Akshay A Bafna1*, Varun Deokate1, Prama Bagani1, Sai Prasad2, Majid mulla1 and Varun Bafna1
1Rajarshi Chhatrapati Shahu Maharaj Government Medical College, Kolhapur, Maharashtra, India
2Diamond hospital, Kolhapur, Maharashtra, India
- Corresponding Author:
- Bafna AA
Rajarshi Chhatrapati Shahu Maharaj Government Medical College
Kolhapur, Maharashtra, India
E-mail: drbafnaakshay@gmail.com
Received Date: November 03, 2021; Accepted Date: November 15, 2021; Published Date: November 22, 2021
Citation: Bafna AA, Deokate V, Bagani P, Prasad S, Mulla M, et al (2021) Acute Lower Limb Ischemia as Presenting Symptom in Case of Infra Renal Coarctation of Aorta: A Rarity. Interv Cardiol J Vol.7 No.11:158
Copyright: © 2021 Bafna AA, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Keywords
Acute ischemia; Aorta; Coarctoplasty; Infra-renal coarctation; Middle
aortic coarctation (MAC); Toe
Introduction
Middle aortic coarctation (MAC) or abdominal aortic stenosisis
an extremely rare form vascular anomaly with almost 200 cases
reported in literature [1]. On the basis of location, it is further
classified as supra-renal, inter-renal and infra-renal coarctation
of aorta. Hypertension proximal to the aortic coarctation
and comparative hypotension distal to it are characteristic
investigative finding in MAC. The clinical manifestations of
MAC include headache, fatigue on slight exertion and bilateral
lower-limb claudication [2]. By the best of our knowledge on the
available literature, we arepresenting first-time the case of infrarenal
coarctation of aorta presented with left lower limb acute
ischemia.
Case Report
A 40-year-old female presented to Diamond Hospital, Kolhapur,
and Maharashtra, India on 13 August 2021 with a complaint
of black discoloration of thirdsmall toe of left lower limb from
2 days and pain from 3-4 days (Figure 1A). She had no past
medical history with any coronary artery disease risk factors. She
reported two successful and uneventful pregnancies. Her blood
pressure was measured as 149/96 mm of Hg with pulse rate
of 120/minute on examination. There were weak pulses noted
bilaterally in left lower limb; however, rest of the other physical
examination and pulsation were within normal limit. The routine blood investigations, including ANA blot test, were within normal
range and ruled out autoimmune disorders. Electrocardiography
revealed sinus tachycardia with no other abnormality. The 2D
echocardiography reported Left ventricular ejection fraction
(LVEF) 60%, and other structures as well dimensional parameters
were within normal limit. A Doppler ultrasonography of abdomen
and lower limb revealed a significant narrowing of abdominal
aorta. There was monophasic blood flow in left lower limb arteries,
bilaterally, with gradient across the coarctation measured as
86 mm of Hg. A computed tomography angiogram reported a
narrow aortic segment of 18.6 mm in length present below the
origin of renal arteries. The diameter of aorta at diaphragm was
16.0 mm, whereas pre and post-coarctation werenoted as 18.2
mm and 16.7 mm, respectively (Figure 2A). The tightness of the
coarctation segment was reported as 6.0 mm (Figure 2A).These
findings suggested for the diagnosis of infra-renal coarctation
of aorta. Preoperative pharmacological management included
Aspirin 75 mg (OD); Clopidogrel 75 mg (OD); Atorvastatin 80
mg (HS); Rivaroxaban 2.5 mg (BID); Pentoxafyllin 40 mg (TID);
cilostazol 50 mg (BID); Telmisartan 40 mg (HS) and Amlodipine
5mg (HS) for optimal reperfusion and blood pressure control.
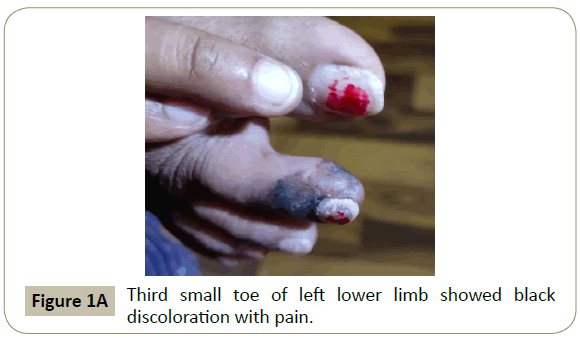
Figure 1A: Third small toe of left lower limb showed black
discoloration with pain.
The coarctoplasty was performed with consultation of
cardiovascular team, using ANDRA-Med balloon (14mm x 4 cm),
and ANDRA-MEDAS XL-43 (16mm x 4cm) stent was inserted
successfully and uneventfully after preserving bilateral renal
arteries (Figure 2B-E). Post coarctoplasty with stenting, the
pressure gradient across coarctation reduced from 86 mmHg to
12 mmHg.
The patient had an uncomplicated postoperative course. Postoperative
management included Aspirin 75 mg (OD); Atorvastatin
80 mg (HS); Rivaroxaban 2.5 mg (BID); Telmisartan 40 mg (HS)
and Amlodipine 5mg (HS). On day three postoperatively, the
pulses were noted normal in the left lower limb. The triphasic
pulse waveform restored in arteries of left lower limb bilaterally
was confirmed with Doppler ultrasonography (Figure 2F). The
gradient at the site of coarctation reduced to 12 mm Hg postoperatively.
A clinical improvement was observed in pain and
blackish discoloration (Figure 1B).
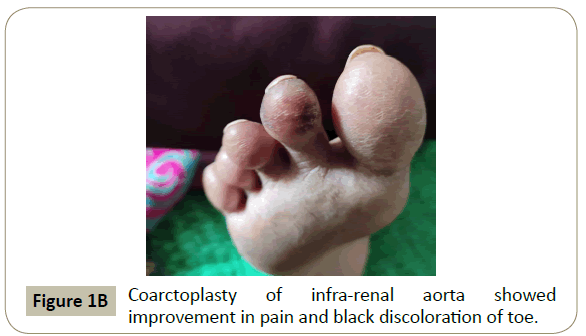
Figure 1B: Coarctoplasty of infra-renal aorta showed
improvement in pain and black discoloration of toe.
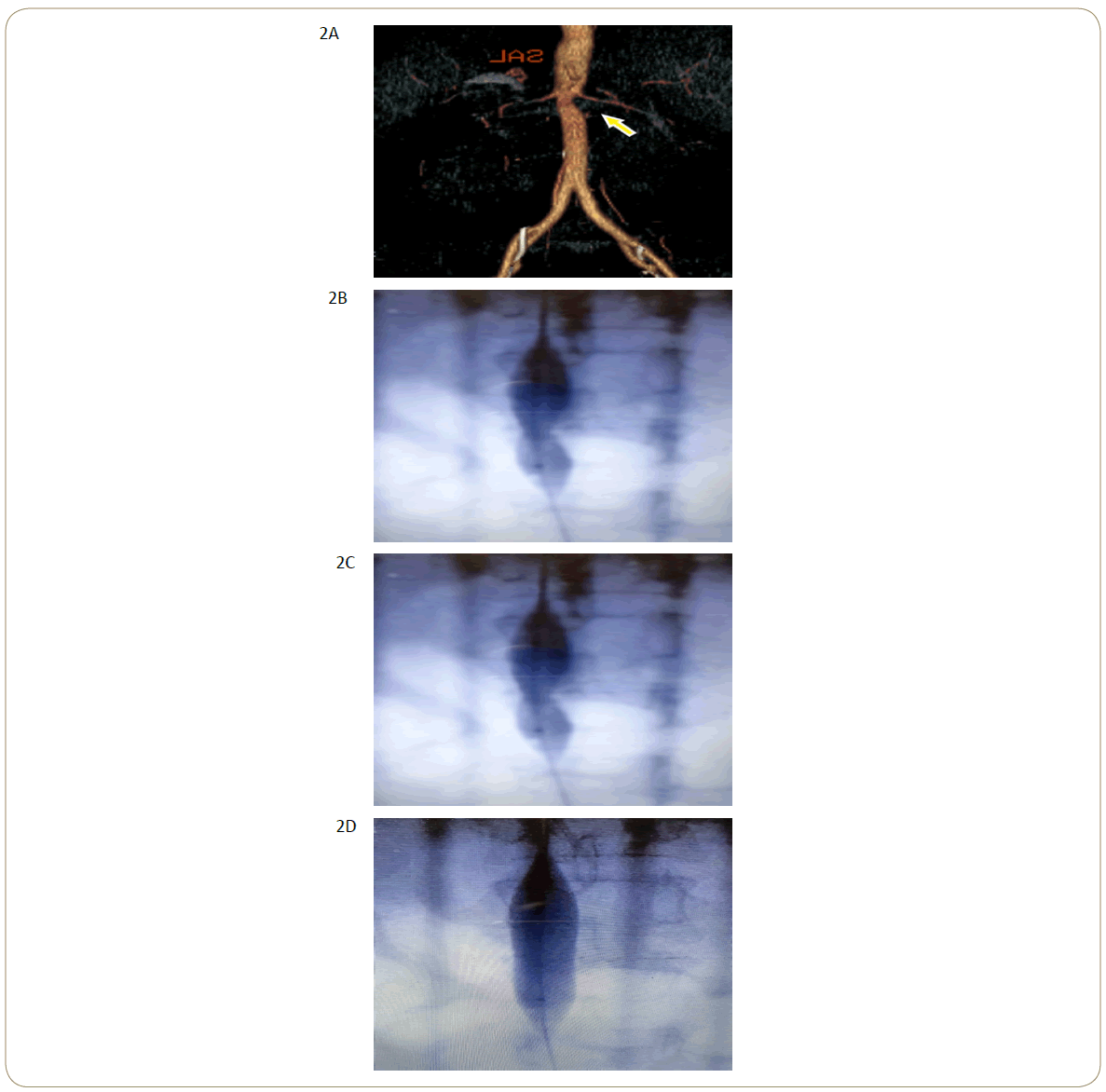
Figure 2: Computed tomography angiography of the abdominal aorta and both lower extremities of patient, before and after procedure
showing A, severe stenosis of abdominal aorta just below to origin of the renal arteries with pre and poststenotic dilation
associated with the evidence of infra-renal aortic stenosis; B-D, evidence of coarctoplasty using ANDRA-Med balloon (14 mm x 4
cm); E-F, evidence of an implantedANDRA-MEDAS XL-43 (16mm x 4cm) stent proximal to the renal arteries with a good patency of
abdominal aorta, ciliac artery, superior mesenteric artery, and renal arteries
Discussion
We demonstrated a rare case of infra-renal coarctation of the
aorta presented with acute left lower limb ischemia manifested
as pain and black discoloration of the third small toe.
Middle aortic coarctation (MAC) is an extremely rare vascular
anomaly with an occurrence rate of almost 0.002%. [3]. Though
the exact etiology of MAC is unknown, proposed causes of
MAC are congenital anomalous development, rubella infection
or syndrome; obliterative pancreatitis, and fibromuscular
dysplasias [4].
MAC has been classified as type I, suprarenal coarctation with
renal artery stenosis; type II, infrarenal coarctation with renal
artery stenosis; type III, suprarenal coarctation with normal
renal arteries; and type IV, infrarenal coarctation with normal
renal arteries [5]. In our case, infra-renal coarctation of the
aorta presented with normal renal arteries. However, on
presentation, her blood pressure was noted high (140/96
mmHg) than normal with a pulse rate of 120/minute. There
was no cardiovascular or another medical history; perhaps
this increased blood pressure might be due to infra-renal
coarctation of the aorta in this case.
The involvement of other arteries stenosis is also common
with MAC [1]. Surprisingly, there was no other arterial stenosis
observed in our patient. Our patient had none of the investigative
findings associated with the etiologic diseases or factors. The
routine blood investigations, including the ANA blot test, were
within normal range and ruled out autoimmune disorders in the
present case. Thus, we demonstrated a case with a rare type of
infrarenal abdominal aortic coarctation presented with acute
lower limb ischemia.
Conclusion
We reported the first case of infra-renal coarctation of aorta
presented with left lower limb acute ischemia which is a very
rare finding. Infra-renal coarctation of aorta or MAC may lead
to lower limb acute ischemia and tissue necrosis and may be
presented with painful and discoloration of tissue.
References
- Price TP, Whisenhunt AK, Policha A, Ayad MT, Gardiner GA, et al. (2014) Middle aortic coarctation. Ann Vasc Surg 28: e15-21.
- Delis KT, and Gloviczki P (2005) Middle aortic syndrome: from presentation to contemporary open surgical and endovascular treatment. Pers Vasc Surg Endovasc Ther 17: 187-203.
- Leoce BM, Dardik H, Bikkina M, Bernik TR (2017) Atypical infrarenal aortic coarctation. J Vasc Surg Cases Innov Tech 3: 96-7.
- Vincent D, Avantsa R, Tejaswi KV (2020) An Intriguing Case of Infrarenal Aortic Hypoplasia. Journal of Clin & Dia Res 14: 20-25.
- Fitzpatrick CM, Clouse WD, Eliason JL, Gage K, Podberesky DJ, et al. (2006) Infrarenal aortic coarctation in a 15-year-old with claudication. J Vas Sur 44: 1117.