Rania Osman A1*, Hassna Ali2, Hala Musa2 and Nidal Ali2
1Senior Educator, Jazan University, Jazan, Saudi Arabia
2Faculty of Nursing, Jazan University, Jazan, Saudi Arabia
- Corresponding Author:
- Rania Osman A
Senior Educator, Jazan University
Jazan, Saudi Arabia
E-mail: dr.raniaosman@hotmail.com
Received Date: September 25, 2019; Accepted Date: October 05, 2019; Published Date: October 12, 2019
Citation: Rania Osman A, Ali H, Musa H, Ali N (2019) Thrombocytopenia in Critically Ill Adult Patients in Medical Intensive Care Unit (ICU): Frequency and Risk Factors in King Fahad Central Hospital, Jazan, KSA. J Intensive & Crit Care Vol.5 No.3:12
Copyright: © 2019 Rania Osman A, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Background: Thrombocytopenia is defined as a platelet count of less than
150 × 109/l. The various comorbidities in the severely ill patient affect platelet
homeostasis, and consequently, thrombocytopenia is very common in critically ill
patients treated in the ICU.
Objective: To assess the frequency of thrombocytopenia in patients admitted to
the medical intensive care unit (ICU) of King Fahad Central Hospital and its risk
factors, during the period from October 2018-January 2019.
Methodology: Data were collected from 160 adult patients admitted to the ICU.
The baseline platelet count was measured and was repeated every other day (for
one-week) during the ICU stay period. Thrombocytopenia was defined as platelet
count of less than 150x109/l.
Results: Among 160 critically ill patients admitted to ICU, 92 (57.5%) were males
and 68 (42.5%) were females. The majority of them 72 (45%) found in age group >60
years. The mean of platelets at admission was 237.6 ± 4.6 and after one-week the
mean of platelets was 121 ± 31.8 (P=0.000). The prevalence of thrombocytopenia
was 70%. Thrombocytopenia was significantly developed in the patients found in
age group >60 years (50%) (P=0.008). The occurrence of thrombocytopenia was
significantly high in the patients received thromboprophylaxis (75%; P=0.000),
antibiotic (89.3%; P=0.000), sedation and mechanical ventilator support (50%;
P=0.003). Additionally the SOFA score was significantly high in the patients with
thrombocytopenia (5.0 ± 0.2 vs. 3.7 ± 0.3; P=0.002) and all the patients (n=4; 100%)
with score 10-12 and the most of the patients (85.7%) with score 7-9 developed
thrombocytopenia (P=0.046).
Conclusion: Thrombocytopenia is common in critically ill patients admitted in the
ICU. Also, thrombocytopenia was significantly associated with elders, in addition
to the patients received thromboprophylaxis, antibiotic, sedation and mechanical
ventilator support as well as the patients with higher SOFA score.
Keywords
Intensive Care Unit; Platelets; Thrombocytopenia; Critical ill
Introduction
Thrombocytopenia is defined as a platelets count <150,000/
mm3. It is the commonest hemostatic disorder in the ICUadmitted
patients affecting around half of them [1]. Severe
thrombocytopenia is when the platelets count drops below 50,000/mm3. It affects around 2-15% of the critically ill
patients [2].
The mechanism for the development of thrombocytopenia can
either be central, peripheral or mixed. Individuals with a central
cause tend to bleed, while those with a peripheral cause are at risk of thrombosis. Further, it can be classified as acquired or
genetic.
There are many risk Factors for the development of
thrombocytopenia that include: sepsis, male gender, use of
inotropes, high severity of illness, renal replacement therapy,
liver failure, and drug induced. And it has been found that sepsis
and trauma are the commonest causes for thrombocytopenia in
the ICU [3]. A decrease in the platelets count is directly linked to
sepsis. Thus, the platelets count is incorporated in the Sequential
Organ Failure Assessment (SOFA) score [4].
Though there are many known causes for thrombocytopenia,
the cause of thrombocytopenia cannot be clearly identified in
more than half of the critically ill patients. This etiology unknown
thrombocytopenia, found in critical illnesses (e.g. sepsis, septic
shock, and trauma) has been termed as “thrombocytopenia in
critically ill patients” TCIP. And it’s suspected to be a predictor of
poor prognosis in these patients [5]. In this study we aimed to
examine this relation in an observational manner in the medical
ICU of King Fahad Central Hospital, as to have a local view of this
issue.
Methodology
Study design
A cross sectional study was conducted over four months in King
Fahad Central Hospital; in the period from October 2018-January
2019. This study was enrolled 160 critically ill patients admitted
to ICU. Personal data, admitting diagnosis, presence of comorbidities,
thromboprophylaxis use, antibiotic use, sedation
and mechanical ventilator support, in addition to SOFA score
were collected. The baseline platelet count was measured and
was repeated every other day (for one-week) during the ICU stay
period. Thrombocytopenia was defined as platelet count of less
than 150x109/l.
Inclusion and exclusion criteria
All patients who were hospitalized in the ICU during the data
collection day were included. Patients with a platelets count
<150,000/mm3 upon admission to the ICU and those with an
admitting diagnosis of coagulopathy were excluded.
Statistical analysis
The study variables were analyzed using SPSS 21.0 (IBM Corp.,
Armonk, NY, USA) and presented as frequencies with percentages.
Qualitative data is going to be analyzed using the Chi-Square test
and P-value considered significant if <0.05.
Results
A total of 160 critically ill patients admitted to ICU were
participated in the present study. 92 (57.5%) were males and 68
(42.5%) were females. The majority of them 72 (45%) found in
age group >60 years (Table 1).
| |
Number |
% |
| Gender |
|
|
| • Male |
92 |
57.5 |
| • Female |
68 |
42.5 |
| Age |
|
|
| • <40 |
52 |
32.5 |
| • 40-60 |
36 |
22.5 |
| • >60 |
72 |
45.0 |
Table 1 Showed the age and gender of the critically ill patients admitted to ICU (N= 160)
Concerning to the clinical characteristics, the majority of the
patients 64 (40%) had hypertension. Also, 104 (65%) received thromboprophylaxis, 116 (72.5%) received antibiotics and 68
(42.5%) underwent sedation and mechanical ventilator support.
In SOFA scoring, the mean of the patients was 4.6 ± 2.1 and the
most of the subjects 128 (80%) found in score range from 0-6
(Table 2).
| |
|
Number |
% |
| Comorbidities |
|
|
| • Hypertension |
64 |
40.0 |
| • DM |
44 |
27.5 |
| • Thyroid dysfunction |
8 |
5.0 |
| • CVD |
24 |
15.0 |
| • Renal diseases |
12 |
7.5 |
| Thromboprophylaxis use |
104 |
65.0 |
| Antibiotic use |
116 |
72.5 |
| Sedation and mechanical ventilator support |
68 |
42.5 |
| SOFA score (mean ± SD) |
|
(4.6 ± 2.1) |
| • 0-6 |
128 |
80.0 |
| • 7-9 |
28 |
17.5 |
| • 10-12 |
4 |
2.5 |
Table 2 Showed the clinical characteristics of the critically ill patients admitted to ICU (N= 160)
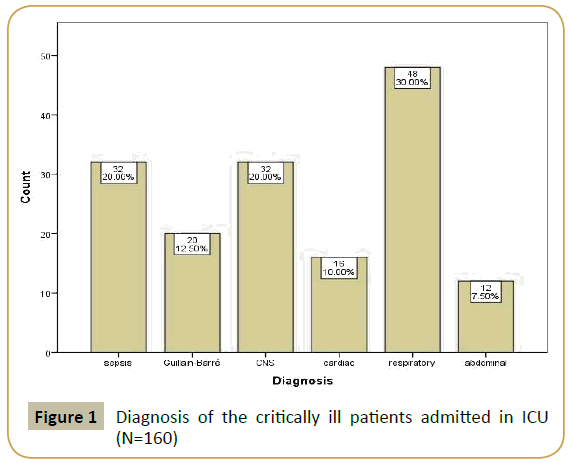
Concerning the admitting diagnosis, the majority of the patients
had respiratory system diseases (Figure 1).
Figure 1: Diagnosis of the critically ill patients admitted in ICU (N=160)
In the platelets counts among the study participants, the mean
of platelets at admission was 237.6 ± 4.6 and after one-week the
mean of platelets was 121 ± 31.8. The difference was statistically
significant (P=0.000) (Table 3).
| |
At admission |
After one-week |
P value |
| |
(mean ± SD) |
(mean ± SD) |
|
| Platelets count (109/l) |
237.6 ± 4.6 |
121 ± 31.8 |
0.000 |
Table 3 Showed the means of platelets counts at admission and after one-week among critically ill patients (N= 160)
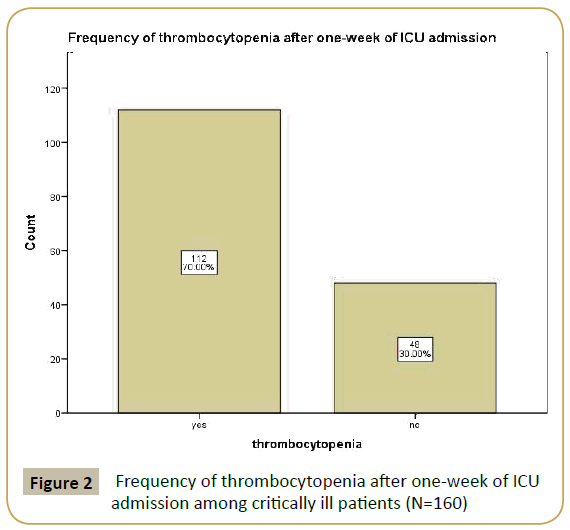
According to the development of thrombocytopenia, 112 (70%)
of the critically ill patients admitted to ICU had thrombocytopenia
(Figure 2).
Figure 2: Frequency of thrombocytopenia after one-week of ICU admission among critically ill patients (N=160)
The age of the patients was significantly associated with
the development of thrombocytopenia as the majority of
thrombocytopenia developed in the patients found in age
group >60 years (50%) (P=0.008). Additionally, the gender
showed in significant association with the development of
thrombocytopenia (P=0.140) (Table 4).
| |
Thrombocytopenia |
|
| |
Yes (n= 112) |
No (n= 48) |
P value |
| Gender |
|
|
0.140 |
| •Male |
68 (60.7%) |
24 (50%) |
| •Female |
44 (39.3%) |
24 (50%) |
| Age |
|
|
|
| •<40 |
28 (25%) |
24 (50%) |
0.008* |
| •40-60 |
28 (25%) |
8 (16.7%) |
| •>60 |
56 (50%) |
16 (33.3%) |
*P. value is significant (< 0.05)
Table 4 Showed the association between development of thrombocytopenia with age and gender of the critically ill patients admitted to ICU (N= 160)
In same manner, the admitting diagnosis of the patients was no significantly associated with the development of
thrombocytopenia (P=0.059) (Table 5).
| |
Thrombocytopenia |
|
| |
Yes (n= 112) |
No (n= 48) |
P value |
| Sepsis |
24(21.4%) |
8(16.7%) |
0.059 |
| Guillain-Barré |
16(14.3%) |
4(8.3%) |
| CNS |
20(17.9%) |
12(25%) |
| Cardiac |
12(10.7%) |
4(8.3%) |
| Respiratory |
36(32.1%) |
12(25%) |
| Abdominal |
4(3.6%) |
8(16.7%) |
Table 5 Showed the association between development of thrombocytopenia and admitting diagnosis of the critically ill patients admitted to ICU (N= 160)
Regarding the association between thrombocytopenia and
clinical characteristics of the patients; there was insignificant
relationship between the thrombocytopenia and the presence
of co-morbidities (P>0.05). Moreover, the occurrence of
thrombocytopenia was significantly high in the patients received
thromboprophylaxis (75%; P=0.000), antibiotic (89.3%; P=0.000),
sedation and mechanical ventilator support (50%; P= 0.003).
Additionally the SOFA score was significantly high in the patients
with thrombocytopenia (5.0 ± 0.2 vs. 3.7 ± 0.3; P=0.002) and all
the patients (n=4; 100%) with score 10-12 and the most of the
patients (85.7%) with score 7-9 developed thrombocytopenia
(P=0.046) (Table 6).
| |
Thrombocytopenia |
|
| Comorbidities |
Yes |
No |
P Value |
| • Hypertension |
44(39.3%) |
20(41.7%) |
0.425 |
| • DM |
32(28.6%) |
12(25%) |
0.398 |
| • Thyroid dysfunction |
6(5.4) |
2(4.2%) |
0.641 |
| • CVD |
20(17.9%) |
4(8.3%) |
0.093 |
| • Renal diseases |
10(8.9%) |
2(4.2%) |
0.536 |
| Thromboprophylaxis use |
84(75%) |
20(41.7%) |
0.000* |
| Antibiotic use |
100(89.3%) |
16(33.3%) |
0.000* |
| Sedation and mechanical ventilator support |
56(50%) |
12(25%) |
0.003* |
| SOFA score (mean ± SD) |
5.0±0.2 |
3.7±0.3 |
0.002* |
| • 0-6 |
84(65.5%) |
44(34.4%) |
0.046* |
| • 7-9 |
24(85.7%) |
4(14.3%) |
| • 10-12 |
4(100%) |
0(0%) |
*P. value is significant (< 0.05)
Table 6 Showed the association between development of thrombocytopenia and clinical characteristics of the critically ill patients admitted to ICU (N= 160)
Discussion
Although thrombocytopenia appears as a common finding in the
ICU, yet it is still unclear whether thrombocytopenia is the cause
or just a risk factor for ICU-related mortality. The present study
demonstrated that the incidence of thrombocytopenia of at least
one platelet count of less than 150×109/l was 70% among medical
patients in ICU. Our finding was found in the range of the occurrence
of thrombocytopenia in ICU patients (35% to 80%) [6].
Our results were also found higher than the findings of Mohammad
A, et al. (20%) [7] and Divya K, et al. (67.5%) [8]. these variations
in the frequencies of thrombocytopenia might be referred to the
differences in geographical areas, origins, techniques used and
sample sizes.
There was no difference between thrombocytopenic and
nonthrombocytopenic patients in terms of age, in which one the
majority of the patients developed thrombocytopenia were elder
patient (>60 years) (P=0.008). These findings were agreed with
the results of Richard S. et al who stated There was difference
between thrombocytopenic and nonthrombocytopenic patients
in terms of age, as elder patients (>55 years) tend to developed
thrombocytopenia than other (P<0.05) [9]. In other side our
study failed to assess significant association with gender.
The preset study also showed that, the occurrence of
thrombocytopenia was significantly high in the patients
received thromboprophylaxis (75%; P=0.000). Similar
findings were obtained by Williamson D. et al. The risk of
thrombocytopenia was higher in patients who received LMWH
thromboprophylaxis [10].
Also the current study showed that, antibiotic (89.3%; P= 0.000),
Sedation and mechanical ventilator support (50; P= 0.003), and the
SOFA score (5.0 ± 0.2 vs. 3.7 ± 0.3; P= 0.002) were independently
associated with the development of thrombocytopenia in
critically ill patients. Our results were gone in same line with the
studies of Mohammad A et al. [7] and Divya K et al. [8].
ICU admission indications and presence of comorbidities did not
differ in thrombocytopenic and nonthrombocytopenic patients
(P>0.05). This was in agreement of the study of Mohammad A
et al. [7].
Conclusion
The present study concluded that, thrombocytopenia is common
in critically ill patients admitted in the ICU. Also, thrombocytopenia
was significantly associated with elders, in addition to the patients
received thromboprophylaxis, antibiotic, sedation and mechanical
ventilator support as well as the patients with higher SOFA score.
Recording of the baseline platelet count for critically ill patients
admitted to the ICU is recommended with further continuous
monitoring of the platelet count during the whole ICU stay.
References
- Strauss R, Wehler M, Mehler K, Kreutzer D, Koebnick C, et al. (2002) Thrombocytopenia in patients in the medical intensive care unit: bleeding prevalence, transfusion requirements, and outcome. Crit Care Med 30: 1765-1771.
- Rice TW, Wheeler AP (2009) Coagulopathy in critically ill patients: part 1: platelet disorders. Chest 136: 1622-1630.
- Greinacher A, Selleng S (2016) How I evaluate and treat thrombocytopenia in the intensive care unit patient. Blood 128: 3032-3042.
- Larkin CM, Santos-Martinez MJ, Ryan T, Radomski MW (2016) Sepsis-associated thrombocytopenia. Thromb Res 141: 11-16.
- Chang JC (2016) Thrombocytopenia in critically ill patients due to vascular microthrombotic disease: pathogenesis based on “two activation theory of the endothelium”.Vascul Dis Ther 2.
- Selleng S, Malowsky B, Strobel U, Wessel A, Ittermann T, et al. (2010) Early-onset and persisting thrombocytopenia in post-cardiac surgery patients is rarely due to heparin-induced thrombocytopenia, even when antibody tests are positive. J Thromb Haemost 8: 30-36.
- Mohammad A Faramawy, Iman H Galal, Asmaa M Elasser (2014) Assessment of thrombocytopenia in critically ill patients. Egypt J Bronchol 8: 143-148.
- Divya Khurana, Shilpa A Deoke (2017) Thrombocytopenia in Critically Ill Patients: Clinical and Laboratorial Behavior and Its Correlation with Short-term Outcome during Hospitalization. Indian J Crit Care Med 21: 861-864.
- Richard Strauss, Markus Wehler, Katrin Mehler, Daniela Kreutzer, Corinna Koebnick, et al. (2002) Thrombocytopenia in patients in the medical intensive care unit: Bleeding prevalence, transfusion requirements, and outcome. Crit Care Med 30: 1765-1771.
- Williamson DR, Albert M, Heels-Ansdell D, Arnold DM, Lauzier F, et al. (2013) Thrombocytopenia in critically ill patients receiving thromboprophylaxis: frequency, risk factors, and outcomes. Chest 144: 1207-1215.