Keywords
black and minority ethnic (BME)
groups, devolution, evidence-based research, health
and social care, Wales
Introduction
The emergent research and development agenda in
Wales on black and minority ethnic (BME) health and
social care issues must be placed in the context of
constitutional change. Chaney and Drakeford (2004,
p.16) have referred to the devolved administration as essentially a ‘social policy Assembly’, indicating that in
the areas of education, health, housing and social
services responsibility is now entirely devolved to
Wales. This significant shift in the locale of policy
making is accompanied by a strong political rhetoric that speaks of ‘Made in Wales’ policies and ‘framing
policies tailored to Welsh needs’ (Welsh Assembly
Government (WAG) 2003a, pp.1 and 11) and by an
impetus to become ‘a country that develops its policies
on the basis of evidence, and that has mechanisms in
place to improve the health and social care of the
people of Wales’ (WAG, 2002, p.4). The vision for the
WAG’s strategic agenda is for a fairer,more prosperous,
healthier and better educated country (WAG, 2003a),
and key to this was the merging of health with social
care resulting in the recent creation of the Health and
Social Care Department and the appointment of a
Minister for Health and Social Services.
There has been considerable debate as to the extent
to which policy in the devolved nations does and will
diverge from other parts of the UK (Mooney et al,
2006) and particularly in relation to health policy
(Greer, 2006). Since its inception the WAG has steadily
gained increased powers with a total of 24 Acts
granting powers to the Assembly in 2006. Now in its
third term, the granting of primary legislative powers
under the Government of Wales Act 2006 will usher in
a strengthened indigenous policy-making process to
complement the policy levers it has used to date. One
area where Wales has a unique profile, by comparison
with elsewhere in the UK, is with regard to the equalities.
Equality of opportunity is identified as one of
three cross-cutting themes permeating policy making
in the new government. Central to this is the statutory
duty enshrined in the Government of Wales Act
(1998) that states that ‘the Assembly shall make
appropriate arrangements with a view to securing
that its functions are exercised with due regard to
the principle that there should be equality of opportunity
for all people’ (Section 120). This equality
imperative applies to all the devolved functions of
government in Wales. This duty, Chaney and Fevre
(2004) argue, is unique and represents a significant
divergence from equality laws in operation in other
parts of the UK, not least because it modifies all
Westminster statutes,where the Assembly has powers,
in their implementation. As Chaney and Fevre (2004)
suggest, the merits of the ‘Welsh model’ equality duty
are based on the fact that it is all embracing in scope,
requires government to be proactive in all equality
matters and conveys legally enforceable rights.
Coupled with the requirements of the Race Relations
(Amendment) Act 2002 relating to the UK, this
statutory framework suggests a strong equalities context
within which to develop health and social care
strategies for people from BME communities.
The context: what is known
about the health and wellbeing
of BME groups in Wales?
In view of the changes outlined above, the need to
address the multiple threats to the health and social
wellbeing of a diverse population has taken on some
urgency. In terms of the health of the general population,
Wales’ record is by any measure poor. It has
some of the worst child poverty rates in Europe
(Bradshaw, 2002). In the last census 12% of people
in Wales reported that their health had been ‘not good’
over the past 12 months and almost one-quarter
(23%) reported having a limiting long-term illness
or disability which restricted their daily activity (Office
of National Statistics, 2001). Wales comprises
some of the most deprived regions in Europe, and
huge inequalities in health outcomes exist for the most
deprived communities. Wales has a BME population
of just under 62 000 (2.1%) out of a population
of approximately 2.9 million people (www.statistics.
gov.uk). It is important to note that its long history of
minority ethnic settlement and the diverse nature of
the histories, settlement patterns, residential status
and occupational profiles of BME groups in Wales
suggest it is markedly different from other parts of the
UK (Williams et al, 2003). For example, the ethnic
profile and socio-economic status of BME individuals
from the more rural north of Wales are markedly
different from those in Cardiff (Williams et al, 2005a),
as are the issues of access to healthcare that they face
(Williams et al, 2005b). In addition, factors of considerable
diversity and dispersal have meant that natural or
politicised collectivities have not arisen in articulating
health needs as has happened in other parts of the UK.
Such distinctiveness, it is argued, suggests specific
responses tailored to need within the country.
Moreover, in their analysis of devolution in Wales,
Williams et al (2003) have argued that devolution
represents an opportunity to shift from a laissez faire
approach to a structured programme of nationally
responsible policies. The distinctive lethargy and subsequent
legacy of neglect of race equality issues in
Wales, however, has hampered development in Welsh
institutions in as much as there has been a paucity of
statistical evidence, with many public bodies having
developed idiosyncratic approaches to ethnic auditing
and monitoring. In addition there has been a dearth of
research studies, with those that have been available
‘being small scale, parochial, lacking in methodological
rigour and contributing little to vigorous theoretical debate’ (Williams et al, 2003, p.142). Recent Welsh
studies have sought to identify the health promotion
needs of BME groups in Wales (Papadopoulos and
Lay, 2005); the mental health information and treatment
needs of BME groups in Cardiff (Saltus and
Kaur-Mann, 2005); the experiences of carers from
BME backgrounds (Welsh Assembly Government,
2003b); the health and social care needs of unaccompanied
children seeking asylum (Hewett et al, 2005);
and BME communities’ needs and experiences in
accessing legal and related social welfare advice services
(Williams et al, 2005b). A few studies have been
undertaken that focused exclusively on specific groups,
for example on the experiences of Bangladeshi patients
in primary care settings (Hawthorne et al, 2003), the
care needs of elders (Patel, 1994), and support needs of
Bangladeshi carers (Merrell et al, 2005).
Despite this important research activity, it is evident
that much more work is necessary. In his recent
systematic review, Peter Aspinall (2006) identified
the major gaps in national Welsh studies, such as the
Welsh Health Surveys, and the unreliability of ethnicity
data, for example the Patients’ Episode Database
for Wales (PEDW), in highlighting the needs of BME
groups. More recently, both the Welsh Assembly’s
Strategy for Older People in Wales (2003c) and the
document on child poverty in Wales A Fair Future for
our Children (Welsh Assembly Government, 2006)
note the dearth of reliable data on ethnicity to guide
policy making in these areas. In her review, entitled
Health,Well-being and Access to Health and Social Care
of Selected Minority Groups (2004), Vivienne Walters
highlighted the apparent lack of information and
access to care for BME populations in Wales. Key
issues of concern included the lack of appropriate
information, language barriers, culturally alien services,
and institutional discrimination – issues that are
mirrored by the research findings of studies conducted
elsewhere in the UK (Modood et al, 1997; Arai and
Harding, 2002).
The aim of the scoping study
and methods of data collection
This paper examines one aspect of the findings of a
scoping study conducted in 2005, the findings of
which were further tested throughout 2006 in a series
of focus groups and stakeholder meetings. The particular
aspect of the 2005 study explored in this paper
is the perceived priorities and the challenges of improving
the health and social care of BME groups in
Wales as understood by key stakeholder groups. By
reflecting on the main themes that emerged from the
study and subsequent consensus-gathering work, this paper offers a framework for future appraisals and
seeks to identify some of the key issues raised by such
network-based approaches to research, policy and
practice development.
A short questionnaire was developed and piloted
with a sample of academics, health and social care
service providers and voluntary agencies working with
BME groups. The questionnaire comprised six questions
which explored the following topics: health and
social care issues affecting BME groups; research
priorities and challenges affecting research on the
health and social care of BME groups; opportunities
and expectations of a research and development network
and views on the way forward in developing the
network. The sample was purposive, with snowballing
technique/reference sampling also employed. The inclusion
and exclusion criteria reflected the aim of
developing a sample of BME service users, patients
and members of the public, staff working in voluntary
and statutory health, social care and social welfare
settings whoworkedwith a significant number of people
from the targetedBMEbackgrounds aswell as academics
working in Welsh universities. Following established
ethical guidelines, all participants were informed as to
the purpose of the study and were assured of confidentiality.
All data were anonymised and stored securely.
Funding constraints meant that the research instruments
were designed to be delivered in English only.
The research team and 23 co-workers disseminated
the questionnaire to their networks and service user
groups via meetings, email correspondence, and telephone
exchanges. The questionnaire was also distributed
by email discussion group managers to relevant
discussion groups. Data were collected between March
and April 2005. The questionnaires to stakeholders in
academic, NHS, and voluntary health and social care
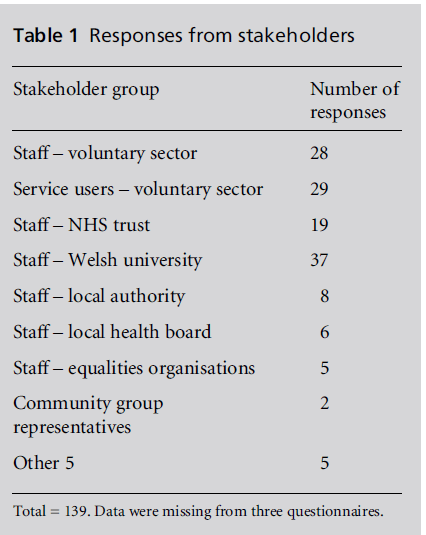
sectors yielded 142 responses (see Table 1), and gave
evidence from service users, practitioners and researchers
about their perceptions of research priorities.
In April 2005, three consensus focus groups were
also held, the aims of which were to: provide the
opportunity for team members to present and summarise
the responses to the questionnaires, reach a
consensus regarding the key issues raised in the responses
and scope the way forward. Summaries of the responses
from the questionnaires and notes from the focus
group discussions were produced. The size of the consensus
focus groups varied from three to 13 participants,
and the same inclusion/exclusion selection
criteria were used.
Findings
Table 1 :Responses from stakeholders
The key themes emerging from the questionnaires and
developed further in the census group discussions are organised in such a manner as to reflect some of the
key issues highlighted by these interested parties.
Further analysis of the findings of this study, together
with the findings from subsequent data gathering and
consultation exercises conducted after the study,
throughout 2005 and 2006, will not be discussed in
this paper. What the following section provides is a
snapshot of some of the key research priorities and
challenges that emerged from the scoping study (see Box 1).
Key priorities
The first theme that emerged from the data was the
concern regarding illness at different points in the life
cycle, including postnatal depression, services for
children and young people and the health of BME
elders. Concerns about a lack of information and understanding, for example of women in their middle
years, and the training of residential care home workers
about the needs of BME users were expressed.
A second theme identified was illnesses either specific
to BME groups or with a higher incidence in BME
communities. The majority of respondents listed
coronary heart disease, hypertension, diabetes and
haemoglobinopathies (such as sickle cell anaemia) as
well as some cancers. In all the focus groups, mental
illness was identified as a key concern, and in one focus
group there was a strong emphaisis placed on the
treatment of sexually transmitted diseases.
As well as specific illnesses, the findings revealed
a concern with specific problems associated with
particular social groups, for example, asylum seekers’
unfamiliarity with health and social care provision,
post-traumatic stress disorder and malnourishment.
For Travellers and Gypsies, questions of eviction, homelessness
and poverty have implications for health and
wellbeing.Racial discrimination and institutional racism
against asylum seekers, Gypsies and Travellers were
important concerns.
A fourth theme identified was the broader determinants
of health and wellbeing, including housing,
poverty, racism and education. This related to a further
set of priorities regarding access to services. In particular,
a lack of translation and interpreter services
was felt to be a key factor influencing access to social
and healthcare services and information. The need for
appropriate health promotion programmes was highlighted
as a key issue, along with encouragement to
participate in the various screening services which,
although available, have a very low take-up rate among
BME groups. These factors of course are similar to the
concerns of other parts of the UK.
A fifth theme was the need to develop culturally
sensitive services and the importance of increasing
staff knowledge and competencies through training.
As one respondent wrote:
‘Cultural awareness does not always lead to cultural
competency. There is a need to address the education
and training of those providing services’.
Box 1: Key research priorities and challenges.
There was a general consensus that protected time
should be made available for others working in health
and social care to pursue training. This training
should be offered to all staff, including front-line staff
such as receptionists, who are important in supporting
access to services. Lastly, the need for more BME
voluntary health and social care/welfare organisations
andBME service user groups was identified as being of
significant importance, for these organisations do not
only provide necessary services and support, they also
are ideally positioned to provide other sectors with
culturally competent practice models.
Key challenges
A number of key challenges affecting research about
the health and social care ofBME people in Wales were
identified through the study. First was the desirability
of user involvement and community engagement in
the formulation of research agendas and in the way
research is conducted inBMEcommunities,which is a
principle now well established in healthcare research
(Gunaratnam, 2003). As one commentator appropriately
suggested, there is a tension between research
outcomes and research process in this respect:
‘... the main challenge is the brokerage of research data
between acceptable output parameters required by health
and social care methodologies and the completely different
set of input values from the BME community. The
translation is a non-trivial matter and difficult ...’
Second, linked to this was the view that BME people
in Wales have been the subject of considerable research
overload and are left disillusioned when findings
apparently fail to influence policy and make an immediate
difference in their experiences of health and
social care. The census group discussions highlighted
the challenges raised by the paucity and short-term
nature of funding for research with BME groups.
These factors confirm findings from a number of
research studies (Arai and Harding, 2002). Finding
ways of ensuring more effective sharing of knowledge
and good practice around particular interventionswas
also identified as a challenge. The implementation gap
between researchmessages and changes in practice has
long been recognised, but this study highlighted the
potential for a more strategic and facilitative approach
to the support of practitioners. The need for effective
consultation mechanisms pitched towards BME households
as opposed to community groups was also seen
as a research priority.
A third challenge was rooted in the need for an
effective mainstreaming of the equality agenda. As one
respondent stated, there was a need to ‘ensure that
research that is considered to have important implications for BME communities in Wales is actively
considered, implemented or if not, good reasons are
given for not doing so’. This raises wider political
issues about the priorities given to BME research by
funding bodies inWales, and the current capacitywithin
research institutions to incorporate diversity and difference
in their agendum.
Finally, the specific strategies needed in areas of
Wales with low concentrations of BME people and
groups were also identified as a challenge. Very little is
known about how the particular needs of people from
BME backgrounds are met in virtually all those areas
in which they represent less than 2% in a locality. This
is particularly the case in north and mid-Wales. From
the focus groups it became clear that different challenges
and research priorities were emerging. For
example, in the north, concerns were expressed about
the needs of new migrants to the area, in particular
migrant workers for the EU accession states, issues of
attracting funding to such areas and issues of access to
services (Hold et al, 2007).
Conclusion: postscript on the
way forward
The scoping study represented a strategic Wales-wide
approach to a consideration of research priorities for
BMEs. The use of a participatory methodology meant
that the voice of user groups and key stakeholders
across the country shaped this major call for focused
research and development activity at a national level.
This activity itself provided for a mobilisation of key
stakeholders and the political prioritisation of the
needs of BMEs. As such it challenges the ad hoc, laissez
faire approach that has been previously taken to BME
research, with the concomitant tendency towards
small-scale and frequently duplicated studies. Recommendations
from the study proposed the establishment
of a research infrastructure aimed at enabling
regional and all-Wales research to be reviewed and
prioritised and to provide a dedicated research and
development context in which to link issues of ethnicity
and race to the key biomedical, clinical and healthcare
research underway.
Such an approach to the development of research
priorities is not without all the caveats incumbent on
user-engagement strategies. This account of BME
need must necessarily be partial, given the considerable
diversity amongst this population, competing
priorities and the orchestration of views which are
not always complementary. The scoping study provided
only a snapshot of the current articulation of
the issues, and began the process of mapping out
areas of need from an all-Wales, multisector and interdisciplinary perspective. It also raised wider questions
about the framing of need and responses at
nation-specific level, given the way in which minority
groups organise and coalesce beyond the boundaries
of the nation state, in both the articulation of needs
and the ways in which they seek responses for and
organise around them.
There is an extensive literature on the needs of BME
groups UK wide (inter alia Ahmad, 1993; Atkins and
Anionwu, 2001; Nazroo, 2003). This body of evidence
exists to establish patterns of disadvantage in relation
to specific conditions, access issues, racism in service
delivery and the needs of particular groups such as
Gypsy Travellers and asylum seekers. The experiences
of BME peoples in Wales may be typical, in many
respects, of BME experience elsewhere, but contextual
factors, such as a history of policy neglect, specific
social, economic and political factors including legislative
and policy divergence under devolution, make
pressing the need to find Welsh solutions for Welsh
problems. Devolution has produced what some commentators
(Adams and Robinson, 2002) have called
‘policy laboratories’, that provide opportunities for
novel experiments that can produce outcomes for
policy learning elsewhere. It is to be hoped that the
Welsh cross-sector system of collaboration and cooperation
that connects academic research with user,
community and public in the development of policy
and practice will provide such fruitful lessons.
ACKNOWLEDGEMENTS
The authors would like to thank all the participants
who took part in the scoping study, the 23 coapplicants
who distributed the questionnaire and
helped to collate data and the Wales Office of Research
and Development (WORD), who funded the study.
CONFLICTS OF INTEREST
None.
References
- Adams J and Robinson P (2002) Divergence and the centre. In: Adams J and Robinson P (eds) Devolution in Practice: public policy differences within the UK. London: Institute of Public Policy Research, pp. 198–227.
- AhmadW(1993) ‘Race’ and Health in ContemporaryBritain. Buckingham: Open University Press.
- Arai L and Harding S (2002) Health and Social Care Services for MinorityEthnicCommunities in the United Kingdom: areview of the literature on access and use. OccasionalPaper No 9. Glasgow: Research Medical Council.
- Aspinall P (2006) A Review of the Literature on the Health Beliefs, Health Status, and Use of Services in the MinorityEthnic Population and of appropriate Health and Social Care Interventions. Cardiff: WelshAssemblyGovernment.
- Atkins KandAnionwu E (2001) The Politics of SickleCell and Thalassaemia. Buckingham: Open University Press.
- Bradshaw J (ed) (2002) The Wellbeing of Children in the UK. London: Save the Children.
- Bradshaw J and Mayhew E (eds) (2005) The Well-being of Children in the United Kingdom. London: Save the Children.
- Chaney P and DrakefordM(2004) The primacy of ideology: social policy and the first term of the National Assembly for Wales. Social Policy Review 16:121–42.
- Chaney P and Fevre R (2004) ‘An absoluteduty’: an evaluation of the first five years Of The WelshAssembly’sStatutoryEqualityDuty.Wales Journal of Lawand Policy – CylchgrawnCyfraith a PholisiCymru 3:135–56.
- Greer S (2006) The politics of health-policy divergence. In: Adams J and Schmeuker K (eds) Devolution in Practice. London: Institute for Public Policy Research, pp. 98–120.
- Gunaratnam Y (2003) Researching ‘Race’ and Ethnicity – Methods, Knowledge and Power. London: Sage Publications.
- Hawthorne K, Rahman J and Pill R (2003) Working with Bangladeshi patients in Britain – perspectives from primary care. Family Practice 20:185–91.
- Hewett T, Smalley N Dunkerley D and Scourfield J (2005) Uncertain Futures. Childrenseekingasylum in Wales. Cardiff: Wales Programme of Save the Children.
- Hold M, Korszon S, Kotchekova E and Grzesiak F (2007) Migrant Workers in Flintshire. Conwy: North Wales Race Equality Network.
- Merrell J, Kinsella F, Murphy F and Philpin S (2005) Support needs of carers of dependentadults from a Bangladeshi community. Journal of Advanced Nursing 51:549–57.
- Modood T, Berthoud R, Lakey J et al (1997) EthnicMinorities in Britain: diversity and disadvantage. London: Policy Studies Institute.
- Mooney G, ScottG and Williams C (2006) Rethinking social policy throughdevolution. Critical Social Policy 26:483– 97.
- Nazroo J (2003) The structuring of ethnicinequalities in health: economic position, racial discrimination and racism. American Journal of Public Health 93:277–84.
- Office of National Statistics (2001) ONS 2001 Census, available at www.statistics.gov.uk
- Papadopoulos I and Lay M (2005) Enhancing the Health Promotion Evidence Base on MinorityEthnic Groups, Refugees/AsylumSeekers and GypsyTravellers. Cardiff: WelshAssemblyGovernment.
- SaltusRand Kaur-MannK(2005) Black and minorityethnic mental health service users in Wales: a snapshot of theirviews. Mental Health Nursing 25:4–7.
- WaltersV(2004) Health, Well-being and Access to Health and Social Care of SelectedMinority Groups. Paperpresented to the WelshAssemblyGovernment’sSelectedMinorityEthnic Groups Committee.
- WelshAssemblyGovernment (2002) A Health and Social Care Research and Development Strategic Framework for Wales. Cardiff: WelshAssemblyGovernment.
- WelshAssemblyGovernment (2003a)Wales A Better Country: the strategic agenda of the WelshAssemblyGovernment. Cardiff:WelshAssemblyGovernment.
- WelshAssemblyGovernment (2003b) Challenging the Myth, ‘They Look afterTheirOwn’. Cardiff: WelshAssemblyGovernment.
- WelshAssemblyGovernment (2003c) Strategy for Older People in Wales. Cardiff: WelshAssemblyGovernment.
- WelshAssemblyGovernment (2006) A Fair Future for our Children. Cardiff: WelshAssemblyGovernment.
- Williams C, Evans N and O’Leary P (2003) A Tolerant Nation? Exploringethnic diversity in Wales. Cardiff: University of Wales Press.
- Williams C, Turunen S and Jeffries J (2005a) The BEST Report: ethnicminorities in North Wales: amappingexercise. Commissioned by Black and EthnicMinorities Support Team – Scarman Trust, MEWN Cymru, AWEMA, BVSNW and WelshAssemblyGovernment. www.best-cymru.org (accessed 23 June 2007).
- Williams C, Turenen S, Leighton P and Evans R (2005b) Communities and Advice Services Project. Cardiff: MEWN Cymru.