Research Article - (2022) Volume 8, Issue 1
Barotrauma-Induced Coronary Vessel
Perforation
Bartosz Zieba* and
Grzegorz Sobieszek
Department of Cardiology, 1st Military Hospital, Poland
*Correspondence:
Bartosz Zieba, Department of Cardiology, 1st Military Hospital,
Poland,
Email:
Received: 03-Jan-2022, Manuscript No. IPIC-22-12227;
Editor assigned: 05-Jan-2022, Pre QC No. IPIC-22-12227;
Reviewed: 19-Jan-2022, QC No. IPIC-22-12227;
Revised: 24-Jan-2022, Manuscript No. IPIC-22-12227;
Published:
31-Jan-2022, DOI: 10.21767/2471-8157.8.1.165
Introduction
Coronary artery perforation is characterized by a rupture of the
arterial lumen and blood extravasation in to the myocardium,
pericardium or heart caves. It is a rare but potentially serious
complication of percutaneous coronary interventions. The reported
incidence of 0.2-0.0, 79% in standard PCI, 1, 4-2, 9% in
CTO cases [1-2].
Ellis classification divides perforations into four types: Type I:
extra luminal crater with no linear contrast extravasation that
suggests dissection, Type II: myocardial or pericardial blushing
with an orifice < 1 mm; Type III: frank contrast medium
extravasation into the pericardium through an orifice > 1 mm
in diameter; Type IV: perforation with contrast extravasation
directly into the left ventricle, to the coronary sinus or other
vascular [3]. Dippel et al. distinguish the Type V of perforation
from modified Ellis classification: distal coronary artery perforation
caused by guidewires[4]. Brilakis presented different
4-grade classification of perforation in the CTO interventions:
main vessel perforation, distal vessel perforation, septal collateral perforation and epicardial collateral perforation. And each
of the above types requires sometimes a different treatment
method [5].
To clinical factors that are associated with an increased risk of
perforation belong female sex and advanced age. Another procedural
factor is complexity of PCI. The main role in the formation
of perforation is played by anatomical factors (treatment
of lesions type B or C, chronic total occlusion and the presence
of coronary calcification) and the type of tools used (catheters,
balloon caterers, cutting balloons, rotational atherectomy,
stents). Most of perforations occur during balloon or stent
expansion, which is related to the balloon or stent-vessel mismatch.
Distal coronary vessel perforation presents another
mechanism of damage usually caused by guidewire placed in
small peripheral side branch or terminated with a loop shape
in narrow distal segment of coronary vessel [6-7].
Pressure injury called barotrauma is physical damage to body
tissues (coronary vessel wall) that can be caused by a direct
exposure to high pressure with balloon or stent inflation, shock
wave after balloon rupture or administration of fluid as contrast with high pressure especially to small vessel. The effect of
high pressure can be used intentionally as in case of granadoplasty.
However mostly the effect of too high pressure is uncontrolled
[8].
Barotrauma induced coronary perforation can reveal after contrast
administration to coronary artery through a diagnostic or
guide catheter. The severity of the injury can vary from slight
intimal dissection to full-length dissection, sometimes spiral
dissection or perforation. Such a complication is often initiated
by mechanical damage to the endothelium by the catheter or
selective intubation of small branch. In this situation, contrast
administration can cause vessel damage and perforation (Figure
1-3).
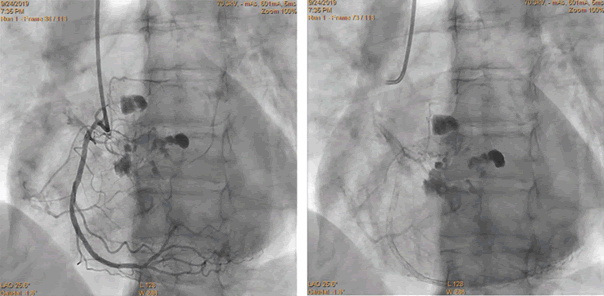
Figure 1: A 71-year-old woman with NSTEMI and hypertension. Diagnostic coronary angiography, 6 Fr JR4.0.
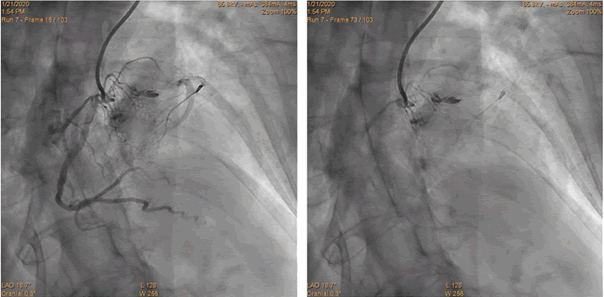
Figure 2: A 65-year-old woman with NSTEMI, hypertension and COPD. Diagnostic coronary angiography, 6 Fr AL 1.0.
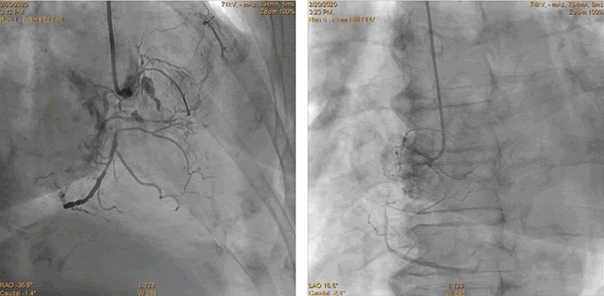
Figure 3: A 81-year-old woman with Chronic Coronary Syndrome, diabetes mellitus, hypertension, after STEMI of inferior wall and PCI LAD, CTO RCA. Diagnostic coronary angiography, 6 Fr JR4.0.
Method
It is retrospective, five cases analysis (4 women and 1 man) of
special kind of coronary artery perforation induced by barotrauma.
The reason of diagnostic coronary angiography was
Chronic Coronary Syndrome in three patients and Acute Coronary
Syndrome in two patients. The right artery was engaged
with a 6 Fr JR4.0 guiding catheter in three patient, in case of
the other two 6 Fr AL 1, 0 and 6 Fr Tiger were used. After administration
of contrast, we observed multifocal extravasation
of the contrast within the distal segment of small vessels. In
four patients (cases 1-4) repeated control echocardiography demonstrated no pericardial effusion and the patients showed
no symptoms (Figure 1-5).
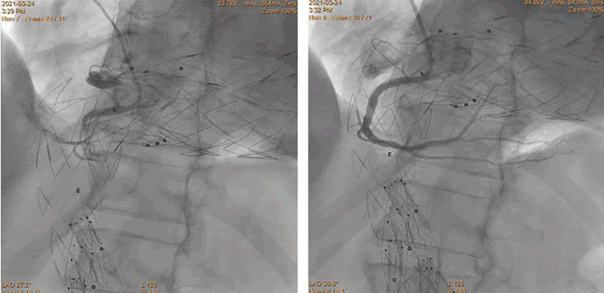
Figure 4: A 66-year-old woman with chronic coronary syndrome ,diabetes mellitus, atrial fibrylation, prior PCI LAD, after stent graft implantation of a in the descending aorta. Diagnostic coronary angiography, 6Fr Tiger.
Discussion
In the cases presented above, the small coronary vessels were
damaged during contrast administration. In all cases it was related
to branches of the right coronary artery. In three cases
it was the first and in two cases the second contrast injection
to intubated artery. In all cases, the damage occurred during
coronarography with a diagnostic catheter.
In all cases the reason of perforation was selective intubation
of a small branch, mostly cone branch and high force administration
of contrast what resulted in and large volume of contrast
flow with high pressure in small vessel.
Contrast extravasation in the above cases is characterized by
typical angiographic image. In the first phase, multifocal extravasation
of contrast as polycyclic brightening in the area of
vascularization of the SB can be observed. The multifocal of
brightening are enlarging during few seconds and the growing
weakly saturated zone of brightening; creating a characteristic
haze can be observed [Figure6].
In four patients (cases 1-4) repeated echocardiography demonstrated
no pericardial effusion and the patients showed no
symptoms. In following cases conservative treatment was
sufficient. Although they all received 5000 IU unfractionated
heparin before procedure, no tamponade symptoms or pericardial
effusion were observed. . In one case (Case 5 ) a serious
complication in the form of tamponade occurred about half an
hour after procedure. This patient received complete heparinization
and had before barotrauma-induced perforation PCI of
another artery .
To avoid the barotrauma-induced perforation, it is indicated to
confirm position of diagnostic or guide catheter after intubating
an artery. Gently applying a small amount of contrast will
allow visualizing the position of the catheter. It is also worth to
check blood pressure and when it is too low, that may indicate
a damping in the small vessel, so the reposition of the catheter
is needed. Avoid using high force to give a contrast is mandatory.
In most cases, conservative treatment is sufficient. Pre-planned
angioplasty should be postponed as it poses a risk of sub-acute
tamponade after a full dose of heparin.
In severe cases, typical coronary perforation treatment is needed,
such as prolonged balloon dilatation, stent or graft implantation
in main vessel. The standard side branch treatment is
also possible using cut balloon technic (CBT) , coils, fat or spongostan to embolized. (Figures 5 and 6).
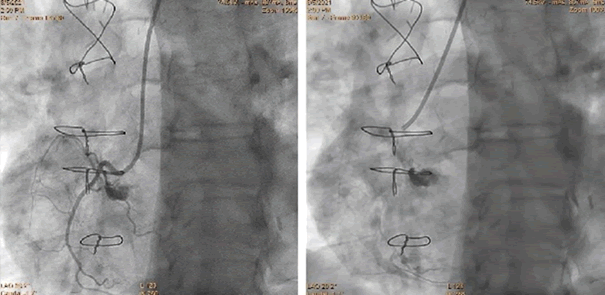
Figure 5: A 55-year-old man with chronic coronary syndrome, after CABG. Diagnostic coronary angiography, 6 Fr JR4.0.
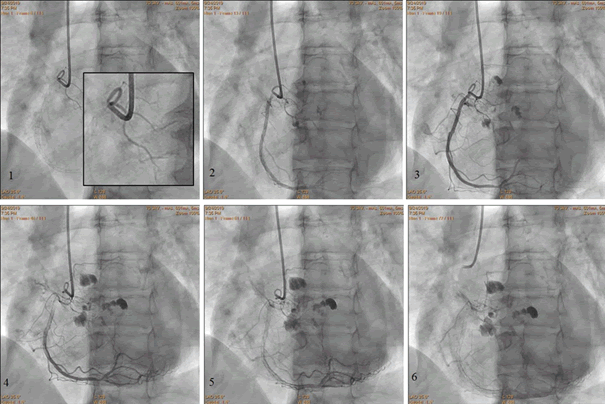
Figure 6: Stages of extravasation
Conclusion
In the cases described by us, the reason for perforation was
selective intubation of the side branch and the administration
of a large volume of contrast under the high pressure. This resulted
in multiple damage to the distal branches, blood extravasations and in one case sub-acute cardiac tamponade.
REFERENCES
- Nawale JM, Chaurasia AS, Borikar NA, Nalawade DD, Shah MM, et al. (2019) Single Center 7 Year Experience of Coronary Artery Perforation: Angiographic and Procedural Characteristics, Management and Outcome. Heart Views 20: 93-100.
[CrossRef] [Google Scholar] [PubMed] [Research Gate]
- Kinnaird T, Anderson R, Ossei-Gerning N, Cockburn J, Sirker A, et al. (2017) Legacy Effect of Coronary Perforation Complicating Percutaneous Coronary Intervention for Chronic Total Occlusive Disease An Analysis of 26 807 Cases From the British Cardiovascular Intervention Society Database. Circ Cardiovasc Interv 10: e004642.
[CrossRef] [Google Scholar] [PubMed] [Research Gate]
- Rogers JH, Lasala JM (2004) Coronary artery dissection and perforation complicating percutaneous intervention. J Invasive Cardiol 16: 493-499.
[CrossRef] [Google Scholar] [PubMed] [Research Gate]
- Dippel EJ, Kereiakes DJ, Tramuta DA, Broderick TM, Shimshak TM, et al. (2001) Coronary perforation during percutaneous coronary intervention in the era of abciximab platelet glycoprotein IIb/IIIa blockade: an algorithm for percutaneous management. Cathet Cardiovasc Interv 52: 279-86.
[CrossRef] [Google Scholar] [PubMed] [Research Gate]
- Brilakis E (2017) Manual of Chronic Total Occlusion Interventions 2nd Edition Elsevier.
[CrossRef] [Research Gate]
- Chin Yong A, Tan Wei Chieh T (2013) Coronary Perforation Complicating Percutaneous Coronary Intervention A Case Illustration and Review. ASEAN Heart J 21: 3.
[CrossRef] [Google Scholar] [PubMed] [Research Gate]
- Teis A, Fernández-NofrerÃas E, RodrÃguez-Leor O, Tizón H, Salvatella N, et al. (2010) Coronary Artery Perforation by Intracoronary Guidewires: risk factors and clinical outcomes. Rev Esp Cardiol 63: 730-734.
[CrossRef] [Google Scholar] [PubMed] [Research Gate]
- Christopoulos G, Luna M, Brilakis ES (2015) The clinical implications of balloon rupture during cardiovascular interventions. J Invasive Cardiol 27: E45-50.
[CrossRef] [Google Scholar] [PubMed] [Research Gate]
Received: XXXXXXXX; Accepted: XXXXXXXX; Published: XXXXXXXX
Citation: XXXXXXXX
Copyright: © XXXXXXXX
Competing interests: The authors have declared that no competing interests exist.
Sources of funding: GB´s PhD-project on ethical challenges and decision-making in nursing homes has been financially supported by the Norwegian Extra Foundation for Health and Rehabilitation through EXTRA funds (grant no. 2008/2/0208).
Copyright: This is an open access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.