Parth J Parekh1, Dawn Burleson2, Craig Lubin3 and David A Johnson4*
1Department of Internal Medicine, Division of Gastroenterology, Carilion Clinic, Virginia Tech School of Medicine, Roanoke, VA, USA
2Department of Clinical and Regulatory Affairs, HyGIeaCare Inc., Charlotte, NC, USA
3Austin Gastroenterology, Austin, TX, USA
4Department of Internal Medicine, Division of Gastroenterology, Eastern Virginia Medical School, Norfolk, VA, USA
*Corresponding Author:
David A. Johnson
Department of Internal Medicine
Division of Gastroenterology
Eastern Virginia Medical School
Norfolk, VA, USA
Tel: +1 757-446-5600
E-mail: dajevms@aol.com
Received date: February 16, 2018; Accepted date: March 02, 2018; Published date: March 06, 2018
Citation: Parekh PJ, Burleson D, Lubin C, Johnson DA (2018) Colon Irrigation: Effective, Safe, and Well-Tolerated Alternative to Traditional Therapy in the Management of Refractory Chronic Constipation. J Clin Gastroenterol Hepatol Vol.2: No.1:5. doi:10.21767/2575-7733.100034
Keywords
Chronic constipation; Colonic irrigation; Colon hydrotherapy
Introduction
One of the most common complaints faced by both primary care physicians and gastroenterologists is constipation. In the United States, constipation affects between 12% and 19% of the general population [1]. More concerning is that this trend appears to be rising [1-3]. Unfortunately, despite this commonality, constipation remains under diagnosed and often times under treated. Perhaps this is because clinicians do not fully understand the patient-related scope of impact. Perhaps this is because the term constipation encompasses a blanket term that can have different meanings to individual clinicians and patients alike (i.e. hard stools, excessive straining, infrequent bowel movements, incomplete evacuation, bloating, or the need to manually disimpact in order to achieve defecation). Irrespective, constipation takes a significant toll on the individual patient [4-8] as well as on overall direct and indirect health care costs [1-3]. Many care providers may not appreciate the significant burden on emergency room visits for this patient population [3], in particular female patients as they have the highest likelihood of seeking medical attention for constipation-related issues [9].
At an individual level, constipation can have a dramatic impact on the patient’s overall well-being. This includes influencing their psychosocial state (e.g. anxiety, depression, somatization, and sexual dysfunction) [4,5,10] as well as societal (e.g. time lost off work) [5], both of which are common amongst patients suffering from constipation. A national survey, which included 10,030 respondents, assessing symptoms and disease burden, found that up to 72% of patients with constipation felt that their constipation was very to extremely bothersome, disrupting productivity by nearly 5 days per month [6]. The BURDEN-CIC trial, which included 1,223 patients with chronic idiopathic constipation (CIC), demonstrated that the majority of patients felt either frustrated or stressed with their constipation (70%) whereas only a minority of patients (23%) felt that their symptoms were under control [7].
At a macro level, the management of constipation utilizes a significant portion of healthcare resources. Studies have found a recent surge of emergency department visits for constipation-related issues, with an increase in more than 40% over a 5-year period with an associated 120% increase in aggregate national costs over the same timeframe [1]. In 2011 alone, there were over 700,000 visits to the emergency department with a primary diagnosis of constipation, with an aggregate cost in excess of $1.6 billion dollars [1]. This trend held particularly evident in the younger population [2]. In addition, the cost of management carries significant burden with estimates suggesting that upwards of $800 million dollars are spent annually on over-the-counter laxatives alone [1,3,10]. For severe constipation, it is expected that highvolume colon irrigation is an easier and less expensive alternative to gastrograffin enemas, which are routinely performed by radiologists at an X-ray facility [11-18].
Diagnosis and Treatment
Constipation can be divided into acute and chronic constipation. Acute constipation is typically transient resulting from a stressor, be it physiologic (e.g. surgery, immobility, change in diet, electrolyte imbalance, or recent travel) or psychologic (e.g. life-changing event). Chronic constipation refers to symptoms that have been persistent for at least several months. Chronic constipation can be further categorized as primary constipation (e.g. normal or slow colon transit, pelvic floor dysfunction) or secondary to a variety of systemic disorders or medication-induced. Primary, or functional, constipation can be further subdivided into different subtypes each with its own set of diagnostic criteria. Table 1 outlines the diagnostic criteria for each. The focus of our study is on the management of chronic constipation [19-21].
| Subtype |
Functional constipation |
Functional defecation |
Dyssynergia |
Inadequate propulsion |
| References |
[19] |
[20] |
[21] |
[20] |
| Diagnostic Criteria |
Criteria fulfilled for at least 3 months with symptom
onset at least 6 months prior to diagnosis |
Criteria fulfilled for at least 3 months with symptom onset
at least 6 months prior to diagnosis |
Manometric or EMG evidence of
dyssynergia during attempted defecation |
Inadequate propulsive forces measured with manometry with
or without inappropriate contraction of the anal
sphincter and / or pelvic floor muscles |
| At least 2 of the following: |
During repeated attempts to defecate, must have features of impaired
evacuation as demonstrated by 2 of the following 3: |
1 of the following: |
- |
| Straining during 25% of defecations |
Abnormal balloon expulsion test |
Abnormal balloon expulsion test |
- |
| Lumpy or hard stools in more than 25% of defecations |
Abnormal anorectal evacuation pattern with manometry or anal surface
electromyography (EMG) |
Abnormal defecography |
- |
| Sensation of incomplete evacuation in more than 25% of defecations |
Impaired rectal evacuation by imaging |
Abnormal colon transit study |
- |
| Sensation of anorectal blockage in more than 25% of defecations |
- |
- |
- |
| Manual maneuvers to facilitate a bowel movement in more than 25% of defecations |
- |
- |
- |
| Fewer than 3 spontaneous bowel movements per week |
- |
- |
- |
Table 1: Chronic constipation subtypes.
There are several factors which place patients at high-risk for constipation. An international population-based study demonstrated female, elderly, and patients of lower socioeconomic status have the highest predilection towards the development of chronic constipation [10,11]. Additionally, the opioid epidemic currently plaguing the United States is further contributing to the incidence of chronic constipation. Recent studies have demonstrated this parallel, suggesting that more than 80% of patients on chronic opiate medications experience constipation. [10] Additionally, greater than 80% of patients on chronic opiates feel that the constipation they experience significantly impacts their quality of life and activities of daily living, despite the use of laxatives [12].
The current mainstay in treatment involves a multidisciplinary approach which includes patient education, behavior modification, dietary changes, and/or laxative therapy. Severe cases may result in manual digital disimpaction or even surgical intervention. The most commonly prescribed therapy involves laxative medications, be it surfactant, osmotic, stimulant laxatives, or varying combinations. These medications can often carry significant cost, produce undesirable side effects, or cause significant electrolyte shifts that can have deleterious effects in patients with hepatic or renal impairment [13].
Health care providers feel the frustration as well. The BURDEN-CIC trial, which included 331 health care providers, demonstrated that health care providers also perceived inadequate treatment in the majority of their patients. In this study, health care providers reported their patients seemed to feel frustrated (72%), stressed (49%), and fed-up (43%) with their current treatment regimen [7]. A recent meta-regression analysis evaluating the relationship between pain intensity and bowel patterns demonstrated the effective treatment of constipation decreases discomfort, independent of specific drug mechanisms [14].
A recent meta-regression analysis which evaluated the relationship between pain intensity and bowel patterns demonstrated the effective treatment of constipation decreases discomfort, independent of specific drug mechanisms [14]. Focused on an effort to alleviate constipation and the symptoms associated with constipation, we evaluated the use of high-volume colon irrigation in relieving constipation.
Methods and Aims
Focused on an effort to alleviate constipation and the symptoms associated with constipation, we evaluated the use of high-volume colon irrigation in relieving constipation. 175 patients with refractory constipation of varying etiology were referred to perform a high-volume colon irrigation procedure from August 2016 to January 2018. All patients were referred to the HyGIeaCare Clinic by prescription. Patients were not given any specific preparation instructions for their procedure.
Patients ranged in age from 19-99 years old (mean of 62 years of age). 20% of patients were male and 80% were female. Pertinent past medical history for those enrolled included: 10 (6%) with IBS, 5 (3%) with Crohn’s Disease, and 3 (2%) with Diabetes Mellitus. When asked for the frequency of the bowel movements, 53% of the patients reported either <3 bowel movements per week or reported weekly or less frequent bowel movements.
The HyGIeaCare® System is intended for colon cleansing when medically indicated, such as before a radiological or endoscopic examination. The HyGIeaCare® System, illustrated in Figure 1, is an instrument for colonic irrigation. Filtered water is introduced at a comfortable temperature into the large intestine, thus cleansing the colon of its contents. It is hygienic, comfortable and painless. Water temperature is controlled. Temperature, flow and pressure are controlled by one switch operated by the user.
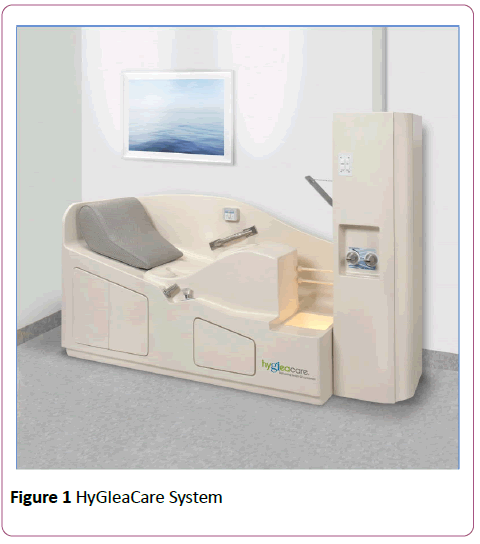
Figure 1: HyGIeaCare System
The entire system is flushed with a chlorine disinfectant solution before and after each patient which disinfects the HyGIeaCare® System. In addition, all surfaces were wiped with Cavicide which manually disinfects the system. The system includes disposable tubing and a sterile, disposable rectal nozzle intended for single use only.
The HyGIeaCare® System procedure is performed by a certified practitioner specifically trained on the safe use of the system. The patient is seated on the disinfected basin and a sterile and a disposable nozzle is introduced into his/her rectum about an inch. A gentle stream of warm water then flows into the bowel, loosening stool, allowing the patient to comfortably and discreetly evacuate his/her colon. Water continues to flow and gently cleans the colon until the practitioner instructs the patient on completion of the procedure.
The HyGIeaCare® System encompasses the following safety features:
• Gently arched rectal nozzle, with a diameter of less than 1 cm
• Water flows through a sediment and UV filter
• Water flows gently, driven only by gravity
• Temperature of the water is steadily maintained
• Water automatically stops flowing into the patient if temperature of the water exceeds the safe range of 99° to 103°F (37°C-39°C)
Our hypothesis was that the HyGIeaCare® System (Austin TX) could offer a well-tolerated, safe, and effective alternative therapy in treating chronic constipation. The HyGIeaCare® System could treat chronic constipation via a multi-faceted approach by (1) cleansing the bowel without the need for aggressive medical therapy or manual and/or surgical intervention, and (2) theoretically altering the commensal microbiome with the hopes of repopulating a more favorable microbial profile. This however, needs to be studied further.
The primary endpoint of the procedure was successful passage of stool during colonic irrigation with secondary endpoints being patient satisfaction and a favorable side effect profile.
Results
The HyGIeaCare® System cleansing was successfully completed in all 175 patients. 100% of patients had solid stool excrement who underwent the high-volume colon irrigation procedure. The excrement characteristics were divided into 4 phases. Table 2 describes each phase and the YES/NO answer as it related to whether each phase was discerned and verified through the observation tube associated with the device. The amount of water used for irrigation directly related to the excrement characteristics: <8 gallons of water was used in 62 (35%) of the patients; 9 to 16 gallons used in 112 (64%) of the patients; and > 16 gallons was used in 1 (<1%) of patients.
| Phase discerned and verified during procedure (N=175) |
Yes |
No |
| Dense: Very large solid matter usually from the recto-sigmoid junction, sigmoid and descending areas of the colon. |
132 (75%) |
43 (25%) |
| Broken: Mostly fragmented stool usually from the transverse colon. |
164 (94%) |
11 (6%) |
| Chyme: Noticeable food residues/cloudy material usually from the ascending and cecal areas of the colon with potentially audible gas release. |
146 (83%) |
29 (17%) |
| Clear: Numerous clear outflows of clear water but only after the above phases have been discerned. |
119 (68%) |
56 (32%) |
Table 2: Excrement phases
The most common symptoms experienced during the procedure, which represent 9% of the patients studied, were nausea and abdominal cramping. There were no serious or severe adverse events reported. Additional details are noted in Table 3.
| Most common symptoms (N=175) |
None |
Very little OR Some |
Quite a bit OR a lot |
| Nausea |
152 (87%) |
16 (9%) |
7 (4%) |
| Vomiting |
171 (98%) |
3 (2%) |
1 (<1%) |
| Dizziness |
166 (95%) |
7 (4%) |
2 (1%) |
| Abdominal cramping |
150 (86%) |
15 (9%) |
10 (6%) |
Table 3: Symptoms experienced during the procedure.
Discussion
Nearly 20% of the United States population complains of constipation, with evidence indicating an uptrend. This represents a significant burden on the current state of health care with increased cost both direct (chronic medical therapy, frequent emergency room visits, and/or surgical intervention) and indirect (quality of life and its impact on the psychosocial state). Despite its commonality, advances in pharmacotherapy have not made significant headway when compared to traditional treatment options. High-volume irrigation with the use of the HyGIeaCare® system provides a safe, effective, and well-tolerated alternative to traditional therapy. This study, which totaled 175 patients with chronic constipation of varying etiology, demonstrated the effectiveness and a favorable side effect profile of the HyGIeaCare® system. The volume of water used for these patients is comparable to that used in standard use of HyGIeaCare® for standard precolonoscopy preparations.
Conclusion
Future studies are needed to study the longevity of response duration, however HyGIeaCare® System may have a lasting effect that goes beyond immediate relief. Recent studies have demonstrated the alterations in microbial homeostasis that could result in or propagate chronic constipation [15-18]. Thus, high volume irrigation may alter the microbiome in ways that could potentially promote growth of more favorable bacteria resulting in long lasting relief. Second, high-volume irrigation offers more definitive removal of fecal obstructing debris compared to traditional therapy. High-volume colon irrigation appears to be a well-tolerated and safe alternative to medical therapy for patients suffering with constipation with a high willingness to repeat.
Ongoing assessment will help define the true value of this as a sustainable and practical effective option for long-term effectiveness, albeit the short-term data is favorable.
References
- Sommers T, Corban C, Sengupta N, Jones M, Cheng V, et al. (2015) Emergency department burden of constipation in the United States from 2006 to 2011. Am J Gastroenterol 110: 572-579.
- Sharma A, Rao S (2017) Constipation: pathophysiology and current therapeutic approaches. Handb Exp Pharmacol 239: 59-74.
- Singh G, Lingala V, Wang H, Vadhavkar S, Kahler KH, et al. (2007) Use of health care resources and cost of care for adults with constipation. Clin Gastroenterol Hepatol 5: 1053-1058.
- Lee C, Doo E, Choi JM, Jang SH, Ryu HS, et al. (2017) The increased level of depression and anxiety in irritable bowel syndrome patients compared with healthy controls: Systematic review and meta-analysis. J Neurogastroenterol Motil 23: 349-362.
- Roalfe AK, Roberts LM, Wilson S (2008) Evaluation of the Birmingham IBS symptom questionnaire. BMC Gastroenterol 8: 30.
- Heidelbaugh JJ, Stelwagon M, Miller SA, Shea EP, Chey WD (2015) The spectrum of constipation-predominant irritable bowel syndrome and chronic idiopathic constipation: US survey assessing symptoms, care seeking, and disease burden. Am J Gastroenterol 110: 580-587.
- Harris LA, Horn J, Kissous-Hunt M, Magnus L, Quigley EM (2017) The better understanding and recognition of the disconnects, experiences, and needs of patients with chronic idiopathic constipation (BURDEN-CIC) study: Results of an online questionnaire. Adv Ther 34: 2661-2673.
- Rao SS, Seaton K, Miller MJ, Schulze K, Brown CK, et al. (2007) Psychological profiles and quality of life differ between patients with dyssynergia and those with slow transit constipation. J Psychosom Res 63: 441-449.
- Pare P, Ferrazzi S, Thompson WG, Irvine EJ, Rance L (2001) An epidemiological survey of constipation in Canada: definitions, rates, demographics, and predictors of health care seeking. Am J Gastroenterol 96: 3130-3137.
- Quigley EM, Neshatian L (2016) Advancing treatment options for chronic idiopathic constipation. Expert Opin Pharmacother 17: 501-511.
- Suares NC, Ford AC (2011) Prevalence of, and risk factors for, chronic idiopathic constipation in the community: systematic review and meta-analysis. Am J Gastroenterol 106: 1582-1591.
- Sonu I, Triadafilopoulos G, Gardner JD (2016) Persistent constipation and abdominal adverse events with newer treatments for constipation. BMJ Open Gastroenterol 3: e000094.
- Serrano-Falcon B, Rey E (2017) The safety of available treatments for chronic constipation. Expert Opin Drug Saf 16: 1243-1253.
- Nelson AD, Camilleri M, Chirapongsathorn S, Vijayvargiya P, Valentin N, et al. (2017) Comparison of efficacy of pharmacological treatments for chronic idiopathic constipation: a systematic review and network meta-analysis. Gut 66: 1611-1622.
- Jalanka J, Spiller R (2017) Role of microbiota in the pathogenesis of functional disorders of the lower GI tract: Work in progress. Neurogastroenterol Motil 29: 1-5.
- Tian H, Ge X, Nie Y, Yang L, Ding C, et al. (2017) Fecal microbiota transplantation in patients with slow-transit constipation: A randomized, clinical trial. PloS one 12: e0171308.
- Parthasarathy G, Chen J, Chen X, Chia N, O'Connor HM, et al. (2016) Relationship between microbiota of the colonic mucosa vs feces and symptoms, colonic transit, and methane production in female patients with chronic constipation. Gastroenterology 150: 367-379.
- Parekh PJ, Balart LA, Johnson DA (2015) The influence of the gut microbiome on obesity, metabolic syndrome and gastrointestinal disease. Clin Transl Gastroenterol 6: e91.
- Schmulson MJ, Drossman DA (2017) What is new in Rome IV. J Neurogastroenterol Motil 23: 151-163.
- Rao SS, Bharucha AE, Chiarioni G, Felt-Bersma R, Knowles C, et al. (2016) Anorectal disorders. Gastroenterology 150: 1430-1442.
- Rao SS, Patcharatrakul T (2016) Diagnosis and treatment of dyssynergic defecation. J Neurogastroenterol Motility 22: 423435.


