Keywords
Percutaneous dilational Tracheostomy, Fiberoptic bronchoscopy,
Intensivist, Ciaglia blue rhino, Griggs technique.
Introduction
Pediatric Intensive Care implies looking for critic patient’s
wellbeing who suffered acute changes in their physiological and
biochemical parameters with a high risk of death [1], this is the
description used by Marilyn to define critical care in context.
There are many multidisciplinary therapies, which give and keep
wellness to pediatric patient’s health, and it is important to
mention that ECMO can be a treatment option to treat critical
patients refractory to conventional medical treatment. There are few centers in the world with adequate hospital facilities for this
technology, and experience in this area has been increasing along
with new studies have been done about its use, benefits, adverse
effects, patient’s mortality. The most questionable aspect of
this therapy is high mortality rate related to long and short term
ECMO complications, Important questions mentioned by Loren
and López in their respective works, on the various complications
during the use of ECMO such as clot formation, thrombosis,
infections and hemolysis; problems in anticoagulation therapy
during ECMO therapy and massive bleeding, all this to list some
of the most important [2,3], Similarly, other important authors such as Hwa Jin and Barton emphasize the time of anticoagulation
administration in ECMO, underlying disease, type of ECMO,
systemic perfusion parameters and indications for ECMO as part
of the risk in patient mortality [4,5]. Finally, Doymaz comments
that associating complications from anticoagulation during ECMO
with poor systemic perfusion data related to hemodynamic values
such as lactate and venous reserve can negatively influence
patient survival, increasing mortality considerably [6].
Materials and Methods
This is a retrospective observational cohort study using multiple
logistic regression. Fifty neonatal and pediatric patients recorded
on ECMO Muguerza Department electronic database from January
1, 2013 to June 1, 2019. Patients without ECMO treatment were
excluded and, according to exclusion criteria, pediatric patients
suffering critical disease were not included, as well as ECMO use
criteria that for some reason ECMO department records were
missing which did not have a relationship with mortality or base
disease improvement.
This statistical analysis was made using R Comander Kit and
R Statistic Analysis. Quartile comparison graphic methods
distribution was analyzed, variables are expressed as medium
and standard deviation in case of normality, and median
and interquartile range in case of no normality. Comparison
between measures of central tendency is made using parametric
or no parametric statistics depending on their distribution.
A distribution different to the normal was identified; hence
variables are expressed in terms of median and interquartile
range (Table 1). Then, a continuous variables comparison was
made ranking patients according to their survival using a Mann-
Whitney U Test, a non-parametric test (Table 2). As exploratory
test, a logistic regression model was made with the maximum
model:
| Variable |
Median |
Interquartile range |
| Average ACT |
213 |
56.7 |
| Average Heparin (av U/Kg) |
21 |
7.7 |
| Average initial U (ds U/Kg) |
15 |
7.75 |
| Maximum U (max. U/Kg) |
30 |
15 |
| Average Lactate |
3 |
2 |
| VSO2 |
73 |
9.5 |
| Average Days Age |
18 |
328 |
| ECMO Days |
5 |
3.75 |
Note: ACT = Activated Coagulation Time; VSO2 = Central Venous Saturation; ECMO = Extracorporeal Membrane Oxygenation
Table 1 Continuous Variables with abnormal presentation.
| Variable |
Dead |
Alive |
P Value |
| Average ACT |
231.6 |
199.7 |
0.06 |
| Average Lactate |
4.8 |
3.1 |
0.06 |
| VSO2 (Central Venous Saturation) |
71.7 |
75.03 |
0.1 |
| U/Kg ds |
15.78 |
17.22 |
0.4 |
| U/Kg max |
32.1 |
32.3 |
0.9 |
| U/Kg average |
20.4 |
22.5 |
0.4 |
| ECMO Days |
7.3 |
5.6 |
0.2 |
Note: ACT =Extracorporal Coagulation Time; VSO2 = Central Venous Saturation; U/Kg ds = HNF Initial Units; U/Kg max = HNF maximum units; U/Kg average = HNF average units; ECMO Days = Extracorporeal Membrane Circulation days.
Table 2 Continuous variables comparison with survival. Mann-Whitney U Test.
DEATH = average ACT + average lactate + average U/Kg (nonfractionated
heparin) + VSO2 + ECMO total time + initial U/Kg
non-fractionated heparin + maximum U/Kg non-fractionated
heparin + gender
Variance factor was calculated eliminating variables with results
above three. Then, a mathematical model was made using Type II
ANOVA Models, reaching a minimal model with all the significant
variables.
“DEATH = ECMO (VA/VV) + AVERAGE LACTATE + AVERAGE
VSO2”
A Non-significant Theorical Model was calculated, making
a comparison with the Minimal Model obtained at the end
of the modeling, obtaining statically significant differences: p-value<0.001. As response variables were categorical and
continuous, a multiple logistic regression model was made;
significance of the model was evaluated using a common
likelihood ratio test with theoretical null model. Final model
was significant. The calculation of the generalization was made
through the coefficient R2 equal to 0.05, so the mortality is
associated to 5% to these final variables: “DEATH = ECMO (VA/
VV) + AVERAGE LACTATE + AVERAGE VSO2”
Results
The goal of the study was to identify influence of variables on
death of population. Since 2013, a total of 50 neonatal and
pediatric patients were recorded, who were treated using ECMO.
In demographics, there were 25 female patients (50%) vs 25
male patients (50%); 23 pediatric patients (46%) vs 27 neonatal
patients (54%). In pediatric patients, average age range was 31.3
months vs 2.3 days age in neonatal patients; the death average
age range was 4 months (124 days) (Table 3). In anticoagulation
standards, average ACT in pediatric patients was 196 seconds,
224 seconds in neonatal patients, and death average ACT was
233 seconds. Initial heparin units in case of death de average was
15.7 U/Kg, and average maximum units in case of death was 31
U/Kg (Table 4).
Total Patients
50 patients |
50 patients |
Gender
1.- Male
2.- Female |
Age range
death |
| Pediatric |
23 (46%) |
|
|
| Neonatal |
27 (54%) |
|
|
| Dead |
19 patients (38%)
6 pediatric (12%)
14 neonatal (26%) |
Pediatric:
1.- 4 (21%)
2.- 2 (10.5%)
Neonatal:
1.- 6 (31.7%)
2.- 7 (36.8%) |
124 days (4 months) |
Table 3 Demographic variables description, gender, age.
PATIENTS
50 TOTAL PATIENTS |
AVERAGE ACTIVATED COAGULATION TIME |
AVERAGE DS U/KG |
AVERAGE U/KG MAX |
| PEDIATRIC |
196 sec |
17 units |
35.3 units |
| NEONATAL |
224 sec |
16.3 units |
30.5 units |
| DEAD |
233 sec |
15.7 units |
31 units |
Table 4 Anticoagulation variable description related to mortality.
Average ECMO therapy time was 6 days, 5.4 days for pediatric
patientsvs 6.1 days for neonatal patients, and average time of
death of 5.7 days. ECMO type used was VA type for 42 patients
(84%), 23 were pediatric patients (46%) vs 19 neonatal patients
(73%). VV ECMO was used in eight neonatal patients (16%).
Mortality was more related to VA ECMO (73%) compared to
VV ECMO (27%). On diagnosis, in pediatric group 14 patients
underwent ECMO by cardiac disease (48%), 3 patients by
respiratory disease (13%), and 6 patients by infectious diseases
(26%). Into the neonatal group, 13 patients underwent ECMO by
cardiac cause (48%), 13 patients by respiratory disease (48%), and
1 patient by infectious disease (4%). The most mortality related diagnosis was cardiac disease (57% of deaths) (Table 5). In case
of Central Venous Oxygenation, the average value related to
more mortality was 68% CVO2, and 5.6 mmol/Lt average lactate
value as well(Tables 6-8). We have a 66 % survival value and 38%
in mortality.
PATIENTS
50 TOTAL PATIENTS |
AVERAGE ECMO TIME |
ECMO TYPE |
DIAGNOSIS
1. CARDIAC
2. RESPIRATORY
3. INFECTIOUS
|
| PEDIATRIC |
5.4 days |
VA 46%
VV 0% |
1. 14 (60%)
2. 2. 3 (13%)
3. 3 6 (26%)
|
| NEONATAL |
6.1 days |
VA 38%
VV 16% |
1. 13 (48%)
2. 2. 13 (48%)
3. 3. 1 (4%)
|
| DEAD |
5.7 days |
VA 14 (73%)
VV 5 (27%) |
1. 11 (57%)
2. 2. 7 (36%)
3. 1 (7%)
|
Note: VA = Venous-Arterial, VV = Veno-Venous, ECMO = Extracorporeal
Membrane Circulation
Table 5 Variables description related to time, ECMO type and diagnosis.
PATIENTS
50 TOTAL PATIENTS |
AVERAGE CENTRAL VENOUS SATURATION |
AVERAGE BLOOD LACTATE |
| PEDIATRIC |
73.5 % |
3.2 mmo/Lt |
| NEONATAL |
73.5% |
4.6 mmo/Lt |
| DEAD |
68% |
5.6 mmol/Lt |
Table 6 Hemodynamic Variables description related to mortality.
| Variable |
Name |
Description |
Category/ Measurement unit |
Variable Type |
| U/Kg ds |
Units |
Induction dose to start anticoagulation |
International Units |
Continuous |
| U/Kg max |
Units |
Maximum dose needed to induce anticoagulation |
International Units |
Continuous |
| U/Kg average |
Units |
Average dose to induce anticoagulation |
International Units |
Continuous |
| ECMO Time |
Time |
Time of use of anticoagulation therapy |
Days |
Continuous |
| Blood Lactate |
Lactate |
Average numerical value of blood lactate by venous gasometry in ECMO patients |
Mmo/Lt |
Continuous |
| Central Venous Oxygen Saturation |
SVO2 |
Average numerical value of central venous oxygen saturation taken from a central access to the heart. It is estimated in percentage |
Percentage |
Continuous |
| ACT |
Activated Coagulation Time |
Average ACT result |
Seconds |
Continuous |
| Average age |
Days |
Average age in days |
Days |
Continuous |
Table 7 Continuous variables.
| Survival |
Death |
Dead patients during ECMO Therapy |
1 (alive)
2 (dead) |
Discrete
Dichotomous |
| ECMO Type |
VA ECMO
VV ECMO |
ECMO type used for support |
1. VA
2. VV |
Discrete
Dichotomous |
| Diagnose |
Cause to start ECMO |
Diagnostic reason to start ECMO therapy |
1. Cardiac
2. Respiratory
3. Infectious |
Discrete
Dichotomous |
Table 8 Dichotomous Discrete Variables.
Here below statistical analysis results are described using multiple
logistic regression.
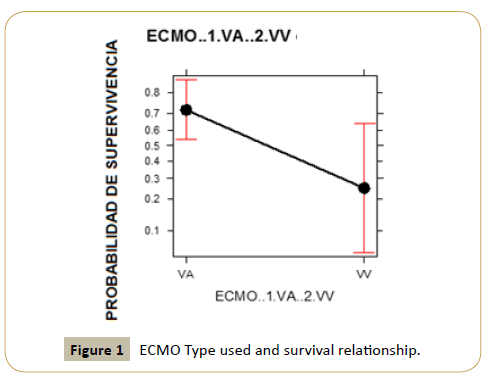
Figure 1 is an effect representative graphic where ECMO type
and its related survival are shown, and we can determine that VA
ECMO use increases survival probability compared to VV ECMO,
which decreases patient’s survival.
Figure 1: ECMO Type used and survival relationship.
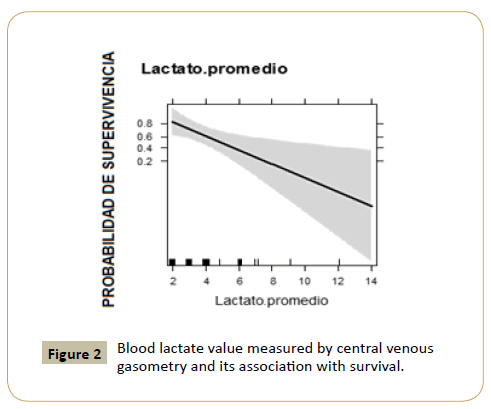
Figure 2 is an effect representative graphic presenting central
venous SBG blood lactate value and survival relationship. We can determine that as blood lactate increases, survival probability
decreases significantly, compared to blood lactate decreasing
which is related to higher survival probability.
Figure 2: Blood lactate value measured by central venous gasometry and its association with survival.
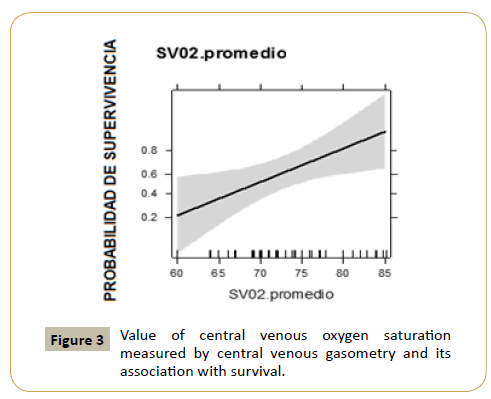
Figure 3 represents central venous SBG central venous saturation
related to survival. We can determine that, when central SVO2
increases, survival probability increases significantly compared
to low central SVO2 which is related to lower survival probability.
Figure 3: Value of central venous oxygen saturation measured by central venous gasometry and its association with survival.
Discussion
In this study, we recorded 50 patients into the mentioned period.
With the obtained results we can discuss that, based on the
analysis of the descriptive databasevariables (Table 7-8). Most of
patients needed a progressive increase of non-fractioned heparin unit/kg dose in continuous infusion to obtain wider ranges of
correct anticoagulation, calculated in this study by ACT (Activated
Coagulation time). A 213 seconds median was obtained with a
56.7 interquartile range, when we determined ACT in surviving
patients (199.7 sec) compared to non-surviving patients (231.6
sec). Mortality did not have a significant p calculated using a
Mann-Whitney U Test; p value was 0.06 when we analyzed the different variables related to patient’s anticoagulation under
ECMO expressed as average of U/Kg of non-fractioned heparin
during ECMO[7-9].
There was no significant statistical difference between nonfractionated
heparin, initial and maximum dose units in dead
patients (20.4 U/Kg) and surviving patients (22.5 U/Kg), with
non-relevant 0.4 p. In terms of ECMO therapy related to nonfractioned
heparin time of use, there was no statistical significance
as there were patients who died into 7.3 days of therapy vs 5.6
days in surviving patients, obtaining a 0.2 p. This is in contrast
to the global literature that according to Cashen documents that
the risk of mortality increased by up to 50 to 60% depending on
anticoagulation therapy[10]; besides, Hee Lee’s study documents
an inherent increase in mortality and complications with ECMO
use related to anticoagulation itself, reaching 40-80%[11].
There was no significant difference in the use of non-fractioned
heparin, including initial, maximum and average doses, as well as
any mortality relationship between therapy time and ACT values;
with all these, we can relate if the patient would be treated using
some type of ECMO therapy.
Anticoagulation protocols used in ChristusMuguerza Alta
Especialidad Hospital have shown benefits non related directly to
patient’s mortality during ECMO. AurunSaini mentions about the
difficulty to keep an adequate anticoagulation in ECMO patient
with 30-60% more probability of bleeding and deathdeath[12].
Although Roeleveld describes that in pathologies with altered
coagulation, between 6 and 30 hours can pass without heparin
perfusion in ECMO, but in our study we did not have intrinsic
complications of the associated pathology[13].
The aim of this study was to identify the influence of variables
on population mortality. Variables themselves did not document
some type of statistical significance, but when variables were put
into a group a significant model was obtained using the Multiple
Logistic Regression Model, showing a 5% mortality related to
these final variables.
“DEATH = ECMO (VA/VV) + AVERAGE LACTATE * AVERAGE VSO2”
Relationship of patient’s mortality, central VSO2 and blood
lactate is globally known, and it is mentioned in much type of
pathologies in the world. Even, medical training textbooks in
Internal Medicine, Pediatrics, Intensive Care, and more, relate
SVO2 increase with survival, and blood lactate increase with high
mortality[14]; but it is important to mention that nowadays there
are no studies documenting direct relationship to survival and
the three variables mentioned above in ECMO patients.
According to previous model, we can relate a better survival
probability with higher central VSO2, and this probability
increases twofold every 5% increase of central SVO2 over 70%
central VSO2; in terms of blood lactate, survival probability
decreases considerably twofold over 4 mmol/Lt blood lactate,
being null survival in case of blood lactate over 10 mmol/Lt.
In world literature, it is well known the relationship between these
two variables and its direct effect on mortality. Asenjo describes
briefly in his work about the need to improve continuously
patient’s values of VSO2 and blood lactate during extracorporeal circulation[15], because they might be related to important hypo
perfusion and high death risk, but without specifying concrete
values on these data. Boedy suggests that mortality is related to
high blood lactate and low central VSO2, therefore treatment
should focus to improve patient’s tissue perfusion monitoring
these two variables; as variable values improve, patient’s
survival would improve[16], but an association variable is not
documented, let alone a cut-off number is indicated for patient’s
improvement, even we know survival should improve, though.
Finally, it is important to note that we could relate ECMO type
use to survival, Venous-Arterial (VA) and Veno-Venous (VV).
There was a better survival probability using VA ECMO compared
to VV ECMO which patients present 4 timer higher probability
to die. Nowadays on this area, there are no reports in literature
related directly to ECMO type, mortality and survival. According
to Ann Arbor and Moreno G, in their respective works, comment
on mortality in ECMO therapy, mentioning anticoagulation as a
direct factor of mortality, but not associating the ECMO[17,18],
but it is important to note that learning curve, heterogeneous
diagnoses in pediatric patients requiring ECMO in our hospital
might have had some influence, and survival improvement due
to a better experience. This is a simple supposition, though, being
a high complexity in this moment to relate directly to a specific
variable because we only related patients to ECMO type. We still
need to determine directly the mortality in each ECMO type, as
world literature reports similar characteristics in complications
and mortality without predominance of one ECMO therapy over
another.
Conclusion
This study demonstrates evidently that Extracorporeal
Membrane Oxygenation (ECMO) stands a maximum responsibility
in monitoring, surveillance, following and multidisciplinary
management for this type of patients.
It was evident in this study that nowadays there is no a significant
relationship between anticoagulation used in ECMO patients
and mortality, this is in our ECMO team and our experience,
even though big success in our surveillance and anticoagulation
monitoring scheme used by our team in ChristusMuguerza Alta
Especialidad Hospital. But this is not to be taken lightly, because
it has been reported a high mortality in patients requiring ECMO,
even in the best facilities hospitals in the world, so we should
consider multiple complications secondary to anticoagulation in
ECMO patients.
Besides, it is an important finding that 5% mortality is related to
central VSO2 and blood lactate. It was possible to give evidence
as probability in these variables, and give more attention on
therapeutic management to systemic perfusion to improve
effectively these variables values, and have a direct influence
on patient’s survival. Another important point is the survival
probability related to ECMO types, but we can’t still have
absolute conclusions on this area because patient’s age, different
diagnoses and multiple co-morbiditywere not evaluated on this
study and they may have some influence on this area, but this
cause was not our goal in this study, giving an opportunity for
more investigation.
Evaluate our work through a good feedback will give strength to
our ECMO Team in ChristusMugherza Alta Especialidad Hospital,
and will continue guiding our work to excellence and wellbeing
for all our patients.
References
- Marilyn Morris, Richard Ittenbach, Rodolfo Godinez, Joel Portnoy, Sarah Tabbutt, et al. (2004) Critical Care Medicine. Crit Care Med 4: 1061-1069.
- Loren C, Raman L, Dalton H (2017) Pediatric extracorporeal membrane oxygenation. Critical Care Clinics 33: 825-841.
- López M (2017) Factores asociados a mortalidad en pacientes tratados con membrana de oxigenación extracorpórea (ECMO) en el trasplante de pulmón. Universidad de Cantabria. Facultad de Medicina Departamento de Medicina y Psiquiatría. España.
- Hwa Jin Cho, Do Wan Kim, Gwan Sic Kim, In Seok Jeong (2017) Anticoagulation therapy during extracorporeal membrane oxygenator support in pediatric patients. Chonnam Medical Journal 53: 110-117.
- Rebecca Barton, Vera Ignjatovic, Paul Monagle (2019) Anticoagulation during ECMO in neonatal and paediatric patients. Tromb Res 173: 172-177.
- Doymaz S (2018) Anticoagulation during ECMO: The Past, Present and Future. J Intensive & Crit Care 4: 12.
- Segura S, Cambra F, Moreno J, Thio M, Riverola A, et al. (2009) ECMO: experiencia en edad pediátrica. Anales de Pediatría 70: 12-19.
- Nilesh M Mehta, David Turner, Brian Walsh, David Zurakowski, Peter Betit, et al. (2010) Factors associated with survival in pediatric extracorporeal membrane oxygenation—a single-center experience. J Pediatric Surgery 45: 1995-2003.
- Kattan J, González A, Castillo A (2013) Oxigenación con membrana extracorpórea neonatal-pediátrica. Revista Chilena de Pediatría 84: 367-378.
- Cashen K, Reeder R, Dalton HJ, Berg RA, Shanley TP, et al. (2018) Hyperoxia and Hypocapnia during pediatric extracorporeal membrane oxygenation: Associations with complications, mortality, and functional status among survivors. Pediatr Crit Care Med 19: 245-253.
- Hee Lee S, Soo-Shin D, Ran J, Kim H (2017) Factors associated with mortality risk in critical care patients treated with veno-arterial extracorporeal membrane oxygenation. Heart and Lung: The Journal of Acute and Critical Care 46: 137-142.
- Arun Saini, Philip C Spinella (2014) Management of Anticoagulation and Hemostasis for Pediatric Extracorporeal Membrane Oxygenation. Clin Lab Med 34: 655-673.
- Roeleveld PP (2017) What is new in Pediatric ECMO? Eur J Heart Fail 19: 92-96.
- Nikoleta SK, Susan LB, Frank WM, Edward LB, Richard GO, et al. (2003) Outcome of pediatric patients treated with extracorporeal life support after cardiac surgery. Ann Thorac Surg 76: 1435-1441.
- Asenjo M, Eiguren K (2017) Soporte vital extracorpóreo. Oxigenación por membrana extracorpórea. ECMO. Revista Española de Perfusión 62: 5-26.
- Boedy F, Howell C, Kanto W (1990) Hidden mortality rate associated with extracorporeal membrane oxygenation. The Journal of Pediatrics 117: 462-464.
- Ann Arbo (2017) ECLS Registry Report International Summary. 2800 Plymouth Road, Building 300, Room 303, ELSO, USA.
- Moreno G, Martinez AG, Berrocal AR, Castilla MS, Fernández JG (2018) Experiencia en el manejo de terapia ECMO como factor de riesgo de mortalidad. Revista Española de Anestesiología y Reanimación 65: 90-95.