between polymeric chains is decreased, which leads to more exposure of hydrophilic moieties for water and subsequently swelling is increased.
Drug release
Release profile of moxifloxacin from drug loaded carbopol-clpoly( HEMA) hydrogels was evaluated in pH simulated wound fluid (pH=8.0) and results are shown in Figure 10 and Table 1. Drug release occurred without any burst effect, suggesting that the major part of the drug was incorporated within cross-linked polymer. Moreover, the electrostatic interactions between drug and polymer, although weak, may account for slowing the release of the drug.
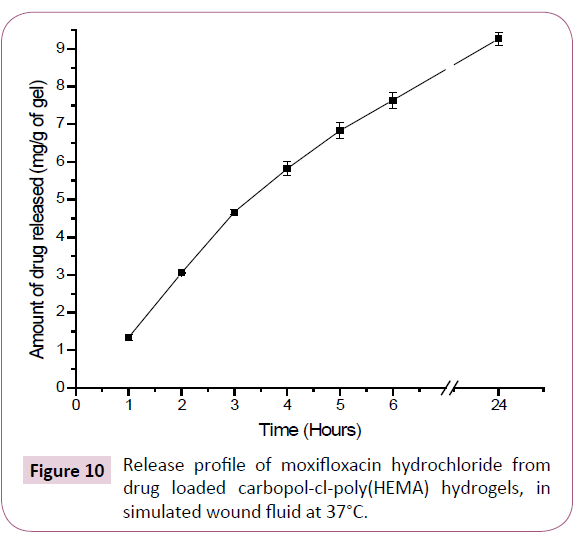
Figure 10:Release profile of moxifloxacin hydrochloride from drug loaded carbopol-cl-poly(HEMA) hydrogels, in simulated wound fluid at 37°C.
Diffusion exponent and various diffusion coefficients for the release of drug from the drug loaded polymers have been calculated and results have been presented in Table 1. The release of moxifloxacin from hydrogels occurred through non-Fickian diffusion mechanism. Non-Fickian or anomalous diffusion occurs when the rates of diffusion and polymer chain relaxation are comparable [44]. Jana et al. [45] have found that release of aceclofenac from drug loaded carbopol gels occurred through non-Fickian diffusion mechanism. The values of initial diffusion coefficients were slightly higher than late time diffusion coefficients for moxifloxacin release. The in vitro drug release data from carbopol-cl-poly(HEMA) hydrogels was evaluated kinetically using various important mathematical models like zero order, first order, Higuchi, Korsmeyer–Peppas and Hixson-Crowell models (Table 1). When the respective R2 were compared, it was found that drug release from the hydrogels has obeyed all the kinetic models and followed best by Hixson-Crowell model with highest values of regression coefficient. In case of Hixson- Crowell model the drug is dissolved from a material, where the dissolution occurs in planes that are parallel to the drug surface if the diminish proportionally, in such a manner that the initial geometrical form keeps constant all the time [46]. The results of drug release reveal that carbopol-cl-poly(HEMA) hydrogel films could also serve as a reservoir for bioactive and antimicrobial agents which could be sustainably released at the wound site for accelerated infection free wound healing. Overall, it was observed form the results that carbopol-cl-poly(HEMA) hydrogels can act as drug encapsulating and drug releasing device, in addition to their ability to absorb simulated wound fluid. Characterization of the polymer by various techniques showed that modification of the carbopol backbone with poly(HEMA) has occurred.
| Model | Value | |
|---|---|---|
| Diffusion exponent ‘n’ | 0.975 | |
| Gel characteristic constant ‘k102 | 0.288 | |
| Correlation coefficient (R2) | 0.993 | |
| Diffusion coefficients (cm2/min): | Initial Di`106 | 7.422 |
| Average DA´106 | 2.479 | |
| Late Time DL´106 | 5.315 | |
| Zero Order Model: | R2 | 0.989 |
| k0 × 102 (min-1) | 0.226 | |
| First Order Model: | R2 | 0.996 |
| k1×102 (min-1) | 0.524 | |
| Higuchian Model: | R2 | 0.998 |
| kH × 102 (min-1/2) | 6.15 | |
| Korsmeyer-Peppas Model: | R2 | 0.993 |
| kKP × 102 (min-n) | 0.288 | |
| Hixson Crowell’s Model: | R2 | 0.999 |
| kHC × 102 (min-1/3) | 0.13 | |
Table 1 Results of diffusion exponent ‘n’, gel characteristic constant ‘k’, various diffusion coefficients, and correlation coefficients of different models for release profile of moxifloxacin hydrochloride from drug loaded carbopol-cl-poly(HEMA) hydrogels, in simulated wound fluid at 37ºC.
Conclusion
It is concluded from the forgone discussion that nature of swelling medium has influenced the swelling of the hydrogel films. These polymer films showed smooth, homogenous surface which is confirmed by SEM and AFM techniques. Grafting of poly(HEMA) onto carbopol backbone has been confirmed by FTIR and 13CNMR studies. Moxifloxacin release from the drug loaded hydrogels occurred through non-Fickian diffusion mechanism and best followed Hixson-Crowell model with highest values of regression coefficient. Beside simulated wound absorption capacity of carbopol-cl-poly(HEMA) hydrogel films make them more suitable for use as wound dressing. Slow drug release properties associated with wound fluid absorption make these polymeric films a suitable material to be considered as future wound dressing.
Acknowledgement
One of the author wishes to thank University Grant commission, New Delhi, India for providing financial assistance in the work. (Letter No. F.17-40/08(SA-I), dated 27 April, 2012).