Keywords
Health services research; Population-based cancer screening; Colorectal cancer; iFOBT; Healthcare contacts; Telephone helpline
Abbreviations
CRC: Colorectal Cancer; FOBT: Fecal Occult Blood Test; iFOBT: Immunochemical Fecal Occult Blood Test
Introduction
Among the Northern European countries, Denmark has the highest age-standardized incidence rate of Colorectal Cancer (CRC) in men (69.2 per 100,000), and the second-highest age-standardized incidence rate in women (53.4 per 100,000) [1]. Screening with the biennial Fecal Occult Blood Test (FOBT) has shown a 15% relative risk reduction in CRC mortality in the general population, and a 25% relative risk reduction for those attending at least one round of screening [2]. Programs using FOBT have shown uptake rates of 53-67%, with the highest uptake for programs using the Immunochemical Fecal Occult Blood Test (iFOBT), compared with Guaiac Fecal Occult Blood test (gFOBT) [3].
By 2008, national CRC screening was either ongoing, or in the process of being established in 19 of 27 EU countries. Of the remaining countries (Belgium, Denmark, Estonia, Ireland, Lithuania, Luxembourg, Malta, and the Netherlands), all have since implemented CRC screening programs [4,5]. The Danish CRC screening program was implemented in March 2014 as the first population-based cancer screening program offered to both men and women; routine screening for breast cancer and cervical cancer has been offered to Danish women for several years. The CRC screening program offers home-based iFOBT self-sample kits, sent directly to the home, with the invitation to participate in the screening program. There is also a recommendation to make use of the helpline in instances of queries regarding the screening process. The telephone helpline is seen as providing an opportunity for citizens and patients to readily reach healthcare providers, and constitutes a necessary safety measure implemented by the provider. In most countries, telephone helplines are key components of the healthcare system; they facilitate communication with health professionals, and help to ensure patient safety. Supposedly, all of the CRC screening programs offer a telephone helpline to assist those with questions or concerns. However, thus far, systematic analyses of the calling patterns of telephone helpline users have not been undertaken. This represents a missed opportunity to learn about unfulfilled needs, or barriers to the success of population-based screening. The aim of this study was to analyze the calling patterns for a telephone helpline used to support the Danish CRC screening program in the Central Denmark Region, which is the second-largest region, constituting 22.4% of the Danish population [6]. Our analyses contain a description of the sex and age characteristics of helpline users, compared to a background population, and explore their motives for calling, with a particular focus on the screening invitation.
Methods
Setting
Denmark has a population of 5,717,000 with 1,282,000 citizens residing in the Central Denmark Region. The administration of all public cancer screening programs in this region is centralized to a single screening unit, based in a regional hospital (Randers). During implementation of the screening program in Denmark (2014-2018), all citizens aged 50-74 will be invited once. Thereafter, eligible individuals will be invited every other year. In 2016, approximately 384,000 citizens in the Central Denmark Region will be aged 50 to 74.
Procedures in the Danish colorectal cancer screening program
Invitations to participate in CRC screening are mailed to individuals aged between 50 and 74 years of age. Pending their first screening round, citizens are randomly invited according to their month of birth, except those aged 49, who are invited just before they turn 50. In addition, individuals aged 74 are contacted if they turn 75 before the pending screening round are over. The invitation letter contains an offer to participate in screening, a pamphlet from the health authorities about the benefits and risks associated with participation, an iFOBT self-sample screening kit with a user guide, and a pre-addressed, pre-paid envelope with which to return the sample to a screening lab. Failure to respond to the invitation will trigger a reminder after 45 days. If the individual participates and the result is negative, this result is transmitted via secure e-mail. In cases of a positive test, the test result is sent to the screening unit, which dispatches the result to the individual by mail, including a pre-booked appointment for a colonoscopy, and laxative for bowel preparation. Secretarial staff complete the calls in the vast majority of cases but also, on occasion, divert calls to those with medical expertise (general practitioner or surgeon). It is possible to unregister from the screening program online (www.sundhed.dk), by calling the helpline, or by sending a letter. The screening invitation explains that individuals with a prior colorectal cancer diagnosis are ineligible for participation. This also goes for individuals who are regularly examined for polyps. Patients with Morbus Crohn or Colitis Ulcerosa are asked to discuss participation with their doctor.
Design
This was a cross-sectional study using questionnaires and register data from an in-house database; the study constitutes part of a quality control program in the department.
Questionnaire data
The questionnaire was developed to collect data about the age and sex of each caller, and motives for calling. Secretarial staff completed the questionnaire during and immediately after telephone calls about CRC screening. The questionnaire was developed following participant observation by the first author in the screening administration unit for one month [7]. This observation involved informal conversations with unit staff about their experiences with helpline users, and observations of their telephone conversations. In this process, recurrent questions and preliminary insights were noted by the secretaries and the researcher, with categories subsequently devised for the questionnaire. A questionnaire was then drafted, installed on tablets, and pilot-tested by the secretaries to provoke further suggestions. After one month of iterative refinement, the final version of the questionnaire was installed, and the pilot-phase was terminated. Questionnaire data included age and sex, together with the following categories: ‘Unsubscribing from screening’, ‘New screening kit', ‘Counseling', ‘Rebooking appointment for colonoscopy’, ‘Referral to other personnel', ‘Test reply’, and ‘Other'. Each category consisted of variables, e.g. 'Stick' in the category 'New screening kit'. Each telephone call might touch on several topics, and thus contribute to more than one category and variable. Each category contained an 'Other' variable, with a free text option, e.g. 'New screening kit, other: [free text]'. At the end of the questionnaire was a final free text option categorized as "other", which served as a "catchment" for any supplementary information. If the authors assessed that a free text entry belonged to an already defined variable, then this text was re-assigned as appropriate. Free text entries that did not belong to an already defined variable were placed in a new variable if more than 15 entries shared a feature/a topic. The secretaries collected questionnaire data for all telephone consultations from April 23rd 2015 until June 24th 2015, 43 work days in total.
Register data
In-house register data for the background population included age, sex, and date of invitation. Invitations to participate are mailed, allowing the postal service a 3-day delivery window. In-house register data for all eligible individuals were retrieved from April 20th 2015 until June 24th 2015.
Data analyses
Pearson’s chi-squared test was used to estimate differences in sex and age between helpline users and the background population. Multiple logistic regression analyses with adjusted odds ratios were used to examine sex and age characteristics associated with topics in the helpline calls. The age group 49-54, and female sex was reference variables in our analyses. All estimates are presented with 95% confidence intervals, carried out to a 5% significance level. The reporting of the results adheres to the STROBE guidelines [8].
Ethics
According to Danish law about ethical approval of healthcare studies, quality control program studies, questionnaire studies and register-based studies without human tissue are exempt from notification to the Danish National Committee on Health Research Ethics [9]. Accordingly there is no obligation to obtain formal consent from individuals whose calls were registered.
Results
Age and sex characteristics associated with calls to the helpline
During the study period, 1,666 telephone calls were registered by the helpline staff, of which 1,630 were sufficiently registered to be included in the analyses (Figure 1).
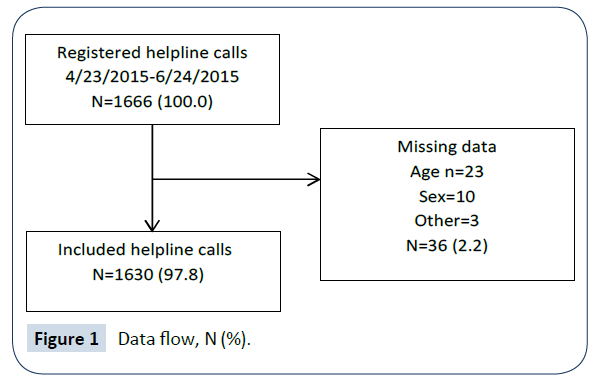
Figure 1: Data flow, N (%).
The background population comprised all 22,692 citizens in the catchment area who had received a screening invitation during the study period. Thus, the helpline was ultimately used by 7.3% of citizens invited to the screening program. Men and women were equally distributed in the background population (50.0%; 95% CI: 49.43-50.8), but not in the telephone helpline group (43.3%; 95% CI: 40.9-45.8) and this difference was statistically significant. Overall, there were a lower number of men than women using the helpline. This difference was statistically significant and held for all age groups (38.3%; 95% CI: 32.7-44.1 (helpline) and 51.0%; 95% CI: 49.9-52.2 (background)) except for those aged 71-75, where no significant differences were detected (50.7%; 95% CI: 46.0-55.4 vs. 50.0%; 95% CI: 48.4-51.5) (Table 1).
| |
Helpline group |
Background population |
| N=1,630 (%) |
N=22,692 (%) |
| 95% CI |
95% CI |
| Sex |
|
|
| Female |
924 (56.7) |
11,327 (50.0) |
| 54.2-59.1 |
49.26-50.6 |
| Male |
706 (43.3) |
11,365 (50.0) |
| 40.9-45.8 |
49.43-50.8 |
| Total |
1,630 (100.0) |
22,692 (100.0) |
| Age group (years) |
|
| 49-54 |
113 (38.3) |
3,529 (51.0) |
| 32.7-44.1 |
49.8-52.2 |
| 55-60 |
105 (42.2) |
2,183 (48.8) |
| 36.0-48.6 |
47.3-50.3 |
| 61-65 |
107 (40.5) |
1,822 (50.7) |
| 34.6-46.7 |
49.0-52.3 |
| 66-70 |
153 (41.1) |
1,857 (49.5) |
| 36.1-46.3 |
47.9-51.1 |
| 71-75 |
228 (50.7) |
1,974 (50.0) |
| 46.0-55.4 |
48.4-51.5 |
Table 1: Age group and sex characteristics.
Motives for calling
In the majority of cases, unsubscribing from the screening program was the main motive for calling (25.3%), followed by queries about the screening kit (22.7%), counseling (22.2%), re-booking of appointment for colonoscopy (14.5%), other personnel (e.g. calls directed to a surgeon) (12.8%), test reply (2.5%), and other queries (1.6%) (Table 2).
| Categories |
Unsubscribing
N=412
n (%)
95% CI |
Screening kit
N=370
n (%)
95% CI |
Counselling
N=362
n (%)
95% CI |
Re-booking
N=237 (%)
n (%)
95% CI |
Other personnel
N=209 (%)
n (%)
95% CI |
Test reply
N=40 (%)
n (%)
95% CI |
Other
n (%)
95% CI |
| |
| Sex |
| Women |
259 (28.0) |
217 (23.5) |
189 (20.5) |
124 (13.4) |
104 (11.3) |
27 (2.9) |
17 (1.8) |
| |
25.2-31.1 |
20.8-25.4 |
17.9-23.2 |
11.3-15.8 |
9.2-13.3 |
1.9-4.2 |
1.1-2.9 |
| Men |
153 (21.7) |
153 (21.7) |
173 (24.5) |
113 (16.0) |
105 (14.9) |
13 (1.8) |
9 (1.3) |
| |
18.7-24.9 |
18.7-24.9 |
21.4-27.9 |
13.4-18.9 |
12.2-17.5 |
1.0-3.1 |
0.6-2.4 |
| Age group (years) |
| 49-54 |
30 (10.2) |
94 (31.9) |
77 (26.1) |
50 (17.0) |
33 (11.2) |
7 (2.4) |
6 (2.0) |
| |
7.0-14.2 |
26.6-37.5 |
21.2-31.5 |
12.9-21.7 |
7.6-14.8 |
1.0-4.8 |
0.8-4.4 |
| 55-60 |
51 (20.5) |
67 (26.9) |
57 (22.9) |
40 (16.1) |
30 (12.1) |
5 (2.0) |
3 (1.2) |
| |
15.7-26.0 |
21.5-32.9 |
17.8-28.6 |
11.7-21.2 |
8.0-16.1 |
0.7-4.6 |
0.3-3.5 |
| 61-65 |
64 (24.2) |
57 (21.6) |
67 (25.4) |
29 (11.0) |
37 (14.0) |
8 (3.0) |
9 (3.4) |
| |
19.2-29.9 |
16.8-27.1 |
20.2-31.1 |
7.5-15.4 |
9.8-18.2 |
1.3-5.9 |
1.6-6.4 |
| 66-70 |
123 (33.1) |
62 (16.7) |
75 (20.2) |
51 (13.7) |
50 (13.4) |
8 (2.2) |
6 (1.6) |
| |
28.3-38.1 |
13.0-20.9 |
16.2-24.6 |
10.4-17.6 |
10.0-16.9 |
0.9-4.2 |
0.6-3.5 |
| 71-75 |
144 (32.0) |
90 (20) |
86 (19.1) |
67 (14.9) |
59 (13.1) |
12 (2.7) |
4 (0.4) |
| |
27.7-36.5 |
16.4-24.0 |
15.6-23.1 |
11.7-18.5 |
10.0-16.2 |
1.4-4.6 |
0.1-16.0 |
| Total |
412 (25.3) |
370 (22.7) |
362 (22.2) |
237 (14.5) |
209 (12.8) |
40 (2.5) |
26 (1.6) |
| |
23.2-27.5 |
20.7-24.8 |
20.2-24.3 |
12.9-16.4 |
11.2-14.5 |
1.8-4.0 |
1.0-2.3 |
Table 2: Motives for calling the helpline.
Calls about the screening invitation
Certain calls to the helpline would result in a request for a new screening kit to be dispatched, usually because of a broken kit (stick n=14, paper n=33), sampling failure (n=25), or missing ID label (n=100); these are summarized in Table 3 as 'New kit due to inappropriate use' (N=172). Other calls concerned missing invitations or samples (N=166). These included individuals who had mislaid their invitation (n=67), had their samples lost in the post (n=79), or other related miscellaneous errors (n=20). There were no statistically significant differences between the sexes or across age groups in terms of these calls. Questions about the invitation letter (n=187), advice on how to collect the stool sample (n=43), and when/how to return it to the laboratory (n=47), are summarized (N=277) in 'Counseling about screening invitation'. The calls were evenly distributed across age groups and sex. Calls about a follow-up colonoscopy, including questions about diet or bowel preparation (n=34), various worries (n=5), or questions about common diseases (n=1), are summarized in 'Counseling about colonoscopy'. The majority of these calls came from men, with this gender difference being statistically significant (OR=2.2, 95% CI: 1.8-4.3), and apparent across the age groups (Table 3).
| |
New kit due to inappropriate use* |
New kit due to lost invitation or sample** |
Counselling about screening invitation^ |
Counselling about follow- up colonoscopy^^ |
| |
N=172 |
OR |
N=166 |
OR |
N=277 |
OR |
N=40 |
OR |
| |
n (%) |
(adjusted) |
n (%) |
(adjusted) |
n (%) |
(adjusted) |
n (%) |
(adjusted) |
| |
|
95% CI |
|
95% CI |
|
95% CI |
|
95% CI |
| Sex |
| Women |
102 (59.3) |
1 |
93 (56.0) |
1 |
150 (54.1) |
1.00 |
15 (37.5) |
1 |
| Men |
70 (40.7) |
1 |
73 (44.0) |
1.2 |
127 (45.9) |
0.71 |
25 (62.5) |
2.2 |
| |
|
0.7-1.5 |
|
0.8-1.8 |
|
0.43-1.17 |
|
1.8-4.3 |
| Age group (years) |
|
|
|
|
|
|
|
|
| 49-54 |
41 (23.8) |
1 |
38 (22.9) |
1 |
63 (22.7) |
1 |
9 (22.5) |
1 |
| 55-60 |
34 (19.8) |
1.3 |
28 (16.9) |
1.1 |
46 (16.6) |
1 |
5 (12.5) |
0.7 |
| |
|
0.7-2.5 |
|
0.6-2.0 |
|
0.4-2.4 |
|
0.2-2.1 |
| 61-65 |
28 (16.3) |
1.2 |
27 (16.3) |
1.3 |
45 (16.3) |
0.5 |
12 (30.0) |
1.6 |
| |
|
0.6-2.4 |
|
0.7-2.6 |
|
0.2-1 |
|
0.6-4.2 |
| 66-70 |
25 (14.5) |
0.9 |
33 (19.9) |
1.7 |
59 (21.3) |
0.8 |
7 (17.5) |
0.8 |
| |
|
0.5-1.7 |
|
0.9-3.2 |
|
0.4-1.8 |
|
0.3-2.2 |
| 71-75 |
44 (25.6) |
1.2 |
40 (24.1) |
1.2 |
64 (23.1) |
0.7 |
7 (17.5) |
0.6 |
| |
|
0.7-2.2 |
|
0.7-2.1 |
|
0.3-1.5 |
|
0.2-1.7 |
| |
*Paper or stick broke during sampling, sampling failed, or ID label missing |
**Invitation or sample went missing in the mail, or failure made by distribution company |
^Questions about invitation, how to take the sample and when/how to send it in |
^^Questions about diet or bowel preparation, worry, or ordinary disease |
Table 3: Calls about the screening invitation.
Discussion
The helpline was used by 7.3% of the individuals invited to the screening program during the study period. Significantly fewer men than women used the helpline, and this difference was statistically significant in all age groups except for those aged 71-75 years. The main motives for calling the helpline were unsubscribing from the program, the screening kit, and a need for counseling. In calls about the screening invitation, no statistically significant differences were detected between men and women, or across age groups, except for calls about follow-up colonoscopy where more calls came from men than women.
Strengths and Limitations
The helpline staff made a considerable contribution to the design of the questionnaire, and rehearsed the final version for one month in a pilot study. Ensuring that the staff felt confident about using the questionnaire was a quality control measure designed to reduce the risk of incorrect entries. The exact number of unique callers remains unknown as each individual might call more than once. However, we assumed that these multiple calls would be rare. Our study showed a significant difference between calls from men versus women regarding unsubscribing and counseling about colonoscopy. It is important to bear in mind that the number of calls about unsubscribing from the service does not reflect the actual number of those leaving the program, as this option was also available on the internet, and in writing. More importantly, calls about follow-up colonoscopy may not reflect the actual need for counseling as citizens may instead opt to approach their general practitioner or surgery for advice related to the procedure. The fact that more men than women called about follow-up colonoscopy may also reflect the greater proportion of men that receive a positive screening result, and hence a larger number of invitations for follow-up colonoscopy.
It could be argued that the period of registration used was not representative for the entire program, but routine surveillance of the number of calls to the helpline showed that usage during the study period was in line with the average call number ordinarily received.
Interpretation
Our study identified fewer calls to the helpline from men versus women, which mirrors their lower participation rate in CRC screening programs [10]. In Denmark, population-based cancer screening programs for breast and cervical cancer have been available to women for many years. As a consequence, women may have grown accustomed to screening invitations as opposed to men, for whom this is a relatively new phenomenon. It may also reflect that healthcare-seeking behavior and management of health differ between men and women [11]. It might be more socially legitimate for women to discuss their health with their friends, family, and colleagues, more so than for men. Besides being rooted in physiology and gender roles, the difference between men and women in their healthcare-seeking behavior is also influenced by medical advances and political priorities [12]. Our study showed that only in those aged 71-75, did the proportion of men relative to women in the calling group match that of the background population. In other analyses of those using the helpline, no significant differences across age groups were identified, other than in the category 'Counseling about colonoscopy'. This finding might be explained by the higher proportion of men invited to a follow-up colonoscopy, although our data showed that age was not a predictor for calling about any specific topic.
Calls requesting replacement screening kits hamper the screening program. In an attempt to reduce the number of these calls, the self-sampling procedure could be refined by optimizing the paper design for the toilet bowl, with a better fit and stronger texture. Likewise, issues with the ID label might also be accommodated. The current procedure is to instruct the participant to double-check the label, and then attach it to the sample, thereby reducing the risk of misidentification. However, direct labeling prior to shipment could reduce the number of samples that are necessarily discarded because of faulty labeling.
In 2014, a short instruction video was uploaded to YouTube by the Capital Region of Denmark, and by February 1st 2017 it had been viewed 8,000 times. A link to this type of video might be included in invitation letters to support the written instructions enclosed with the screening kit, thereby reducing the number of calls. Future research should evaluate the effect of such web-based support.
Calls to a helpline are, in part, an outcome of an unmet need for individuals invited to a screening program. Helpline services are an essential remit of public health programs, and a tacit acknowledgement that no amount of written information can substitute for personalized advice. However, the limited degree to which individuals currently engage with the helpline in the second-largest region in Denmark, suggests that this service could, perhaps, be scaled back without jeopardizing safety. A feasible approach would be some degree of centralized, crossregional service.
Conclusion
The Danish CRC screening program is the first population-based cancer screening program offered to both men and women in Denmark. It is essential for the operation and maintenance of a screening program to understand which individuals call the helpline and their motives for calling. Our experience from the helpline service in the second-largest region in Denmark may guide future initiatives to establish support services, either online or by telephone, to individuals about population-based screening programs in other countries.
Declarations
Ethics
Approval by the National Committee on Health Research Ethics is not required because the data are based on questionnaires and registers [9].
Consent to participate
There is no obligation to obtain formal consent in this type of study [9].
Competing interests
The authors declare that they have no competing interests.
Authors' contributions
PK, MBL and BA designed the study. PK conducted the pilot study and finalized the questionnaire. MBL and BA assisted with the analysis, and PK made the final write-up of the manuscript. All authors read and approved the final manuscript.
Acknowledgements
We wish to thank the secretarial staff at Department of Public Health Programmes, Central Denmark Region, and data manager Anne Marie Schak Jensen from DEFACTUM, Central Denmark Region, and Denmark.
References
- Ferlay J, Steliarova-Foucher E, Lortet-Tieulent J, Rosso S, Coebergh JW, et al. (2013) Cancer incidence and mortality patterns in Europe: estimates for 40 countries in 2012. Eur J Cancer 49: 1374-1403.
- Hewitson P, Glasziou P, Watson E, Towler B, Irwig L (2008) Cochrane systematic review of colorectal cancer screening using the fecal occult blood test (hemoccult): an update. Am J Gastroenterol 103: 1541-1549.
- Holme O, Bretthauer M, Fretheim A, Odgaard-Jensen J, Hoff G (2013) Flexible sigmoidoscopy versus faecal occult blood testing for colorectal cancer screening in asymptomatic individuals. Cochrane Database Syst Rev 9: CD009259.
- Organisation for Economic Co-operation and Development (OECD) (2012) Screening, survival and mortality for colorectal cancer: in health at a glance: Europe 2012. OECD Publishing, UK.
- Zavoral M, Suchanek S, Zavada F, Dusek L, Muzik J, et al. (2009) Colorectal cancer screening in Europe. World J Gastroenterol 15: 5907-5915.
- Statistics Denmark (2016) FOLK1A: Population at the first day of the quarter by region, sex, age and marital status.
- Spradley JP (2006) Participant observation: the ethnographic interview. Admin Sci Q 25: 526-530.
- Vandenbroucke JP, Von Elm E, Altman DG, Gotzsche PC, Mulrow CD, et al. (2007) Strengthening the reporting of observational studies in epidemiology (STROBE): explanation and elaboration. PLoS Med 4: e297.
- The Danish Ministry of Health (2011) Ministry of health - pools for research and health.
- Clarke N, Sharp L, Osborne A, Kearney PM (2015) Comparison of uptake of colorectal cancer screening based on fecal immunochemical testing (FIT) in males and females: a systematic review and meta-analysis. Cancer Epidemiol Biomarkers Prev 24: 39-47.
- Charles N, Walters V (2008) 'Men are leavers alone and women are worriers': Gender differences in discourses of health. Health Risk Soc 10: 117-132.
- Schofield T, Connell RW, Walker L, Wood JF, Butland DL (2000) Understanding men's health and illness: a gender-relations approach to policy, research, and practice. J Am Coll Health 48: 247-256.