Keywords
cultural diversity, educational models,
medical undergraduate
Introduction
The publication in 1993 of Tomorrow’s Doctors by the
General Medical Council (GMC) placed cultural diversity
on undergraduate medical school curricula in
theUK, although the relevance of the subject tomedical
students had been raised some years previously. In the
mid-1980s, a questionnaire postal survey of deans of
English medical schools found that all of the 18
respondents (out of a possible 23) reported that their
schools gave no specific teaching on the cultural aspects
of ethnic minority medicine (Poulton et al, 1986). A
decade later a survey of postgraduate and undergraduate
medical education institutions conducted by the British Medical Association found that little
had changed (Robins, 1995).
Another decade later and there appears to have been
some progress, in that 72% of schools now report
some teaching of cultural diversity (Dogra et al, 2005).
However, the number of respondents reporting that
their school is teaching the subject compares less
favourably with the USA (Flores et al, 2000), albeit
more favourably than with Canada (Azad et al, 2002).
There appeared to be a great deal of uncertainty about
what constituted cultural diversity teaching.
The use of the term culture in this paper is broadly
consistent with the perspective on the concept of
culture adopted by the Association of American Medical
Colleges (AAMC) Task Force (1999) which stated
that:
Culture is defined by each person in relationship to the
group or groups with whom he or she identifies. An
individual’s cultural identity may be based on heritage
as well as individual circumstances and personal choice.
Cultural identity may be affected by such factors as race,
ethnicity, age, language, country of origin, acculturation,
sexual orientation, gender, socioeconomic status, religious/
spiritual beliefs, physical abilities and occupation,
among others. These factors may impact behaviors such
as communication styles, diet preferences, health beliefs,
family roles, lifestyle, rituals and decision-making processes.
All of these beliefs and practices, in turn can influence
how patients and health care professionals perceive
health and illness and how they interact with one another.
(AAMC, 1999, p. 25)
Cultural diversity is taken to mean diversity of different
cultures based on how an individual defines him/
herself based on the idea that Frosh (1999, p. 413)
described. He stated the view that identity draws from
culture but is not simply formed by it.
Educational models
Some of the difficulties in establishing cultural diversity
teaching may be related to a lack of coherent
educational models for the topic (Dogra, 2004). The
usefulness of considering a number of different models
is that they highlight potential problems with all
approaches, especially when there is a lack of coherence
between educational philosophy, course design,
delivery and learning outcomes. A selection of models
is therefore discussed below.
The LEARN model
Berlin and Fowkes (1983) developed a teaching model
that focused on a process for improving communication,
which they felt is central to effective crosscultural
interactions between patients and physicians.
Although their model does not emphasise dissemination
of cultural information, they did perceive this
to be helpful. They named their model LEARN:
• Listen with sympathy and understanding to the
patient’s perception of the problem
• Explain your perceptions of the problem and
strategy for treatment
• Acknowledge and discuss the differences and similarities
between these perceptions
• Recommend treatment while remembering the
patient’s cultural parameters
•. Negotiate treatment.
This model does not expressly address the ways in
which doctors’ biases and influences may affect how
they hear and respond to what their patients are telling
them, or the value they place on what their patients say.
The transcultural nursing model
Leininger’s (1991) transcultural nursing model is
rooted in anthropology and focuses on comparing
and contrasting cultural values, beliefs and practices
about health and illness, with the aim of providing
culturally appropriate care through culture care preservation
– working within the patient’s frame of reference;
culture care accommodation – helping people to
cope with health changes within their cultural framework;
culture care repatterning – helping people cope
with imposed changes (Leininger and McFarland,
2002). It is very similar to the cultural competence
model in the way that culture is used and ethnicity
defined (Cross et al, 1989). In the USA, nurses and
nurse educators have begun to express dissatisfaction
with Leininger’s model and challenge it. One such
example is Duffy (2001), who proposes a new transformative,
post-modern approach to cultural education.
This requires greater critical self-reflection
and an acknowledgement of the self. Duffy (2001)
did not comment on whether the suggested changes
would be sufficient to meet the educational needs of
future healthcare providers.
Cultural safety model
As described by Polaschek, culturally safe nursing
practice involves ‘actions which recognise, respect
and nurture the unique cultural identity of the Tangata
Whenua and safely meet their needs, expectations and
rights’ (Polaschek, 1998, p. 453). This model acknowledges
the need to recognise negative attitudes towards
and stereotypes of individuals because of the ethnic
group to which they belong, but it contains the
assumption that, while all those within the ethnic
group may be diverse, their attitudes are likely to be
similar. Polaschek’s paper highlighted the fact that the
concept of cultural safety has yet to be clearly articulated
with methodological rigour by its proponents,
and it is therefore difficult to present it as a viable
alternative to other models.
The cultural humility model
Tervalon and Murray-Garcia (1998) sought to deliver
healthcare effectively and respectfully to the increasingly
diverse populations of the USA. The cultural
humility model stresses the need to define educational
and training outcomes consistent with this aim. The
authors argue that the detached mastery of a theoretically
finite body of knowledge expected by the cultural
competence model may be inappropriate for multicultural
medical education.
A systems-theoretic view
Kim (1992) presented a systems-theoretic view that
emphasises the dynamic, interactive nature of communication
between two or more individuals. Like the
relationship between the mind and the reality it
experiences, the relationship between an individual
and the environment is viewed as mutually reinforcing.
All parties involved in an encounter, and also the
social context in which the encounter takes place,
codetermine the communication outcome. Thismeans
that no single element in a multiperson communication
system can be separated out as being solely responsible
for the outcomes. Each person has his or her own
reality and tokens of significance in terms of which
new experiences are organised (Kim, 1992, p. 371).
The Papadopoulos, Tilki and Taylor
model
Papadopoulos et al (2004) provided a conceptual map
of a four-stage teaching process, concentrating on
cultural awareness, cultural knowledge, cultural sensitivity
and cultural competence. They argued that
attaining cultural awareness is an essential first stage in
the process of achieving cultural competence.
The study
Weber’s construct of ideal types (Giddens, 1971;
Morrison, 1995) was used to compare two models of
teaching cultural diversity to medical undergraduates:
through cultural expertise and through cultural sensibility
(Dogra, 2003). The comparison was based on
four major areas of course development: educational
philosophy and policy; the educational process; course
content; and learning outcomes. The cultural expertise
model is founded on the belief that, through gaining
knowledge about another culture, one can become an
expert in it. This concept is used in programmes that
try to teach cultural competence. The concept of developing
cultural sensibility contains the notion not of
acquiring expertise about others, but of recognising
that we need to be aware of our perspectives and how
they affect our ability to be open to other perspectives.
Sensibility may be defined as openness to emotional
impressions, susceptibility and sensitiveness. It relates
to a person’s moral, emotional or aesthetic ideas or
standards. Cultural sensitivity is not the same as cultural
sensibility. Sensitivity is more limited than sensibility,
and does not take into account the latter’s
interactional nature. If one is open to outside experience,
one is more likely to reflect on and change
because of that experience.
Transparency and clarity about the philosophy
of a teaching programme inform its organisation,
content and outcomes (Dogra, 2003). However,
such transparency requires that those developing a programme are aware of their own biases. It is evident
that models of diversity teaching such as those outlined
above do not always present a clear rationale for
the organisation of cultural diversity teaching. It is not
yet clear how models are being utilised and how awareness
of them influences the organisation of cultural
diversity teaching. This report is part of a PhD thesis
(Dogra, 2004) on the views held by key stakeholders in
medical education on the teaching and learning of
cultural diversity. This paper reports specifically on
the place of cultural diversity in the undergraduate
curriculum and how the curriculum might be organised.
Method
Devising the interview schedule
A qualitative approach informed the development of
a semi-structured interview schedule (Strah, 2000).
This schedule drew on the literature base in sociology,
medical education, education and intercultural studies
(Dogra, 2004); previous research (Dogra, 2001; Dogra
and Karnik, 2003); clinical, educational and personal
experience; earlier interviews with members of the
GMC Education Committee responsible for the first
edition of Tomorrow’s Doctors; and an internet search
of all UK medical school websites. After an introduction,
each interview was conducted in three parts.
• Part 1 collected basic demographic data (age and
sex), as well as roles and experience.
• Part 2 began with four open-ended questions and
respondents talked unprompted, with the interviewer
clarifying if necessary. The four questions
were:
1 howdoyouunderstand the term cultural diversity?
2 what do you think should be taught at undergraduate
level about cultural diversity?
3 what main topics do you think cultural diversity
teaching should encompass at undergraduate
level?
4 how do you think cultural diversity should be
taught?
• The interview then continued open-ended but
focused on specific aspects of teaching such as learning
outcomes, delivery methods, assessment, and
influence on clinical practice and student perspectives.
• Part 3 asked for theways inwhich respondents used
or understood key terms such as race, ethnicity and
multiculturalism.
Each interview concluded by asking respondents
about their experience and/or training in cultural
diversity.
The interview was piloted with two policymakers
and one diversity teacher, after which minor modifications
were made to the schedule. A flexible design
was used when delivering the interviews, allowing
modifications as part of the research process (Strah,
2000).
The interview schedule is available from the author
on request.
Sample and sample size
The samples of participants in this study were selected
to represent the diversity and variety of stakeholders,
within certain parameters generated from the literature,
and in line with the aims of the research. Those
interviewed were not representative or presumed to be
representative of their group, but in most cases they
were key informants within their group and often to
other stakeholders outside their group. This sample
was not a representative sample of various groups:
demographic attributes such as race, age, sex, socioeconomic
status and the like were not applied to the
sample selected. The professional status, job title or
role was the characteristic used to identify the sample.
The sample was not random in that key individuals
were targeted. Using a broad range of stakeholders
with different priorities means that various perspectives
were explored.
There were two stages of sampling. The first sampled
different groups of stakeholders; the second sampled
different individuals from these groups. In this study,
units that could be sampled consisted of different
groups of stakeholders. Within the main groups, there
was also overlap: for example, policymakers may also
be medical educationalists, be practising clinicians or
work in patient forums. The sampling strategy ensured
that interviews continued until saturationwas achieved.
Box 1 shows the groups sampled. There were no exclusion
criteria.
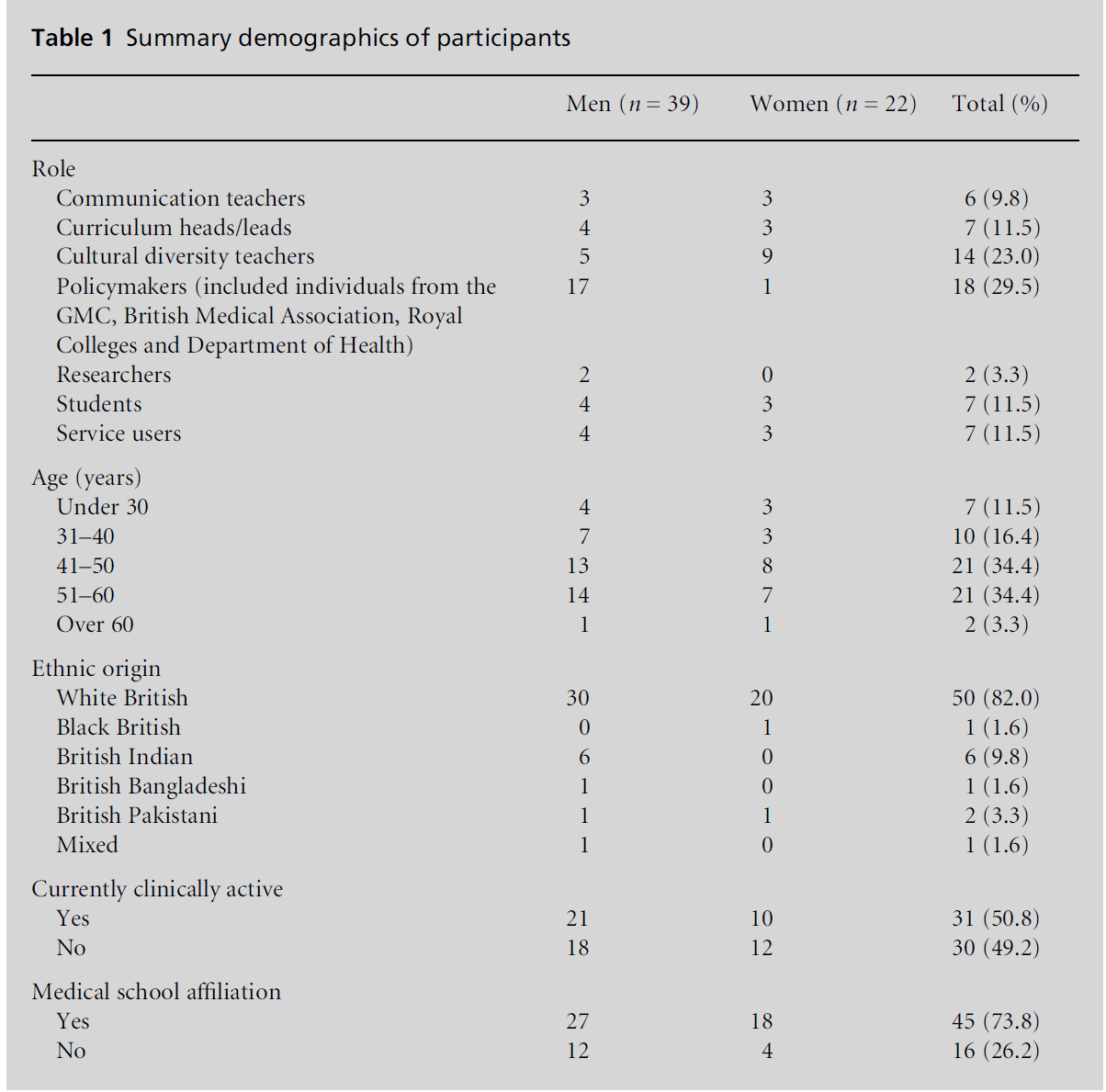
Using sampling and snowballing, a total of 61 individuals
were recruited and interviewed. Table 1 provides
some basic demographic information on the
participants. Formal association with a medical school
was defined as being employed by the medical school
(including clinical NHS staff appointed as honorary
teachers and external examiners), or being a student
at a UK medical school. Individuals from 14 of the 26
established medical schools in the UK were involved
(two schools have campuses at two sites; therefore, 12
curricula were effectively covered). Members from 11
policy-making organisations and six medical disciplines
were interviewed. Other clinical perspectives
included pharmacy, social work, community youth
work and nursing. Non-clinical participants came
from sociology, anthropology, accountancy, research
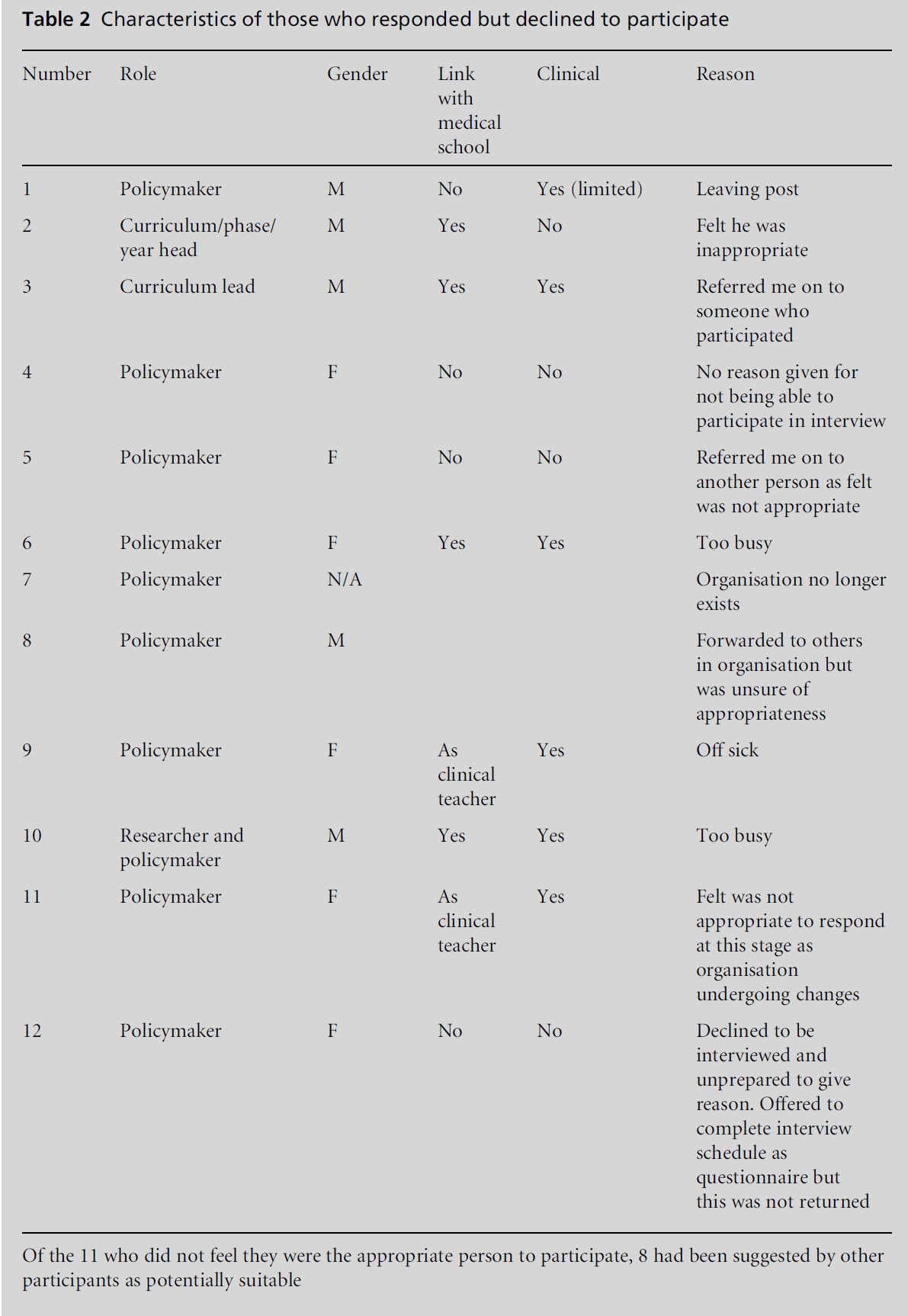
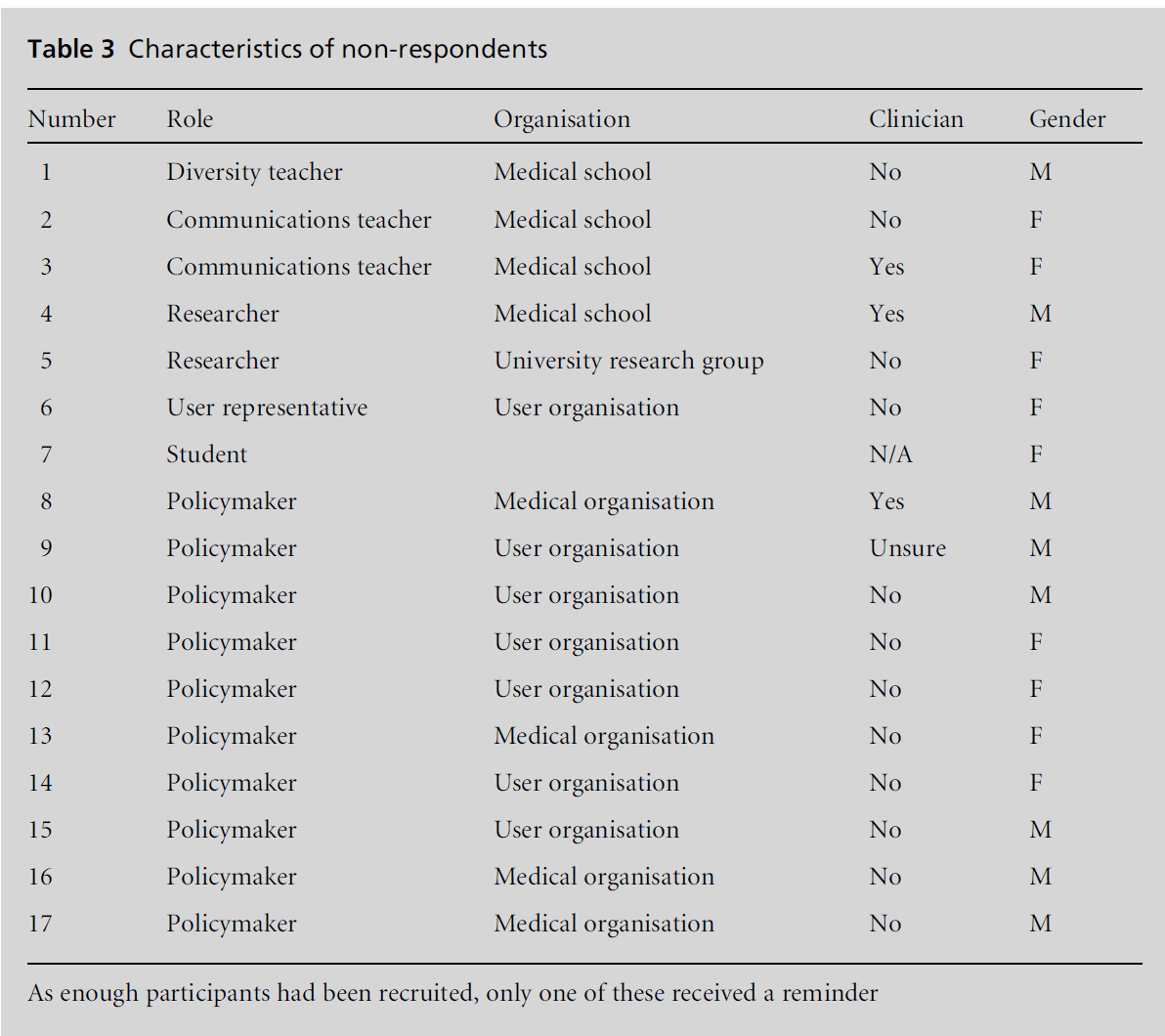
and advocacy work. Table 2 shows those individuals who responded but did not participate and Table 3
provides some data on non-respondents. Policymakers
were the most likely to not respond.
Procedure
Interviews lasted about an hour and were conducted
face to face where possible, or alternatively by telephone.
Initial contact was made in a formal introductory
letter outlining the purpose of the research and inviting
participation in it. The letter also stated that the
interviews would be confidential and that the local
research NHS ethics committee had approved the
project. If there was no response, the initial letter
was followed up by email or by a second letter until the target number was achieved. No onewas contacted
more than twice if they failed to respond. Most of
those who agreed to take part did so by letter or email;
copies of this correspondence were kept, making
written consent forms unnecessary. Interviews were
audiotaped and transcribed verbatim.
Table 1: Summary demographics of participants
The researcher’s part in the research
and interview process
This research was undertaken by a female, of Indian
origin, aged 40 years, brought up and educated in the
UK, who works as a senior clinical academic in child
and adolescent psychiatry at an East Midlands medical
school. Having undertaken the development of a
module in cultural diversity, she had some professional
familiarity and experience with the topic. As Robson (2002) has highlighted, all these factors
may influence the research.
Analysis
Qualitative thematic analysis was undertaken (Joffe
and Yardley, 2004) and followed a series of systematic
steps outlined by Miles and Huberman (1994). There
was also some frequency coding of responses to enable
comparison between groups (Seale, 1999). The content
of the interviews was analysed to identify word and
phrase frequencies and intercorrelations. Themes were
identified by the author and discussed with the project
supervisor to facilitate reliability. The categories were
compared across scripts to develop ideas beyond description.
Qualitative research provides a deeper understanding
of the social processes and is data driven rather than hypothesis driven (Silverman, 2001). Consequently,
further themes emerged as the data were
coded. These were then combined and sorted into
meaningful areas. Key themes were identified from
the transcripts as a whole and from collations of
responses to specific themes. Key themes were
categorised under the origins, organisation, content,
delivery and outcomes of the curriculum. The justification
for thiswas the need to relate findings to existing
theory. The themes for the organisation of cultural
diversity teaching were organised under the headings
when, where and how such teaching might take place.
Table 2: Characteristics of those who responded but declined to participate.
Table 3: Characteristics of non-respondents.
Findings
The key findings for each area are summarised in Box 2.
Introducing cultural diversity teaching
into the curriculum
The organisation of a curriculum is about implementing
policies that relate to the subject in question,
and one policymaker raised the issue of a national
curriculum to ensure consistency of teaching programmes:
‘This is one of the questions of course, why don’t we have a
core curriculum, nationally for undergraduate medicine?’
(Policymaker)
The issue of a national curriculumis a difficult one for
the GMC, because so many individuals and organisations
need to be satisfied with the final document.
However, the GMC may be missing a key opportunity
to lead and support medical schools in an area that has
proven difficult to address.
While most respondents were committed to cultural
diversity teaching in the curriculum, the idea that it is
always welcomed was challenged:
‘One question is how much sort of resistance is there to
embracing this really, either within a medical school curriculum
... [ND: ‘‘Sorry, how much resistance is there to ... ?’’]
Howmuch resistance is there, either students or staff to sort
of, resistance is perhaps too strong aword, howmuch either
hostility or negativismis there in bringing, confronting these
issues [cultural diversity], bringing it into the curriculum
and howmuch again is it viewed negativelywithin thewider
health community itself.’ (Communication teacher)
Staff not directly involved in cultural diversity teaching
tended to be unaware of teaching in this area, even
within their own medical school. This is perhaps not
specific to cultural diversity but is highly relevant, especially if the aim of integration of diversity into
clinical practice is to be achieved.
Where in the curriculum should
cultural diversity be taught?
There was genuine enthusiasm among respondents
for cultural diversity to be part of the curriculum for
undergraduate medical education and no one felt that
it should be an optional component. The widespread
acceptance of the view that the social sciences are just
common sense has meant that curricula merely accommodate
social science topics rather than challenge
this view. It is possible that senior medical staff and
faculty members deliberately or inadvertently collude
with students in this:
‘I know it’s quite interesting how, it started off with social
class in medical education and then the psychologists felt
left out ... It’s interesting how often they [psychology and
sociology] cover the same ground in different medical
schools. Some people would argue quite strongly that you
have to bring them together, that you can’t just teach or
use them in isolation of one another.’ (Diversity teacher)
There was little consensus on where in the curriculum
cultural diversity might be taught.
Modular or integrated teaching?
When asked whether cultural diversity (meaning
diversity associated with ethnicity or race) should be
taught separately from other aspects of diversity or
with them, the majority of participants (45) felt that all
aspects should be taught together. Only five thought
that it should be taught separately. The students among
these respondents said that this was mostly for practical
reasons. The justification of one of the policymakers
was that it is a current (political) agenda.
Several participants said that cultural diversity needs
to be addressed regularly in clinical sections of the
course in a way that is consistent with preclinical
teaching.
One of the justifications for teaching all aspects of
diversity together was:
‘My fear is that if you just do it discretely, which is actually
what we are doing now, it kind of, it gets sort of compartmentalised.
I mean people are pleased that we are doing
this, I’m sure they are with you, but this is, ‘‘Oh well,
they’re doing this there, so that’s fine’’, sort of ‘‘been
there, done that’’. We are trying for it to be a core and that
it goes right the way through, as far as curriculum, all the
way through.’ (Diversity teacher)
Three participants favoured combined teaching for
practical reasons, for example:
‘I think they should probably be taught together and I say
that partly because of the very constrained time we have got in the curriculum. I suspect it would be unlikely we
would find time to teach them individually, plus the fact I
think there are so many common themes running through
it, because it’s about how you relate to people who might
not be the same as you in one of theways.’ (Curriculumlead)
Others supported it for educational reasons:
‘I’m cautious about this but I think there probably is a
generic attitudinal thing about diversity. I might be
wrong, because we know that so many other skills like
problem solving, for example, that everybody had hoped
was generic is actually very context specific. You might be
fantastically open minded and reflective about working
with people from an ethnic minority background and
whatever, but homophobia might be your particular issue
and you just can’t handle working with gay people. I think
it has to be the individual issues, the individual ’isms, have
to be addressed separately but against a foundation of
being reflective about it.’ (Diversity teacher)
A communication teacher felt that although cultural
diversity issues should be an integral part of the curriculum
there is a high risk that they would not be
taught if not covered in a dedicated module:
‘Within each culture there are going to be different priorities,
so I think what you are going to tease out, by experience,
experiential process, you are going to learn about
what are the key things about each of those cultures. I
think there should be, rather than just doing a practical
exercise, there should be some basic lecture format to
support it.’ (Communication teacher)
This response indicates a cultural expertise approach,
with each ‘culture’ being fairly homogeneous and its
members sharing similar needs.
One student was in favour of integration of diversity
teaching because:
‘I think to create a module say of cultural diversity would
be an error. A lot of universities have gone down a route
like this and have had behavioural sciences. What you’ve
got to do is fit them in where appropriate. So you could be
teaching genito-urinary medicine and you could include
in that a lecture on gender and sexuality issues and that
wouldn’t need to be taught in a module of behavioural
science. It would then be very relevant. Likewise for
ethnicity, like if you were doing diabetes, then you could
include cultural differences in the Asian population that
would be related to that.’ (Student)
This is again consistent with the cultural expertise
model, in that it presupposes that sexuality issues are
relevant only in a single context, when they could
easily feature in other contexts, such as diabetes. The
consensus was that cultural diversity is not the province
of any specific discipline and that it should be
taught throughout the curriculum, rather than just as
a separate module. It was less clear how this might
happen in practice. Policymakers, students and service
users were less likely than the other groups of respondents
to say that the teaching should be integrated.
When should cultural diversity be
taught?
The question ‘At which stage of the medical student’s
career should the teaching take place?’ elicited a fairly
consistent response, although justifications varied.
Fifty of the 61 respondents said that diversity teaching
should begin in year one and continue throughout
training. Three respondents felt that the teaching
should take place before students have contact with
patients, which would determine when it might begin.
Communication teachers, curriculum heads and
diversity teachers talked about diversity teaching (with
or without a professional and personal development
component) in terms of the weave of a fabric, by
running vertically throughout the years of medical
education and horizontally across the modules of the
curriculum. Justifications for early inclusion included:
‘Certainly within the first term. Just that it’s an underpinning
principle really. That medicine is about people,
not about bodies.’ (Service user)
The point that medicine is about people is an important
one. As most medical students spend a significant
part of their first year of medical school in anatomy
laboratories they mightwell feel that medicine is about
inanimate objects, rather than human beings. Diversity
teaching at this stage might remind them that they
will be dealing with living people. One policymaker
guarded against introducing diversity teaching too
early without preparing students adequately:
‘I just think that doing everything right at the beginning
isn’t always great. So I think that in a sense it should be
there anyway, I mean it should be imbued in the teaching,
the construction of teaching materials should be informed
by an awareness of the diversity of the population that you
are considering ... I think students sometimes find it very
difficult to really engage with some of the ethical things
that we try to teach them early on before they understand
the doctor/patient contract and what medical care is all
about.’ (Policymaker)
Eight respondents wanted to introduce the subject
early to influence students more strongly:
‘I think to reinforce that, at the beginning, that those are
the right values to have and to build on those and to learn
from those being taught as well.’ (Service user)
This and other comments indicate a belief that there is
a ‘right’ view or value. If this is stated at the outset, it
may inhibit students from exploring their own beliefs.
While there was consensus that cultural diversity
should be taught early and should be integrated into
the curriculum, the reasons for this were variable and
there was little detail on how it might be achieved.
Although the majority of respondents had a philosophy
for teaching cultural diversity more consistent
with the cultural expertise model, the organisation of cultural diversity teaching by integrating it into the
curriculum is more consistent with the cultural sensibility
model.
There were three main reasons for supporting early
learning in diversity: to prepare students appropriately
for clinical training, to get in early and challenge
them before they became ‘medicalised’, and tomaximise
learning opportunities. No one touched on whether or
not any evidence is available to determine when such
teaching is likely to have the greatest effect, although
most thought that it should continue throughout the
curriculum. Policymakers, students and service users
did not mention integration as explicitly as respondents
fromthe other groups, perhaps because they are
less aware of different types of curricula and methods
of delivering educational objectives. The GMC is
certainly less clear on how the curriculum should be
delivered than on what it should contain (GMC, 1993;
2002).
How much time should be spent on
cultural diversity?
The question of the amount of time that needs to be
spent in this area was relatively difficult for many
respondents and there was no consistent response.
Some drew comparisons with other parts of the
curriculum to suggest the number of hours. For
some respondents, the amount of time spent did not
matter as long as the learning outcomes were met.
‘I think one has to look at the rest of the curriculum and
put it into proportion, as well as teaching it. What we
should be [doing] is reinforcing it all the way through
so that it may be that you only have a small amount of
the curriculum devoted to it because if you then keep
reinforcing that, you don’t need to keep teaching it again
as a separate subject.’ (Curriculum head)
Those who had struggled to get their own clinical
disciplines onto the curriculum were more forward in
suggesting a specific number of hours:
‘I suppose I find that a very difficult question to answer
because I think there are so many constraints on the
curriculum. When I think of stuff, for example my subject
area, and how little time they have for that, I would say at
least 20 to 30 hours [of formal contact teaching time].’
(Communication teacher)
A respondent having difficulty in answering the question
made the following response after prompting:
‘I think cumulatively it’s got to be much more than 12 hours,
but then again I don’t want to give the impression that
somehow, we are so bad at this that somehowwe have got to
have this huge onslaught. But actually 12 hours in the
totality of 5 years’ training is a drop in the bucket still compared
towhatwemight spendonother things.’ (Policymaker) There were also those who thought that notmuch time
was needed, although the justification for their belief
was unclear:
‘Probably not that much time ...’ (Student)
This respondent generally had a very cultural expertise
approach, in that she thought cultural diversity teaching
would largely involve learning information about
groups, and she may not have considered that much
time is needed to impart factual information. Another
student felt that cultural diversity would be more
demanding thanmany of the other learning experiences
if it was addressed appropriately. He felt that learning
time should include opportunities for reflection, demonstrating
a higher-level approach to learning:
‘I would have a week of lectures, seminars and group
work, so each day would be a normal, sort of phase-one
style medical school day, maybe 6 hours’ teaching at the
most. I actually think a lot of these issues are much more
draining to deal with than a lot of the sort of bland basic
science that you learn ... I think the way I’d teach it is
having a lot of small-group work sessions with people
coming in, and it always raises debate and debate’s hard
work.’ (Student)
This response suggests that, in practice, course design
may fit more with curriculum structure than educational
theory or evidence.
‘I think you need to have the equivalent of a module
throughout the course, basically, in the same way that you
would have a module on any of the other major issues.’
(Policymaker)
The difficulty in using a term such as module is that a
module is likely to consist of different amounts of time
in each school. Perhaps the message to be taken from
this is that diversity teaching warrants a significant
block of time, rather than being an add-on or afterthought.
There were also concerns about achieving an overall
balance and how this might be done:
‘This is a hugely controversial issue at the moment.
Certainly some of my colleagues think there’s far too
much time in the curriculum already devoted to this ...
But there is criticism that Tomorrow’s Doctors has kind of
swung almost too far away from clinical knowledge.’
(Diversity teacher)
There were concerns that the subject should not be
‘overdone’, as students would then just become bored.
‘Formal teaching, probably it would be appropriate in
every year of the course, a teaching session, just to remind
them. You don’t want to do it to death because the
students will switch off then ... We are expecting the staff
who are teaching in clinical situations to be aware of the
cultural issues as well as the formal teaching.’ (Curriculum
head)
There was, perhaps not unsurprisingly, little consensus
on the time that should be spent on cultural
diversity.
Discussion
One hypothesis was that cultural diversity would
be taught systematically, but this was challenged
significantly by the review of the literature and the
interviews. There were many individual differences in
approaching cultural diversity and its introduction
into the curriculum. In the interviews, few based their
ideasonclear theoretical underpinnings.Many acknowledged
the complexity of this area and the absence of
clear definitions of the terminology involved.
Medical curricula have developed in an ad hoc
fashion (Dennick, 1998). Anything that does not firmly
belong to the physical sciences continues to be attributed
to the behavioural sciences. This means that
psychology and sociology may be taught as one block,
without enough regard for the distinct approaches of
these disciplines (Dogra and Karnik, 2004). Cultural
diversity teaching is in limbo – on the one hand it is not
thought simply to be part of the behavioural sciences,
but on the other that is where it is mostly taught.
Through this placement, cultural diversity becomes
associated with the lower status of the behavioural
sciences in medicine. This was certainly reflected in
the responses given.
Some medical schools were clearly finding it difficult
to identify exactly where and when cultural diversity
should be taught in an integrated curriculum. As
there was considerable confusion about where cultural
diversity should be taught, it is unsurprising that the
organisation of cultural diversity teaching was unsystematic.
The lack of a systematic approach to the
introduction of cultural diversity into the curriculum
is a recurrent theme in interviewees’ responses.
Before a subject can be integrated successfully into
a curriculum, there needs to be clarity about what is
being taught and an understanding of its relevance to
the curriculum as awhole. There is no evidence to date
that cultural diversity has achieved this position. No
one in the interviews raised the issue that, if cultural
diversity were not taught separately, students might
not realise that it was being taught; nor did anyone
advocating integrated teaching comment on the need
to ensure that students are aware that it is being
taught. This is perhaps particularly important in light
of a recent finding by Wachtler and Troein (2003) that
students often miss the hidden curriculum.
Whether diversity teaching is integrated or not,
there may be a need to be transparent about its inclusion.
Those developing problem-based programmes
may assume they have addressed such issues, but deeper examination shows this is often not the case
(Turbes et al, 2002). One teacher had reservations
about whether their problem-based learning course
covered cultural diversity at all, and if it did, that itwas
being addressed only superficially. It was clear from
the interviews that, on the whole, cultural diversity
teaching is not yet integrated into medical school
curricula, either vertically through the years or horizontally
across different modules, although there are
programmes that aim to develop this, especially within
professional personal development (Dogra et al, 2005).
Many accepted that it should be an integral part of
clinical practice. Pragmatically, however, participants
thought that if not addressed as a separate issue, it is
unlikely to be taught. Until there is a clearer educational
framework, it is unlikely that the place of cultural
diversity teaching can be clarified. Until that has
been addressed, it is difficult to see how the teaching
can become systematic and proactive rather than a
reaction to political pressures. This would perhaps
suggest that specific teaching on cultural diversity is
required irrespective of whether it is integrated into
other teaching.
Time spent on cultural diversity teaching in reported
programmes ranges from as little as one 90-
minute seminar (e.g. Sifri et al, 2001) to 20 2- or 3-hour
sessions (Crandall et al, 2003), which reflects the
widely ranging views shown above. Participants in
this study felt that student attention and time might be
better guaranteed by ensuring that such issues had a
place in high-stake examinations. There was also the
pragmatic approach that one has to work with whatever
the conditions are, and it is easier to start and then
improve a course rather than waiting for a perfect
course to be developed before implementation. Most
participants, however, believed that cultural diversity
should be part of the core curriculum and that it
warrants more than a one-off teaching slot or being
taught as an add-on to other modules, suggesting it
needs more priority than it currently has.
The findings suggest that medical schools and
perhaps also other institutions may benefit from
reviewing their cultural diversity teaching and reflecting
on whether it is organised in an educationally
coherent way. Teachers establishing new courses may
want to consider how they organise their teaching.
A limitation of this study is that some staff not
involved in cultural diversity but involved in medical
education, who do not value diversity,were unlikely to
be identified or participate. The ‘right’ people may not
have been selected. Given that interviews rely on the
relationship established between the researcher and
the participants, there is always the limitation that the
research can be contaminated by the characteristics of
the researcher. As the policymaker group is perhaps
the most influential and fairly broad, more members
of this group were invited to participate than from other groups and their views may be over-represented.
However, their views were not dissimilar to the range
of views of other groups.
Conclusion
Although the respondents were enthusiastic about the
inclusion of cultural diversity in the curriculum, some
felt that they did not necessarily reflect the views of
others within medical schools. There was a consensus
that cultural diversity needs to be taught early and
most felt that it should incorporate more than just
ethnicity.Most felt that it should be integrated into all
aspects of the curriculum. There is no evidence to
suggest that existing approaches to the development of
cultural diversity teaching have been systematic. This
has created a mismatch between what is actually happening
and what respondents felt should be happening.
The fact that cultural diversity teaching has been
indicated by the GMC, but without implementation
guidelines, has resulted in an unsystematic approach
to its inclusion in medical school curricula. Thismeans
that the place and organisation of cultural diversity
teaching in the medical curriculum remain unclear
and variable, and the subject appears to lack credibility
with faculty and students. There is clear consensus
among stakeholders regarding how the subject should
be taught, although methods are mostly unsupported
by any theoretical framework. It is promising that
cultural diversity teaching is on the educational agenda.
However, there is a need to develop diversity education
within a coherent educational framework that
will make it clear where and why it is being taught.
ACKNOWLEDGEMENTS
ND conducted the study, analysed the data and wrote
the paper. She would like to acknowledge the support
of the University of Leicester through a semester’s
sabbatical to complete her PhD and also all those who
participated in the study. Thanks are also due to her
PhD supervisor Dr Nick Jewson. She would also like to
acknowledge the contribution of Lynette Maddock
who helped with some editorial support. The reviewer
comments were also most helpful.
References
- Association of American Medical Colleges (1999) Report III Contemporary Issues in Medicine. Communication in medicine: spirituality, cultural issues and end of life care. Medical School Objectives Project. Washington: Association of American Medical Colleges.
- Azad N, Power B, Dollin J and Chery S (2002) Cultural sensitivity training in Canadian medical schools. Academic Medicine 77:222–8.
- Berlin EA and Fowkes WC Jr (1983) A teaching framework for cross-cultural health care: application in family practice. Western Journal of Medicine 139:934–8.
- Betancourt J (2003) Cross-cultural medical education: conceptual approaches and frameworks for evaluation. Academic Medicine 78:560–9.
- Crandall SJ, George G, Marion GS and Davis S (2003) Applying theory to the design of cultural competency training for medical students: a case study. Academic Medicine 78:588–94.
- Cross T, Bazron B, Dennis KW and Isaacs MR (1989) Towards a Culturally Competent System of Care, Volume 1. Washington DC: Georgetown University Child Development Center, CASSP Technical Assistance Center.
- Dennick R (1998) The Teaching Improvement Project. Nottingham: The University of Nottingham.
- Dogra N (2001) The development and evaluation of a programme to teach cultural diversity to medical undergraduate students. Medical Education 35:232–41.
- DograN(2003) Cultural competence or cultural sensibility? A comparison of two ideal type models to teach cultural diversity to medical students. International Journal of Medicine 5:223–31.
- Dogra N (2004) The Learning and Teaching of Cultural Diversity in Undergraduate Medical Education in the UK. PhD thesis. Leicester: University of Leicester.
- Dogra N and Karnik N (2003) First-year medical students’ attitudes toward diversity and its teaching: an investigation at one US medical school. Academic Medicine 78:1–10.
- Dogra N and Karnik N (2004) Teaching cultural diversity to medical students. Medical Teacher 26:677–80.
- Dogra N, Conning S, Gill PS, Spencer J and TurnerM(2005) The learning and teaching of cultural diversity in UK and Eire Medical Schools. British Medical Journal 330:403–4.
- DuffyME(2001) A critique of cultural education in nursing. Journal of Advanced Nursing 36:487–95.
- Flores G, Gee D and Kastner B (2000) The teaching of cultural issues in US and Canadian medical schools. Academic Medicine 75:451–5.
- Frosh S (1999) Identity. In: Bullock A and Trombley S (eds) The New Fontana Dictionary of Modern Thought, 3rd edn. London: Harper Collins.
- General Medical Council (1993) Tomorrow’s Doctors. London: General Medical Council.
- General Medical Council (2002) Tomorrow’s Doctors, 2nd edn. London: General Medical Council.
- Giddens A (1971) Capitalism and Modern Social Theory: an analysis of the writings of Marx, Durkheim and Max Weber. Cambridge: Cambridge University Press.
- Kim YY (1992) Intercultural communication competence: a systems-theoretic view. In: Kavanagh KH and Kennedy PH (eds) Promoting Cultural Diversity: strategies for health care professionals.
- Newbury Park, California: Sage, p. 371. JoffeHand Yardley L (2004) Content and thematic analysis. In: Marks DF and Yardley L (eds) Research Methods for Clinical andHealth Psychology. London: Sage Publications, pp. 56–68.
- Cultural diversity teaching to medical undergraduates 245 LeiningerM(1991) Culture Care, Diversity and Universality: a theory of nursing. New York: National League for Nursing Press.
- Leininger M and McFarland M (2002) Transcultural Nursing: concepts, theories, research and practice (3e). New York: McGraw Hill. Miles MB and HubermanAM (1994) Qualitative Data Analysis: an expanded sourcebook (2e). London: Sage, pp. 56–68.
- Morrison K (1995) Marx, Durkheim, Weber: formation of modern social thought. Thousand Oaks, CA: Sage.
- Papadopoulos I, Tilki M and Lees S (2004) Promoting cultural competence in healthcare through a research-based intervention in the UK. Diversity in Health and Social Care 1:107–15.
- Polaschek NR (1998) Cultural safety: a new concept in nursing people of different ethnicities. Journal of Advanced Nursing 27:452–7.
- Poulton J, Rylance GW and Johnson MRD (1986) Medical teaching of the cultural aspects of ethnic minorities: does it exist? Medical Education 20:492–7.
- Robins S (1995) Multicultural Health Care: current practice and future policy in medical education. London: British Medical Association.
- Robson C (2002) Real World Research (2e). Oxford: Blackwell Publishers. Seale C (1999) The Quality of Qualitative Research: introducing qualitative methods. London: Sage, pp. 119–39.
- Sifri RR, Glaser K and Witt DK (2001) Addressing prejudice in medicine during a third-year family medicine clerkship. Academic Medicine 76:508.
- Silverman D (2001) Interpreting Qualitative Data: methods for analysing talk, text and interaction (2e). London: Sage. StrahM(2000) Qualitative interviewing. In: Burton D (ed.) Research Training for Social Scientists. London: Sage Publications, pp. 196–214.
- Tervalon M and Murray-Garcia J (1998) Cultural humility versus cultural competence: a critical distinction in defining physician-training outcomes in multicultural education. Journal of Health Care for the Poor and Underserved 9:117–25.
- Turbes S, Krebs E and Axtell S (2002) The hidden curriculum in multicultural medical education. Academic Medicine 77:209–16. Wachtler C and Troein M (2003) A hidden curriculum: mapping cultural competency in a medical programme. Medical Education 37:861–8.