Keywords
ethnic monitoring, ethnicity and primary care, patient monitoring
Introduction
Alongside concern to reduce health inequalities (Department of Health, 2000) in the UK, the Race Relations (Amendment) Act 2000 introduced a general duty requiring public authorities, such as the NHS, to promote race equality (Commission for Racial Equality, 2002). Thus the NHS has a duty to provide services that take appropriate account of religious, cultural and linguistic requirements. However, information about these requirements, in terms of individual patients, is not routinely available.
Minority communities form around 9% of the UK population and are younger than the majority population (30% aged under 15 years compared to 19%; Scott et al, 2001). For example, 16% of the white population are aged 65 years and over compared to 10% of the black Caribbean group and 4% of the Pakistani group (National Statistics, 2001). This has implications because of ethnic diversity in patterns of illness and health needs (NHS Health and Social Care Information Centre, 2005). For example, the prevalence of type 2 diabetes is much higher among Indians, Pakistanis and Bangladeshis than in the general population. Diseases such as coronary heart disease and type 2 diabetes are strongly related to age, and so the burden among ethnic minorities is likely to increase.
There remains disagreement about whether and how ethnic groups might be categorised and howuseful it is to do this in relation to monitoring health status (Aspinall, 2000a). Within the health service ‘ethnic monitoring’ of hospital inpatients has been compulsory since 1995 but has not been undertaken in any uniform or consistent way. Information is limited, with no primary care or outpatient data for comparison and so has been little used (Aspinall, 2000b). NHS Direct has included ethnic monitoring as part of callers’ demographic information since 2003. However, as over 90% of contacts with the NHS occur in general practice (Royal College of General Practitioners (RCGP), 2004), recording such information in primary care, and sharing this with secondary care where necessary, may make more sense, and reduce duplication of effort.
In order to provide information to develop appropriate and effective services and monitor equity for all patients, ethnicity profiling should include as large a proportion of the population as possible and form a routine part of information gathering in primary care. The absence of ethnicity data in the NHS has also dogged effective health services research and development (Department of Health, 1999). Although better ethnicity data have been available from the 2001 Census at ward/locality level, this has not been sufficiently detailed for individual general practices with relatively small numbers of patients from different ethnic groups. Moreover, patient mobility is high in some practices and census data become out of date too quickly to be used reliably for small areas.
Past experience of collecting ethnicity data in primary care
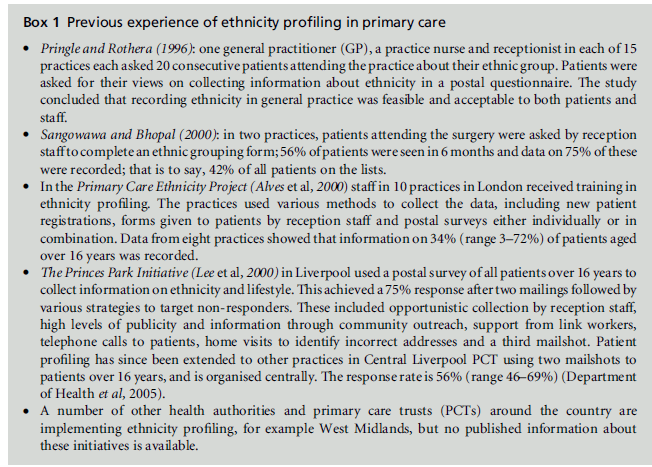
There have been several pilot schemes of ethnic monitoring in primary care (King’s Fund, 2002). However, findings are incomplete or difficult to access, with limited published experience of routine collection in general practice (see Box 1). For example, the Improving Health among Ethnic Minority Populations initiative (Department of Health, 1998) included two projects on collecting ethnicity data in primary care, but the results of only one have been published (Lee et al, 2000). Information on how data have been used to benefit patients is even more limited (Department of Health et al, 2005; Lee et al, 2000).
Box 1: Previous experience of ethnicity profiling in primary care
Various methods have been used but with little consensus about how to standardise data. Some studies (for example, Pringle and Rothera 1996; Sangowawa and Bhopal, 2000) have asked questions about ethnic group alone, but most current ethnicity profiling forms in primary care include questions on ethnicity, religion and spoken and written language, and some have additional questions, for instance about country of origin, cultural needs and carers. The experience of four projects is summarised in Box 1.
Not all data collection has followed recommendations to ask about ethnicity in the same order and format as in the 2001 Census, and this may affect the way people answer the question (Commission for Racial Equality, 2001; Department of Health, 2001). Forms have not been translated as it is not generally known in advance which is the best language for each patient, and the cost of translating forms completed in other languages would be too high. A sentence, in the main languages spoken in the local community, explaining the purpose of the data collection has been included on some forms.
Several studies have enlisted the support of community groups to widen understanding of the purpose of the data collection and so improve response rates (see for example Alves et al, 2000; Lee et al, 2000). There have been major problems with the lack of appropriate Read codes, and difficulties with recording and extracting data from some older clinical computer systems but the range of Read codes has increased since the 2001 Census (Department of Health et al, 2005; Kumarapeli et al, 2006).
Children are an additional consideration. It is an important principle of ethnicity profiling that it is selfdetermined. There is some disagreement over whether information should be collected on children under 16 years, forwhomthe information is often provided by a parent. The Princes Park Initiative collected data on patients aged over 16 years (Lee et al, 2000) as does the Central Liverpool PCT patient profiling project (Department of Health et al, 2005, p.32). In practices where large numbers of patients are from black and minority ethnic groups, the under 16 years age group may form a sizeable proportion of the total list, as in Birmingham for example (Bower and Patel, 1998). Department ofHealth guidance (2005) currently recommends that parents should speak on behalf of babies and young children, and older children should be asked their views where possible.
Our experiences of collecting ethnicity data in primary care
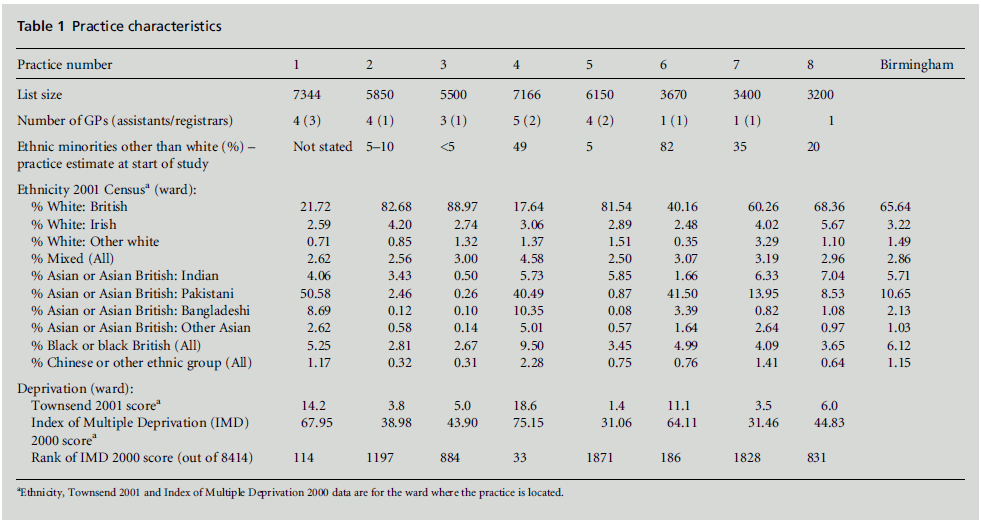
The study reported here aimed to explore methods and practical experience of collecting ethnicity data in primary care in practices in Birmingham with a range of populations (see Table 1) and took place in 2001/02.
Methods
Eight practices using the EMIS computer system were recruited from members of MidReC (Midlands Research Practices Consortium). These included practices from areas with differing social and ethnic diversity, and practices with high and low computer use, in order to explore a wide range of issues and problems that could arise in the data collection. Following discussion at a MidReC Practice Managers’ Forum, a form was designed for completion by patients to collect information about their ethnic group, religion and preferred written and spoken language (see Appendix). None of the practices sought additional information. Data collection in reception, by mailshot, and at new patient registration was considered. Ethical reviewwas not thought necessary, as local primary care organisations were beginning to promote ethnicity data collection. This pilot study supported the practices in collecting these data as part of local service development.
A template was designed to record the information on the EMIS computer system with the appropriate Read codes. Practice staff were trained in ethnic profiling based on the Department of Health training developed for secondary care (Department of Health, 2001). The practice manager and one or two other staff (receptionists and practice nurses) from five practices joined together for training. Three practices were trained individually, and all administrative staff received training where possible. The practices were set targets of one-third of patients profiled after 6 months and twothirds after 12 months. Practices were contacted regularly by telephone and practice visits to provide support and advice. Computer searches of the data collected were carried out after 6–12 months of data collection.
Findings
Experience of implementing the data collection
The varied experiences of participating practices are shown as brief case studies in Box 2. Initially practices were confident data collection would be straightforward and targets achievable. However, in several practices there were long delays before this began. These were mainly attributed to staff shortages, particularly in reception. All the practices in this study chose to begin the data collection in reception, thinking that this would be relatively easy to do. This proved to be the case, with only one practice (Practice 6) reporting problems due to large numbers of non- English-speaking patients.
Table 1 :Practice characteristics.
Practices 1, 4 and 6, with large numbers of non- English-speaking patients, were offered an interpreter for one to two sessions per week to assist with data collection. However, two of these practices (1 and 4) did not proceed with this or implement data collection and the third (Practice 6), with bilingual receptionists, preferred to interpret for their patients themselves.
The number of patients refusing to complete a form was low, as most patients who questioned the reasons for the data collection completed the form when given an explanation by staff. Practices were inconsistent about collecting data on young children, and some practices chose not to collect data on babies.
Plateau effect on data collection
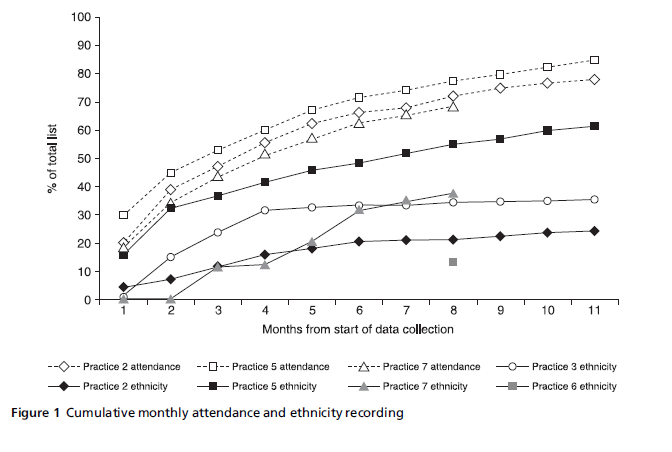
After 3 or 4 months, practices reported that data collection slowed when data on around 20–40% of patients had been collected (see Figure 1). Practices reported that they were frequently asking patients to complete a form when they had already done so. Reception staff became demoralised as they felt there was little reward for their effort.
Practice 5 targeted patients who had not completed a form by flagging the ‘arrivals screen’ on the computer system in advance of the patient’s appointment, and this was very effective. However, it also proved time consuming and expensive and was not possible for appointments booked at short notice. Practice managers commented that marking the cover of patients’ paper notes to show that they had completed an ethnicity form was less helpful, as many patients’ notes already had such coloured codes in abundance.
Consultation data
To explore possible reasons for the observed plateau effect, the number of patients attending practices was estimated. In Practices 2, 5 and 7 the majority of consultations were recorded on the computer system, so an analysis of the consultations with a doctor or a nurse was undertaken. At these three practices, 75– 85% of the practice population had had a consultation over the previous 12 months, but the figures were around 50% after only 3 months (see Figure 1).
Although this annual consultation rate was similar to national data (RCGP et al, 1995), the high consultation rates over shorter periods of 1–3 months were unexpected, particularly as in two practices this occurred during the summer months when consultation rates are lower than in the winter. Around half the practice populations attended a consultation in a 3- month period, and only an additional 25–35% of patients attended in the following 9 months. This suggested data collection in reception is likely to find many repeat attenders after 3 months.
Using different methods for data collection
Practices were encouraged to use other methods that appeared appropriate for their practice to assist data collection. This included putting a message on the electronic message board in the waiting area inviting patients to complete an ethnicity form, sending forms to nursing homes, and targeting special clinics. One practice sent the ethnicity form with a reminder letter about the flu clinic to all eligible patients and had a good response.
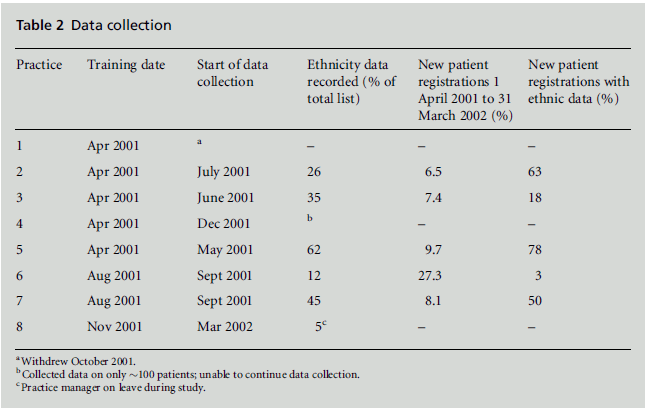
An obvious time to collect data on ethnicity is at new patient registrations when patients are asked to provide a range of personal information to practices. All study practices opted to collect data at new patient registrations, but most failed to use this opportunity fully and only collected data on a small proportion of their new patients (see Table 2). The number of new patients registered in the practices that implemented the data collection was less than 10% (range 6.5– 27.3%) of the total patient lists, except in Practice 6 where it was 27%.
Box 2: Cumulative monthly attendance and ethnicity recording.
Discussion
Our study suggests that common recommendations on ethnicity profiling (Alves et al, 2000; Lee et al, 2000) are unlikely to be easily translated and incorporated into routine primary care practice without more dedicated resource and organisational support.
This study was undertaken when many PCTs and individual practices were, at best, tentatively planning to collect ethnicity data, and was consistent with thinking at the time. NHS guidance (Department of Health, 2001) referred only to data collection in secondary care, and Read codes for use in primary care were limited. Progress has been made since then. New NHS guidance is now wide-ranging, and advocates data collection in primary and secondary care, NHS Direct, social services, mental health care and local authorities (Department of Health et al, 2005).
Following the Race Relations (Amendment) Act 2000, there has been more investment in equality training. Developing patient profiling is becoming a key area of race equality schemes prepared by PCTs. However, progress has been patchy, suggesting that the challenges found in our study continue. For example, in the Heart of Birmingham Teaching PCT (2005), where ‘minority’ ethnic communities formthemajority population, no systematic programme is currently in place as attempts to introduce a system have faltered. Difficulties with recording data and adapting the data collection to local circumstances remain. For example, Waltham Forest PCT (2005) has reported that only 20% of GPs are collecting information, and the data collection has been delayed by problems with templates for computer systems.
The new Quality and Outcomes Framework within the General Medical Services contract for general practice has been effective at improving the quality of data recording in many areas of primary care (The Information Centre, 2006). From April 2006, this has provided an important new incentive for practices to ‘record ethnic origin for 100% of new patient registrations’ (NHS Employers, 2006, p.72). This must be welcomed, although, particularly where patient turnover is low, more complete profiles of practice patients will only develop in the long term. Nevertheless, practices may be stimulated to implement procedures to record ethnicity data more routinely.
Recommendations
A range of methods is needed to maximise the data collection. Our findings suggest that the data collection in primary care may bemost effective when carried out intensively in reception for 3–4 months followed by a mailshot. After a time, the amount of information collected in reception may not justify staff effort unless it is targeted at patients known not to have completed a form.
Systems to ensure that information is collected on all new patients at registration will help. However, collection undertaken opportunistically at other consultations or contacts with patients will be needed to maximise data, for example, by including a form with other routine letters sent to patients. Aside from new patient registration, we suggest that for some practices, particularly those in deprived areas, it will not be feasible to collect ethnicity data at other times due to organisational difficulties and limited staff resource. Here a mailshot might be undertaken on behalf of practices, for instance by the PCT, with resource implications, and strategies for non-responders (Department of Health et al, 2005, p.32; Race for Health, 2006). To facilitate implementation, concerted measures will be needed to include all practice staff, rather than an interested few, in relevant training that underlines the importance and utility of ethnicity profiling, and enhances ownership of the process.
Conclusion
Changes in the organisation of primary care, and the creation of incentives in relation to monitoring the quality of care, offer vital new opportunities to develop ethnicity profiling and to use the data to benefit patients and their care. Nevertheless, collecting information on ethnicity in primary care remains a considerable challenge. As our experience demonstrates, the amount of wider support and work involved in practices with their associated costs should not be underestimated. A range of methods, appropriately resourced, within and external to practices is needed.
ACKNOWLEDGEMENTS
This study was supported by MidReC (Midlands Research Practices Consortium). We would like to thank the practices that took part in the study, Dr Amjid Riaz for developing the data entry template for the computer system and Hilda Parker for her comments on a draft of this paper.
CONFLICTS OF INTEREST
None.
References
- Alves B, Kapasi R, Silvera M and Thomas P (2000) The Primary Care Ethnicity Project: evaluation report. London: WeLReN.
- Aspinall PJ (2000a) The new 2001 Census question set on cultural characteristics: is it useful for the monitoring of the health status of people from ethnic groups in Britain? Ethnicity and Health 5:33–40.
- Aspinall PJ (2000b) The mandatory collection of data on ethnic group of inpatients: experience of NHS trusts in England in the first reporting years. Public Health 114: 254–9.
- Blackwell L (2000) Fragmented life courses: the changing profile of Britain’s ethnic populations. National Statistics: Population Trends 101:6–10.
- Bower C and Patel M (1998) Action Plan for Black and Minority Ethnic Communities: November 1988–November 2001. Birmingham: Birmingham Health Authority.
- Commission for Racial Equality (2001) Ethnic Monitoring: a guide for public authorities. London: Commission for Racial Equality.
- Commission for Racial Equality (2002) The Duty to Promote Race Equality: performance guidelines for health organisations. London: Commission for Racial Equality.
- Department of Health (1998) £1.3 Million Funding for Pilot Projects to Improve Ethnic Minority Health [press release] www.dh.gov.uk/PublicationsAndStatistics/PressReleases/ PressReleasesNotices/fs/en?CONTENT_ID=4024664&chk=yD9unl (accessed 21 February 2007).
- Department of Health (1999) Health Survey for England: the health of minority ethnic groups ’99. London: Department of Health.
- Department of Health (2000) The NHS Plan: a plan for investment, a plan for reform. London: Department of Health, Chapter 13.
- Department of Health (2001) Collecting Ethnic Category Data: guidance and training material for implementation of the new ethnic categories from April 2001. London: Department of Health.
- Department of Health, Health and Social Care Information Centre and NHS Employers (2005) A Practical Guide to Ethnic Monitoring in the NHS and Social Care. London: Department of Health.
- Heart of Birmingham Teaching PCT(2005) EqualitiesReport submitted to HoBtPCT board meeting April 2005, p5. (www.hobtpct.nhs.uk/_docs/board/trust/2005/200504/ Encl%2013%20Equalities%20Board.doc (accessed 21 February 2007).
- Keable-Elliott D and Campion AM (1997) Ethnic monitoring in general practice. British Journal of General Practice 47:329–30.
- King’s Fund (2002) Ethnic Health Issues for Primary Care, March 2002. Information and Library Service. London: King’s Fund.
- Kumarapeli P, Stepaniuk R, de Lusignan S, Williams R and Rowlands G (2006) Ethnicity recording in general practice computer systems. Journal of Public Health 28:283–7.
- Lee B, Gardner K, Jones B and Qassim TA (2000) Ethnicity Profiling in Primary Care – the Princes Park Health Centre Model. Liverpool: Liverpool John Moores University.
- National Statistics (2001) Social Trends 31. Table 1.5, Population: b y ethnic group and age, 1999–00. London: National Statistics. www.statistics.gov.uk (accessed 21 February 2007).
- NHS Employers (2006) Revisions to the GMS Contract 2006/ 07. Annex 1: Quality and Outcomes Framework Guidance, p72. www.nhsemployers.org/primary/primary-890.cfm%20 (accessed 21 February 2007).
- NHS Health and Social Care Information Centre (2005) Health Survey for England 2004: the health of minority ethnic groups – headline tables. London: NHS Health and Social Care Information Centre.
- Pringle M and Rothera I (1996) Practicality of recording patient ethnicity in general practice: descriptive intervention study and attitude survey. BMJ 312:1080–2.
- Race for Health (2006) Lambeth PCT Peer Review: outcome paper. www.raceforhealth.org/fm/upload/PCTs/Lambeth /Lambeth%20Outcome.pdf (accessed 21 February 2007).
- Royal College of General Practitioners (2004) General Practitioner Workload. RCGP Information Leaflet No. 3. London: Royal College of General Practitioners.
- Royal College of General Practitioners, Office of Population, Censuses and Surveys and Department of Health (1995) Morbidity Statistics from General Practice: fourth national study, 1991–1992. London: HMSO.
- Sangowawa O and Bhopal R (2000) Can we implement ethnic monitoring data in primary health care and use the data? A feasibility study and staff attitudes in North East England. Public Health Medicine 2:108–10.
- Scott A, Pearce D and Goldblatt P (2001) The sizes and characteristics of the minority ethnic populations of Great Britain – latest estimates. National Statistics: Population Trends 105:6–15.
- The Information Centre (2006) National Quality and Outcomes Framework Statistics for England 2005/06. London: The Information Centre, Prescribing Support Unit. www. ic.nhs.uk/pubs/qof/qofstatbul/file (accessed 21 February 2007).
- The Race Relations (Amendment) Act 2000. London: Home Office Waltham Forest PCT (2005). Race Equality Scheme 05/08, p15. www.walthamforest-pct.nhs.uk/Publications/docs/ overview1.pdf (accessed 21 February 2007).