Original Article - (2017) Volume 18, Issue 3
Department of 1Clinical Pharmacology and Chemotherapy and 2Surgery #7, N.N. Blokhin Russian Cancer Research Center, Moscow, Russia
Received March 22nd, 2017-Accepted May 04th, 2017
Objectives We aimed to evaluate clinical factors that can predict second-line chemotherapy benefit in patients with pancreatic cancer. Methods In this retrospective study records of patients who received first-line chemotherapy since 2000 to 2015 were analyzed. A number of clinical and laboratory factors were evaluated for prognostic significance in a multivariate Cox proportional hazards model with overall survival as the end-point. Based on independent prognostic factors the prognostic model was constructed to dichotomize patients into two groups of prognosis. Results Records of 172 patients matched the inclusion criteria. Karnofsky performance status ≤70% and neutrophil-to-lymphocyte ratio >5 at the time of disease progression after first-line chemotherapy were independent poor prognostic factors. Administration of second-line chemotherapy improved outcome only in patients with favorable prognosis: median overall survival increased from 1.7 to 5.5 months for patients who received chemotherapy (n=23) and BSC (n=90), respectively (p=0.002). Median overall survival in the group of poor prognosis were 2.3 and 1.7 months for patients who received chemotherapy (n=20) or only BSC (n=39), respectively (p=0.233). Conclusion This novel prognostic model can potentially predict second-line chemotherapy benefit in patients with pancreatic cancer. However it needs to be validated in further trials.
Nomograms; Pancreatic Neoplasms
An estimated 337,800 people were diagnosed with pancreatic cancer around the world in 2012; more than 330,000 patients succumbed due to this disease [1]. Furthermore, the incidence of pancreatic cancer tends to increase. The disease is expected to take second place in cancer mortality in the United States by 2030 [2].
FOLFIRINOX, gemcitabine in combination with nabpaclitaxel or gemcitabine monotherapy are current frontline regimens for the treatment of locally advanced and metastatic pancreatic cancer [3, 4]. On the contrary second-line chemotherapy regimens for this disease are not standardized. Most patients do not receive secondline chemotherapy, mainly due to the rapid deterioration of performance status following cancer progression [5, 6]. Other relevant clinical factors, such as efficacy of previous chemotherapy, lesions sites and sizes, weight loss and laboratory parameters, are usually not taken into account.
All current second-line regimens have modest efficacy: objective response rate is usually below 10% [7], median progression-free survival is approximately 2 months [5]. Therefore patients should be carefully selected for chemotherapy and there is an unmet medical need for a predictive model which would facilitate patient selection for second-line chemotherapy.
Patients
Records of patients with pancreatic cancer who had been treated at the department of clinical pharmacology and chemotherapy of N.N. Blokhin Russian Cancer Research Center since 2000 to 2015 were analyzed. Eligibility criteria for this retrospective analysis were: 1) morphologically confirmed locally advanced/metastatic or recurrent pancreatic cancer, 2) disease progression within 6 months after the last cycle of first-line chemotherapy or adjuvant chemotherapy.
Patient’s clinical and laboratory characteristics at the time of progression after previous chemotherapy were evaluated for prognostic and predictive significance. The following clinical and laboratory factors were analyzed: gender, age, family history/ supposed hereditary cancer (yes vs. no), smoking status (current or former smokers vs. never smokers), body mass index, percentage of body weight loss over the periodduring the course of the disease, diabetes mellitus (yes vs. no), metformin , aspirin or statins intake (yes vs. no), Karnofsky performance status (100-80% vs. 70% vs. ≤60%), previous chemotherapy setting (adjuvant vs. neoadjuvant ± adjuvant vs. first-line), previous chemotherapy regimen (containing gemcitabine vs. not contain gemcitabine), objective response to previous chemotherapy (yes vs. no), time to progression following previous chemotherapy, site of the primary tumor (head vs. body or tail of the pancreas), maximum primary tumor size, presence of regional lymph nodes involvement (yes vs. no), presence (yes vs. no) and maximum size of metastases in retroperitoneal lymph nodes, liver, lung, peritoneum, presence of ascites (yes vs. no), tumor grade (G1 vs. G2 vs. G3), CEA and CA19-9 levels, albumin level (normal vs. below lower limit of normal), total bilirubin level (normal vs. above upper limit of normal [ULN]), alkaline phosphatase level, levels of hemoglobin, white blood cells, platelets and neutrophil-to-lymphocyte ratio (NLR).
Prognostic value of the all above mentioned factors has been assessed by univariate Cox proportional hazards model with overall survival (OS) as the endpoint. OS was calculated from date of progression following previous chemotherapy to death or last contact with a patient for censored cases. Kaplan-Meier method was used to assess OS. Cutoff levels of quantitative factors were chosen using the ROC-curves analysis. Three months survival rate was selected as the endpoint for ROC-curve analysis.
Factors, that demonstrated a statistically significant impact on OS according to the results of univariate analyses, were further analyzed in the multivariate Cox proportional hazards model with stepwise exclusion of variables. Factors that showed statistically significant impact on OS were considered independent prognostic factors. The prognostic model was constructed based on these factors dichotomizing patients into groups with poor or favorable prognosis. Hazard ratios for each independent prognostic factor were taken into consideration for prognostic score calculation. Then an impact of second-line chemotherapy on overall survival was evaluated with stratification into two prognostic groups.
Statistical analysis of the data was conducted using Microsoft Excel 2007 and IBM SPSS Statistics v. 20.
Patients Characteristics
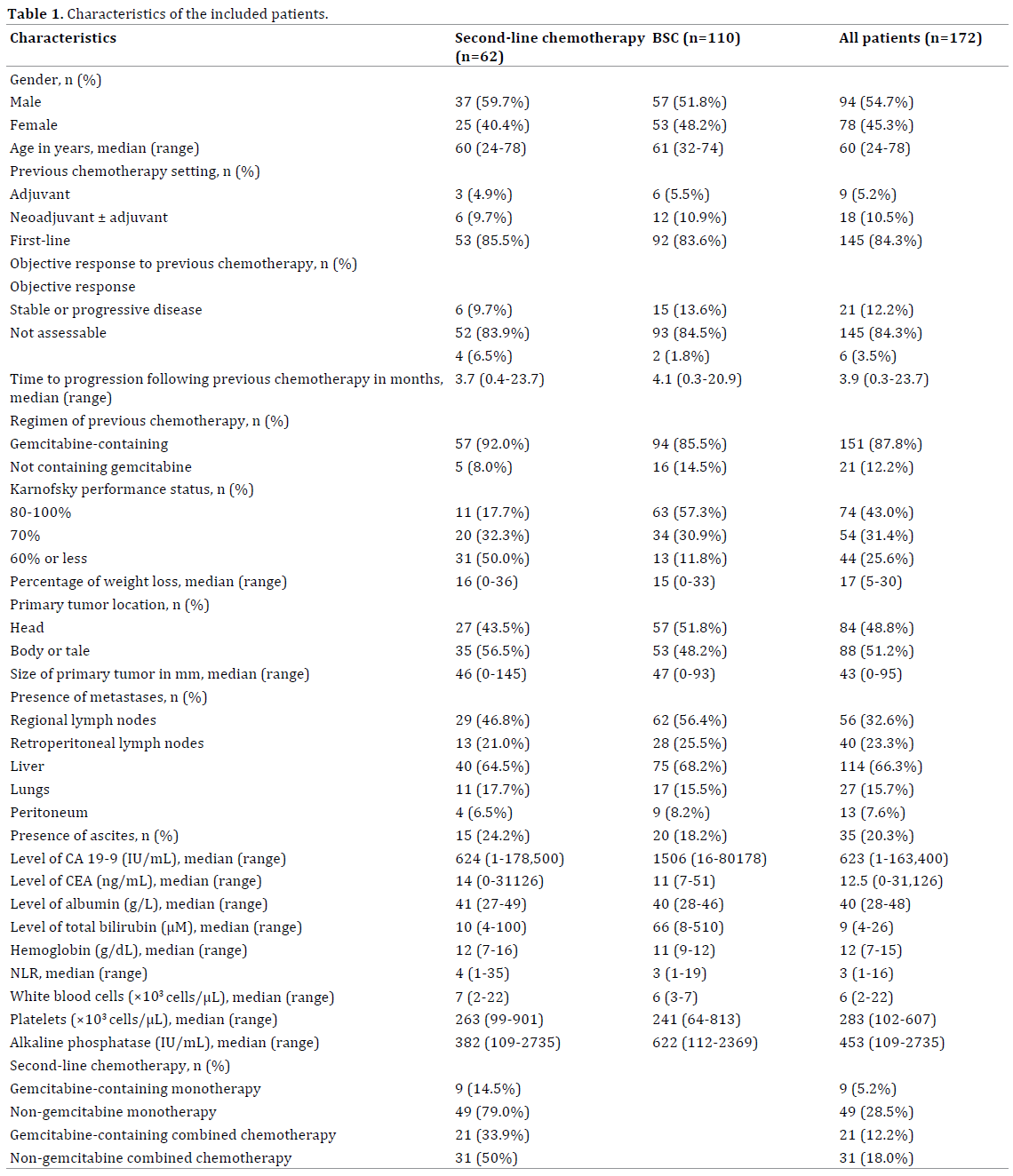
A total of 347 patients received primary chemotherapy. Of them 172 patients met the inclusion criteria for the present analysis (Figure 1). Median OS in the whole cohort of patients was 3.4 months (95% confidential interval (CI) 2.8-4.0 months). Characteristics of included patients are presented in Table 1.
Factors of Unfavorable Prognosis
Univariate Cox regression analyses showed that the following variables had negative impact on OS: presence of liver metastases greater than 20 mm in maximum dimension [hazard ratio (HR) 1.513, 95% CI 1.090-2.101], presence of ascites [HR 1.941, 95% CI 1.303-2.890], Karnofsky performance status ≤70% [HR 1.818, 95% CI 1.502-2.201], albumin level <35 g/L [HR 1.766, 95% CI 1.069-2.917], total bilirubin >ULN [HR 1.656, 95% CI 1.122-2.445], hemoglobin ≤11 g/dL [HR 1.404, 95% CI 1.002-1.965], NLR> 5 [HR 1.845, 95% CI 1.236-2.755] and alkaline phosphatase > 5 times higher ULN value [HR 2.424, 95% CI 1.374-4.277].
These factors were further analyzed in the multivariate Cox regression analysis with stepwise variable exclusion. Multivariate analysis results are presented in Table 2.
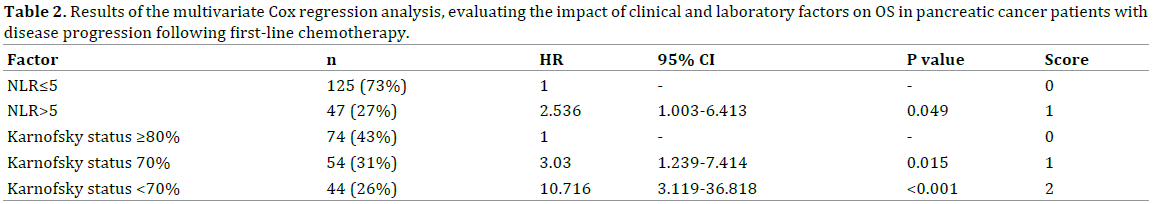
Two factors - Karnofsky status 70% or less and NLR>5 – were shown to be independent poor prognostic factors in pancreatic cancer progressing after first-line chemotherapy. Groups of favorable (score 0-1) and poor prognosis (score ≥2) were formed based on HR values of these two factors.
Figure 2 shows Kaplan-Meier curves for OS in these two risk groups. Median OS were 5.0 and 1.8 months for groups of favorable and poor prognosis, respectively (p<0.001).
Efficacy of Second-line Chemotherapy
OS in patients who received second-line chemotherapy or BSC only was compared with stratification by prognostic groups (Figures 3 a,b). Median OS in the favorable prognosis groups was 5.5 and 1.7 months for patients who received chemotherapy and BSC only, respectively (HR 2.119, 95% CI 1.302-3.448, p=0.002). Median OS in the poor prognosis group was 2.3 and 1.7 months for patients who received chemotherapy and BSC only, respectively (HR 1.392, 95% CI 0.798-2.428, p=0.233).
Efficacy of second-line chemotherapy is usually low in most patients with pancreatic cancer. However, there are limited data suggesting that selected patients receiving second-line chemotherapy can benefit from its administration compared to BSC.
A small randomized trial comparing efficacy of OFF regimen (oxaliplatin / folinic acid / 5-fluorouracil) versus BSC in patients who had tumor progression following gemcitabine-containing front line chemotherapy demonstrated increased median OS in the OFF group [8].
A systematic analysis of published trials of secondline chemotherapy in pancreatic cancer demonstrated a consistent increase in the proportion of patients receiving second-line chemotherapy during the recent years. The authors found that the increase in the second-line chemotherapy utilization had a positive impact on OS [5].
Less than half of the patients receive second-line chemotherapy, mostly due to a rapid deterioration of general condition [9, 10]. Good performance status is a major factor supporting the decision to start second-line chemotherapy [11].
There are few studies evaluating the prognostic role of clinical and laboratory factors other than performance status in pancreatic cancer progressing after first-line chemotherapy. Nakachi K et al. evaluated the impact of several clinical and laboratory factors on OS of 74 patients with pancreatic cancer progression following gemcitabinecontaining chemotherapy. The multivariate Cox proportional hazards model showed that three factors - C-reactive protein ≥5 mg/dL, ECOG status ≥2 and presence of peritoneal metastases were independent poor prognostic factors [12].
Marechal et al. demonstrated that CA19-9 level ≥400 IU/ mL and albumin ≤3.5 mg/dL were independent negative prognostic factors for OS [13]. Herrmann et al. showed that time to progression on first-line chemotherapy correlated with OS of patients on second-line chemotherapy [14]. Kim ST et al. showed that ECOG status ≥2, lack of response to first-line chemotherapy and albumin level <3.5 mg/dL were independent factors of poor prognosis [15].
Limitations of the most above mentioned studies were small number of patients and patient selection bias. Only those patients who received second-line chemotherapy were included so it is impossible to evaluate whether identified prognostic factors can also be predictors of second-line chemotherapy failure.
In the recent retrospective study authors evaluated an impact of 50 clinical factors on OS of pancreatic cancer patients who received first-line chemotherapy in Besancon hospital in France. Elderly age, smoking, liver metastases, poor performance status, pain, jaundice, ascites and short duration of gemcitabine-based first-line chemotherapy were found to be independent negative prognostic factors [16]. Based on these prognostic factors patients were divided into three groups. However, secondline chemotherapy improved OS in each of these groups although the HR in the high risk group was lower than in the low risk group [16]. Uncertain correlation between death risk and chemotherapy benefit limits the use of such a model for prediction of chemotherapy benefit.
The present analysis is consistent with previous reports demonstrating that patient performance status estimated by Karnofsky scale as 70% or below is an independent factor of poor prognosis. Another independent factor of poor prognosis is NLR> 5. NLR is a marker of inflammation. A number of studies demonstrated significant influence of inflammation on tumor progression, invasion and metastasis [17-19]. A metaanalysis of nine studies with 2035 participants demonstrated prognostic value of NLR in primary pancreatic cancer [20]. Cut-off values of NLR varied from 2 to 5 in these nine studies.
Results of the present analysis support the prognostic significance of NLR in patients with disease progression following first-line chemotherapy. These findings are consistent with reported by Nakachi K et al. who demonstrated an independent prognostic value of another inflammation marker, C-reactive protein, in patients with progression after gemcitabine-containing chemotherapy [12].
Patients treated with second-line chemotherapy and patients who received BSC only were included in the present analysis (Table 1). The presence of the latter group allowed us to analyze the impact of chemotherapy on OS with stratification into two prognostic groups and compare it to OS of patients received no chemotherapy.
Our results have shown that second-line chemotherapy can improve outcomes only in the favorable prognostic group of patients. In the poor prognosis group secondline chemotherapy failed to demonstrate a statistically significant impact on the outcome.
It should be noted that due to limited number of patients the benefit of second-line therapy cannot be excluded in the poor prognostic group. However, this minimal benefit can be easily ruined by the toxicity of the treatment. Thus, despite the fact that second-line chemotherapy improves OS compared to BSC, it seems rationale to limit the use of second-line chemotherapy to selected patients.
New prognostic model for pancreatic cancer patients with progression following first-line chemotherapy has been developed. Retrospective nature and a small number of patients should be considered as limitation of this analysis. Advantages of this model are the use of widespread parameters, available in routine clinical practiceand its ability to serve as a predictive model of second-line chemotherapy failure.
The authors have declared that no competing interests exist.