Ruby Chang1, Leah Greene2 and Kristine McCluskey1*
1Department of Pathology and Immunology, Baylor College of Medicine in Houston, Texas, USA
2Department of Pathology, University of Texas Health Science Center in Houston, Texas, USA
*Corresponding Author:
Kristine McCluskey
MHS, PA (ASCP)cm is a Pathologists’
Assistant and Faculty at Baylor College of Medicine
Department of Pathology and Immunology in Houston
Houston, Texas, USA
Tel: 713-873-0742
E-mail: mccluske@bcm.edu
Received date:November 01, 2017; Accepted date: November 06, 2017; Published date: November 12, 2017
Citation: Chang R, Greene L, McCluskey K (2017) Pathology Teaching and Quality Improvement Tools. J Cancer Epidemiol Prev. 2017, 2:1.
Copyright: © 2017 McCluskey K, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Keywords
Pathology; Mastectomy; Lumpectomy; Tumor
Introduction
The College of American Pathology (CAP) developed recommended protocol templates for diagnostic sampling and turnaround time, or time for processing resulting in final diagnosis. The American Joint Committee on Cancer (AJCC) developed guidelines for tumor size and location of cancer involvement. To help prosectors meet each of the guidelines, breast history and specimen grossing worksheets have been implemented by Baylor College of Medicine staff since 2008 at Ben Taub General Hospital. These worksheets have been used as teaching tools which facilitated the grossing process.
At our institution prior to 2008, details were written on sheets of paper, requisition slips or on specimen containers. Formal instruction was confined to a single breast grossing lecture during the resident orientation period and further instruction occurred during intraoperative gross consultation by a pathologist. A single grossing manual existed in the gross room of the hospital. No breast grossing templates were available. Gross dictations were corrected by residents, fellows and pathologists upon pre-screening of microscopic slides and sign out before final reports were sent to clinicians. One breast pathologist and one breast fellow were present to generate those reports which resulted with a turnaround time, in a 2-7 day period, of 15%, with the target turnaround time being 5 days for report completion of mastectomies and lumpectomies. Prior to 2008, the residents noted that there was a lack of immediate and consistent teaching presence and the specimens were held until teaching was available. There was a return to the specimens for additional sampling which required additional processing time.
Literature has shown that turnaround time is affected by trainees in academic settings. Pathology residency training programs in one study published by CAP reported that an extra day or two is added to turnaround time and generally seems to be the experience of many centers with residency programs “simply because of the inefficiencies of dealing with trainees new to the process. Sometimes they get more complex specimens that they don’t know how to handle well, and you might have to go back and put in more sections [1].
Additional guidance and education was needed to address suboptimal quality and efficiency at our institution. In 2008, the breast history and specimen worksheets were added as teaching resources. Our pathologists’ assistant gross instructor encountered a similar worksheet utilized as a communication tool to facilitate specimen processing and diagnosis between pathology and radiology departments for stereotactic breast core biopsies. This tool included specimen fixation time, biopsy location, imaging details and radiologic differential diagnosis [2]. Timely and accurate information was vital to decision making and history was often incomplete and inaccurate. Therefore, implementation of guidelines and forms improved the completeness of pathology reporting. Furthermore, there was potential for decreasing errors in confusing patient information when there were several similar procedures during the day. Literature suggests eliminating a reliance on memory [3]. Utilizing worksheets became a succinct, additional review and reminder of the grossing process when the single lecture during the orientation period and a brief review with the pathologist during intraoperative gross consultation was insufficient.
Methods
Our studies regarding this manuscript, H-41220, H-42502 and 17-11-1794 received approval from Baylor College of Medicine's Institutional Review Board and Harris Health System.
After consultation with the breast pathologists and reviewing both AJCC guidelines and CAP Cancer Protocol Templates and, we designed our three worksheets using Microsoft Word but other computer programs could be used to create similar tables and graphics [4,5].
Our first worksheet, the breast history worksheet, was most useful for intraoperative consultation (Supplementary File 1). We drew tables and entitled them with a question to consider or basic patient identification. The identification included patient name and medical record number. Laterality, size and location were demonstrated in two clock face diagrams labeled with “R” and “L” for right breast and left breast, respectively. Diagnosis was listed and included the grade, growth pattern and biomarker status (ER, PR and Her-2). The following questions were posed such as “Is there a biopsy clip? If yes, what type of clip is present such as wing, ribbon, coil, barrel, bar, etc.? Is there palpable lymphadenopathy or lymphadenopathy seen on imaging? If yes, is it palpable or imaged? Is there lymphovascular invasion on initial biopsy? Was the patient treated? If yes, what type of therapy was given?” The choices for this question were hormonal or chemotherapy. “What was the patient’s original tumor size before treatment if treated and what is the current tumor size?” We also added a box to include that patient’s BRCA, breast cancer gene, status.
We completed these sheets after reviewing the surgery schedules one day in advance of the scheduled intraoperative consultation in preparation for intraoperative frozen section diagnosis and/or gross consult if necessary.
Our second worksheet, the lumpectomy worksheet, was most useful for lumpectomy specimen processing (Supplementary File 2). We drew tables and the specimen diagrams and entitled them with “specimen”, “ink code”, “tumor”, “slices”, “and other”, “diagram”. The specimen portion included size, weight, size of skin and skin color if attached to the specimen. Our orientation ink codes listed the colors specific to our practice and can be adjusted as we used four colors and do not use six to traditionally represent all margins. Due to the manner in which the specimen was cut from medial to lateral marginal ends, all four colors met at those ends and the ends were noted in the section code in designated cassettes. Tumor features included size, shape, color, consistency, and its distance from all six margins. The number of slices, slice with biopsy clip, and slices with tumor could be noted. Indicated in the “other” table were the appearance of remaining breast tissue and additional lesions present. The diagram slices were drawn as circles, numbered and labeled with cut direction, placement direction on the cutting board and the margins.
Lastly, most useful for mastectomy processing was the mastectomy worksheet (Supplementary File 3). We drew tables and specimen diagrams and entitled them with “specimen”, “tumor”, “ink code”, “slices”, “other” and “diagram”. Specimen size, weight, skin size and color if attached, nipple size, areola size, skin lesions, axillary tail size, pectoralis attachment (includes 2 clock face diagrams labeled with “R” and “L” for right breast and left breast) were entered in the first table. Tumor size, shape, color, consistency, distance from the superficial superior, superficial inferior and deep margins were recorded in the second table. We used 3 ink code choices designating the superficial superior, superficial inferior and deep margins and those using the worksheets can customize their own scheme. Number of slices, location of clips, and location of tumor or biopsy sites, nipple location were indicated in the slice table. The table labeled as “other” could be used to indicate the percentage of fibrous tissue and adipose tissue within the remaining specimen, additional lesions, and axillary tail lymph node sizes and cut surface appearance with or without biopsy clip presence. The mastectomy slice diagram contained numbered of slices drawn as half circles reflecting the curvaceous superficial surface and the flat deep fascial plane with labeling provided to show the medial to lateral direction.
We organized the lumpectomy and mastectomy sheet entries in the same order as seen on the final gross description used in the reports. We attached our worksheets to the requisition slips sent to the assigned attending pathologists.
After 9 years, 30 residents and 10 PA students were sent a questionnaire concerning the worksheets which was followed with a statement that their participation constituted consent to underlying research.
Results
Thirteen people (n=13) responded to the questionnaire. The breast history worksheet strongly directed them to find the most pertinent information and prepared them for the grossing service (Figure 1). The lumpectomy worksheets offered an organized approach to grossing (Figure 2). The lumpectomy worksheets allowed the participant to focus upon recording pertinent details concerning processing lumpectomies for diagnostic purposes (Figure 1). The mastectomy worksheets organized grossing approach (Figure 2). The mastectomy worksheets 100% allowed the participant to “always” focus upon recording pertinent details concerning processing mastectomies for diagnostic purpose. Early in training, the participants found that the worksheets were valuable to processing breast specimens and increased their confidence level (Figure 3). All of participants answered that they plan to use worksheets like these in the future. The breast worksheets were useful teaching tools (Figure 3).
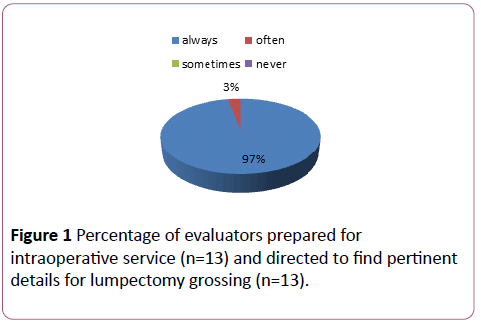
Figure 1: Percentage of evaluators prepared for intraoperative service (n=13) and directed to find pertinent details for lumpectomy grossing (n=13).
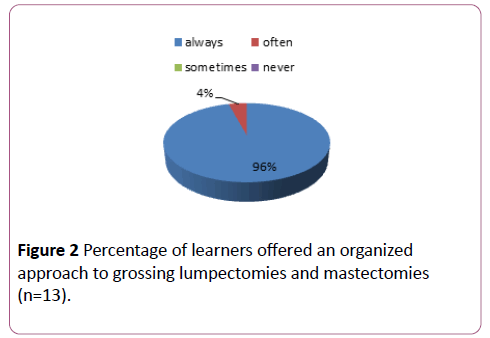
Figure 2: Percentage of learners offered an organized approach to grossing lumpectomies and mastectomies (n=13).
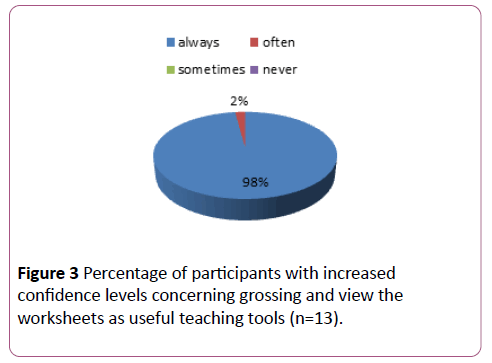
Figure 3: Percentage of participants with increased confidence levels concerning grossing and view the worksheets as useful teaching tools (n=13).
The residents responded as follows when asked for their opinion regarding the worksheet resources:
• “I can’t finish my dictations without consulting the worksheets to make sure that I remembered everything to include in the report”.
• “This is a smart, systematic approach that makes the grossing process easier to learn and to complete cases”.
• “Without templates and worksheets, it would take much longer to finish our cases, we wouldn’t have enough direction and it would reduce exposure to additional new learning cases on our grossing days”.
• “These worksheets are an indispensable resource.”
The breast history worksheets were an instant, direct and comprehensive reference tool during intraoperative gross consultation when maximum time allowed for the pathologist to review the specimens was 20 minutes as per CAP regulation. It was rare to reference electronic patient charts during the intraoperative consultation because the history pertaining to the breast cases were reviewed in advance unless the prosectors for the cases were unprepared.
The diagrams demonstrated exact tumor site, the exact location of margin sampling, the clip site as clips must be removed from the tissue to avoid hindrance of microtome sectioning during slide preparation and record the needle localization site’s insertion if present. The pathologists could easily see the pictorial view of the specimen without retrieving the specimen and direct additional sampling. The prosector could in turn match the diagrams to the remaining tissue and the questionable slides to ensure sampling accuracy. In relation to the dictation, if our Dictaphone equipment malfunctioned or if the dictation was lost in some other manner, the vital details were recorded and another dictation could be constructed. We also used the sheets to check discrepancies when typos occurred or misconstrued words could be transcribed when some prosectors were more difficult to understand. The worksheets created a larger picture offering direction, organization and preparation resulting in error reduction while increasing efficiency.
In relation to the efficiency provided by the worksheets, in 2008, the turnaround time in a 2-7 day period increased to 41% with one pathologist and one fellow reading slides and generating final reports after the implementation of the worksheets. In 2010-2012, with one pathologist and one fellow signing out, the turnaround time was 40% within a 7 day period and 100% of reporting was completed in an average of 8 days (Figure 4). The average of 40%in a 2-7 day period with 100% on an eighth day continued in the following years to present day with one attending pathologist stationed at Ben Taub and with no consistently present fellow. There had been multiple PAs and PA students stationed at Ben Taub as a teaching resource since before 2008 and worksheets were non-existent.
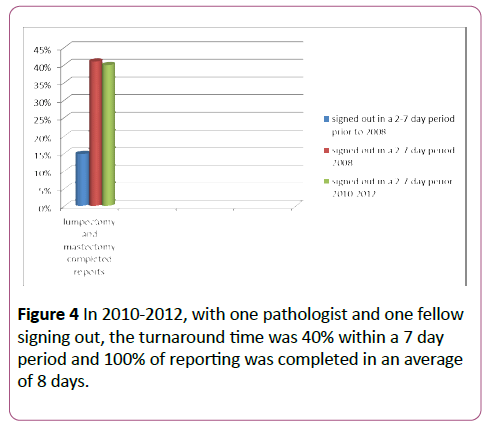
Figure 4: In 2010-2012, with one pathologist and one fellow signing out, the turnaround time was 40% within a 7 day period and 100% of reporting was completed in an average of 8 days.
These worksheets were adopted by several learners to use in future practice, were required by the breast service and were used as orientation materials for pathologists new to the department. They were distributed to the Baylor College of Medicine’s private group, Community Pathology Associates, who may be involved with intraoperative gross consultation at smaller outside surgery centers to instill consistency, efficiency and optimal patient care. Additional hospitals serviced by Baylor staff use these resources as well.
Discussion
These worksheets served as a condensed version of the patient history for immediate recall of pertinent information during the intraoperative gross consultation and direction for gross permanent sampling thereafter.
The worksheets were attached to the patient report and filed for future reference. The worksheets were copied and provided in all grossing spaces and their availability required monitoring. The worksheet templates were uploaded to a sharing site where they could be accessed by all prosectors with the patient information cut and pasted or typed into the template and then uploaded to patient reports.
Future facilitation included attaching the worksheets to reports electronically for easier access. Gross photographs could be added to the report and incorporated into the worksheets for the most accurate view of the gross specimen. New camera systems providing the immediate uploading of specimen photographs could readily deliver this purpose.
Acknowledgements
We would like to thank Virginia Niebuhr, PhD for her mentorship during the writing process and Margaret Ehling for her assistance with data analysis.
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Conflicts of Interests
The authors declare that there is no conflict of interest.
References
- Bowers J (2012) On complex surg path, how do TATs compare? CAP Today Online.
- Askew JB (2008) Private Practice Pathology, Breast Care, and Economics. Seminars in Breast Disease, pp: 129-135.
- Nakleh RE, Gephart G, Zarbo RJ (1999) Necessity of Clinical Information in Surgical Pathology: A College of American Pathologists Q-Probes Study of 771,475 from 341 Institutions. Archives of Pathology and Laboratory Medicine 13: 615-619.
- Edge SB (2010) AJCC Cancer Staging Manual. New York, Springer.
- Amin MB, Edge S, Greene F, Byrd DR, Brookland RK, et al. (2016) Primary Source AJCC Cancer Staging Manual. Springer.