Case Report - (2022) Volume 5, Issue 7
Evoking Chyle Production to Facilitate Cervical Catheterization and Embolization of Injured Thoracic Duct: Case Report
Adel Ahmed*,
Laila Qadan and
Muhammad Shozab Ahmed
Department of Radiology, Kuwait University, Kuwait City, Kuwait
*Correspondence:
Adel Ahmed, Department of Radiology, Kuwait University, Kuwait City,
Kuwait,
Email:
Received: 21-Jul-2022, Manuscript No. IPJIIR-22-14004;
Editor assigned: 23-Jul-2022, Pre QC No. IPJIIR-22-14004(PQ);
Reviewed: 06-Aug-2022, QC No. IPJIIR-22-14004;
Revised: 10-Oct-2022, Manuscript No. IPJIIR-22-14004(R);
Published:
17-Oct-2022, DOI: 10.21767/2471-8564.5.7.30
Abstract
Iatrogenic Thoracic Duct (TD) injury is a serious complication of neck surgery. TD embolization after Intranodal Lymphangiography (INL) has been reported to be safe and successful. Retrograde catheterization of the TD through a cervical lymphocyte without using INL could be challenging due to difficult visualization of the TD. The authors describe a method to increase the turgor of the TD thus facilitate its visualization and cannulation by evoking chyle production using high fat diet in combination with a closed drainage system. The method proved to be practical and safe.
Keywords
Chyle leak; Thoracic duct injury; Thoracic duct embolization
Introduction
Inadvertent Thoracic Duct (TD) injury with chylous leakage is a
serious complication of neck surgery [1-7]. Percutaneous
antegrade and retrograde embolization of the TD following
Intranodal Lymphangiogram (INL) have been used with high
rates of safety and success. Retrograde visualization and
cannulation of the TD under fluoroscopic guidance without
INL could be challenging [8]. Here, we report a transcervical
percutaneous catheterization of a transected TD at the point
of its communication with a cervical lymphatic collection.
Retrograde fluoroscopic visualization and cannulation of the
TD was possible after 24 hours of a high fat diet coupled with
the creation of a closed drainage system.
Case Presentation
Institutional review board approval for case reports is not
required at our institution. A 28 years old female with a history of papillary thyroid cancer underwent total
thyroidectomy with lymph node dissection. The patient was
discharged one day postoperatively to present three weeks
later with a palpable le t supraclavicular swelling. Ultrasound
(US) showed a 6 x 5.6 x 5 cm luid collection. The luid aspirate
had a triglyceride concentration of 525 mg/dL consistent with
chyle. The patient was readmitted to initiate conservative
management namely oral fat restriction, total parenteral
nutrition, somatostatin infusion, and percutaneous drainage
of the luid collection. Nine days of conservative measures
failed to stop chyle leakage. Due to her recent extensive
thyroid bed surgery, surgical ligation of the TD was not
favored, and TD embolization seemed to be the treatment of
choice. Preprocedural Magnetic Resonance
Lymphangiography (MRL) using heavily T2 weighted
sequences revealed a luid collection in the le t
supraclavicular area communicating with a severed TD at its
posteromedial aspect (Figure 1).
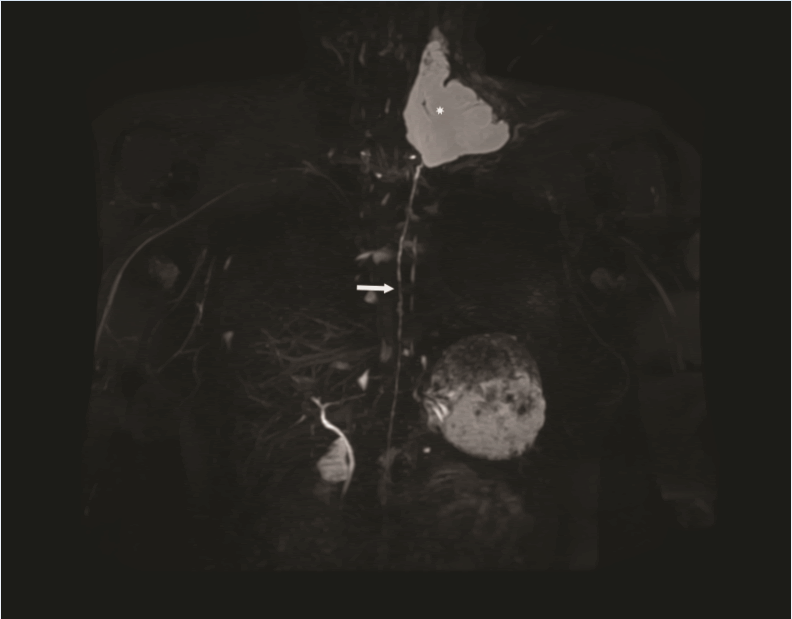
Figure 1: Coronal heavily T2-weighted MR image showing the
entire length of the thoracic duct (white arrow) with a
severed end communicating with a fluid collection at the base
of the left neck (asterisk).
A plan to attempt retrograde catheterization of TD using the
preexisting drainage catheter was formulated. Under
fluoroscopic guidance, the fluid collection was aspirated, and
iodinated water soluble contrast (Visipaque 270 mg/ml, GE
healthcare) was then injected. However, the contrast failed to
demonstrate a reflux into the TD (Figure 2).
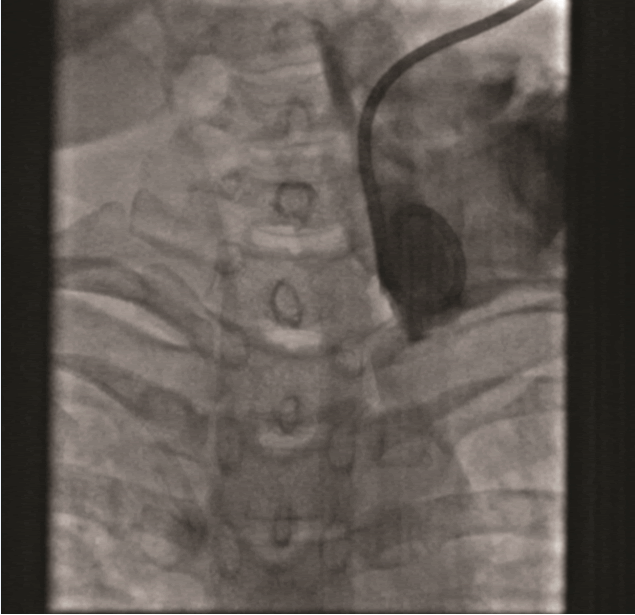
Figure 2: Spot fluoroscopic image after injection of water
soluble iodinated contrast through the drainage catheter with
no retrograde filling of the thoracic duct.
Therefore, the drainage catheter was removed over a Bentson
wire (cook medical, Europe), and a multipurpose catheter was
introduced instead with an attempt to cannulate the TD at the
previously MRL visualized communicating junction with the
collection, but the TD was inaccessible. Thus, it was assumed
that the ongoing conservative therapy (with oral fat
restriction and continuous external drainage of the chylous
collection) has resulted in a low pressure system with a collapsed TD which is hard to catheterize. Therefore, the
drainage catheter was reintroduced and closed to external
drainage. Additionally, the patient was placed on a high fat
diet for 24 hours to enhance chyle production, and octreotide
was held. The hypothesis was that a high outflow of chyle into
a closed drainage system would likely increase the turgor of
the TD, dilate it and promote its retrograde filling with
contrast. The patient was given prophylactic antibiotics
coverage (Clindamycin 600 mg). Next day, water soluble
contrast medium was injected through the drainage catheter
into the chylous collection, this time the distal severed end of
the TD at the posteromedial aspect of the collection was
clearly visualized with reflux of contrast into the upper third
of the TD (Figure 3).
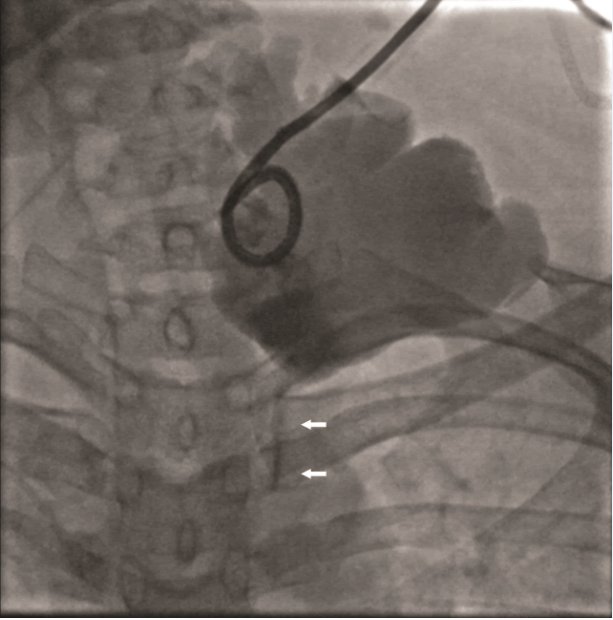
Figure 3: Spot fluoroscopic image obtained after direct
injection of contrast into the closed drainage system following
24 hours of a high-fat diet, demonstrating reflux of contrast
into the thoracic duct (white arrows).
A micro puncture set (MAK 401 merit medical, Ireland) was
used to access the fluid collection under fluoroscopic
guidance. The micro puncture needle was pointed towards
the severed end of the TD. A wire was introduced and a 5-F
dilator (cook medical, Europe) with a manually formed 45
degree angle at its tip was advanced into the collection. A
0.035 glide wire (Terumo, Europe) was then used to
selectively catheterize the TD. A 4-F C-2 glide catheter
(Terumo, Europe) was advanced to the level of the Cisterna
Chyli (CC). A lymphangiogram was obtained using water
soluble contrast and concurred with the MRI findings (Figure
4).
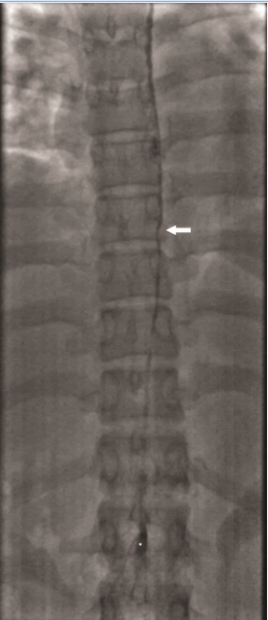
Figure 4: Spot fluoroscopic image demonstrating successful
retrograde catheterization of the thoracic duct with 4-F Cobra
Catheter (arrow at catheter tip) with contrast opacified
cisterna chyli (asterisk).
Embolization from the CC up to the severed end of the TD was
done using a 1:3 mixture of N-Butyl Cyanoacrylate (NBCA)
(Glubran2-GEM, Italy) and lipiodol (Guerbet, France). A
column of polymerized glue was seen throughout the TD.
However, few minutes later the column started to flocculate
(Figure 5A and B).
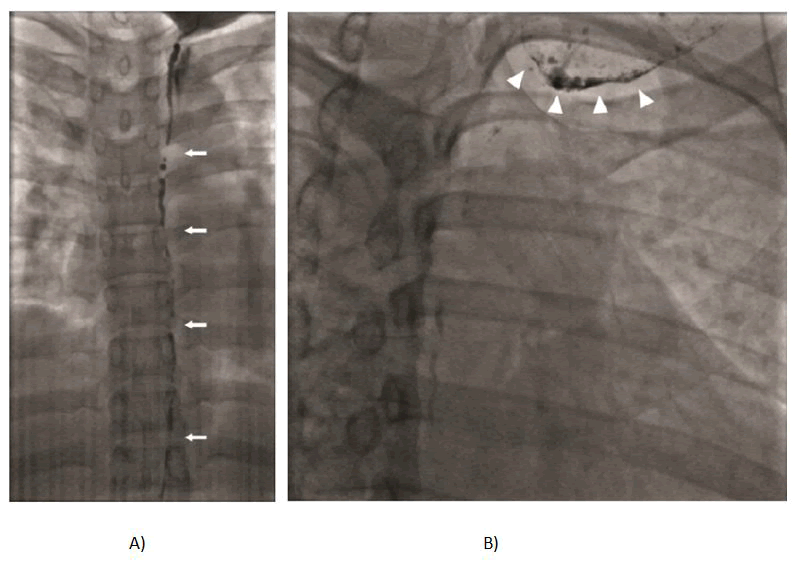
Figure 5: A) Spot Fluoroscopic image obtained 5 minutes after
embolization showing fragmentation of embolic NBCA:
Lipiodol (1:3) mixture (white arrows). The embolic material
travelled in an ante grade direction and accumulated at the
point of leakage into the chylous collection; B) Antegrade
migration of the embolic mixture is visualized with
accumulation at the leakage site of the thoracic duct into the
lymphocyte (arrow heads).
The procedure was aborted anticipating that the glue would
seal the leaking end of the TD, but chyle drainage through the
catheter continued for 24 hours after the procedure. A plan to
re attempt embolization was set. In preparation for the
procedure, the drainage catheter was closed again to external
drainage and the patient was put once again on a high fat
diet. Twenty four hours later, fluoroscopic images showed
reanalyzed severed TD. Similar puncturing and catheterization
techniques to the initial attempt were utilized. A micro
catheter (2.7/2.9 F procreate; Terumo, Europe) was advanced
to the CC, 4 mm coils (vortex diamond 18, Boston scientific,
Ireland) were deployed in the TD at 3-4 cm intervals and a 1:1
mixture of NBCA and lipiodol was used. Fluoroscopic images
taken 10 minutes later showed an adequately solidified
mixture throughout the entirety of the TD (Figure 6).
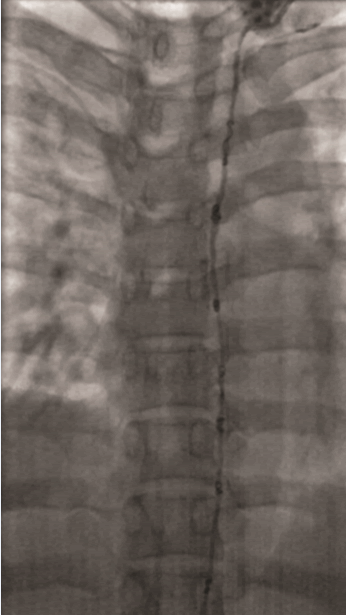
Figure 6: Fluoroscopic image showing successful
retrograde embolization of the thoracic duct with NBCA:
Lipiodol (1:1) mixture and multiple micro coils.
The drainage catheter was left in situ and no fluid output was
detected for 24 hours. A next day CT scan of the neck
and chest showed lipiodol cast embolization of the entire TD
with no fluid collection in the neck (Figure 7).
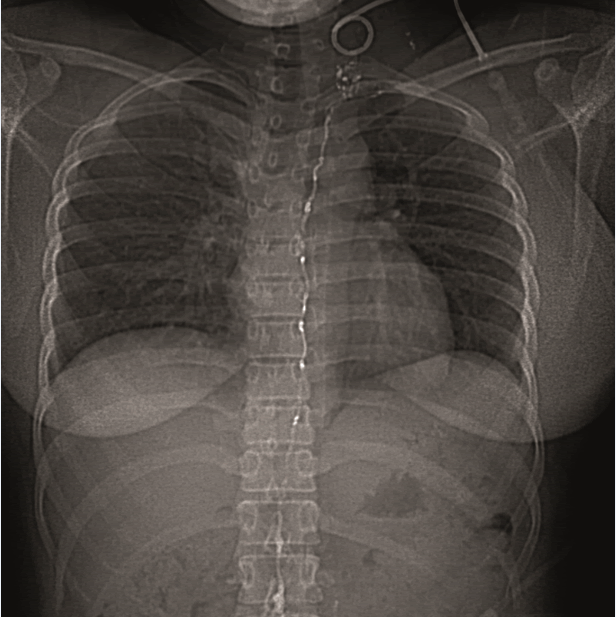
Figure 7: Follow up coronal CT scan gram of the neck and
chest showing stable NBCA: Lipiodol cast and micro coils
throughout the entire thoracic duct 24 hours after
embolization.
The drainage catheter was removed, and the patient was
discharged home a day later. At one, two and six months
follow ups, the patient was asymptomatic, had neither neck
nor lower limbs swelling [9-14].
Results and Discussion
TD injury is a known complication of head and neck surgery
with a reported incidence that ranges between 0.5 up to 8%
depending on the type of surgery and lymph node dissection
(1-6). It is associated with increased morbidity due to
prolongation of hospitalization, risk of malnutrition,
immunosuppression, and electrolyte imbalance. In many
cases, conservative measures are successful in controlling the
leakage. However, in those where these measures fail, a
surgical or interventional radiological solution would be
required. Although surgical intervention was originally
thought by some as the optimal approach, it has been
associated with increased morbidity and mortality in addition
to possible failure. Over the last decade, percutaneous
embolization of the TD gained momentum as a safe and
successful alternative in the treatment of a leaking lymphatic
duct following neck dissection. Most described approaches to
TD embolization are with trans abdominal or retrograde
accesses following INL. INL is time consuming, logistically
demanding and requires oil based contrast which carries an
embolic risk. Therefore, different groups tried alternative
approaches without the need for INL. Transvenous retrograde
embolization after neck dissection has been reported by
Arslan. This approach requires the identification of the
confluence of TD with the subclavian vein which could be
quite challenging. US guided direct puncture of the TD at its
venous insertion has been described recently and seems to be a promising alternative. Retrograde access of the TD via a
cervical lymphocyte without an INL was done by warren, who
stated that although the approach is feasible it is not
necessarily amenable in all cases, with the possible failure to
visualize and emblaze the injured duct. That failure proved to
be true both when Pieper et al attempted a similar approach
and during our first attempt to visualize the TD, by injecting
contrast material into the lymphocyte. Physiological
expansion of the lymphatic duct by increasing the lymphatic
flow using a high fat diet and increasing back pressure by
clamping the drainage catheter seemed to exert enough
pressure on the TD to dilate it and make it accessible to
visualization and cannulation. This proved to be efficacious
and reproducible since the procedure was repeated after
failure of the first embolization. Over expansion of a closed
drainage system can result in sepsis especially in a patient
with a prolonged external drainage and possible bacterial
colonization, therefore, prophylactic antibiotics coverage was
used for the procedure. MRL plays a significant role in
negating the need for INL too. It provides information on both
the anatomy and the pathology of the lymphatic system. In
our case, MRL clearly delineated the chylous collection and its
point of communication with the severed TD and it played a
key role in planning for the procedure. Therefore, we
recommend doing MRL using heavily T2 weighted sequences
in preparation for all cases of planned cervical retrograde
annulation. Although NBCA dilution of 1:3 has been used
successfully for TD embolization, the same dilution was
reported to be unsuccessful. Furthermore, a dilution of 1:4
was deemed partially successful and required reembolization.
This could reflect a difference between NBCA
formulations regarding viscosity and rate of polymerization. In
our first embolization attempt, a 1:3 dilution of Glubran 2
NBCA was used and monitored for polymerization. Few
minutes after the initial polymerization the column
flocculated and the TD re opened. Re embolization using a 1:1
dilution with coils was successful. Therefore, if Glubran 2
NBCA formulation were to be used, we recommend a 1:1
dilution with or without coils for a higher rate of success.
Conclusion
In conclusion, the combination of a high fat diet and a closed
drainage system seems to dilate the TD thus make it more
accessible to catheterization and embolization via a
retrograde approach. Although the success of such
combination was reproducible in our patient, and averted the
need for INL, the future applicability in a series of patients
would be more assertive.
References
- Delaney SW, Shi H, Shokrani A, Sinha UK (2017) Management of chyle leak after head and neck surgery: review of current treatment strategies. Int J Otolaryngol. 2017:1-12.
[Crossref][Google Scholar][Indexed]
- Park I, Her N, Choe JH, Kim J, Kim JH (2018) Management of chyle leakage after thyroidectomy, cervical lymph node dissection, in patients with thyroid cancer. Head Neck. 40:7-15
[Crossref][Google Scholar][Indexed]
- Polistena A, Vannucci J, Monacelli M (2016) Thoracic duct lesions in thyroid surgery: an update on diagnosis, treatment and prevention based on a cohort study. Int J Surg. 28:33-37.
[Crossref][Google Scholar][Indexed]
- Ilczyszyn A, Ridha H, Durrani A (2011) Management of chyle leak post neck dissection: A case report and literature review. J Plast Reconstr Aesthetic Surg. 64:223-230
[Crossref][Google Scholar][Indexed]
- Jin S, Sugitani I (2021) Narrative review of management of thyroid surgery complications. Gland Surg. 10:1135-1146
[Crossref][Google Scholar][Indexed]
- Moussa A, Maybody M, Gonzalez Aguirre A, Buicko J, Shaha A, et al. (2020) Thoracic duct embolization in post-neck dissection chylous leakage: A case series of 6 patients and review of the literature. Cardiovasc Intervent Radiol. 2020;43(6):931-937
[Crossref][Google Scholar][Indexed]
- Warren P, Hogan M, Shiels W (2013) Percutaneous transcervical thoracic duct embolization for treatment of a cervical lymphocele following anterior spinal fusion: a case report. J Vascv Intrev Radiol. 24:1901-1905
[Crossref][Google Scholar][Indexed]
- Pieper C, Schild H. Direct cervical puncture for retrograde thoracic duct embolization in a postoperative cervical lymphatic fistula. J Vasc Interv Radiol. 2015;26:1405-1408
[Crossref][Google Scholar][Indexed]
- Guevara C, Rialon K, Ramaswamy R, Kim S, Darcy M (2016) US guided, direct puncture retrograde thoracic duct access, lymphangiography, and embolization: feasibility and efficacy. J Vasc Interv Radiol. 27:1890-1896
[Crossref][Google Scholar][Indexed]
- Pieper C (2020) Nodal and pedal MR lymphangiography of the central lymphatic system: techniques and applications. Semin Intervent Radiol. 37:250-262
[Crossref][Google Scholar][Indexed]
- Arslan B, Masrani A, Tasse JC, Stenson K, Cenk Turba U. Super selective retrograde lymphatic duct embolization for management of postoperative lymphatic leak. Diagn Interv Radiol. (5):379-380.
[Crossref][Google Scholar][Indexed]
- Lorenz J, Thomas J (2006) Complications of percutaneous fluid drainage. Semin Intervent Radiol. 23:194-204.
[Crossref][Google Scholar][Indexed]
- Praveen A, Sreekumar K, Nazar P, Moorthy S (2012) Technical note: thoracic duct embolization for treatment of chylothorax: a novel guidance technique for puncture using combined MRI and fluoroscopy. Indian J Radiol Imaging. 22:89-92
[Crossref][Google Scholar][Indexed]
- Hur J, Hur S, Shin J, Kwon S, Hyun D, et al. (2021) Reversed approach through lymphocele/lymphatic fluid collection for glue embolization of injured lymphatic vessels. J Vasc Interv Radiol. 32:299-304
[Crossref][Google Scholar][Indexed]
Citation: Ahmed A, Qadan l, Ahmed MS (2022) Evoking Chyle Production to Facilitate Cervical Catheterization and Embolization
of Injured Thoracic Duct: Case Report. J Imaging Interv Radiol. 5:30.
Copyright: © 2022 Ahmed A, et al. This is an open-access article distributed under the terms of the Creative Commons
Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author
and source are credited







