Research Article - (2017) Volume 25, Issue 3
Mesfin Beharu*
School of Nursing, Institute of Health, Faculty of Health Sciences, Jimma University, Ethiopia
Israel Bekele
School of Nursing, Institute of Health, Faculty of Health Sciences, Jimma University, Ethiopia
Zewdie Birhanu
Department of Health Education and Behavioral Science, Institute of Health, Faculty of Health Sciences, Jimma University, Ethiopia
Ibrahim Yimam
School of Nursing, Institute of Health, Faculty of Health Sciences, Jimma University, Ethiopia
Corresponding Author:
Israel Bekele
Jimma University Institute of Health
Faculty of Health Sciences, School of Nursing and Midwifery
Jimma, Oromia 378, Ethiopia
Tel: 251915419518
E-mail: israel.bekele90@gmail.com
Submitted date: : March 28, 2017; Accepted date: May 25, 2017; Published date: June 01, 2017
Background: Globally the increasing diversity in the population has led to concerns over disparities in health status between diverse patient populations. Language and cultural issues can have a significant impact on health disparities when not addressed by health care organizations. Even though disparity in health care increase very few studies have provided the opportunity for researchers to explore the issue of culturally and linguistically appropriate health care in a broad and organized fashion throughout the worldwide and none of them done across the country.
Objective: To explore cultural sensitiveness in health care delivery of Jimma university specialized and teaching hospital.
Methods: Institution based qualitative study was employed in JUSTH among 10 key informants (administrative and health workers) purposively selected from different service areas and 10 patients selected through purposive random sampling from different backgrounds. Data were collected using unstructured questionnaire through In-depth interview and analyzed by using ATLAS.ti7.1. Open Coding was carried out line-byline. Following the coding process, family coding, themes and theoretical constructs were developed from both the field notes and the interview transcripts.
Results: One of the most prominent challenges identified by this study is the image of cultural and linguistic sensitive diverse patients need care does not come to hospital plan image, which often results in a lack of financial and other resources for culture and language service. Developing supportive infrastructure, work force, data collecting and using, community engagement, organizational relationship, integrating cultural need into organizational planning, accommodating the specific need of patients and helping patients to manage their care are the major activities expected from the hospital as the study participants to deliver cultural sensitive/appropriate care for diverse patient populations.
Conclusion: Without cultural appropriate health care services it is difficult for the hospital to deliver patient centered non disparity quality health service. For health care organizations to deliver patient centered non-disparity health service there must be conceptual framework guide the health care organization to develop a cohesive message about meeting the needs of diverse patient populations and better communicate this vision to staff, clients and the public. Thus framework must develop based on the culture of the clients/community served at the health care organization and medical indication of the patient cases.
Cultural sensitiveness; Health care delivery
Universal Health Care (UHC) ensures equality in coverage and access to health services for all people. However, social policy at the national level cannot be successful without recognizing within household and within country inequalities based on discrimination due to gender, race, ethnicity, age, disability, religion, sexual orientation, refugee status or other status [1,2].
Integrated health services encompasses the management and delivery of quality and safe health services so that people receive a continuum of health promotion, disease prevention, diagnosis, treatment, disease-management, rehabilitation and palliative care services, through the different levels and sites of care within the health system and according to their needs throughout the life course [3].
The cause of health disparities is certainly multi-factorial. It is related to the interplay between individual/personal factors, socioeconomic, neighborhood/environmental, institutional and other social determinants of health that occur in certain sub populations [3,4].
Globally the increasing diversity in the population has led to concerns over disparities in health status between ethnic/racial minorities and the ethnic/racial majority [5,6]. Language and cultural issues can have a significant impact on health disparities when not addressed by health care organizations [7]. As the diversity of nation continues to grow, hospitals are encountering more patients with cultural and language barriers [8,9].
For decades, the prevalence of racial and ethnic disparities in health care delivery and outcomes in the United States ha s been increasingly recognized. Culturally and linguistically diverse groups and individuals of limited English proficiency typically experience less adequate access to care, lower quality of care and poorer health status and outcomes due to low cultural and linguistic sensitive care [9-11].
The health care environment of today presents many challenges for health care organizations, individual practitioners, patients and families. That includes legal, regulatory and accreditation standards, improve health care outcomes and safety among their patients and respect bottom lines [12,13].
A framework of cultural competence interventions - including minority recruitment into the health professions, development of interpreter services and language-appropriate health educational materials and provider education on crosscultural issues emerged to categorize strategies to address racial/ ethnic disparities in health and health care [14,15].
Due to the sensitive nature of certain practices, patients may be reticent to readily discuss certain issues, but as trust is built and continuity of care occurs over time, there may be opportunities for more sensitive discussion and disclosure [16,17].
Similarly, cultural competency has been proposed as a way for health care organizations to reduce disparities in care. Study done in California found that practice sites with highest cultural competence reported better asthma outcomes for Medicaid recipients [18,19].
Health care professionals do not consider it to be their responsibility to adapt to ethnic diversity, If health professionals do not feel a responsibility to adapt, they are less likely to be involved in culturally sensitive health care. Yet patient attitudes about health, religious views and concepts of death often influence compliance, affect disease management and alter health outcomes. Views of race and power also influence the nature of the communication between clinician and patient [20- 23].
Communication related medical errors occur through mistakes in medical history taking, patients’ lower adherence to treatment because of inability to understand and follow instructions and over-treatment of patients. In the acute care setting, communication failures lead to increases in patient harm, length of stay and resource use, as well as more intense caregiver dissatisfaction and more rapid turnover [24].
Refugees from urban centers in Ethiopia have experience with Western-style medicine, but rural people have trouble understanding the concept of disease and the causes, means of transmission and methods of prevention. Because Ethiopians are accustomed to receiving antibiotics or other medications for every illness, they feel it is a waste of time to go to a doctor if no medication is given, even for a minor illness. This is a common point of dissatisfaction with health care in Seattle [25].
For the past decade, the CDC’s Racial and Ethnic Approaches to Community Health (REACH) program has empowered residents to seek better health, helped change local healthcare practices, ensuring cultural competence/sensitivity among health care providers, improving health literacy among patients and give culturally and linguistically appropriate care and mobilized communities to implement evidence-based public health programs to reduce health disparities across a broad range of health conditions [8,22].
Appropriate communication and understanding between patient and provider are essential to safe, quality healthcare [8,10,20]. Very few studies have provided the opportunity for researchers to explore the issue of culturally and linguistically appropriate health care in a broad and organized fashion throughout the worldwide and none of them done across the country therefore Policymakers and Researchers can use finding of this study to expand their understanding of current practice and inform future policy development and additional inquiry. The finding provides a unique insight into the challenges, activities and client’s perception of hospital in providing culturally and linguistically appropriate care.
The Aim of this study is to explore cultural sensitiveness in health care delivery of Jimma university specialized and teaching hospital Jimma town, south west Ethiopia 2016.
Study setting/area
The study was conducted at Jimma University specialized and teaching Hospital (JUSTH). JUSTH is one of the oldest public hospitals in Ethiopia. Geographically, it is located in Jimma city 352 km southwest of Addis Ababa. Currently it is the only teaching and referral hospital in the southwestern part of the country, providing services for approximately 15,000 inpatient, 160,000 outpatient attendants, 11,000 emergency cases and 4500 deliveries in a year coming to the hospital from the catchment population of about 15 million people for Oromia, SNNP and Gambela region. The hospital provided more than 19 clinical services With work force of more than 552 nurses (including midwifes), more than 145 residents, more than 21 General medical practitioner, 89 specialized doctors, more than 53 Pharmacist, more than 48 Laboratory technologists, 50 administrative workers and more than 587 supportive staffs.
Study design/approach
Abbreviated version of grounded theory study design was employed in JUSTH from March 10-30, 2016 G.C. The abbreviated version of grounded theory that involves the coding of data only was used. The abbreviated version of grounded theory works with the original data only. The interview transcripts are analyzed following the principles of grounded theory (i.e., the processes of coding and constant comparative analysis); however, theoretical sensitivity, theoretical saturation and negative case analysis can only be implemented within the texts that are being analyzed. The researcher does not have the opportunity to leave the confines of the original data set to broaden and refine the analysis. The abbreviated version of grounded theory should be used due to time or resource constraints prevent the implementation of the full version of grounded theory.
Study participants
Ten key informants on different service position related to organizational cultural and linguistic sensitiveness in delivering health services and Health workers with rich experience in different service delivery points of patient care and related services; and administrative activities were selected. Ten patients from different backgrounds including ethnicity, language, literacy, residence, sex, age and from different service area were interviewed to maximize variations. However, psychiatric patient and critically ill patient were not included in the study. Interview questionnaire consisted of a combination of key interviews parts and patient’s interviews parts. A total of 20 participants were included in this study which was appropriate sample size as rules of thumb estimate the sample size for grounded theory approach. Data were collected within three weeks.
Study participant’s selection procedures
Purposive sampling was used to select key informants from JUSTH staff members to get detail information on how organization sensitive to culture and language of its patients in providing culturally and linguistically appropriate care. All key informants were selected based on their current position related role to answer the research questions. Purposeful Random Sampling was used to select Patients from different backgrounds including ethnicity, language, literacy, residence, sex, age and from different service are. Admitted patient or out-patient those visit at least OPD, Pharmacy and Laboratory services were include in the study.
Phenomenon
The study is aimed to explore.
Culturally sensitivity healthcare: Services those are respectful of and responsive to the health beliefs and practices and cultural and linguistic needs of diverse patient populations. It has been proposed as a way for health care organizations to reduce disparities in care.
Culture: Refers primarily to characteristics of human behavior associated with race, ethnicity, dressing, diet, language and religion
Translation: Refers to the conversion of written communication from one language to another.
Interpreter/interpretation/interpreting: An interpreter is a person who renders a message spoken in one language into one or more languages. The practice of interpreting is distinguished in this report from translating to include only spoken language.
Patient safety and provision of care: Issues of patient safety permeate all areas of care provision, recognizing the importance of both language and culture in providing safe care to diverse patients. Hospitals should formalize their processes for translating patient education materials, including patient rights and informed consent documents, into languages other than English and evaluating the quality of these translations. Hospitals should take advantage of the internal and external resources available to educate them on cultural beliefs they may encounter.
Quality improvement: In the absence of information systems that facilitate linkages between important components of patient level data (e.g. demographics and outcomes), hospitals will be challenged to identify, monitor and address inequities of care that may exist between their patient populations. Failing to do so may have negative long-term consequences for both diverse patient populations and the hospitals trying to care for them. The importance of documenting specific data about a patient’s race, ethnicity, language, culture and learning needs has been established by numerous studies as a starting point for hospitals to provide culturally and linguistically appropriate care. Accurate patient-specific data are essential to understanding the proportion of patients with a specific need in a given hospitals.
Language services: While language and culture are known to impact the safety and quality of care, conversations about patient safety initiatives seldom address these issues. It should involve consideration of community data, aggregate patient demographic data and other data that demonstrate the need for interpreter services. Aside from the legal and regulatory requirements for the provision of language services, hospitals have a more compelling need to communicate effectively with patients in order to provide care safely.
Leadership awareness and commitment: A hospital’s leaders provide the framework for planning, directing, coordinating, providing and improving care, treatment and services to respond to community and patient needs and improve health care outcomes Leaders create an organizational culture and can serve as models of culturally competent behavior. One way that some hospitals have demonstrated a commitment to meet the needs of diverse patients is to designate an individual responsible for managing cultural and linguistic programs.
Human resource policies and programs: One approach to ensuring that hospital staff possesses a minimum level of cultural and/or linguistic competence is developing written human resource policies that establish requirements for staff member’s cultural and/or linguistic competency.
Work forces: Hospital’s efforts to provide culturally and linguistically appropriate care by diversifying the demographics and skills of their workforce. Key components of this domain include staff recruitment and retention, demographics, development and training, competence and skills and employee perceptions. Developing a diverse workforce that reflects the community and patient population is one strategy recommended to foster the provision of culturally and linguistically appropriate care.
Successes and needs: A clear understanding of a patient’s cultural context is indispensable to a provider when attempting to practice culturally and linguistically appropriate care. This includes understanding a patient’s health beliefs and values and any needs that stem from those beliefs including spiritual beliefs, folk remedies, traditions or rituals, complementary and alternative medicines, level of health literacy, socioeconomic status and epidemiologic implications for treatment.
Communication throughout the organization: Establishing collaborative relationships with community entities can provide hospitals with detailed information on issues such as community member’s health-seeking practices and resources like ethno-medical healers, which can help hospitals tailor interventions to the communities they serve.
Community engagement: Hospitals should consider partnering with local ethnic media to promote better understanding of available hospital services and appropriate routes for accessing care among all community members. Hospitals should make use of the community resources available through community networks, collaborations and partnerships, including the involvement of community members from diverse cultures and language groups on formal boards and in hospital planning processes.
Assessing and meeting patient needs: From diagnoses to treatment plans, the patient care process hinges on the identification and understanding of patient needs. Similarly, the provision of culturally and linguistically appropriate care depends on an accurate assessment of a patient’s cultural and linguistic needs. A strategic approach that integrates an understanding of community needs with community collaboration can improve a hospital’s provision of culturally and linguistically appropriate care, thereby increasing quality for diverse populations and potentially reducing healthcare disparities.
Data Collection procedures
Un-structured guide was used to collect data from the participants. The abbreviated version of grounded theory that involves the coding of data only was used. The abbreviated version of grounded theory works with the original data only. The interview transcripts or note taken are analyzed following the principles of grounded theory (i.e., the processes of coding and constant comparative analysis); however, theoretical sensitivity, theoretical saturation and negative case analysis can only be implemented within the texts that are being analyzed. The researcher does not have the opportunity to leave the confines of the original data set to broaden and refine the analysis. The abbreviated version of grounded theory should be used due to time or resource constraints prevent the implementation of the full version of grounded theory.
Face to face In-depth interviews (IDIs) were conducted to collect data. IDIs are an appropriate method to understand these issues because they enable narratives of individuals to be elicited (participated), such that the interviewer can explore what was meaningful to the organization that was be expected to providing culturally and linguistically appropriate care. All interviews were recorded with participant’s permission and then transcribed word-by-word into plain text, then translated into English.
Data collection tool/instruments: Un-structured Interview guides developed prior to literature review were used to collect information from participants of the study. Audio recorder was used to record the interviews. The interview were translated to local language Afan Oromo and Amharic and translated back to English for analysis.
Data collectors: Two research assistants (degree in health education and behavioral science) those have previous experience in collecting qualitative data were used to collect data. Training was given to research assistants prior to IDIs period. Researcher and research assistants were conducted the interviews.
Data analysis and management: Once interviews were finished, the data were transcribed word-by-word into plain text, translated into English (as needed) and were imported directly into ATLAS.ti7.1 (is a powerful workbench for the qualitative analysis of large bodies of textual, graphical, audio and video data) for coding at the end of each day or the next day. Coding was carried out line-by-line. Later stages of analysis were integrating a lot of these into higher-level analytic categories. Since, the abbreviated version of grounded theory was used; here, the depth of analysis generated by line-by-line coding is needed to compensate for the loss of breadth that accompanies the researcher’s dependence on the original data set. All paper field notes, audio files, contact summary form, consent forms and any other notes were kept securely. On-going analyses were characterized by frequently going back to the original transcripts to ensure text is coded within context.
Trustworthiness
The researcher has adopted the research methods, purposive random sampling of individuals to serve as informants, member checking, triangulation by the use of a wide range of informants. Ensure honesty in informants when contributing data each person who is approached was given opportunity to refuse to participate in the project so as to ensure that the data collection sessions involve only those who are genuinely willing to take part and prepared to offer data freely. Iterative questioning to uncover deliberate lies, frequent debriefing sessions, peer scrutiny/ examination of the research project by colleagues, peers and academics should be welcomed, feedback at any presentations (more defense) and examination of previous research findings to assess the degree to which the project’s results are congruent with those of past studies to ensure credibility, transferability, dependability and conformability/objectivity of the data.
For this study, the transcription method reflected the interpretative approach underpinning the qualitative research, striving to convey as fully as possible the experiences and representations of the participants. This was includes wordfor- word transcription and recording all emotions. Major interruptions by other people or telephones were recorded to contextualize any breaks in speech or repetitions. However, minor interruptions were not recorded in order to ensure the flow of the transcript supports interpretation and analysis. The transcriptions were proof-read against the audio file by both the supervisors and the researcher to check for accuracy, identify any missed or misheard words and to clarify any areas of confusion or unclear terminology. All key informant participants were asked to revise and confirm their own transcripts after the interview to ensure data accuracy, member checking were done for patient interview; and, the transcript content was compared with the reviewed literature in an effort to determine whether any of the themes required further description and interpretation.
Ethical considerations
This study was approved by the Jimma university (JU) ethical review board. The permission letter was taken to JUSTH and after permission obtained from the hospital, permission asked from the participants. Verbal consent was taken from the participants to ensure the participant’s willingness to participate and willingness to record tape was approved prior to data collection. Strict rules of confidentiality were followed during the data collection, analysis and reporting of this study. Each interview subject was provided anonymity. All notes and audio files were kept with the field worker/note taker at all times. Participants and non-participants were not allowed to view the notes at any time and content of discussions and interviews were not be revealed to anyone else, to protect participants from possible harm at the revelation of such information except key informants to check for accuracy of their own interviews.
Dissemination of findings
The finding of the research will be disseminated to Jimma University postgraduate and research study office, regulatory affairs, ministry of health and other concerned body working in the area of culture and language sensitivity. Besides the findings of the works will be presented at different seminars and training organized by the Ministry of Health, partners, professional associations and regional health bureau. Also attempt will be made to publish on reputable journal.
Socio-demographic characters of study participants
The mean age of the key informant interview participant was 35.5 years with minimum of 26 years and maximum of 56 years.Key informants interview were taken 40-55 min. The mean age of patient interview participants was 32.3 years with the minimum of 19 years and maximum of 52 years age. Patients interview were taken 25-40 min (Table 1).
Challenges JUSTH faces and how JUSTH is addressing those challenges when providing care and services to culturally and linguistically diverse populations.
Developing supportive infrastructure, work force, data collecting and using, community engagement, organizational relationship, integrating cultural need into organizational planning, accommodating the specific need of patients and helping patients to manage their care are the major themes expected from the hospital to deliver cultural sensitive/ appropriate care for diverse patient populations.
Developing a supportive infrastructure for cultural sensitivity
Developing a supportive infrastructure for culturally sensitive care can be reflected by incorporating these ideals into an organization’s guiding principles, organizational planning, hospital-wide policies, Executive Level Staff Involvement, Hospital Vision, Mission, Value statements and Care provider commitment.
Executive level staff involvement
As study participants reported JUSTH has no designate individual and unit responsible for managing cultural and linguistic programs to meet the needs of diverse patients to express its commitment. As key informants expressed the JUSTH managements/executive level made poor support to recognize, prioritize and often drive efforts that establish policies and procedures that directly improve cultural appropriate care to better meet the needs of diverse populations. One of study participant explains executive level staff involvement as:
“…poor managerial conditions, medical controlling systems are weak, Monitoring and evaluations are not good so it needs strict follow up, medical director and the hospital management should be sensitive to this issue and made day to day follow up…” (24-years, Male, PI-5).
Hospital vision, mission, value statements
| Participants | Description (In-depth interview) | Total participants |
|---|---|---|
| Patients | A total of five males and five female participants. There age is between 19-52 years. Their religions vary from Muslim, Protestant, orthodox, catholic, Adventist and Wake feta. Their ethnicities vary from Oromo, Amhara, Hadiya, Kefa, Woliata, Dewuro, Nuer, Yem, Guraghe and mezhanger. Their residence areas also vary from rural village, woreda town and Zonal town. Their primary spoken languages also vary accordingly with their ethnicity. Their educational levels also vary from no formal education to masters students. | 10 |
| Key informant interview | A total of 3 females and 7 males. There age is between 26-56 years. From them three of them are orthodox, two them Muslim and five of them are protestant. The key informants were included from Administrative staffs, Nurse, Pharmacy, Physician, Laboratory technician and dietary staff. | 10 |
Table 1: Socio-demographic characters of study participants.
As key informants of the study reported and some of them share the hospital mission, vision, or values drive from Jimma University to me, although JUSTH did not directly mention cultural sensitivity in its mission statements, it had values statements that referred to “Community first”, “Quality Care”, “Compassion”, “Accountability”, “Collaboration “ and “Caring relationships”. JUSTH use a variety of terms to refer to their commitment to meeting the needs of diverse populations in their values statements as terms listed above.
As some of study participants noted JUSTH strategic plan “…is develop to increase patients satisfactions and to increase quality of services it does not include cultural and linguistic needs of the patients it only consider gender equity and HIV patients in its strategic and budget plan which share 2% hospital budget both are cross cutting issue in our plan…” (32 years, Male, KI-1)
Making cultural sensitivity a part of organizational planning
As key informant participants reported there are many standard guidelines such as nursing standard, pharmacy standard and the like which includes issue of cultural sensitive care indirectly, otherwise the hospital has no standard guidelines that directly show how to deliver cultural sensitive care to meet diverse patient needs. The hospital has different plan such as strategic plan, budget plan and business plan, while none of this considers or include the diverse cultural need of patients as its part directly, because the issue of cultural sensitive care does not come to the hospital image yet.
And also since the hospital has no guidelines facilitate delivery of cultural sensitive care, the care providers’ skills and commitment to follow ethical professional principles to meet diverse cultural need of the patient matters the quality of services delivered. One of the key informant participant said that “…hospital planning to have policy how to accommodate diverse patients’ culture in the future, but right know it is the challenges…”(30 years, Male, KI-10).
As key informants words the hospital also fail to incorporate patient demographic data into their strategic and business plans to better serve their patients/clients. The other participants also mentioned this issue as “there are no recognized formal plan, rule and regulation that included demographic data of population in our hospital to deliver non disparity health care to diverse patients’ populations. Each professions/disciplines has their own ethical principles to serve their diverse patients need.”(29 years, Male, KI-7).
Hospital policies for cultural sensitivity
As key informants reported that many staff of JUSTH is not aware of ways to meet the needs of diverse patients and are sometimes not aware that it is part of their responsibility. While hospital strategic plan does not includes developing and coordinating interpreter services (including the training and recruitment of interpreters); organizing diversity fairs and events within and external to the hospital; developing and implementing staff education programs on cultural sensitivity; use of language services; and related issues. The hospital strategic plans include equity as one principle which helps to address cultural and linguistic needs of the patients even if it is complex and unclear at institutional level. At time of interview the hospital doing with peoples who are not really professional interpreters /translators, but in the future the hospital has plan to recruit professional interpreters / translators.
One of key informants elaborate it as “…Equity is one of the principles the hospital used to address issue such as cultural diversity not only for Ethiopian in future we want to be medical truism center that requires even global culture to accommodate culture from different countries too, the main challenge is here equity in what term it is a very complex and unclear principle at institution level to operationalize…” (30 years, male, KI-10).
All of the interview participants in the study mentioned that JUSTH has no refrain from the use of family, or other untrained individuals as interpreters, rather the organization encourage using them since there is no other option to overcome language barriers in the hospital. Although staff interviews revealed that many of them face challenges when handling situations in which patients bring a family member or friend. One of the participant express lack of policy to overcome language barriers as follows “…actually relatives are used as the interpreters since the patient come always with relatives and some of them are knows Amharic language and they translate interprets the patient idea or the staffs used as interpreters these are the two main option, may be other people also used as interpreters…” (56 years, Male, KI-5).
Government policies for culture and language sensitivity
As some key informants assumed many government policies were supportive, some of them are complex and unclear at institutions level and while there are also lack of supportive policies in some cases. One of key informants explains government policies as follows:
Some of the government policy supportive for deliver nondisparity health care, while there is also luck of policy support us, for example the secularism principles be neutral from the religions, ethnicity, but when we became neutral some of the patients offend us for example in hospital the Muslim may want wear ‘hijab’ we not allow because of secularism policy to wear the hospital already identified kind of clothes. There is also no category on employments list for interpreter/ translators we should ask for category and salary. At institutions level it talks about gender sensitivity and equity which are the very complex one, equity in what sense but there is no such things about culture and language sensitivity issue (30 years, Male, KI-10).
Care providers commitment
Many of study participants raised majority of care provider commitment/efforts’ specifically to deliver cultural and language sensitive services is poor. And also they raised care providers commitments affected by many factors such as incentives, enough salary, enough supply, adequate and working environments.
One of participants elaborate commitments as “…Depends on individual motives if it is supported by third party saying management body and gets any encouragements it will be better. In absence of incentives, enough salary, enough supply, adequate and convenient working environments for professionals it will be difficult to talk about commitment. Also commitment affected by the ability immediate supervisors/ boss and commitments from higher officials…” (29 years, Male, KI-7).
A few study participants in contrast believe that health care providers highly commitment to deliver patients culture and language sensitive care except sometimes when they fall under high stress from behaviour of their job. One participant expresses care providers commitment as: they are highly committed because they are come from diverse cultural and linguistic backgrounds but it is also well known health professionals work under very high stress and high pressure this might be reflected on patients by showing them disrespect or not showing compassion care/ respect but may believe is they really try to do their best to respect culture and language needs of their patients because they are the reflection of this community (32 years, Male, KI-1).
Also the study participant rose, “…because frequent complaints from public health institution in Ethiopia ministry of health develop the initiative called Caring Respectful and Compassion (CRC) of professionals in its 2nd growth and transformation plan, but yet not functional. CRC really incorporate the cultural and linguistic issue of the patients so it helps to address this issue. If there are 100 health professionals two, three or four of them might not respect the cultural and language of their patients as whole this hospital employers are committed to respect culture and language of their patients…” (30 years, Male, KI-10).
As patient interview participant the hospital and the care providers must aware the difference between them and the patients, then accept that differences as normal and try to do their best to serve patients in one eye.
One of study participant expresses it as “…here the main thing done is that recognize our difference, we are different and people recognize our differences and respect our differences. It is difficult to dress and to walk on the same way but what will e done is aware people there is difference and respect each other’s. The hospital provides us clothes for dressing actually the clothes provide to us is almost not contradict with our culture both for male and females…” (35 years, male, PI-4).
Integrating culture and language into organizational systems
Incorporating the ideals of cultural sensitivity into planning processes, guiding principles and policies is a strong starting point for cultural sensitivity. The key elements of this theme are Integrating Cultural sensitivity into Patient Care, Determining appropriate culture and Language Services, Incorporating Interpreters into Patient Care and Translating Written Materials.
Integrating cultural sensitivity into patient care
Interview participants noted and many of them share the patient’s medical record card with me, that JUSTH medical card record system includes a field for recording a patient’s name, age, sex, address and phone number (optional) only, it does not include data such as race/ethnicity, primary spoken and/ or written language, religion, sexual orientation, disabilities, cultural needs, dietary needs and health literacy level. And those data on medical record card collected during initial (first) assessment and they used only to relate medical case only, they not related cultural need of the patients care.
One of the interview participants expresses it as follows
“…there are some data collected from patients at card room, the professionals relate some of them to patient conditions for example malaria related to environment you live may be in river area they analyze address in such manner. Totally they related your demographic information to medical conditions only…” (35 years, male, PI-4)
As interview participants reported that a challenge was failure to collect all patient level data listed above were results in failure to identify patients’ diverse needs, to match these needs to appropriate services and to effectively communicate with patients throughout the provision of care.
Determining appropriate culture and language services
As key informants reported JUSTH has no tools/process or guidelines to help guide staff through the decision process of selecting appropriate language services and present information for accessing those service. One of interview participant expresses this issue as:
In our hospital there are no any procedures or policy to address those challenges related to cultural and language aspects of the patients. But in each disciplines there are sort of agreements for example in nursing there is nursing care should be holistic saying it consider all aspects and all parts of the patients such as medical, social, psycho-social, religious and other cultural factors this might not for physicians, pharmacy and the other health professions. If there is a formal written policy or procedures to address those challenges related to cultural and linguistic sensitive services it is important and useful for every patient. Most of the rule and regulations are not formal procedures or policy rather they are mostly professionals ethics (29 years, Male, KI-7).
Incorporating interpreters into patient care
JUSTH has no professional and employed interpreter rather care providers use any nearby available individual weather they are family member, staffs or any other individual understand care provider language and patient language as word of all study participants. As this expressed by one interview participant as follows.
The care providers search for those individual working in the hospital and talking that language if they are available and willing to interpret that language we use them as interpreters. It is not such significant problem by the way the patients come with attendant either attendant or the patients know something about working languages Amharic or Afan Oromo. We faces difficulty on patients come from Gambela sometimes, but many of them competent enough to talk the English so the professionals can also use English. We use these mechanisms to overcome language barriers even if the hospital has no its own recognized interpreters and translators…” (29 years, Male, KI-7).
The key informants also rose that the JUSTH has no formal guidelines or procedures to trust the interpreted data as the hospital use non-professional interpreters; it is up to the health care professionals to trust those data through their own mechanism.
As this idea elaborated by participant words as follows:
We use those interpreters or translators not to trust the data but something is greater than nothing so we use them since we have no other options. There is no any mechanism/procedures used in hospital to trust the data. The professionals try their best through physical examination; laboratory finding and other diagnostic procedures to trust the data by compare it with interpreted history of the patients even if it is not possible to say trustworthy of the data totally addressed…” (39 years, Gender- Male, KI-4).
Translating written materials
As interview participants JUSTH was provides written informed consent in Amharic and Afan Oromo language only. Despite these the hospital provides written material such as educational materials, written instructions and medication information was provided with English language which was neither local language nor national language. They also add that JUSTH also not used formal symbols on medication labels to communicate instructions for taking medications to patients. As some key informants using English language for educational materials, written instructions and medication information was since the English language was international language it easy anything for those even came out of Ethiopia.
Work force
Work force concentrates on hospital’s efforts to provide culturally and linguistically appropriate care by diversifying the demographics and skills of their workforce. Key components of this domain include staff recruitment and retention and Human Resource Policies and Programs support cultural or linguistic sensitivity.
Recruiting and sustaining a diverse staffs
The key informants of the study reported JUSTH efforts to increase the language concordance between their staff and patient population especially for lower worker recruitment the hospital used both Afan Oromo and Amharic language for interview test, while higher worker allocated by Ministry of health. Recruiting a diversified workforce does not come without challenges. As key informants lack of resources for undertaking these types of recruitment efforts was cited by JUSTH as one of the major challenges they face. The lack of supportive policy from the ministry of health and federal government, preference of work place by employee, lack of incentive for employee and lack of availability of competent diverse human power can pose additional challenges for sustaining a diverse workforce as many of key informants noted.
One study participant elaborate it as:
According to federal principle institutions if you want hire the employee test/ examine them in Amharic language we taught that was not an appropriate way and we try to examine them in Afan Oromo also, because the gardens and cleaner they communicate most of the time with patients speak only Afan Oromo so it is not really logical to hire someone speak Amharic, but cannot speak Afan Oromo while majority of people speak Afan Oromo this is also one of our principles. The porters and runners also must to speak Afan Oromo, so this is the way we are trying to address their linguistic needs. If it is difficult for some of the people to interpret translate and they want professional interpreter/translators we do not have that kind translators, otherwise we try to solve the linguistic needs of majority which is Oromo people through such process… (30 years, Male, KI-10).
As key informants reported the hospital has never collect data on staffs diversifications while it collects data on reason for staff retention and the hospital consider collecting of employee composition data is the responsibility of ministry of health as the hospital is under federal government. As one participant support this idea by saying that:
“…I see data collected only on staffs turn-over and stay in hospital, I never seen the data directly collected on cultural and linguistic composition of the staffs…” (42 years, Gender-Male, KI-9)
Human resource policies and programs support cultural or linguistic sensitivity
As interview held with key informants the hospital has no formal policies in place regarding requirements for staff cultural or linguistic competency/sensitivity. I also asked key informants to identify which human resource programs (new employee orientation, ongoing training and competency assessments) addressed culturally and linguistically appropriate care and for which staff type. Many of them reported that new employee orientation addresses culturally and linguistically appropriate care more often than ongoing training or competency assessments for all staff categories because relatively information about majority of patient, type of patient, type of employee, hospital setting and the like shared more than ongoing training at new employee orientation.
As all key informants told me all ongoing training was professional training it does not include cultural and linguistic need of patients may be due to the need of partner organization deliver the training. As on study participant express it as:
“…professional training does not include cultural and linguistic aspect of patients, maybe it is due to this issue did not come to image for hospital and NGO those provide training in collaboration with the hospital…” (28 years, female, KI-2).
As all key informants noted JUSTH has no less formal methods for developing staff knowledge about cultures and languages of patient present in the hospital. The skills of working with non-professionals interpreters and to trust the translated data is up to the care providers, since the hospital has no formal and less formal plan to facilitate process of interpretation and process of trust translated or interpreted data which was left great challenge to the care providers to assure the trustiness of the interpreted and translated data as most of interpreter used in the hospital was family members.
Collecting and using data to improve services
Elements explored within this theme include collecting community level data, patient level data collection, using data to improve culture and language services, obtaining patient feedback, stratifying data and establishing a baseline of culture and language services.
Collecting community level data: As all key informants reported JUSTH has no a steering committee to review demographic data from the community to determine community health needs and plan for appropriate services and also the hospital never conduct community composition and need assessment. One study participant explains it as follows:
“…the hospital still does not conduct community or patients need assessments, therefore it has no identified planned patients safety issue related to culture and language of the patients. Of course the patients have right to practice his cultural practice even if the hospital does not prepared/fulfill any special considerations for patients cultural needs…” (56 years, Male, KI-5)
Collecting patient level data: As all study participants noted JUSTH was only collect and use data on name, age, sex and address to strengthen patient centered medical care to compare clinical outcomes rather than use those data for cultural and language need sensitive patient services and staff recruitment processes. Also they mentioned the hospital fail to collect patient level data such as race/ethnicity, primary spoken and/or written language, religion, health literacy and socioeconomic status. Participants also mentioned that patient data record format used in the hospital does not includes space to record data such as race/ethnicity, primary spoken and/or written language, religion, health literacy and socioeconomic status.
Few key informants reported that among the patient data record format used in the hospital only nursing standard format includes space to record cultural, language and every aspect of patients. As one participant elaborate it as:
The patient card includes the patients profile data such as, sex, age, name, address and phone number, which only used for diagnosis and medical issue. Only nursing standard care includes all aspect of patients data, but it only used by nurses even if it help to assess all aspect of patients need in every professions. It is complete, holistic and more comprehensive approach of assessments includes 11 functional patterns of patients. But I do not know the reason behind why other professionals not used may be due to professional gaps. I see the medical assessments format while the physicians clerk the patients the formats does not include all aspects of patients needs… (26 years, Male, KI- 8).
Using data to improve culture and language services: JUSTH does not collect data such as primary language, race/ ethnicity, educational level, etc., which is base to deliver cultural sensitive non-disparity care to diverse patient populations need as mentioned under collecting patient level data as study participants reported. One interview participant support staffs are committed to respect culture and language of patient by said that
“…they are committed because they are come from diverse cultural and linguistic backgrounds but it is also well known health professionals work under very high stress and high pressure this might be reflected on patients by showing them disrespect or not showing compassion care/ respect but my believe is they really try to do their best to respect culture and language needs of their patients because they are the reflection of this community…” (35 years, female, KI-6).
Establishing a baseline of culture and language services: As interview participants reported the JUSTH has no designed offices or focal person to monitor, facilitate and follow up how the hospital delivers cultural and language sensitive health care to meet diverse patient needs. While every care provider provides services by their own way since they have no any guiding principle and process, even many of them did not consider giving cultural sensitive services to meet diverse patient need was their responsibility. One of study participant expresses it as
“…there is no formal focal person or no formal way/process to facilitate cultural and linguistic needs of the patients in the hospitals. In developed countries once the patients admitted the food services are totally supplied by the hospitals according to the patients need and dietitian consult but in our setting we do not provide food services as patients needs unlike developed countries, simply the hospitals deliver what it has according to the already prepared hospital food menu and the relatives also bring food from their home for the patients, except the food contradicted medically.” (56 years, Male, KI-5)
Obtaining patient feedback: As study participants reported a JUSTH collected and reviewed patient complaint and/or patient satisfaction data to identify issues that could be better addressed by their services. One caveat to this practice is that patient complaint and satisfaction data are often collected through paper surveys. A JUSTH obtained patient feedback through informal patient interviews and suggestion box to identify patient care issues as a way to collect data to improve care and Culture and language services. One participant expresses obtaining feedbacks as
“…We always use the satisfaction result in our plan and we want to raise the satisfaction level and we take their feedbacks through suggestion boxes. Patients complain by coming to the office, but people do not complain about the translators/ language issue, religion issue because they might think it does not solve at hospital level. They complain about appointments, physician issue, nurse’s treatments, medications, laboratory and I hope we include about the culture and linguistic needs of the patients in our survey questionnaire in the future…” (30 years, Male, KI-10).
The other key informants also expresses as “…the hospital board members also represent the Zonal health departments, town health offices and community representatives they will also bring the problem and feedback of the clients and we try to accommodate the problems…”(38 years, Female, KI-3).
Stratifying data
As mentioned earlier, collecting accurate data regarding patient age, gender, race/ethnicity, primary spoken and/or written language, religion and other demographic characteristics can help organizations better assess the need for culture and language service. As participants report JUSTH does not have information systems that allow patient demographic data and quality measures to be easily linked. JUSTH does not stratify data by demographic variables even it does not collect such as race/ethnicity, primary spoken and/or written language and religion. As one participant said
“…generally in our country using secondary data and data generation is very poor, because there is lack of technology to save and generate data. There is huge problem/gap on using, having and storing appropriate data in the hospital totally…” (29 years, Male, KI-7).
Accommodating the needs of specific populations
Accommodating the needs of specific populations reflects the organizational efforts that directly address the language, cultural and health literacy issues of specific populations.
Training to support effective communication
As key informants of the study participants JUSTH does not provided staff with language courses of patient language as a Second Language during on-going/on jobs training. While such courses may alleviate some specific communication barriers staff members may have, they do not provide a means of bridging language barriers between staff and patients. As study participant hospital should keep in mind that the ability to communicate effectively is important for all staff, as it is not only health care professionals who interact and communicate with patients during the health care encounter.
Training to support cultural competence and sensitivity
As report of many key informants a JUSTH has no plan of training of its staff on cultural competence and sensitivity, all of its training focus on professional aspect rather than focus on culture and language need of diverse patients. One of study participant reported that
“…all training given here are professional training does not include cultural and linguistic aspect of patients, maybe it is due to this issue did not come to image for hospital and NGO those provide training in collaboration with the hospital…” (42 years, Male, KI-9).
While some key informants said that some of the training provided by hospital has directly or indirectly support cultural competence and sensitivity.
One of participant support this idea expresses it as “…some training include for example I participate in some training not more than three one of them include how to approach patients, how treat patients, how we can identify the needed data and the like…” (26 years, Male, KI-8).
Creating an environment that meets specific patient needs
Interview participant reported that providing culturally appropriate care requires an assessment of the hospital’s entire environment from the patient perspective. As diverse patient populations may contain different ethnic, religious, language, literacy groups and so on, hospitals should consider all perspectives when providing care.
Another significant component of an inclusive environment is the presence of directional signage and other critical postings in a format that is appropriate and accessible. However, achieving a patient friendly environment encompasses more than just having bilingual signage; health literacy levels should also be taken into account. As participant of the interview remarked the JUSTH has no appropriate guider, no bilingual signage and has little billboard with only Amharic and English may be Afan Oromo which was very difficult to get appropriate site of services even for educated person. Also they raised JUSTH does not used universal healthcare symbols and only have one information desk for formality which was not deliver services to meet both literacy and language needs. One of study participant elaborates it as:
“…Most of the places are unknown you do not know the real locations and it is difficult to go where you want to go, so most of places are not clear to get and some of the facilitators are not interested to tell the real information…” (24 years, Male, PI-5)
One study participant expresses enhancing the Hospital’s Physical Space as:
“…You cannot accommodate/prepare pray area for all religions really challenging so the hospital planning to have policy how to accommodate diverse patients’ culture in the future, but right know it is the challenges because it difficult to prepare praying area to all religions…” (30 years, Male, KI-10).
Assessment of patient needs
As key informants reported the JUSTH has no formal process to identify cultural and linguistic needs of patients except it is up to care providers to identify patient cultural and linguistic needs. While the data collected at admission was used for medical purpose only since the issue of cultural and linguistic sensitive care does not come to image for hospital to use those data to identify cultural and linguistic needs of patients.
Some key informants revealed specific elements of the assessment that staff use to determine patient needs, sometimes involving the judgment of individuals other than the patient. For example, one participant told me, “…We might identify them by clothing, a dialect they speak, material nearby them, whatever…” (35 years, Female, KI-6).
Several other participants identified the patient’s family as a good source of information about their particular needs. Yet another participant revealed that staffs sometimes make their own judgments about patient’s language needs because they are uncomfortable asking patients for this information. The participant also explains, just listen to what they’re saying and then try to determine what their language is and then they search for an interpreter as needed.
Adapting services to address cultural beliefs
As key informants reported some female patients prefer to be seen with female care providers, a JUSTH does not locate a female Muslim patient to a different unit to accommodate her cultural preference for a female provider. Even if the hospital does not locate female provider for female Muslim patients the staff found ways to show their respect for female Muslim patients.
A few key informants mentioned the hospital adapting its food service programs menu prepared from common traditional diet of the country, from experience shared from different hospital nationally and internationally. As on study participant said:
“…based on experiences from others hospital we visit many hospitals in India, Korea and others countries and also based on the our budget such kind of menu satisfies the budget and also the balanced patients need, it also includes the recommendations from nutritionist and the Ethiopian culture we use ‘injera’ with wat the common Ethiopian food, because it has most of ingredients presents in other foods…” (30 years, Male, KI-10).
As some patient interview participant the type of food menu was not based on their cultural needs, while other participant has no complain with type of food rather complain on the quality of diet preparation such as not cooked well, it has no food sniff/ smell and even there was doubt on the meat provided whether it cultural acceptable meat or not. Developing menus that are more attuned to the cultures of patient populations is not only a food preference issue. As one patient interview participant “… Many patients/clients joking to each other by saying “Does it donkey’s meat or pig’s meat…” (19 years, Gender-Male, PI-2).
The other patient interview participant also express food services of hospital as “…for us the food provides here is not favorite we use ganfo and milk in our area, if we show how it prepared and our food provide to us it is better…” (35 years, Gender-male, PI-4).
The other important issues in Hospital food services is how and by whom it prepared which matter the quality and content of food in line with medical need. As key informants interview participants the hospital has no dietitian for long time but recently there is one dietitian even if still it not properly starts supporting the diet services. The surprising issue is here the food services is managed and coordinated by environmental and sanitary professionals with traditional women cocked and prepare food traditionally without any training. As one key informant said “….Personally I know the food services controller; she is environmental and occupational health professional…” (39 years, Male, KI-4).
As many patient interview participants rose there is difference between the units in services they provide, there are some units provides services in good manner while there are also services units not properly give services. One of the study participants expresses the difference between service units as problems commonly seen on Guards, card room workers and laboratory service worker. For example I stay/wait for laboratory services for full day while many people come after I give sample took the result since they know the laboratory technicians. I hear when they say to each other he is my social/relatives please give priority to him. The laboratory and pharmacy services many times they said it is not present and send us to private clinic and drugstore this also lead as to financial crisis… (45 years, female, PI-8).
Helping patients manage their care
This theme shows hospital’s effort to reduce disparity health care through patient education. It includes providing patient education and use of technology in patient education.
Providing education for patient: As interview participant JUSTH employed several practices to educate patients in Amharic and Afan Oromo language. Nurses of the hospital always deliver regular health education to patient on daily bases and record all topic of education they delivered. There is also patient education at time of discharge and also there is information provided for patient at admission time. There are also regular health education sessions for HIV/AIDS and Tb patient two times daily with peer educators in collaboration with nurse.
As participants of the study even though several practice employed in the hospital there is no formal process and formal designed person to facilitate the services and there are no education programs for sign language, for deaf and hard of hearing patients. As participants of the study reported an effort to meet both the educational and cultural needs of the patient population, hospitals may also alter how they provide education to account for traditional customs. All of the educations delivered to patient in JUSTH were focus on the medical aspect and medical need only it expected much from hospital to make patient education program more culture and language sensitive.
Using technology in patient instruction and education: As many of study participants said JUSTH used web and radio program to reach the community, to deliver information, message and educate community with only English, Amharic and Afan Oromo languages, which actually not satisfy all diverse language and health literacy of community needs. As one of key interview participant expresses:
“…We have program on radio (radio Fana broadcasting corporations) we transfer our messages such as the services we deliver, what expected from patients, what are the services functional at hospital currently, payment mechanism, what are the services delivered freely and so on which has its own role to address the community needs…” (42 years, Male, KI-9).
Understanding health beliefs, needs and values: Nearly all participants reported that the hospital tries its best to address the cultural needs of patients through religious, dietary and psychosocial methods. Sometimes if people come from Gambela, Somalia and Afar they really do not like to eat the regular food they like ‘pasta’ and rice the hospital try to accommodate their needs. The hospital provide diet services equitably for all religion accordingly for example if the meal is meat it should the same for Muslims and Christians, but different from their sources as their religions. As key informants the hospital has separate room and refrigerators for Muslims meat and Christians meat accordingly, even if the hospital does not know the source is it really slaughter by Muslim persons or not and the same for Christians.
Key informants rose that the hospital also try to accommodate the dietary needs of patients to same extent for example the patients may need porridge we will not prepare that because we just provide already prepared food and widely available for example ‘injera’ delivered by different company as well as bread are delivered by another company, but there is lack of company to deliver uncommon diet type like porridge. One of key informants support this idea by said “…so we cannot say we accommodate 100% the patients dietary needs we say we accommodate dietary need based on medical indication and trying to accommodate based on the cultural needs…” (30 years, Gender-Male, Religion-protestant, ethnicity -Oromo).
Some patient interview participants express the hospital services were lack understanding health beliefs, needs and values of patient need, rather it based and considers medical need of the patients. One of the participants explains it as by considering a culture I do not think so. For example one way let me say language so when we come and try to seek something language may consider for example no translators here that is appointed to be paid because now there is referral from our area to here, but no person who can translate here only students in this university they stop studying and said please come on help me over here why they do not find another way this is government hospital the government find the way to serve the peoples too. Also the way we dress and the way we look/personal images not all peoples some peoples see us negatively but not all people, just to tell them accept the difference as it is. Some people say white or black something like that out of us related to color and residence name oh he come from this area so he is this…this for example if you come from Borena they said this people live their they thus…thus so they approach you negatively and they not serve you in good way… (35 years, Male, PI-4).
Many patient’s interview participants rose that in their culture priority is given to old peoples, pregnant women, severely ill patients and patients highly in need for support, but here mostly priority is given to social, friendship and relatives which was contradict with their culture. Also here most of services providers are reluctant they did not feel your problem as their problem.
One interview participant expresses it as …according to my culture we give priority to the person who face the problem means other persons is sensitive to the persons needs help. Here they did not feel your problem us their own problems, unlike what we feel in our culture. They are reluctant about your problems and your culture they simple ask you questions you respond they jot dawn and then they prescribe you a medications. They did not ask your way of thinking, your feelings and your needs…” (37 years, female, PI-9).
Provision of language services: As study participants mentioned the linguistic service most commonly available in JUSTH hospital is the family members/relative interpreter; followed closely by bilingual staff interpreter and any other individual understand the client’s language volunteer to interpret were used. Other language service mechanisms such as hospital-employed interpreters, contract interpreters, or volunteer interpreters were not provided by than JUSTH. All study participants reported using untrained staff interpreters, untrained patient relatives and untrained bilingual staff. One participants support non-professional use of language services in hospital as “…actually relatives/family members are used as the interpreters since the patient come always with relatives and some of them are knows Amharic language and they translate interprets the patient idea or the staffs also used as interpreters these are the two main option, may be other people also used as interpreters…” (35 years, Female, KI-6).
All of key informants reported that they use family member or friends as interpreters because they have no other options. And also the key informants reported there was limited awareness of risks associated with using family members to interpret among interview participants and the JUSTH has no clear stance on the issue of using family members. Also JUSTH has no established policies discourage the use of staff from family members or friends as interpreter as key informants words. One of participant elaborate use of family members as “…use those interpreters or translators not to trust the data but something is greater than nothing so we use them since we have no other options. There is no any mechanism/ procedures used in hospital to trust the data. The professionals try their best through physical examination; laboratory finding and other diagnostic procedures to trust the data by compare it with interpreted history of the patients even if it is not possible to say trustworthy of the data totally addressed…” (29 years, Gender-Male, KI-7).
Patient safety
All of key informants have identified direct relationship between patient’s linguistic needs and patient safety issues as well as reported a direct relationship between patient safety and patients’ cultural needs. Also they raised lacks of patient-level data such as primary language, race and ethnicity, along with health information systems limitations and limited awareness have inhibited study of the patient safety connection to culture and language. One interview participant expresses hospital patient safety issue as “…the hospital still does not conduct community or patients need assessments, therefore it has no identified planned patients safety issue related to culture and language of the patients. Of course the patients have right to practice his cultural practice even if the hospital does not prepared/fulfill any special considerations for patients cultural needs…” (56 years, Male, KI-10).
Establishing collaborations
Collaborative practices is both internal and external encompass those activity bring together multiple departments, organizations, professionals and individuals to deliver culturally and linguistically appropriate care.
Establishing internal collaborations
Working together within the hospital: As key informants mentioned JUSTH was lucky enough as it has different professional levels from diverse ethnic, language, religions, culture and different social backgrounds which help to share different culture and experience which its own positive impact on quality of services hospital provides to diverse patients. As one key interview respondents explained
“…Luckily enough even though we did not identify staff composition percentages most of the staffs in this hospital are from diverse religious and ethnic groups, so in the future I think the federal government has also a plan to determine the ethnic composition of each of federal staffs in federal institutions that time we will implement, but luckily here some found from SPNN, most of them are Oromo but I cannot say the majority because it is very mixed and diversified ethnic group…” (30 years, Male, KI-10).
All professions in the hospital work together with different initiative such as Health Services Development Army agent (HSDAA) meeting, Morning sessions, rounding, management meeting and etc., which encourage collaborative work. One key informant study participant expresses working together within hospital as
“…health services development army agent meeting at the end of working hours which participate all staffs has great importance if use properly. The meeting include discussion of activity performed, challenge they face and possible measure to solve the challenges…” (56 years, Male, KI-5).
Establishing a cultural diversity committee/unit
As participant of the study even if JUSTH has no established committee or unit facilitate cultural diverse need of patient services for time being, it is better if establish committee involving staff from across the organization throughout the development and implementation of culturally sensitivity cares is essential to helping identify all the needs to be addressed and to provide feedback on solutions to meet those needs. Along these lines, among the most common suggestion reported by interview participants the establishment of a Cultural Diversity Committee comprising administration, management, employees, members of the community or patient population. As suggestion of interview participants it is better if these groups are often tasked with providing mentorship, education, information sharing and other activities related to offering cultural and language (C&L) services. One of study participant explain Establishing a Cultural Diversity Committee/ unit as “…Having cultural and linguistic unit is also important even if it is not simple to our hospital since our country have too many culture and language and every culture have must respected and have representatives which is difficult in terms of feasibility…” (32 years, Male, Religion, KI-1).
Establishing external collaborations
Building bridges with other health care organizations: As key informants said the JUSTH has also organizational relationship in addition to all hospitals and health center in Jimma zone and also has relationship with different four hospitals with south to south hospital relationship initiative while all of this relationship was not directly focus cultural and linguistic need of diverse patients. This relationship has its own importance for the hospital for example each health center conduct different community discussion forum and they bring their community feedback and need to JUSTH this helps the hospital to identify its patient needs and problems.
One study participant elaborates the hospital relationship with other health care organization as:
We have relationship with different organizations such as insurance company and also we collect the feedbacks from this organizations from zonal health departments, from town health offices and from woreda health offices because they frequently conduct community conversations here about their concern of this hospital they will give us feedbacks based on these feedbacks we try to address the issues. (30 years, Gender-Male, KI-10).
Sharing existing resources: Some key informants reported that JUSTH was deliver medication near to expire for all hospital and health center found in Jimma Zone, also the hospital give mentoring, training and share experience for those organization. In some cases, sharing existing resources can help resolve issues related to time, finances and staff. And by sharing resources through partnership program, the hospital may find new methods of filling gaps in their own materials and programs as expressed by study participants.
Engaging the community
Community outreach: Interview participants reported that the JUSTH conduct community outreach program with different departments to address medical need of community. Ophthalmology and POC were the department conduct community outreach program, the program includes activities such as identify the needs of the patients on artificial limb or walking aid they needs (crutch, winchers, artificial leg, special shoes) prepare those material according to the community needs and deliver it to the community, actually it is not issue directly related to culture and language of patients. The JUSTH has relationships with all districts in Jimma zone, insurance company and different organizations in Jimma town and surrounding area to facilitate care of their patients. The JUSTH Transfer health information such as the services the hospital deliver, what expected from patients; what are the services functional at hospital currently, payment mechanism, what are the services delivered freely were some of activities addressed through organizational relationships.
One participant explain JUSTH outreach program as:
The hospital has four outreach programs in Jimma zone and Gambela region one of them is ophthalmology department outreach program for cataract surgery with health education. The other one is prosthetic orthopedics center (POC) provide material such wheelchair, crutch and the like according to patients needs. The other one is PMTC mentoring and monitoring of HIV/AIDS services in all Jimma Zone health centers it is capacity building program for health center. The hospital also provide drug near to expire for hospital like Shenen Gibe, Limmu Genet and Agaro hospital freely. The hospital also provides capacity building training for all hospital in the Jimma Zone. Actually the hospital cannot include assess the cultural needs of the community while going for the outreach program in the community…” (26 years, Male, KI-8).
The JUSTH has agreement with different woreda to refund the cost of services after the patients get services and also collect the feedbacks from zonal health departments, from town health offices and from woreda health offices because they frequently conduct community conversations about their concern of JUSTH and they were give us feedbacks based on these feedbacks the hospital try to address the issues. The hospital board members also represent the Zonal health departments, town health offices and community representatives they were also bring the problem of the clients and the hospital were try to identify the cultural and linguistic need of community through these relationship and try to accommodate the problems.
Community partnerships: As key informants reported the JUSTH has relationship with Jimma University (JU) and different non-government organization through the University for different kind of professional training while this training mainly focus on the professional need perspectives rather than patient culture and language perspectives.
The major challenge reported by patient interview participants was that the hospital allowed post services payment only with Jimma Zone Woreda that makes patients come from outside of Jimma Zone catchment area feel disparity related to residency. Most of patient interview participants reported if the hospital has such agreement with all Woreda out of Jimma zone it is better for them. One of the patient interview participants expresses it as follows:
The other major problem I think need study is issue of free services and back payments/refunding services for example I have free services paper from the woreda, but the hospital told me I cannot get the free services since I come from the SPNN and they told me the services delivered only for those people come from the Oromia region. Also the refunding services agreement also made with Jimma zone woreda rather than including all the catchment area the hospital cover… (23 years, male, PI-10).
Using community leaders to bridge cultural barriers: As participant of the study even if JUSTH has many diverse patients having diverse cultural needs related to religious beliefs; hospital not develop relationships with local religious leaders and religious institutions to provide resources and guidance for serving patients with specific needs. In addition, JUSTH has no chaplains often serve as cultural brokers, helping hospitals address patient’s cultural needs. While these partnerships may help fill existing gaps in a hospital’s culture and language related services, they can also present major challenges. As one key interview mentioned, the secularism principle of country and University principle not allow the hospital to have hospital chaplains and collaborations with religious leader. Staff training on accessing these services and understanding their role in the provision of culturally competent care may also be required, even if JUSTH has no such culture and religious focus training to meet the patient needs.
This explained by one study participant as “…according to the Ethiopian government secularism principle and the University guidelines on secularism religious issues should be individual concern as institution we have secularism enough we have to be neutral from patient’s religion and culture…” (39 years, Male, KI-4).
Conceptual model
There are eight themes emerged from the data all themes have direct contribute for hospital cultural sensitive service. There is continuous circular relationship between each theme as shown in below figure. Continuing sequences of activity seen in each emerged theme. Give emphasize on an activities in each theme rather than the connecting arrow or flow. There is no higher hierarchal relationship between each theme (Figure 1).
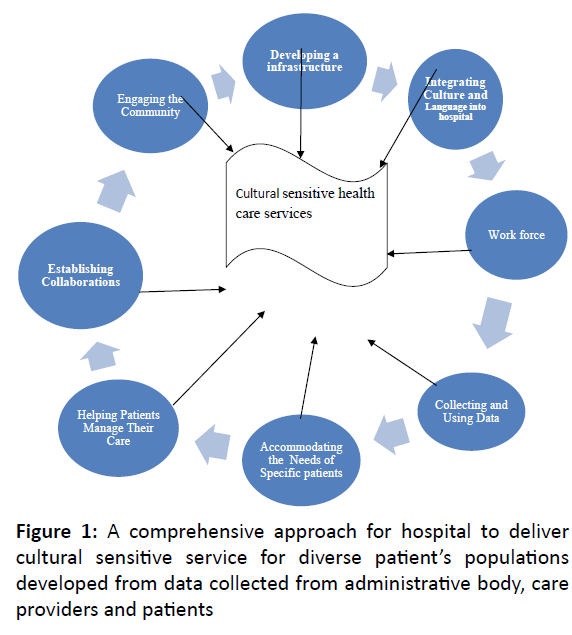
Figure 1: A comprehensive approach for hospital to deliver cultural sensitive service for diverse patient’s populations developed from data collected from administrative body, care providers and patients
Executive leaders play an important role in guiding and integrating the hospital’s programs for the provision of culturally and linguistically appropriate care, including providing the necessary resources [26]. Leaders create an organizational culture and can serve as models of culturally sensitive behavior. JUSTH has no designate individual and unit responsible for managing cultural and linguistic programs to meet the needs of diverse patients to express its commitment.
As hospitals in the HLC study demonstrated, one way to integrate these needs into organizational planning is to use the Office of Minority Health’s National Standards for culturally and Linguistically Appropriate Services (CLAS) in Health Care as a blue print to guide equitable care [27]. JUSTH has no standard mechanism show how to deliver cultural sensitivity care to meet diverse patient need since there is no clear law support this service at national ministry of health level, the hospital has not yet uses any guidelines and policy to deliver culture and language sensitive services to meet diverse patient needs.
Hospital can use other standards and frameworks from the literature to guide organizational planning. Other resources include The Joint Commission’s standards, the HLC research framework from Exploring Cultural and Linguistic Services in the Nation’s Hospitals: A Report of Findings (HLC Report of Findings) [13] and performance expectations from AMA’s Ethical Force report Improving Communication Improving Care: How Health Care Organizations Can Ensure Effective, Patient-centered Communication with People from Diverse Populations [28].
Policies offer an additional vehicle to clearly communicate the organization’s commitment to cultural competence and equitable care to patients. Many staff of JUSTH is not aware of ways to meet the needs of diverse patients and some of them not aware that it is part of their responsibility as the hospital has no policies for cultural sensitivity. Several HLC study hospitals mentioned that organizational policies reinforce cultural sensitivity in the provision of care. Staff awareness and cultural sensitivity should be built upon a shared desire to understand and meet the needs of patients, rather than a means of avoiding punishment [29].
Changes in patient care are necessary to complement cultural sensitivity at the organizational planning and systems levels. JUSTH medical card record system includes a field for recording a patient’s name, age, sex, address and phone number only it does not includes data such as race/ethnicity, primary spoken and/or written language, religion, sexual orientation, disabilities, cultural needs, dietary needs and health literacy level, a challenge was that lack of these data were result in failure to identify patients’ diverse needs, to match these needs to appropriate services and to effectively communicate with patients throughout the provision of care. Patient needs should subsequently be documented over time as they are identified in order to provide both effective hand-off and patient-provider communication [12].
As with systems for tracking patient needs, hospitals developed a variety of tools, including decision trees and charts to help guide staff through the decision process of selecting appropriate language services and present information for accessing those services [13]. These tools give hospitals an additional opportunity to communicate to staff any related policies or procedures regarding culture and language specific services. JUSTH has no tools/process or guidelines to help guide staff through the decision process of selecting appropriate language services and present information for accessing those services. This has direct and indirect impact on the hospital cultural and linguistic sensitive services to diverse patient needs.
HLC study hospitals developed systems for providing medication information and prescription labels in a patient’s primary language and also considers using symbols to bridge barriers presented by health literacy [13]. A JUSTH, for example, not used symbols on medication labels to communicate instructions for taking medications to patients. JUSTH was provides written informed consent in Amharic and Afan Oromo language only which may show less effort of hospital to facilitate understandable easy hospital services.
Hospitals can prioritize diversity within recruitment and hiring processes in order to incorporate cultural sensitivity considerations at the workforce level [12]. The participant of the study reported JUSTH efforts to increase the language concordance between their staff and patient population especially for lower worker recruitment the hospital used Afan Oromo and Amharic for interview test as majority of patients are Afan Oromo and Amharic speakers, while higher worker allocated by ministry of health.
Developing a diverse workforce that reflects the community and patient population is one strategy recommended to foster the provision of culturally and linguistically appropriate care as well as the complimentary benefits of increased patient trust, increased market share and decreased staff turnover [30].
One approach to ensuring that hospital staff possesses a minimum level of cultural and/or linguistic sensitivity is developing written human resource policies that establish requirements for staff member’s cultural and/or linguistic sensitivity. As interview held with key informants the hospital has no formal policies in place regarding requirements for staff cultural or linguistic competency/sensitivity.
At this time, The Joint Commission Accreditation Standards do not specifically require ongoing training in cultural and linguistic competence but do require orientation on “cultural diversity and sensitivity”, which may account for the higher percentage of hospitals including this training in their orientation programs but not in ongoing training programs [31]. The literature calls for increased training on cultural competence/ sensitivity and the use of language services for medical students and students in the health professions [32].
JUSTH does not have steering committee to review demographic data from the community to determine community health needs and plan for appropriate services and the hospital never conduct community composition and need assessment unlike many of hospital participate in HCL study. Data collected at the community level provides insight into populations that actively use hospital services as well as groups that may need targeted outreach to increase access and interaction with the organization/hospital.
JUSTH has no designed offices or focal person to monitor, facilitate and follow up the how the hospital delivers cultural and language sensitive health care to meet diverse patient needs. While every care provider provides serve by their own way since they have no any guiding principle and process, even many of them did not consider giving cultural sensitive services to meet diverse patient need was their responsibility. This has great impact on patient outcome and on quality of services as well as it was no of major challenge for care provider in their way to deliver services.
Collecting patient feed-back data following the provision of Culture and language services allows an organization to evaluate those services from the patient perspective A JUSTH collected and reviewed patient complaint and/or patient satisfaction data to identify issues that could be better addressed by its services. A JUSTH obtained patient feedback through informal patient interviews and suggestion box to identify patient care issues as a way to collect data to improve care and Culture and language services.
Although exploring Cultural and Linguistic Services in the Nation’s Hospitals: A Report of Findings (HLC Report of Findings) advocates using technology as a tool to facilitate data stratification. In the absence of information systems that facilitate linkages between important components of patient level data (e.g. demographics and outcomes), hospitals will be challenged to identify, monitor and address inequities of care that may exist between their patient populations [13]. Failing to do so may have negative long-term consequences for both diverse patient populations and the hospitals trying to care for them. Data systems that support the collection and facilitate the use of these data will allow hospitals to refine their quality, performance and outcome measures in order to improve culture and language services.
The role of effective communication in patient safety has been well documented in the current literature [33]. Organizations can highlight the importance of communication throughout the continuum of care by training staff to improve their communication skills with patients. Another way to enhance communication with patients is to provide staff education on how to work with a professional health care interpreter during medical encounters. A JUSTH does not provided language courses of patient language as a Second Language for its staff. While such courses may alleviate some specific communication barriers staff members may have, they do not provide a means of bridging language barriers between staff and patients.
Hospitals are undertaking numerous efforts to create a physical environment that supports the diversity of their patient population. The physical environment includes everything from the layout of waiting areas and waiting rooms to navigational signage and decor. Beyond redesigning the elements of an existing physical space, an inclusive environment may also require structural additions. Some hospitals are making adjustments to accommodate the needs of both patients and staff. One northeastern USA hospital opened up a mosque and work with the Imams in the community and with physicians [12]. This practice reflects a structural modification targeted to a specific population and illustrates the importance of engaging community leaders to improve hospital services for patients and staff. As interview participants the JUSTH has no mosque, church or any other designed praying area, even if it allow its patients/clients to pray in any area convenient for them.
The JUSTH has no formal process to identify cultural and linguistic needs of patients except it is up to care providers to identify patient cultural and linguistic needs. While the data collected at admission was used for medical purpose only since the issue of cultural and linguistic sensitive care does not come to image for hospital to use those data to identify cultural and linguistic needs of patients. From diagnoses to treatment plans, the patient care process hinges on the identification and understanding of patient needs. Similarly, the provision of culturally and linguistically appropriate care depends on an accurate assessment of a patient’s cultural and linguistic needs.
Informed consent is an essential component of the health care process and must be an interactive exchange between patient and provider [34]. Each hospital must build supports into the informed consent process that account for patient’s cultural and linguistic needs in order to facilitate information flow regarding risks, benefits and alternative treatment options from the patient to the provider and from the provider back to the patient. Participants reported that their informed consent processes consider linguistic needs of patient those understand Amharic and Afan Oromo. Consent is obtained through the use of non-professional interpreter for those patients did not understand Afan Oromo and Amharic.
Patients must have the appropriate education and training to make informed decisions, actively participate in and manage their care [35]. Even though several practice employed in the JUSTH there is no formal and well organized process to facilitate the services and there are no education programs for sign language for deaf and hard of hearing patients. In an effort to meet both the educational and cultural needs of the patient population, hospitals may also modify how they provide education to account for traditional customs. Hospitals should remember that although technology is a more convenient or efficient channel to convey information; it is the quality of the message and materials that will ultimately determine whether the needs of patients are being met [36]. JUSTH used radio program to reach ear of the community to deliver information, message and educate community with only Amharic and Afan Oromo languages, which actually not satisfy all diverse language and health literacy of community.
A clear understanding of a patient’s cultural context is indispensable to a provider when attempting to practice culturally and linguistically appropriate care [37]. It may be that these issues are not specifically addressed in JUSTH policies; it incorporated into professional ethics. Every profession has its own professional ethics which includes understanding patient needs and values from patient perspective rather than from your own perspectives which help to identify patients need and heart beat.
Along with meeting the cultural needs of patients, hospitals have established programs to meet various religious and spiritual needs of patients [13]. JUSTH has no developed interfaith chaplaincy programs comprised of leaders from a variety of different religious groups due to secularism principle of the country as well as University principles. Even if spiritually or culturally centered committees can play an important role in the development of centralized programs, the hospital lacks both committees. In addition to the use of focus groups, these committees can inform the development and implementation of such centralized programs.
The linguistic service most commonly available in JUSTH hospital is the family members/relative interpreter; followed closely by bilingual staff interpreter and any other individual understand the client’s language volunteer to interpret were used. Other language service mechanisms such as hospitalemployed interpreters, contract interpreters, or volunteer interpreters were not provided by than JUSTH. JUSTH reported using untrained staff interpreters, untrained patient relatives and untrained bilingual staff.
The use of family members, particularly minors, to serve as interpreters for medical encounters is highly discouraged by many authoritative sources [38]. Several studies have shown that the use of family members or other ad hoc interpreters are more likely to misinterpret information, omit or add information, or insert their own values or judgements into the conversation [39]. While the use of family members is not firmly prohibited by Title VI, it is not recommended [40]. JUSTH could find itself at risk by relying on family members to interpret since there is no way to determine the competency of the family member nor is there a way to make sure no conflict of interest exists between the family member and the patient.
Recognizing the importance of both language and culture in providing safe care to diverse patients, all of key informants have identified direct relationship between patients’ linguistic needs and patient safety issues as well as reported a direct relationship between patient safety and patient’s cultural needs. Lacks of patient-level data such as primary language, race and ethnicity, along with health information systems limitations and limited awareness have inhibited study of the patient safety connection to culture and language.
A strategic approach that integrates an understanding of community needs with community collaboration can improve a hospital’s provision of culturally and linguistically appropriate care, thereby increasing quality for diverse populations and potentially reducing healthcare disparities [41]. Hospital must understand the communities they serve, including how sociocultural beliefs impact patient health and perceptions of health and health care, in order to develop effective health care options.
Establishing collaborative relationships with community entities can provide hospitals with detailed information on issues such as community member’s health-seeking practices and resources like ethno-medical healers, which can help hospitals tailor interventions to the communities they serve [42]. Interview participants reported that the JUSTH conduct community outreach program with different departments to address medical need of community. The JUSTH were work with both public and private agencies to meet their communities’ transportation needs and to address socio-economic needs of patients.
Collaboration with academic institutions and training programs has the power to provide a comparable opportunity for hospitals that are not affiliated with health professional teaching programs to establish potential sources for recruiting and training a more diverse workforce. As interview participants reported the JUSTH has relationship with Jimma University (JU) and different non-government organization through the University for different kind of professional training while this training mainly focus on the professional need perspectives rather than patient culture and language perspectives. Developing new training programs requires both time and money, which can be difficult to find, but a number of partnerships have made available the structure of their programs as well as some lessons learned, upon which hospitals can draw [43-45].
The JUSTH has many diverse patients having diverse cultural needs related to religious beliefs; hospital not develop relationships with local religious leaders and other institutions to provide resources and guidance for serving patients with specific needs. The National Center for Cultural Competence’s sharing a Legacy of Caring: Partnerships between Health Care and Faith-Based Organizations may help organizations explore the potential benefits and barriers to developing these types of collaborations [46].
Knowing that cultural differences as well as similarities exist, without assigning values (i.e., Better or worse right or wrong) to those cultural differences. This usually involves internal changes in terms of attitudes and values. Awareness and sensitivity also refer to the qualities of openness and flexibility that people develop in relation to others [47]. JUSTH only focus is how to give only medical services, they are not consider where you come from or where is your place, what do you needs or what is you culture needs, your educational status, your backgrounds and the like they are not sensitive about your culture and your way of life which may open door for non-disparity health care.
Principles of theoretical sampling and theoretical saturation are only applied within the already collected data or within data at hand. The data does not include all representatives of diverse patients backgrounds perception’s those served in the JUSTH. Data is subject to variation in accuracy based on respondent’s level of knowledge and possible intentional deceptions.
Conclusion
Without an organizational commitment to cultural sensitivity and subsequent action at the policy and procedure level, it is difficult to provide patients culture and language sensitive services. It should be accompanied or supported by data collection and evaluation, accommodations to patient needs and internal and external collaborations, community engagement, integrating cultural need into organizational planning and helping patients to manage their care. For example, data collection on patient needs and community demographics is crucial to developing strategic initiatives, determining staff recruitment targets/staff-patient concordance goals and developing patientcentered visits and communications. Systematically collect data allows the effectiveness and utilization of cultural and language (C&L) services to be monitored, measured and evaluated. These practices can be useful for planning and designing services to provide safe, quality care and decrease health disparities.
There is no doubt that collaboration needs to play a role in all the practices outlined in this report. For example, as hospitals develop culture and language related organizational policies and procedures, leadership should engage and bring together stakeholders from multiple departments in order to understand the environment (supports, constraints, etc.) In which current procedures are being carried out. Collaboration may also have implications for data collection as hospitals may find external organizations that they can work with to collect communitylevel data. Additionally, partnerships with external organizations may increase access to resources that supplement the services provided by the hospital. Building active relationships with cultural brokers, traditional healers, chaplains, religious leaders and other individuals may enhance and extend the hospital’s services related to culture and language services. While collaborative efforts come with their own challenges, building partnerships that bring together the champions of culturally and linguistically appropriate care has the potential to move the entire field forward.
• Hospital should consider establishing a centralized program and committee with executive level reporting to coordinate services relating to language and culture as a part of the organization’s commitment to culture and language sensitive health care.
• Financial incentives should be created to promote, develop and maintain accessibility to qualified health care interpreters/translators.
• Hospital should prepare diet menu based on the client’s needs and medical indication with follow up.
• Hospital should have its own professional interpreters or translators to facilitate communication and have trusted quality of data.
• Hospital need to determine practical ways of integrating patient demographic data such as race, ethnicity and primary language into information systems.
• Hospital staff should be provided ongoing in-service training on ways to meet the unique needs of their patient population, including regular in-services on how and when to access language services for patients, especially with limited Amharic and Afan Oromo proficiency.
• Accrediting bodies should require continuing education and training that supports the provision of culturally and linguistically appropriate care.
• Research is needed to measure and understand the benefits of increased racial, ethnic and linguistic concordance of hospital workforces and their patient populations.
• Hospital should formalize their processes for translating patient education materials, including patient rights and informed consent documents, into languages used by its patient in addition to Amharic and Afan Oromo and evaluating the quality of these translations.
• Hospital should build active relationships cultural brokers, traditional healers, chaplains, religious leaders and other individuals may enhance and extend the hospital’s existing culture and language services.
• Hospital should implement policies that do not permit the use of family members, particularly minors, for interpreting during medical encounters, except in the case of an emergency when no other option is available.
• Ministry of health should have dialogue with hospitals on how to allocate diverse health care professional as real situation of hospitals need considering culture and language of the community.
• Hospital should consider partnering with local ethnic media to promote better understanding of available hospital services and appropriate routes for accessing care among all community members.
• Patients should aware their right to appropriately ask for their culture and language need to get their specific cultural and language appropriate services.
We would like to thank the followings for their contribution: Jimma University, College Health Sciences, for providing us ethical clearance; Jimma University specialized hospital, our data collectors, Study participants and others who participated directly or indirectly in this study.
Mr. Mesfin Beharu wrote the proposal, participated in data collection, analyzed the data and drafted the paper, Israel Bekele, Mr. Zewdie Birhanu and Mr. Ibrahim Yimam approved the proposal, participated in data analysis and revised subsequent draft of the paper. All authors read and approved the final manuscript.