Keywords
Mobile phone; Maternal and child health care; Equity; Access to care;
Governance; Nouna; Burkina Faso
Abbreviations
BCG: Bacille Calmet Guerin; CHW: Community Health Worker;
GSM: Global Messaging System; HIV: Human Immunodeficiency Virus; ICT:
Information Communication and Technology; IDRC: International Development
and Researches Centre; ITU: International Technology Union; IVR: Interactive
Voice Messaging System; LMIC: Low and Middle Income Country; MOS@N: Mobile
Santé Nouna; MT: Mobile Technology; NEPAD: New Partnership for Economic
Development of Africa; NHD: Nouna Health District; NHDSS: Nouna Health and
Demographic Surveillance Site; SMS: Short Message Service; TAM: Technology
Assessment Model; WHO: World Health Organization
Background
Nowadays, the most accessible technology among the most
disadvantaged populations in the world remains the mobile
phone. Statistics released by the International Technology
Union (ITU) indicate that over the past 15 years, information
and communication technologies (ICTs) have grown up in an
unprecedented way, providing huge opportunities for social and
economic development.
Nearly 5 billion mobile phones are connected worldwide and
over 85% of the world population is now covered by cell phone
networks of which two billion live in developing countries [1]. A
recent World Bank report noted that more Africans now have a
mobile phone than have a toilet [2,3].
According to Van [4], service and care providers, researchers and
national governments are excited at the opportunities mobile
health (mHealth) has to offer in terms of improving access to
health care, engagement and delivery, and health outcomes.
mHealth is seen as one of the great opportunities at providing [5] targeted interventions to poor populations living in remote areas [5].
The World Health Organization (WHO) has defined mHealth
as “Medical and public health practice supported by mobile
devices, such as mobile phones, patient monitoring devices,
personal digital assistants, and other wireless devices” [6].
Although Africa has experienced a delay in adopting information
and communications technology (ICT), there is more and more
interest in its possible role in enhancing access to health care
information and related opportunities.
Like several other African countries, Burkina Faso has recently
increased its use of mobile phones for various purposes. A recent
estimate of the Nouna Health and Demographic Surveillance Site
(NHDSS) showed that the household ownership of mobile phones
in this rural area increased from 3.8% in 2006 to 46% in 2009.
In 2010, 28.13% of rural households and 63.80% semi-urban
households owned at least one cell phone [7]. At national level,
cell phone coverage is estimated at about 70%.
In the context of poverty, low educational level and high rate
of maternal and infant mortality in Africa, the New Partnership
for Economic Development of Africa (NEPAD) in 2002 adopted
a resolution to tackle health issues through use of ICTs among
its 10 priorities [8]. Therefore, many pilot projects have begun
to emerge in a number of countries such as Senegal, Rwanda,
Mauritania, and Mali [9,10].
Indeed, maternal, newborn and child mortality and morbidity in
developing countries remain high despite efforts undertaken by
most countries. It is the main source of public health inequity [11].
Many systemic, economic, socio-cultural and geopolitical factors
contribute to this situation. To address this health challenge, the
use of ICT is increasingly seen as a promising solution [12-15].
The contribution of mobile phones in particular, earlier referred
to as “mHealth,” promises to provide remote access to health
services, and to facilitate training and sharing of knowledge
between health workers [16]. mHealth can also contribute to
diagnosing disease in rural and marginalized areas where health
services are often scarce or nonexistent [15,17].The deployment of mobile devices may well be decisive in the prevention and
control of diseases by promoting health behavior change in
population and health workers [18].
The mobile phone is also appreciated as a work tool that can
help to take decision and promotion of good health practices and
behaviors among populations [19]. As part of a study in Gambia,
a mHealth project was implemented to connect the community
health workers in villages with the hospital through mobile
phone technology. In cases of emergencies related to pregnancy
and child health, the health worker in rural areas immediately
contact the ambulance service in charge of the maternity for
rapid transfer [20].
In Bangladesh, in the face of significant shortages of highly
trained health care personnel, there has been a growing interest
in the possible ways that the use of mhealth, can improve access
to safe, effective and affordable health services and advice in low
and middle income countries [21].
A number of ehealth and mhealth initiatives have already been
implemented since the late 90’s. These have mainly focused
on mobile phones, especially important amongst the rural
and underserved communities for their potential to overcome
geographical boundaries. In 2011, WHO reported Bangladesh as one
of the 15 countries using mHealth to raise health awareness [22].
In Kenya, mHealth was used in several initiatives. Indeed, the
effect of mobile phone text-message reminders on Kenyan
health worker’s adherence to malaria treatment guideline was
assessed through a cluster randomized trial. Adherence on
malaria treatment guideline in intervention area was higher than
control area where health workers did not receive text-message
reminders [23].
India has a long standing experience in the use of mobile phone
to support health care delivery. With greater avaialability of
cheaper phones in the market, the user base mobile phones in
India is increasing rapidly [24].
Mobile phone was also adopted across various sector in India
such us Banking, telemedicine and governance.
From the health program manager’s perspective in India,
the direct benefit of mHealth for healthcare consumers and
healthcare providers yield overall program benefits such us early
case identification, better quality of health care and improved
compliance to treatment.
mHealth is being used in many forms in health related programs
in India. Currently, Mother and Child Tracking System (MCTS) is
arguably the biggest such program in India, operational since
2009.
Sending mobile based SMS to beneficiaries to alert them
regarding services due to them, or services which have become
overdue, communicating with other health care providers are
some examples of how the mHealth system is being utilized in
MCTS [24].
In early 2016, Government of India launched a nationwide
mobile health program « MOTECH » designed to train community health workers and to directly reach millions of women within
three years. With the funding from the Bill & Melinda Gates
Foundation, Grameen Foundation created MOTECH as an opensource
platform that works across key areas for health services:
behavior change, managing patient data, improving worker
performance, strengthening last-mile supply chain, and improving
patient adherence.
Nevertheless, as it was reported in much systematic review on
mHealth, the impact of mobile health in developing countries
remains relatively understudied [11,25,26]. Moreover, the few
studies investigating the issue show that the impact of mobile
health projects on population health are not always directly
perceptible in terms of cost-effectiveness. However, the rapid
proliferation of mobile telephony is widely considered as a
promising opportunity to improve health services and benefits in
developing countries [19,25].
According to Labrique et al [19], there is a need for more evidence,
as the current results are usually limited to pilot phases, and are
more focusing on the process of mHealth implementation. The
question of how much mHealth can be seen as a health systemstrengthening
tool and better integrated within the health
system, remains open and to be better addressed. Challenges in
process implementation also need more attention.
This viewpoint was shared by Tomlison [27] for whom
despite hundreds of pilot studies; there has been insufficient
programmatic evidence to inform implementation and scaleup
of mHealth. The example of Uganda reported by the author
translates better the difficulties in moving forward with a specific
initiative. Indeed, approximately 23 of 36 mHealth initiatives
implemented across the country between 2008 and 2009 did not
move beyond the pilot phase.
In a review of empirical studies related use of ICTs, many studies
focused on SMS. Some studies investigate in mobile ring tones,
paying for parking, mobile gaming, mobile ticketing, and mobile
insurance. Others are more generic and are related to advertising
(SMS advertising, mobile social advertising), mobile commerce,
mobile shopping, Internet mobile banking, mobile payment,
mobile brokerage etc.
According to Diniz [28], mobile technology, viewed as a payment
or banking channel, has the potential to allow two important
questions to be addressed at the same time: on the demand
side, it represents an opportunity for financial inclusion among a
population that is underserved by traditional banking services. On
the supply side, it opens up possibilities for financial institutions
to deliver a great diversity of services at low cost to a large
clientele of the poorest sections of society and people living in
remote areas.
Mobile banking is becoming a new paradigm in developing
countries where a majority of Banks branch is offering Mobile
Financing Services (MFS) to users.
MFS is an umbrella term, often referred to as mobile money. MFS
uses a “mobile wallet” or a separate electronic money account used
for payments other than prepaid or post-paid mobile airtime. Within MFS, there are three main categories: mobile payments, mobile
credit/savings/insurance and mobile banking [29].
As Miller [30] noted it, in countries where access to traditional
banking services is limited, more and more people are utilizing
cell phones to send money to family members, pay bills or keep
track of savings.
In Kenyan, the M-Pesa system is the largest mobile phone banking
platform in the world. It has exploded in popularity over the last
decade and now serves more than 13 million active customers.
Developed by Vodafone and launched commercially by the
company’s Kenyan affiliate Safaricom, M-PESA is a small-value
electronic payment and store of value system accessible from
ordinary mobile phones. Once customers have an M-PESA account,
they can use their phones to transfer funds to both M-PESA users
and non-users, pay bills, and purchase mobile airtime credit for
a small, flat, per-transaction fee. The affordability of the service
has been key in opening the door to formal financial services for
Kenya’s poor [31].
Similarly in Ethiopia, the M-Birr service was operational since
2014.
M-Birr is a mobile money service that enables the banked and
unbanked people of Ethiopia to conduct financial transactions
from the convenience of their mobile phone. The launch of the
services, which allow customers to make payments or receive
money via a mobile that is linked to a bank account, mirrors
technology used in other African nations that has drawn millions
of people into the financial system [32].
Many other LMIC are using mobile financial services such
as Burkina Faso since 2010 with airtel-money, mobi-cash in
partnership with local Banks.
However, as noted Beshouri, although there are more than 120
mobile money projects being undertaken in about 70 emerging
markets [33], mobile payment has only become a normal practice
in a few countries, despite its huge potential.
The introduction of ICT in the field of health, however, is not
done without difficulty. Obstacles to the implementation of
mobile technology in the field of health remain both technical
and financial. One of the main challenges is the development
of digital networks for communication between the various
health actors and various equipment used [13,34]. Another
major obstacle is the lack of competence and expertise for the
development and implementation of projects tailored to health
problems especially in rural areas [35].
The existing literature on mobile health pilot projects shows that
in Africa many external barriers are responsible for failures [36].
In addition other obstacles are related to the design of individual
projects and their adaptation to the local contexts in which they
are implemented. Unlike external factors, the factors associated
with projects themselves can be monitored and controlled during
the implementation phases.
Another important challenge is related to gender issue and
mhealth interventions.Indeed, as noted some authors, the gender divide in access to
and use of mobile phone technologies is well documented in
developing countries [32,37].
In a systematic review conducted by Jennings [37], he concluded
that the current mHealth literature described several positive
transformations in the interaction of men and women. One
finding was that the provision of mobile-based health information
empowered couples to discuss health. Despite evidence on the
positive effects of mHealth interventions on women’s health
and care-seeking, there is growing concern that mobile-based
programs geared towards women may exacerbate gender
inequalities [37].
In this same line some evidence suggests that while mHealth
programs hold the potential to shift gender roles by empowering
women through improvements in knowledge, decision-making,
and economic gain [16,38], and some mHealth interventions
may exacerbate gender inequalities by reinforcing existing power
differentials [37].
In this context, Burkina Faso has been engaged in the
implementation of several mHealth projects. One of these
projects, MOS@N, was implemented over the last two years by
the Nouna Health Research Centre in the rural health district of
Nouna. The implementation was supported by the International
development research centre (IDRC/Canada).
The mHealth project (MOS@N) is an interactive mobile phone
communication system deployed at community and health facility
levels. The platform was developed using open source software
and allow access to health information related to maternal and
child health care and to patient living with HIV. The platform
has a reminder component so that to increase compliance with
planned visits and follows up patients in remote area without
access to health information.
The key actors for the project are community health workers
located in the project selected area and health workers in the
project catchment area. All actors were provided with cell
phones that allow communication. In addition all health facility
was provided with laptops allowing patients registration at the
point of care. There is an automatic synchronization of patient’s
information with a central server based in project headquarters.
The main aim of the mHealth project is to increase awareness
in the use of health facilities related services by community
member via interactive mobile communication system. As such,
pregnant women, HIV patients are regularly informed about the
importance of seeking care and the necessity to follow planned
visits through tailored education messages.
The mHealth project implemented in 2013 and running until 2017
has brought together local healthcare providers, community
health workers, ICT technicians, and public health researchers
in an interactive communication system tailored for the specific
health information needs of an underserved area. This research
project aimed at interconnecting a network of health facilities in
the Nouna Health District through an innovation technology to
improve access to information and care.
The objective of the study was to document and analyze an innovative mobile phone platform that aims to help in
overcoming barriers experienced by community members in
accessing health services. Special emphasis was given to gender
related inequalities. Furthermore, this article examines lessons
learned that should be considered for possible similar technology
implementation by other countries.
Methods
Study site
The study was conducted within the Nouna Health District (NHD),
in rural Burkina Faso. The NHD is located at about 300 km in the
northwest of Ouagadougou, the capital of Burkina Faso. It is one of
the six districts of Boucle du Mouhoun Health Region and covers
the geographical area of the Kossi Province in the western part of
the country. Nouna is the capital of the Kossi Province. The health
district comprises of the town of Nouna with a total population of
29,297 inhabitants and a rural area of about 331,020 inhabitants.
The health infrastructure of the NHD consists of one District
Hospital in Nouna, and over 43 dispensaries. Due to deficient
road infrastructure, only 69.13% of health facilities are accessible
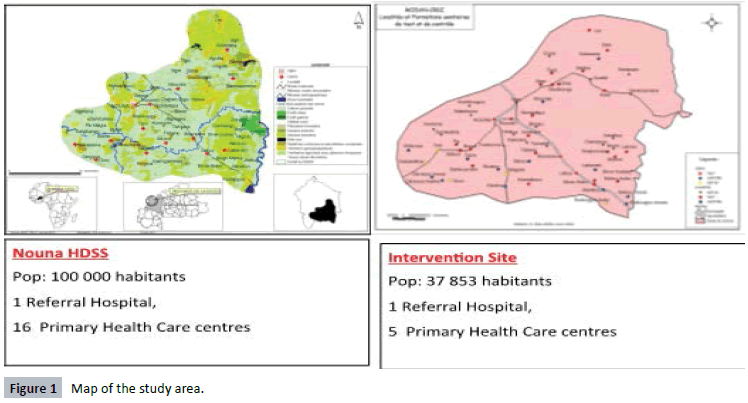
all over the year with a mean distance of 8.48 km [39]. The Figure
1 shows the NHD map and study areas.
Figure 1: Map of the study area.
Study design and methods
The study used a quasi-experimental design with pre- and postintervention
study comparison between two groups of health
facilities (HF) with one arm assigned for the intervention and
the other as control. Overall, 10 HF within the Nouna Health and
Demographic Surveillance System (NHDSS) were included in the
study, among which 5 were randomly allocated for the control.
The study combined both qualitative and quantitative methods
to collect baseline data among community members and health
service providers. Baseline HF was collected prior to the mHealth
intervention implementation in 2013 and over the project course
in order to document the change between pre-intervention and
post intervention. For that purpose, key health indicators related
to maternal and child health care, as well as to HIV patients, were
collected and monitored quarterly. They were also compared
with baseline data after 24 months of implementation.
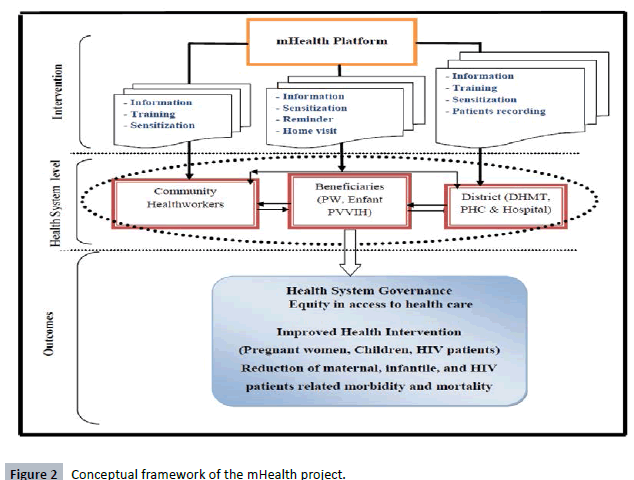
The conceptual framework in Figure 2 describes the logic of the
mHealth technology implementation and interaction within the
health system and the potential expected outcomes.
Figure 2: Conceptual framework of the mHealth project.
mHealth technology development
The mHealth platform was developed locally based on an extensive
review of the diversity of mHealth solutions implemented across
different countries.
An interactive voice messaging system (IVR) was developed and
incorporated five local languages (Bwamu, Dafing, Dioula, Mooré and
French) to overcome literacy barriers. In addition, an automated patient
reminder system for follow-up appointments was incorporated in the
technology that was developed by local experts familiar with mobile
health technology. For ease of deployment, open software developed
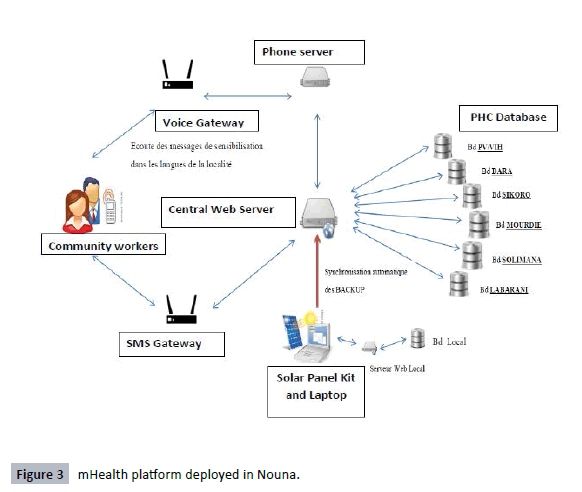
under PHP Symphony Framework was adopted. The Figure 3 shows the technical features of the platform developed and its interaction with
health facilities and community members.
Figure 3: mHealth platform deployed in Nouna.
The mHealth technology incorporated the following components:
a GSM internet connexion, an Interactive Voice Messaging
System, an automatic patient reminder system, and an automated backup system including data synchronization with a central
server hosted in Nouna. In addition, a core health information
system was developed and incorporated within the district health
facilities to collect data relevant for decision-making. The Figure
3 describes the key components of mHealth platform deployed.
Ethical consideration
The research protocol was approved by the National Ethic
Committee and an institutional review board approved in 2013.
Results
The results section is structured in three components: The
acceptability of the technology by key stakeholders; the effects
of the mHealth project; and the challenges related to its
implementation.
Acceptability of mHealth according to in-depth
interviews
In-depth interviews were conducted with different actors
purposely selected — 15 health workers out of 30 and 25
community health workers out of 52 — involved in the project
just before it was launched. The interviews aimed to document
the acceptability and usefulness of the technology according to
these actors.
Overall all actors noted that the mobile phone already played an
important role in their daily activities. At a health facility level,
the phone is used to convey routine health information data at
each level of the system; it is often used to call an ambulance
in case of emergency. Community members value the mobile
phone as a symbol of wealth, and tend to consider that it can
empower women and encourage their use of health services. It
is also perceived as a tool to get information from relatives, from
health facilities and stay in touch with family abroad. Its role in reducing unnecessary visits to health facilities was mentioned by
a respondent:
“The mobile phone contributes to reducing distance and
inconvenience due to road traffic. Also in case of a death, the
bereaved families no longer need to walk or travel to inform the
neighbouring villages. We can make calls instead of moving to the
village” (woman in the village of Sikoro).
Technology acceptance assessment
WHO technology assessment model (TAM) was used to assess
community and health workers acceptance toward the mobile
phone.
Acceptability of MT by community health
workers
A total of 48 community health workers (CHWs) were interviewed
for technology assessment using the WHO standard structured
questionnaire on the acceptability of mobile phone technology. Overall
mobile phone possession was about 35% among CHWs. Mobile phone
was used mainly for voice calls by 94% of phone owners.
Regarding the perceived usefulness of mobile technology (MT),
the majority of CHWs (94%) perceived it useful with 100%
intention to use it for communication and sensitization for
pregnant women and children.
Acceptability of MT by health workers
A total of 19 health workers were interviewed in five health facilities using the WHO TAM. 100% of health workers had a
mobile phone and 4 others had in addition a laptop.
The most common application used by health workers are voice
calls in 100% of cases and SMS for 63% of respondents. In terms
of acceptance, 74% agree that the use of mobile phones could
help make patient care more quickly and convey routine health
information to management levels.
Effects of mHealth project in health care
utilization
The effects of the mHealth project were measured through key
performance indicators in line with those used by the Ministry of
Health. The measure was done at pre-intervention in 2013 and at
mid-intervention in 2015 based on the listed indicators:
1. Antenatal care 1 (ANC1)
2. Antenatal care 4 (ANC4)
3. Tetanus Toxoid vaccine (TT2)
4. Intermittent Preventive Treatment of Malaria (IPT2)
5. Pregnancy at risk referred (PAR)
6. Infant to Mother Transmission of HIV (IMCT)
7. Assisted delivery (AD)
8. Postpartum care (PPC)
9. Contraceptive prevalence (CP)
10. Oral Polio Vaccine (OPV)
11. BCG vaccine (BCG)
12. Loss of followed up HIV (LFU)
Results linked to mHealth implementation
process
Overall more than 100 health workers and 62 community health
workers were trained to mHealth platform use as well as mobile
phone use. This was found fundamental to make the project
functioning well
The involvement of CHWs was determinant for the project to
achieve substantial results among which: 181 pregnant women
newly registered, 992 pregnant women referred to antenatal care
(ANC) services, 826 women followed-up for postpartum care;
more than 2318 access to voice messages for sensitization; 413
home visits performed and 811 automatic reminders for visits
received by CHWs.
Effects of the mHealth project on maternal and
child health, and people living with HIV
The effects of the mHealth intervention were measured against
selected performance indicators. The comparison was made
between the intervention and control sites performance at
baseline and mid-intervention in 2015 as in Table 1.
| Indicators |
Intervention site |
Control site |
Difference (%) |
P-value |
| ANC4 |
58.07 |
45.47 |
12.6 |
P<0,001 |
| TT2 |
84.04 |
79.50 |
4.54 |
|
| IPT2 |
87.92 |
95.60 |
-7.68 |
|
| PMTCT |
97.32 |
83.59 |
13.73 |
P<0,001 |
| AD |
87.93 |
89.97 |
-2.04 |
|
| PPC |
49.35 |
64.36 |
-15.01 |
|
| CP |
66.85 |
65.93 |
0.92 |
|
| OPV |
100 |
89.08 |
10.92 |
|
| BCG |
100 |
89.08 |
10.92 |
|
| Combined p-value |
|
Legend: ANC4: Antenatal Care4; TT2: Tetanus Toxoid2; IPT2: Intermittent Preventive Treatment of Malaria; PMTCT: Prevention of Mother to Child HIV Transmission; AD: Assisted Delivery; PPC: PostPartum Care; CP: Contraceptive Prevalence; OPV: Oral Polio Vaccine; BCG: Bacilli Calmette Guerin
Table 1: Performance between intervention and control sites in 2015.
The data showed that there was a gain of 12.6% in the intervention
area compared to the control area, which is equivalent to 8%
increase of antenatal care uptake. Similarly, there was a gain of 13.75% in PMTCT coverage in intervention area compared to
control area. Both differences were found statistically significant
(P-value<0.0001). However, some indicators such as assisted
delivery and TT2 didn’t change between the two sites.
The effects of the project were also measured in intervention
sites and compared between baseline and mid-intervention
mean performance as shown in Table 2.
| Indicators |
2013 |
2016 |
Difference% |
Progress (%) |
P-Value |
| ANC4 |
52.8 |
58.07 |
5.27 |
10 |
P<0,0001 |
| TT2 |
62 |
84.04 |
22.04 |
36 |
P<0,0001 |
| IPT2 |
85 |
87.92 |
2.92 |
3 |
P<0,0015 |
| PMTCT |
78.33 |
97.32 |
18.99 |
24 |
P<0,0001 |
| AD |
62.5 |
87.93 |
25.43 |
41 |
P<0,0001 |
| PPC |
62 |
49.35 |
-12.65 |
-20 |
|
| CP |
50.8 |
66.85 |
16.05 |
32 |
|
| OPV |
100 |
100 |
0 |
0 |
|
| BCG |
100 |
100 |
0 |
0 |
|
| LTFU/HIV |
10 |
1.6 |
-8.4 |
-84 |
P<0,0001 |
Legend: ANC4: Antenatal Care 4; TT2: Tetanus Toxoid2; IPT2: Intermittent preventive treatment of Malaria; PMTCT: Prevention of Mother to Child HIV Transmission; AD: Assisted Delivery; PPC: Post-Partum Care; CP: Contraceptive Prevalence; OPV: Oral Polio Vaccine; BCG: Bacilli Calmette Guerin; LTFU/HIV:Lost to Follow up HIV Patients
Table 2: Comparative mean performance in intervention site between
2013 and 2015.
When considering the intervention area alone between 2013
and 2016, there is an improvement in a majority of the indicators
selected. For example, for the ANC4, we noted a 10% increase
from the baseline to mid-intervention in 2016 (P<0.001). There
was also a 41% increase in assisted delivery, a 36% increase in TT2
coverage and a reduction of about 84% in lost to follow up of HIV
patients. These results were statistically significant (P<0.0001).
Overall, of the 971 HIV patients followed-up by hospital, 262
were registered via the mHealth platform and followed up.
Indeed, with the automated system implemented through CHWs,
patients were reached easily and were informed about the
benefits to seek care in formal health facilities.However, as many health interventions were ongoing in both
health facilities led by the Ministry of health, such us the
subsidized care for maternal and neonatal care; this could explain
the non-difference in some indicators.
Challenges linked to mHealth implementation
and solutions
MOS@N experienced important challenges, related to both
technological implementation and human resources.
The technological challenges were posed by the lack of robustness
of the mobile phone devices used in the project. Despite the
choice of relatively robust phones, over 65% of the phones
was out of service after 24 months of implementation, and was
replaced. In the meantime, 21% of solar recharging systems were
also replaced. The fact that, most users were not familiar with
phone use could explain the high rate of damaged cell phones.
The other technological challenge was the poor Internet
connectivity within the intervention zones. The high penetration
of mobile phones in the study area contrasted with the low
accessibility to reliable network (both mobile and Internet)
access, and this, despite efforts made by the national supplier.
The project was designed around an interactive system,
which required data synchronization via a central server. This
synchronization, however, was not possible due to a lack of access
to Internet in most of the peripheral health facilities. However,
alternative solutions were developed to download data in an USB
stick and to update later the central server based in the project’s
headquarters by simple loading the data in the server.
Concerning the human resource challenges, the main issue was
the high turnover of health workers, moving toward other health
facilities, or national level for training purpose. The turnover was
estimated at 30% after two years of project implementation. One
consequence of that is a continual renewal of the staff and the
need to train health workers newly appointed to participating
health facilities. This provoked discontinuity in the project.
There were also challenges related to changes within the group
of participating (CHWs), for personal purpose or conflict with
husband regarding their participation in the project. In terms of
gender representativeness in the project, 54 CHWs were female
and 8 were male.
Notwithstanding these issues, the mHealth project was able to
mobilize local community members with the ultimate goal to
increase their access to health facilities and their involvement in
local health governance. Some lessons were also learned in terms
of reinforcing the feasibility and acceptability of such a mHealth
project and this, right from the implementation stage.
Discussion
The study showed that the use of mobile phones at community
level could improve their access to health care and ensure that
equity dimension is fully considered for those who otherwise
cannot access to health services by their status.
MOS@N, a mHealth project implemented over two years, shows
that the intervention is feasible technically and acceptable by
health workers and community members. It has led to substantial improvement in healthcare access, whether it is for maternal and
child health, or for people living with HIV.
These results are consistent with the findings of other projects
such as MobiSan (Mobile Santé) [40] that aims to improve
maternal and child health through the development of service
based on mobile and implemented in the eastern part of Burkina
Faso. Indeed, this mHealth initiative implemented in 2010
registered more than 3 million users and led to an increase of
child survival (1.7 points) in 5 months and threefold increase of
health service utilization by mothers.
A mHealth project in Mali which targeted data transmission
through routine health information systems among under five
years showed an increase in health service use by beneficiaries
compared to control group who does not benefit of the mHealth
intervention [41].
The fact that ICT, and the mobile phone in particular, has been
used as a means to convey health information, is well documented
elsewhere. Indeed mHealth and other applications can contribute
to remote diagnosis in places where health services are scarce
or non-existent in marginalized rural communities [15,42]. The
deployment of mobile devices may be decisive in the prevention
and control of diseases by promoting health behaviour change
among the population [17].
mHealth is also appreciated as a powerful tool that can enhance
the promotion of behaviour and good health practices among
the population [26]. A similar study in the Gambia aimed at
connecting community health workers with the hospital through
mobile phone devices yielded tremendous results in emergency
management related to high-risk pregnancies [20].
However, what could be the effects of mHealth interventions
on the health of populations? As part of improving the health
of populations, several health interventions may be needed to
produce the expected changes.
After 24 months of implementation, MOS@N has contributed in
increasing some key health indicators. Indeed, with a 10% increase
of antenatal care uptake in 2016 compared to the baseline 2013,
41% increase of institutional deliveries and 24% increase of
PMTCT services, mHealth is a promising tool to complement ongoing
health strategies.
Our results are consistent with those reported by Bagayoko [9],
according to whom the use of mHealth and eHealth initiatives
implemented in Mali contributed in improving medical diagnosis
in cardiology and obstetrics (92.6%), as well as the patient
management system on site (96.2%). In Rwanda too, an SMSbased
system was developed to improve maternal and child
health (MCH) using RapidSMS, a free and open-sourced software
development framework launched in 2011. RapidSMS led to a
27% increase in facility-based delivery from 72% twelve months
before to 92% at the end of the twelve-month pilot phase [10].
In Bangladesh, WHO reported that the Ministry of Health reached
98% of its target population through SMS on health education but
did not provide messages in Bangla, which is the first language
of the majority of the population posing a problem of equitable
access to health information [24].
A systematic review [25] conducted in LMICs on seven mHealth
projects also shows that SMS reminders have improved patient
participation rates to appointment visits compared to patients not
included in the projects. Overall, participation in appointments
was 67.8% for the group without reminders, and 78.6% for the
group with SMS reminders.
However, as noted some authors, if the contribution of the mobile
phone in the provision of care is a new paradigm largely adopted
by most developing countries[42,43], the literature also reveals
that the results are sometimes mixed and often lack of evidence
[44]. Some have indeed argued that the impact of mHealth in
developing countries remains relatively understudied [3,44].
Moreover, the few studies that investigated the issue show that
the impact of mobile health projects on population health is not
always directly perceptible in terms of cost-effectiveness [19,26].
Challenges linked to mHealth implementation
Despite many reported benefits associated with the use of
mobile phones in the provision of care, some challenges also
arose in most projects implemented that need to be overcome
at the beginning and through the process. These challenges are
mainly due to technological issues and human resource capacity
to use this technology.
Indeed, as reported by several authors, even successful mHealth
programs in low-resource settings face particular challenges [3, 27]. While in MOS@N major challenges were posed in terms of
cell phone robustness, weak energy availability and poor network
connectivity, other authors have noted the inadequacy of mobile
phones in LMICs who can only accommodate voice and SMS
text messages [3]. The fact that the majority of cell phones were
replaced in our project was also documented in a mHealth pilot
project implemented in Rwanda [10].
Moreover, system integration and interoperability was identified
as a challenge in most mHealth projects implemented in LMICs.
Indeed, many mHealth interventions were implemented in a
parallel way, without being integrated within the national health
information system [45].
Challenges such as the scarcity of reliable energy source,
confidentiality of patient data and integration into a standard
information system and technology were also commonly reported
elsewhere [9,27,46].
In terms of human resources, running a mHealth project requires
highly qualified information technology workforce, right from
the design of the technological platform. This expertise is very
often missing in LMIC and this poses a problem of transfer of
technology [15].
Managerial, policy implications and
recommendations
In terms of managerial aspects related to the mhealth
intervention, there is a need to involve health managers and
health workers at all stages of the technology development and
deployment for more ownership. Beneficiaries need also to be
more informed about the potential benefits of mHealth and the
way their rights are protected and their access to storage data.
In terms of policy implication of mHealth intervention, researchers
should raise policy makers about the importance of mHealth
solution and potential benefits to improve population access to
health information and oriented health care. The adoption of
mhealth policy at countrywide rely on the perceived usefulness
by policy makers.
We recommend therefore that:
1. Policy maker adopt mHealth intervention as part of health
system strengthening tool.
2. Integrate mHealth intervention within health care delivery
system in health facilities.
3. Ensure scaling up of mHealth intervention at country level
and facilitate access to reliable cell phone network.
Conclusion
The contribution of mHealth in the access to health information
and to improve population health is undeniable. In the context
of a high penetration of mobile telephony within communities, it
offers as an opportunity for improving health outcomes in many
different ways.
Mobile phones can also strengthen the role of the community
in their participation to local health governance and empower
women regarding their access to antenatal care and healthy
childcare service.
However, it is essential to anticipate at the early stage the
challenges linked to mHealth implementation and to identify
ways to avoid failure during the implementation process.
The main challenges due to weak phone connectivity, unfamiliarity
of community health workers need to be further assessed before
the implementation of this kind of project in order to improve the
sustainability of the project.
Acknowledgement
This study has been funded by International Development
Researches Centre (IDRC/Canada) under grant agreement number
N° 106229-009/2013 within SEARCH programs (Strengthening
Equity through Applied Research Capacity building in eHealth) in
low-and middle-income countries
References
- ITU (2014)Publishes its annual global ICT data and rankings of countries according to the index of ICT development.
- World Bank (2014) World Development Report, Washington DC.
- Hampshire K, Porter G, Owusu SA, Mariwah S, Abane A, et al. (2015) Informal m-health: How are young people using mobile phones to bridge healthcare gaps in Sub-Saharan Africa? SocSci Med 142: 90-99.
- vanHeerden A, Tomlinson M, Swartz L (2012) Point of care in your pocket: a research agenda for the field of m-health. Bull World Health Organ 90: 393-394.
- Braa J, Monteiro E, Sahay S (2004) Networks of open source health care action: sustainable health information systems across developing countries. Society for information management and the management information systems research center, Mineapolis, MN, USA.
- WHO (2011)mHealth: New horizons for health through mobile technologies: second global survey on eHealth. Geneva Switzerland pp: 1-112.
- Niamba L, Sie A, Bagagnan C, Yé M (2011)Annual report of the demographic surveillance system and health nouna.
- Grebot E (2002) Contribution of new information and communications technology in the health service in Africa within the NEPAD.
- Bagayoko CO, Traoré D, Thevoz L, Diabaté S, Pecoul D, et al. (2014) Medical and economic benefits of telehealth in low- and middle-income countries: results of a study in four district hospitals in Mali. BMC Health Serv Res 14: S1-S9.
- Ngabo F, Nguimfack J, Nwaigwe F, Mugeni C, Muhoza D, et al. (2012) Designing and implementing an innovative SMS-based alert system (RapidSMS-MCH) to monitor pregnancy and reduce maternal and child deaths in Rwanda. Pan Afr Med J 13: 31.
- Nurmatov UB, Lee SH, Nwaru BI, Mukherjee M, Grant L, et al. (2016)The effectiveness of mHealth interventions for maternal, newborn and child health in low– and middle–income countries: Protocol for a systematic review and meta–analysis. J Glob Health 4: 010407.
- Craig J, Patterson V (2005) Introduction to the practice of telemedicine. J TelemedTelecare 11: 3-9.
- Patricia M, Hima B, Nadi K, Sarah S, Ada K, et al. (2010) Barriers and gaps affecting mhealth in low and middle income countries. Columbia, USA.
- UIT (2008) Implementing e-Health in developing countries. Guidance and Principles.
- Vital Wave C (2015)eTransformAfrica: health sector study. Sector assessment and opportunities for ICT.
- Arul C, Helena MV, Josib C (2016)mHealthadoption in low-resource environments: a review of the use of mobile healthcare in developing countries - Journal of Health Communication.
- Higgs ES, Goldberg AB, Labrique AB, Cook SH, Schmid C, et al. (2014) Understanding the role of mHealth and other media interventions for behavior change to enhance child survival and development in low- and middle-income countries: An evidence review. J Health Commun1: 164-189.
- Head KJ, Noar SM, Iannarino NT, Grant Harrington N (2013) Efficacy of text messaging-based interventions for health promotion: a meta-analysis. SocSci Med 97: 41-48.
- Labrique AB, Vasudevan L, Kochi E, Fabricant R, Mehl G (2013) mHealth innovations as health system strengthening tools: 12 common applications and a visual framework. Glob Health SciPract 1: 160-171.
- Agarwal S, Perry HB, Long LA, Labrique AB, et al. (2015) Evidence on feasibility and effective use of mHealth strategies by frontline health workers in developing countries: systematic review. Trop Med Int Health 20: 1003-1014.
- Ahmed T, Lucas H, Khan AS, Islam R, Bhuiya A, et al. (2014) eHealth and mHealth initiatives in Bangladesh: a scoping study. BMC Health Serv Res 14: 260.
- WHO (2011) mHealth: New horizons for health through mobile technologies: Second global survey on ehealth.
- Zurovac D, Talisuna AO, Snow RW (2012) Mobile phone text messaging: tool for malaria control in Africa. PLoS Med 9: e1001176.
- Majumdar A, Kar SS, S GK, Palanivel C, Misra P4 (2015) mHealth in the prevention and control of non-communicable diseases in India: Current possibilities and the way forward. J ClinDiagn Res 9: LE06-10.
- Drjack G (2011) Information and communication technology in emergency public health.
- Hall CS, Fottrell E, Wilkinson S, Byass P (2014) Assessing the impact of mHealth interventions in low- and middle-income countries--what has been shown to work? Glob Health Action 7: 25606.
- Tomlinson M, BorusRMJ, Swartz L, Tsai AC (2013)Scalingup mHealth: Where is the evidence? 10: e1001382.
- Diniz E, Albuquerque J, Cernev A (2011) Mobile money and payment: literature review based on academic and practitioner oriented publications 2001-2011.
- WEF (2011) Amplifying the impact: Examining the intersection of Mobile Health and mobile finance, a discussion guide for collaborative insight presented by World Economic Forum in partnership with mHealth Alliance.
- Miller T (2011) Mobile banking could be global health tool. Cell phone user in Kenya.
- World Bank (2011)Mobile payments go viral: M-PESA in Kenya.
- Blair E (2015) Ethiopia launches mobile money schemes to extend banking reach.
- Beshouri C, Chaia A, Cober B, Gravrak J (2010) Banking on mobile to deliver financial services to the poor. In: Mertz R (edn) Global financial inclusion, McKinsey and Company, USA.
- WHO (2007) eHealth for health-care delivery; Department of Essential Health Technologies.
- WHO (2005) The World Health Report 2005 - Make every mother and child count.
- Aranda-Jan CB, Mohutsiwa-Dibe N, Loukanova S (2014) Systematic review on what works, what does not work and why of implementation of mobile health (mHealth) projects in Africa. BMC Public Health 14: 188.
- Jennings L, Gagliardi L (2013) Influence of mHealth interventions on gender relations in developing countries: a systematic literature review.Int J Equity Health 12: 85.
- Cabanes J, Acedera K (2012)Mobile phones and mother-fathers: Calls, text messages, and conjugal power relations in mother-away Filipino families.
- Nouna (2013)Action plan of the health district of nouna. Nouna, Burkina Faso.
- GRET (2015)The mobile service of maternal and child health in the province of Gourma: Project Case MobiSan.
- Simonyan D, Gagnon MP, Duchesne T, Weil AR (2013) Effects of a telehealthprogramme using mobile data transmission on primary healthcare utilisation among children in Bamako, Mali. J TelemedTelecare19:302-306.
- Lechat L, Ridde V, Bonnet E (2010)Action Research on the relevance of a free IVR to improve health governance in Burkina Faso.
- UrganciGI, de Jongh T, JamsekVV, Atun R, Car J (2013) Mobile phone messaging reminders for attendance at healthcare appointments. Cochrane Database Syst Rev 12:CD007458.
- Car J, UrganciGI, de Jongh T, JamsekVV, Atun R. Mobile phone messaging reminders for attendance at healthcare appointments. Cochrane Database Syst Rev7:CD007458.
- Pratyaya M (2014) Challenges and Opportunities for mHealth in Kenya, TechChange, The Institute for Technology and Social Change.
- Ye M, Sie A, Bagagnan C (2015)Technique fifth period report of the project Mos@n: Improving governance and equity in the use of ICT: Case study applied to maternal and child health care, and support of PLWHA in the Health District Nouna, Burkina Faso,CRSN.