Research Paper - (2009) Volume 17, Issue 3
Harm-Jan A Weevers MSc1 , Allard J van der Beek PhD2*, Atie van den Brink-Muinen PhD3 , Jozien Bensing MD PhD4 Ce´ cile RL Boot PhD5 Willem van Mechelen MD PhD6
2Professor of Occupational Epidemiology and Vice-Head of Department VU University Medical Center, EMGO Institute for Health and Care Research, Department of Public and Occupational Health, The Netherlands
4Professor of Clinical and Health Psychology and Director Netherlands Institute for Health Services Research (NIVEL), The Netherlands
6Professor of Occupational and Sports Medicine and Head of Department VU University Medical Center, EMGO Institute for Health and Care Research, Department of Public and Occupational Health, The Netherlands
Received date: 17 February 2009; Accepted date: 28 April 2009
Background Work-related musculoskeletal disorders (MSDs) are common in general practice. The communication between a general practitioner (GP) and patient is a key element of adequate general practice. No study has investigated the characteristics of communication about work-related matters during consultation of the GP by working patients with MSDs. Objectives The aim of this study was to describe the communication about work-related matters between the GP and his patients with paid work who are consulting for MSDs. Method Descriptive analysis of 680 systematic observations of GP consultations of patients in paid work who were consulting for MSDs. Results Work was discussed in 227 of 680 consultations in general practice. In 69% of these consultations the patient started communication concerning work-related matters, with an average number of 38.5 (standard deviation 45.7) verbal utterances, equalling, on average, 15% of the total consultation time. In 36% of consultations the patient’s working conditions were discussed and in 12% the GP advised on whether to stay at home or return to work. There was a statistically significant positive correlation between the extent to which GPs rated the patient’s MSDs to be work related and the number of utterances the GP and patient made about work-related matters during the consultation.Conclusions Work is not a standard topic of conversation during the GP consultation. GPs could more often start communication about patients’ work. A challenge for future GP practice and education is to include discussion of patients’ work to optimise patient-centred care.
communication, family practice, musculoskeletal disorders, referral and consultation, work
A large proportion of patients in general practice have paid work. Health complaints may have negative consequences for functioning at work, and may lead to sick leave or work disability. Factors in the workplace may be associated with musculoskeletal pain, fatigue and other health complaints.[1,2] Work disability and sick leave, in turn, may have negative consequences for existing health complaints. On the other hand, work meets important psychosocial needs, and employment is a major driver of social gradients in physical and mental health, as well as mortality.[3] To maintain or enhance participation in paid work, communication in general practice about work is an essential first step and therefore of major importance.[4,5] Discussing the patient’s work fits well within a patient-centered approach and contributes to a good therapeutic relationship. [6–10]
Some disorders are caused bywork, and these workrelated disorders form a separate category in general practice. The prevalence of work-related disorders in general practice is high.[11] The general practitioner (GP) has an important role in identifying and managing work-related disorders.[12–14] In many healthcare systems the GP is the first point of diagnosis of a workrelated disorder.
For the treatment of disorders and health complaints that may have consequences for functioning at work and the management of return to work, it is important that the GP is informed about the patient’s occupation and working conditions.[15] The understanding of working conditions and the reciprocal relationship between work and disease can be improved by the GP through instrumental and ‘affective’ communication with the patient.[14,16] Affective communication between the GP and the patient about work can also be important to improve interpersonal interaction. [15,17] Communication about issues related to disease, such as the patient’s work, gives the patients the feeling that they are being treated as a human being and not as a disease in itself.[18] Including the patient’s work as a topic in GPs’ practice and education would be beneficial for patient care.
Musculoskeletal disorders (MSDs) are the most common category of health problems related to work seen in general practice.[11] Low back pain is a major health problem within this category.[19] The one-year incidence of consulting a GP for low back pain varies between 3.8% and 7.0%.20–22 Work-related factors have been shown to be important prognostic indicators in back pain, and recent guidelines recommend that the primary care management of this condition includes advice to stay at work or return to work as soon as possible.3 Thus, the role of the GP in prevention and treatment of MSDs is very important.
The extent to which the GP classifies the patient’s MSDs as work related may be associated with characteristics of communication concerning work-related matters. It is hypothesised that the GP’s judgement on the work-relatedness of MSDs is positively correlated with the number of utterances concerning workrelated matters.
The aim of this study was to gain insight into communication aboutwork between theGPand patients in paid work during consultation for musculoskeletal disorders. These insightswere obtained by describing the percentage of consultations inwhich work-relatedmatters were discussed, and the characteristics of the utterances. In addition, the study aimed to explore the extent to which GPs rated the relationship between anMSDand work with the characteristics of communication concerning work-related matters during consultation.
This was a descriptive analysis of data from the second Dutch National Survey of General Practice (DNSGP-2) of the Netherlands Institute for Health Services Research (NIVEL). The DNSGP-2 was carried out in 2001 in collaboration with the National Information Network ofGPs (LINH), a national computerised information network of general practices. The DNSGP-2 study forms a representative national sample of both GPs and patients. This study examined the taped consultations (n = 2784) of this national sample.
Videotapes of consultations were taken from GPs during a routine working day. Patients were asked to participate when they entered the waiting room. When the patient decided to participate, both the GP and the patient signed an informed consent form. Next, a small video camera with automatic settings taped the GP– patient communication, in order to maintain the reallife situation and minimise disturbance.
The characteristics of communication were systematically observed and coded into specific categories using an adapted version of the Roter Interaction Analysis System (RIAS).[23] The RIAS is a widely used method of coding doctor–patient interactions. The RIAS can be used to discriminate between instrumental (task-related) and affective (socio-emotional) verbal utterances by GPs and patients. Instrumental communication was categorised into biomedical talk and psychosocial talk. This included asking questions, and giving information and counselling about medical and therapeutic issues, such as issues of lifestyle (such as work-related matters), social context, psychosocial problems and feelings. Affective communication included social talk and personal remarks (laughter, jokes, approval), signs of agreement (such as ‘yes’, ‘hmmm’), showing empathy, legitimisation, support, concern, worry, (asking for) reassurance, encouragement, optimism and paraphrases, checks for understanding, asking for clarification, opinion, or repetition. Each statement concerning work-related matters made by either the GP or the patient was assigned to either instrumental or affective communication, which were mutually exclusive. The number of utterances was used as a proxy for consultation time. It should be mentioned that communication about work did not necessarily have to relate to the patient’s current work, since work in the past may have resulted in current MSDs.
For consultations in which work was discussed, the characteristics of communication about work were systematically observed and scored using eight questions:
1 Who started the communication on work-related matters?
2 What was the average number of utterances per consultation about work-related matters by the GP or patient?
3 How many utterances concerning work-related matters were instrumental?
4 How many utterances concerning work-related matters were affective?
5 Did the GP or the patient speak about the influence of work on the musculoskeletal disorder or musculoskeletal complaints?
6 Did the GP or the patient speak about the influence of the disorder on the work of the patient?
7 Did the GP or patient speak about the patient’s work demands or possible adaptations at the workplace?
8 Did the GP give advice about staying at home or returning to work?
After each consultation, the GP answered the following question: ‘Was there a relationship between the health complaint and the patient’s work?’ with answering categories on a five-point Likert scale: no (1), weak (2), moderate (3), quite strong (4), strong (5).
Analysis
The questions were scored with the program ‘The Observer’ (Noldus, Wageningen, The Netherlands), a manual event recorder for the collection, management and analysis of observational data.[24] Descriptive analysis was used on the observed utterances from the videotaped consultations of GPs, to describe the characteristics of communication concerning work-related matters. The association between the work-relatedness of MSDs according to the GP (range 1–5) and the communication about work (total number of utterances about work per consultation) was explored using a correlation coefficient (Spearman’s rho). All analyses were performed using SPSS for Windows.
Population
In this study, 77% of GPs were male, 23% female. Furthermore, 26% of GPs had a solo practice and 74% were in duo- or group practice. From all taped consultations (n = 2784), patients with paid work were selected, which left 1773 (64%) videotapes. Next, patients consulting the GP for MSDs were selected, which resulted in 680 (38%) videotapes. These videotapes of 680 different patients were observed and analysed in depth if ‘work’ was mentioned during the consultation. The selection process is presented in Figure 1.
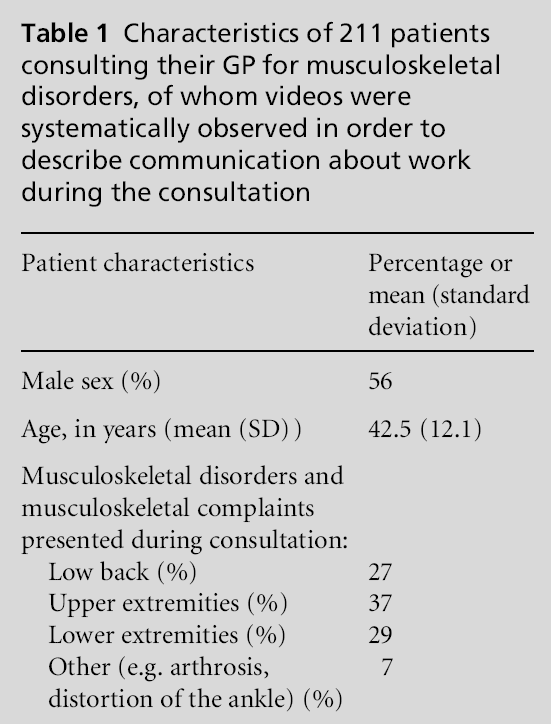
In 33% (227/680) of consultations, the work of the patient with a MSD was discussed. Of the 227 videotapes analysed, 16 (7%) had to be excluded due to misclassification (e.g. the patient appeared to have unpaid work or to have retired early), which left 211 videotapes. The average duration of the consultations was 11.4 minutes (standard deviation (SD): 4.5 minutes). Patient characteristics are presented in Table 1. The distribution of different verbal utterances of communication about work was similar to the distribution of verbal utterances in the total communication within the DNSGP-2.
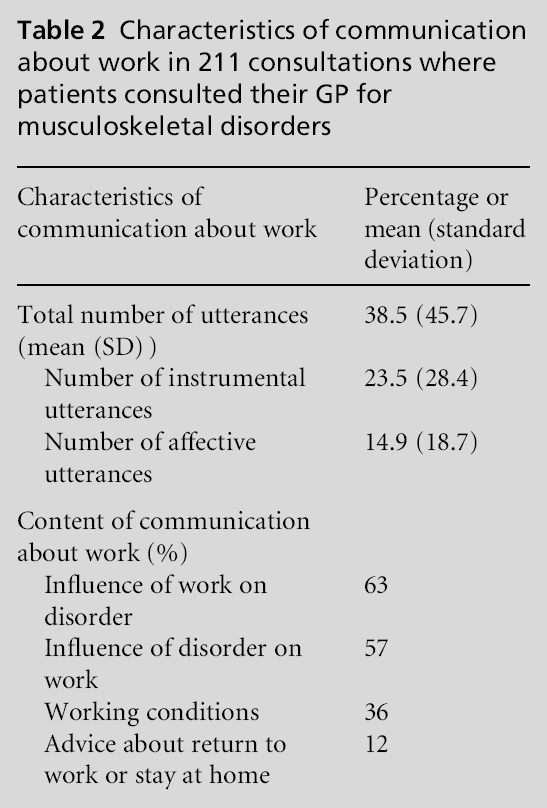
The patient started communication concerning workrelated matters in 69% of these 211 consultations (see Figure 1). These work-related matters were discussed with an average total number of utterances per consultation of 38.5 (SD 45.7). This number of utterances constituted on average 15% of the total consultation time, meaning a total duration of 1.7 minutes. Table 2 shows that the average number of instrumental utterances was 23.5 (SD 28.4), and the average number of affective utterances was 14.9 (SD 18.7). In 63% of the consultations in which ‘work’ was mentioned, the influence of work on the disorder was discussed. In 57% of the consultations the influence of the disorder on the patient’s work was discussed, and in 36% the working conditions. In 12% of the consultations the GP gave advice to stay at home or return to work.
There was a statistically significant positive correlation between the extent to which GPs rated the patient’s MSD to be work related (range 1–5) and the total number of utterances the GP and patient made about work-related matters during consultation (Spearman’s rho = 0.43, degrees of freedom (df) = 160, P < 0.001).
This study showed that in one-third of the consultations for patients with paid work consulting for MSDs, the topic of work was discussed by the GP and patient. Most often, the patient started the conversation about work. If work was discussed, it was discussed most extensively when the GP assumed a link between the patient’s work and the health complaint or disorder. Only one study, to the authors’ knowledge, has investigated work-related encounters in general practice. In this study, only 2.6% of all consultations were about work.[25] However, this latter study was about work-related issues in particular, whereas the present study did not focus on causal associations between work and health.
This study showed that on average 15% of the total consultation time was dedicated to communication on work-related matters, which was in line with findings of Johanson et al. [26] However, the finding that the patient predominantly introduced discussion of workrelated matters is in contrast with another study by Johanson et al, in which it was found that the GP initiated communication about work more often.[27] When a GP is alert to work-related matters, this may have benefits for the patient regarding future functioning at work. Proactive GP communication was found to be associated with a greater likelihood of return to work (RTW),[28] and improvements in communication may also improve disability outcomes and the doctor–patient relationship.[15] In contrast, poor communication between GPs and patients, occupational physicians and other stakeholders is an obstacle to RTW.[29] Communication training for GPs in the area of work-related disorders is rare, but there are challenges and opportunities for improvement.[12]
Strengths and limitations of the study
One of the strengths of this study was the relatively large sample size of observational data from the DNSGP-2. The results of the study are most applicable to the Dutch population of GPs. Another strength was the use of RIAS, a systematic and objective observation and coding system, resulting in a dataset of mutually exclusive categories.[30] This innovative approach enabled description of GP–patient communication on workrelated MSDs using accurate observations instead of questionnaires. This is valuable, since discrepancies may exist between what GPs actually say or do and what they report in questionnaires.
The present study relied on descriptive analyses, which implies that the dynamics of the communication between the GP and the patient could not be taken into account. More research is needed to achieve this, which will give valuable information on the process of communication about work-related factors. Another point of consideration was the chosen moment for observation. The taped consultation was one random interaction in a mostly long-lasting relationship between the GP and patient. It was not known what the GP and the patient had discussed before. This may have led to an underestimation of the percentage of consultations in which work had previously been the subject of communication. The relationship between disorder and work might have been explored in a previous consultation. We investigated whether there was a difference between a first and repeat consultation. A difference was found, but this was not statistically significant. However, in an ideal situation, work should be discussed in all consultations, since working conditions may change or may initiate new health complaints. The data presented here were collected in 2001. The situation may have changed since then, so it would be valuable to repeat this study with more recent data.
Implications for practice and research
The results of this study give us more information about communication between GPs and patients during consultations. The innovative approach of observing rather than asking has great potential. Future research should further develop this method to enable analysis of the dynamics of the process of communication. Integration of discussion about work into the GP consultation is important for early intervention and RTW, since the GP is often the first physician in contact with the patient. Work-related factors have been shown to be important prognostic indicators in back pain, and recent guidelines recommend that the primary care management of this condition include advice to stay at or return to work as soon as possible.3 Just talking about work is often not sufficient, but advice about return to work or to stay at home should be in accordance with the specific situation of the patient. In case of MSDs, early return to work is a proven strategy to enhance health.3 One way to get more attention from GPs about the work of their patients is to incorporate this in education programmes for GPs.
This study aimed to increase insight into the communication about work between GPs and patients with paid work consulting about MSDs. Work was discussed in one-third of the consultations with patients withMSDswhowere in paid employment. The initiative to discuss work was mainly taken by the patient. When the GP assumed a relationship between the patient’s work and his or her disorder, it was discussed more extensively. The study findings suggest that GPs should ask questions regarding the patient’s work more often, since the present results show that this is not a standard topic of conversation.
We thank all patients and GPs for their participation in this study and NIVEL for collecting and providing the data. We also thank F Tromp for helpful and inspiring comments during the observations and H Abrahamse for the data management.
No external funding.
Ethical approval was obtained from VU University Medical Centre. Confidentiality of collected data was safeguarded according to privacy regulations.
Not commissioned; externally peer reviewed.
None.