International Exchange - (2010) Volume 18, Issue 5
1Clinical Resident, Department of Neurology, Cleveland Clinic Florida, USA
2Senior Lecturer in Psychiatry, Department of Clinical Medical Sciences
3Lecturer in Chemical Pathology, Department of Paraclinical Sciences
4Nephro logy Department, National Medical Center "La Raza", IMSS, Mexico City, Mexico
5Professor of Anatomy, Department of Preclinical Sciences Faculty of Medical Sciences, The University of the West Indies, St Augustine, Trinidad
Received date: 29 November 2009; Accepted date: 13 April 2010
Background The scientific literature is deficient in studies looking at the achievement of primary care diabetes treatment targets as stipulated by best practice guidelines in the Caribbean. Aims Assessment of treatment goals attained by patients according to the Caribbean Health Research Council (CHRC)/Pan-American Health Organization (PAHO) guidelines for diabetes management in primary care centres in North Trinidad. The primary interest of this study was the extent to which stated intermediate outcomemeasures were achieved. Secondarily, process measures and adherence to specific recommendations on pharmacotherapy were evaluated. Methods This was a cross-sectional study where 225 patients with diabetes from five primary care centres were interviewed in October and November 2007. Data collected included age, sex, ethnicity, religious background, educational level and duration, diabetes type and duration since diagnosis, the presence of hypertension, current blood pressure, level of physical activity and current medications. Last documented serum cholesterol and HbA1c within the past year were obtained from patient records. Anthropometric measurements recorded were weight, height and waist and hip circumferences. Results Of patients with available values, 49.3% achieved the target total cholesterol of less than 200 mg/dL while 56.6% had an HbA1C level of less than 6.5%. Only 47.7% attained a blood pressure target of less than or equal to 130/80 mmHg. 25.2% had a Body Mass Index (BMI) of less than 25 kg/m2. For waist circumference measurements, 40.8% of males and 2.1% of females were within recommended limits. Only 13.5% had 20 minutes or more of at least moderate exercise daily. No patient met all recommended target values for these six parameters. ConclusionsThere is poor achievement of treatment goals as set by best practice diabetes management guidelines. Results from this study may serve to inform primary care strategy revisions aimed at more widespread achievement of control targets which would ultimately abate the burden of illness in this population.
Caribbean, diabetes mellitus type 2, goals, guidelines, primary care
The human and economic cost of diabetes is primarily due to preventable complications which can be minimised with appropriate disease management.[1] In this regard, the scientific community has been active in establishing and revising diabetes guidelines for best clinical practice based on available evidence.[2,3] It has been argued that international guidelines may not fully apply to practice in developing countries. This was one reason why the CHRC in collaboration with the PAHO published the revised manual Managing Diabetes in Primary Care in the Caribbean in 2006.[4] It took into account the most recent international guidelines and regional expert opinions on the management of hypertension, diabetes, obesity and related dyslipidaemia. The manualwas geared to the culture, economic situation and healthcare systems in the Caribbean and was designed to serve as a key tool in improving patient care.
The target treatment goals for the various lifestyle, clinical and biochemical outcome measures were intended for patients with both type 1 and type 2 diabetes. However, the recommendations on exercise, BMI and waist circumference were pertinent to obesity as it impacts type 2 diabetes. It was left to the clinician to make individualised targets for these three parameters in patients with type 1 diabetes. The manual was distributed in the English-speaking Caribbean among primary care doctors, nurses, nurse practitioners and other healthcare personnel involved in the care of persons with diabetes.
Trinidad and Tobago is a twin-island republic and the most southerly nation in the Caribbean archipelago. It has a population of approximately 1.26 million, with a male to female ratio of 1:1. There are two major ethnic groups, with those of African and East Indian ancestry comprising 37.5% and 40.0% respectively. Those with ‘mixed’ ancestry constitute 20.5%.5 The local prevalence of diabetes mellitus has been estimated at 8% to 16% in Africans and 20% in East Indians.[6]
The public health services are provided under the Ministry of Health which utilises five Regional Health Authorities as managerial bodies. The country is divided into nine counties (eight in Trinidad, one in Tobago), each of which is managed by a County Medical Officer of Health. The county subdivision of St George Central has a total population of approximately 200 000 with roughly 58% of African, 20% of East Indian and 21% of ‘mixed’ ancestry.[5] There are 11 primary care health centres serving this northern catchment area which comprises both urban and rural populations.
The primary healthcare providers within this public health delivery system are expected to follow the guidelines of the CHRC/PAHO manual as it applies to managing patients of the diabetes clinics in the different health centres. To date, there has been little formal assessment of diabetes management in the context of meeting recommended guidelines within this setting. This paper seeks to achieve this objective, evaluating intermediate outcome and process measures using data collected from health centres in the county subdivision of St George Central.
The study was cross-sectional in design and consecutive sampling was employed.
Subjects
We included diagnosis confirmed patients with both type 1 and type 2 diabetes attending primary care health centres in the county subdivision of St George Central, Trinidad.
All patients attending the diabetes clinics in the five selected health centres within the course of the study period were asked to participate. The El Socorro, Aranguez, Morvant, Santa Cruz and Success/Laventille health centres participated in this study. These five health centres in the St George Central County were chosen primarily based on proximity, ease of accessibility and convenience.
Out of a total of 254 patients approached during the period from 28 October to 29 November 2007, 225 patients were interviewed. Patients were interviewed consecutively by appointment date and time of their visit to the diabetes clinic.
Inclusion and exclusion criteria
All participants were documented, diagnosis confirmed patients with either type 1 or type 2 diabetes (an established prerequisite for enrolment into all five diabetes clinics). The diagnosis of diabetes was met as per the American Diabetes Association (ADA) criteria.[7] Patients must have been seen during their scheduled clinic appointments within the sample timeframe: 28 October to 29 November 2007.
Patients who had already been seen in the diabetic clinic within the study timeframe were excluded. This included patients attending more than one of the five selected health centre clinics in the study (to prevent possible measurement bias).
Informed signed consent was obtained from all participants and all reasonable steps were taken to maintain patient confidentiality.
The CHRC/PAHO manual Managing Diabetes in Primary Care in the Caribbean includes targets for total cholesterol (<200 mg/dL),HbA1c (<6.5%), blood pressure (<or=130/80 mmHg), BMI (18.5–25 kg/m2), and waist circumference (males <37 inches, females <32 inches). Individualised needs preclude the posting of well-defined exercise targets but the manual does state ‘regular aerobic activity should be sustained for 30–60 minutes at least five times weekly. The level and intensity of physical activity should be guided by age and ability of the patient’.
The primary interest of this study was the extent to which recommended intermediate outcome targets were achieved. A secondary objective of the study was the evaluation of relevant process measures.
Interviewers administered a demographic and health status questionnaire. Interviewers consisted of research staff from the Department of Paraclinical Sciences as well as volunteer medical students fromthe University of the West Indies, St Augustine, Trinidad. All interviewers had attained at least tertiary-level education and were trained by the investigators in the standardised administration of the study questionnaire. Data collected included age, sex, race, religious background, education level and duration, diabetes type and duration since diagnosis, the presence of hypertension and level of physical activity. The various assigned categories of exercise (light, moderate, strenuous, very strenuous) were defined by the guide to physical activity levels in the CHRC/PAHO manual. Current blood pressure, weight, height, waist and hip circumferences and medications were recorded. Last documented blood cholesterol and HbA1c values within the past year were also obtained from clinical records. Patients willingly asked their primary care physicians during the encounter to provide these values on paper, and these were subsequently shared with the interviewer. This strategy was employed to minimise the loss of confidentiality that might have occurred if the entire clinical record had been accessed (even with consent) for the study. The patients’ current medication data were collected because of another secondary objective of looking at adherence to the pharmacotherapy recommendations also found in the CHRC/PAHO manual. Data were analysed using SPSS for Windows, Version 12.
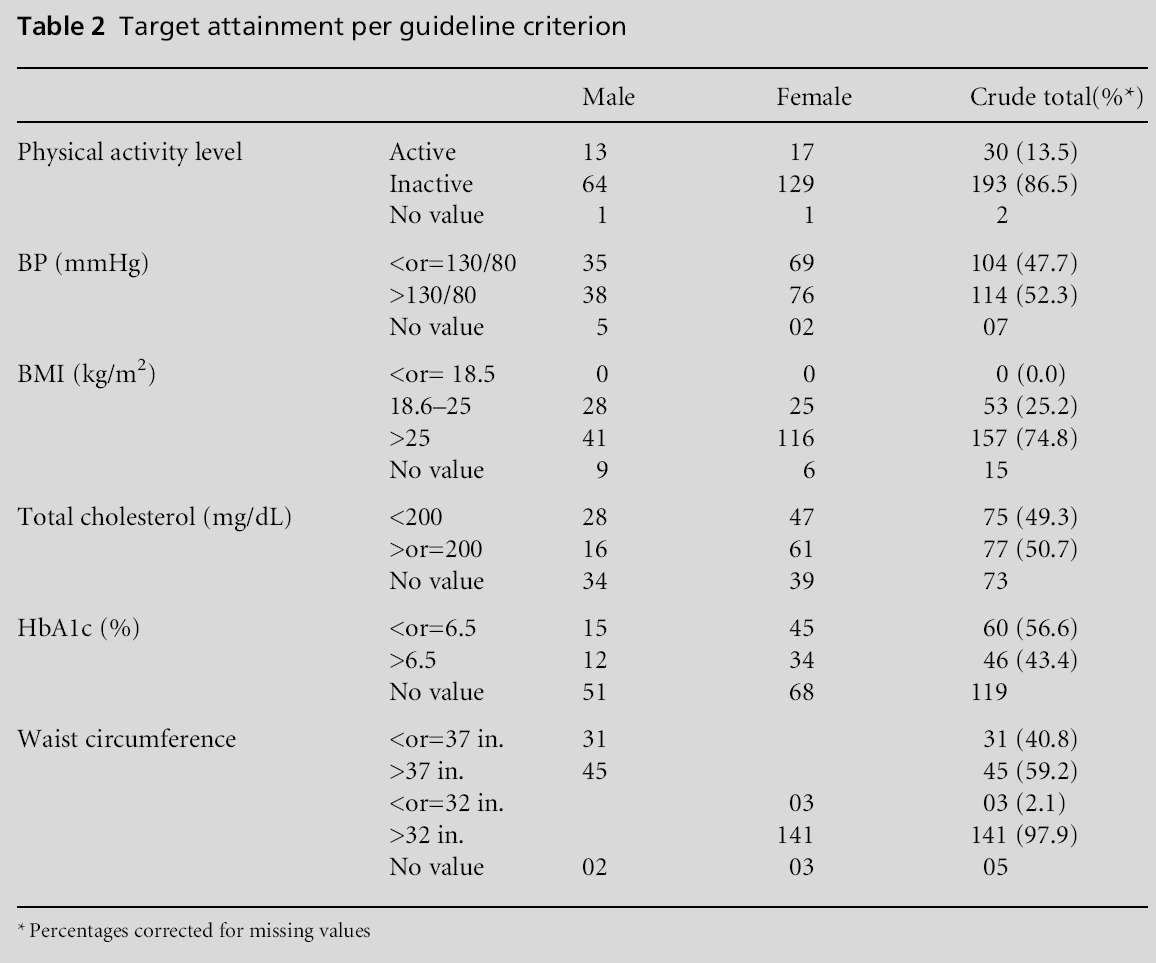
Tables 1 and 2 outline the baseline demographic characteristics and health status data for our study population.
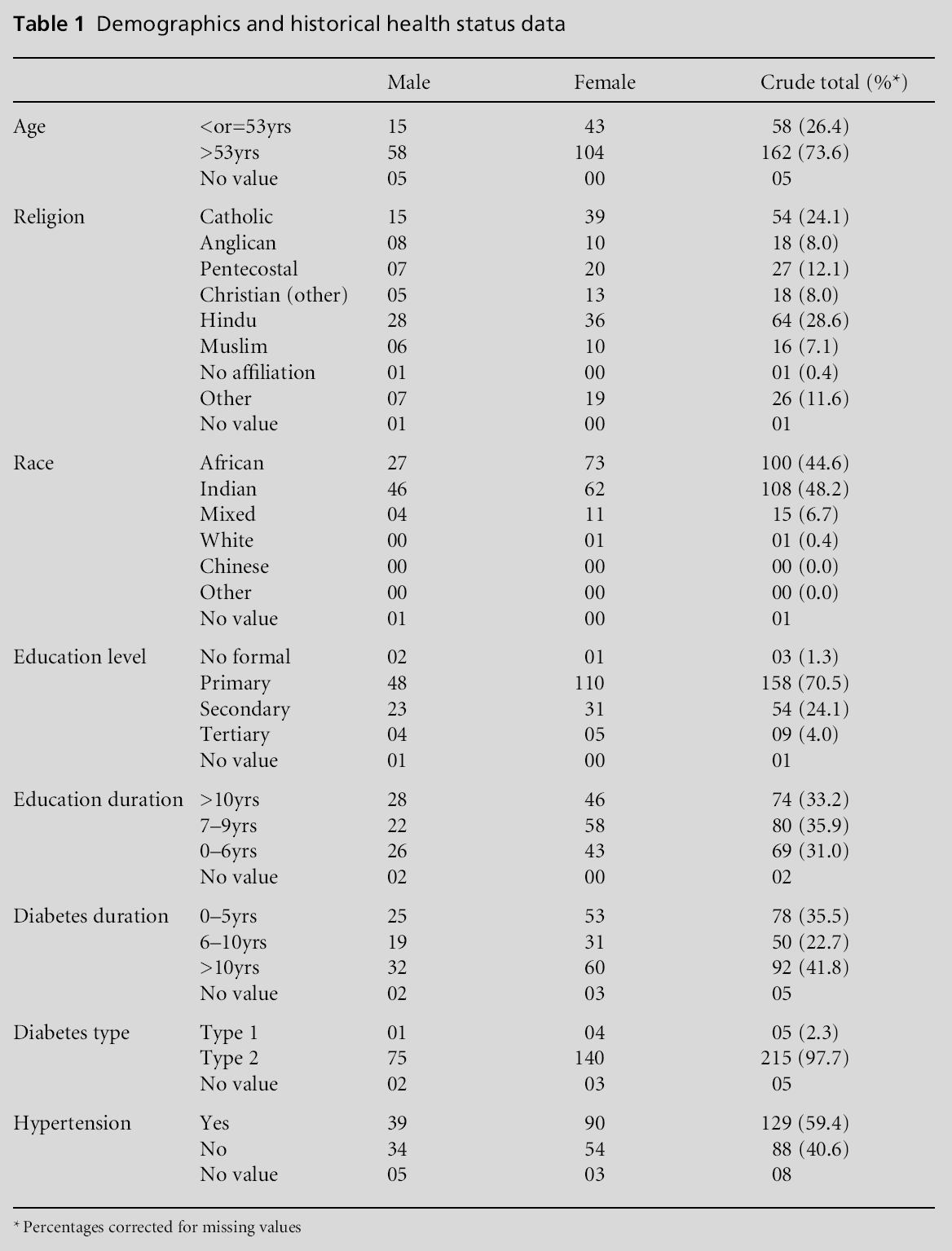
There were 225 diabetics (response rate 88.6%) interviewed in our study: 78 males and 147 females. The mean age for females was 60.27 years compared to 62.47 years for males. The ethnic distribution was 44.6% African, 48.2% East Indian, 6.7% mixed and 0.4% Caucasian. The average duration since diagnosis of diabetes was ten years with two patients having had a diagnosis for about 41 years. There were only four patients with type 1 diabetes in the sample.
The frequency of attainment of targets for each guideline criterion is shown in Figure 1. This shows data on the intermediate outcome measures which we were primarily interested in. Secondarily, we were able to analyse process data. Only 87 patients in the sample had values recorded for all six relevant target parameters: blood cholesterol, HbA1C, blood pressure, waist circumference, BMI and exercise; 67.6% of the sample had serum cholesterol values while 47.1% had HbA1C levels recorded in the past year. Of those with available values, 49.3% had attained the target total cholesterol of less than 200 mg/dL, while 56.6% achieved the target for HbA1C of less than 6.5%. Only 47.7% of the patients with diabetes surveyed had a recorded blood pressure meeting the target of less than or equal to 130/80mmHg. Those with a BMI in the target range of 18.5 to 25 kg/m2 constituted 25.2% of patients. For waist circumference measurements, 40.8% of males were below the recommended The frequency of attainment of targets for each guideline criterion is shown in Figure 1. This shows data on the intermediate outcome measures which we were primarily interested in. Secondarily, we were able to analyse process data. Only 87 patients in the sample had values recorded for all six relevant target parameters: blood cholesterol, HbA1C, blood pressure, waist circumference, BMI and exercise; 67.6% of the sample had serum cholesterol values while 47.1% had HbA1C levels recorded in the past year. Of those with available values, 49.3% had attained the target total cholesterol of less than 200 mg/dL, while 56.6% achieved the target for HbA1C of less than 6.5%. Only 47.7% of the patients with diabetes surveyed had a recorded blood pressure meeting the target of less than or equal to 130/80mmHg. Those with a BMI in the target range of 18.5 to 25 kg/m2 constituted 25.2% of patients. For waist circumference measurements, 40.8% of males were below the recommended 338 JA Morren, N Baboolal, GK Davis et al limit of 94 cm (37 inches) and only 2.1% of females were below their benchmark of 80 cm (32 inches). Just 13.5% of the sample reported taking more than or equal to 20 minutes of at least moderate exercise on average per day. The distribution of patients meeting different numbers of these guideline targets is illustrated in Figure 2.
Patients taking statins represented 41.1% of the sample, whereas 69.2% were taking aspirin. Of the 126 patients with both diabetes and hypertension, 59.5% were on a thiazide and 65.1% were taking an angiotensin converting enzyme (ACE) inhibitor/ angiotensin II receptor blocker (ARB).
Our sample, comprising almost twice as many females as males, may reflect differences in healthcare seeking behaviour at local primary care facilities. Similar differences have been reported in several West Indian studies in the past.[8–10] Although county statistics show that there are three times as many people of African as there are of East Indian ancestry, in our sample the ratio for both ethnicities was approximately 1:1. We believe the major reason for this disparity is the difference in prevalence of diabetes between these two groups, Indo-Trinidadians being affected more than twice as frequently.[6]
The average duration since diagnosis of diabetes was ten years. This is similar to previous findings in comparable studies. That done by Duff, O’Connor, McFarlane-Anderson et al (2003) in Jamaica reported a mean duration of diabetes in men of seven years and in women of 10.5 years.[10]
Approximately one-third of the patients sampled had had no blood cholesterol measurements over the previous year, and of those that did about half had unacceptably high levels. This lack of cholesterol measurements was also mirrored in other local data where only 51.8% had had lipid profiles done within one year.8 This shows inadequate cardiovascular risk assessment in this high-risk patient group. A recent study by Tomkin[11] reinforces that treatment of diabetic dyslipidaemia is essential in reducing cardiovascular disease in diabetes.
Monitoring of glycaemic control in the local primary care setting has changed markedly over the years. In the paper by Mahabir and Gulliford the proportion of patients with a blood glucose test in the preceding year increased from 33% in 1993 to 91% in 2003.[12]
Since HbA1c has emerged as the current standard for evaluating glycaemic control, one would have expected to see a similarly high rate for this test. Nonetheless, the finding that HbA1c was done in only half our sample was not as low as the 1.6% to 7% seen in the study by Pinto Pereira, Hinds, Ali et al.8 This implies that the healthcare team has little objective feedback on glycaemic control for many patients, leading to uninformed decisions regarding management.[13] Of the minority of patients who had had HbA1c reported in the past year, almost half had missed the target of less than or equal to 6.5%. This finding was comparable to that obtained by Apparico, Clerk, Henry et al from a similar primary care setting in Trinidad.[14] Another local study also reported 54% of the patients in 2003 as having ‘poor’ blood glucose control.[12] Bobb, Gake, Manmohan et al in yet another Trinidadian study found 61.5% of their sample ‘well-controlled’ but their acceptable upper limit for HbA1c was 7.0%.9 This confirmation of poor blood glucose control in the majority of patients in our study reinforces the need for recommended three- to six-monthly HbA1c evaluations.
A little over half our sample had blood pressures exceeding the recommended target of 130/80 mmHg. Duff, O’Connor, McFarlane-Anderson et al described 73% as being over this limit in their study.10 Schernthaner commented that ‘aggressive blood pressure control may be the most important factor in preventing adverse outcomes in patients with type 2 diabetes’.15 Considering that the Managing Diabetes in Primary Care in the Caribbean manual states that systolic pressure of less than 120 mmHg is a desirable target, the need for remedial measures is justified. Cunningham found poor knowledge and understanding of hypertension among African Caribbean people with type 2 diabetes.[16]
Comorbid obesity was especially high in our sample. Three-quarters of the patientswith diabetes had a BMI greater than 25 (overweight or obese) which compared to 81% in a recent Jamaican study which described a cultural basis for acceptance or even ‘glamourisation’ of obesity.[10] The prevalence of obesity in our sample was supported by waist circumference where most males and nearly all females exceeded acceptable measurement limits. Additionally, 86.5% had inadequate levels of physical activity (less than ‘moderate’) which may have contributed to the high rates of obesity.[17] This is concerning given that in a previous Trinidadian study the lifestyle advice recorded by clinicians in 1993 and 2003 had increased significantly, from 35% to 67% for diet and 3% to 61% for exercise.12Our findings are comparable to the Jamaican study by Duff, O’Connor, McFarlane-Anderson et al where 71% exercised for fewer than 3.5 hours per week, with 32% reported taking no exercise.10 de Lusignan, Sismanidis, Carey et al (2005) found similar results for BMI in a British primary care population with diabetes: the authors noted that BMI under 25 kg/m2 fell from 27.0% in 1994 to 19.4% in 2001, indicating that the prevalence of obesity in the diabetic population is rising.[18]
Our study revealed that approximately three-quarters of the patients with diabetes had two or more additional cardiovascular risk factors and were candidates for specific pharmacotherapy as indicated in the CHRC/PAHO guidelines. Indeed, evidence supports the view that statins should be prescribed to all diabetics, unless a specific contraindication exists.[19] Only 41.1% of our sample were on statins.[20] Over twothirds of patients in the sample, however, were on aspirin.
Of the almost 60% of patients with diabetes and concomitant hypertension, two-thirds were on an ACE inhibitor/ARB and a similar fraction were on a thiazide diuretic. Mahabir and Gulliford found a lower use of thiazides (38%) and a similar rate of ACE inhibitor use (72%).[12] The high use of thiazides in our sample accords with the recommendation for thiazides as the antihypertensive of first choice in diabetes.[21] The Managing Diabetes in Primary Care in the Caribbean manual reaffirms that there is compelling evidence for earlier use of ACE inhibitors/ ARBs in patients with diabetes since their use has been shown to improve cardiovascular outcomes in high-risk patients with or without hypertension.[22] Arguably, as is the case with statins and aspirin, a significant proportion of patients for whom ACE inhibitors/ARBs are indicated may not be receiving these medications due to a history of drug allergy or intolerance. Remarkably, about two-thirds of the patients known to be comorbidly hypertensive had high blood pressure readings on the day they were interviewed, which highlights the need for better management of hypertension.[15,23]
No patient achieved all the recommended target values for HbA1c, total cholesterol, blood pressure, BMI, waist circumference and exercise. There was one patient who met targets for five parameters but not that for exercise. 61.3% of the sample had at least one missing value out of six and therefore could not be fully assessed. The results we found were similar to the 2008 Norwegian study by Jenssen, Tonstad, Claudi et al in which only 13% reached the combined targets for glucose, blood pressure and cholesterol control.[24] A comparable 2004 American study of 218 primary care patients looking at target attainment using the American Diabetes Association (ADA) guidelines showed better results: the mean number of ADA treatment goals attainedwas 4.9 out of a possible ten.[25]
Mahabir and Gulliford found that in spite of changes in the processes of care, there were no changes in intermediate outcomes including glycaemic control, blood pressure or body weight.[12] Bryant and colleagues noted, in a recent review, that the diabetes guidelines seem ‘easier to preach than to practise’.26 Ra¨tsep, Kalda, Oja et al also concluded that practice guidelines may be a useful source of information but they should not be overestimated.[27]
The sample size and study timeframe were limited by the resources available. The five health centres in the St George Central County were primarily chosen for proximity and ease of access. Thus we employed both convenience and consecutive sampling. These nonprobability sampling methods may not represent the reference population accurately and these results cannot be extrapolated to all patients with diabetes receiving primary care in North Trinidad.
The characteristics (including reason for refusal) of non-respondents (11.4%) would have been useful in the assessment of selection bias.
It would have also been useful to document the proportion of clinicians who had actually read the Managing Diabetes in Primary Care in the Caribbean manual. One would expect that physicians who were unaware of the practice guidelines would be less likely to have patients attaining target goals. Notably, in a 2003 Trinidadian study only 44% of clinicians had actually read the recent guidelines on diabetes care.[12]
For the small minority (1.78%) of the sample with type 1 diabetes BMI, waist circumference and exercise target non-attainment may have been overvalued since the clinical implication in this group is usually less adverse. The other parameters assessed were quite
applicable to the optimal management of patients with type 1 diabetes, justifying their inclusion in the study.
We may have underestimated target non-attainment since non-attendees are less likely to adhere to treatment
There should be more rigid adherence to the recommended schedule for three- to six-monthly HbA1c and annual fasting lipid profiles. Our findings highlight the need for more effective implementation of therapies that would optimise disease control.
Targeted strategies must be employed to address the issue of weight loss not only by diet but also through exercise.
Primary care physicians should frequently reassess patients to ascertain their eligibility for statin, aspirin, thiazide and ACE inhibitor/ARB use as advised by evidence-based guidelines.
We need to continually assess compliance with best practice guidelines for diabetes management in our primary care setting. Data collected from these evaluations may serve to inform critical strategy revisions geared towards more widespread achievement of control targets. This would help reduce the burden of illness seen in this vulnerable population.[28,29]
The authors would like to thank Dr Harry Singh (CMOH, St George Central County), Ms Teppany Skinner, Ms Jaya Ramchandani and Mr Steve McKell for their invaluable contributions.
The majority of work involved in this projectwas done on a voluntary/non-fee basis. The minimal expenses incurred were covered by funds allocated to faculty research by the University of the West Indies, St Augustine, Trinidad and Tobago
Ethical approval was obtained from the Ethics Committee of the Faculty of Medical Sciences, the University of the West Indies, St Augustine, Trinidad and Tobago
Not commissioned; externally peer reviewed.
None.