International Exchange - (2011) Volume 19, Issue 5
Doctor, Department of Obstetrics and Gynecology, College of Medical Sciences, Delta State University, Abraka, Nigeria and Women’s Health and Action Research Centre
Afolabi Hammed
Women’s Health and Action Research Centre
Friday Ebhodaghe Okonofua
Professor,Women’s Health and Action Research Centre and Department of Obstetrics and Gynecology, College of Medical Sciences, University of Benin, Nigeria
Okpani Anthony Okpani
Professor, Department of Obstetrics and Gynaecology, College of Health Sciences, University of Port Harcour, Nigeria
Oyinkondu Collins Koroye
Doctor, Federal Medical Centre, Yenagoa, Nigeria
Sylvester Ojobo
Doctor, Ponders Medical Center, Benin City, Nigeria
Iyore Itabor
Doctor, Association of Private Obstetrics Providers in Nigeria, Asaba, Nigeria
Olakunle Daramola
Doctor, Women’s Health and Action Research Centre
Received date: 22 November 2010; Accepted date: 25 July 2011
Background Abortion is widespread in the Niger- Delta region of Nigeria, with resulting high rates of morbidity and mortality. It is thought that the private sector provides the majority of abortion services in Nigeria as a result of the restrictive abortion law in the country. The oil-rich Niger- Delta region accounts for 90% of the country’s resource, is economically active and has increased opportunities for sexual networking. Method This study assays the attitudes of staff at family planning (FP) services and practices of reproductive health and FP services among private practitioners in four states ofNiger-Delta of Nigeria (the states of Edo, Delta, Bayelsa and Rivers). ResultsWomen who had unwanted pregnancies were attended by 119 (87.5%) respondents. However, only 33 (24.0%) provided services for termination of pregnancy. Indeed, just over half (72; 53.4%) counselled women to continue the pregnancy while fewer (35; 25.9%) referred women to other clinics. However, there was no evidence to suggest that doctors followed up on those women counselled to continue their pregnancies. Most private sector service providers of abortion services in Nigeria (69.7%) are non-specialist doctors. ConclusionEducation of private practitioners in the principles of abortion, post-abortion care and FP is recommended to alleviate abortion-related morbidity and mortality in Nigeria.
abortion, family planning, Niger-Delta region, Nigeria, private practitioner, women’s health
Each year, an estimated 210 million women throughout the world become pregnant and about one in five of these women seek abortion. Out of 42 million abortions performed annually, 20.2 million are estimated to be unsafe and 97% of all unsafe abortions occur in developing countries.[1] The World Health Organization( WHO) defines unsafe abortion as a procedure for terminating an unwanted pregnancy either by persons lacking the necessary skills or in an environment lacking the minimal medical standards – or both.[2] The burden of unsafe abortion lies primarily in the developing world; the highest rates are in Africa and in Latin America and the Caribbean, followed closely by South and South-East Asia. At the opposite extreme, the rate of unsafe abortion in Europe and North America is negligible. A recent study found even more alarming data on the maternal mortality ratio in Kano, Nigeria, finding that 2420 women died of problems related to pregnancy and childbirth for every 100 000 live births.[3] Abortion is one of the major causes of maternal morbidity and mortality in most parts of sub-Saharan African countries.[4–6]
Previous research in Nigeria has shown that reproductive health service utilisation is influenced by sociocultural and religious considerations.[7] Women often seek services that are confidential, private and which they have adjudged to be of reasonable quality. Although the cost of services and attitudes of health providers are also important, the need for privacy is often uppermost in the minds of women seeking reproductive health services. A restrictive law that only allows termination of pregnancy to save the life of a woman has a significant influence on the increasing rate of unsafe abortion in Nigeria. The laws, introduced during British colonial rule in 1916, restricted abortion to saving the life of the woman. The criminal code was then adopted throughout the country and, 43 years later, the penal code was introduced to replace the criminal code in northern Nigeria in order to reflect the norms of British law in colonial India – India being an Islamic country, and Islam being the predominant religion in the northern region of Nigeria. The criminal code – sections 228, 229 and 230 – was retained in southern Nigeria.[5,8] Section 228 stipulates guilt of felony for persons that perform abortion and liability to a 14-year jail term. Section 229 prescribes guilt of felony for a woman who induces an abortion in herself or submits herself for abortion and liability to seven years imprisonment. Section 230 prescribes guilt of felony on a supplier of materials used for an abortion and liability to three years imprisonment.
The relevant sections of the penal code that operates in northern Nigeria are sections 232, 233 and 234.[5] Section 232 prescribes 14 years imprisonment, the option of a fine or both for the person who performs the abortion. In section 233, it is stipulated that if the procedure results in the death of the woman, the person who has performed it is liable to imprisonment which may extend to 14 years and is also liable to a fine. If the procedure was done without the consent of the woman, the person who undertook the procedure is liable to a jail term for life or less and is also liable to a fine. Section 234 prescribes punishment for someone who causes miscarriage unintentionally by force, if it was unknown that the woman was pregnant; the person is liable to three years imprisonment or a fine or both. Knowing that the woman was pregnant may cause the jail term to be extended to five years.
Social stigma and political pressure impair the ability of healthcare providers to offer abortion services and effective post-abortion family planning (FP) services even within the law. Consequently women experiencing unwanted pregnancies are unable to obtain effective safe abortion services and counselling within the public health sectors. By contrast, the private sector (especially private medical practitioners) provide a substantial proportion of the abortion services in many parts of the country.[8–11] Yet few use established effective and evidence-based methods that are available elsewhere. Thus, abortions provided by many private doctors may be unsafe.[8–11] This is confirmed by the experiences of many tertiary hospitals that treat women with induced abortion complication. [8–11] In addition, it is unknown howmanywomen receive any form of post-abortion FP counselling after having abortion by private practitioners to prevent the repetition of unintended pregnancy.
Private doctors are of great importance when it comes to expanding access to safe abortion and postabortion care services in Nigeria. Despite the preference for private medical practitioners for provision of FP and reproductive health services in Nigeria, there is currently limited information on the knowledge, attitudes and practice of abortion services and postabortion FP. This information is critically important, as it would justify the need for a retraining programme aimed at increasing the skills of private practitioners in rendering evidence-based services in relation to abortion and post-abortion FP as part of reproductive health service delivery in Nigeria.
The objective of this study was to determine the attitudes and practice of abortion services and postabortion FP in four states of the Niger-Delta region in Nigeria. The results will assist in designing an intervention programme aimed at scaling up abortion and post-abortion FP services for the prevention of at-risk pregnancy in Nigeria.
This study was undertaken as part of a project entitled ‘Expanding access to safe abortion to young underserved and vulnerable women through private practitioners’ initiatives in four states of the Niger-Delta region of Nigeria’ with the aim of using the results to design an intervention programme to improve abortion and post-abortion FP services in Nigeria.
The study was carried out by the Women’s Health and Action Research Centre, a non-governmental organisation located in Edo State in Southern Nigeria. The study was conducted as part of a needs assessment for a project aimed at building the capacity of private practitioners in delivering safe abortion services to young underserved and vulnerable women in four states of the Niger-Delta region: the states of Edo, Delta, Bayelsa and Rivers.
As part of the study, we obtained detailed lists of registered hospitals and clinics from the respective ministries of health of the four states. The lists obtained revealed that the major hospitals in these states employ an average of five to ten doctors. From the list obtained from each state, we used a simple ballot method to randomly select a total of ten hospitals and clinics with five private practitioners from each for inclusion in the study. Thus, a total of 200 private practitioners were expected to be sampled from the four states, 50 from each state. However, only 136 (68%) of the private practitioners who agreed to participate in the studywhen approached returned the completed questionnaires. Those that declined to respond, despite being part of the initial meeting where they were given the background to the study, were excluded from the study and were not followed up.
A pre-tested questionnaire with pre-coded responses was designed for this study based on the information obtained from an initial meeting with some of the private practitioners. The questionnaire was divided into four modules. The first module elicited information on the socio-demographic characteristics of the respondents which included age, sex, marital status, length of practice and area of specialisation. The second module obtained information on the characteristics of the clinic, facilities available and scope of services, while the third module sought specific information about knowledge, attitudes and practices relating to abortion services and management. Finally, the last module sought information about the provision of post-abortion FP services and sexually transmitted infection (STI) management. The questions on medical area of specialisation, most common health problems encountered in practice and who performed the abortion procedure had a category of response coded as ‘other’.
The questionnaires were self-administered and directed to the most senior practitioner in each of the private hospitals/clinics. A project coordinator visited the clinics to distribute the questionnaire and returned one week later to retrieve completed questionnaires. Respondents were assured of confidentiality and no names of persons were included in the questionnaires. The study was approved by the Ethical Review Board of the University of Benin Teaching Hospital.
Completed questionnaires were collated, coded, entered and analysed using the statistical package for social scientists (SPSS). Results are presented as simple descriptive statistics.
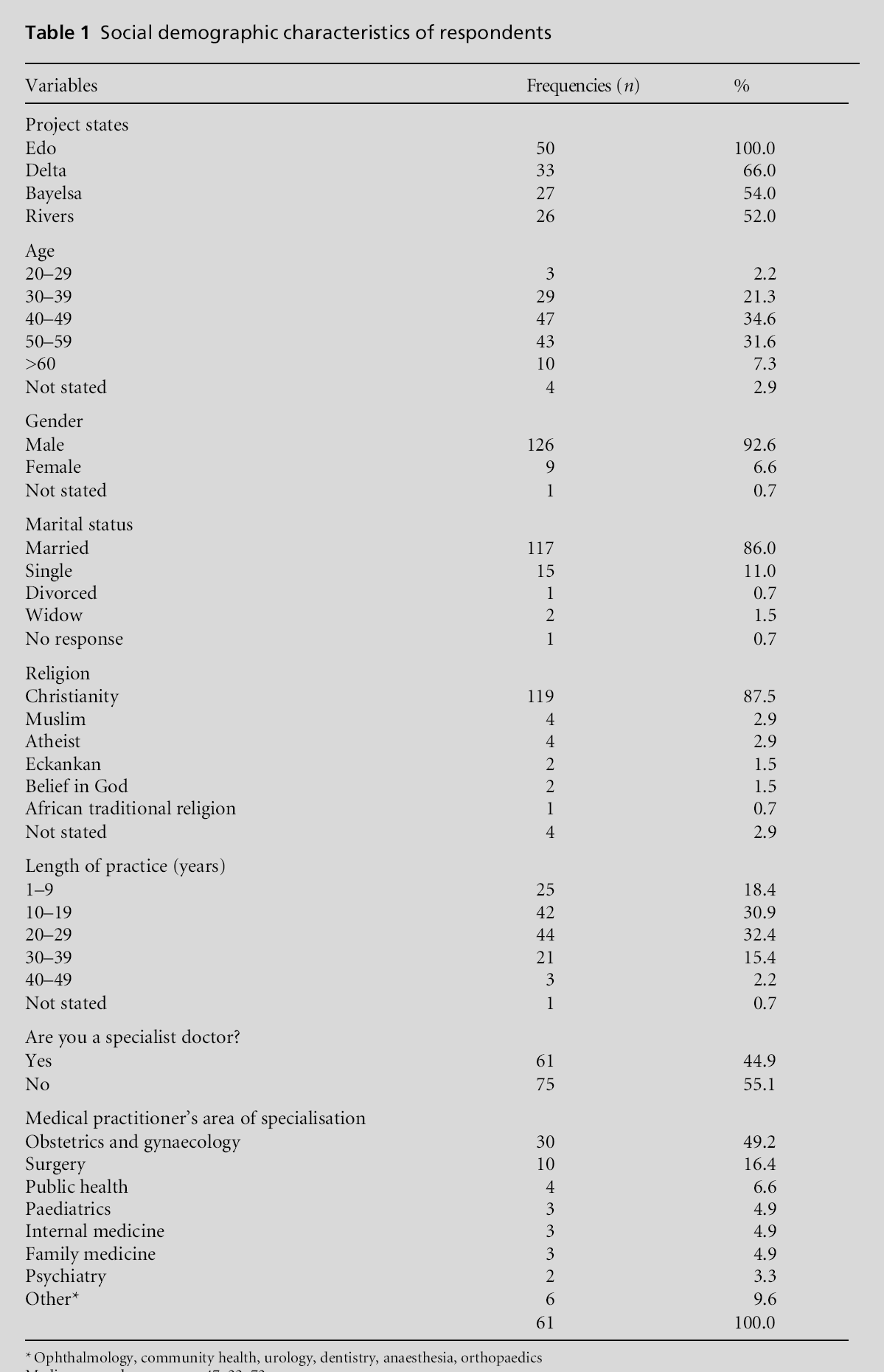
Two-hundred potential participants were sent questionnaires and 136 (68%) returned completed questionnaires, the rate varying by state (Table 1). The median age of respondents was 47 years (range 22–72 years), and most (87.5%) were in the 30–59 years category.Most respondents were male (92.6%), married (86.0%), Christian (87.5%) and had been in practice for between 10 and 29 years (63.3%). Fewer than half (44.9%) of the respondents were specialist practitioners and the leading specialty was obstetrics and gynaecology (44.9%) followed by surgery (16.4%).
The characteristics of the clinics/hospitals involved in the survey are presented in Table 2. The most commonly encountered health problems were unwanted pregnancy (87.5%), infertility (26.5%), pelvic inflammatory disease (19.9%) and malaria in pregnancy (18.4%).
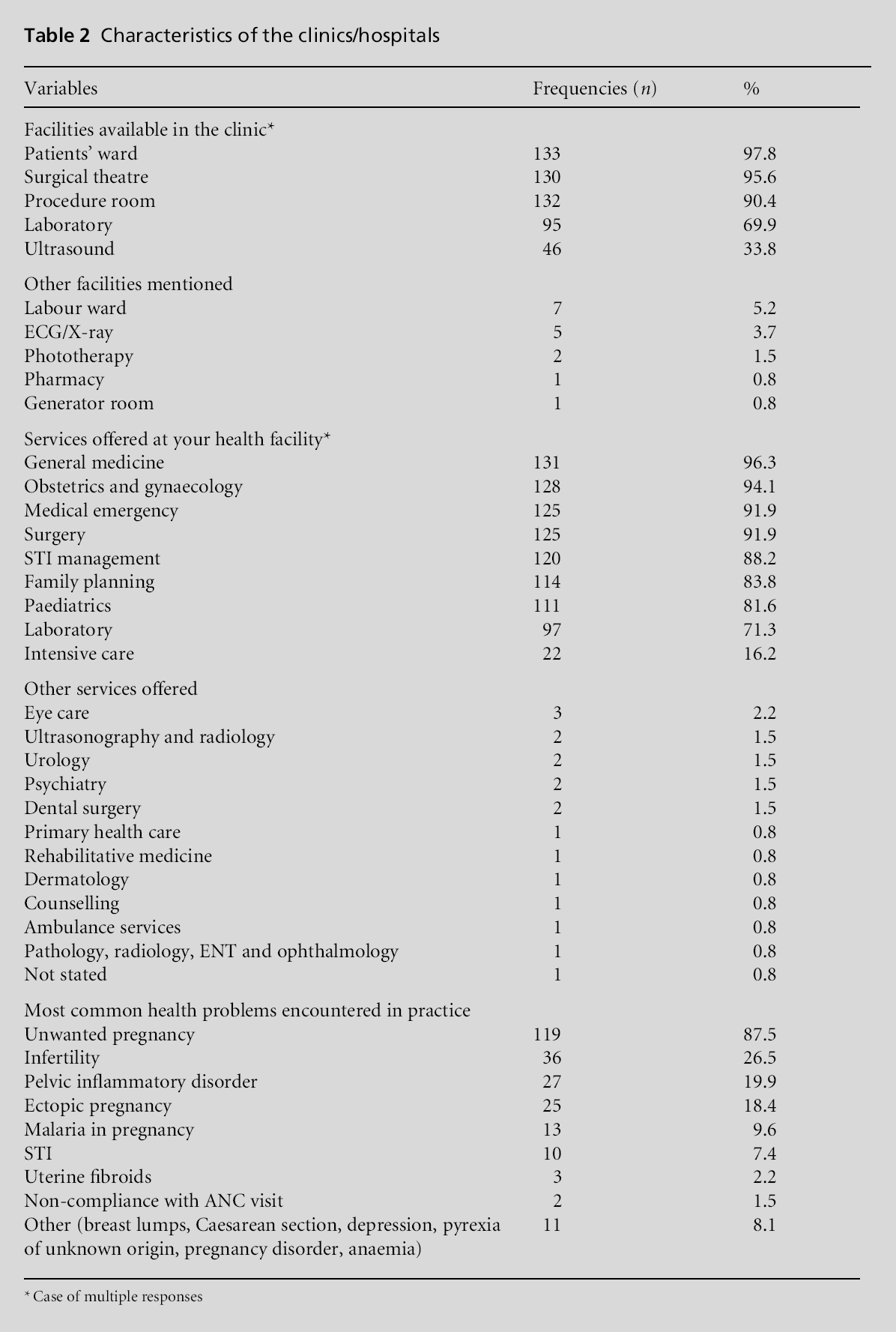
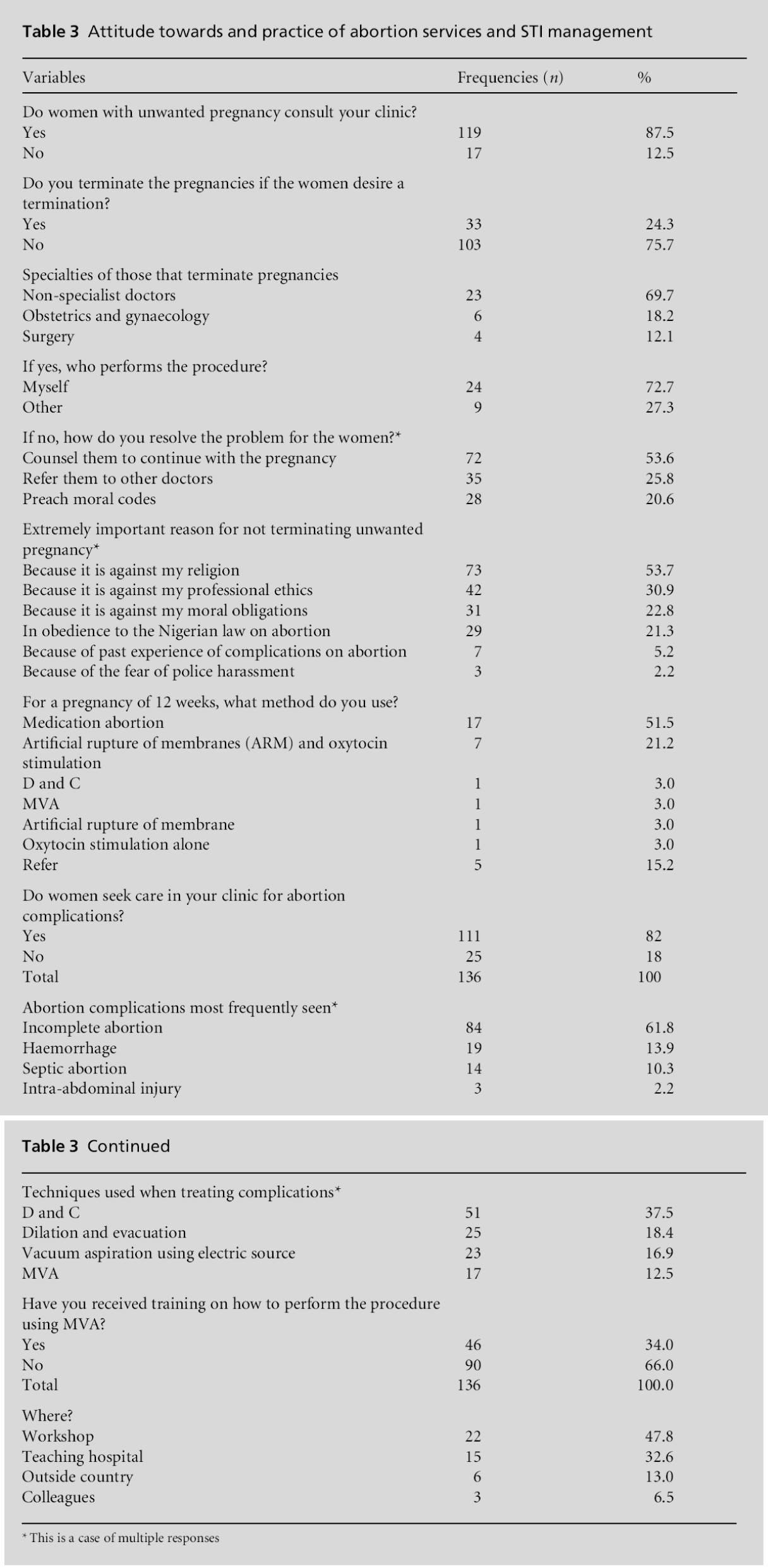
Table 3 shows respondents’ attitudes towards and practices of abortion and management of abortion complications and the source of training on the use of manual vacuum aspiration (MVA). Over two-thirds of respondents reported seeing womenwith unwanted pregnancy in their practice but only a quarter admitted to performing termination of pregnancy. Respondents largely (72.7%) provided abortion themselves in their clinics and those that did not provide abortion usually counselled clients to continue with the pregnancy (however, these clients were not followed up): a quarter referred them to other doctors or in one-fifth of the cases preached moral codes to clients. Reasons why respondents would not terminate pregnancies included religious grounds, professional ethics, moral obligations and Nigerian abortion law. The methods commonly used for early termination of pregnancy (less than 12 weeks) were MVA, medical abortion and dilatation and curettage (D and C). For later termination, medication abortion was the most frequently used method (51.5%) followed by amniotomy and oxytocin stimulation. Mifepristone alone and mifepristone combined with misoprostol was used for medical termination. Of the respondents, 82% reported that women with post-abortion complications sought treatment in their clinics and that incomplete abortion was the leading complication. Training in the use of MVA had been received by 34% of the respondents and this was mainly from workshops (47.8%) followed by training in a teaching hospital (32.6%).
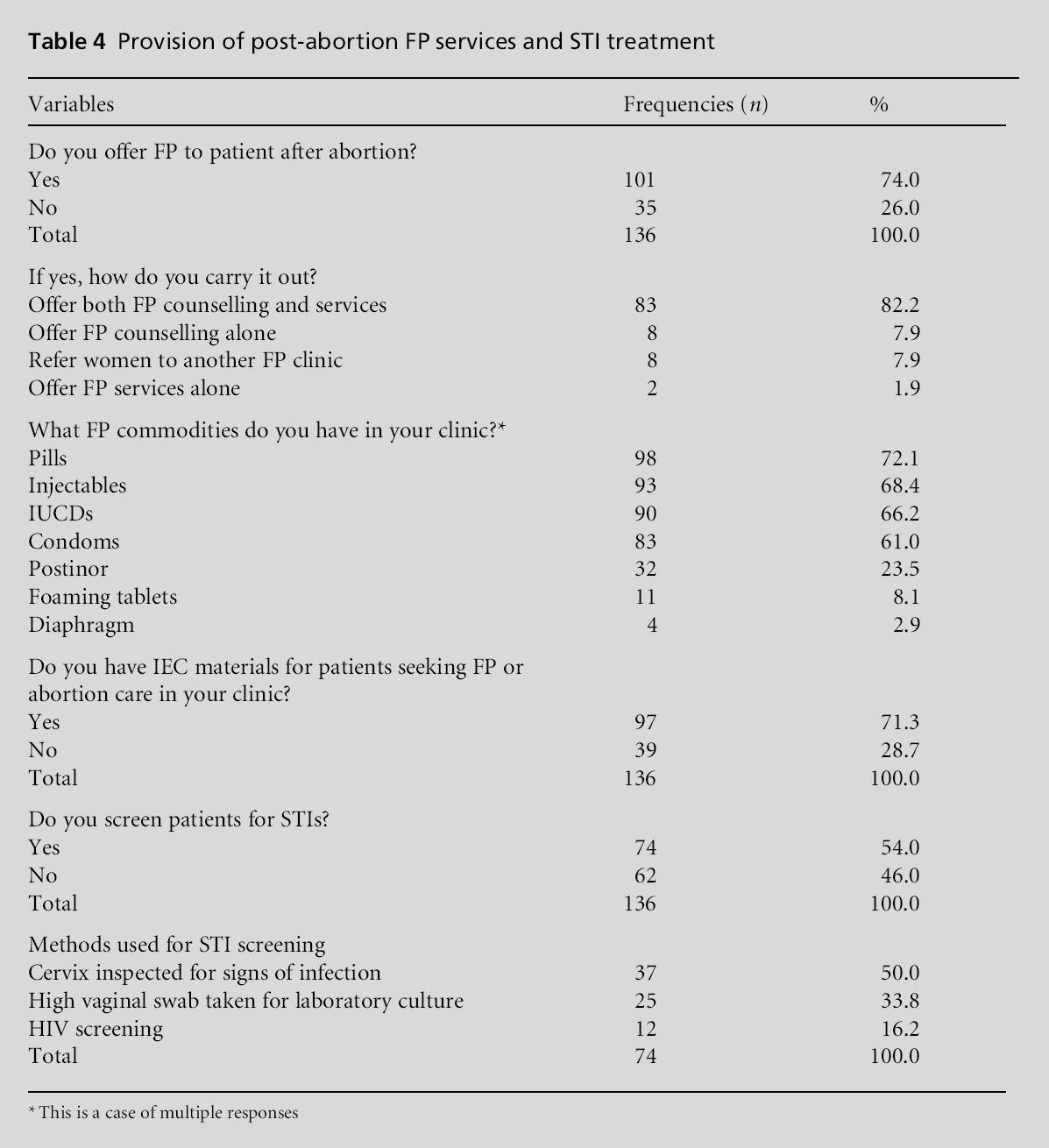
Findings on the provision of post-abortion FP services and STI treatment are presented in Table 4; 74% of respondents offered post-abortion FP to their clients by way of counselling or direct provision of services (82.2%).
This study demonstrated that unwanted pregnancy and abortion are common reasons for medical consultations in private healthcare facilities in the Niger- Delta region, which is consistent with previous studies.[12–15] Only a quarter of private practitioners provided abortion services which resulted in most clients who sought abortion receiving no care.[12–15] Many who were not offered help opted for providers who were untrained or unskilled.[12] Religious, ethical, legal, or moral considerations were more often cited as reasons for not offering termination rather than lack of training.[12–15] Good public healthcare information, education andcommunication (IEC) programmes are needed to improve this situation.
MVA is currently the method of choice for early termination or management of incomplete abortion in the first trimester, as it is easier to perform than the traditional D and C and less likely to result in lifethreatening complications.[16,17] However, only onethird of respondents had any formal training in MVA, often at workshops where practical exposure is poor, and only one-eighth were conversant with its use. Most abortion service providers were non-specialist doctors. This highlights the need for greater training in the use of MVA at all levels of medical education, particularly at undergraduate level, because many private practitioners possess only a basic medical qualification.[13]
Only about one-quarter of the respondents provided second trimester termination of pregnancy but many did not use the evidence-based methods available in developed countries, such as medical termination with misoprostol, mifepristone or a combination of both, and evacuation after cervical ripening using laminaria tents or prostaglandins.[18,19] Many respondents providing second trimester termination of pregnancy used artificial rupture of membranes followed with high-dose oxytocin infusion, which is obsolete in many parts of the world and associated with increased rates of maternal morbidity and mortality.[13]
This study shows a persuasive need to provide continuing education and retraining for private medical practitioners in the Niger-Delta region on evidencebased principles and practice of safe abortion care for women. Such education must include a comprehensive explanation and practical demonstration of appropriate methods for managing abortion and abortion complications in the first and second trimesters of pregnancy.[13] Despite the availability of medical abortifacients such as misoprostol and mifepristone in Nigeria, they are scarcely used in the procurement of abortion and rarely reported to be used in the management of abortion complications. The reason for this is very likely to be attributable to private practitioners’ lack of the requisite knowledge and the skills for the use of these methods. Therefore there is a compelling need for training of service providers on these evidence-based methods of nonsurgical and non-invasive procedures of management of abortion and abortion complications, and also a need to link them to the source of supply of these abortifacient drugs.
Integrated STI management and FP services seem to be fairly well practised as part of abortion care by the respondents in this study. This differs from findings of previous reports, where STI management and FP services were poorly integrated into abortion services. [13,14] However, the syndromic approach which has been recommended for the diagnosis and management of STIs by the WHO since 1990[20,21] was rarely used. The traditional methods of diagnosing STIs by laboratory tests are often unavailable or too expensive, particularly in low resource settings.[21] We hypothesise that in this study, because most of the clinics have laboratories, the syndromic approach was considered economically unwise and non-profitable. Over two-thirds of the respondents offered FP to clients after abortion, and the majority offered both FP counselling and services. Indeed the counselling services seem to be firmly established as over two-thirds of the clinics also distributed IEC materials to patients seeking FP or as part of post-abortion care.
Private medical practitioners in the Niger-Delta region of Nigeria reported frequent presentation of unwanted pregnancy and requests for abortion in their clinics. Only a quarter of those clinics offered termination of pregnancy, whereas others sent clients away without follow-up. The procedures used for termination of pregnancy by the few providers who undertook such procedures were largely safe and contemporary. However, training in procedures and knowledge of medical abortion was poor. These factors might contribute to abortion-related morbidity andmortality in the country. The private sector provides most abortions in this region but few use effective and evidence-based methods. Thus education of private practitioners in the principles of abortion, postabortion care and FP is recommended as an effective intervention to alleviate abortion-related morbidity and mortality in Nigeria.
Unfunded.
The study was approved by the Ethical Review Board of the University of Benin Teaching Hospital.
Not commissioned; externally peer reviewed.
None.