Original Article - (2019) Volume 20, Issue 1
1Department of General Surgery, University of Illinois Hospital and Health Sciences System, Chicago, IL
2Division of Surgical Oncology, University of Illinois Hospital and Health Sciences System, Chicago, IL
3Department of Surgical Oncology, Edward Cancer Center, Naperville, IL
Received November 25th, 2018 - Accepted January 10th, 2019
Introduction We aim to develop a nomogram that predicts the nodal status in pancreatic ductal adenocarcinoma. Methods The National Cancer Database for pancreatic ductal adenocarcinoma was used. Patients without distant metastasis who received R0 resection and had ≥12 nodes retrieved were considered for the analysis. Significant predictors of N1 were concluded from a multivariate regression model and were used to establish the nomogram, which was internally validated using the 10-fold cross-validation method. Results 6,422 patients were found eligible to derive the nomogram. Overall survival of N0 vs. N1 patients was 35.15±1.45 vs. 21.82±0.44 months. The multivariate regression identified increasing age and receiving neoadjuvant radiation as favorable predictors, whereas pancreatic head cancers, lymph-vascular invasion, histologic grade, and pathologic T stage were identified as poor predictors of nodal metastasis. The bias-corrected concordance index for the nomogram was 0.756 (95% CI 0.743-0.769). Calibration was tested based on decile groups and no difference was noted between the predicted and observed N1 (p=0.804). Youden’s index identified the predicted probability of 53.40% to be the optimal cut-off for the nomogram. When applied to pancreatic ductal adenocarcinoma patients with inadequate node sampling (<12), overall survival for predicted N0 vs. N1 based on the nomogram were 29.90±1.41 vs. 20.57±0.72 months which is comparable to those with confirmed N0 vs. N1. Conclusion Prediction of nodal status in pancreatic ductal adenocarcinoma is critical. Development of a nomogram based on available clinicopathological features of the primary tumor to predict nodal involvement in light of inadequate node dissection is feasible.
Adenocarcinoma; Lymph Nodes; Nomograms; Pancreas
OS overall survival; PDAC pancreatic ductal adenocarcinoma
Pancreatic cancer inflicts more than 400,000 deaths annually worldwide [1] and ranks fourth among the most common killer cancers in the United States [2, 3]. Exocrine pancreatic cancers, dominated by pancreatic ductal adenocarcinoma (PDAC), remain a dreadful finding for only 20% of patients are determined eligible for a curative surgical resection at the time of diagnosis [4] and all are expected to eventually succumb to this disease.
Our current knowledge of PDAC indicates that lymph node status is one of the most significant predictors of local recurrence, and subsequently disease-free and overall survival (OS) [5, 6, 7]. The adequate extent of prognostic lymphadenectomy in PDAC of the head and neck of the pancreas currently follows the recommendations of the consensus meeting of the International Study Group on Pancreatic Surgery (ISGPS) [8] to include the hepatoduodenal ligament nodes (stations 5, 6, 12b1, 12b2, 12c), the hepatic artery nodes (station 8a), the posterior pancreatic head nodes (stations 13a and 13b), the superior mesenteric artery nodes (14a and 14b) and anterior pancreatic head nodes (stations 17a and 17b) [9]. For PDAC of the body or tail, the standard extent of lymphadenectomy entails the removal of the hilar splenic nodes (station 10), splenic artery nodes (station 11), and inferior pancreatic nodes (station 18) [10]. Adherence to the standardized description of lymphadenectomy in PDAC is expected to yield ≥12 nodes per the recommendation of the American Joint Committee on Cancer (AJCC) during pancreatic resection for adequate nodal stating of this disease [11].
In some instances, however, the number of retrieved lymph nodes does not meet this requirement despite the surgeon’s best effort to comply with the technical guidelines. Therefore, several studies attempted to compensate for this shortage by addressing the ratio, rather than the absolute number, of positive lymph nodes [12, 13, 14, 15]. The main criticism of this approach revolved around the repeated need for a large number of lymph nodes to yield a precise ratio, which results in a possible inflation in survival due to stage migration [16, 17]. It was suggested in some reports that the retrieval of a higher number of negative nodes, thus decreasing the ratio of positive nodes, might outline an improved local control or surgical downstaging of the disease [18, 19]. However, a large body of evidence generated a broad agreement that extended lymphadenectomy in PDAC resections carries higher rates of morbidity without evidence of survival benefit [8, 10, 20, 21, 22, 23, 24].
In this study, we use the National Cancer Database (NCDB), a large population-based cancer registry collected and maintained by the American College of Surgeons Committee on Cancer (ACS-CoC), which captures approximately 70% of the cancer cases nationwide, to develop a clinicopathological nomogram that predicts nodal metastasis in PDAC. This nomogram can be utilized as a tool for nodal staging in cases where the retrieval of the required 12 nodes is not achieved.
The NCDB for PDAC between 2004-2015 was used for the analysis. A series of inclusion and exclusion criteria were applied as follows:
• Only patients who were found to have pancreatic duct adenocarcinoma (PDAC) on final pathology were included.
• Patients with metastatic disease (M1) were excluded.
• Patients who were reported to receive any type of treatment with a palliative intent were excluded.
• Only patients who received a surgical treatment with a curative intent for their diagnosed PDAC and achieved R0 resection were included.
• All patients were staged in compliance with the American Joint Committee on Cancer (AJCC) 7th edition for PDAC as reported in the NCDB for the years of data collection.
• Only patients who had a known T stage to be T1-T3 were included in the analysis. Patients with T0, Tis, TX, and T4 (unresectable disease per the AJCC 7th edition TNM staging) were excluded.
• Only patients who had a known number of retrieved nodes and a known number of positive nodes were included.
• After conclusion of the predictive variables of N1 in the logistic regression model, patients who had missing data of any of the predictive variables were excluded from the analysis for that would affect the calculation of the predicted probability of that case.
Binary univariate and multivariate logistic regressions were applied to identify the predictors of nodal involvement in PDAC (N0 vs. N1). This regression model was used as the basis of our nomogram. The nomogram model was then constructed following the formula:
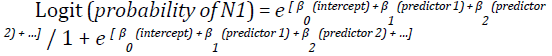
Patients whose data of the predictive variables were missing were excluded from the final analysis. Given the relatively large size of the study population, we internally validated the derived model using the 10-fold cross-validation method where 1/10 of observations are removed and the reduced, fixed dataset is used to exercise the model (i.e. training group). The results derived from the larger training group are then applied to predict the nodal involvement in the smaller group that was left out (validation group).
To protect the analysis from random splitting, this cross-validation was repeated 200 times to conclude the bias-corrected concordance index (CI) of our database.
Kaplan-Meier method was used to compare the OS of our patient population. Log-rank test was utilized the compare the survival results between patient groups based on the status of their nodal involvement and treatment modalities. Significance was set at <0.05 throughout the analysis.
The NCDB reported 340,780 patients with pancreatic malignancies between 2004-2015. After application of the inclusion criteria, 9,153 patients were identified to have non-metastatic PDAC of stages T1-T3, for which they received R0 surgical resection with a curative intent and a known number of retrieved and positive nodes. Of these patients, 6,422 (70.2%) had at least 12 lymph nodes retrieved during surgery. Table 1 summarizes the demographics and clinical characteristics of the selected population.
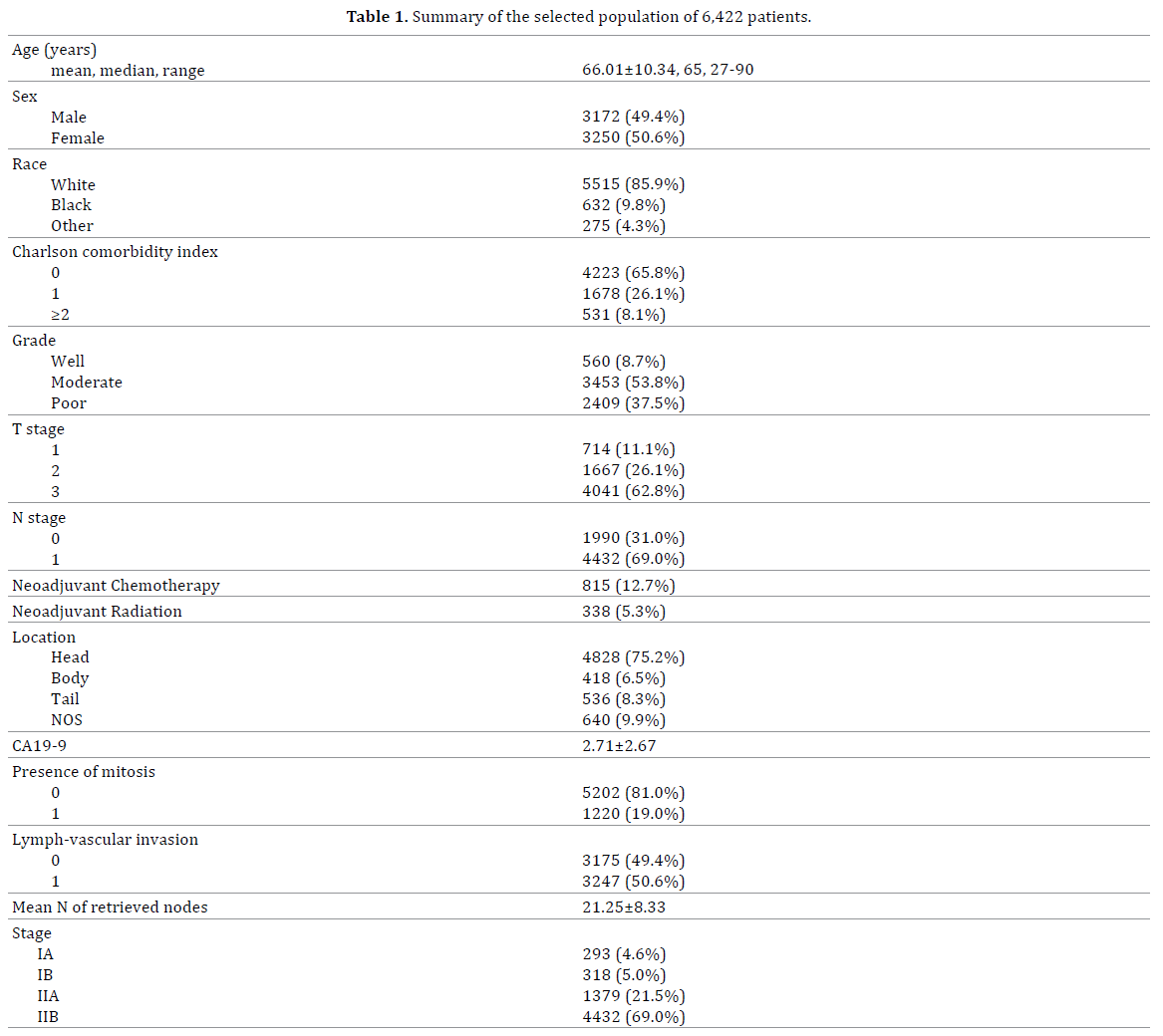
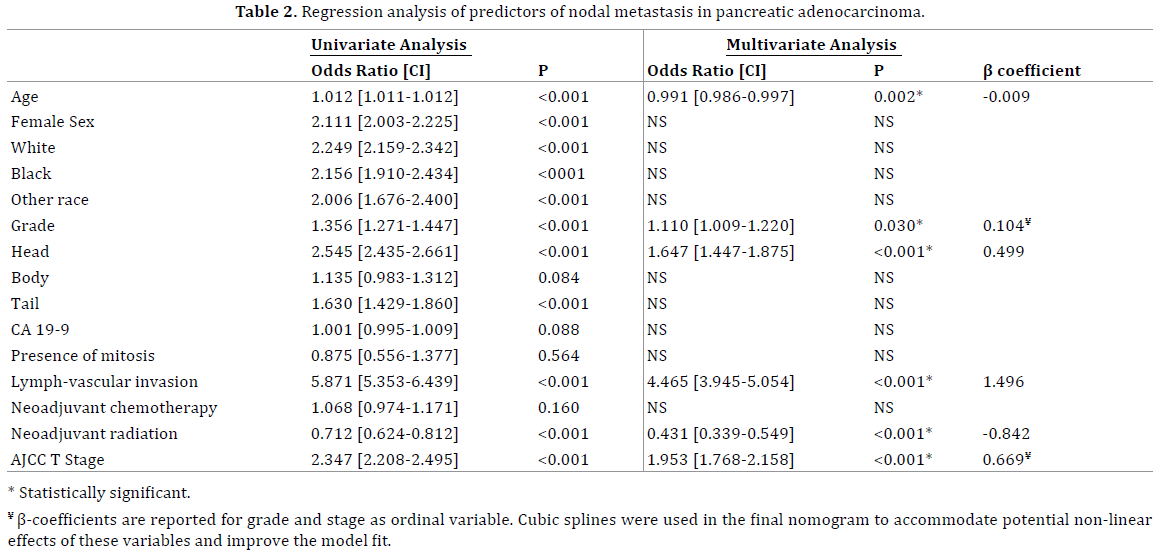
Table 2 demonstrates the results of the binary logistic regression analysis. Our results show that age, as a continuous variable, and receiving neoadjuvant radiation are favorable predictors of nodal involvement, whereas pancreatic head cancers, lymph-vascular invasion (LVI), histologic grade, and pathologic T stage represent risk factors of nodal metastasis. Sex, race, neoadjuvant chemotherapy, mitotic rate, CA 19-9 and Chromogranin A (CgA) levels did not demonstrate significant predictive values. Odds Ratio (OR) with 95% confidence interval are reported as a parameter of effect size in the logistic regression model.
Upon calculation of predicted probabilities of nodal involvement, age was modeled as a continuous variable, whereas for grade and stage, the ordinal variables in the model, cubic splines were applied to accommodate potential non-linear effects of increasing grade or stage and improve the model fit. The dataset was randomly split into training and validation subsets as described above; the training group was used to derive the predictors’ coefficients to be included in the nomogram’s final model, which was then tested for prediction of nodal involvement in the validation group. The process was repeated 200 times. The bias-corrected CI for the nomogram was 0.756 (95% confidence interval 0.743-0.769; asymptotic significance <0.001). The Receiver Operating Curve (ROC) for the nomogram performance is shown in Figure 1A.
Calibration of this predictive model was tested. The dataset was divided into deciles based on the predictive value of the nomogram for each case. Within each decile, the predicted outcomes were compared to the observed outcomes and plotted on the calibration curve shown in Figure 1B. Hosmer-Lemeshow goodness-of-fit test was conducted on the decile groups and showed no statistical difference between the observed and expected nodal involvement (p=0.804).
Based on the final model of the nomogram, a scoring table was designed which can be used as a tool to calculate the predicted probability of N1 in any given patient who meets the inclusion criteria of our study. The nomogram table is shown in Figure 2.
For cutoff determination, we used the Youden index (J statistic) to define the optimum of sensitivity and specificity on the ROC. Our results indicate that the optimal point for a cutoff is at Youden’s index of 0.394, which correlates with a predicted probability of 53.40%.
We then used the 2,731 patients who had inadequate sampling (<12 nodes retrieved) for indirect external validation of the nomogram. We compared the OS of these patients based on their predicted nodal status, which was determined per the aforementioned cutoff, to those who have a confirmed nodal status from the adequately sampled patients. Median OS of nomogram-predicted N0 vs. N1 patients was 29.90±1.41vs. 20.57±0.72 months (p<0.001) which are comparable to those of the adequately sampled patients. Figures 3A and 3B show the Kaplan-Meier plots of OS between the predicted N0 and N1 patients.
Figure 3. Kaplan-Meier survival graphs. (a). overall survival in PDAC patients treated with R0 resections and adequate node sampling: median survival of N0 patients 35.15±1.45 months, N1 patients 21.82±0.44 months; p<0.001. (b). overall survival in PDAC patients treated with R0 resections and inadequate node sampling: median survival of nomogram-projected N0 patients 29.90±1.41 months, N1 patients 20.57±0.72 months; p<0.001.
According to the 7th edition of the AJCC TNM staging, prognosis of nodal involvement follows a binary system of N0 vs. N1, where any nodal involvement advances the stage into IIB at least, with a detrimental regression in survival and a significantly poorer prognosis.
In this study, we explore the NCDB for PDAC to study the surgically managed patients with a focus on the associated lymphadenectomy. Interestingly, the NCDB reports a remarkable nationwide compliance with the recommended retrieval of ≥12 nodes during surgical resection (~70%). These cases of ‘adequate’ lymph node sampling were used to derive the nomogram assuming that nodal staging is then accurate.
Our analysis identified a group of clinicopathological factors that can serve as predictors of nodal involvement; increasing age and neoadjuvant radiation were favorable predictors of nodal involvement, whereas head PDAC, LVI, grade, and T stage were negative prognosticators of nodal metastasis. Modeling these factors in a predictive nomogram yielded an AUC of 0.756, which indicates a very good discrimination, along with acceptable calibration of the model.
The clinicopathological factors used to build the model are simple and routinely available for patients undergoing surgical resections of their PDAC. The inversely proportional relationship between age and local recurrence has been demonstrated previously in the Memorial-Sloan Kettering nomogram [25], hence it would be reasonable to observe less likelihood of node metastases as patients age since nodal involvement is a predictor of local recurrence. Moreover, the logical correlation between LVI, poorer tumor differentiation, and large tumors (i.e. higher T stage) and node metastasis has been repeatedly demonstrated in overall and disease-specific survival predictor models [25, 26, 27, 28, 29]. Having higher rates of positive nodes in pancreatic head tumors compared to body/tail tumors is evident for neuroendocrine tumors [30], in accord with our findings for PDAC, perhaps due to the abundant blood and lymph supply of the head of the pancreas. The role of neoadjuvant radiation has been an area of extensive study for borderline resectable pancreatic tumors; nonetheless, receiving neoadjuvant radiation has proven to facilitate higher rates of R0 resection and yield higher rates of N0 staging at final pathology [31]. In our analysis, neither sex, race, neoadjuvant chemotherapy, nor any of the conventional tumor markers had a predictive role of nodal metastasis in PDAC.
We realize that the shortcomings of this study are several. The retrospective nature of the analysis and using a national databank have inherent weaknesses including, but not limited to, inconsistent reporting and missing datapoints which generally lead to exclusion of potentially important variables in the model. Also, the NCDB reports the absolute numbers of retrieved and positive nodes without reporting the nodal stations included in the lymphadenectomy. In light of the growing evidence on the prognostic role of para-aortic lymph nodes in PDAC [32, 33, 34], this technical detail becomes of high importance to improve the function of the model. Most importantly, the main question that arises is the impact of nodal status on guiding the decision on adjuvant treatments. All PDAC patients are recommended to undergo adjuvant chemotherapy based on randomized trials with variable regimens [35, 36, 37] regardless of the nodal staging, whereas the role of adjuvant radiation remains an area of debate and ongoing research. Our analysis suggests that neoadjuvant radiation reduces the risk of disease dissemination to the lymph nodes. But if nodal involvement is evident in that particular case, offering adjuvant radiation would be out of question.
Nonetheless, we believe that the main value of this nomogram lies in its ability to better predict the prognosis of PDAC patients based on readily available factors in case of inadequate node sampling, a scenario that is not uncommon. Prognosis stratification in patients with PDAC, especially in face of uncertain nodal staging, can also play a critical role in patients’ eligibility for certain ongoing clinical trials, which might offer a potential of altering the disease course and prolonging survival in some individuals.
Any nomogram or predictive model entails several external validations in different patient populations before concurring its soundness. In our study, the internal validation was incorporated in the steps of nomogram development given the relatively satisfactory population size, in addition to an indirect external validation to the group of ‘inadequate sampling’ by comparing the survival or predicted N0 vs. N1 to the confirmed N0 vs. N1, with an acceptable correlation.
Prediction of nodal status in PDAC is critical. Herein, we establish a nomogram based on clinicopathological features to predict nodal involvement. This nomogram can be used to better predict patients’ prognosis following R0 resection of PDAC in light of inadequate nodal sampling. Adding more variables to the model might increase its accuracy, bearing in mind the availability of the factors and the generalizability of its application. Further external validations are warranted to confirm the accuracy of this nomogram.
We acknowledge Dr. Shaun Dougherty from the Department of Public Policy at the University of Connecticut for ensuring the technical soundness of the statistical analysis.
The authors have no conflicts of interests to declare.